The DCB Technology Symposium Coronary Session The DCB

The DCB Technology Symposium - Coronary Session: The DCB Technology Symposium - Coronary Long-Term Survival Benefit of DCB Versus DES for ISR Despite Angiographic Disadvantage of DCB Azeem Latib MD Montefiore Medical Center New York, USA

Disclosure Statement of Financial Interest Within the past 12 months, I or my spouse/partner have had a financial interest/arrangement or affiliation with the organization(s) listed below. Affiliation/Financial Relationship • Grant/Research Support • Consulting Fees/Honoraria • Scientific Advisory Board Company Medtronic, Mitralign, Millipede, Amaranth Medical, Nuvera, Supira, Philips, Acist Medical, Abbott Vascular, Keystone Heart, ICS, Cardiovalve, Cor. Flow, Bioventrix
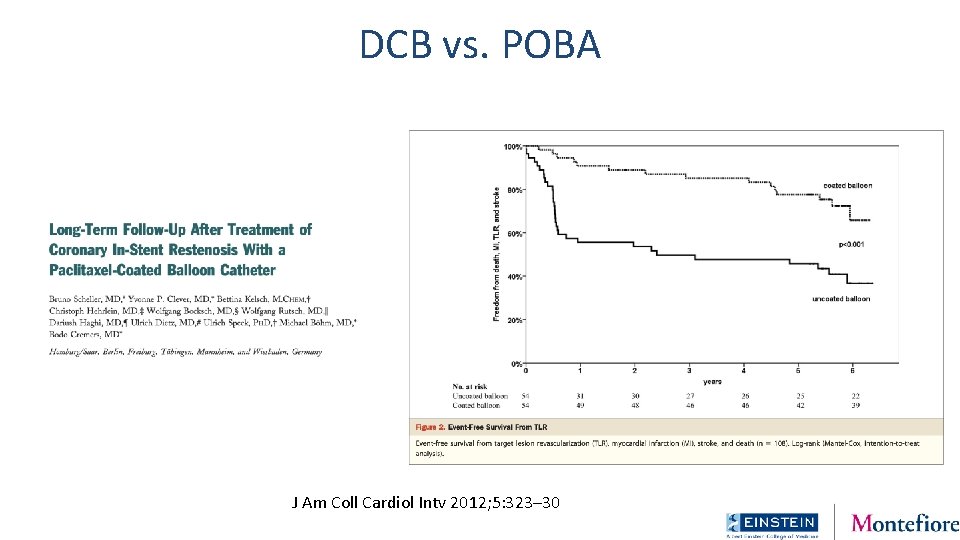
DCB vs. POBA J Am Coll Cardiol Intv 2012; 5: 323– 30
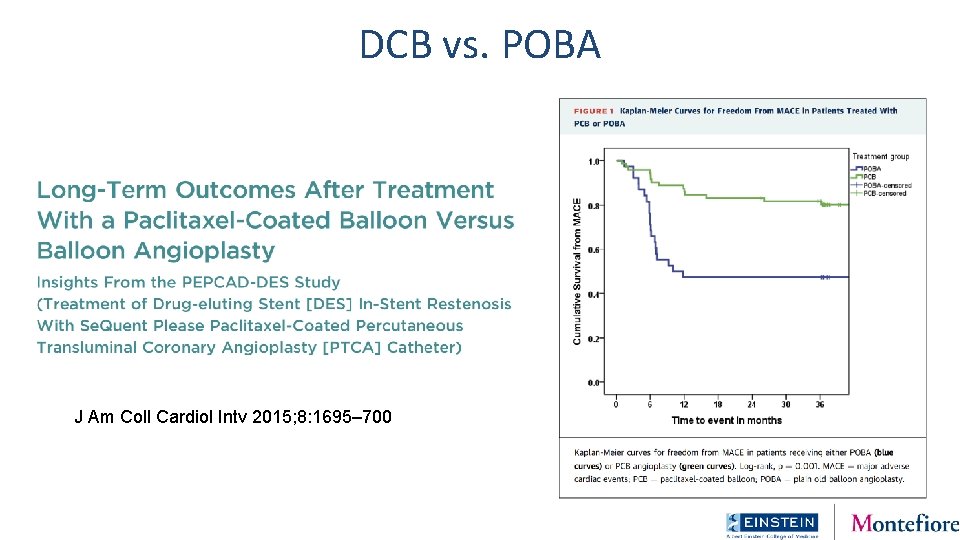
DCB vs. POBA J Am Coll Cardiol Intv 2015; 8: 1695– 700
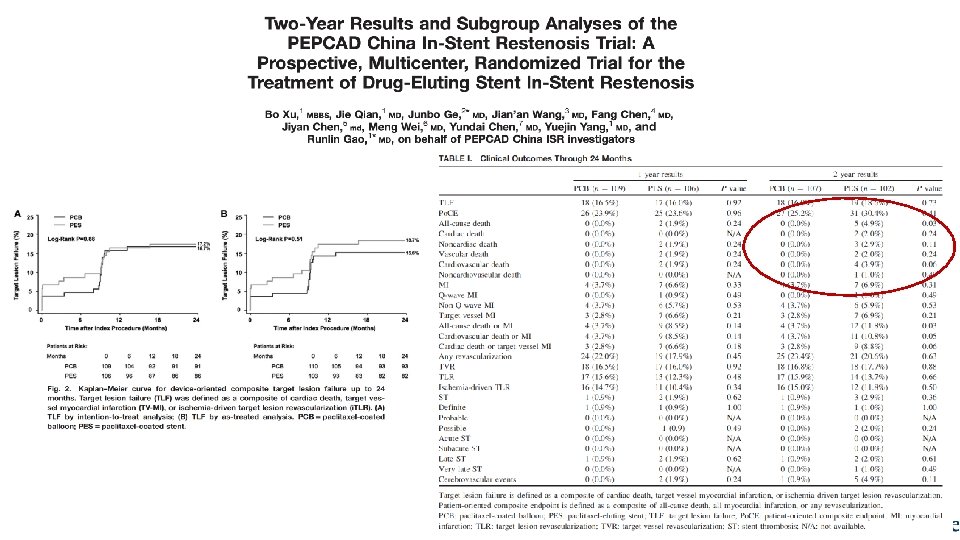
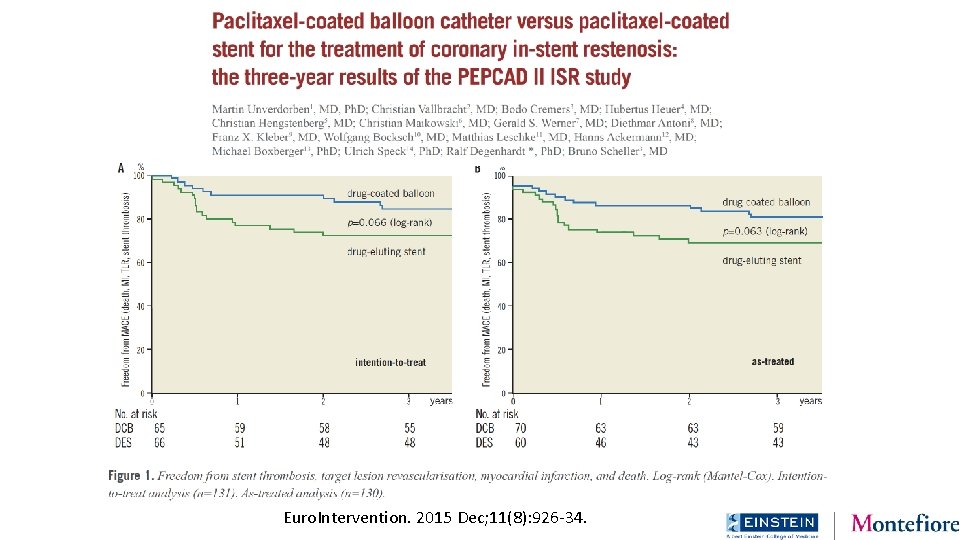
Euro. Intervention. 2015 Dec; 11(8): 926 -34.
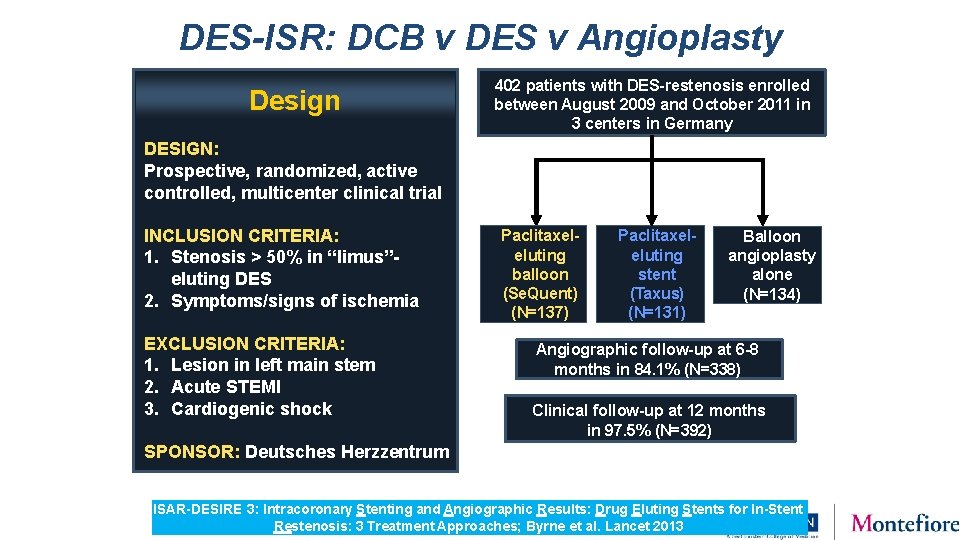
DES-ISR: DCB v DES v Angioplasty Design 402 patients with DES-restenosis enrolled between August 2009 and October 2011 in 3 centers in Germany DESIGN: Prospective, randomized, active controlled, multicenter clinical trial INCLUSION CRITERIA: 1. Stenosis > 50% in “limus”eluting DES 2. Symptoms/signs of ischemia EXCLUSION CRITERIA: 1. Lesion in left main stem 2. Acute STEMI 3. Cardiogenic shock SPONSOR: Deutsches Herzzentrum Paclitaxeleluting balloon (Se. Quent) (N=137) Paclitaxeleluting stent (Taxus) (N=131) Balloon angioplasty alone (N=134) Angiographic follow-up at 6 -8 months in 84. 1% (N=338) Clinical follow-up at 12 months in 97. 5% (N=392) No significant differences across groups ISAR-DESIRE 3: Intracoronary Stenting and Angiographic Results: Drug Eluting Stents for In-Stent Restenosis: 3 Treatment Approaches; Byrne et al. Lancet 2013
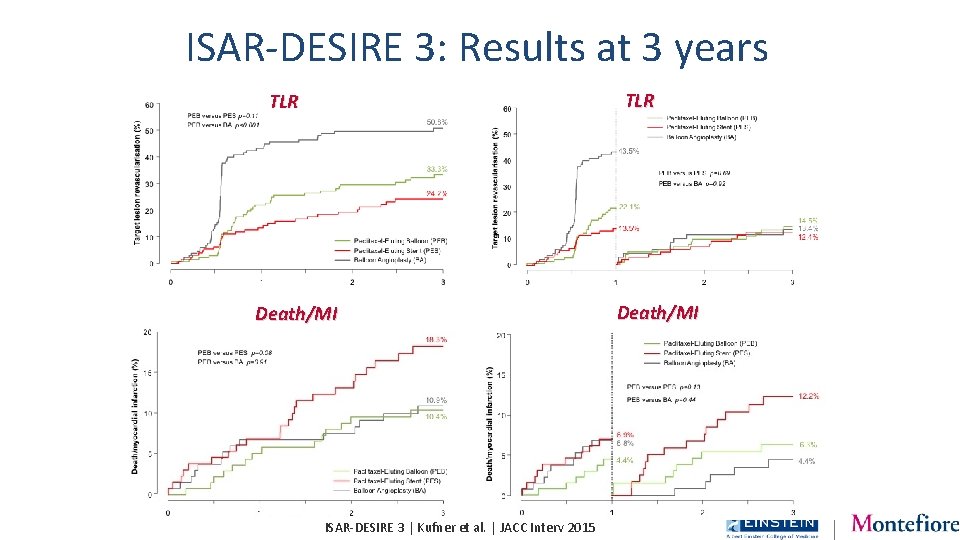
ISAR-DESIRE 3: Results at 3 years TLR Death/MI ISAR-DESIRE 3 | Kufner et al. | JACC Interv 2015 Death/MI

RIBS IV (Januray 2010 – August 2013) Inclusion Criteria Informed Consent 309 Pts DES-ISR Randomization Rx Centralized Stratification: ISR Length & Edge Xience Prime (Abbott Vascular) 4 Died 18 Refused 1 Thrombosis Se. Quent Please 155 Pts EES 100% Angiographic Success 154 Pts DEB 133 Pts Angio FU QCA Primary End-point (90%) 139 Pts Angio FU 155 Pts Clinical FU 3 -Year Clinical FU (100%) 154 Pts Clinical FU (B. Braun) 3 Died 12 Refused
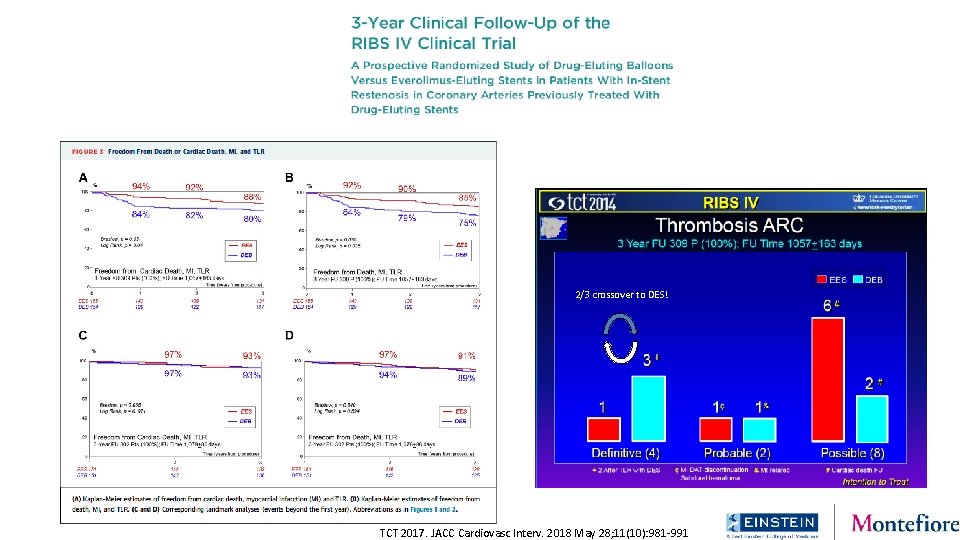
2/3 crossover to DES! TCT 2017. JACC Cardiovasc Interv. 2018 May 28; 11(10): 981 -991

Lesson learned from DCB pre-dilatation in ISR Suboptimal angiographic result of pre-dil before DCB predicts TLR • Retrospective analysis of ISRs treated by DCB with PTCA pre-dil • N=166 classified as “adequate” or “inadequate” based on pre-dil results: • “adequate” (N=98): TIMI 3, %DS ≤ 30%, NO major dissections • “inadequate (N=68): TIMI <3 or %DS >30% or major dissections • median follow-up: 808 days Tanaka A, Latib A, Jabbour RJ, Kawamoto H, Giannini F, Ancona M, Regazzoli D, Mangieri A, Mattioli R, Chieffo A, Carlino M, Montorfano M, Colombo A. Impact of Angiographic Result After Predilatation on Outcome After Drug-Coated Balloon Treatment of In-Stent Coronary Restenosis. Am J Cardiol. 2016 Aug 24. pii: S 0002 -9149(16)31366 -2
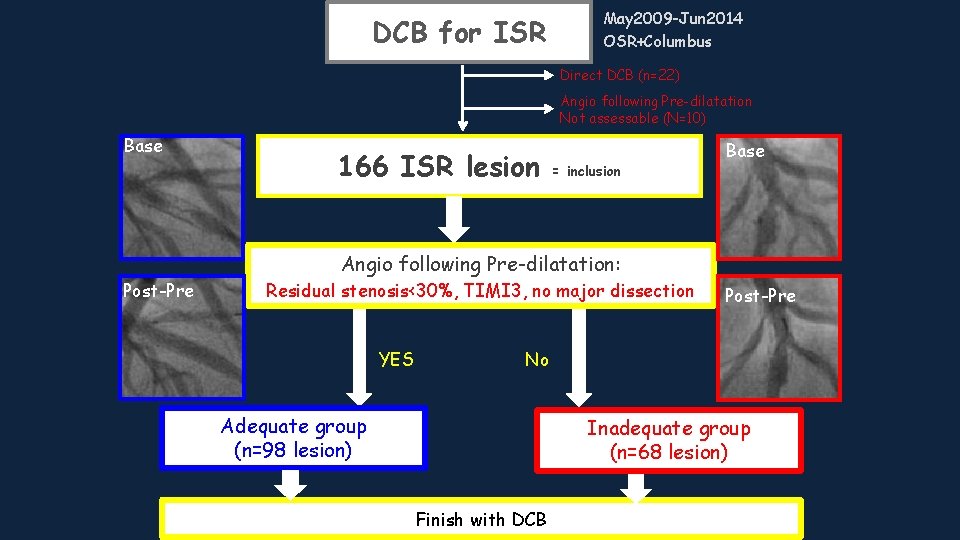
DCB for ISR May 2009 -Jun 2014 OSR+Columbus Direct DCB (n=22) Angio following Pre-dilatation Not assessable (N=10) Base 166 ISR lesion = inclusion Base Angio following Pre-dilatation: Post-Pre Residual stenosis<30%, TIMI 3, no major dissection YES Post-Pre No Adequate group (n=98 lesion) Inadequate group (n=68 lesion) Finish with DCB
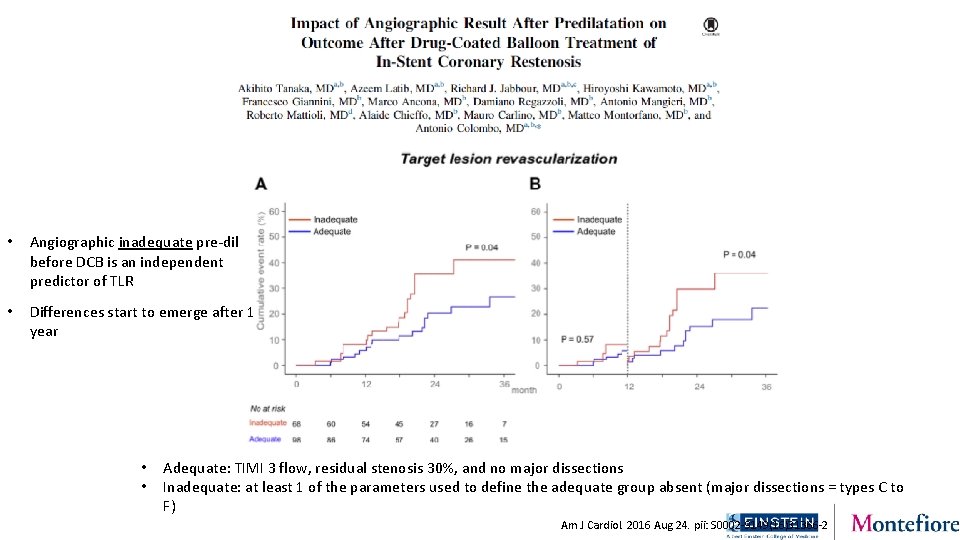
• Angiographic inadequate pre-dil before DCB is an independent predictor of TLR • Differences start to emerge after 1 year • • Adequate: TIMI 3 flow, residual stenosis 30%, and no major dissections Inadequate: at least 1 of the parameters used to define the adequate group absent (major dissections = types C to F) Am J Cardiol. 2016 Aug 24. pii: S 0002 -9149(16)31366 -2
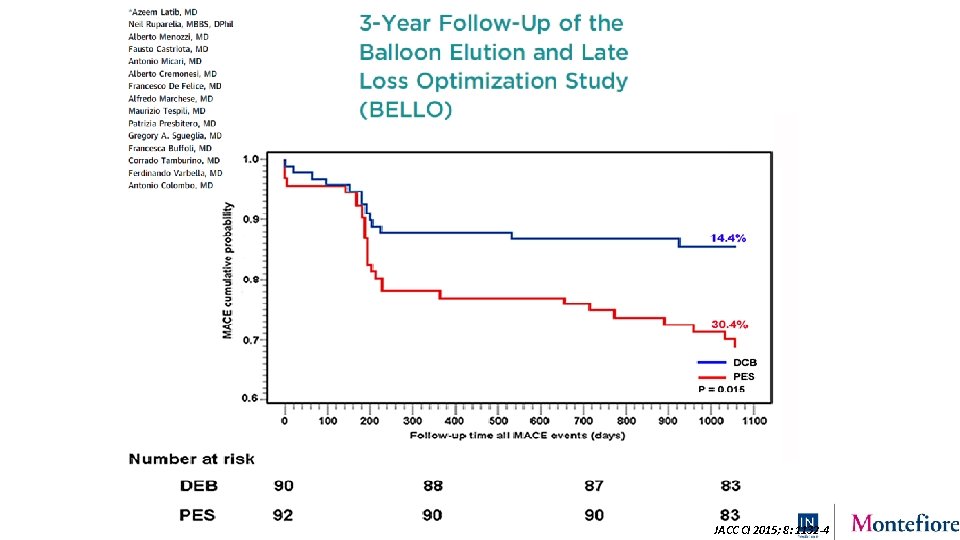
JACC CI 2015; 8: 1132 -4
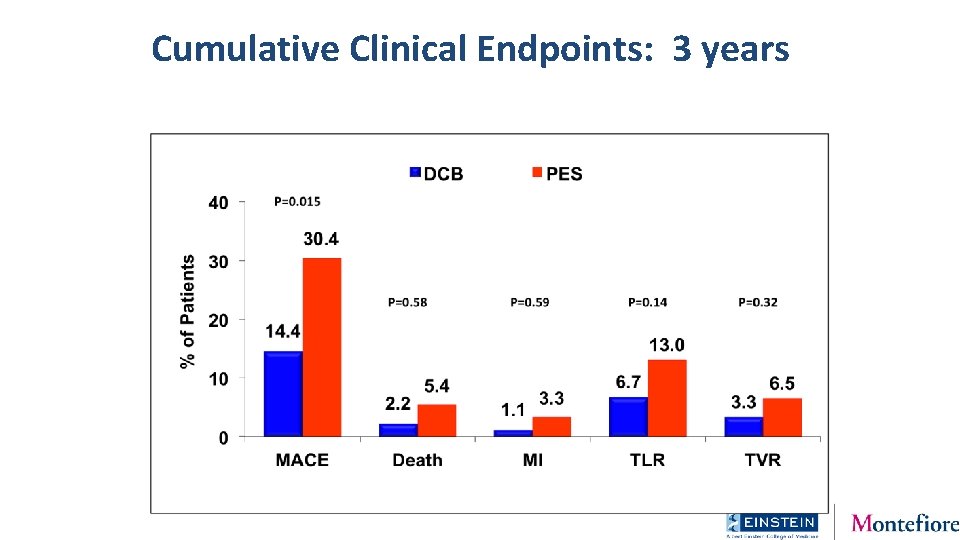
Cumulative Clinical Endpoints: 3 years
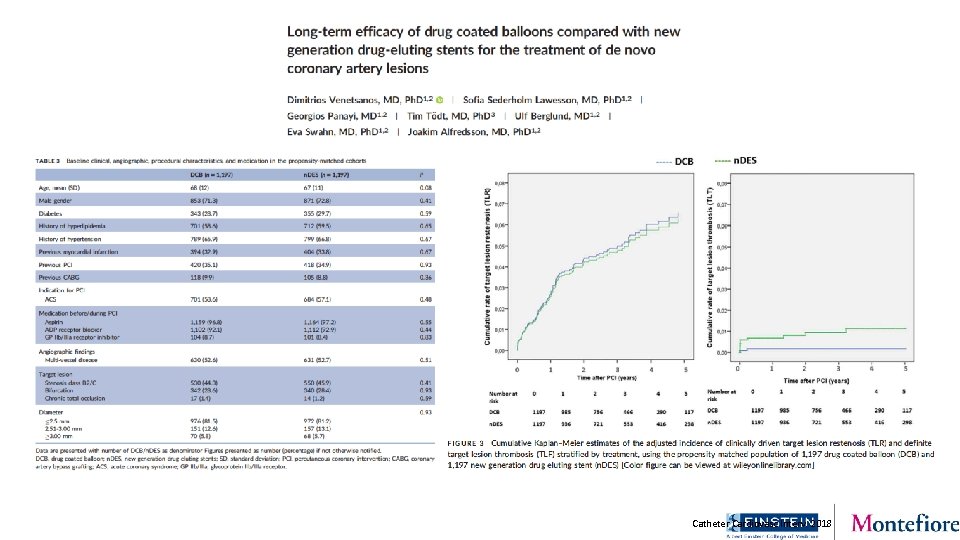
Catheter Cardiovasc Interv. 2018
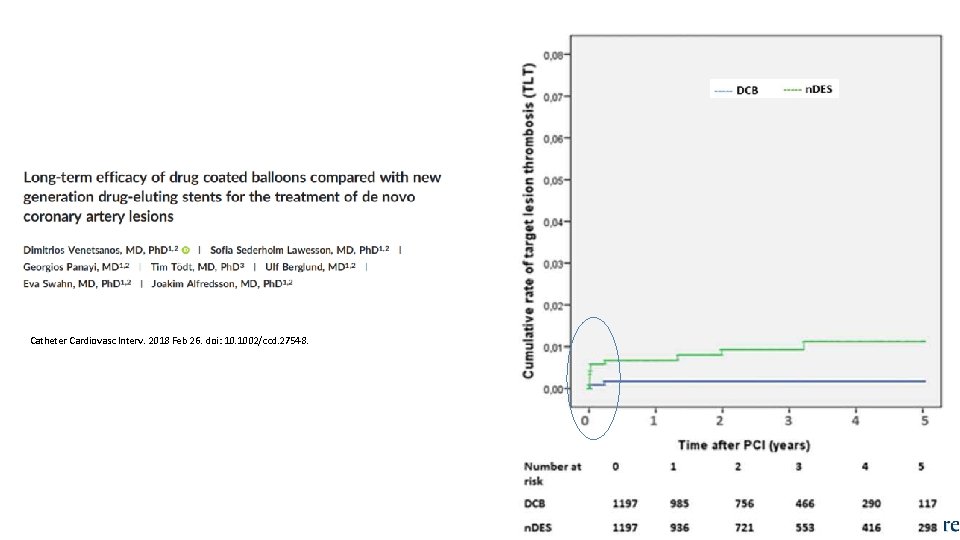
Catheter Cardiovasc Interv. 2018 Feb 26. doi: 10. 1002/ccd. 27548.

Conclusions • Angiographic result after lesion prep is most important factor in deciding between DCB vs. stent • Results with DCB are improved by having a better angiographic result • Limited long-term data on DCB • Available data confirm good long-term outcomes and no mortality signal after treatment of ISR and de novo disease • Mechanism? ? Absence of metallic cage? ?
- Slides: 18