The Chronic Care Model Developed by Ed Wagner

The Chronic Care Model

Developed by Ed Wagner, MD, MPH and colleagues Mac. Coll Institute for Healthcare Innovation Group Health Cooperative of Puget Sound home of the Robert Wood Johnson Foundation National Program, Improving Chronic Illness Care

The IOM Quality report: A New Health system for the 21 st Century

The IOM Quality report: A New Health system for the 21 st Century “The current care systems cannot do the job. ” n “Trying harder will not work. ” n “Changing care systems will. ” n

Usual Chronic Illness Care n n n 15 minute visit, poorly organized Symptoms and lab results focus of discussion and exam, not preventive assessment Patient’s attempts to discuss difficulties in living with the condition are discouraged Focus is on physician’s treatment, not patient’s role in management. Treatment plan is limited to prescription refill and encouragement to make appointment if not feeling well Visit ends with physician rifling through drawers looking for a pamphlet improving chronic illness care
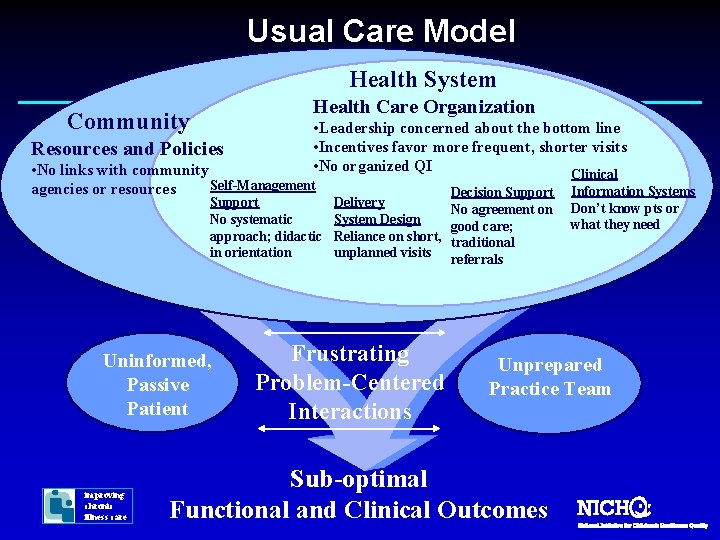
Usual Care Model Health System Health Care Organization Community Resources and Policies • Leadership concerned about the bottom line • Incentives favor more frequent, shorter visits • No organized QI Clinical • No links with community Self-Management agencies or resources Support No systematic approach; didactic in orientation Uninformed, Passive Patient improving chronic illness care Delivery System Design Reliance on short, unplanned visits Frustrating Problem-Centered Interactions Decision Support No agreement on good care; traditional referrals Information Systems Don’t know pts or what they need Unprepared Practice Team Sub-optimal Functional and Clinical Outcomes
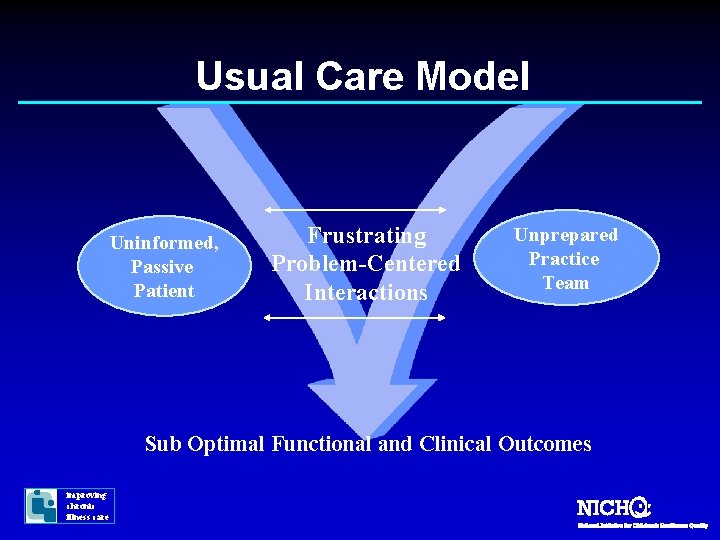
Usual Care Model Uninformed, Passive Patient Frustrating Problem-Centered Interactions Unprepared Practice Team Sub Optimal Functional and Clinical Outcomes improving chronic illness care

Chronic Care Model Informed, Activated Patient Supportive, Integrated Community Productive Interactions Prepared, Proactive Practice Team Functional and Clinical Outcomes Satisfaction Clinical Measures Cost External Review Measures

Chronic Care Model Development 1993 -n n n Initial experience at GHC Literature review RWJF Chronic Illness Meeting -- Seattle Review and revision by advisory committee (40 members (32 active participants) Interviews and site visits with 72 nominated “best practices” Model applied with diabetes, geriatrics, asthma, CHF, and depression with over 200 health care organizations

Themes in the Chronic Care Model n Evidence-based – Valuing excellence (and evidence) over autonomy n Patient-centered – Each patient is the only patient n Population-based
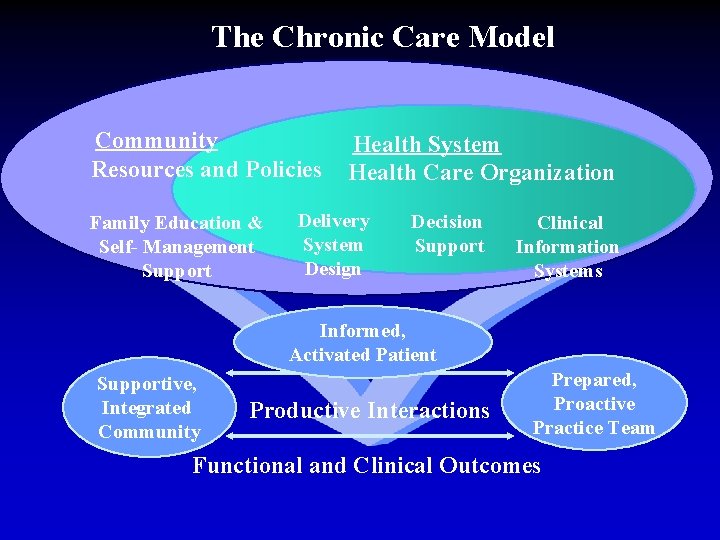
The Chronic Care Model Community Resources and Policies Family Education & Self- Management Support Health System Health Care Organization Delivery System Design Decision Support Clinical Information Systems Informed, Activated Patient Supportive, Integrated Community Productive Interactions Prepared, Proactive Practice Team Functional and Clinical Outcomes
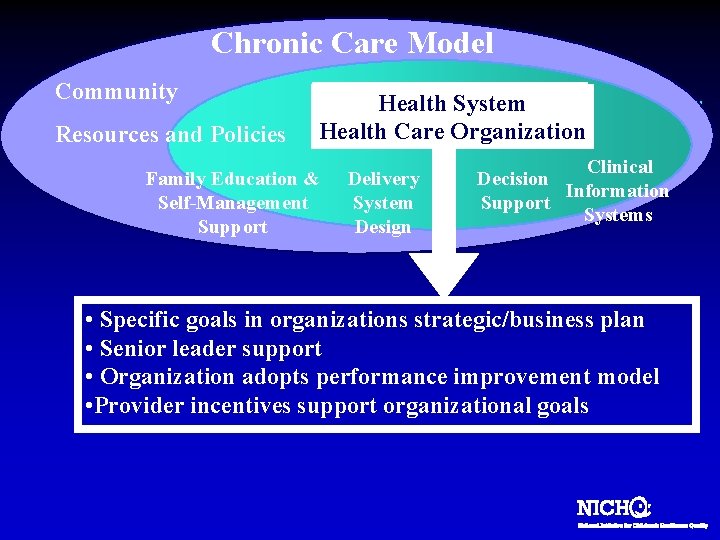
Chronic Care Model Community Resources and Policies Health System Health Care Organization Family Education & Self-Management Support Delivery System Design Clinical Decision Information Support Systems • Specific goals in organizations strategic/business plan • Senior leader support • Organization adopts performance improvement model • Provider incentives support organizational goals
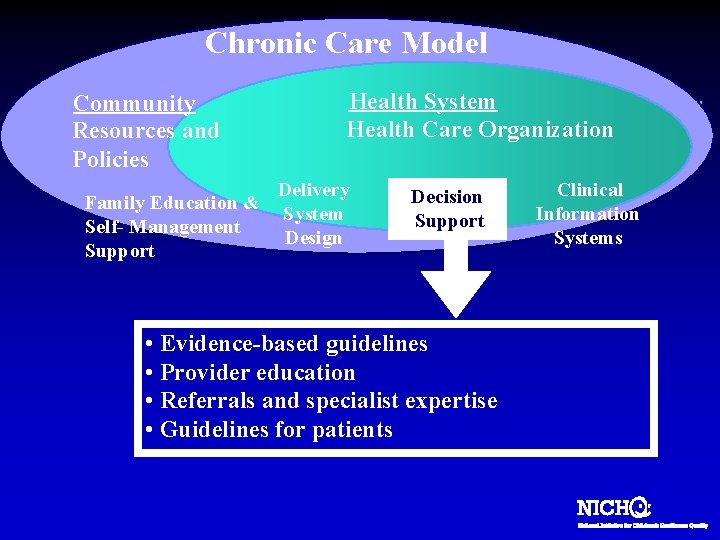
Chronic Care Model Community Resources and Policies Family Education & Self- Management Support Health System Health Care Organization Delivery System Design Decision Support • Evidence-based guidelines • Provider education • Referrals and specialist expertise • Guidelines for patients Clinical Information Systems
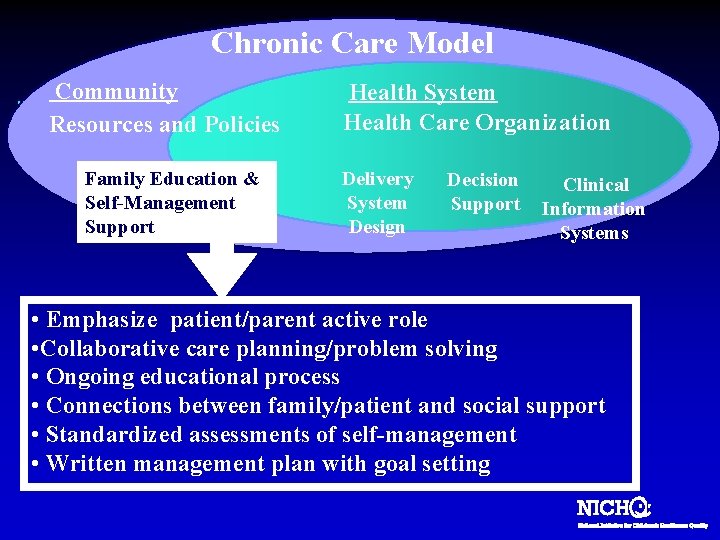
Chronic Care Model Community Resources and Policies Family Education & Self-Management Support Health System Health Care Organization Delivery System Design Decision Support Clinical Information Systems • Emphasize patient/parent active role • Collaborative care planning/problem solving • Ongoing educational process • Connections between family/patient and social support • Standardized assessments of self-management • Written management plan with goal setting
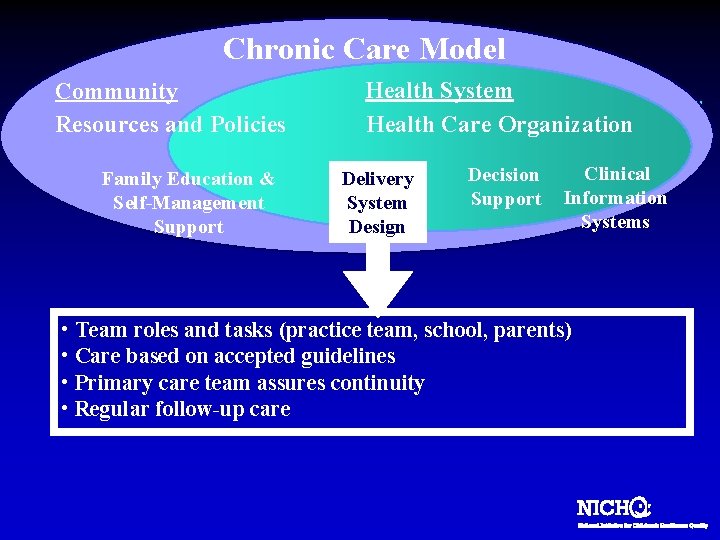
Chronic Care Model Community Resources and Policies Family Education & Self-Management Support Health System Health Care Organization Delivery System Design Decision Support Clinical Information Systems • Team roles and tasks (practice team, school, parents) • Care based on accepted guidelines • Primary care team assures continuity • Regular follow-up care

Chronic Care Model Community Resources and Policies Family Education & Self-Management Support Health System Health Care Organization Delivery System Design Decision Support Clinical Information Systems • Registry to track clinically useful and timely information • Registry reports/data for feedback • Care reminders • Assure timely planned follow-up • Identification/proactive care of relevant patient subgroups • Individual patient care planning
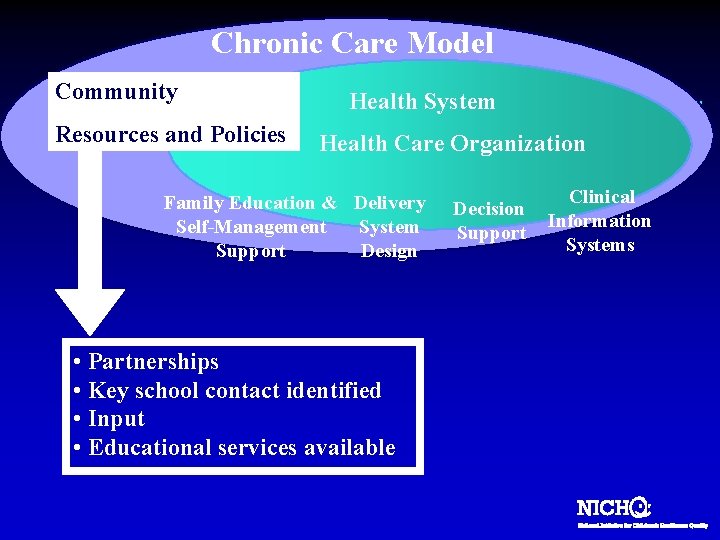
Chronic Care Model Community Resources and Policies Health System Health Care Organization Family Education & Delivery Self-Management System Support Design • Partnerships • Key school contact identified • Input • Educational services available Decision Support Clinical Information Systems

How Would I Recognize Good Care for People with Chronic Illness? Supportive, Integrated Community Informed, Activated Patient Productive Prepared, Proactive Interactions Practice Team Functional and Clinical Outcomes • Assessment and tailoring • Collaborative problem definition • Evidence-based clinical management • Goal-setting and problem-solving • Shared care plan • Active, sustained follow-up • Community integration and support
- Slides: 18