The Challenges of Fungi in Cystic Fibrosis Michael

The Challenges of Fungi in Cystic Fibrosis Michael Tracy, M. D. Clinical Assistant Professor March 10, 2018

Microbes in Cystic Fibrosis MRSA Pseudomona s Bacteria Burkholderia Staph NTM Influenza Viruses RSV Rhinoviru s Candida Fungi Aspergillu s

Everyone is exposed to fungi • Every day we breath: • >20, 000 times/day • We inhale: • ~10, 000 liters of air/day • 1 cubic meter of air >50, 000 fungal spores can contain: Chotirmall SH et al. 2018. Mycopathologia.
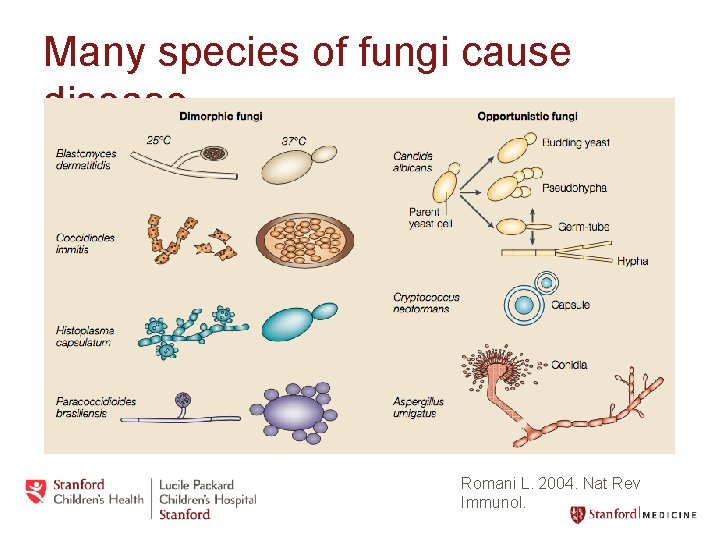
Many species of fungi cause disease Romani L. 2004. Nat Rev Immunol.

Rising awareness of fungi in CF • Increased life expectancy • Increased percentage of immunocompromised CF patients • Detection methods are improving

So many fungi – where do we focus? Chmiel JF, et al. 2014. Ann Am Thorac Soc

How often do we find fungi in CF? • Historically, reported prevalence varies greatly – Aspergillus spp: 0 to 36% – Scedosporium spp: 0 to 9% • Appears to be increasing over time • Multi center studies are showing a higher prevalence of fungi than CF registry data Hong G, et al. 2017. J Clin Microbiol.

Similar prevalence in recent studies Prevalence of fungi in CF patients in USA, France & Germany 45 40 Prevalence (%) 35 30 25 20 15 10 5 0 Aspergillus spp USA Scedosporium spp France Germany Hong G, et al. 2017. J Clin Microbiol. Coron N, et al. 2018. Mycopathologia. Ziesing S, et al. 2016. Med Mycol.

What are risk factors for fungal colonization in CF? • CF lung disease – Impaired mucus clearance – Immunogenic dysfunction • • • Decreased lung function Older age Inhaled and oral antibiotic use Inhaled steroid use Macrolide antibiotics Stolz et al. 2015. NEJM. Sudfeld CR, et al. 2010. J Cyst Fibros. Hong G, et al. 2018. J Cyst Fibros.

We found fungi – now what? • Colonization? • Allergy? • Infection?

Aspergillus species • Over 100 species – A. fumigatus most common • Everywhere in the environment – Soil, water, decomposing material • Wide spectrum of Aspergillus-associated disease – Allergic bronchopulmonary aspergillosis (ABPA) is now well described in CF – What is the role of A. fumigatus in the non-ABPA CF lung? Chotirmall SH et al. 2018. Mycopathologia.
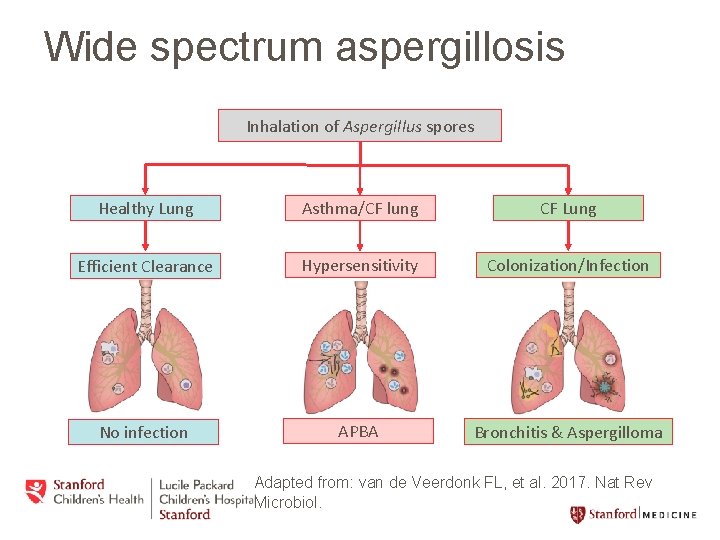
Wide spectrum aspergillosis Inhalation of Aspergillus spores Healthy Lung Asthma/CF lung CF Lung Efficient Clearance Hypersensitivity Colonization/Infection No infection APBA Bronchitis & Aspergilloma Adapted from: van de Veerdonk FL, et al. 2017. Nat Rev Microbiol.

ABPA: Minimal diagnostic criteria • Clinical deterioration • Total serum Ig. E > 500 IU/m. L • Immediate cutaneous reactivity to Aspergillus or in • vitro demonstration of Ig. E antibody to A. fumigatus One of the following: – Precipitins to A. fumigatus or in vitro demonstration of Ig. G antibody to A. fumigatus – New or recent abnormalities on chest radiography (infiltrates or mucus plugging) or chest CT (bronchiectasis) that have not cleared Stevens, DS, et al. 2003. Clin. Infect. Dis.

ABPA: Challenging diagnosis • Overlapping features with other factors causing CF exacerbations • New biomarkers are emerging: “blood tests for ABPA” – Basophil Activation Test + Ig. E for A. fumigatus – CF pts into 3 groups: • Nonsensitized • A. fumigatus–sensitized • ABPA Mirkovic B et al. 2016. JACI.

ABPA: Treatment Anti-inflammatory • Oral steroids • IV steroids • Concerns: • Diabetes • Bone health Antifungal • Oral Triazole • Inhaled Amphotericin • Concerns: • Toxicity • Drug interaction Anti-Ig. E • Omalizumab • Concerns: • Cost • Anaphylaxi s • Injections

non-ABPA: Colonization or Infection? Liu JC, et al. 2013. J Cyst Fibros.

Criteria for “highly probable” CF fungal infection 1. Increased sputum production 2. Multiple isolation of the same fungal species – 3. 4. 5. 6. 7. At least two culture-positive samples in 6 months Pulmonary infiltrate(s) on chest CT scan or X-ray Treatment failure with antibiotic therapy Unexplained lung function decline Exclusion of new/other bacteria Exclusion of ABPA Schwarz C, et al. 2018. Mycopathologia.

Aspergillus infections: Treatment • No consensus in CF • Azole therapy is first line – Voriconazole – Posaconazole • Growing concern for Azole resistance • Amphotericin • Caspofungin Schwarz C, et al. 2018. Mycopathologia.
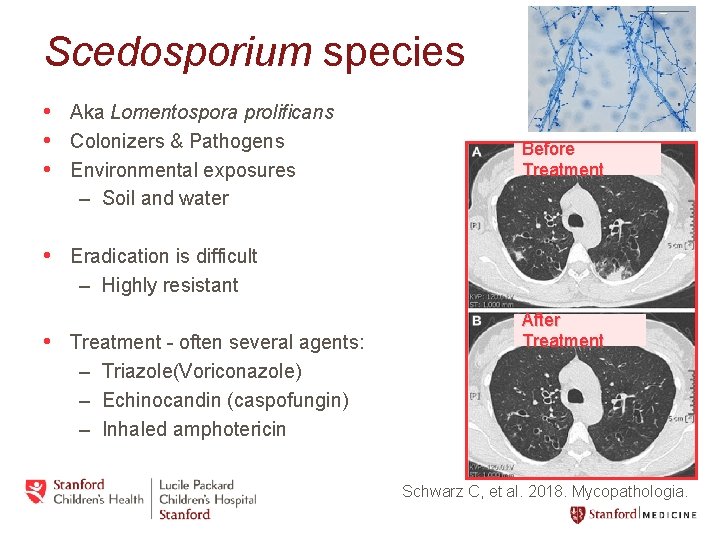
Scedosporium species • Aka Lomentospora prolificans • Colonizers & Pathogens • Environmental exposures Before Treatment – Soil and water • Eradication is difficult – Highly resistant • Treatment - often several agents: After Treatment – Triazole(Voriconazole) – Echinocandin (caspofungin) – Inhaled amphotericin Schwarz C, et al. 2018. Mycopathologia.

Candida species • C. albicans most common – Frequently found in sputum – Oral/genital candidiasis – Infections of devices/lines • Colonization associated with: – Hospitalizations – Exacerbations – Declines FEV 1 and BMI • If colonized, clinical role unclear – no evidence for treatment • Other species may be more pathogenic – Remains unusual cause for infection Chotirmall SH, et al. 2010. Chest. Schwarz C, et al. 2018. Mycopathologia.

Future Questions • When and how to do fungi become pathogenic? – – When they enter the airway? When they colonize? When they sensitive? When they infect? • Should we eradicate? • Which antifungals? For how long?
Resources to learn more • CFF. org – Dr Okorie & Dr. Moss • NACFC 2017 Archives – S 10 – Chair: Dr Moss & Dr Elborn

Thank you!
- Slides: 23