The best bridge between despair and hope is

The best bridge between despair and hope is a good nights sleep

Sleep and Energy Zoe Barr Wendy Smith Megan Bird

Sleep is the new black on the wellbeing agenda

1 in 3 will have problems with sleep at some point in their lives 10% of people will have chronic issues Sleep disorders are a risk factor for stroke and impact on recovery from stroke Improved sleep is a key part of better energy management Many sleep and fatigue issues can be improved by addressing common underlying causes and modifying habits.

Our intention is to underline the importance of. . Sleep for us all The identification of sleep issues And referral to relevant services/ beginning treatment Reinforcing good sleep habits as a secondary prevention measure and to aid stroke recovery

Sleep Awareness What is sleep? Why is sleep important? What are the elements of sleep health? Sleep disorders and stroke What gets in the way of good sleep?

What is sleep? Highly active daily period of rejuvenation which sustains life Different phases of sleep are characterised by specific brain wave activity
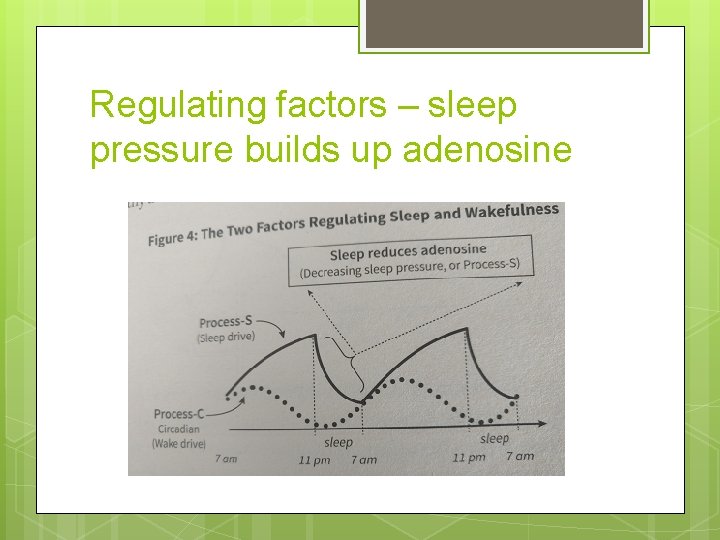
Regulating factors – sleep pressure builds up adenosine
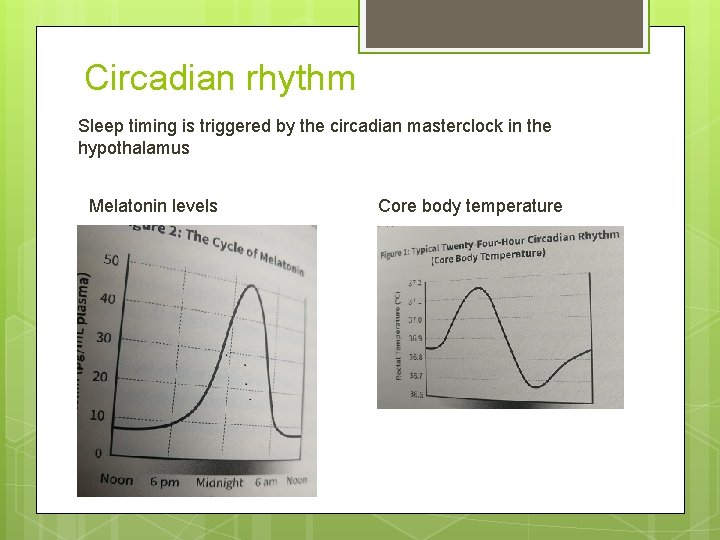
Circadian rhythm Sleep timing is triggered by the circadian masterclock in the hypothalamus Melatonin levels Core body temperature

Sleep Architecture Repeating cycle of 4/5 phases lasting approx. 90 minutes Stage 1 -3/4 of Non REM sleep followed by REM

Why is sleep important? General health benefits: Cardiovascular health Cell repair Metabolic and endocrine health Immunity cognitive functioning Safety and avoiding accidents Healthy aging and overall lengthened lifespan Learning and relearning Creativity mood and stress management improved relationships and lessened conflict Mental health Weight management

What are the elements of sleep health? Duration - optimum 7 -9 hours in one stretch. Architecture – optimum blend of NREM and REM Quality

Sleep and Stroke Reduced sleep duration is linked to cardiovascular disease Sleep is impacted by BMI and poorly controlled blood sugars which lead to sleep apnoea Sleep breathing disorders (e. g. sleep apnoea) are a risk factor for stroke (Herman and Bassetti, 2016) Sleep wake disturbances such as Insomnia are linked with higher incidence of stroke Thought to be inflammatory mechanism linked to sympathetic nervous system activation

Sleep and stroke recovery. . Sleep fosters neuroplasticity Sleep improves learning and memory Sleep enhances motor task performance (Duss and Bassetti, 2017) Promotion of sleep and treatment of disorders is neuroprotective Disturbed sleep can impair stroke outcomes Sleep has an Impact on energy /fatigue levels

Identify any problems. . Ask about sleep: identifying problems and evaluate need to refer on Anyone using any formal assessment tool? What are the problems you’ve come across?

Classifications of Sleep disorders Disorders of sleeplessness -insomnia Disorders of excessive sleepiness - sleep apnoea (SBD – sleep breathing disorders) - narcolepsy - periodic limb movement in sleep - restless legs syndrome Circadian Disorders - delayed sleep phase syndrome - advanced sleep phase syndrome Parasomnias - sleepwalking -night terrors - REM sleep behaviour disorder - sleep paralysis Others - long/short sleep duration (SWD – sleep wake disturbances) - snoring, sleep talking, hypnic jerks

Areas to target 1. 2. 3. 4. Environmental Behavioural Sleep health Psychological

Areas to target Environmental Dark room Cool / ambient temperature Comfortable bed Remove clocks Get enough light (particularly in the morning/ bright light therapy) Well ventilated bedroom

Areas to target Behavioural Regular bedtime and get up time 7 -9 hours sleep opportunity Cease caffeine 6 hrs prior to bed Don’t eat too close to bedtime but avoid hunger Avoid alcohol - sedates but disturbs sleep Wind down routine Avoid too much daytime sleeping Take regular exercise – a. m.

Areas to target Sleep health Avoid sleeping tablets if possible Manage pain as much as possible Manage underlying sleep disorders Such as apnoea, snoring Manage diabetes as poor sugar control interferes with sleep Avoid becoming over tired and triggering adrenaline and cortisol Enough vitamin D Manage fluid intake and continence issues Managing hormones

Areas to target Psychological Manage stressors Avoid being over stimulated close to bedtime Associate bedroom with sleep

Inadequate sleep hygiene: ICSD definition (Stepanski and Wyatt 2003)1. Daytime napping at least two times each week. 2. Variable wake-up times or bedtime. 3. Frequent periods (two to three times per week) of extended amounts of time spent in bed. 4. Routine use of products containing alcohol, tobacco, or caffeine in the period preceding bedtime. 5. Scheduling exercise too close to bedtime. 6. Engaging in exciting or emotionally upsetting activities too close to bedtime. (over stimulating) 7. Frequent use of the bed for non-sleep-related activities (e. g. television watching, reading, studying, snacking, etc. ). 8. Sleeping on an uncomfortable bed (poor mattress, inadequate blankets, etc. ). 9. Allowing the bedroom to be too bright, too stuffy, too cluttered, too hot, too cold, or in some way not conducive to sleep. (unsettled sleep partner) 10. Performing activities demanding high levels of concentration shortly before bed. 11. Allowing mental activities, such as thinking, planning, reminiscing, etc. to occur in bed. (worrying)
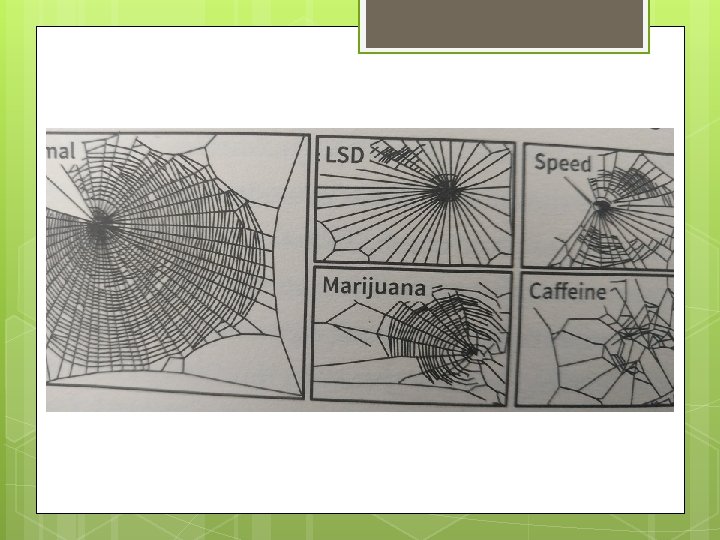

Improving sleep: where to refer? Sleep clinics for further diagnoses of sleep disorders and Polysomnography Medical staff/ nurses to treat underlying health problems, comorbidities, pain Psychologists to treat mood or for CBT
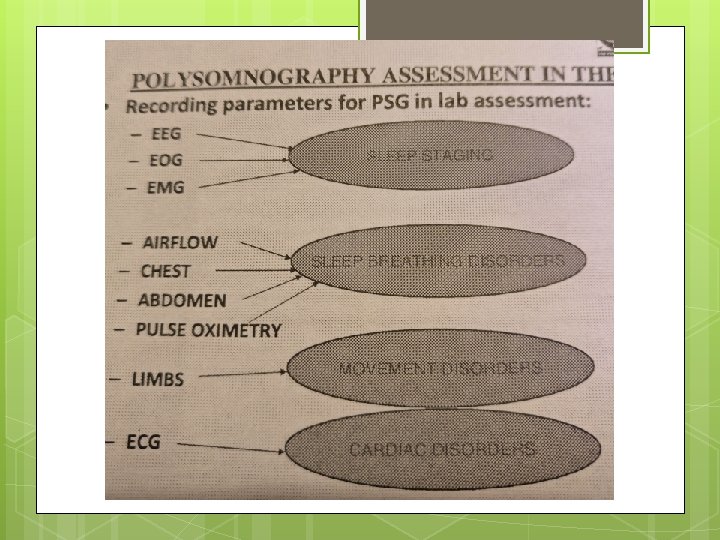

Improving sleep: forms of structured approach Sleep education and sleep hygiene advice (one to one/ in groups) Signpost to leaflets/resources Relaxation/meditation/mindfulness techniques or apps/Rest Assured program CBT for insomnia online such as Sleepio or face to face CBT Sleep programmes/courses Coaching/goalsetting approach

Improving sleep: strategies to aid behaviour change Raising insight and awareness re sleep Motivational aspects - linking to goals/desires Planning first steps to try out Priming for success Cueing and anchoring new habits Feedback – trackers, diaries Exploring core beliefs Planning for backsliding and the cycle of change

What do we do and could we do whilst people in hospital?

Public health key messages (1) (Public Health England 2017) The prevalence of sleep curtailment and sleep disorders is increasing and appears to correlate with a range of poor health outcomes Sleep predicts cardiovascular outcomes and there is a U shape relationship between sleep and cardiovascular risk There is a strong association between mental health and sleep Sleep continuity disorders are observed in nearly all mental health conditions Laboratory and epidemiological studies show that insufficient sleep and circadian misalignment have a negative impact on glucose regulation which can cause insulin resistance and diabetes

Public health key messages (2) (Public Health England 2017) Sleep duration and quality are associated with an increased risk of mortality, particularly amongst the older population Epidemiological studies make the link between short sleep duration and increased body mass index (BMI) Sleep duration and quality are association with an increased risk of mortality The mounting evidence of the health impacts warrants efforts to improve sleep amongst the general population The methodological heterogeneity of studies means that it is difficult to determine the effectiveness of interventions to improve sleep

Summary messages re sleep and our stroke patients Ask about sleep and underlying factors which may be disturbing sleep Raise awareness about the importance of sleep for pre and post stroke health and what impacts it Empower people to prioritize improving sleep and support with building robust sleep hygiene habits

References Manual‐guided cognitive–behavioural therapy for insomnia delivered by ordinary primary care personnel in general medical practice: a randomized controlled effectiveness trial, K Bothelius 2013. Journal of Sleep Research Evidence Briefing: What is the impact of poor sleep on physical and mental health? What is the evidence on the individual interventions to improve sleep? Source: Public Health England - PHE - 12 October 2017 All cause mortality in older adults - a systematic review; Alves de Silva et al 2015 BMJ Open The role of sleep in recovery following ischaemic stroke: Duss & Bassetti ; Neurobiology of sleep and circadian rhythms jan 2017 Use of sleep hygiene in the treatment of insomnia Edward J. Stepanski and James K. Wyatt Sleep Medicine Reviews, Vol. 7, No. 3, pp 215± 225, 2003

Resources www. sleepfoundation. org www. Journalsleep. org Recovery Academy GMMH – overcoming sleep problems course. www. Sleepio. com – CBTi online for free “Why we sleep” - Matthew walker Saebo – sleep after a stroke, the key to faster recovery Waking up to the health benefits of sleep, university of oxford, Professor colin Epsie, RSPH
- Slides: 33