THE BERG BALANCE SCALE AS A PREDICTOR OF

THE BERG BALANCE SCALE AS A PREDICTOR OF DISABILITY, LEGNTH OF STAY, AND DISCHARGE DESTINATION IN POST-STROKE PATIENTS LEAH BATTEN CLINICAL PROBLEM SOLVING I

PURPOSE This presentation aims to describe the physical therapy examination, evaluation, plan of care, and outcomes of a patient who suffered a cerebral vascular accident (CVA). It also aims to explore the research related to the Berg Balance Scale as a valid and reliable outcome measure for predicting length of stay and discharge destination in patients post-stroke.

PATIENT INFORMATION • • “Mr. X” is a 63 year-old Caucasian male Pre-morbid high-level performing Attorney Lives alone Presented to the hospital with these symptoms: § Syncope § Paresthesias of right arm and leg § Trouble remembering simple numbers • Admitted for full-work up for an acute CVA • Results § Acute ischemia in the medial aspect of the left temporal lobe in the posterior left basal ganglia § Occluded proximal left posterior cerebral artery

EPIDEMIOLOGY OF STROKE • The Statistics: § Stroke kills almost 130, 000 Americans each year § Every year, more than 795, 000 Americans have a stroke § Leading cause of serious long-term disability • Primary Characteristics: www. cdc. gov

THE BERG BALANCE SCALE • Equipment Needed • • • Chair with AND without arms 6 -inch stepstool, or step 12 -inch ruler Stopwatch or wristwatch 15 ft. walkway Single object • Scoring • Quality of performance • 5 point ordinal scale (0 – 4) • Max score is 56 • Interpretation • 41 -56 = Independent • 21 -40 = Walking with assistance • 0 – 20 = Wheelchair bound
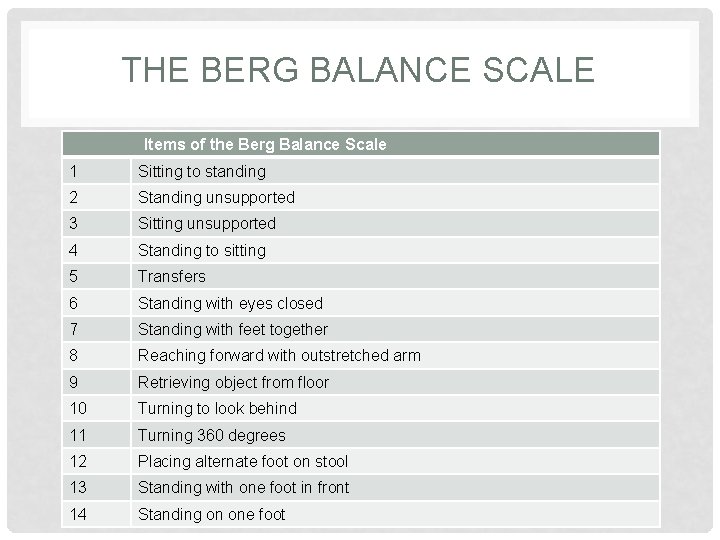
THE BERG BALANCE SCALE Items of the Berg Balance Scale 1 Sitting to standing 2 Standing unsupported 3 Sitting unsupported 4 Standing to sitting 5 Transfers 6 Standing with eyes closed 7 Standing with feet together 8 Reaching forward with outstretched arm 9 Retrieving object from floor 10 Turning to look behind 11 Turning 360 degrees 12 Placing alternate foot on stool 13 Standing with one foot in front 14 Standing on one foot
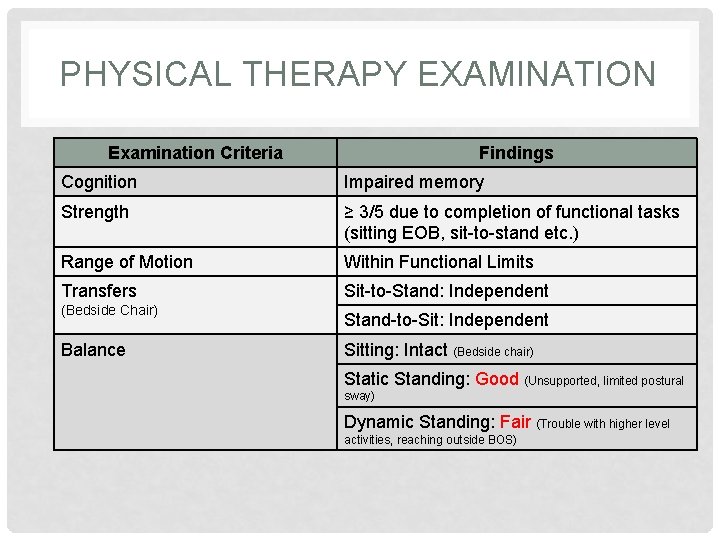
PHYSICAL THERAPY EXAMINATION Examination Criteria Findings Cognition Impaired memory Strength ≥ 3/5 due to completion of functional tasks (sitting EOB, sit-to-stand etc. ) Range of Motion Within Functional Limits Transfers Sit-to-Stand: Independent (Bedside Chair) Balance Stand-to-Sit: Independent Sitting: Intact (Bedside chair) Static Standing: Good (Unsupported, limited postural sway) Dynamic Standing: Fair (Trouble with higher level activities, reaching outside BOS)

ASSESSMENT (DAY 1) • Functional Limitations • Mild slurring of speech • Inability to reach out of BOS without losing balance • Inability to recall simple phone numbers • Disabilities • Unable to perform IADL’s (activities with higher-level reaching) • Unable to work due to memory loss • Patient’s Prognosis: Good • Due to the following factors: • Age • Education level • Motivation to recover

GOALS & PLAN OF CARE • Goals (short-term) • Patient will perform higher-level balance activities/exercises with supervision/set-up within 7 days. • Plan of Care • • • Conduct Berg Balance Scale Ambulation/gait training Stair training Single-leg balance exercises Dynamic balance exercises • Discharge • Home with family support

INTERVENTIONS CONT. (DAY 2) • Berg Balance Score Results Category Deficits Score Reaching forward with outstretched arm while standing 1/4 Pick up object from floor from standing position 3/4 Turning to look behind over left and right shoulders while standing 3/4 Placing alternate foot on stool while standing unsupported (4 times) 2/4 Standing unsupported one foot in front 3/4 Standing on one leg 3/4 Total Score: 47/56 Category: Independent* *A score of <45 indicates a greater risk of falling. Berg, 1992.
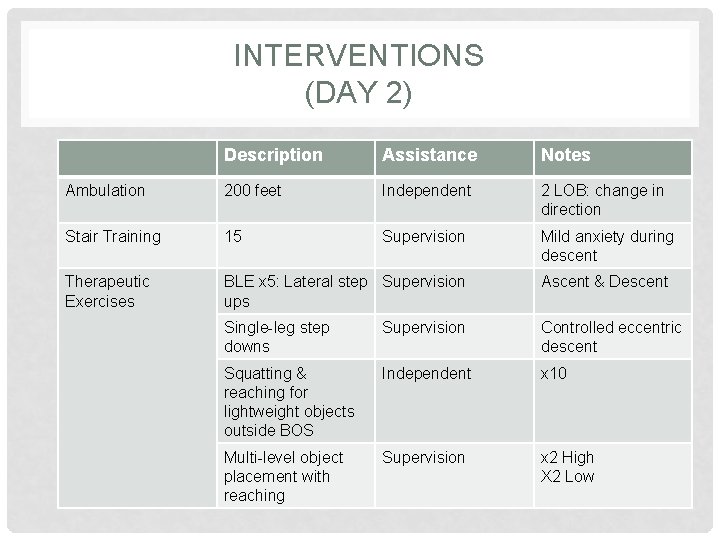
INTERVENTIONS (DAY 2) Description Assistance Notes Ambulation 200 feet Independent 2 LOB: change in direction Stair Training 15 Supervision Mild anxiety during descent Therapeutic Exercises BLE x 5: Lateral step Supervision ups Ascent & Descent Single-leg step downs Supervision Controlled eccentric descent Squatting & reaching for lightweight objects outside BOS Independent x 10 Multi-level object placement with reaching Supervision x 2 High X 2 Low

OUTCOMES • Patient able to perform all exercises with supervision and met his one goal. • Would be a good candidate for outpatient physical therapy for higher-level balance training, with a focus on multi-level and stair activities. • BBS Score: 47/56 • Discharge Destination: HOME • LOS: 2 days

CLINICAL QUESTION FOR A 63 YEAR OLD MALE POST-CVA, IS THE BERG BALANCE SCALE A VALID PROGNOSTIC INDICATOR FOR DISABILITY, LEGNTH OF HOSPITAL STAY AND DISCHARGE DESTINATION?

Validation of the Berg Balance Scale as a Predictor of Length of Stay and Discharge Destination in Stroke Rehabilitation Joy Y. Wee et al 2003

PURPOSE To validate the utility of the Berg Balance Scale (BBS) in predicting length of stay (LOS) and discharge destination in stroke rehabilitation. Level of Evidence: A Prospective Study

METHODS • Participants • 375 patients between April 1, 1998 and August 1, 2000. • Age 50 – 95 yrs. old • Selection Criteria • Ability to: • • follow commands sit unsupported at edge of bed (EOB) for 30 secs. sit up for at least 2 hours in a wheelchair participate in several 30 -minute therapy sessions daily • Medically stable • Exclusion Criteria • Hemiplegia from traumatic causes or tumors • Unable to participate in active rehabilitation or did not complete rehabilitation due to medical complications

PROCEDURE • Data Collected • Admission BBS Score • 0/56 to 54/56 range: Mean 21/56 • Highest score: 56 • “FIM” Disability Score • 35 -125 range; Mean 87. 8 • Highest score 126 • Descriptive Balance Indices • Static Sitting, Standing • Dynamic Sitting, Standing • Length of Stay • Measured as the number of days between admission to and discharge from rehab • Discharge Destination • Private dwellings • Intermediate care facility • Extended care facility • Acute hospital ward
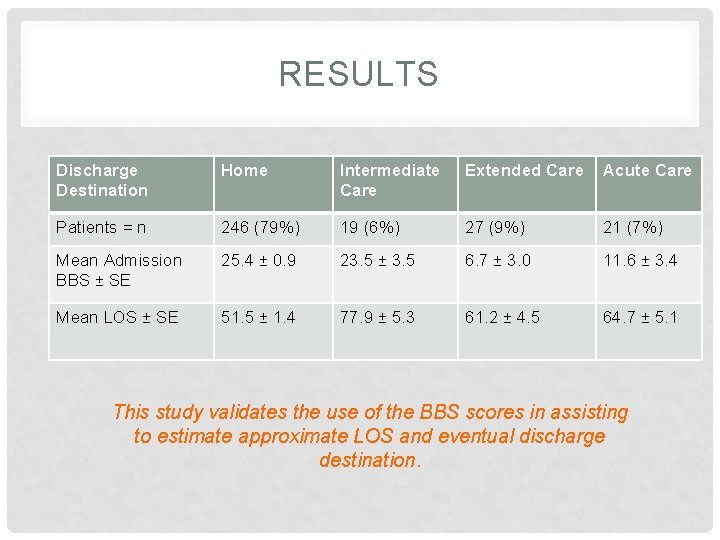
RESULTS Discharge Destination Home Intermediate Care Extended Care Acute Care Patients = n 246 (79%) 19 (6%) 27 (9%) 21 (7%) Mean Admission BBS ± SE 25. 4 ± 0. 9 23. 5 ± 3. 5 6. 7 ± 3. 0 11. 6 ± 3. 4 Mean LOS ± SE 51. 5 ± 1. 4 77. 9 ± 5. 3 61. 2 ± 4. 5 64. 7 ± 5. 1 This study validates the use of the BBS scores in assisting to estimate approximate LOS and eventual discharge destination.
LIMITATIONS Selection bias due to subject population only being from admitted patients to Holy Family Hospital.

Usefulness of the Berg Balance Scale in Stroke Rehabilitation: A Systematic Review Lisa Blum and Nicol Korner-Bitensky 2008
PURPOSE Systematic Review of the psychometric properties of the BBS specific to stroke and to identify strengths and weaknesses in its usefulness for stroke rehabilitation.

METHODS • 21 studies were retrieved (1966 – 2007) based on these key terms: • Balance Scale, Berg Balance Scale, psychometric properties, measurement properties, reliability, repeatability, validity, responsiveness, and appropriateness. • 5 Questions Addressed: • In Patients with Stroke: • • • Does the BBS Have Internal Consistency? Is the BBS a Reliable Measure? Is the BBS a Valid Measure? Does the BBS Have Predictive Validity? Does the BBS Detect Change?
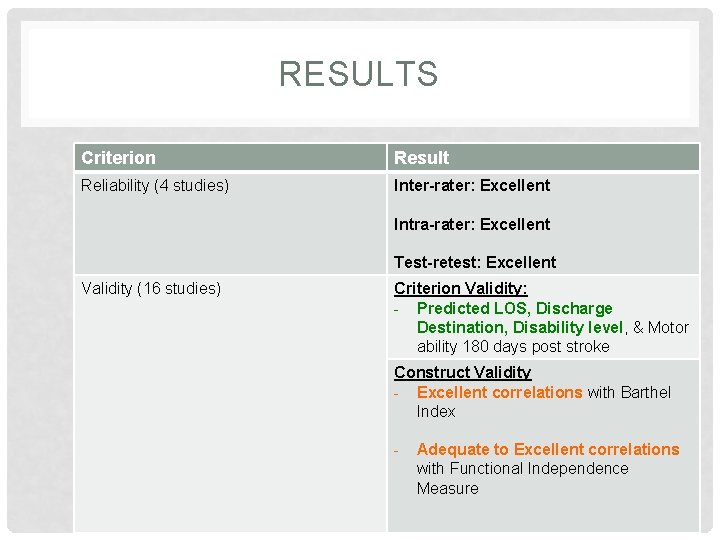
RESULTS Criterion Result Reliability (4 studies) Inter-rater: Excellent Intra-rater: Excellent Test-retest: Excellent Validity (16 studies) Criterion Validity: - Predicted LOS, Discharge Destination, Disability level, & Motor ability 180 days post stroke Construct Validity - Excellent correlations with Barthel Index - Adequate to Excellent correlations with Functional Independence Measure

LIMITATIONS TO BBS • Floor and Ceiling Effects • May not detect meaningful changes when used to asses patients who have severe balance impairments or those who have mild impairments. • Floor Effect: Least demanding item is sitting independently. • Ceiling Effect: With mildly impaired stroke patients, the BBS may miss significant gains in balance that are critical for community and leisure participation. So what about Mr. X?

DOES THIS ANSWER MY QUESTION? • YES! • The BBS is reliable and valid prognostic indicator for disability, length of stay and discharge destination in an acute post-stroke population. Remember that … • Mr. X scored a 47/56 on BBS. Discharged home and LOS was 2 days. However … • For higher-level performing patients (like Mr. X. ) with mild stroke impairments, the BBS may not be the most useful tool. • Further research needs to be done to determine a useful tool that avoids the ceiling effects. • Ultimately, given the limitations, clinicians might want to use the BBS in conjunction with other tests to further classify their patients.
QUESTIONS? THANK YOU!

REFERENCES • Berg K, Wood-Dauphinee S, Williams JI, Maki, B (1992). Measuring balance in the elderly: validation of an instrument. Can. J. Pub. Health July/August supplement 2: S 7 -11 • Donoghue D; Physiotherapy Research and Older People (PROP) group, Stokes EK. (2009). How much change is true change? The minimum detectable change of the Berg Balance Scale in elderly people. J Rehabil Med. 41(5): 343 -6. • Wee JY, Wong H, Palepu A. Validation of the Berg Balance Scale as a Predictor of Length of Stay and Discharge Destination in Stroke Rehabilitation. Archives of Physical Medical Rehabilitation. 2003; 84: 731735. • Blum L, Korner-Bitensky N. Usefulness of the Berg Balance Scale in Stroke Rehabilitation: A Systematic Review. PT Journal. 2008; 88: 559 -566.
- Slides: 27