The association of multimorbidity with health service utilisation

The association of multimorbidity with health service utilisation among patients with dementia in the UK: a population-based study J Browne, DA Edwards, KM Rhodes, DJ Brimicombe, RA Payne Centre for Academic Primary Care
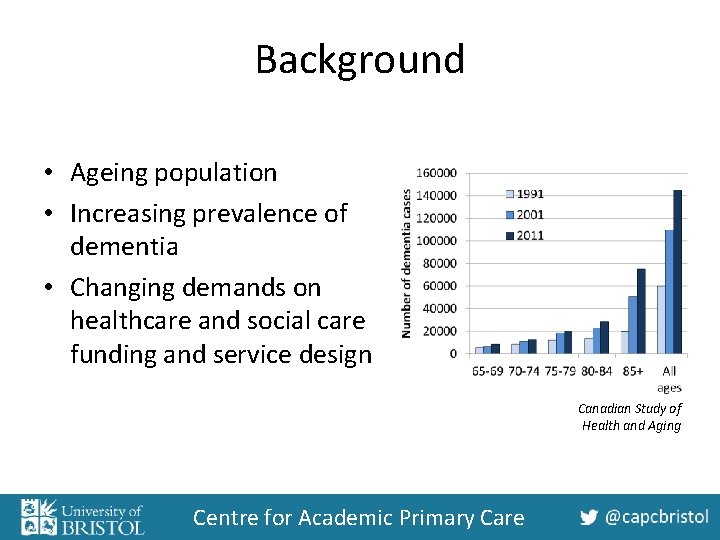
Background • Ageing population • Increasing prevalence of dementia • Changing demands on healthcare and social care funding and service design Canadian Study of Health and Aging Centre for Academic Primary Care
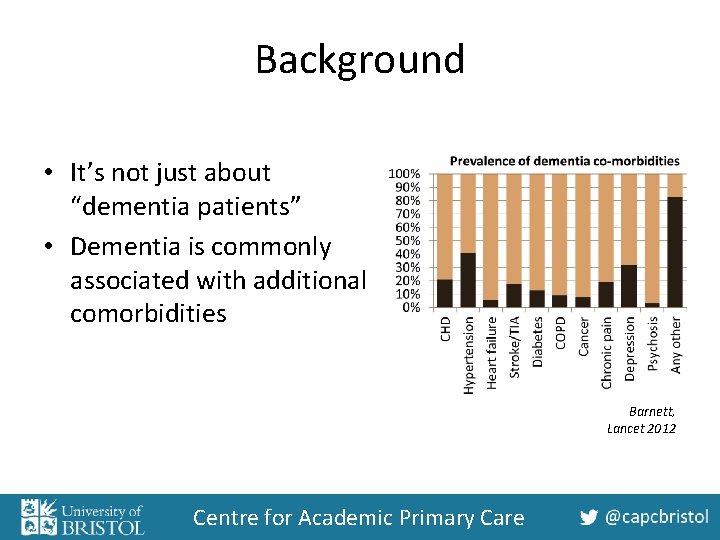
Background • It’s not just about “dementia patients” • Dementia is commonly associated with additional comorbidities Barnett, Lancet 2012 Centre for Academic Primary Care

How do comorbidities impact upon health service utilisation in the dementia population? Centre for Academic Primary Care

Methods • Retrospective cohort study • CPRD • Incident dementia cases diagnosed 2008/9 – 65 Read codes, including any subtype and unspecified • 5 -year follow-up – minimum 3 -months Centre for Academic Primary Care
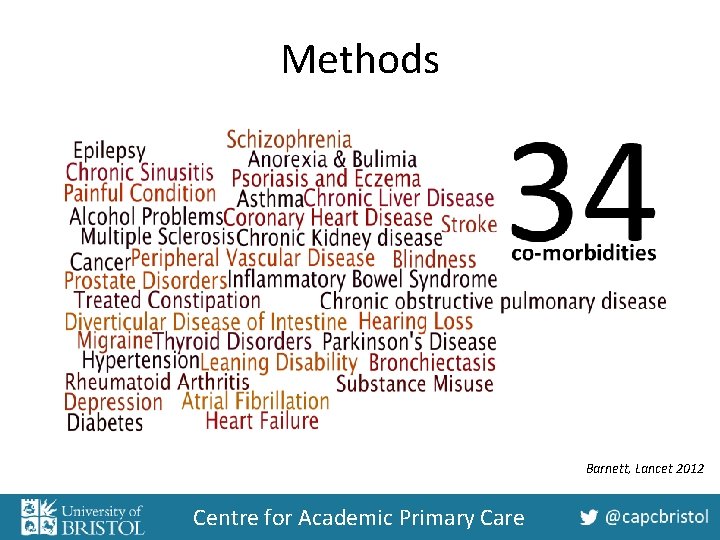
Methods Barnett, Lancet 2012 Centre for Academic Primary Care

Methods • • Primary care consultations All hospital admissions All primary care prescriptions Time to death Centre for Academic Primary Care

Methods • Association between comorbidity count and outcome – Negative binomial regression (service use) – Cox regression (death) • Adjustment for age, gender, practice, dementia treatment, deprivation Centre for Academic Primary Care
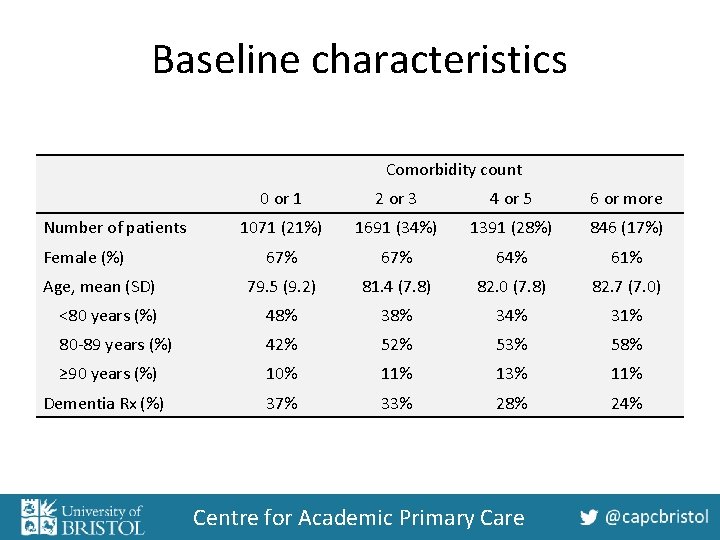
Baseline characteristics Comorbidity count 0 or 1 2 or 3 4 or 5 6 or more 1071 (21%) 1691 (34%) 1391 (28%) 846 (17%) 67% 64% 61% 79. 5 (9. 2) 81. 4 (7. 8) 82. 0 (7. 8) 82. 7 (7. 0) <80 years (%) 48% 34% 31% 80 -89 years (%) 42% 53% 58% ≥ 90 years (%) 10% 11% 13% 11% Dementia Rx (%) 37% 33% 28% 24% Number of patients Female (%) Age, mean (SD) Centre for Academic Primary Care
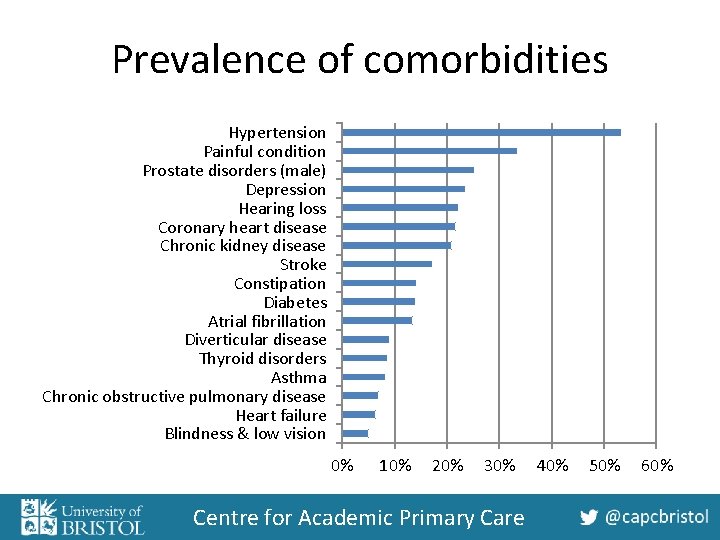
Prevalence of comorbidities Hypertension Painful condition Prostate disorders (male) Depression Hearing loss Coronary heart disease Chronic kidney disease Stroke Constipation Diabetes Atrial fibrillation Diverticular disease Thyroid disorders Asthma Chronic obstructive pulmonary disease Heart failure Blindness & low vision 0% 10% 20% 30% Centre for Academic Primary Care 40% 50% 60%
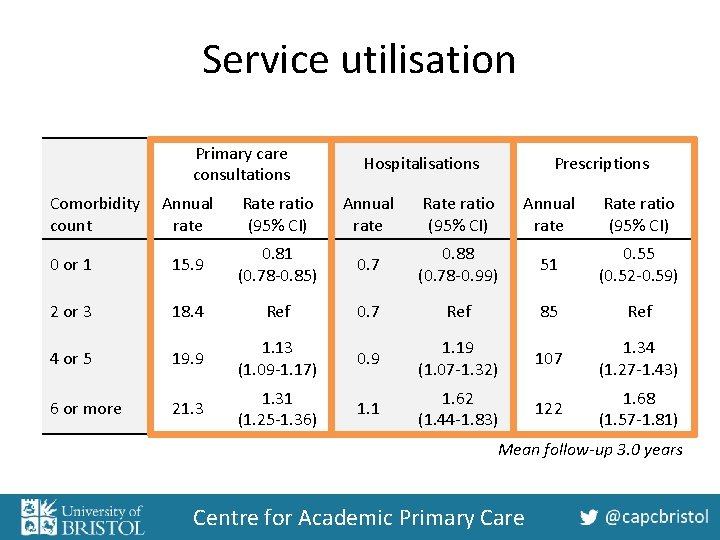
Service utilisation Primary care consultations Comorbidity count Hospitalisations Prescriptions Annual rate Rate ratio (95% CI) 0 or 1 15. 9 0. 81 (0. 78 -0. 85) 0. 7 0. 88 (0. 78 -0. 99) 51 0. 55 (0. 52 -0. 59) 2 or 3 18. 4 Ref 0. 7 Ref 85 Ref 4 or 5 19. 9 1. 13 (1. 09 -1. 17) 0. 9 1. 19 (1. 07 -1. 32) 107 1. 34 (1. 27 -1. 43) 6 or more 21. 31 (1. 25 -1. 36) 1. 1 1. 62 (1. 44 -1. 83) 122 1. 68 (1. 57 -1. 81) Mean follow-up 3. 0 years Centre for Academic Primary Care
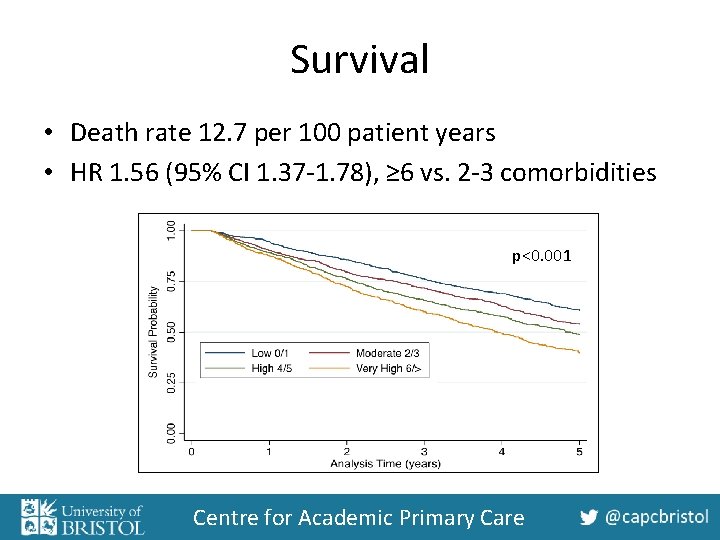
Survival • Death rate 12. 7 per 100 patient years • HR 1. 56 (95% CI 1. 37 -1. 78), ≥ 6 vs. 2 -3 comorbidities p<0. 001 Centre for Academic Primary Care

Consequences • For a woman aged 80 -85 years with 6 or more comorbidities, over 3 years: – 18 more consultations – 131 more prescriptions – 2 more hospitalisations – Additional cost £ 5137 (compared to similar individual with 2 -3 comorbidities) Centre for Academic Primary Care

Strengths and limitations • First such study in UK • Large, representative sample • Range of relevant outcomes • Misclassification of comorbidities varying with health service contact • Crude measures of service use • Differential loss to follow-up Centre for Academic Primary Care

Conclusions • Comorbidities are very common in the context of dementia • Comorbidities drive a substantial increase in health service utilisation • Multimorbidity must be considered when planning care services for people with dementia Centre for Academic Primary Care
- Slides: 15