The Ankle Lower Leg Bones Ankle joint is

The Ankle & Lower Leg
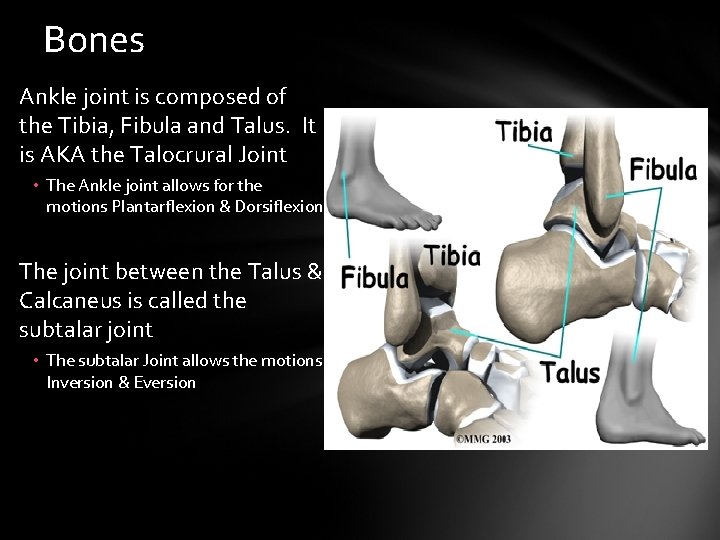
Bones Ankle joint is composed of the Tibia, Fibula and Talus. It is AKA the Talocrural Joint • The Ankle joint allows for the motions Plantarflexion & Dorsiflexion The joint between the Talus & Calcaneus is called the subtalar joint • The subtalar Joint allows the motions Inversion & Eversion
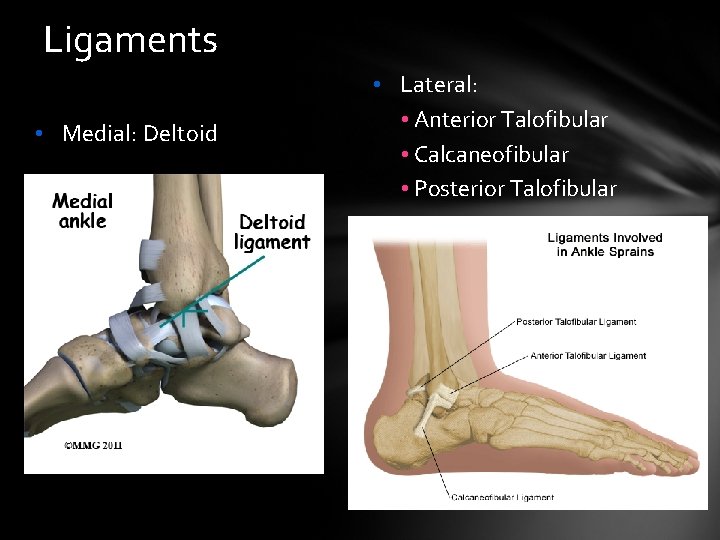
Ligaments • Medial: Deltoid • Lateral: • Anterior Talofibular • Calcaneofibular • Posterior Talofibular
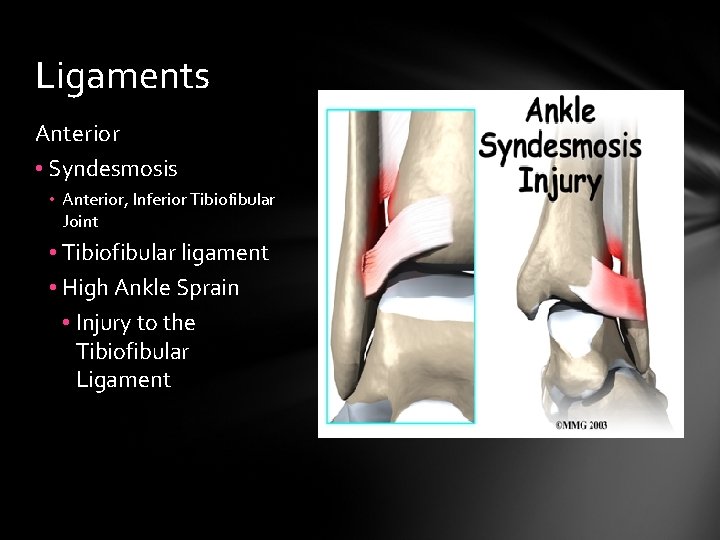
Ligaments Anterior • Syndesmosis • Anterior, Inferior Tibiofibular Joint • Tibiofibular ligament • High Ankle Sprain • Injury to the Tibiofibular Ligament
Ligaments
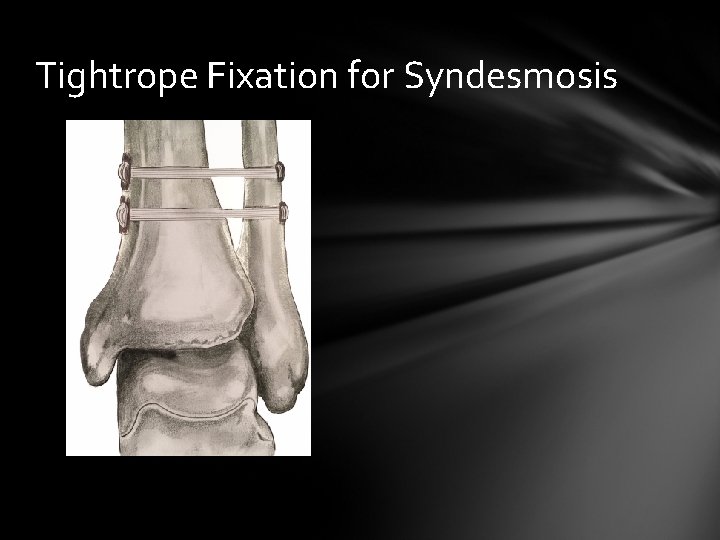
Tightrope Fixation for Syndesmosis
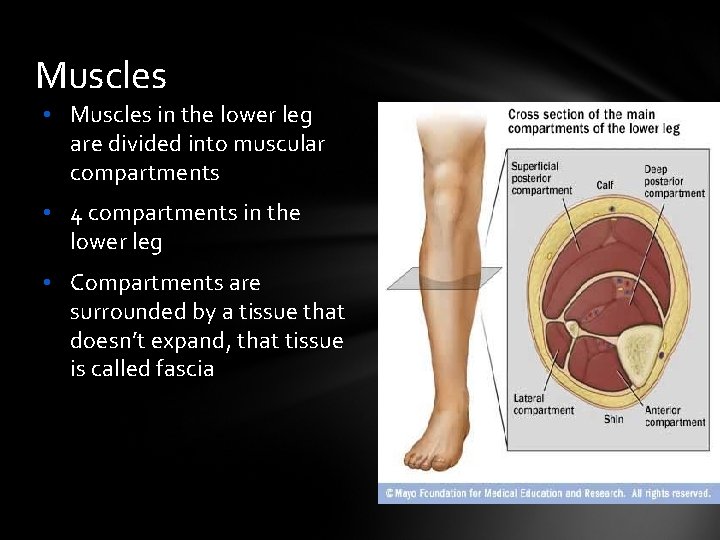
Muscles • Muscles in the lower leg are divided into muscular compartments • 4 compartments in the lower leg • Compartments are surrounded by a tissue that doesn’t expand, that tissue is called fascia
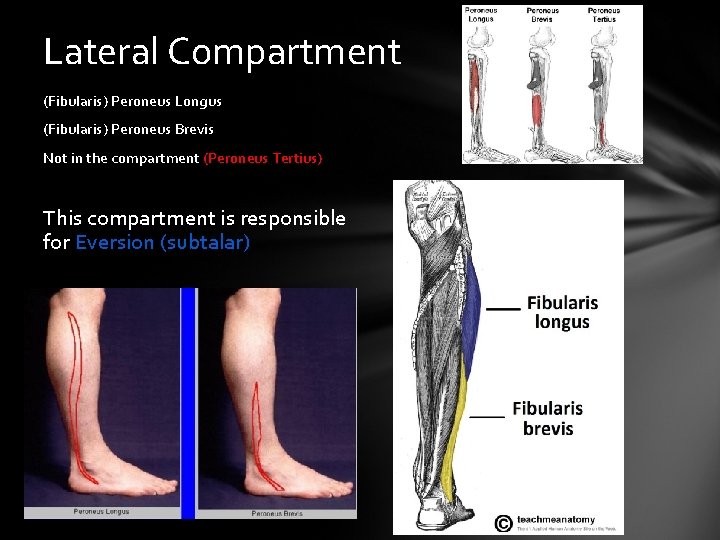
Lateral Compartment (Fibularis) Peroneus Longus (Fibularis) Peroneus Brevis Not in the compartment (Peroneus Tertius) This compartment is responsible for Eversion (subtalar)
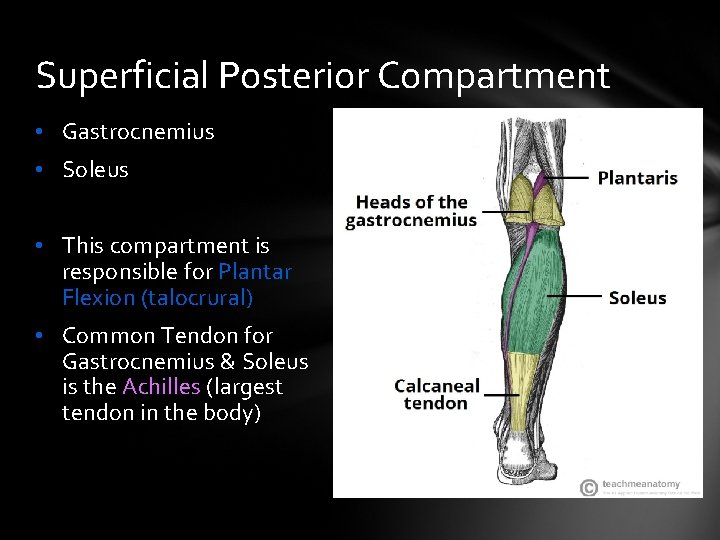
Superficial Posterior Compartment • Gastrocnemius • Soleus • This compartment is responsible for Plantar Flexion (talocrural) • Common Tendon for Gastrocnemius & Soleus is the Achilles (largest tendon in the body)
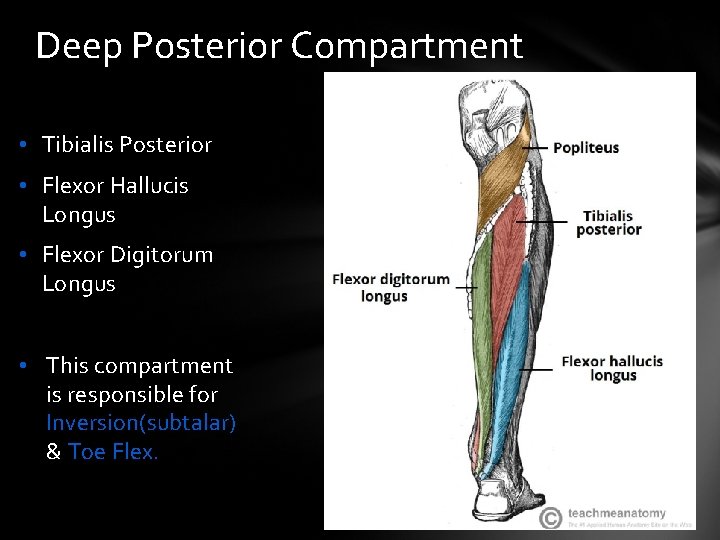
Deep Posterior Compartment • Tibialis Posterior • Flexor Hallucis Longus • Flexor Digitorum Longus • This compartment is responsible for Inversion(subtalar) & Toe Flex.
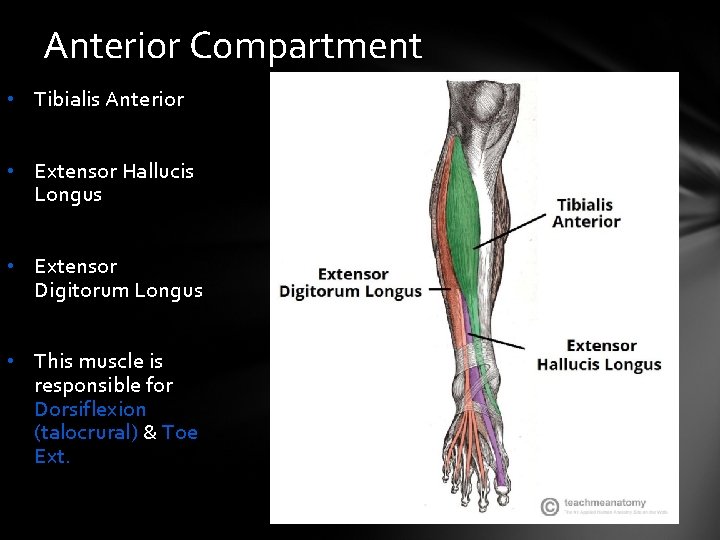
Anterior Compartment • Tibialis Anterior • Extensor Hallucis Longus • Extensor Digitorum Longus • This muscle is responsible for Dorsiflexion (talocrural) & Toe Ext.
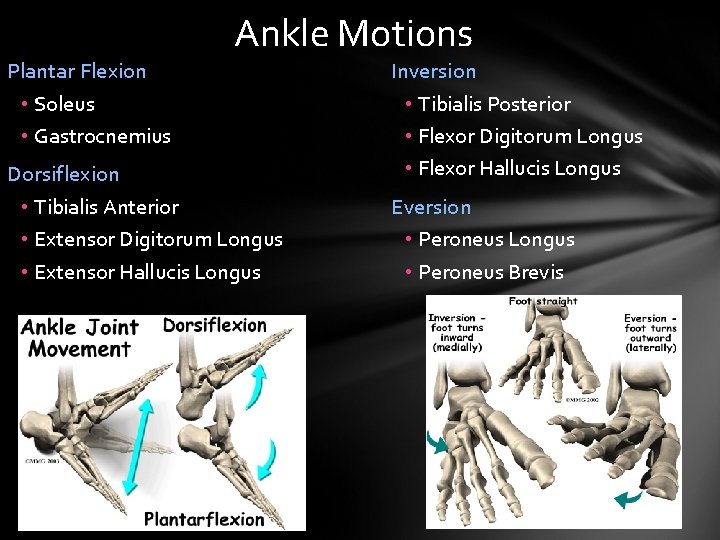
Ankle Motions Plantar Flexion • Soleus • Gastrocnemius Dorsiflexion • Tibialis Anterior • Extensor Digitorum Longus • Extensor Hallucis Longus Inversion • Tibialis Posterior • Flexor Digitorum Longus • Flexor Hallucis Longus Eversion • Peroneus Longus • Peroneus Brevis

Prevention of Ankle & Lower Leg Injuries • Stretching • Strengthening • Improving Neuromuscular Control (Proprioception) • Spatial awareness • Appropriate Footwear • Taping & Bracing when necessary
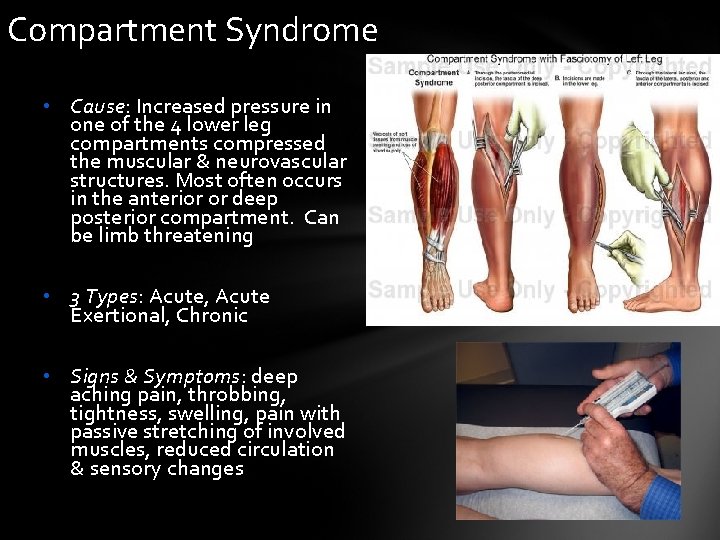
Compartment Syndrome • Cause: Increased pressure in one of the 4 lower leg compartments compressed the muscular & neurovascular structures. Most often occurs in the anterior or deep posterior compartment. Can be limb threatening • 3 Types: Acute, Acute Exertional, Chronic • Signs & Symptoms: deep aching pain, throbbing, tightness, swelling, pain with passive stretching of involved muscles, reduced circulation & sensory changes
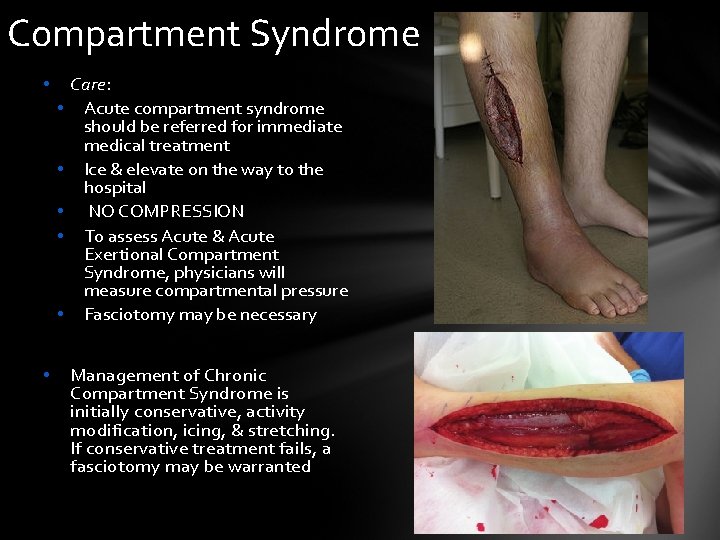
Compartment Syndrome • • Care: Acute compartment syndrome should be referred for immediate medical treatment Ice & elevate on the way to the hospital NO COMPRESSION To assess Acute & Acute Exertional Compartment Syndrome, physicians will measure compartmental pressure Fasciotomy may be necessary Management of Chronic Compartment Syndrome is initially conservative, activity modification, icing, & stretching. If conservative treatment fails, a fasciotomy may be warranted
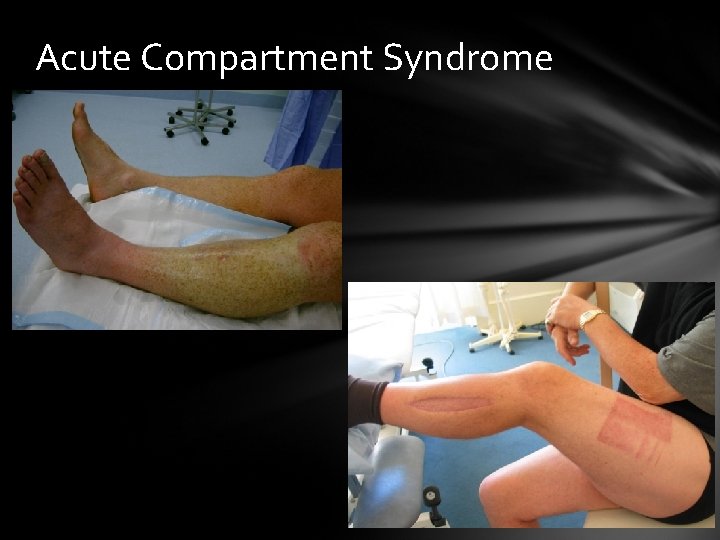
Acute Compartment Syndrome
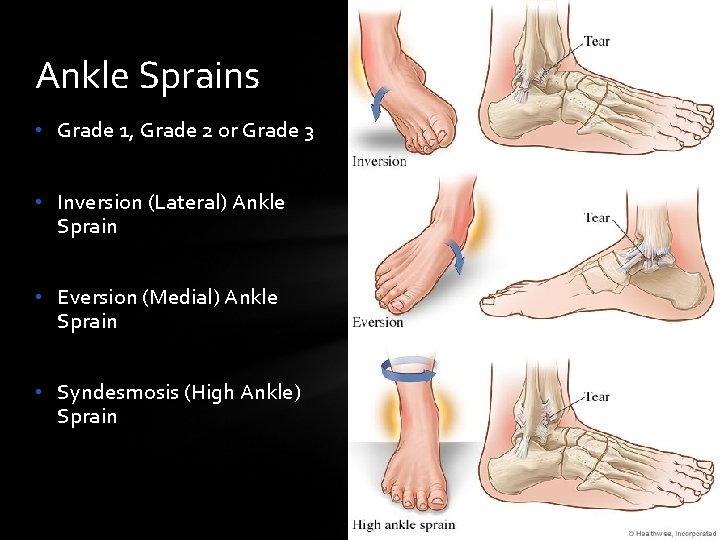
Ankle Sprains • Grade 1, Grade 2 or Grade 3 • Inversion (Lateral) Ankle Sprain • Eversion (Medial) Ankle Sprain • Syndesmosis (High Ankle) Sprain

Inversion Ankle Sprain • Cause: • Forced Inversion. Damages Ligaments on the Lateral aspect of the ankle: Anterior Talofibular, Calcaneofibular, Posterior Talofibular • Inversion (Lateral) Ankle Sprain is the most common type of ankle sprain • The ATF is the weakest of the lateral ligaments & therefore the most commonly injured • Signs & Symptoms: • Swelling, Ecchymosis, Pain, Point Tenderness • Care: • PRICE, F/u with physician, X-ray to rule out fracture, Crutches & Camboot. Heal time can be anywhere from 2 -6 weeks depending on severity, Tape/Brace for return to play
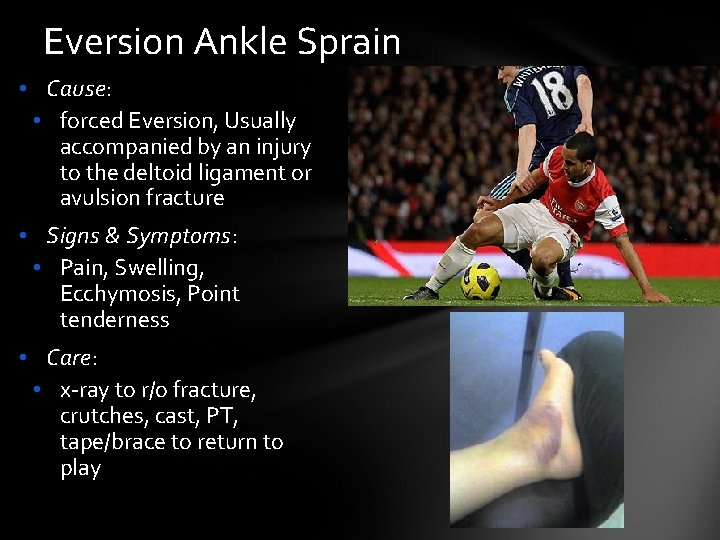
Eversion Ankle Sprain • Cause: • forced Eversion, Usually accompanied by an injury to the deltoid ligament or avulsion fracture • Signs & Symptoms: • Pain, Swelling, Ecchymosis, Point tenderness • Care: • x-ray to r/o fracture, crutches, cast, PT, tape/brace to return to play
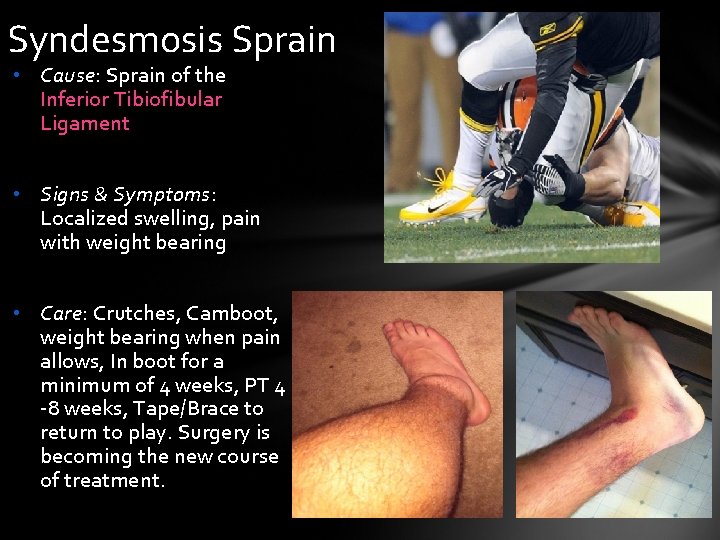
Syndesmosis Sprain • Cause: Sprain of the Inferior Tibiofibular Ligament • Signs & Symptoms: Localized swelling, pain with weight bearing • Care: Crutches, Camboot, weight bearing when pain allows, In boot for a minimum of 4 weeks, PT 4 -8 weeks, Tape/Brace to return to play. Surgery is becoming the new course of treatment.

Ankle Fracture • Cause: can be caused by trauma or mechanisms similar to those for ankle sprains • Signs & Symptoms: Immediate swelling, pain, point tenderness, apprehensiveness with weight bearing or inability to bear weight • Care: Splint, refer for x-ray, Cast, Cam boot, Crutches, PT, displaced fractures may require surgical repair • Malleolus Fracture • Talar Dome Fracture • Avulsion Fracture
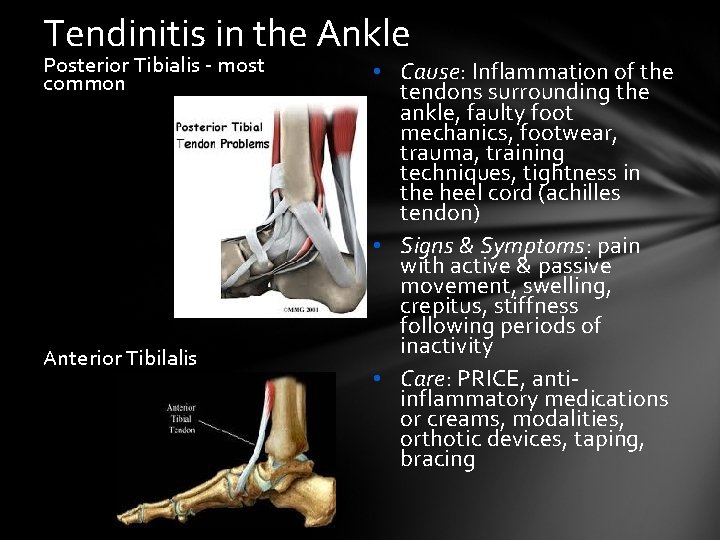
Tendinitis in the Ankle Posterior Tibialis - most common Anterior Tibilalis • Cause: Inflammation of the tendons surrounding the ankle, faulty foot mechanics, footwear, trauma, training techniques, tightness in the heel cord (achilles tendon) • Signs & Symptoms: pain with active & passive movement, swelling, crepitus, stiffness following periods of inactivity • Care: PRICE, antiinflammatory medications or creams, modalities, orthotic devices, taping, bracing
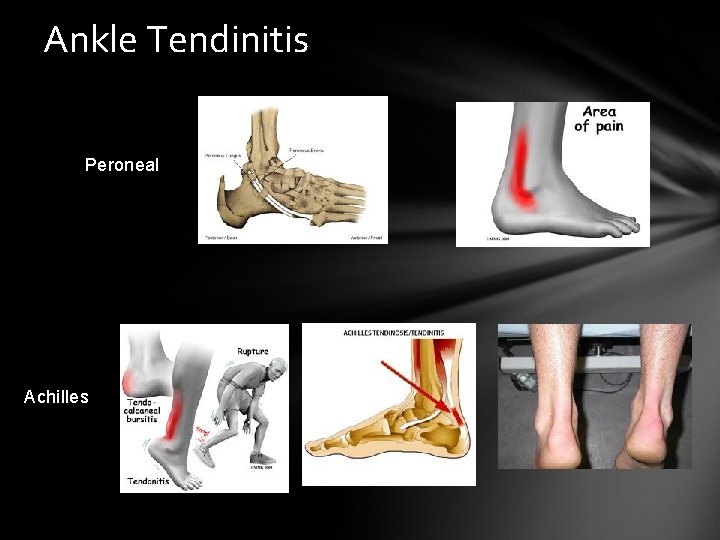
Ankle Tendinitis Peroneal Achilles
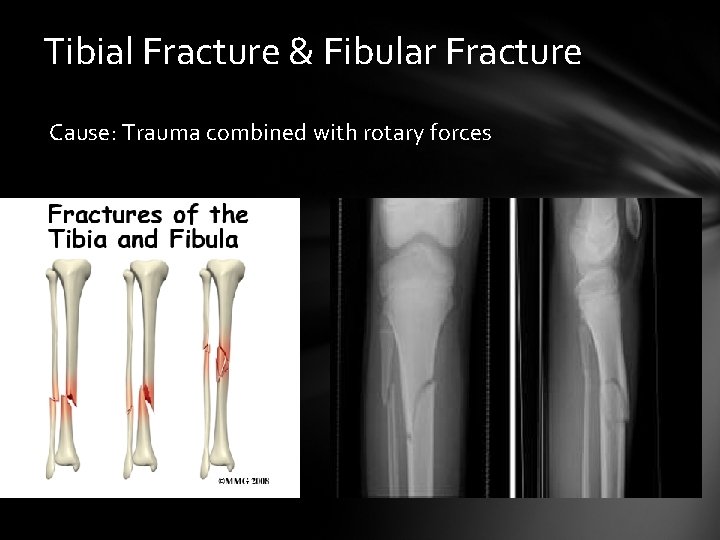
Tibial Fracture & Fibular Fracture Cause: Trauma combined with rotary forces

Lower Leg Fracture Signs & Symptoms: Pain, Swelling, Deformity, Check Circulation, & motion Care: Splint, Transport for medical care. The type of fracture determines whether it is casted or fixed with surgery
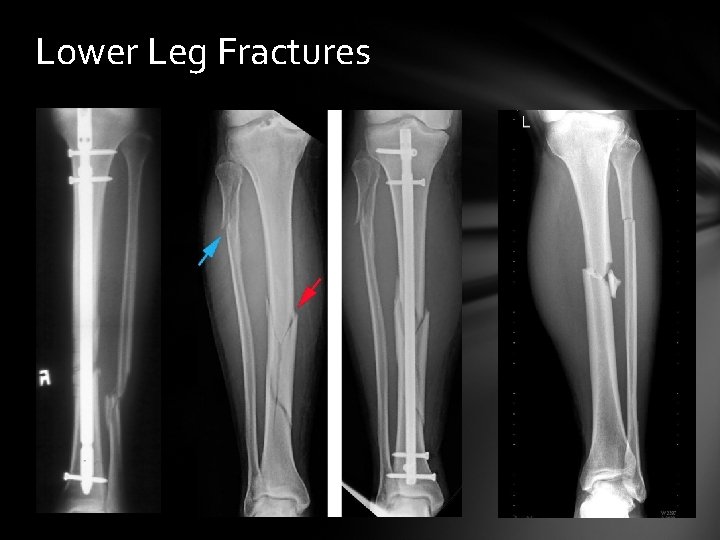
Lower Leg Fractures
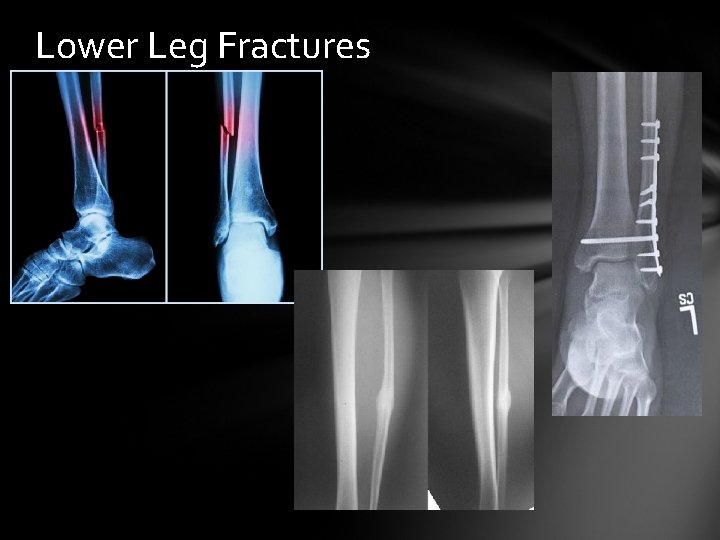
Lower Leg Fractures
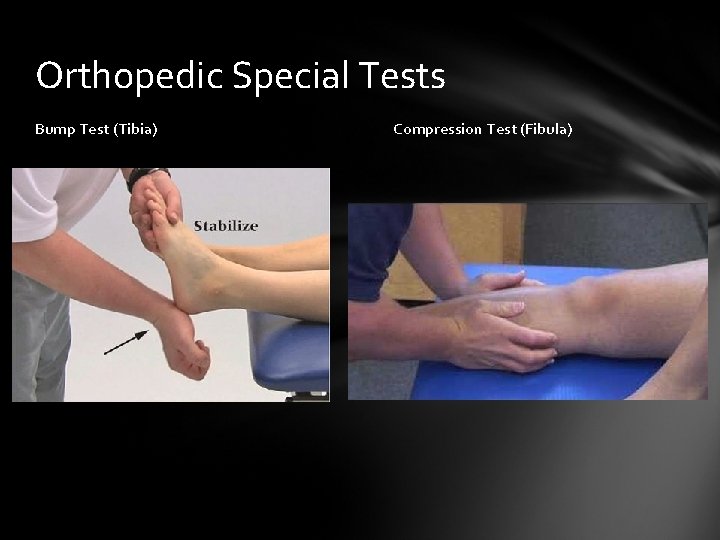
Orthopedic Special Tests Bump Test (Tibia) Compression Test (Fibula)
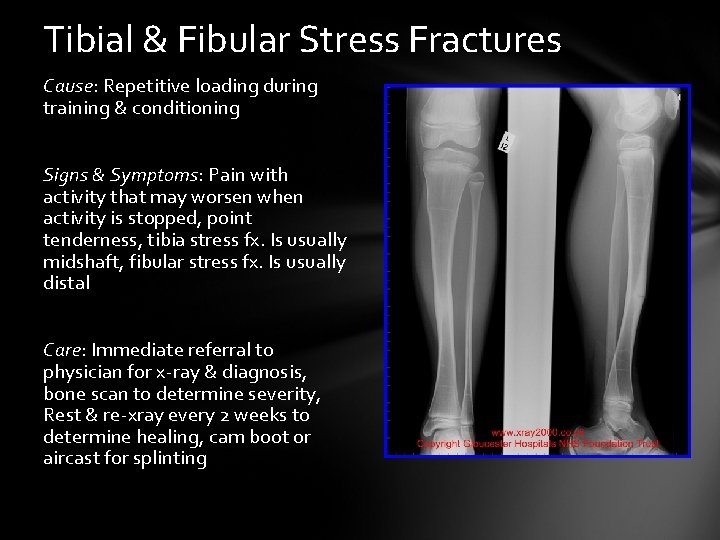
Tibial & Fibular Stress Fractures Cause: Repetitive loading during training & conditioning Signs & Symptoms: Pain with activity that may worsen when activity is stopped, point tenderness, tibia stress fx. Is usually midshaft, fibular stress fx. Is usually distal Care: Immediate referral to physician for x-ray & diagnosis, bone scan to determine severity, Rest & re-xray every 2 weeks to determine healing, cam boot or aircast for splinting
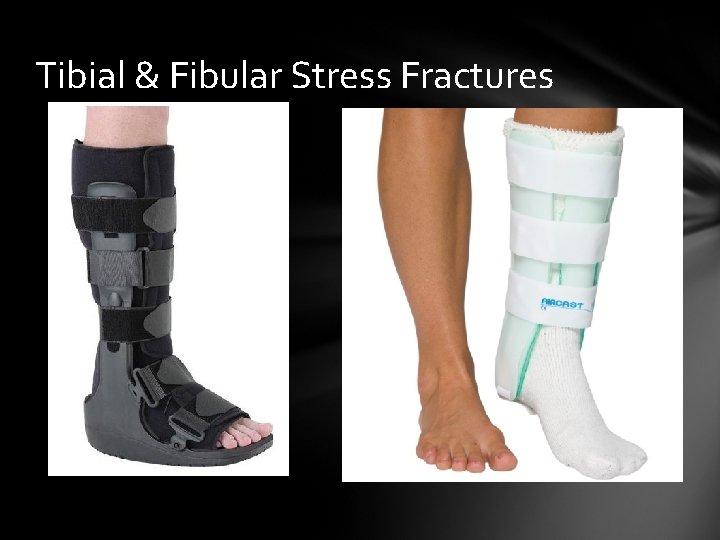
Tibial & Fibular Stress Fractures
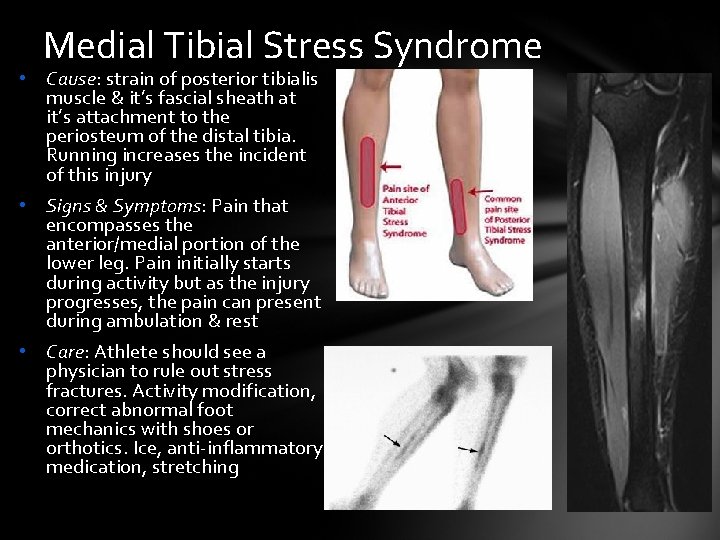
Medial Tibial Stress Syndrome • Cause: strain of posterior tibialis muscle & it’s fascial sheath at it’s attachment to the periosteum of the distal tibia. Running increases the incident of this injury • Signs & Symptoms: Pain that encompasses the anterior/medial portion of the lower leg. Pain initially starts during activity but as the injury progresses, the pain can present during ambulation & rest • Care: Athlete should see a physician to rule out stress fractures. Activity modification, correct abnormal foot mechanics with shoes or orthotics. Ice, anti-inflammatory medication, stretching
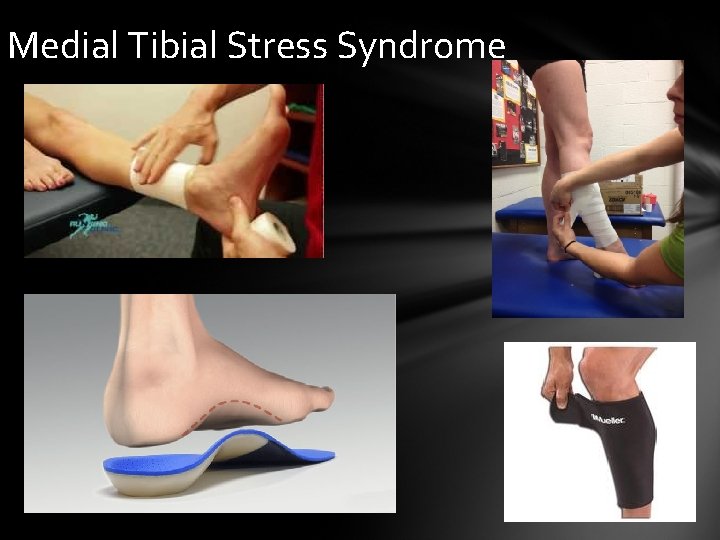
Medial Tibial Stress Syndrome
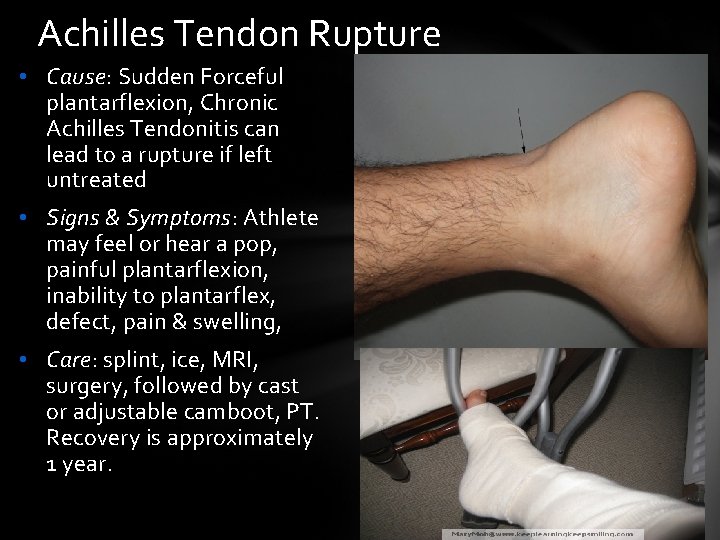
Achilles Tendon Rupture • Cause: Sudden Forceful plantarflexion, Chronic Achilles Tendonitis can lead to a rupture if left untreated • Signs & Symptoms: Athlete may feel or hear a pop, painful plantarflexion, inability to plantarflex, defect, pain & swelling, • Care: splint, ice, MRI, surgery, followed by cast or adjustable camboot, PT. Recovery is approximately 1 year.
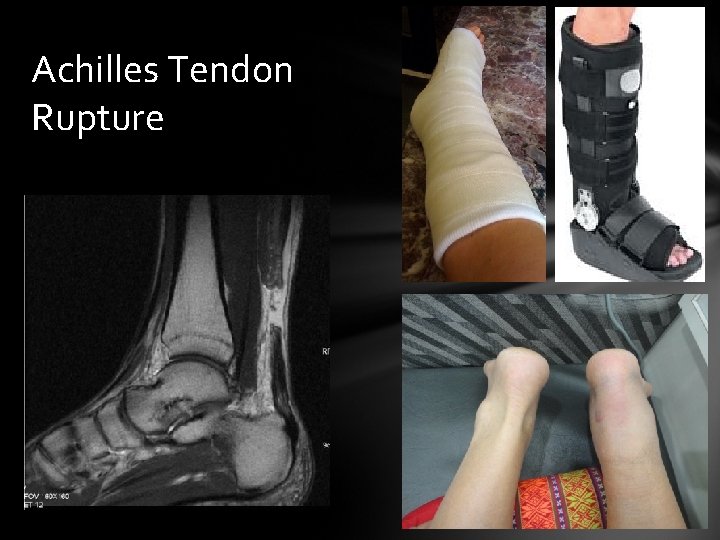
Achilles Tendon Rupture
- Slides: 34