The Anaesthesiologist as a Patient Advocate Eric Hodgson

































- Slides: 35

The Anaesthesiologist as a Patient Advocate Eric Hodgson Inkosi Albert Luthuli Central Hospital & Nelson R Mandela Medical School e. Thekwini-Durban, KZN, SOUTH AFRICA

www. criticalcare 2013. com

Declaration o Advisory boards n Bayer, Boehringer-Ingleheim, Fresenius Kabi, Sanofi-Aventis, MSD, Pfizer o Speaker honoraria n Abbott, Adcock-Ingram, Biopure SA, Astra-Zeneca, Roche, Pfizer, Fresenius Kabi, GSK, Janssen-Cilag, Aspen, Novartis, Nestle, Edwards, Thebe o Travel & accommadotion: F K

Lecture Plan • Patient communication • Advocacy role – Preop – Intraop – Postop • Conclusion

Medical Career Selection

Anaesthesiology as a career choice Andrew F. Smith MRCVFRCA, Make P. Shelly FRCA CAN J ANESTH 1999 / 46: 11 / pp 1082 -1088 • Newly-qualified but unpersonable doctors • Anesthesiology: no direct patient contact – BUT: Chronic Pain, ICU, Need for payment • Serve both surgeons and patients – What do patients know about anaesthetists?

Anaesthesiologists & Patients 2000

Anaesthesiologists & Patients Brazil Braz J Anaesth 2011: 720 -7 13 52 9 26

Anaesthesiologists & Patients

Perioperative Communication How do Anaesthesiologists do? • Results: Overall dissatisfaction – 3 Paeds 1 Adult • 20 x variation between individuals

Perioperative Communication Challenges for Anaesthesiologists • Premed visit – Many patients Little time – Easy to appear rushed / uncaring • Potential solutions – Pre-Anaesthetic leaflet • Esp. Billing in Private – Online Premed (ASA Refresher) • Pre-anaesthetic clinic – All comers vs. Screened? – Cost • Patient & Anaesthesiologist YES

Perioperative Communication How can Anaesthesiologists do better? • Anesthesiologists need to communicate with: – Patients / Families Peers Health Team • Subconscious assessment – Thin-slicing 10 000 hours • Principles – Reflective listening – Utilisation Observing Suggestion Accepting

Perioperative Communication How can Anaesthesiologists do better? • Reflective listening / Observing / Accepting – Patient concerns Solutions – Different realities Accept & Use • “Obviously you’re scared, but none of us are!” • Utilisation – Paeds: “Blow the nasty smell away” – Adults: “Only necessary people are in OR”

Perioperative Communication How can Anaesthesiologists do better? • Establish Rapport – Words convey <10% – Sit down Make contact: Eye & Physical – Mirror Encourage • Obtain information – Closed questions: “How old are you? ” – Open Questions: “ How do you feel about…? ” – Encourage patient questions

Perioperative Communication How can Anaesthesiologists do better? Interview format • Beginning – Ideal setting: private room – Clear your mind for this patient – Introductions: esp. Specialist Anaesthesiologist!! • Middle – Deal with feelings • Uncertainty Anger Anxiety – Information is better than midazolam et. al. • Complex Understandable What was Understood

Perioperative Communication How can Anaesthesiologists do better? Interview format • End – – – Summarise Patient Satisfied Reassure: Will meet in OR Otherwise explain handover Record • Benefits – Satisfaction Anxiety

Perioperative Communication How can Anaesthesiologists do better? Suggestion • Pre-op patients highly suggestible • Positive – Direct: “You” – Indirect: “Most patients” • Negative suggestion – Avoid using emotional terms – “May be sore, but less than expected”

Perioperative Communication Conclusion • Limited time under stressed conditions – Establish Rapport Specialist Qualifications • Provide Reassurance – Esp. Survival – Constant presence – Management of Pain / PONV • Assess patient comprehension – “How do you understand what will be happening? ” • Allow / Encourage questions – Medical / Non-medical (Fees in Private)

Intraoperative Communication • Show respect for patient as sensate being • Communication of respect builds trust • Always speak as if the patient will remember • Limited time to make a good impression

Preoperative Patient Advocacy • Anesthesiologists & HCWs communicate – Multiple levels Whole work day • Complex social transactions – Medical, legal, ethical & personal significance • Different priorities – State – Surgeon vs. Private vs. Patient vs. Anaesthesiologist

Preop Patient Advocacy State Sector • Hierarchical structure – Student Intern Registrar Consultant Ho. D • Concerns at one level referred up – Extent of proposed surgery – Patient’s physiological reserve – Timing - Will delay improve outcome? - Placement on list • Appropriate management by consensus – Conveyed to patient by surgical team – Beware assuming “Gatekeeper” role • “No operation – Anaesthetist says you’re too sick”

Preop Patient Advocacy Private Sector • NO Hierarchy – Each specialist = Every other specialist – Limited (if any) Peer review • Decision made by surgeon alone – Alternatives presented to patients: • Surgery with full recovery • No surgery with progressive discomfort / death • Anaesthesiologist – Can’t operate but understands operations – Able to provide alternative perspective

Preoperative Patient Advocacy The Hippocratic Ethic • Patient submissive & in need • Physician empowered by knowledge – Anaesthesiologist & Surgeon • With this power comes responsibility • Exercise power with tact and respect • Do no harm = speak and act with restraint – Preventing harm means discussion with surgeon

Preop Patient Advocacy Private Sector • Training to specialist level – School + University + Internship + Registrarship – 25+ years of experience • Informed consent – 25+ years impossible in consult / premed – Surgical alternatives part of Premed • Based on likelihood of survival: ASA Grade • Advocacy – Raise alternative options with surgeon first – Unreasonable refusal to consider = conflict

Preop Patient Advocacy Conflict Resolution • Discuss options with surgeon first – Ideal vs. Possible • Whipple’s • Operation vs. Bypass vs. Palliation • Unreasonable refusal to consider options – Senior anaesthetic colleague opinion – Senior surgical opinion • Patient advice – Second opinion for elective cases • Or withdraw – Emergency? ? ? • Proceed but clearly document concerns

Intraoperative Advocacy The “Captain Effect” “It is probable that the tendency of some anesthesiologists not to bother or contradict surgeons, or the reluctance of some nurse anesthetists or residents to call their supervisors, has led to catastrophe…” Gaba DM 1989 IAC

Intra-op Patient Advocacy Error Prevention • Foster equality – Empower team members – Korean Airlines vs. Toyota • Anaesthesia vs. Commercial Flying – Anaesthesia error = >100 fatal crashes/day • WHO surgical checklist – Pioneered by Atul Gawande – Adopted worldwide – Major impact on safety • Wrong operation / site / side

Intra-op Patient Advocacy WHO Checklist

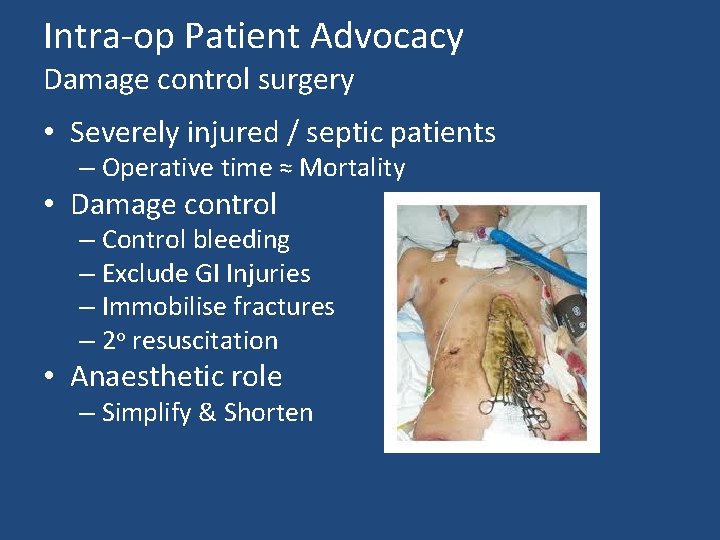
Intra-op Patient Advocacy Damage control surgery • Severely injured / septic patients – Operative time ≈ Mortality • Damage control – Control bleeding – Exclude GI Injuries – Immobilise fractures – 2 o resuscitation • Anaesthetic role – Simplify & Shorten

Intra-op Patient Advocacy Infection control • Personal hygiene – Hand Washing – PPE: Hats Masks Gloves • Injection technique – 3 -way taps Ports – Multi-dose vials • Appropriate antibiotic prophylaxis – Adequate dose within 30 min of incision – 2 nd dose: Long operation >50% blood loss

OR Infection control New Anaesthesia Role? • Particles diminished by: – – – Endoscopic surgery if possible Procedure not unnecessarily prolonged Reduced staff in / circulating in&out of OR 31

Post-op Patient Advocacy • Handovers (Recovery / ICU) – SBAR: – Situation Background Assessment Recommendation – Provide information – Repeat to assess transfer • Pain Management – Multimodal – Special techniques for Special patients

Benefits of Communication & Advocacy Patients Satisfaction Recovery Staff Enhanced self esteem Improved work satisfaction Personal &Professional Growth Healthcare organizations Enhanced reputation Decreased litigation

Facility with a variety of communication skills signifies highly developed professionalism. Literal meaning of “profession” = “speaking forth”

www. criticalcare 2013. com