The Affordable Care Act and Pharmacy PHA 6261

The Affordable Care Act and Pharmacy PHA 6261 Healthcare Administration and Economics

Objectives • Understand the key facets of the Affordable Care Act and its potential impact on the future of US healthcare • To describe the major provisions of the law related to the field of pharmacy 2
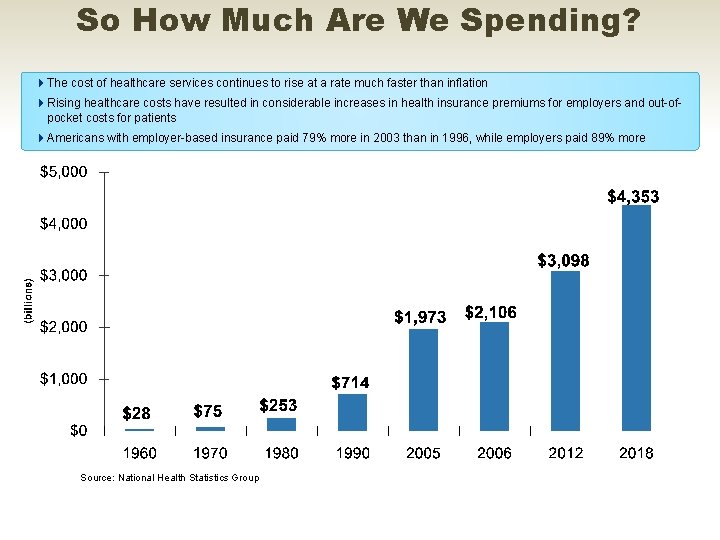
So How Much Are We Spending? 4 The cost of healthcare services continues to rise at a rate much faster than inflation 4 Rising healthcare costs have resulted in considerable increases in health insurance premiums for employers and out-ofpocket costs for patients 4 Americans with employer-based insurance paid 79% more in 2003 than in 1996, while employers paid 89% more Source: National Health Statistics Group
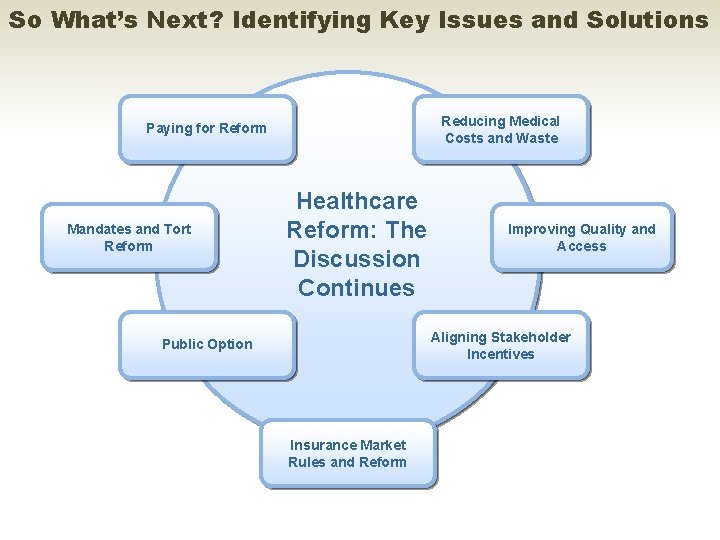
So What’s Next? Identifying Key Issues and Solutions Reducing Medical Costs and Waste Paying for Reform Mandates and Tort Reform Healthcare Reform: The Discussion Continues Improving Quality and Access Aligning Stakeholder Incentives Public Option Insurance Market Rules and Reform
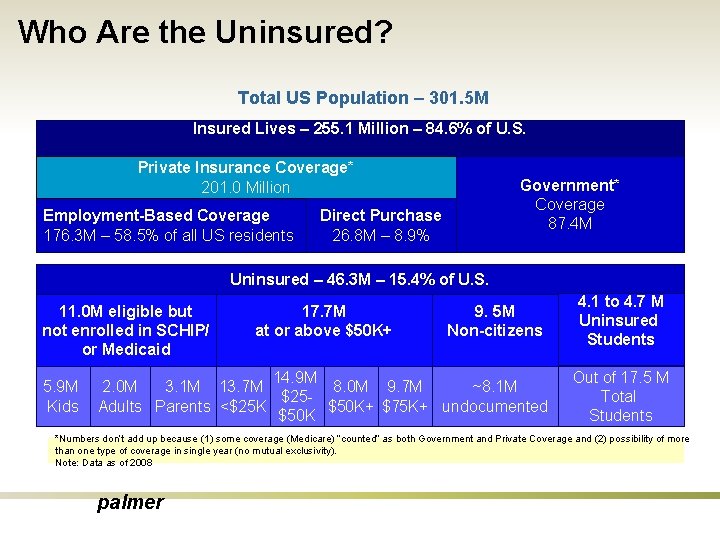
Who Are the Uninsured? Total US Population – 301. 5 M Insured Lives – 255. 1 Million – 84. 6% of U. S. Private Insurance Coverage* 201. 0 Million Employment-Based Coverage 176. 3 M – 58. 5% of all US residents Government* Coverage 87. 4 M Direct Purchase 26. 8 M – 8. 9% Uninsured – 46. 3 M – 15. 4% of U. S. 11. 0 M eligible but not enrolled in SCHIP/ or Medicaid 5. 9 M Kids 17. 7 M at or above $50 K+ 9. 5 M Non-citizens 14. 9 M 2. 0 M 3. 1 M 13. 7 M 8. 0 M 9. 7 M ~8. 1 M $25 Adults Parents <$25 K $50 K+ $75 K+ undocumented $50 K 4. 1 to 4. 7 M Uninsured Students Out of 17. 5 M Total Students *Numbers don’t add up because (1) some coverage (Medicare) “counted” as both Government and Private Coverage and (2) possibility of more than one type of coverage in single year (no mutual exclusivity). Note: Data as of 2008 palmer
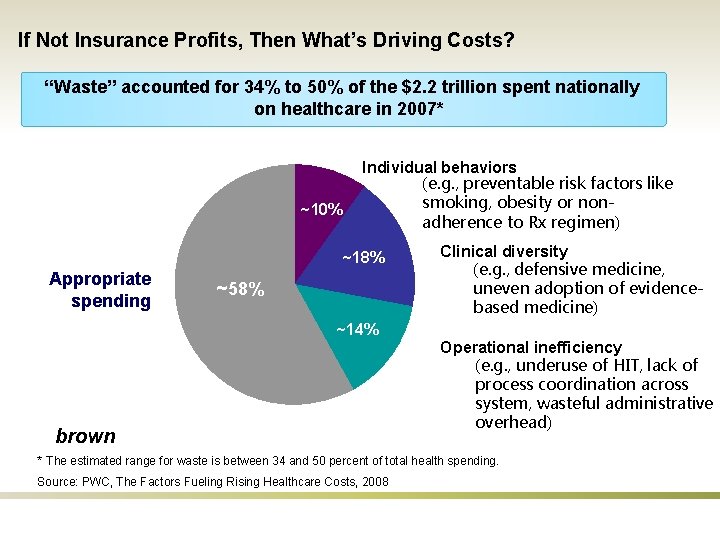
If Not Insurance Profits, Then What’s Driving Costs? “Waste” accounted for 34% to 50% of the $2. 2 trillion spent nationally on healthcare in 2007* ~10% Individual behaviors (e. g. , preventable risk factors like smoking, obesity or nonadherence to Rx regimen) ~18% Appropriate spending ~58% Clinical diversity (e. g. , defensive medicine, uneven adoption of evidencebased medicine) ~14% brown Operational inefficiency (e. g. , underuse of HIT, lack of process coordination across system, wasteful administrative overhead) * The estimated range for waste is between 34 and 50 percent of total health spending. Source: PWC, The Factors Fueling Rising Healthcare Costs, 2008

Myths v. Truths… Getting to the Bottom of the Issues Government-Run System? ? ? Single-Payer System? ? ? Government Limits on Doctors’ Wages? ? ? Death Panels? ? ? Illegal Immigrant Coverage? ? ? No Chemo for Older Medicare Patients? ? ? No Choice on Health Plan Coverage? ? ? Mc. Alpin, Wessler Denial of Care Based on Costs? ? ?

Major Issues and Concerns Facing the Health Sector • Improving quality – medical errors; substance abuse, mental health, asthma, diabetics receive ineffective care • Improving access and coverage - 50. 7 million American lacked insurance coverage in 2009 and millions more had inadequate coverage. • Slowing the growth of health care costs – health care costs are growing much more rapidly than the rest of the economy. • Encouraging healthy behavior – health behavior can help people avoid diseases and injury or prevent disease or disability from worsening. • Improving the coordination, transparency, and accountability of local system of care – problems of quality, cost, and access are largely attributable to the fragmentation and lack of coordination with the system. • Health disparities – inequalities in health status among various income groups, social classes, and ethnic groups

Titles in the PPACA • Title I Quality, affordable health care for all Americans • Title II The role of public programs • Title III Improving the quality and efficiency of health care • Title IV Preventing chronic disease and improving public health • Title V Health care workforce • Title VI Transparency and program integrity • Title VII Improving access to innovative medical therapies • Title VIII Community living assistance services and supports • Title VIII Revenue provisions • Title X Reauthorization of the Indian Health Care Improvement 9

TITLE I—QUALITY, AFFORDABLE HEALTH CARE FOR ALL AMERICANS • Sec. 1001. Amendments to the Public Health Service Act. The first section of the PPACA contains amendments to the Public Health Service Act of 1944. • Sec. 2711. No lifetime or annual limits. Prohibits all plans from establishing lifetime or unreasonable annual limits on the dollar value of benefits. • Sec. 2712. Prohibition on rescissions. Prohibits all plans from rescinding coverage except in instances of fraud or misrepresentation 10

TITLE I—QUALITY, AFFORDABLE HEALTH CARE FOR ALL AMERICANS Sec. 2713. Coverage of preventive health services. Requires all plans to cover preventive services and immunizations recommended by the U. S. Preventive Services Task Force and the CDC, and certain child preventive services recommended by the Health Resources and Services Administration, without any cost-sharing. • Sec. 2714. Extension of dependent coverage. Requires all plans offering dependent coverage to allow unmarried individuals until age 26 to remain on their parents’ health insurance. • 11

TITLE I—QUALITY, AFFORDABLE HEALTH CARE FOR ALL AMERICANS • Sec. 2715. Development and utilization of uniform explanation of coverage documents and standardized definitions. Requires the Secretary to develop standards for use by health insurers in compiling and providing an accurate summary of benefits and explanation of coverage. The standards must be in a uniformat, using language that is easily understood by the average enrollee, and must include uniform definitions of standard insurance and medical terms. The explanation must also describe any cost-sharing, exceptions, reductions, and limitations on coverage, and examples to illustrate common benefits scenarios. • Sec. 2716. Prohibition of discrimination based on salary. Employers that provide health coverage will be prohibited from limiting eligibility for coverage based on the wages or salaries of full-time employees. 12

TITLE I—QUALITY, AFFORDABLE HEALTH CARE FOR ALL AMERICANS • Sec. 2717. Ensuring quality of care. Requires the Secretary to develop guidelines for use by health insurers to report information on initiatives and programs that improve health outcomes through the use of care coordination and chronic disease management, prevent hospital readmissions and improve patient safety, and promote wellness and health. • Sec. 2718. Bringing down the cost of health care coverage. Health insurance companies will be required to report publicly the percentage of total premium revenue that is expended on clinical services, and quality rather than administrative costs. Health insurance companies will be required to refund each enrollee by the amount by which premium revenue expended by the health insurer for non-claims costs exceeds 20 percent in the group market and 25 percent in the individual market. The requirement to provide a refund expires on December 31, 2013, but the requirement to report percentages continues. 13

TITLE I—QUALITY, AFFORDABLE HEALTH CARE FOR ALL AMERICANS • Sec. 2719. Appeals process. Health insurers will be required to implement an effective process for appeals of coverage determinations and claims. • Sec. 1002. Health insurance consumer information. The Secretary shall award grants to States to enable them (or the Exchange) to establish, expand, or provide support for offices of health insurance consumer assistance or health insurance ombudsman programs. These independent offices will assist consumers with filing complaints and appeals, educate consumers on their rights and responsibilities, and collect, track, and quantify consumer problems and inquiries. Provides $30 million in funding and is effective upon the date of enactment of the bill. 14

TITLE I—QUALITY, AFFORDABLE HEALTH CARE FOR ALL AMERICANS • Sec. 1003. Ensuring that consumers get value for their dollars. For plan years beginning in 2010, the Secretary and States will establish a process for the annual review of increases in premiums for health insurance coverage. Requires States to make recommendations to their Exchanges about whether health insurance issuers should be excluded from participation in the Exchanges based on unjustified premium increases. Provides $250 million in funding to States from 2010 until 2014 to assist States in reviewing and, if appropriate under State law, approving premium increases for health insurance coverage and in providing information and recommendations to the Secretary. • Sec. 1004. Effective dates. Except for sections 1002 and 1003 (effective upon the date of enactment of this Act), this subtitle shall become effective for plan years beginning on or after the date that is 6 months after the date of enactment of this Act. 15 • .

Provisions in the Patient Protection and Affordable Act • http: //obamacarefacts. com/summary-ofprovisions-patient-protection-andaffordable-care-act/ 16

Accountable Care Organizations • An ACO is a group of providers who are jointly held accountable for achieving measured quality improvements and reductions in the rate of spending growth. 17

Accountable Care Organizations • Each ACO will be held accountable for the quality, cost, and care of Medicare patients • must operate for at least three years. • Must have a legal structure to receive and distribute shared savings payments • Must have a leadership and management structure to manage the ACO’s clinical and administrative elements 18

Accountable Care Organizations • Each ACO must promote evidence-based medicine and patient engagement, re-port quality and cost measures, and coordinate care. • The team is responsible for ensuring that all of the patient’s health care needs are met. 19

Accountable Care Organizations • ACOs will be required to submit data to CMS on clinical processes and outcomes, patient and caregiver care experience, utilization, and quality of care to evaluate whether they are meeting quality performance standards. • ACOs that reduce Medicare spending will be eligible to keep a percentage of the savings 20

CASE STUDY You are a new Clinical Pharmacy Manager. Your Director of Pharmacy has asked you to prepare a proposal for the Clinical Pharmacists to participate in new Accountable Care Organization (ACO) being formed by your health system. What are three initiatives that can be put into the proposal where pharmacists have a role in ACOs?
- Slides: 21