The afferents carrying sensations of stretch and fullness







































- Slides: 50






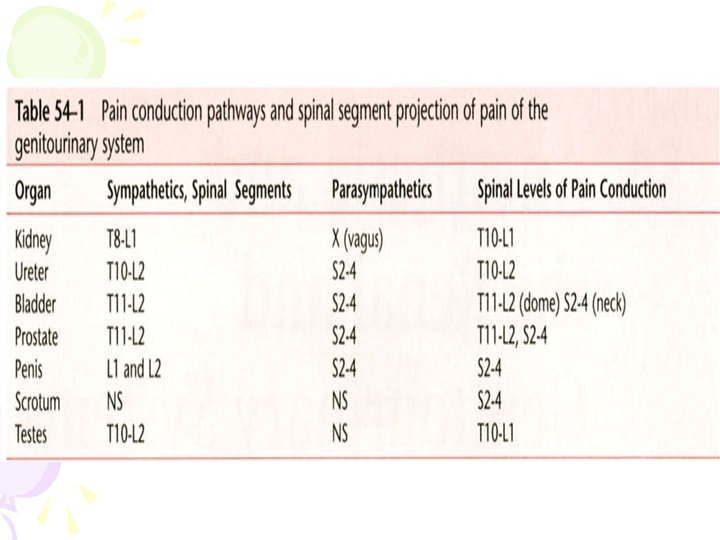
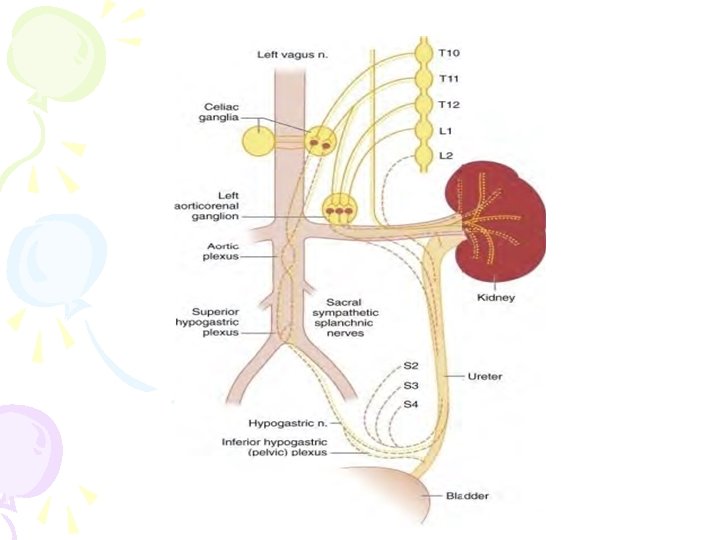
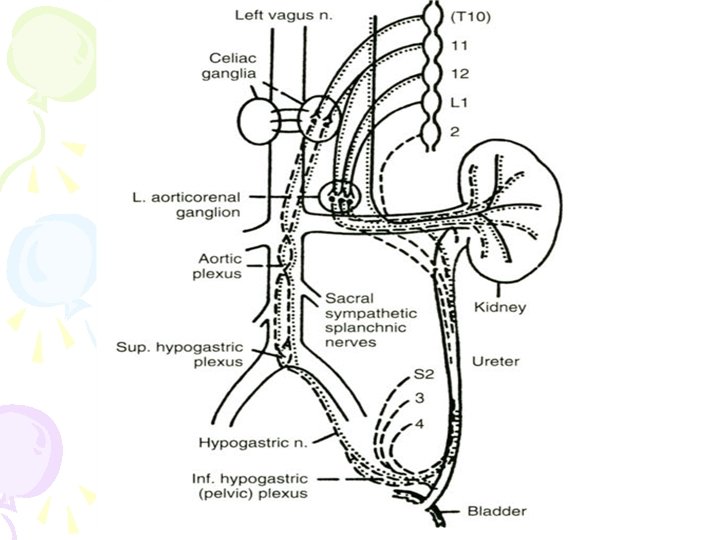
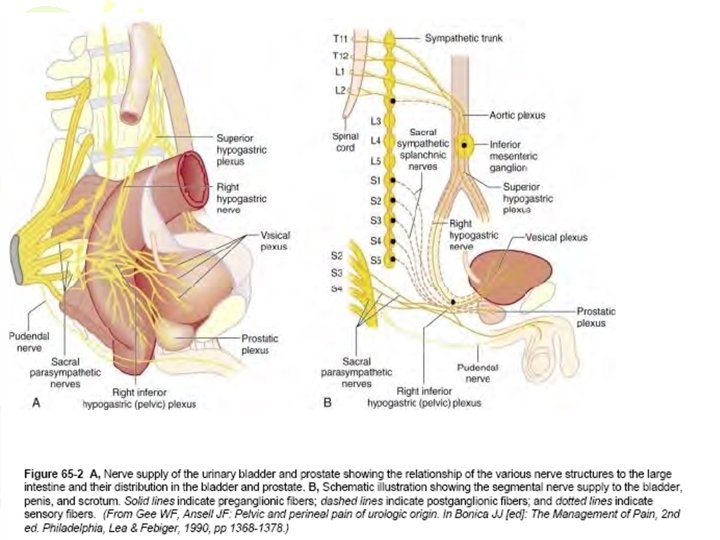
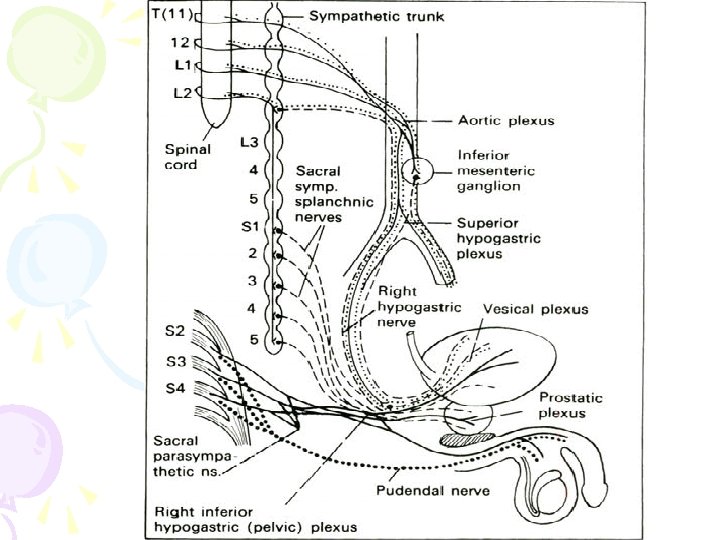
• The afferents carrying sensations of stretch and fullness of the bladder are parasympathetic, • whereas pain, touch, and temperature sensations are carried by sympathetic nerves. • Sympathetic fibers are predominantly a-adrenergic in the bladder base and urethra, and ß-adrenergic in the bladder dome and lateral wall.


Renal blood flow

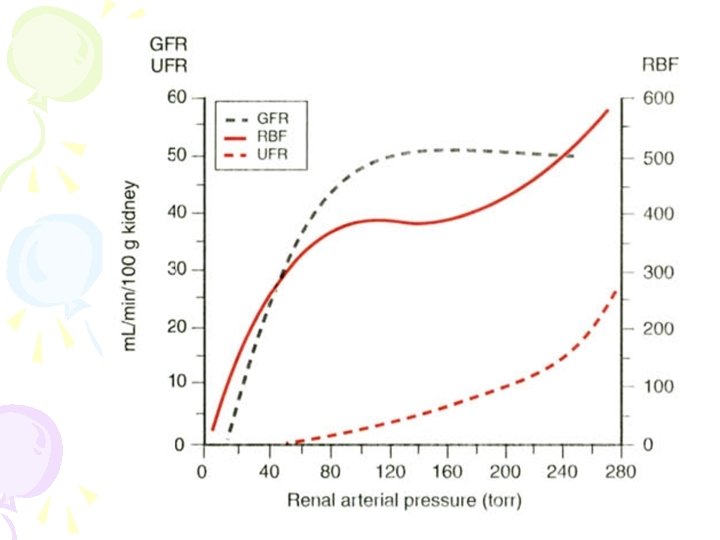
• The kidneys receive approximately 15% to 25% of total cardiac output, or 1 to 1. 25 L of blood per minute through the renal arteries, depending on the state of the body. Most of the blood is received by the renal cortex, with only 5% of cardiac output flowing through the renal medulla, which makes the renal papillae vulnerable to ischemic insults.

• Renal blood flow is regulated by various mechanisms that control the activity of vascular smooth muscle and alter vascular resistance. • Sympathetic tone of renal vessels increases during exercise to shunt renal blood flow to exercising skeletal muscle; similarly, renal blood vessels relax during the resting condition of the body.

• Sympathetic stimulation as a result of surgery can increase vascular resistance and reduce renal blood flow, whereas anesthetics may reduce renal blood flow by decreasing cardiac output.

• Glomerular capillaries separate afferent arterioles from efferent arterioles. • Glomerular capillaries are highpressure systems, whereas peritubular capillaries are lowpressure systems. • Consequently, the glomerular capillaries are a fluid-filtering system, whereas the peritubular capillaries are a fluid-absorbing system.

• vasa recta, a specialized portion of peritubular capillaries formed from efferent arterioles, are important in the formation of concentrated urine by a countercurrent mechanism. An intrinsic mechanism that causes • vasodilation and vasoconstriction of renal afferent arterioles regulates the autoregulation of renal blood flow.

• A decrease in mean arterial pressure also decreases renal blood flow and eventually affects the glomerular filtration rate (GFR) when the pressure decreases to less than 60 mm Hg. • A persistently low mean arterial • pressure greater than 60 mm Hg affects renal blood flow, but does not affect the GFR because of the intrinsic mechanism of autoregulation

• . Autoregulation maintains mean arterial pressure between 60 mm Hg and 160 mm Hg in intact and denervated kidneys.


Anesthesia for patient with renal disease

Evaluation of Renal Function • Renal disease may be discovered incidentally during a routine medical evaluation, or patients may present with evidence of renal dysfunction, such as hypertension, edema, nausea, and hematuria • The initial approach in both situations should be to assess the cause and severity of renal abnormalities.

• In all cases, this evaluation includes • (1) an estimation of disease duration, • (2) a careful urinalysis, and • (3) an assessment of the GFR.

• Further diagnostic categorization is according to anatomic distribution: prerenal disease, postrenal disease, • and intrinsic renal disease.

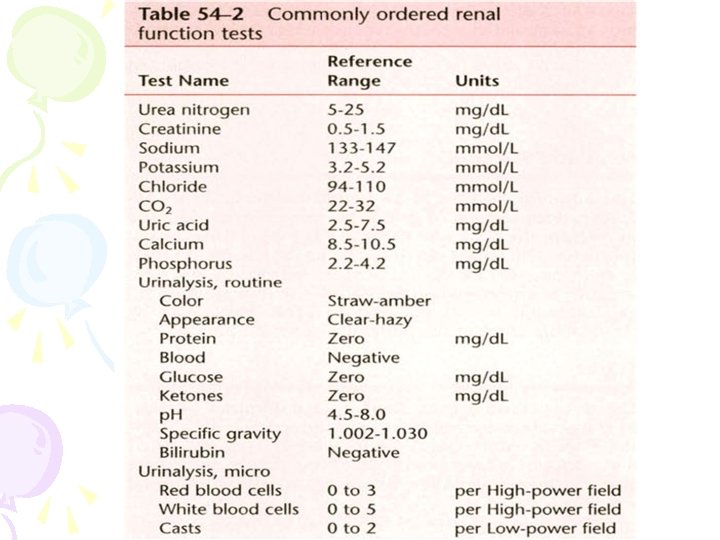
• Intrinsic renal disease can be divided further into • glomerular, • tubular, • interstitial, • vascular abnormalities. Laboratory tests useful in evaluating renal function


Glomerular Function

Glomerular Filtration Rate

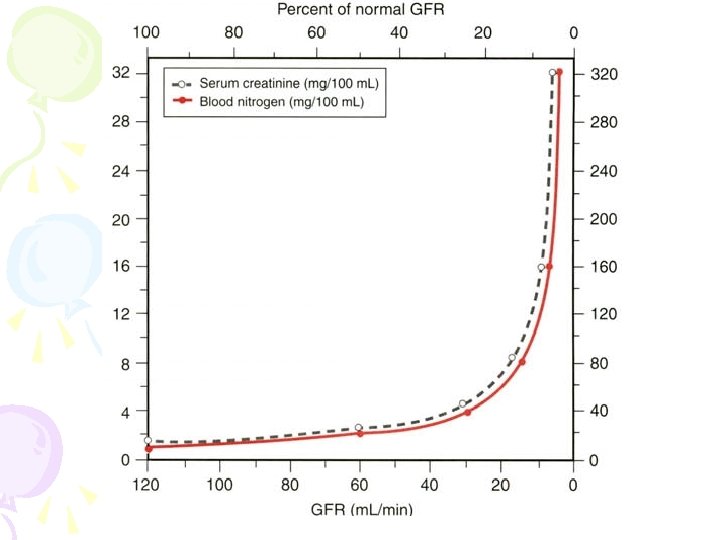
• The GFR is by far tile best measure of glomerular function. • Normal GFR is around l 25 m. L/min. • However, manifestations of reduced GFR are not seen until the GFR has decreased to( 50%)of normal. • When GFR decreases to 30% of normal, a stage of moderate renal insufficiency sets in.

• patients remain asymptomatic with only biochemical evidence of a decline in GFR (i. e. , an increase in serum concentrations of urea and creatinine). • Further workup usually reveals other abnormalities, such as nocturia, anemia, loss of energy, decreasing appetite, and abnormalities in calcium and phosphorus metabolism.

• As the GFR decreases further, a stage of severe renal insufficiency begins. • This stage is characterized by profound clinical manifestations of uremia and biochemical abnormalities, such as acidemia; volume overload; and neurologic, cardiac, and respiratory manifestations.

• At the stages of mild and moderate renal insufficiency, intercurrent clinical stress may compromise renal function further and induce signs and symptoms of overt uremia.

• When the GFR is 5% to 10% of normal, it is called end-stage renal disease (ESRD), and continued survival without renal replacement therapy becomes impossible. • Although most clinical abnormalities of corticotropin-releasing factor (CRF) are reversed by renal transplantation, the response to dialysis is quite variable

Blood Urea Nitrogen

• The blood urea nitrogen (BUN) concentration is not a direct correlate of reduced GFR. • BUN is influenced by nonrenal variables, such as exercise, bleeding, steroids, and massive tissue breakdown. • The more important factor is that BUN is not elevated in kidney disease until the GFR is reduced to almost 75% of normal.

Creatinine and Creatinine Clearance

• Measurements of creatinine provide valuable information regarding general kidney function. • Creatinine in serum results from turnover of muscle tissue and depends on daily dietary intake of protein. • Normal values are 0. 5 to 1. 5 mg/100 m. L; values of 0. 5 to 1 mg/100 m. L are present during pregnancy.

• Creatinine is freely filtered at the glomerulus, and apart from an almost negligible increase in content because of secretion in the distal nephron, it is neither reabsorbed nor secreted.

• Serum creatinine measurements reflect glomerular function and creatinine clearance is a specific measure of GFR.



• This value should be multiplied by 0. 85 for women because a lower fraction of body weight is composed of muscle.

• The serum creatinine concentration and clearance are better indicators of general kidney function and GFR than similar measurements of urea nitrogen

• Table 65 -4 -- Conditions Affecting Blood Urea Nitrogen (BUN) Independently of Glomerular Filtration • Rate • Increased BUN • Reduced effective circulating blood volume (prerenal • azotemia) • Catabolic states (gastrointestinal bleeding, corticosteroid use) • High-protein diets • Tetracycline • Decreased BUN • Liver disease • Malnutrition • Sickle cell anemia • SIADH, syndrome of inappropriate secretion of antidiuretic hormone.

• Table 65 -5 -- Conditions Affecting Serum Creatinine Independently of Glomerular Filtration Rate • Condition Mechanism • Conditions Causing Elevation • Ketoacidosis Noncreatinine chromogen • Cephalothin, cefoxitin Noncreatinine chromogen • Flucytosine Noncreatinine chromogen • Other drugs—aspirin, cimetidine, probenecid, • trimethoprim Inhibition of tubular creatinine secretion • Conditions Causing Decrease • Advanced age Physiologic decrease in muscle mass • Cachexia Pathologic decrease in muscle mass • Liver disease Decreased hepatic creatine synthesis and cachexia • Tubular Function

Tubular Function Concentration Protein Sugar

Important Pathophysiologic Manifestations of Chronic Renal Failure

Hypervolemia • Total-body contents of Na++ and H 2 O are increased in chronic renal failure (CRF), although this increase may not be clinically apparent until the GFR is reduced to very low levels. • Weight gain is usually associated with volume expansion and is offset by the concomitant loss of lean body mass.

Acidemia • Although urine can be acidified normally in most patients with CRF, these patients have a reduced ability to produce ammonia. • In the early stages, the accompanying organic anions are excreted in urine, and the • metabolic acidosis is of the non– anion gap variety.

• With advanced renal failure, a fairly large “anion gap” may develop (to approximately 20 mmol/L), however, with a reciprocal decrease in plasma HCO 3 concentration. • This acidemia is usually corrected by hemodialysis. • Although acidemia is well compensated in moderate CRF, patients can become acidemic and hyperkalemic in the postoperative period

Hyperkalemia • The approximate daily filtered load of K+ is 700 mmol. Most of this filtered load is reabsorbed in tubule segments, • most of the K+ excreted in the final urine reflects events governing K+ handling at the level of the cortical collecting tubule and beyond. • K+ excretion in the gastrointestinal tract is augmented in patients with CRF.

• Hyperkalemia may be precipitated, however, in numerous clinical situations, including protein catabolism, hemolysis, hemorrhage, transfusion of stored blood cells, metabolic acidosis, and exposure to various medications that inhibit K+ entry into cells or K+ secretion in the distal nephron.

Cardiac and Pulmonary Manifestations • Hypertension is a common complication of CRF and ESRD. • Because hypervolemia is the major cause of hypertension in uremia, normotension is usually restored by the use of diuretics in predialysis patients or by dialysis in ESRD patients.

• Patients generally have left ventricular hypertrophy and accelerated atherosclerosis (disordered glucose and fat metabolism). • Pericarditis can be observed in underdialyzed patients versus patients with CRF who undergo regular dialysis.