The ABCs Of Carotid Endarterectomy Does Type of

The ABC’s Of Carotid Endarterectomy: Does Type of Anesthesia and Technique Matter? John. J Ricotta, MD, FACS Professor of Surgery, Georgetown University Chair of Surgery, Washington Hospital Center CRT 2012

John J. Ricotta, MD I have no real or apparent conflicts of interest to report.

Introduction • As a prophylactic operation, CEA should have the lowest possible complication rates • Results of CEA have improved significantly over the last 3 decades -10% S/D in 1980’s to 1 -2% S/D in 2010 • Refinements in patient selection and technique are responsible for this improvement

Deaths after Carotid Endarterectomy Trends in the in-hospital stroke rate following carotid endarterectomy In California and Maryland S. L. Matsen et al J Vasc Surg 2006; 44: 488 -95 • Observational study of administrative data • In-hospital stroke & mortality • All CEA in Maryland 1994 -2003, n=23, 237 • All CEA in California 1999 -2003, n=51, 331 Stroke Death MD 0. 73% 0. 54% CA 0. 45% 0. 48%

Complications after CEA • Death – primarily Cardiac causes – patient selection – anesthetic management • Stroke – Primarily Technical – avoid embolization – maintain cerebral perfusion – avoid thrombosis

Patient Selection • Avoid intervention in “high risk” asymptomatic patients – SAPPHIRE • Detect and treat Occult myocardial ischemia in all asymptomatic patients prior to intervention • Stabilize all medical conditions in symptomatic patients prior to intervention – CEA is an elective, sometimes urgent but never emergent procedure

Anesthetic Management • Hemodynamic Instability occurs in about 20% of CEA patients and some kind of hemodynamic intervention may be required in up to 50% • Patients with poorly controlled hypertension are most at risk • Swings in BP are associated with both cardiac and cerebrovascular complications • Loco. Regional Anesthesia (LRA) may have a role in these patients. Also allows selective shunting
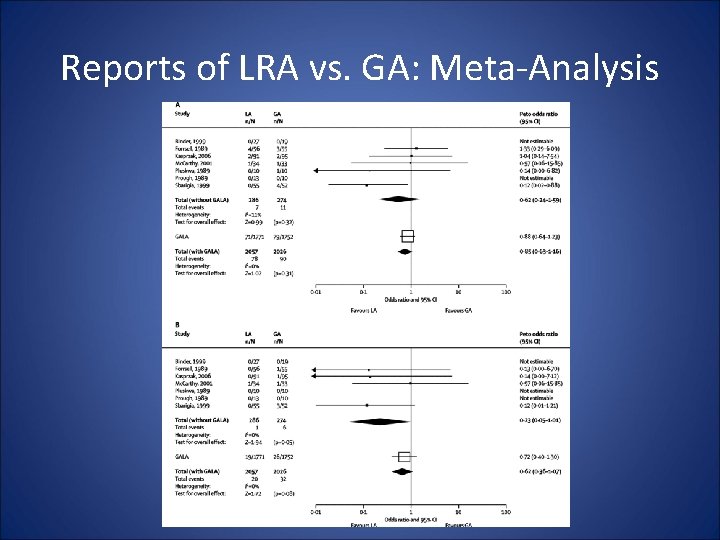
Reports of LRA vs. GA: Meta-Analysis

GALA Trial (Lancet 2008) • Compared LRA and GA in 3500 pts • No difference in stroke or death rate between LRA and GA • “Intervention” for control of BP was more common in GA that LRA Conclusion: LRA will only be of benefit in patients where intraoperative control of BP is likely to be difficult
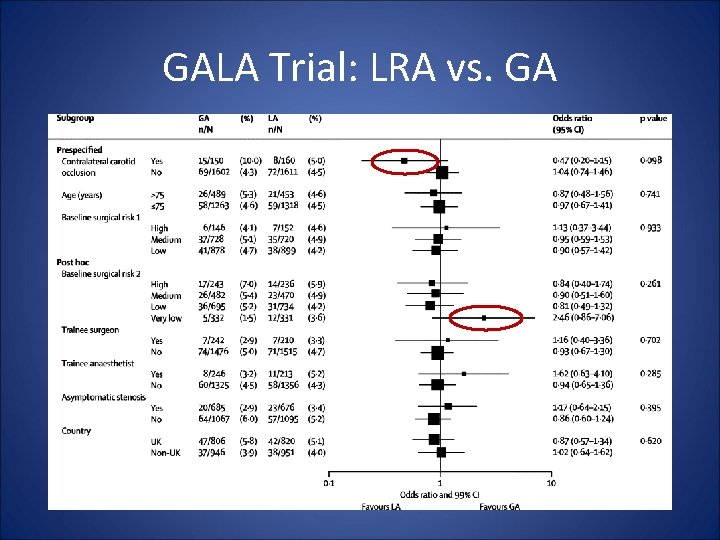
GALA Trial: LRA vs. GA

CEA Technique • Wide Exposure: Digastric – Omohyoid avoid traction injury • Identify and protect CN VII, IX, X, XII • “No touch” , distal clamp first • Arteriotomy in the Midline of the ICA • Visualize Endpoints – tacking sutures as needed • Avoid redundancy – eversion, plication • Routine Patch
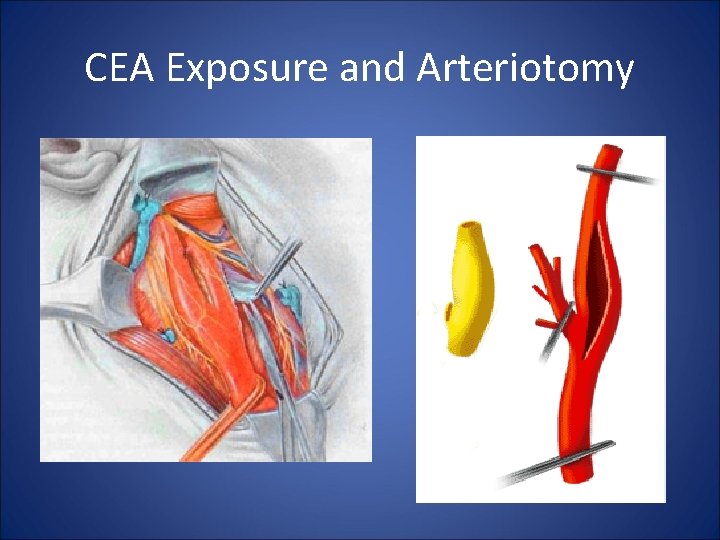
CEA Exposure and Arteriotomy

Cerebral Perfusion Routine vs. Selective Shunt • <10% of pts will require augmentation of CBF during CEA – recent stroke, contralateral occlusion, VBI symptoms • Most symptoms develop within minutes of cross clamping – 4 min of ischemia is OK • No data to show benefit of selective vs. routine shunt – meta analysis • Shunt has its own complications – emboli, flaps, poor visualization of endpoints

When to Shunt? • Recent symptoms • Evidence of poor distal perfusion back pressure ( 25? , 40? , 50? ) • End organ dysfunction – EEG, SSEP • Local Anesthesia • Most pts do not require a shunt, if abnormalities occur check systemic BP • Occasionally place shunt AFTER CEA and prior to closure

Shunting during CEA Personal Perspective • Place shunt under control, never force always back bleed • When in doubt – DO NOT SHUNT • Shunt can be removed if necessary to allow complete plaque removal • Shunt is rarely needed once CEA is in progress.

Preventing Thrombosis: Arterial Closure • Prospective Randomized data favor Routine Patch Closure over Primary Closure for standard CEA for reduced stroke rate and reduced restenosis • Patch Material immaterial • Eversion = Patch Closure • Eversion useful for redundancy, high lesions
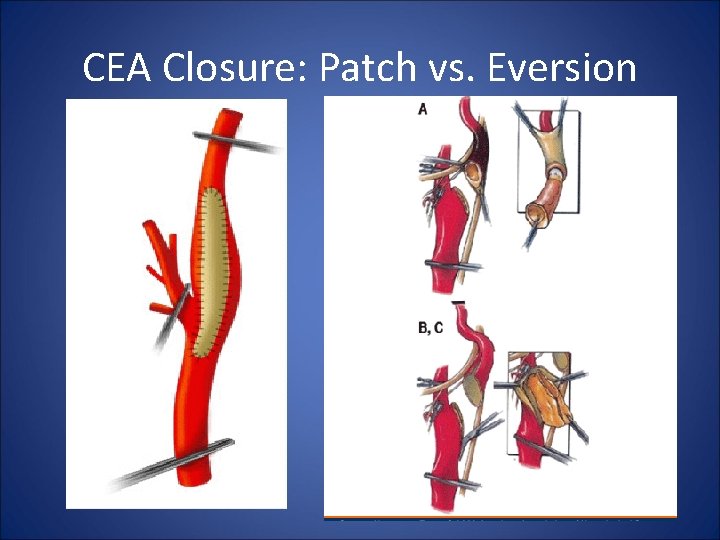
CEA Closure: Patch vs. Eversion
Preventing Thrombosis: Completion Imaging • Routine Completion Imaging has been advocated to reduce complication rates - the significance of most abnormalities remains unclear • With complete plaque removal and appropriate anti thrombotic Rx routine imaging is not needed. • Selective imaging with difficult cases/poor visualization

Preventing Thrombosis: Antithrombotic Rx • Thrombosis is generally worse than bleeding in this situation • CEA creates a raw surface that attracts platelets and thrombi • ASA plus Dextran vs. ASA plus Plavix • Heparin reversal is optional • There is increase bleeding risk but reoperation for bleeding is well tolerated

Summary • Perioperative Management and meticulous technique are critical to maximize the outcomes of CEA - Appropriate Patient Selection and preparation - Selective use of Regional Anesthesia - Optimal Exposure - Complete Plaque Removal under vision - meticulous closure

Summary • Routine Patch Closure or Eversion technique should be performed • The indications for shunting and completion imaging are individualized • Aggressive perioperative antithrombotic therapy is helpful • Stroke / Death Rates <2% should be expected
- Slides: 21