Textbook of Palliative Care Communication Section I Communication

Textbook of Palliative Care Communication Section I: Communication Principles

Chapter One OVERVIEW OF COMMUNICATION

Approaches to Communication • Relationship-driven – Patient and family do not receive information; they co-create messages and construct meaning with providers – Information is not the main outcome of clinical communication • Outcome is the relationship built between provider and patient/family. • Information-driven or sender-based – Outcome is based on delivery and receipt of medical knowledge – Receipt of information is considered effective communication • Outcome derives from the sender’s performance

Our Concept of Communication • Transactional – The parties contribute to and negotiate the meaning of messages, both verbally and nonverbally • Relational – All messages have at least two levels of meaning: the task or informational level and the relationship level, which cues interactants how to interpret and process the message itself • Mutual – Communicators influence one another

COMFORT Communication Model The seven basic principles of palliative care communication, from a relational communication perspective: – Communication (clinical narrative practice) – Orientation and opportunity – Mindful communication – Family – Openings – Relating – Team

Chapter Two A HISTORICAL PERSPECTIVE IN PALLIATIVE CARE COMMUNICATION

Communication: The Cornerstone of Quality Care Early Focus of Communication in Healthcare – Avoided the subject of death and dying – Discussing death and dying was perceived as stressful to patient

Hospice and the Role of Communication Hospice Movement: Strides forward in Communication Hospice providers encouraged open and honest communication – Introduction of team-based care and team communication

Communication Comes to the Forefront National Consensus Project • In 2004, clinical practice guidelines were developed by a consortium of the leading palliative care organizations, representing a major advance in palliative care • Quality communication is at the core of all the palliative care guidelines: – – – – Domain 1 -Structure and Process of Care Domain 2 – Physical Domain 3 – Psychological and Psychiatric Domain 4 – Social Domain 5 – Spiritual Domain 6 – Cultural Domain 7 – End of Life Domain 8 – Ethical and Legal

Current Communication Trends in Palliative Care Literature • Patients’ and families’ desire for honest and open communication • The importance of communicating hope in palliative settings • Barriers to communication • Communication needs among pediatric populations • Use of technology to improve communication

Current Limitations of Palliative Care Communication • Research has focused on physician-patient interactions • Communication education restricted to “breaking bad news” discussions • Protocols or “step” approaches have excluded relational approach • Training has been limited to lecture format

Chapter Three TRANSACTIONAL COMMUNICATION

Transmission Model of Communication • Also called the sender-oriented approach – Sender transmits message to receiver • Shortfalls: – Uneven balance of power between sender and receiver (ex: healthcare provider and patient) – Depicts communication as product of independent parties without a guarantee that important information will be heard and understood by receiver – Little concern for medium and medium’s effectiveness (face-to-face, telephone, email)
Transactional Model of Communication • People are simultaneously senders and receivers in an ongoing process – Each person is influenced by the other – Emphasizes shared meaning and what happens “between people”, between the sender and receiver • Benefits: – Encourages people to share power – Reminds people to be attentive to cues about how others interpret information – Recognizes social, environmental, personal factors

BATHE • A five-part guide for responding to emotions – Background information (Briefly, what has been going on? ) – Affect (How has this affected you? ) – Trouble (What troubles you most? ) – Handling things (How have you been handling this situation? ) – Empathy (It sounds like this is very stressful)

Relationship-Centered Care Model • Focus on how relationships are enacted across all healthcare providers who are serving the patient – Mindful Communication (awareness of self, others, relationships, and being open to new ideas) – Diversity of Mental Models (how to manage diversity within the context of care) – Mutual Respect (team members are honest, respectful of each other) – Mix of Social and Task-Related Interactions (have fun, but be productive)

Chapter Four CONSUMER COMMUNICATION AND PUBLIC MESSAGING

Knowledge of Palliative Care • In 2011, a national poll revealed that 7 in 10 Americans are not knowledgeable about palliative care • Providers are also unfamiliar with the scope of palliative care, equating palliative care to hospice

Definition of Palliative Care • Palliative care is specialized medical care for people with serious illnesses. Its goal is to provide relief from the symptoms, pain, and stress of a serious illness – whatever the diagnosis – to improve the quality of life for both the patient and the patient’s family. • Palliative care is provided by a team of doctors, nurses, and other specialists who work with a patient’s other doctors to provide an extra layer of support. Palliative care is appropriate for all patients suffering from serious illness - at any age and at any stage - and can accompany curative treatment.

Key Messages to Convey about Palliative Care: • Helps provide the best possible quality of life • Helps manage pain, symptoms, and stress of illness • Is a partnership between patient, family, and healthcare providers • Provides the patient and family an extra layer of support • Is appropriate at any age and at any stage of a serious illness, alongside curative treatment

Resources for Palliative Care Communication • Vitaltalk (vitaltalk. org) – Advanced communication skills resources and courses for professionals focused on balancing honesty with empathy, when discussing serious illness. • Palliative Care Communication Institute (pccinstitute. com) – Free teaching materials to advance a patient-centered training program called COMFORT– designed to teach communication strategies for patient-centered palliative care.

Chapter Five COMMUNICATION ETHICS

Communication Ethics • Ethical communication is a form of care, subject to ethical norms: – Respect for personhood – Minimize harm – Maximize benefit • Cecily Saunders summarizes an approach to sensitive communication: “The real question is not ‘what do you tell your patients? ’ but rather ‘what do you let your patients tell you? ’”

Palliative care as a moral practice • Goals of practice need to be well-defined and resonant with larger social values • Palliative care must have shared internal values that promote the goals of practice • Palliative care provides “agency” to patients, allowing care to be patient-centered, enabling the patient to develop and exercise a sense of self by engaging with the world in a manner that sets and achieves goals by doing things for oneself.

Communication as an Ethical Obligation • Communication should seek to: – discern and incorporate the values and preferences of patients and family members, thereby respecting their autonomy – minimize the risk of avoidable harm, thereby respecting nonmaleficence – maximize benefit to patients and families by engaging processes and producing outcomes that are consistent with how they would define “good, ” thereby honoring beneficence.

Communication within the Team • Moral agency of team members is a significant part of the ethical equation • Be attentive, self-aware, and reflective to the emotional responses of oneself and other healthcare providers • Consider professional hierarchy in healthcare

Chapter Six COMMUNICATION IN PALLIATIVE SOCIAL WORK

Social Work Communication • Diagnosis – Tailor information to individual and family needs – Address Psychosocial concerns • Plan of Care – Organize and interpret patient and family data • Advance Care Planning – Support patient autonomy, self-determination – Include caregivers

Social Work Communication • Pain and Symptom Management – Educate patient and family about medication, side effects – Teach complimentary and alternative techniques • Practical support – Discuss home care needs, insurance, financial needs • Assess patient distress – Provide supportive counseling – Reinforce strengths and coping mechanisms

Social Work Communication • Religious, spiritual, existential issues – Discuss degree of religiosity, use of spirituality as coping mechanism – Discuss guilt, regret, need forgiveness • Evaluate role of culture in understanding of illness, role of language, decision-making style • Integrate cultural values into decision-making

Social Work Communication • End of life communication – Discuss practical aspects of patient’s death – Discuss hopes and fears for patient and family – Educate about expected course • Talking about hospice – Participate in intake assessment – Identify psychosocial concerns – Target caregivers with high bereavement distress

Chapter Seven COMMUNICATION IN PALLIATIVE MEDICINE

Why Communication in Palliative Medicine Matters • Findings across research studies illustrate a need for communication: – Only half of all patients discussed hospice with any doctor two months before death – More than half of lung and colorectal cancer patients thought their chemotherapy was curative – Only a third of lung cancer patients understood that radiation would not cure them – Less than 20% of patients had accurate awareness of their prognosis

Key Barriers to Communication • Patient factors – Emotional overwhelm, language barriers, cultural barriers may create mistrust of physicians; patients may have limited health literacy, over-estimate cure • Physician factors – Lack of proper communication skills or training in managing emotions; fear of causing pain or taking away hope • Healthcare factors – No incentives for patient-centered communication, multiple transitions of care, multiple subspecialists
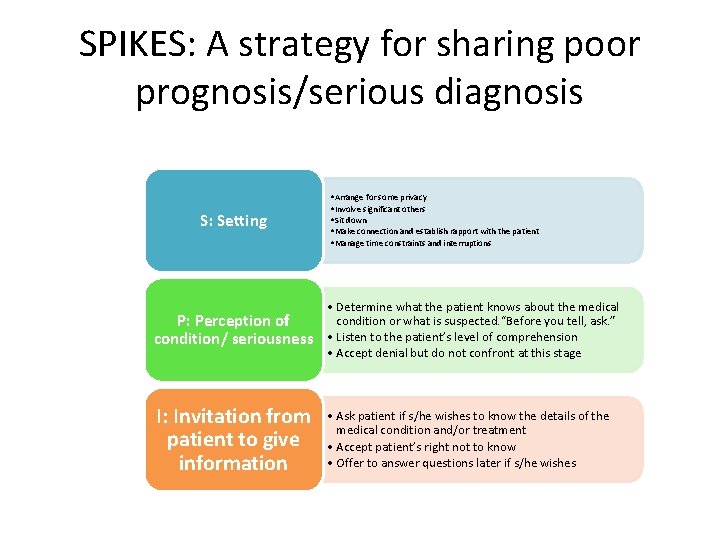
SPIKES: A strategy for sharing poor prognosis/serious diagnosis S: Setting • Arrange for some privacy • Involve significant others • Sit down • Make connection and establish rapport with the patient • Manage time constraints and interruptions P: Perception of condition/ seriousness • Determine what the patient knows about the medical condition or what is suspected. “Before you tell, ask. ” • Listen to the patient’s level of comprehension • Accept denial but do not confront at this stage I: Invitation from patient to give information • Ask patient if s/he wishes to know the details of the medical condition and/or treatment • Accept patient’s right not to know • Offer to answer questions later if s/he wishes
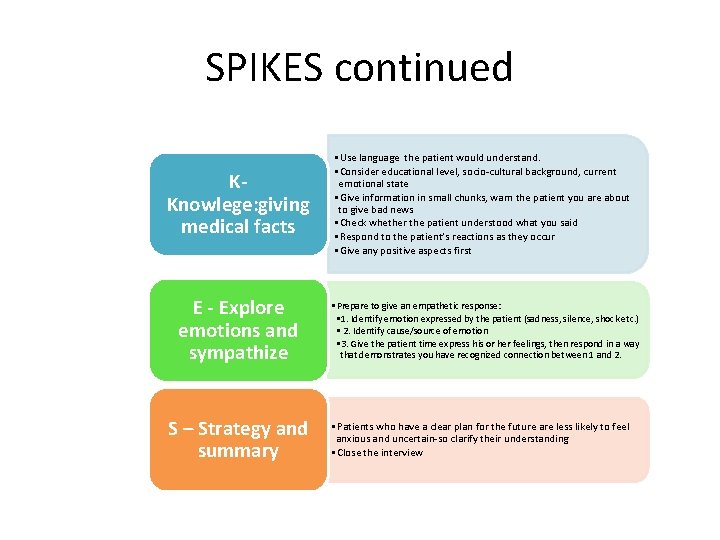
SPIKES continued KKnowlege: giving medical facts E - Explore emotions and sympathize S – Strategy and summary • Use language the patient would understand. • Consider educational level, socio-cultural background, current emotional state • Give information in small chunks, warn the patient you are about to give bad news • Check whether the patient understood what you said • Respond to the patient’s reactions as they occur • Give any positive aspects first • Prepare to give an empathetic response: • 1. Identify emotion expressed by the patient (sadness, silence, shock etc. ) • 2. Identify cause/source of emotion • 3. Give the patient time express his or her feelings, then respond in a way that demonstrates you have recognized connection between 1 and 2. • Patients who have a clear plan for the future are less likely to feel anxious and uncertain-so clarify their understanding • Close the interview

Chapter Eight COMMUNICATION IN PALLIATIVE NURSING

Nurse Communication • Participates in patient assessment and in collaborative care planning with team – Nurses rated by public as most trusted healthcare team member • Uses symptom assessment instruments to evaluate pain, take pain history • Uses verbal or symbolic means appropriate to patient to assess coping

Nurse Communication • Facilitates communication within circle of care – Patient, family, healthcare team, other providers • Assessment and attention to spiritual issues and concerns for patient and family • Elicits cultural identification, strengths, concerns, needs – Determines cultural background as source of resilience and strength for patient and family

Nurse Communication • Communicates signs and symptoms of dying process to patient, family, others • Explains what to expect in the dying process and provides support post-death • Contributes to ongoing discussion about goals of care, promoting understanding of patient’s preferences

Barriers to Nurse Communication • Personal – Cultural norms, shyness, fear of mortality, unresolved personal losses • Educational – Few nursing schools offer instruction in palliative care – Lack of experience with death, dying, and communication – Younger generation of nurses have had little exposure or practice with face-to-face verbal communication • Professional – Inadequate nursing education and role ambiguity

Chapter Nine COMMUNICATION IN PALLIATIVE CARE CHAPLAINCY

Basics of Chaplain Communication • Assist in Meaning-Making – Global meanings are a person’s most basic values and beliefs about the way the world works – Situation meaning is the meaning given to a particular event such as illness or death • Emphasis on active listening rather than information-giving • Do not proselytize or impose one’s beliefs on others

Barriers • Defining chaplaincy – “Being present” is too vague – Any two chaplains do not describe their work in the same way – Need to translate spiritual work into medical language and processes • Healthcare team members do not know how to conduct spiritual assessment; refer to chaplain

Chaplain as Team Member • Expert on spiritual subject matter • Offer guidance on spiritual communication • Provide understanding about family culture and spiritual traditions/rituals • A chaplain is often viewed as a neutral, trusted person as compared to other healthcare providers • Assist with families who are awaiting miracle cure

Future Work • More research is needed to document outcomes and accountability of chaplain services – Document the benefit of chaplain services – Document patients’ spiritual needs ents – Document interventions to reduce spiritual distress

Chapter Ten COMMUNICATION IN CLINICAL PSYCHOLOGY

Clinical Psychologist in Palliative Care • Four key roles: – Assess and target treatment services for patients – Provide education and supportive services to families and caregivers – Participate in educational and support activities that assist the palliative care team

Provision of patient assessment services • Assessment Aims – Symptoms, duration, and situational factors associated with psychosocial health • Assessment Approaches – Interview and self-report questionnaires – Neurocognitive functioning • Assessment Domains – Pre-morbid functioning, health literacy, perception of illness

Provision of treatment services • Goal-setting and Problem-solving – Establishing goals grounded in patient values • Psychotherapy – Cognitive Behavioral Therapy • Tools to modify dysfunctional thinking and behavior – Existential Psychotherapy • Helping patient confront the struggle of being human – Psychotherapy at the End of Life • Assist patient to achieve a respectful death, dignity

Psychologists’ involvement with patients’ family systems • Supporting family communication • Cultural health beliefs • ‘law of double death’ in families – Awareness of likelihood of death, but do not discuss their fears or concerns with one another • ‘third person’ in families – Families cannot discuss anxieties related to death with patient, but can with other parties

The Psychologist as a member of the interdisciplinary palliative care team • Contribute patient information to team • Educate staff • Provide staff support and facilitation of selfcare as a team member – Assistance with compassion fatigue, trauma
- Slides: 52