Text Important Formulas Numbers Doctor notes Notes and

§ § § Text Important Formulas Numbers Doctor notes Notes and explanation 1 Lecture No. 24 “You Will Never Have This Day Again, So Make It Count ”.

UPPER & LOWER MOTOR NEURON LESION Objectives: 1. Appreciate what is meant by upper and lower motor neurons and their functional anatomy 2. Explain and differentiate between features of lesions of the upper and lower motor neurons 3. Describe effects of lesions in pyramidal tracts 4. Describe effects of lesions in the internal capsule 5. Explain the manifestations of complete spinal cord transection and hemisection 6. Explain features of Brown Sequard Syndrome 7. Correlate the site of lesion with pattern of loss of sensations 8. Describe facial, bulbar and pseudobulbar palsy 2
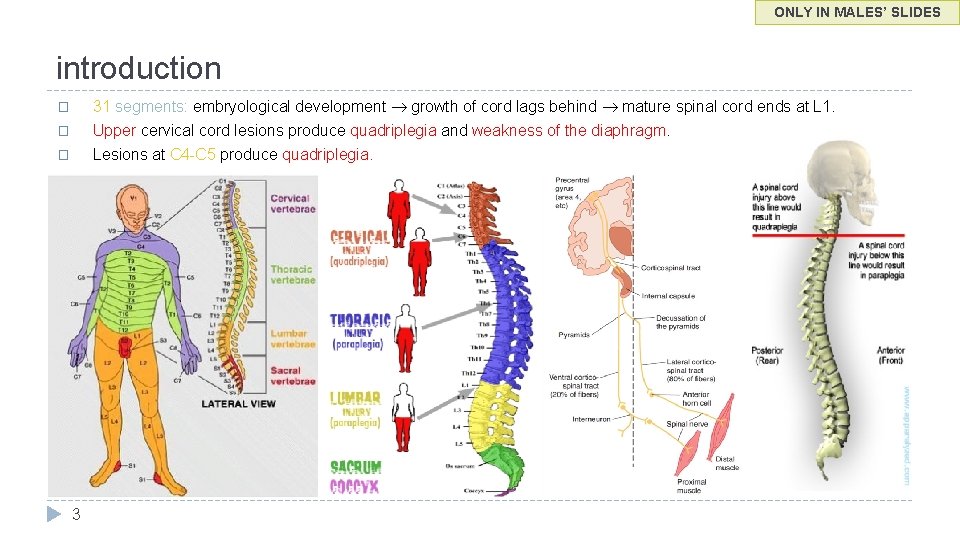
ONLY IN MALES’ SLIDES introduction 31 segments: embryological development growth of cord lags behind mature spinal cord ends at L 1. Upper cervical cord lesions produce quadriplegia and weakness of the diaphragm. Lesions at C 4 -C 5 produce quadriplegia. � � � 3
Comaprison between upper & lower motor neuron lesions ONLY IN MALES’ SLIDES Two sets of neurons are important Upper motor neurones • Paralysis affect movements. • Wasting not pronounced. • Spasticity Muscles • hypertonic (Clasp Knife). • Tendon reflexes increased. • Superficial reflexes diminished. • Babinski’s sign +ve. • NCV- normal • No denervation potentials in EMG Characteristic of upper motor neurone lesions: • no wasting. • Loss of skilled finger/toe movements • increased tone of claspknife Type. • weakness most evident • in anti-gravity muscles. • increased reflexes and clonus. • • extensor plantar responses. 4 Lower motor neurones • Individual muscle or group of muscles are affected. • Wasting pronounced. • Flaccidity. Muscles hypotonic. • Tendon reflexes diminished or absent. • Ncv- abnormal • Denervation potentials in EMG (fibrillations) • Muscle contractures • Trophic changes in skin and nails. Characteristic of upper motor neurone lesions: • Wasting. • Fasciculation (tapping produce it) • Decreased tone (i. E. Flaccidity) • Weakness. • Decreased or absent reflexes. • Flexor or absent plantar responses.
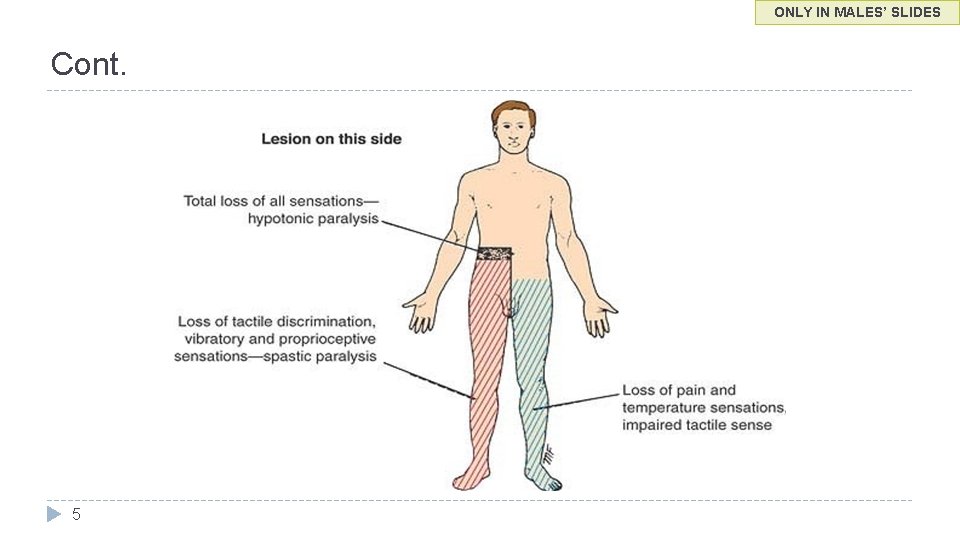
ONLY IN MALES’ SLIDES Cont. 5
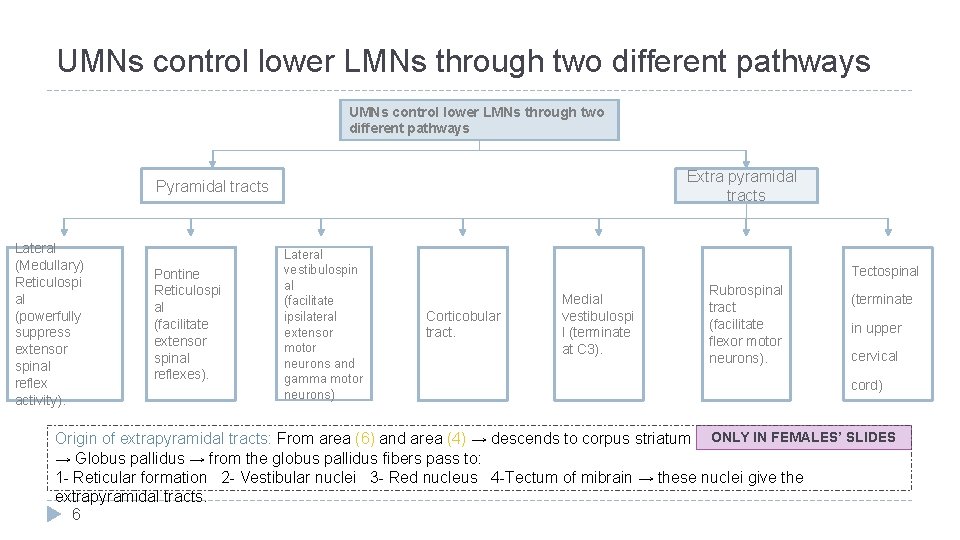
UMNs control lower LMNs through two different pathways Extra pyramidal tracts Pyramidal tracts Lateral (Medullary) Reticulospi al (powerfully suppress extensor spinal reflex activity). Pontine Reticulospi al (facilitate extensor spinal reflexes). Lateral vestibulospin al (facilitate ipsilateral extensor motor neurons and gamma motor neurons) Tectospinal Corticobular tract. Medial vestibulospi l (terminate at C 3). Rubrospinal tract (facilitate flexor motor neurons). (terminate in upper cervical cord) Origin of extrapyramidal tracts: From area (6) and area (4) → descends to corpus striatum ONLY IN FEMALES’ SLIDES → Globus pallidus → from the globus pallidus fibers pass to: 1 - Reticular formation 2 - Vestibular nuclei 3 - Red nucleus 4 -Tectum of mibrain → these nuclei give the extrapyramidal tracts. 6
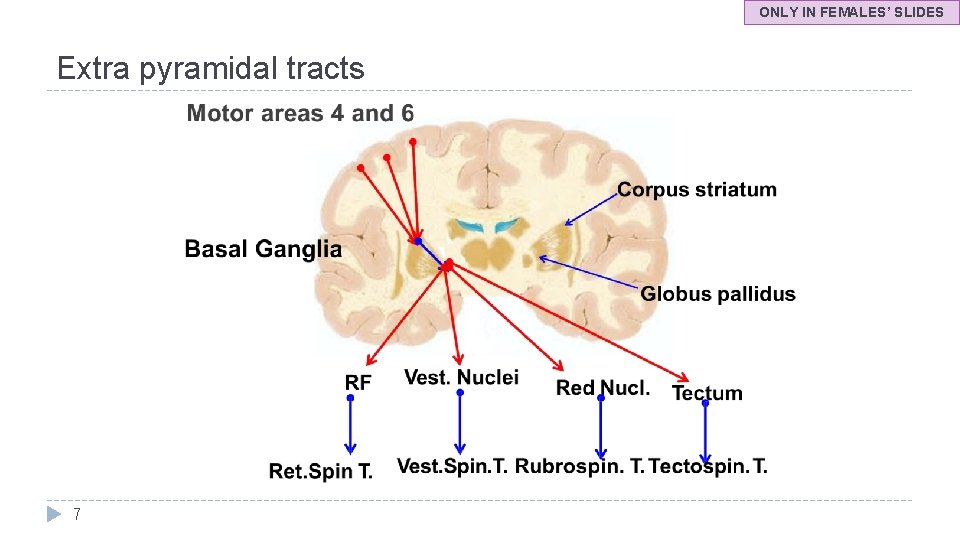
ONLY IN FEMALES’ SLIDES Extra pyramidal tracts 7

Extra UMNs control lower LMNs through two different pathways Pyramidal tracts 8 Extra pyramidal tracts § There is > 1 million of fibers in each corticospinal tract. § 97 % of these are small (<4 µm) and conduct background tonic signals to the spinal cord. § Only 3% of the fibers are large: • (16 µm) fast conducting (Aβ-type). § These fibers originate from giant: • Betz cells ( 60 µm). § These cells are found only in: • the primary motor cortex. § There about 34, 000 of these large Betz cell fibers in each corticospinal tract.
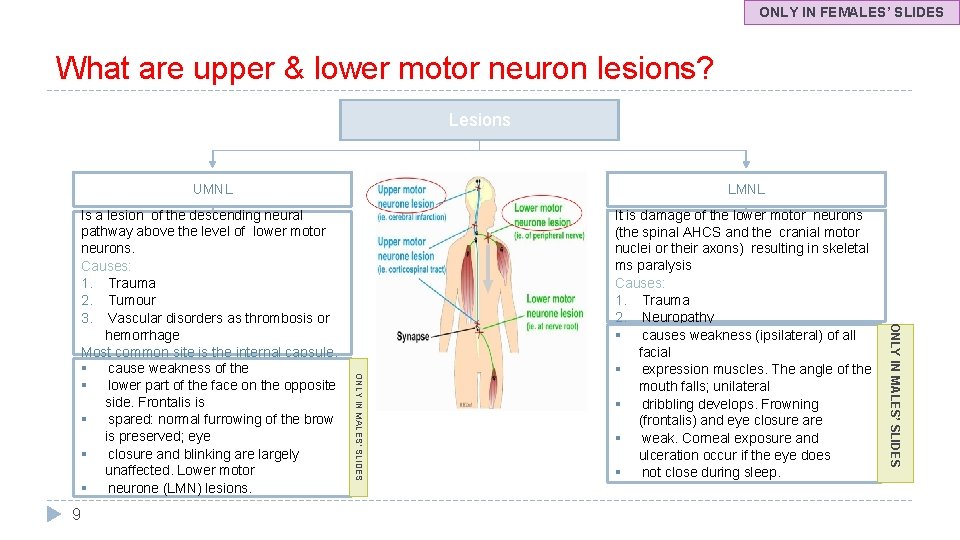
ONLY IN FEMALES’ SLIDES What are upper & lower motor neuron lesions? Lesions Is a lesion of the descending neural pathway above the level of lower motor neurons. Causes: 1. Trauma 2. Tumour 3. Vascular disorders as thrombosis or hemorrhage Most common site is the internal capsule. § cause weakness of the § lower part of the face on the opposite side. Frontalis is § spared: normal furrowing of the brow is preserved; eye § closure and blinking are largely unaffected. Lower motor § neurone (LMN) lesions. It is damage of the lower motor neurons (the spinal AHCS and the cranial motor nuclei or their axons) resulting in skeletal ms paralysis Causes: 1. Trauma 2. Neuropathy § causes weakness (ipsilateral) of all facial § expression muscles. The angle of the mouth falls; unilateral § dribbling develops. Frowning (frontalis) and eye closure are § weak. Corneal exposure and ulceration occur if the eye does § not close during sleep. 9 ONLY IN MALES’ SLIDES LMNL ONLY IN MALES’ SLIDES UMNL
ONLY IN FEMALES’ SLIDES Causes of upper & lower motor neuron lesions Causes of upper & lower motor neurons lesions UMNL LMNL • • Cerebral stroke by haemorrhage (symptoms: depending on the site of injury, paralysis), thrombosis or embolism. The most common site is internal capsule. • Spinal lesion (transaction): tumor or trauma or hemosection (brown squared syndrome). 10 Anterior horn cell lesions (ex: poliomyelitis, motor neuron disease). • Why not posterior or lateral? Because posterior is sensory and lateral is autonomic. • Spinal root lesions or peripheral nerve lesion ( e. g. nerve injury by trauma or compressive lesion) (Trauma, neuropathy)
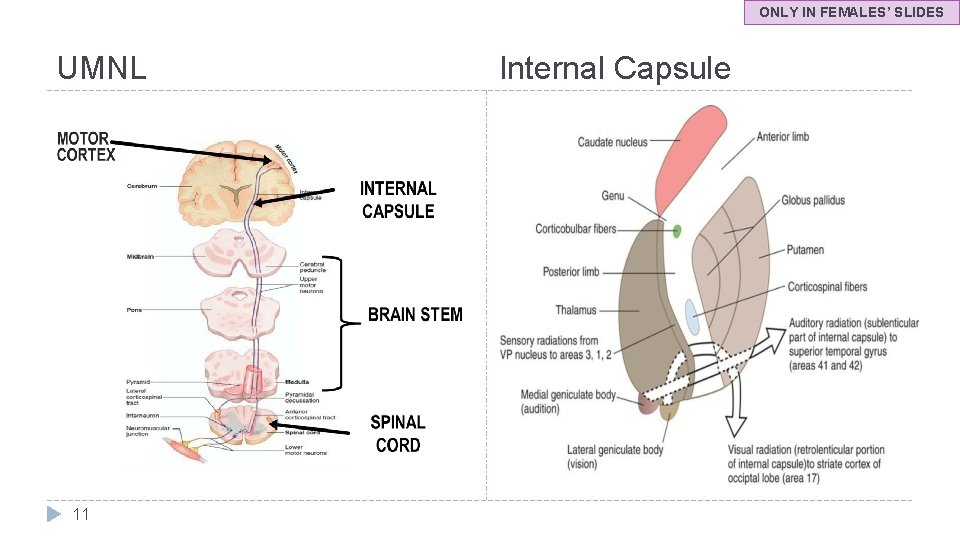
ONLY IN FEMALES’ SLIDES UMNL 11 Internal Capsule
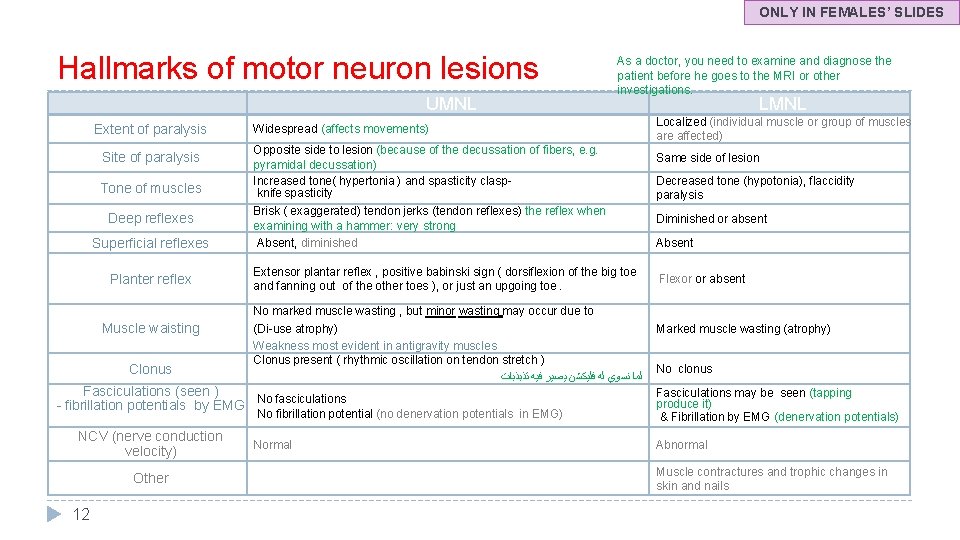
ONLY IN FEMALES’ SLIDES Hallmarks of motor neuron lesions UMNL Extent of paralysis Site of paralysis Tone of muscles Deep reflexes Superficial reflexes Planter reflex Muscle waisting Clonus Widespread (affects movements) Opposite side to lesion (because of the decussation of fibers, e. g. pyramidal decussation) Increased tone( hypertonia ) and spasticity claspknife spasticity Brisk ( exaggerated) tendon jerks (tendon reflexes) the reflex when examining with a hammer: very strong Absent, diminished Extensor plantar reflex , positive babinski sign ( dorsiflexion of the big toe and fanning out of the other toes ), or just an upgoing toe. No marked muscle wasting , but minor wasting may occur due to (Di-use atrophy) Weakness most evident in antigravity muscles Clonus present ( rhythmic oscillation on tendon stretch ) ﻟﻤﺎ ﻧﺴﻮﻱ ﻟﻪ ﻓﻠﻴﻜﺸﻦ ﻳﺼﻴﺮ ﻓﻴﻪ ﺗﺬﺑﺬﺑﺎﺕ Fasciculations (seen ) - fibrillation potentials by EMG No fasciculations No fibrillation potential (no denervation potentials in EMG) NCV (nerve conduction velocity) Other 12 As a doctor, you need to examine and diagnose the patient before he goes to the MRI or other investigations. Normal LMNL Localized (individual muscle or group of muscles are affected) Same side of lesion Decreased tone (hypotonia), flaccidity paralysis Diminished or absent Absent Flexor or absent Marked muscle wasting (atrophy) No clonus Fasciculations may be seen (tapping produce it) & Fibrillation by EMG (denervation potentials) Abnormal Muscle contractures and trophic changes in skin and nails
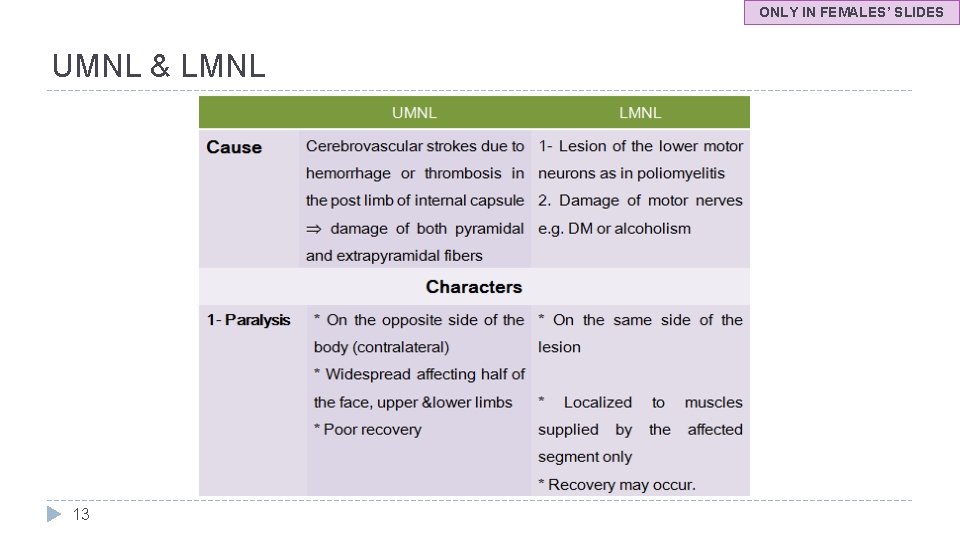
ONLY IN FEMALES’ SLIDES UMNL & LMNL 13
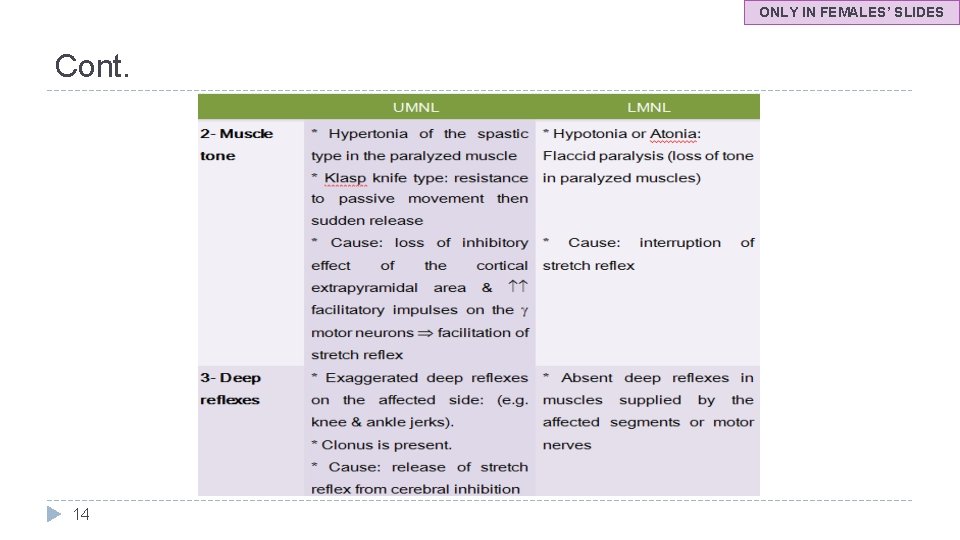
ONLY IN FEMALES’ SLIDES Cont. 14
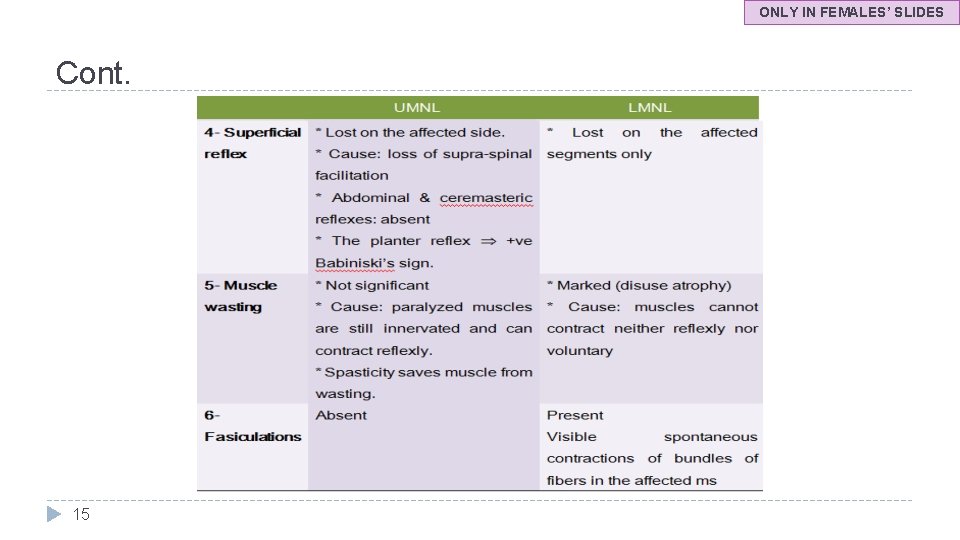
ONLY IN FEMALES’ SLIDES Cont. 15

Effect of a lesion in different parts of the motor system ONLY IN FEMALES’ SLIDES Lesions of pyramidal tract cause paralysis of the UMNL type below the level of the lesion. The side affected and the extent of paralysis vary according to the site of the lesion Side affected Area 4 Extent of paralysis Restricted paralysis (ex: Contralateral monoplegia, paralysis of one limb Because area 4 is widespread and is rarely damaged completely) Corona radiata This leads to contralateral monoplegia or hemiplegia, depending on the extent of the lesion. Internal capsule This often leads to contralateral hemiplegia because almost all fibers are injure Brain stem Contralateral hemiplegia & ipsilateral paralysis of the cranial nerves as follows: • Midbrain lesion: the III and IV • Pons lesion: V, VII and VIII. • Medulla lesion: IX, X, XI and XII Bilateral lesion in brain stem is rare and leads to quadriplegia and bilateral paralysis of the cranial nerves. 16

Extra Effects of a unilateral lesion in posterior limb of internal capsule • Such lesion is called cerebral stroke. • It is usually caused by thrombosis or haemorrhage of lenticulo- striate artery (a branch of the middle cerebral artery). • Patients pass into an acute then chronic stage. 1 - Acute stage lasts a few days up to 2 -3 weeks. It is characterized by acute UMNL manifestations in the opposite side: The main manifestations of this stage include: • Contralateral hemiplegia (paralysis of the opposite half of the body) of the UMNL type (partial recovery occurs after a variable period (possible walking), but the fine skilled movements are permanently lost). • Paralysis including the upper and lower limbs, the lower parts of the face and half of the tongue. • Hemianaethesia (loss of all sensations, due to damage of the thalamocortical fibers). • Permanent loss of fine sensations in the opposite side, but the crude sensations recover gradually. • Hypotonia and areflexia & loss of the superficial reflexes. • • Babinski's sign may be present. Contralateral homonymous hemianopia (loss of vision in the two corresponding haves of the visual fields opposite to side of lesion due to injury to optic radiation • Injury of left optic radiation causes blindness of the right halves of visual field • Diminished hearing power in both ears (by about 50 %), because of damage of auditory radiation. Manifestations of this stage are similar to those of LMNL, but the extent of paralysis is much more than that of LMNL. 17 2 - Chronic (permanent or spastic ) stage
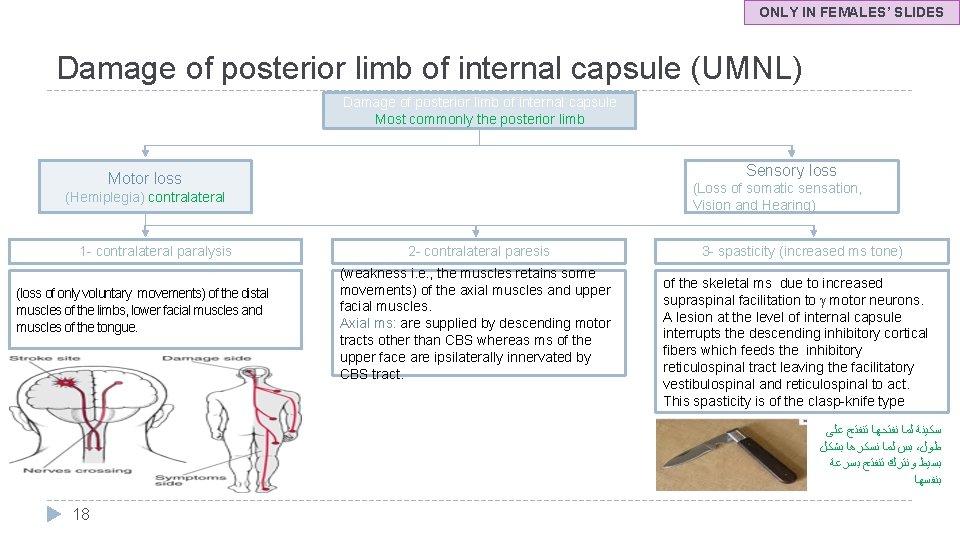
ONLY IN FEMALES’ SLIDES Damage of posterior limb of internal capsule (UMNL) Damage of posterior limb of internal capsule Most commonly the posterior limb Sensory loss Motor loss (Loss of somatic sensation, Vision and Hearing) (Hemiplegia) contralateral 1 - contralateral paralysis (loss of only voluntary movements) of the distal muscles of the limbs, lower facial muscles and muscles of the tongue. 2 - contralateral paresis (weakness i. e. , the muscles retains some movements) of the axial muscles and upper facial muscles. Axial ms: are supplied by descending motor tracts other than CBS whereas ms of the upper face are ipsilaterally innervated by CBS tract. 3 - spasticity (increased ms tone) of the skeletal ms due to increased supraspinal facilitation to motor neurons. A lesion at the level of internal capsule interrupts the descending inhibitory cortical fibers which feeds the inhibitory reticulospinal tract leaving the facilitatory vestibulospinal and reticulospinal to act. This spasticity is of the clasp-knife type ﺳﻜﻴﻨﺔ ﻟﻤﺎ ﻧﻔﺘﺤﻬﺎ ﺗﻨﻔﺘﺢ ﻋﻠﻰ ﺑﺲ ﻟﻤﺎ ﻧﺴﻜﺮﻫﺎ ﺑﺸﻜﻞ ، ﻃﻮﻝ ﺑﺴﻴﻂ ﻭﻧﺘﺮﻙ ﺗﻨﻔﺘﺢ ﺑﺴﺮﻋﺔ ﺑﻨﻔﺴﻬﺎ 18
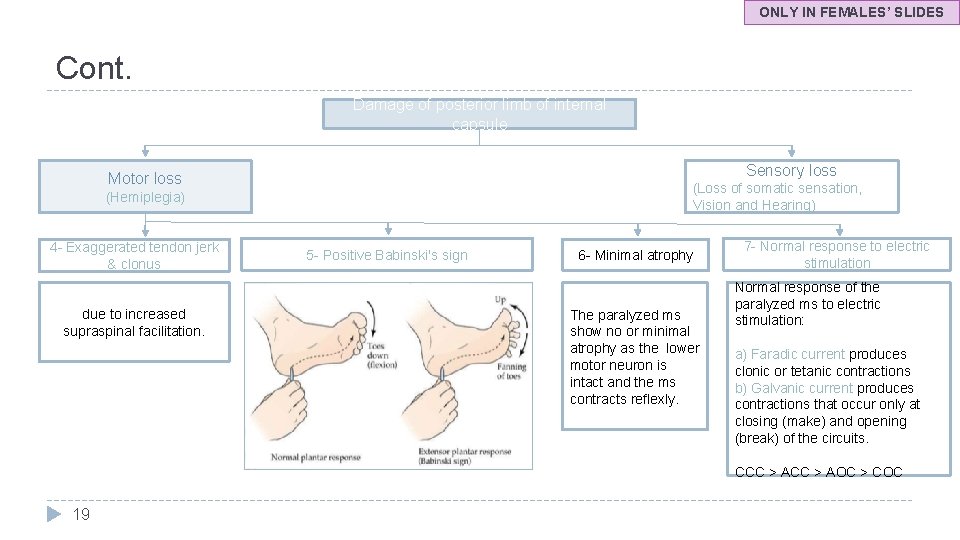
ONLY IN FEMALES’ SLIDES Cont. Damage of posterior limb of internal capsule Sensory loss Motor loss (Loss of somatic sensation, Vision and Hearing) (Hemiplegia) 4 - Exaggerated tendon jerk & clonus due to increased supraspinal facilitation. 5 - Positive Babinski's sign 6 - Minimal atrophy The paralyzed ms show no or minimal atrophy as the lower motor neuron is intact and the ms contracts reflexly. 7 - Normal response to electric stimulation Normal response of the paralyzed ms to electric stimulation: a) Faradic current produces clonic or tetanic contractions b) Galvanic current produces contractions that occur only at closing (make) and opening (break) of the circuits. CCC > AOC > COC 19
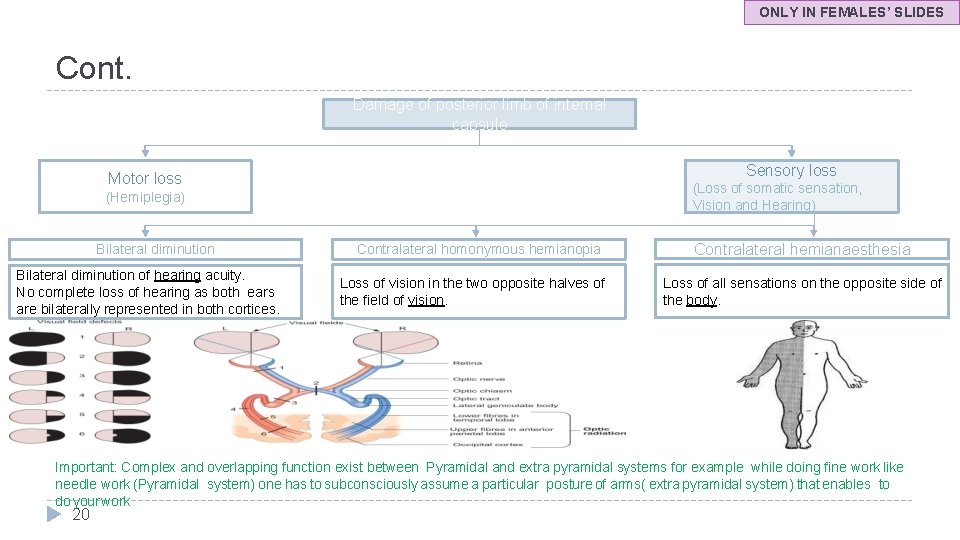
ONLY IN FEMALES’ SLIDES Cont. Damage of posterior limb of internal capsule Sensory loss Motor loss (Loss of somatic sensation, Vision and Hearing) (Hemiplegia) Bilateral diminution of hearing acuity. No complete loss of hearing as both ears are bilaterally represented in both cortices. Contralateral homonymous hemianopia Loss of vision in the two opposite halves of the field of vision. Contralateral hemianaesthesia Loss of all sensations on the opposite side of the body. Important: Complex and overlapping function exist between Pyramidal and extra pyramidal systems for example while doing fine work like needle work (Pyramidal system) one has to subconsciously assume a particular posture of arms( extra pyramidal system) that enables to do your work 20
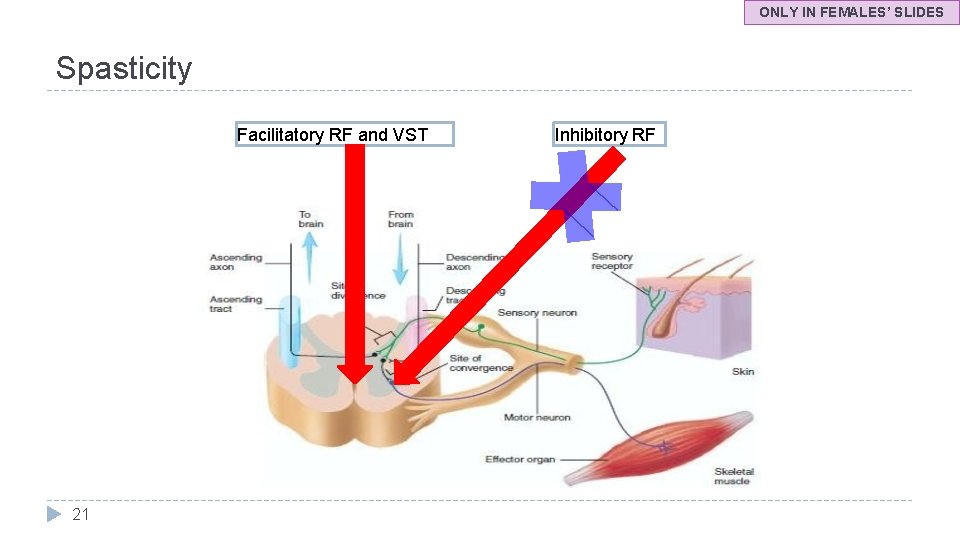
ONLY IN FEMALES’ SLIDES Spasticity Facilitatory RF and VST 21 Inhibitory RF
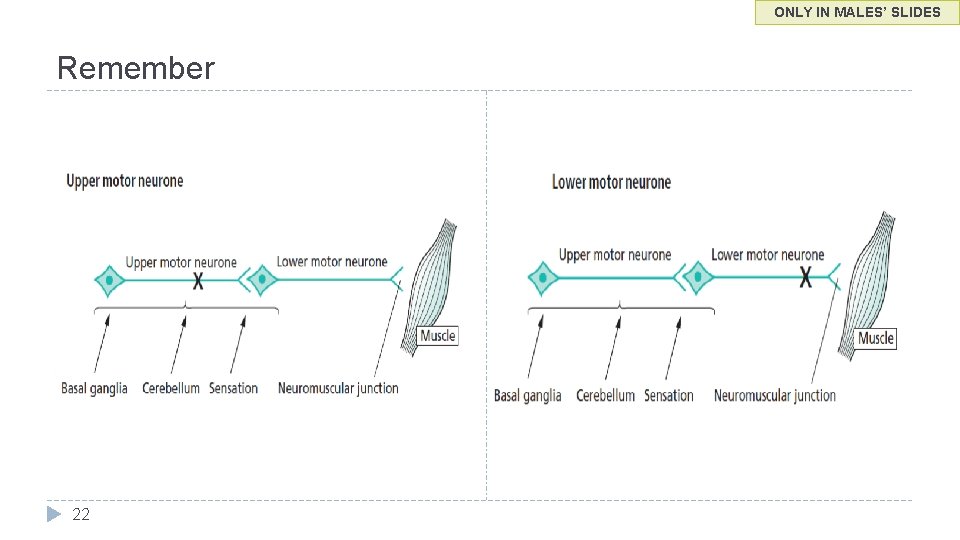
ONLY IN MALES’ SLIDES Remember 22
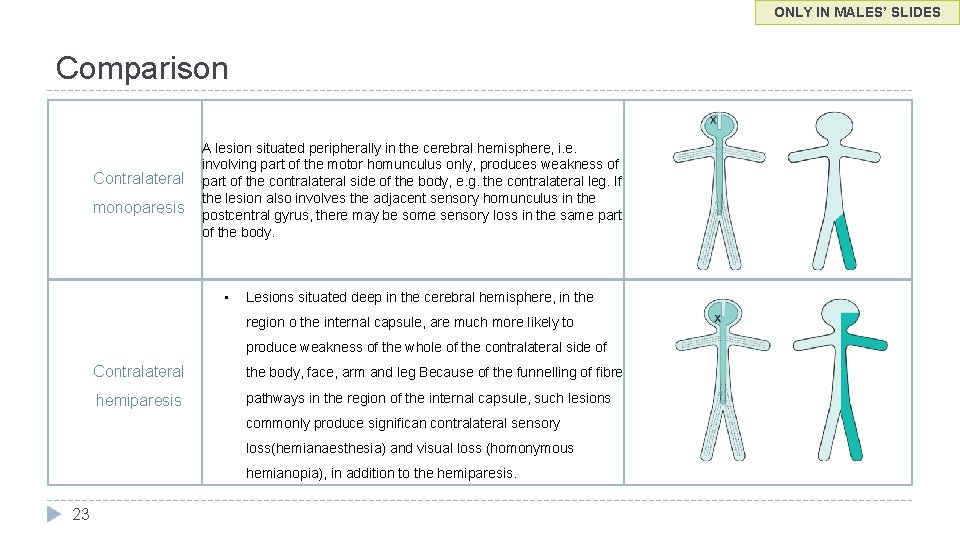

ONLY IN MALES’ SLIDES Comparison Contralateral monoparesis A lesion situated peripherally in the cerebral hemisphere, i. e. involving part of the motor homunculus only, produces weakness of part of the contralateral side of the body, e. g. the contralateral leg. If the lesion also involves the adjacent sensory homunculus in the postcentral gyrus, there may be some sensory loss in the same part of the body. • Lesions situated deep in the cerebral hemisphere, in the region o the internal capsule, are much more likely to produce weakness of the whole of the contralateral side of Contralateral the body, face, arm and leg Because of the funnelling of fibre hemiparesis pathways in the region of the internal capsule, such lesions commonly produce significan contralateral sensory loss(hemianaesthesia) and visual loss (homonymous hemianopia), in addition to the hemiparesis. 23
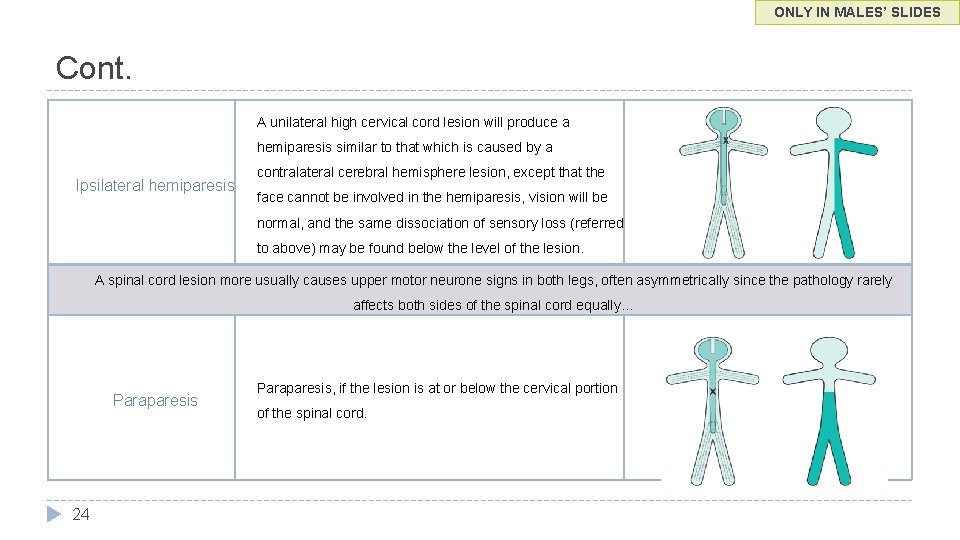
ONLY IN MALES’ SLIDES Cont. A unilateral high cervical cord lesion will produce a hemiparesis similar to that which is caused by a Ipsilateral hemiparesis contralateral cerebral hemisphere lesion, except that the face cannot be involved in the hemiparesis, vision will be normal, and the same dissociation of sensory loss (referred to above) may be found below the level of the lesion. A spinal cord lesion more usually causes upper motor neurone signs in both legs, often asymmetrically since the pathology rarely affects both sides of the spinal cord equally… Paraparesis 24 Paraparesis, if the lesion is at or below the cervical portion of the spinal cord.

ONLY IN MALES’ SLIDES Cont. A unilateral lesion in the spinal cord below the level of the neck produces upper motor neurone weakness in one leg. There Ipsilateral maybe posterior column (position sense) sensory loss in the monoparesis same leg, and spinothalamic (pain and temperature) sensory loss in the contralateral leg. This is known as dissociated sensory loss, and the whole picture is sometimes referred to as the Brown-Séquard syndrome. Tetraparesis or quadriparesis 25 Tetraparesis or quadriparesis, if the lesion is in the upper cervical cord or brainstem.
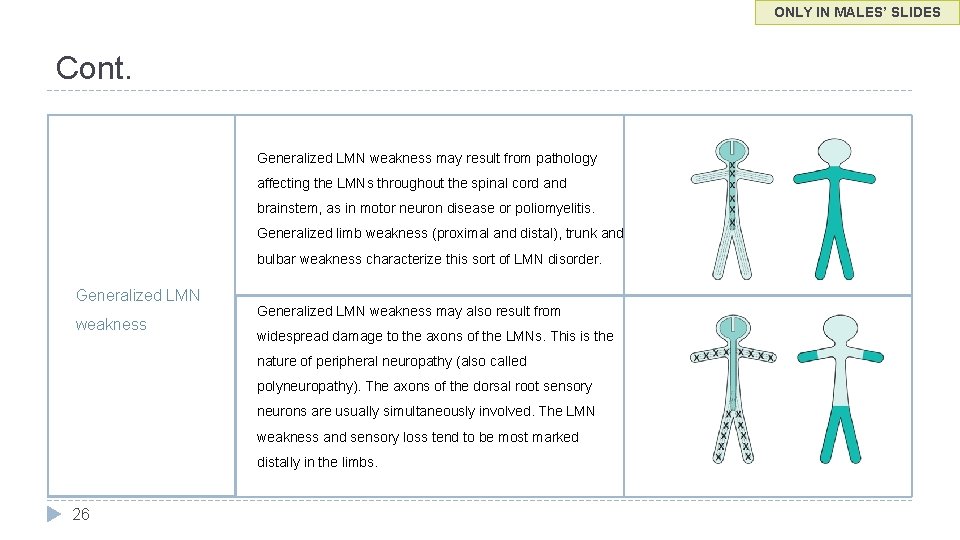

ONLY IN MALES’ SLIDES Cont. Generalized LMN weakness may result from pathology affecting the LMNs throughout the spinal cord and brainstem, as in motor neuron disease or poliomyelitis. Generalized limb weakness (proximal and distal), trunk and bulbar weakness characterize this sort of LMN disorder. Generalized LMN weakness may also result from widespread damage to the axons of the LMNs. This is the nature of peripheral neuropathy (also called polyneuropathy). The axons of the dorsal root sensory neurons are usually simultaneously involved. The LMN weakness and sensory loss tend to be most marked distally in the limbs. 26
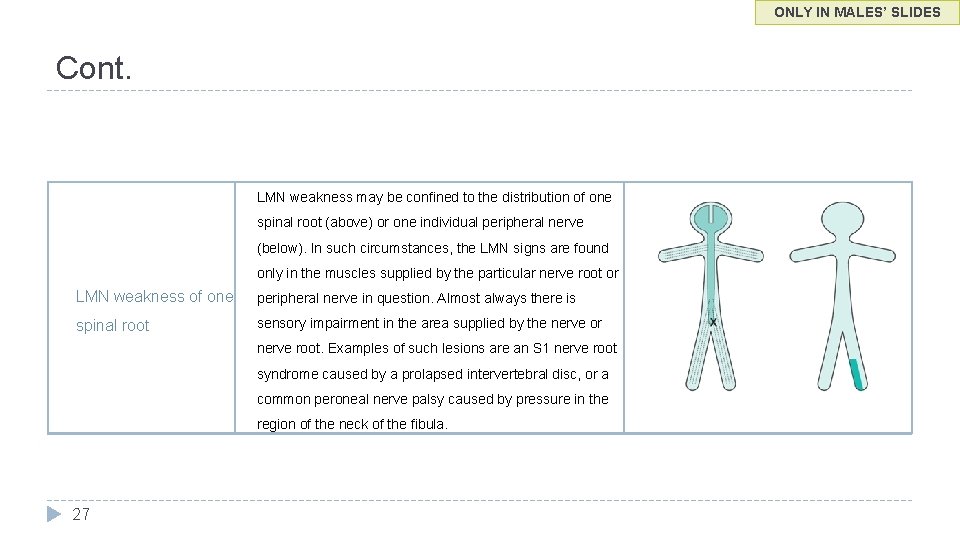
ONLY IN MALES’ SLIDES Cont. LMN weakness may be confined to the distribution of one spinal root (above) or one individual peripheral nerve (below). In such circumstances, the LMN signs are found only in the muscles supplied by the particular nerve root or LMN weakness of one peripheral nerve in question. Almost always there is spinal root sensory impairment in the area supplied by the nerve or nerve root. Examples of such lesions are an S 1 nerve root syndrome caused by a prolapsed intervertebral disc, or a common peroneal nerve palsy caused by pressure in the region of the neck of the fibula. 27
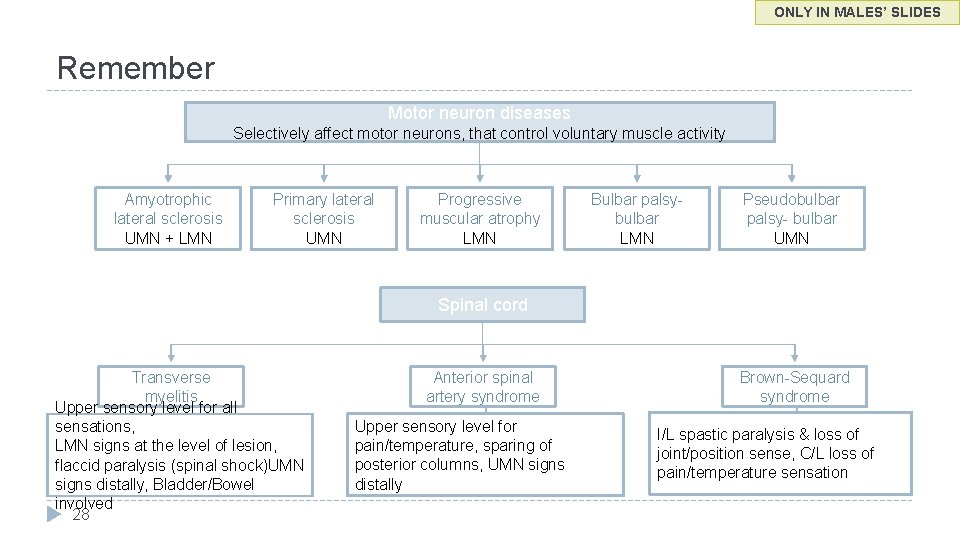
ONLY IN MALES’ SLIDES Remember Motor neuron diseases Selectively affect motor neurons, that control voluntary muscle activity Amyotrophic lateral sclerosis UMN + LMN Primary lateral sclerosis UMN Progressive muscular atrophy LMN Bulbar palsybulbar LMN Pseudobulbar palsy- bulbar UMN Spinal cord Transverse myelitis Upper sensory level for all sensations, LMN signs at the level of lesion, flaccid paralysis (spinal shock)UMN signs distally, Bladder/Bowel involved 28 Anterior spinal artery syndrome Upper sensory level for pain/temperature, sparing of posterior columns, UMN signs distally Brown-Sequard syndrome I/L spastic paralysis & loss of joint/position sense, C/L loss of pain/temperature sensation
ONLY IN FEMALES’ SLIDES Damage of lower motor neuron (LMNL) Structural changes • • In Nerve (degeneration and regeneration In muscle (atrophy and increase Ach receptors 29 Functional changes 1. 2. 3. 4. Flaccid paralysis Fasciculation and fibrillation Dennervation supersensitivity Reaction of degeneration

ONLY IN FEMALES’ SLIDES Cont. Functional changes � Flaccid paralysis: � � Paralysis of denervated ms with loss of all types of movements, "voluntary, postural and reflex". � All reflexes are lost including stretch reflex resulting in loss of � ms tone and tendon jerk (flaccidity). � � � Fibrillations: � As degeneration of the injured axon continues, the axon terminals are now separate from the main axon and hence, from each other. Injury potentials are still The extent of paralysis is usually limited to a small group of generated along the terminals leading to asynchronous contraction of the individual ms fibers attached to terminals. ms. � Invisible to the observer and detected only by EMG (Electromyogram). Fasiculations and fibrillations: � Appears few days or weeks after denervation. � Disappear when the motor nerve completely degenerates or successful re-innervation of the ms occurs. Fasiculations: � Synchronous visible contraction of the motor unit (all ms fibers) supplied by the injured axon. � Result from spontaneous generation of action potential 30 (injury potentials) in distal segment of the injured axon. � Denervation supersensitivity: � Denervated ms becomes supersensitive to acetylcholine. � This is due to increase in the number of A. Ch. receptors which cover the entire surface of ms cell membrane.
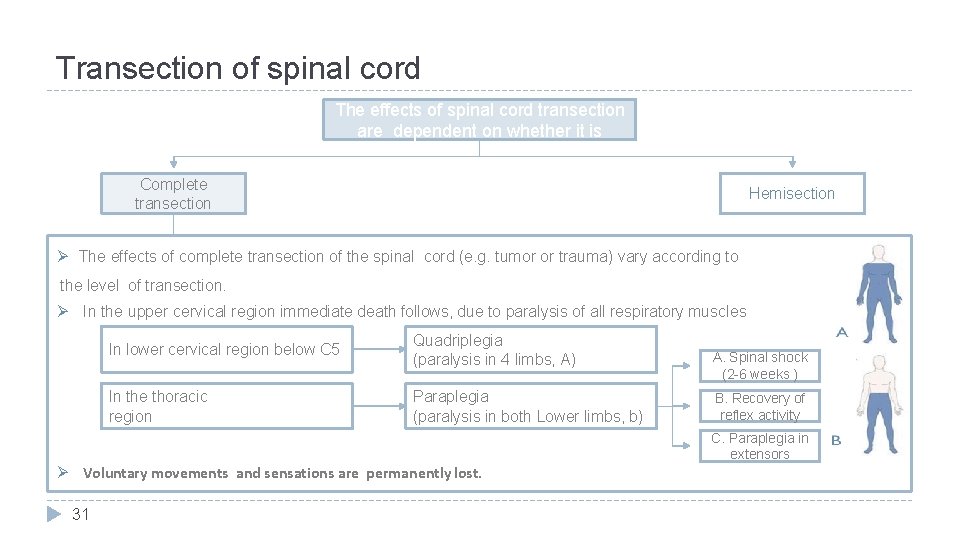
Transection of spinal cord The effects of spinal cord transection are dependent on whether it is Complete transection Hemisection The effects of complete transection of the spinal cord (e. g. tumor or trauma) vary according to the level of transection. In the upper cervical region immediate death follows, due to paralysis of all respiratory muscles In lower cervical region below C 5 Quadriplegia (paralysis in 4 limbs, A) In the thoracic region Paraplegia (paralysis in both Lower limbs, b) A. Spinal shock (2 -6 weeks ) B. Recovery of reflex activity C. Paraplegia in extensors Voluntary movements and sensations are permanently lost. 31
Extra Paraplegia Stages A. Spinal shock (2 -6 weeks ) B. Recovery of reflex activity C. Paraplegia in extensors loss of sensations accompanied by motor paralysis with initial loss but gradual recovery of reflexes Immediately following transection there is: • • • Paralysis of all muscles below the lesion. Loss of reflexes and loss of tone (flaccidity). Loss of all sensations (anaesthesia) and voluntary movements below the level of the lesion due to interruption of all sensory and motor tracts. Loss of muscle tone (flaccidity), and vasomotor tone (vasodilation) leading to fall in blood pressure. Bladder urinary retention with overflow due to paralysis of the wall of the urinary bladder. Cause of spinal shock: sudden withdrawal of supraspinal facilitation on the spinal alpha motor neurons i. e loss of continual tonic discharge transmitted along the excitatory pontine reticulospinal, vestibulospinal and corticospinal tracts. 32
Extra Cont. Paraplegia Stages A. Spinal shock (2 -6 weeks ) B. Recovery of reflex activity C. Paraplegia in extensors • • • As the spinal shock ends, spinal reflex activity returns. The partial recovery may be due: Increased excitability of the spinal cord neurons presumably to compensate for the loss of supraspinal facilitatory influences. Disinhibition of motor neurons as a result of absence of inhibitory impulses from higher motor centers. Hypersensitivity to excitatory neurotransmitters. • • • Features of this stage: Gradual rise of arterial blood pressure due to return of spinal vasomotor activity in the lateral horn cells. Exaggerated tendon reflexes and spasticity. Return of visceral reflexes (micturition & defecation). Mass reflex: a minor painful stimulus to the skin of the lower limbs causes: • o Withdrawal and evoke other autonomic reflexes (bladder and rectum emptying, sweating , blood pressure rise through spread of excitation (by irradiation) • Voluntary movements and sensations are permanently lost • Human patients with complete transection never recover fully because effective regeneration never occurs in the human`s CNS. 33
Extra Cont. Paraplegia Stages A. Spinal shock (2 -6 weeks ) B. Recovery of reflex activity C. Paraplegia in extensors The tone in extensor muscles returns gradually to exceed that in the flexors. The lower limbs become spastically extended. Extensor reflexes become exaggerated, as shown by tendon jerks and by the appearance of clonus. The positive supportive reaction returns and the patient can stand on his feet with appropriate support. Return of the withdrawal reflex and crossed extensor reflex. 34
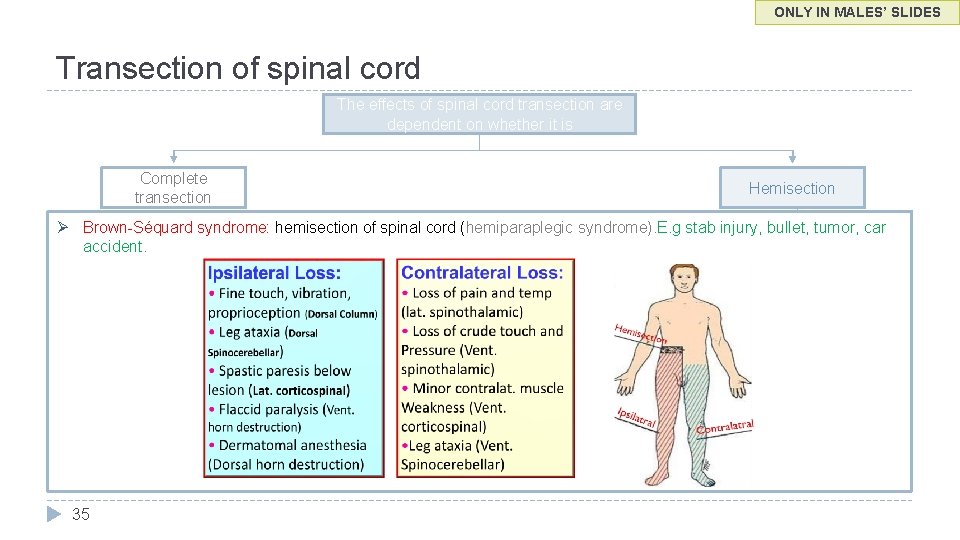
ONLY IN MALES’ SLIDES Transection of spinal cord The effects of spinal cord transection are dependent on whether it is Complete transection Hemisection Brown-Séquard syndrome: hemisection of spinal cord (hemiparaplegic syndrome). E. g stab injury, bullet, tumor, car accident. 35
ONLY IN MALES’ SLIDES Cont. � Ipsilateral lower motor neuron paralysis in the segment of the lesion and muscular atrophy. These signs are caused by damage to the neurons on the anterior gray column and possibly by damage to the nerve roots of the same segment. � Ipsilateral loss of tactile discrimination and of vibratory and proprioceptive sensations below the level of the lesion. These signs are caused b destruction of the ascending tracts in the posterior white column on the same side of the lesion. � Ipsilateral spastic paralysis below the level of the lesion. � Contralateral loss of pain and temperature sensations below the level of the lesion. This is due to destruction of the crossed lateral spinothalamic tracts on the same side of the lesion. � � � An ipsilateral Babinski sign is present, and depending on the segment of the cord damaged, an ipsilateral loss of the superficial abdominal reflexes and cremasteric reflex occurs. All these signs are due to loss of the corticospinal tracts on the side of the lesion. Spastic paralysis is produced by interruption of the descending tracts other than the corticospinal tracts. Ipsilateral band of cutaneous anesthesia in the segment of the lesion. This results from the destruction of the posterior root and its entrance into the spinal cord at the level of the lesion. 36 � � Because the tracts cross obliquely, the sensory loss occurs two or three segments below the lesion distally. Contralateral but not complete loss of tactile sensation below the level of the lesion. This condition is brought about by destruction of the crossed anterior spinothalamic tracts on the side of the lesion. Here, again, because the tracts cross obliquely, the sensory impairment occurs two or three segments below the level of the lesion distally. The contralateral loss of tactile sense is incomplete because discriminative touch traveling in the ascending tracts in the contralateral posterior white column remains intact.
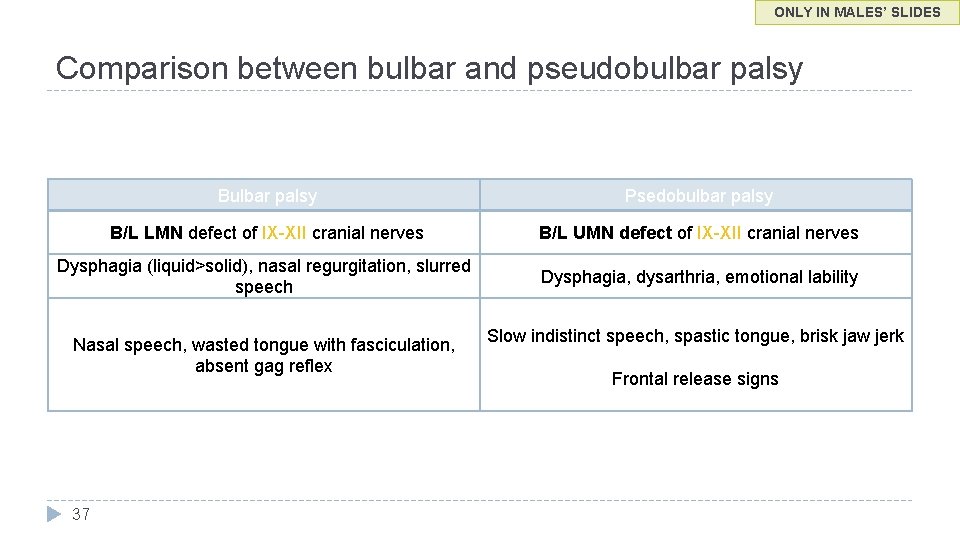
ONLY IN MALES’ SLIDES Comparison between bulbar and pseudobulbar palsy Bulbar palsy Psedobulbar palsy B/L LMN defect of IX-XII cranial nerves B/L UMN defect of IX-XII cranial nerves Dysphagia (liquid>solid), nasal regurgitation, slurred speech Dysphagia, dysarthria, emotional lability Nasal speech, wasted tongue with fasciculation, absent gag reflex 37 Slow indistinct speech, spastic tongue, brisk jaw jerk Frontal release signs
ONLY IN MALES’ SLIDES Cauda equina and conus medullaris lesions Conus medullaris cauda equina B/L saddle anaesthesia asymmetric leg weakness and sensory loss Prominent bowel, bladder symptoms, impotence Relative sparing of bowelbladder function Bulbocavernous ( S 2 -s 4) and anal reflexes (s 4 -s 5) are absent Variable areflexia in lower extremities Muscle strength largely preserved Low back and radicular pain 38
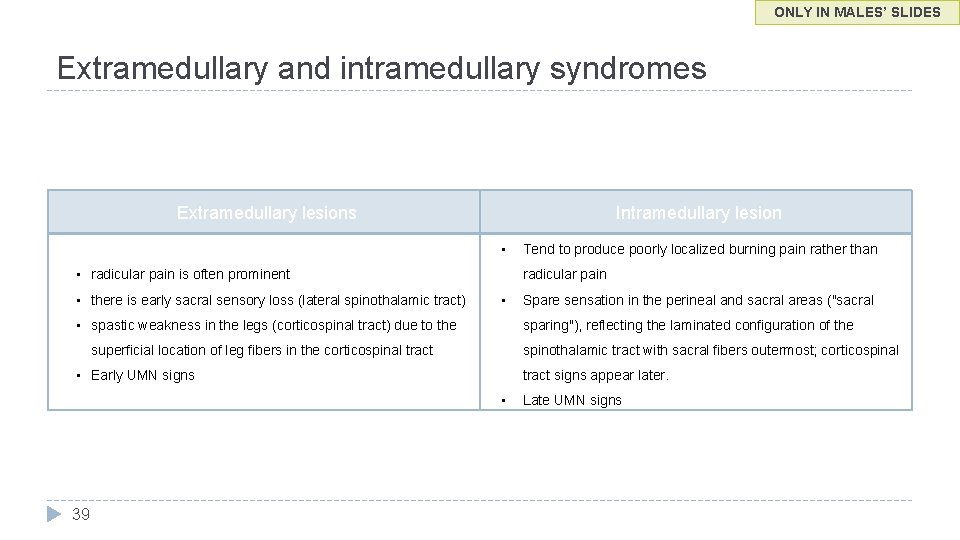

ONLY IN MALES’ SLIDES Extramedullary and intramedullary syndromes Extramedullary lesions Intramedullary lesion • • radicular pain is often prominent • there is early sacral sensory loss (lateral spinothalamic tract) radicular pain • • spastic weakness in the legs (corticospinal tract) due to the Spare sensation in the perineal and sacral areas ("sacral sparing"), reflecting the laminated configuration of the spinothalamic tract with sacral fibers outermost; corticospinal superficial location of leg fibers in the corticospinal tract • Early UMN signs tract signs appear later. • 39 Tend to produce poorly localized burning pain rather than Late UMN signs
Thank you!. ﺍﻋﻤﻞ ﻭ ﺃﻨﺖ ﺗﻌﻠﻢ ﺃﻦ ﺍﻟﻠﻪ ﻻ ﻳﻀﻴﻊ ﺃﺠﺮ ﻣﻦ ﺃﺤﺴﻦ ﻋﻤﻼ ، ﺍﻋﻤﻞ ﻟﺘﻤﺴﺢ ﺩﻣﻌﺔ ، ﺍﻋﻤﻞ ﻟﺘﺮﺳﻢ ﺑﺴﻤﺔ The Physiology 436 Team: Females Members: Basel Almeflh Amira Niazy Rana Barasain Dania Alkelabi Heba Alnasser References: Amal Alshaibi • • Females’ and Males’ slides. Guyton and Hall Textbook of Medical Physiology (Thirteenth Edition. ) 40 Team Leaders: Lulwah Alshiha Laila Mathkour Mohammad Alayed Contact us:
- Slides: 40