TESTICULAR CANCER NUR BKE ABUK MGE GLER VIOLA

TESTICULAR CANCER NUR BÜKE ÇABUK MÜGE GÜLER VIOLA RIGOTTI
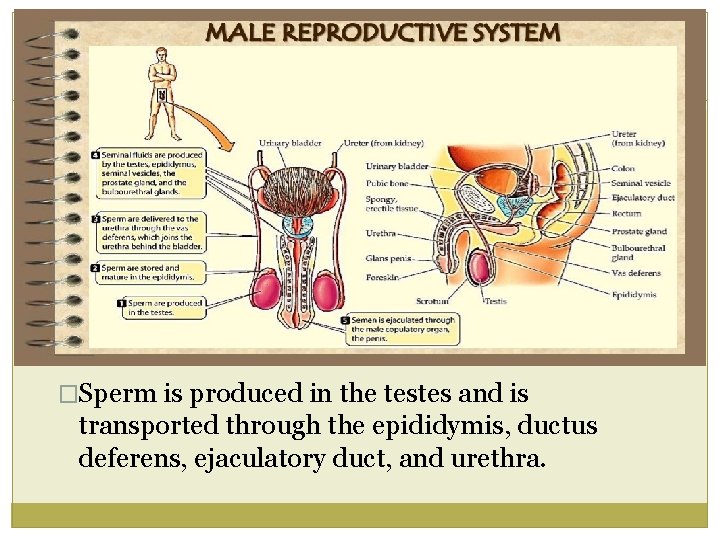
�Sperm is produced in the testes and is transported through the epididymis, ductus deferens, ejaculatory duct, and urethra.
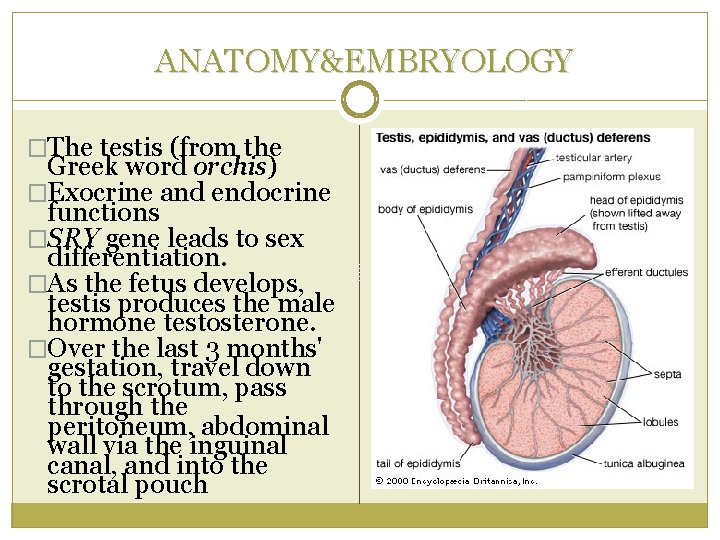
ANATOMY&EMBRYOLOGY �The testis (from the Greek word orchis) �Exocrine and endocrine functions �SRY gene leads to sex differentiation. �As the fetus develops, testis produces the male hormone testosterone. �Over the last 3 months' gestation, travel down to the scrotum, pass through the peritoneum, abdominal wall via the inguinal canal, and into the scrotal pouch
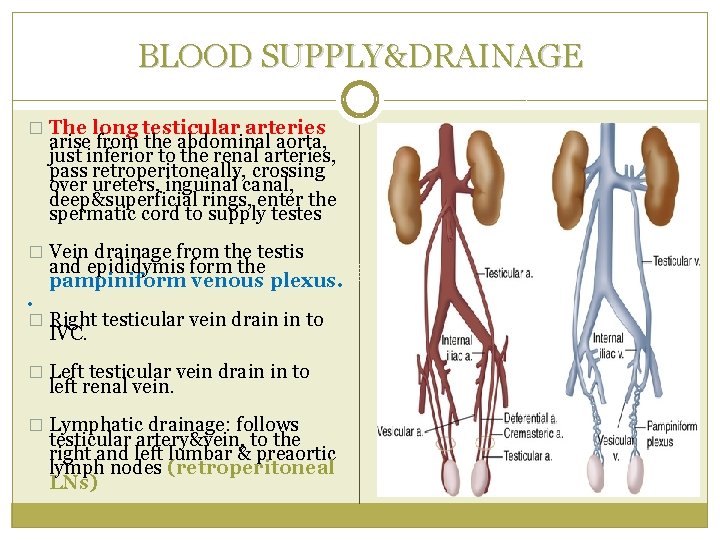
BLOOD SUPPLY&DRAINAGE � The long testicular arteries arise from the abdominal aorta, just inferior to the renal arteries, pass retroperitoneally, crossing over ureters, inguinal canal, deep&superficial rings, enter the spermatic cord to supply testes � Vein drainage from the testis . and epididymis form the pampiniform venous plexus. � Right testicular vein drain in to IVC. � Left testicular vein drain in to left renal vein. � Lymphatic drainage: follows testicular artery&vein, to the right and left lumbar & preaortic lymph nodes (retroperitoneal LNs)
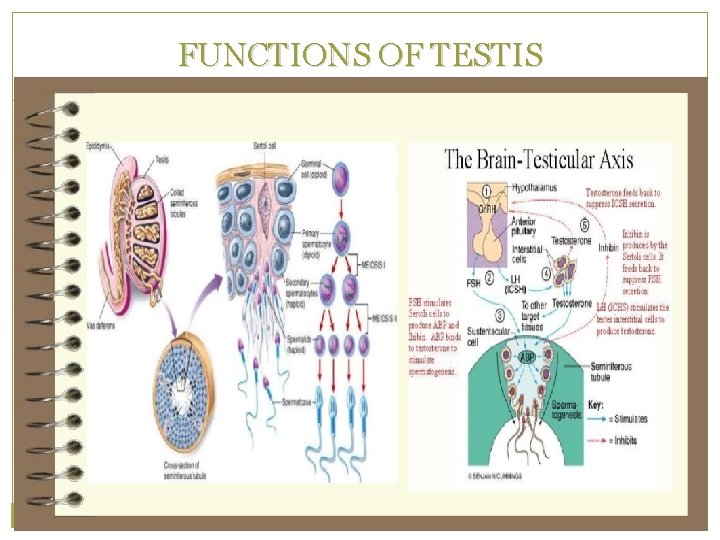
FUNCTIONS OF TESTIS
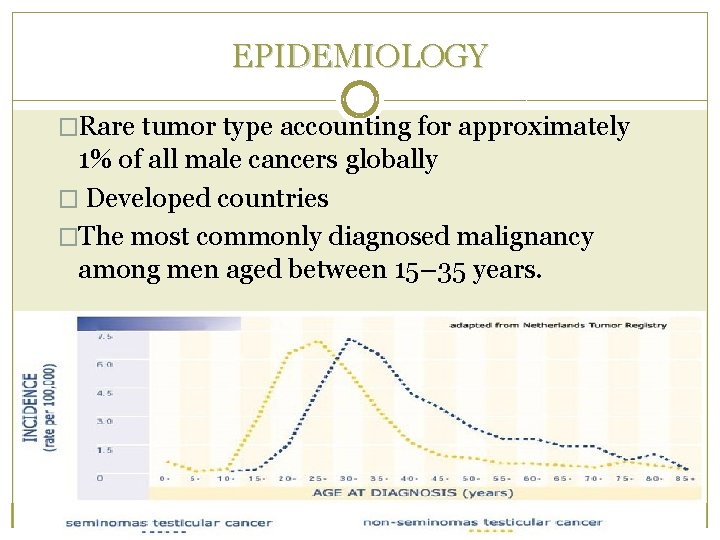
EPIDEMIOLOGY �Rare tumor type accounting for approximately 1% of all male cancers globally � Developed countries �The most commonly diagnosed malignancy among men aged between 15– 35 years.
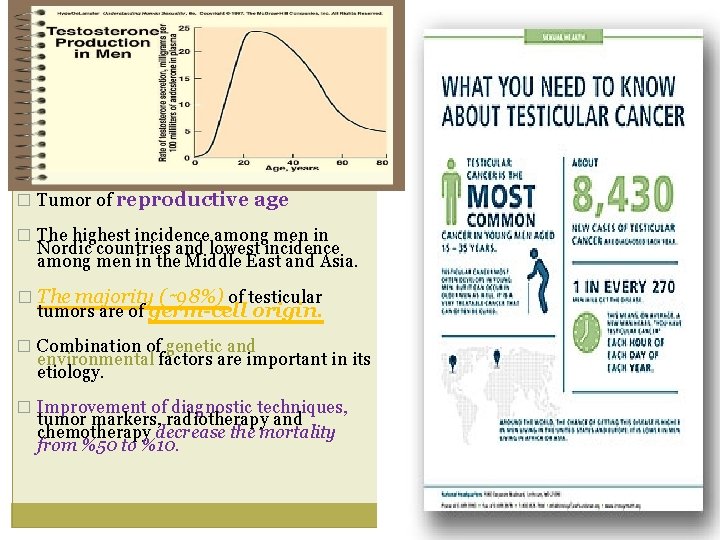
� Tumor of reproductive age � The highest incidence among men in Nordic countries and lowest incidence among men in the Middle East and Asia. � The majority (∼ 98%) of testicular tumors are of germ-cell origin. � Combination of genetic and environmental factors are important in its etiology. � Improvement of diagnostic techniques, tumor markers, radiotherapy and chemotherapy decrease the mortality from %50 to %10.

RISK FACTORS �An undescended testicle �Family history of testicular cancer �HIV infection �Carcinoma in situ of the testicle �Having had testicular cancer before �Being of a certain race/ethnicity �Body size �High estrogen levels in utero
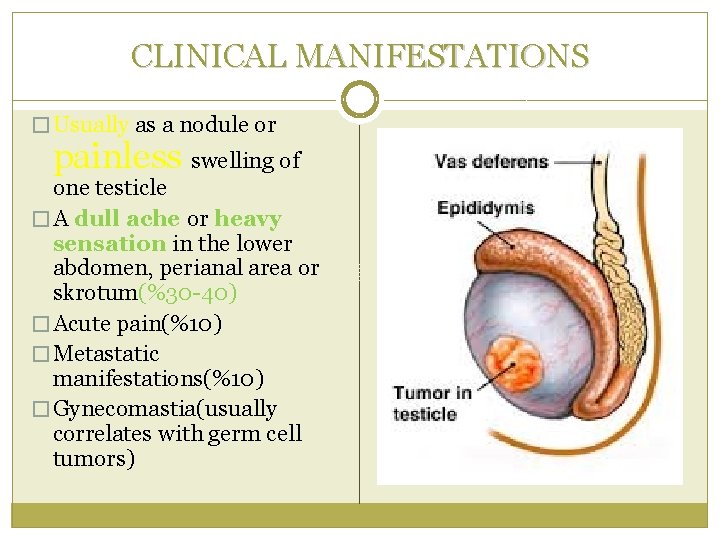
CLINICAL MANIFESTATIONS � Usually as a nodule or painless swelling of one testicle � A dull ache or heavy sensation in the lower abdomen, perianal area or skrotum(%30 -40) � Acute pain(%10) � Metastatic manifestations(%10) � Gynecomastia(usually correlates with germ cell tumors)
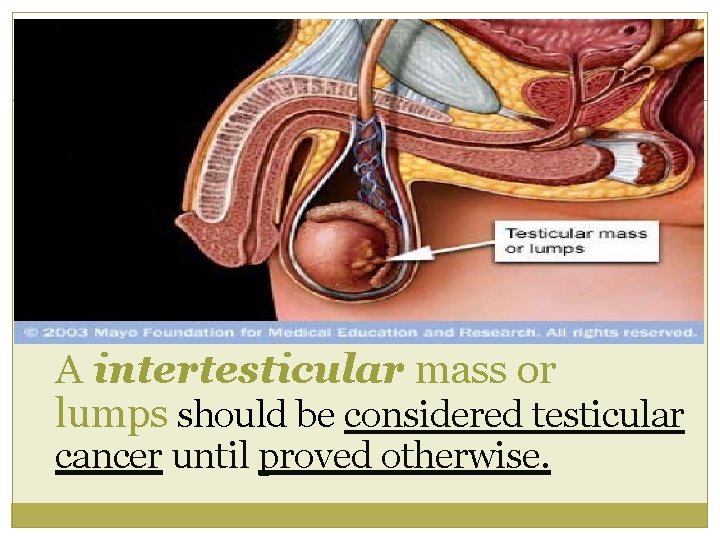
A intertesticular mass or lumps should be considered testicular cancer until proved otherwise.
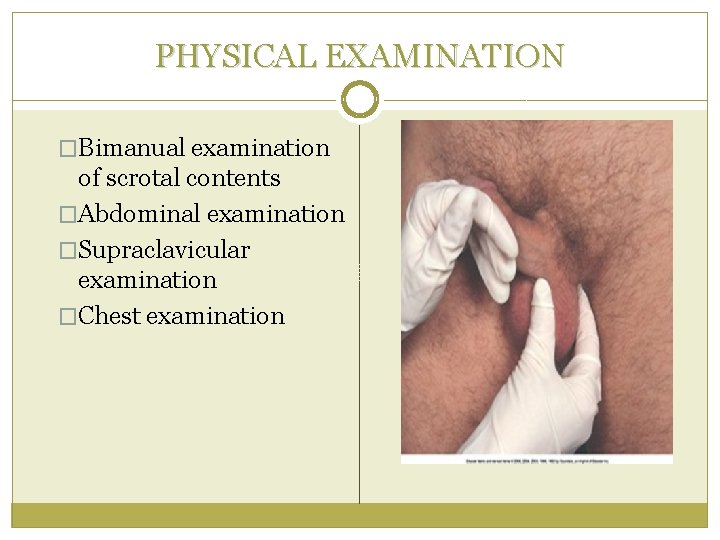
PHYSICAL EXAMINATION �Bimanual examination of scrotal contents �Abdominal examination �Supraclavicular examination �Chest examination
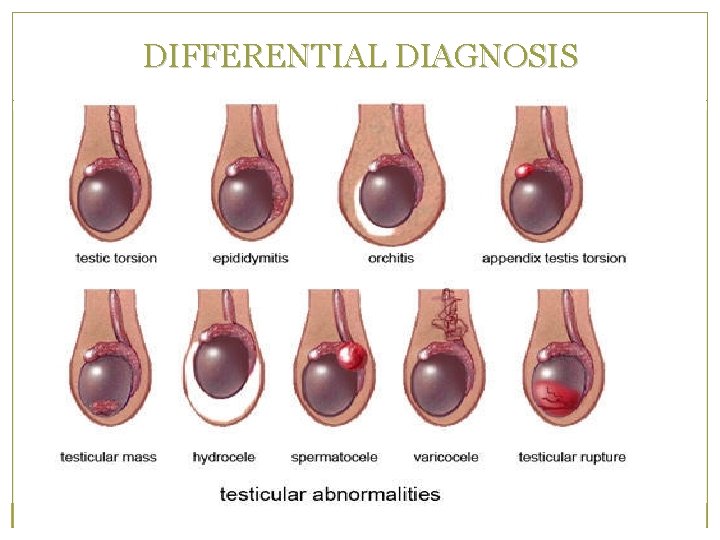
DIFFERENTIAL DIAGNOSIS

DIAGNOSTIC EVAULATION �Scrotal USG �Serum tumor markers �Radical inguinal orchiectomy �CT �MRI �PET �Contralateral testicular biopsy �Retroperitoneal lymph node dissection

SERUM TUMOR MARKERS 1. Alpha Feta Protein Produced by yolk sac 2. Beta h. CG Produced by placenta 3. Lactate dehydragenase General tumor marker
DIAGNOSIS Scrotal USG Serum Tumor Markers Radical inguinal orchiectomy Radiological imaging
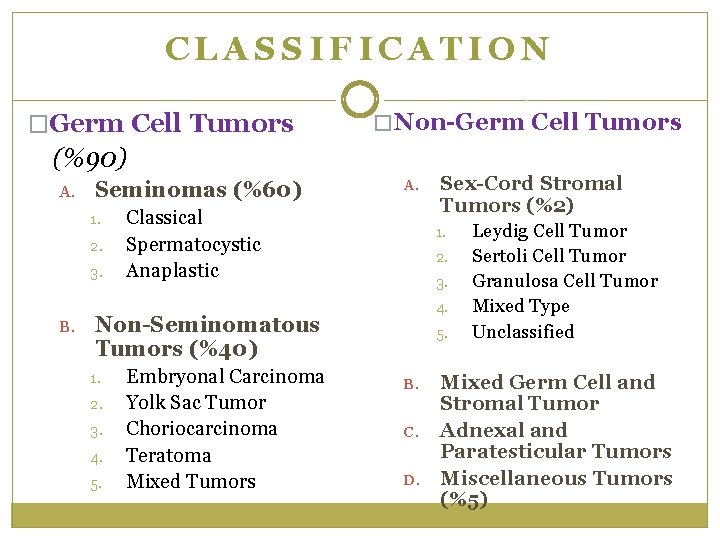
CLASSIFICATION �Germ Cell Tumors � Non-Germ Cell Tumors (%90) A. Seminomas (%60) 1. 2. 3. B. A. Classical Spermatocystic Anaplastic 1. 2. 3. 4. Non-Seminomatous Tumors (%40) 1. 2. 3. 4. 5. Embryonal Carcinoma Yolk Sac Tumor Choriocarcinoma Teratoma Mixed Tumors Sex-Cord Stromal Tumors (%2) 5. B. C. D. Leydig Cell Tumor Sertoli Cell Tumor Granulosa Cell Tumor Mixed Type Unclassified Mixed Germ Cell and Stromal Tumor Adnexal and Paratesticular Tumors Miscellaneous Tumors (%5)

GERM CELL TUMORS �Seminomas v Classical The most common histologic type (%85) v Anaplastic Increased mitotic figures, aggressive v Spermatocystic A rare variant that occurs in older adults (%50 >50 years of age)

GERM CELL TUMORS �Non-Seminomatous Tumors v Embryonal Carcinoma 2/3 metastases at diagnosis Normal range of AFP v Yolk Sac Tumor The most common testicular tumor in children <3 years Increased AFP Schiller-Duval bodies on histology -> PATHOGNOMONIC
GERM CELL TUMORS v Choriocarcinoma Pure choriocarcinoma of the testis is the most aggresive variant of germ cell tumors ->Early hematogenous spread to the lungs Increased beta-h. CG v Teratoma Congenital, rarely diagnosed >4 years of age The second most common germ cell tumor after yolk sac tumors Normal tumor marker values v Mixed Tumors Teratocarcinoma

SEX-CORD STROMAL TUMORS • Leydig Cell Tumor Increased estrogen production resulting in gynecomastia in 1/3 • Sertoli Cell Tumor Increased androgen production resulting in precoccious puberty • Granulosa Cell Tumor • Mixed Type Tumor • Undifferentiated

MANAGEMENT �Diagnosis is established at radical orchiectomy (also the first line of treatment) �Subsequent therapy depends upon: - Histology (seminomas vs NSGCTs) - Presence or absence of more extensive disease - Other risk factors

TNM STAGING American Joint Committee on Cancer (AJCC) T the extent of spread of the primary tumor to the tissues next to the testicle N number of lymph nodes affected M metastasis +/S indicates the serum level of tumor markers (specific for certain types of testicular cancers)
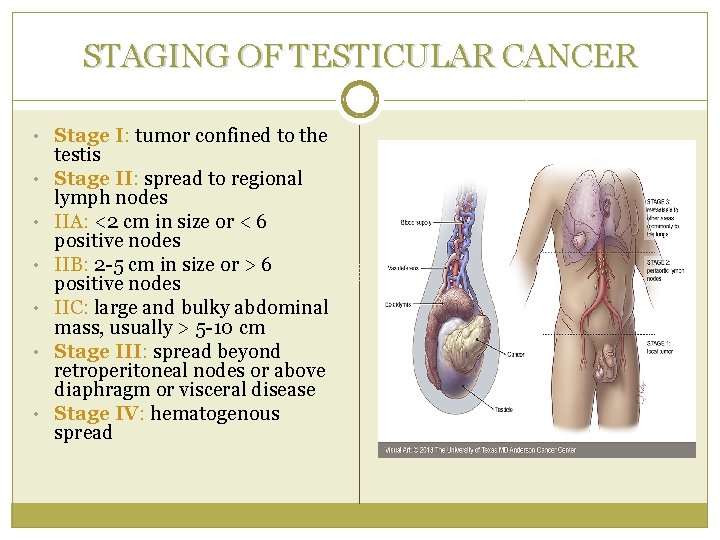
STAGING OF TESTICULAR CANCER • Stage I: tumor confined to the • • • testis Stage II: spread to regional lymph nodes IIA: <2 cm in size or < 6 positive nodes IIB: 2 -5 cm in size or > 6 positive nodes IIC: large and bulky abdominal mass, usually > 5 -10 cm Stage III: spread beyond retroperitoneal nodes or above diaphragm or visceral disease Stage IV: hematogenous spread

FERTİLİTY AND SPERM BANKING - Baseline sperm count and sperm banking prior to diagnosis and staging - Semen cryopreservation
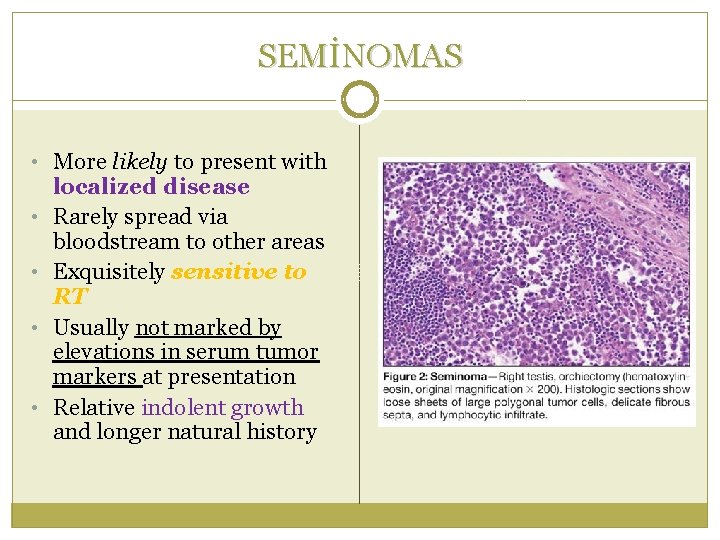
SEMİNOMAS • More likely to present with • • localized disease Rarely spread via bloodstream to other areas Exquisitely sensitive to RT Usually not marked by elevations in serum tumor markers at presentation Relative indolent growth and longer natural history
TREATMENT OF SEMINOMAS Low grade (stage I and IIA) Radical inguinal orchiectomy Surveillance RT or single agent carboplatin High grade (stage >IIA) Radical inguinal orchiectomy RPLND RT and/or CT
NON-SEMINOMATOUS GERM CELL TUMOR �Management of men with NSGCT stage I depends on the presence of factors that present an increased risk of relapse: - Lymphovascular invasion - Predominance of an embryonal carcinoma component - A T 3 or T 4 primary tumor
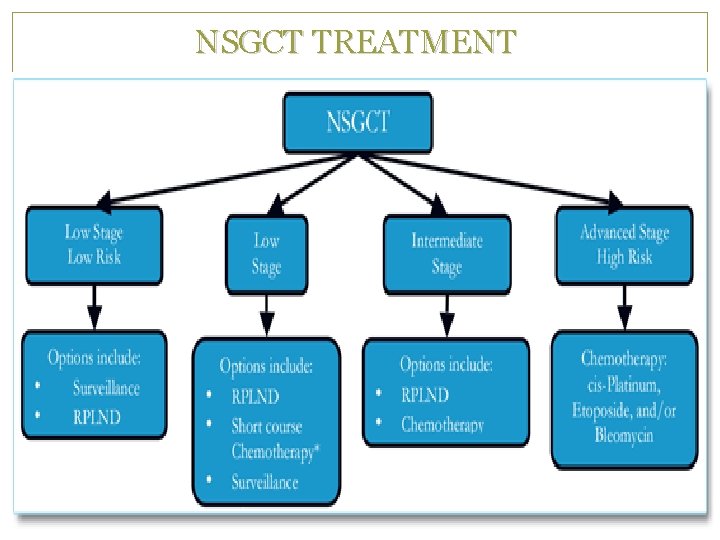
NSGCT TREATMENT
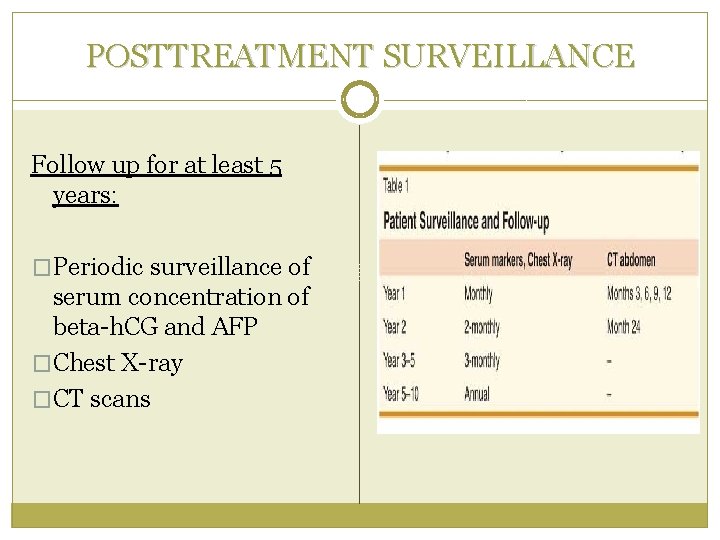
POSTTREATMENT SURVEILLANCE Follow up for at least 5 years: �Periodic surveillance of serum concentration of beta-h. CG and AFP �Chest X-ray �CT scans

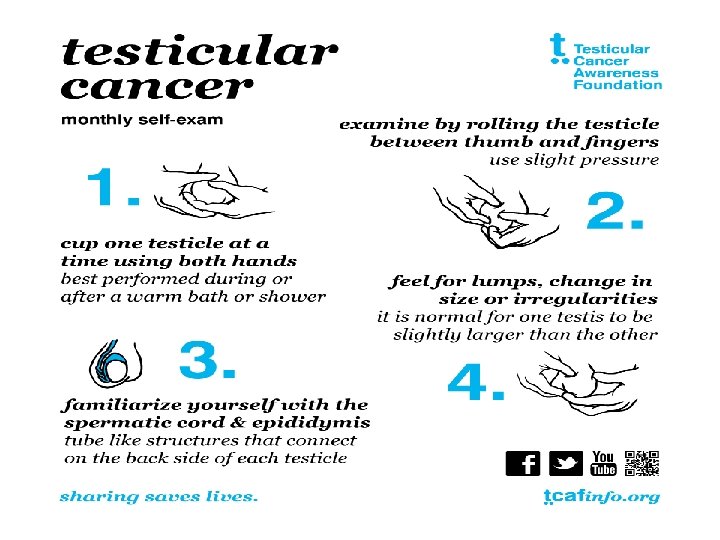
RISK OF RELAPS OR SECONDARY TUMOR Importance of regular testicular self examinations

PROGNOSIS �Testicular cancers are curable even in the presence of metastatic disease. � 5 year survival rate: Localized stage: 99% Regional stage: 96% Distant: 72%

REFERANCES �www. uptodate. com �www. medscape. com �www. cancer. org TEŞEKKÜRLER…
- Slides: 34