Temperature Control in the Neonate Learning objectives Thermoneutral

Temperature Control in the Neonate

Learning objectives Thermoneutral temperature Mechanisms of heat loss Degrees of hypothermia Management Prevention

INTRODUCTION Newborn baby is a homoeothermic, but his ability to stay warm may easily be overwhelmed by extremes of environmental temperatures

Thermoregulation is the capacity to maintain equilibrium between heat production and heat loss in order to sustain body temperature within a normal range An environmental temperature at which the infant uses minimal oxygen and expends the least energy and thrives well is defined as a neutral thermal environment.

Importance of temperature regulation Warmth is one of the basic needs of a newborn baby Others basic needs are Normal breathing Mother’s milk Protection from infection It is critical to the baby’s survival and well being. Unlike adults, newborn babies are often not able to keep themselves warm.

Why newborns are at risk?

Why newborn are susceptible? 1. Large surface area of babies as compare to their weight. 2. Limited heat generation mechanism. 3. Vulnerebility to getting exposed.

Additional contributory factor in LBW babies 1. Decreased subcutaneous fat and brown fat. 2. More permeable skin. 3. Larger surface area than term babies. 4. Poor homeostatic response to hypothermia.
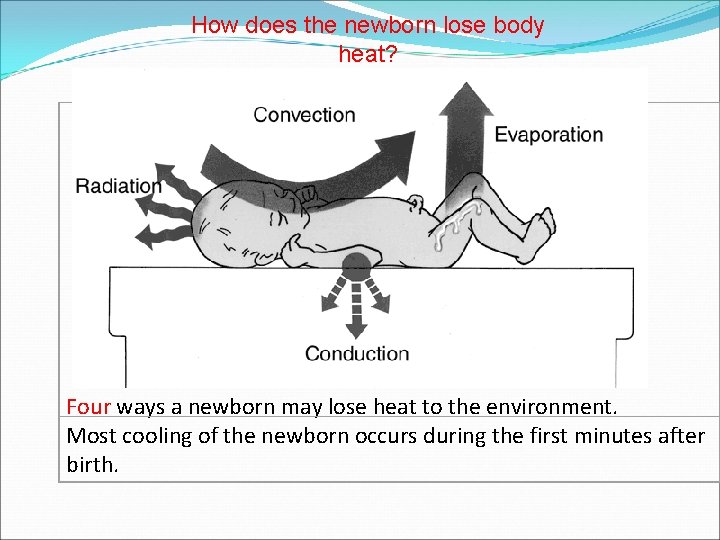
How does the newborn lose body heat? Four ways a newborn may lose heat to the environment. Most cooling of the newborn occurs during the first minutes after birth.

Temperature regulation

Temperature regulation Shivering thermogenesis Non shivering thermogenesis

Heat gain: Non-shivering thermogenesis • Heat is produced by increasing the metabolism especially in brown adipose tissue • Blood is warmed as it passes through the brown fat and it in turn warms the body
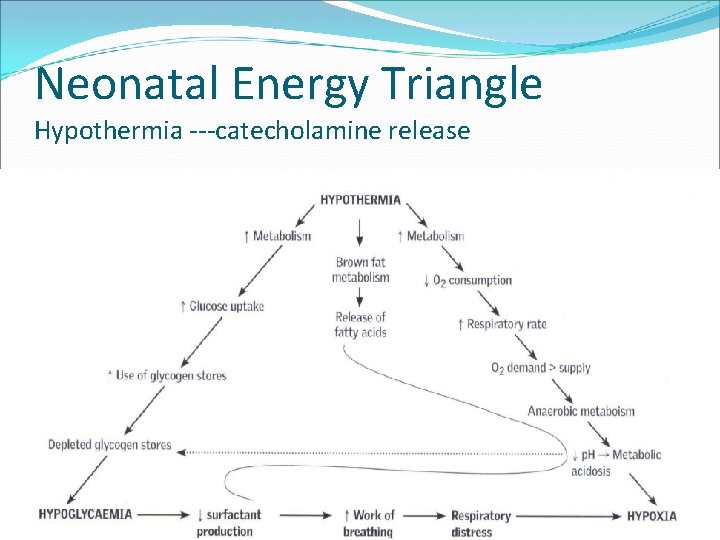
Neonatal Energy Triangle Hypothermia ---catecholamine release

Grades of hypothermia. WHO Classifications of core body temperature for newborns: Normal = 36. 5 - 37. 4 C Mild Hypothermia or Cold Stress = 36 - 36. 4 C – cause for concern Moderate Hypothermia = 32 - 35. 9 C – danger, warm baby Severe Hypothermia = < 32 C – outlook grave, skilled care urgently needed.

Definition & degrees of hypothermia Normal range Cold stress 37. 5 o 36. 5 o Cause for concern 36. 0 Moderate hypothermia o Severe hypothermia 32. 0 o Danger, warm baby Outlook grave, skilled care urgently needed - 15
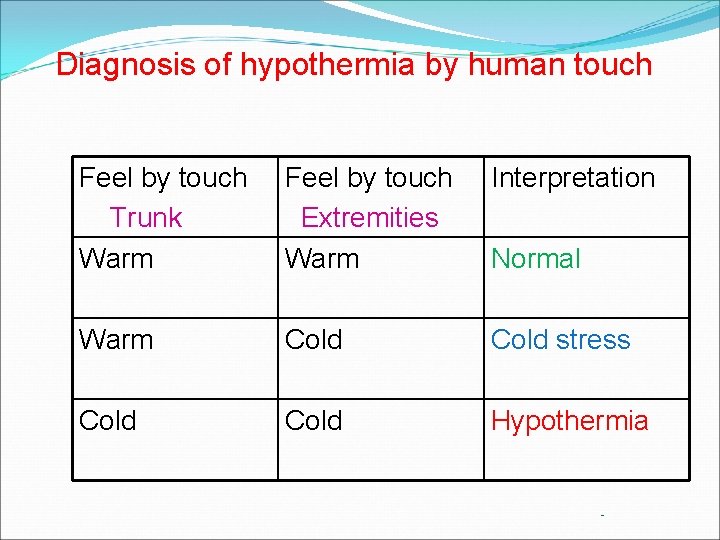
Diagnosis of hypothermia by human touch Feel by touch Trunk Warm Feel by touch Extremities Warm Interpretation Warm Cold stress Cold Hypothermia Normal -

Temprature recording By ? ? ? Accurate temperature recording is needed if a baby is: -preterm/LBW or sick -admitted to hospital regardless of reason -suspected of being either hypothermic or hyperthermic -rewarmed during management of hypothermia. -cooled down during management of hyperthermia.

Axillary temprature As good as rectal temprature but much safer. Steps of recording axillary temprature 1. Make sure thermometer is clean. 2. Shake is down, so that it read less then 35°c. 3. Place the bulb end of thermometer under baby’s dry armpit. 4. Keep thermometer in place for 3 minute. 5. Remove thermometer and read the temperature. 6. Keep thermometer in sterile condition.

Risks At birth During transport Within the hospital/home

Causes of hypothermia 1. The room is too cold 2. The baby is exposed to cold draft 3. The newborn is wet 4. The baby is uncovered, even for short time 5. The baby is placed on a cold surface or near cold wall or window 6. The baby has an infection 7. Baby has birth asphyxia and does not have energy to keep warm 8. The baby is not feeding well 9. Mother & baby are not together 20

Sign and symptom of hypothermia (a) Peripheral vasoconstriction (c) Increased metabolism Acrocyanosis Hypoglycemia Cool extremities Hypoxia Decreased peripheral Metabolic acidosis perfusion (b) Systemic depression Apnea Poor feeding Restlessness fb Lethargy Bradycardia Hypotension Inc PAP -Distress -Tachypnea Feed intol abdo distension (d) Chronic signs Weight loss, poor weight gain

PREVENTION?

Warm Chain: Is a set of ten interlinked procedures carried out at birth and during the following hours and days which will minimize the likelihood of hypothermia in all newborns.

Warm chain 1 Warm delivery room. . 2. Immediate drying. 3. Skin-to-skin contact. 4. Breast-feeding. 5. Bathing and weighing postponed. 6. Appropriate clothing and bedding. 7. Mother and baby together. 8. Warm transportation. 9. Warm resuscitation. 10. Training/awareness raising.

Prevention of hypothermia at birth • Conduct delivery in a warm room (>250 C) • Dry baby including head immediately with warm clean towel • Wrap baby in pre-warmed linen; cover the head and the limbs • Place the baby in skin-to-skin contact with the mother • Initiate early breastfeeding • Postpone bathing till? NT- 25

The delivery room temperature should be at least ? ? ? Adults should never determine the temperature of the delivery room according to their comfort.

The delivery room temperature should be at least 25°C. Adults should never determine the temperature of the delivery room according to their comfort.
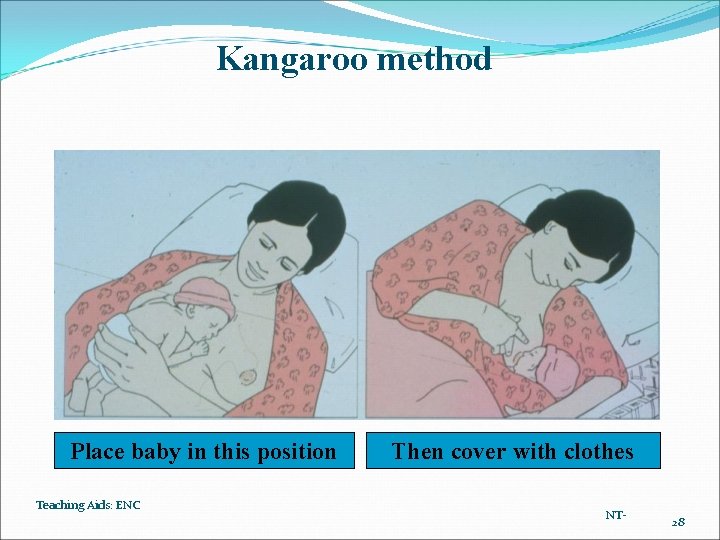
Kangaroo method Place baby in this position Teaching Aids: ENC Then cover with clothes NT- 28

The primary features of kangaroo-mother care are: • Uninterrupted use of adult body heat (skin-toskin contact) in order to maintain the newborn's body temperature; and, • Exclusive breast-feeding.
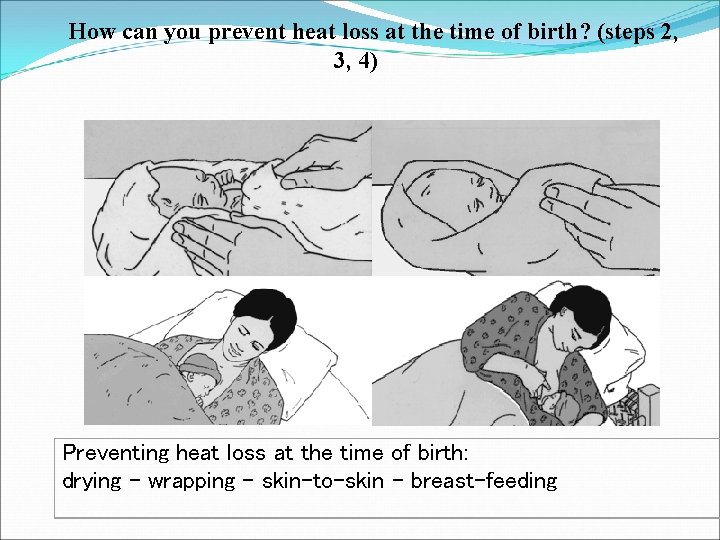
How can you prevent heat loss at the time of birth? (steps 2, 3, 4) Preventing heat loss at the time of birth: drying - wrapping - skin-to-skin - breast-feeding
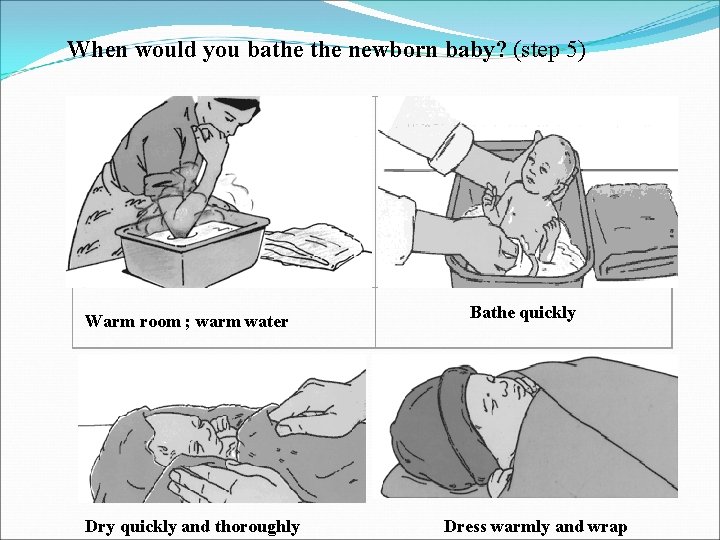
When would you bathe newborn baby? (step 5) Warm room ; warm water Bathe quickly Dry quickly and thoroughly Dress warmly and wrap
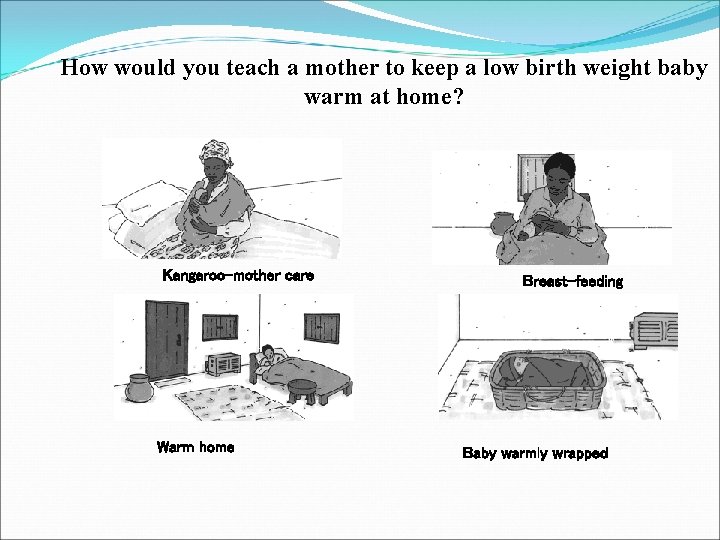
How would you teach a mother to keep a low birth weight baby warm at home? Kangaroo-mother care Warm home Breast-feeding Baby warmly wrapped
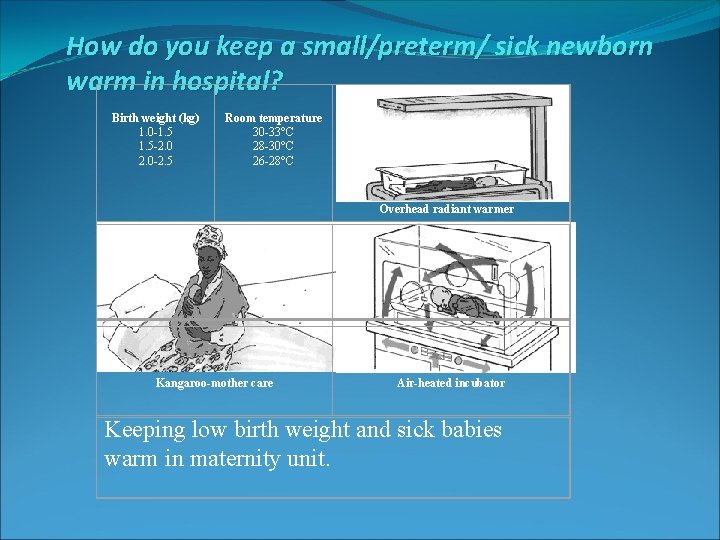
How do you keep a small/preterm/ sick newborn warm in hospital? Birth weight (kg) 1. 0 -1. 5 -2. 0 -2. 5 Room temperature 30 -33°C 28 -30°C 26 -28°C Overhead radiant warmer Kangaroo-mother care Air-heated incubator Keeping low birth weight and sick babies warm in maternity unit.

Treatment

Management : Cold stress Cover adequately Warm room Adequate measure to reduce heat Ensure skin-to –skin contact with mother breast feeding

Management : moderate hypothermia Skin to skin contact Warm room , warm bed Take measure to reduce heat Provide extra heat - 200 w bulb - Heater, warmer, incubator

Management: severe hypothermia Provide extra heat preferably under radiant warmer or air heated incubator. Rapidly warm till 34°c, then slow rewarming. Monitor axillary temp. every hourly for 3 hrs, then 2 hrly till normal then 3 hrly for 12 hrs Take measure to reduce heat loss IV fluids : 60 -80 ml/kg of 10%dextrose Oxygen and inj Vit-k If still hypothermic consider antibiotics, assuming sepsis. Monitor HR, BP and glucose if possible.
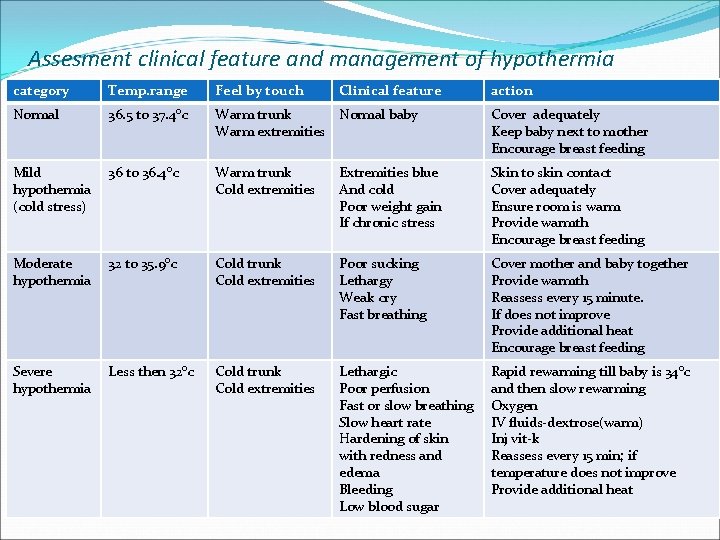
Assesment clinical feature and management of hypothermia category Temp. range Feel by touch Clinical feature action Normal 36. 5 to 37. 4°c Warm trunk Warm extremities Normal baby Cover adequately Keep baby next to mother Encourage breast feeding Mild hypothermia (cold stress) 36 to 36. 4°c Warm trunk Cold extremities Extremities blue And cold Poor weight gain If chronic stress Skin to skin contact Cover adequately Ensure room is warm Provide warmth Encourage breast feeding Moderate hypothermia 32 to 35. 9°c Cold trunk Cold extremities Poor sucking Lethargy Weak cry Fast breathing Cover mother and baby together Provide warmth Reassess every 15 minute. If does not improve Provide additional heat Encourage breast feeding Severe hypothermia Less then 32°c Cold trunk Cold extremities Lethargic Poor perfusion Fast or slow breathing Slow heart rate Hardening of skin with redness and edema Bleeding Low blood sugar Rapid rewarming till baby is 34°c and then slow rewarming Oxygen IV fluids-dextrose(warm) Inj vit-k Reassess every 15 min; if temperature does not improve Provide additional heat

Devices

Incubator Device that provides sufficient warmth to the body to maintain a desired temperature. Premature babies have very less fat around them and lose heat rapidly to the surrounding environment.

Indication When they are not maintaining their own temperature with clothing and wrapping. at risk of abnormal heat loss. known infection/ or the potential to develop sepsis. nutritional concerns small for gestational age. large wound site. New stoma or exposed bowel.

Incubators consist of the baby tray that is enclosed in a box like structure to provide a fix warm environment. Generally made of fibre glass or acrylic which is transparent This heat is used to warm the air mixture. Temperature control can be automatic as well as manual Available with single wall and double wall, .

Radiant warmer Warming device to provide heat to the body. Consists of an open tray and a heating mechanism mounted overhead. The skin temperature can be monitored by a temperature measuring probe. Can be manual or automatic

HYPERTHERMIA Hyperthermia occurs when the newborn's body temperature rises above 37. 5°C (99. 5°F), because the environment is too hot for the baby is overdressed.

Signs of hyperthermia Tachycardia, tachypnoea, apnoea Hypotension Warm extremities, flushing, perspiration Lethargy, hypotonia, poor feeding Central temperature lower that peripheral temperature

Signs of hyperthermia due to fever Pale, cool extremities Core temperature greater than peripheral temperature.
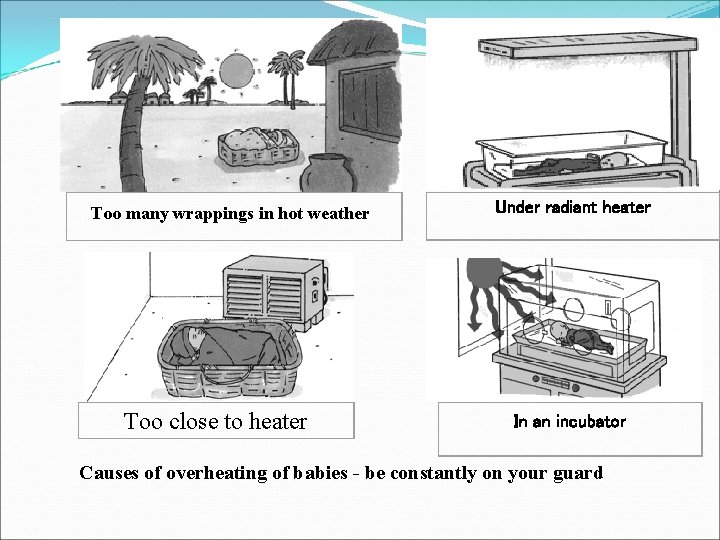
Too many wrappings in hot weather Too close to heater Under radiant heater In an incubator Causes of overheating of babies - be constantly on your guard

MANAGEMENT OF HYPERTHERMIA Assess for infection. Move baby away from the source of heat and undress. Give baby a bath if necessary. Give frequent breast-feeds. Monitor temperature.

Queries ?
- Slides: 50