Teach Asthma Management TAM Provided by Generously supported

Teach Asthma Management (TAM) Provided by: Generously supported by the Robert Wood Johnson Foundation Some slides adapted from Physician Asthma Care Education, developed by Noreen Clark, University of Michigan, School of Public Health

Part I of II

Overview of Asthma Michael Zacharisen, M. D. Allergist Children’s Hospital of Wisconsin

OBJECTIVES: Increase your knowledge of pediatric asthma epidemiology § Improve your clinical and community care of children with asthma and their families §
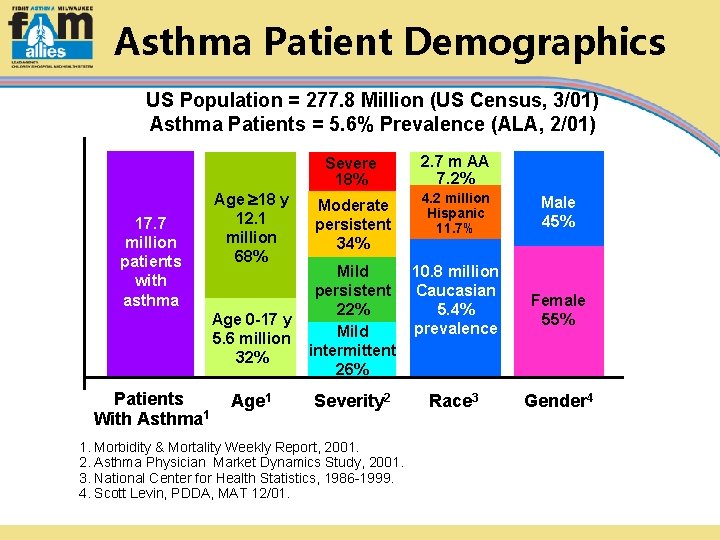
Asthma Patient Demographics US Population = 277. 8 Million (US Census, 3/01) Asthma Patients = 5. 6% Prevalence (ALA, 2/01) 17. 7 million patients with asthma Age 18 y 12. 1 million 68% Age 0 -17 y 5. 6 million 32% Patients With Asthma 1 Age 1 Severe 18% 2. 7 m AA 7. 2% Moderate persistent 34% 4. 2 million Hispanic 11. 7% Mild 10. 8 million persistent Caucasian 22% 5. 4% prevalence Mild intermittent 26% Severity 2 1. Morbidity & Mortality Weekly Report, 2001. 2. Asthma Physician Market Dynamics Study, 2001. 3. National Center for Health Statistics, 1986 -1999. 4. Scott Levin, PDDA, MAT 12/01. Race 3 Male 45% Female 55% Gender 4

CDC Press Release 9 million children <18 have been diagnosed with asthma § >4 million have had an asthma attack in the past 12 months § 12% of children <18 have been diagnosed with asthma Boys 14%, Girls 10% Poor families 16%, Not poor families 11% § www. cdc. gov/nchs released 3/2004
Burden of ASTHMA in Wisconsin 12% of adults and 8% of children have been told they have asthma (Overall = 9%) § 5, 000 asthma hospitalizations (2002) Costs of $36 million in 2002 Average charge of $6, 942/stay § 22, 418 asthma emergency department visits Costs of $13. 3 million in 2002 § Wis. DHFS; PPH 45055 (03/04) http: //dhfs. wisconsin. gov

Burden of ASTHMA in Wisconsin 80% report asthma symptoms in past 30 days § Only 48% report having a routine health care visit for asthma in past 12 months § Only 40% report daily medication use § In past 12 months: 14% adults had ED visit 18% adults had limited daily activities due to asthma § Wis. DHFS; PPH 45055 (03/04) http: //dhfs. wisconsin. gov

Definition of Asthma A chronic inflammatory disease of the airways with the following clinical features: • Episodic and/or chronic symptoms of airway obstruction. • Bronchial hyperresponsiveness to triggers. • Evidence of at least partial reversibility of the airway obstruction. • Alternative diagnoses are excluded.
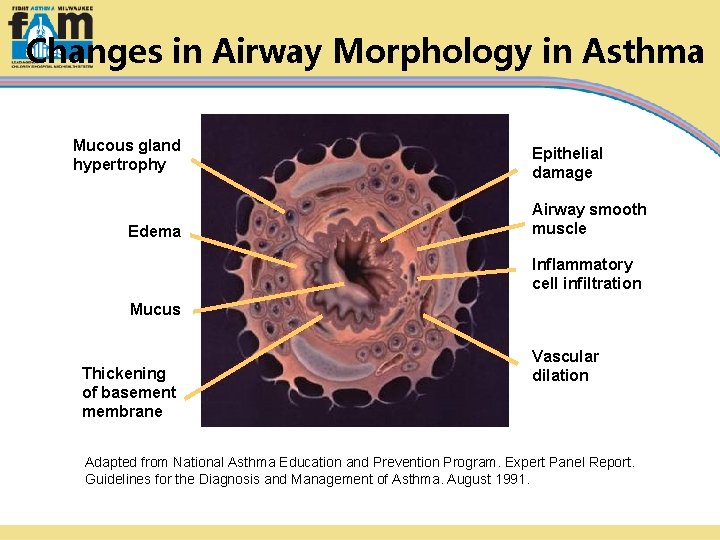
Changes in Airway Morphology in Asthma Mucous gland hypertrophy Edema Epithelial damage Airway smooth muscle Inflammatory cell infiltration Mucus Thickening of basement membrane Vascular dilation Adapted from National Asthma Education and Prevention Program. Expert Panel Report. Guidelines for the Diagnosis and Management of Asthma. August 1991.
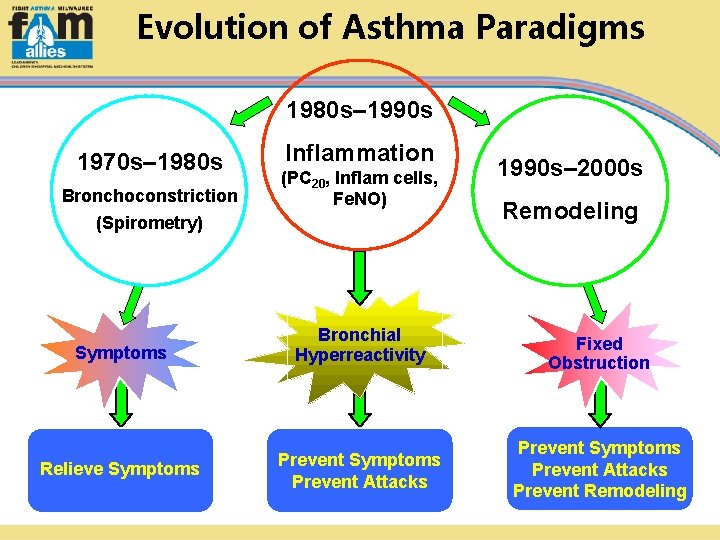
Evolution of Asthma Paradigms 1980 s– 1990 s 1970 s– 1980 s Bronchoconstriction Inflammation (PC 20, Inflam cells, Fe. NO) (Spirometry) 1990 s– 2000 s Remodeling Symptoms Bronchial Hyperreactivity Fixed Obstruction Relieve Symptoms Prevent Attacks Prevent Remodeling
A Lot Going On Beneath The Surface Symptoms Airflow obstruction Bronchial hyperresponsiveness Airway inflammation

Expert Panel Report 2: Four Components of Asthma Management n Measures of Assessment and Monitoring n Control of Factors Contributing to Asthma Severity n Pharmacologic Therapy n Education for a Partnership in Asthma Care

Component 1: Initial Assessment and Diagnosis of Asthma n Determine that: Patient has history or presence of episodic symptoms of airflow obstruction Airflow obstruction is at least partially reversible Alternative diagnoses are excluded n Methods for establishing diagnosis: Detailed medical history Physical exam Spirometry to demonstrate reversibility

Component 1: Initial Assessment and Diagnosis of Asthma (continued) Does patient have history or presence of episodic symptoms of airflow obstruction? n Wheeze, shortness of breath, chest tightness, or cough n Asthma symptoms vary throughout the day n Absence of symptoms at the time of the examination does not exclude the diagnosis of asthma

Initial Assessment and Diagnosis of Asthma (continued) Is airflow obstruction at least partially reversible? n Use spirometry to establish airflow obstruction: FEV 1 < 80% predicted; FEV 1/FVC <65% or below the lower limit of normal n Use spirometry to establish reversibility: FEV 1 increases >12% and at least 200 m. L after using a short-acting inhaled beta 2 -agonist

Component 2: Control of Factors Contributing to Asthma Severity n Assess exposure and sensitivity to: Inhalant allergens Occupational exposures Ask specifically about work-related triggers Irritants: Indoor air (including tobacco smoke) Air pollution

Component 2: Control of Factors Contributing to Asthma Severity n Assess contribution of other factors: Rhinitis/sinusitis Gastroesophageal reflux Drugs (NSAIDs, beta-blockers) Viral respiratory infections Sulfite sensitivity (continued)
Pediatric Differential Diagnosis § Chronic sinusitis § Vocal cord dysfunction (VCD) § Croup § Tracheomalaci a §Foreign body §Bronchiolitis §Cystic fibrosis / Ciliary dysfunction §GERD §Hyperventilatio n syndrome

Viruses and Asthma Viral infections frequently cause wheezing 30 -60% of children will wheeze in 1 st 5 years Frequent cause of asthma exacerbation § Unable to directly link viral infections with development of asthma Proven risk factors include: § Family history of asthma Environmental smoke exposure History of severe bronchiolitis in 1 st 18 months

Benchmarks of Good Asthma Control § § § Infrequent coughing or wheezing No shortness of breath or difficulty breathing No waking up at night due to asthma Normal physical activities No childcare or school absences due to asthma No missed time from work for parent or
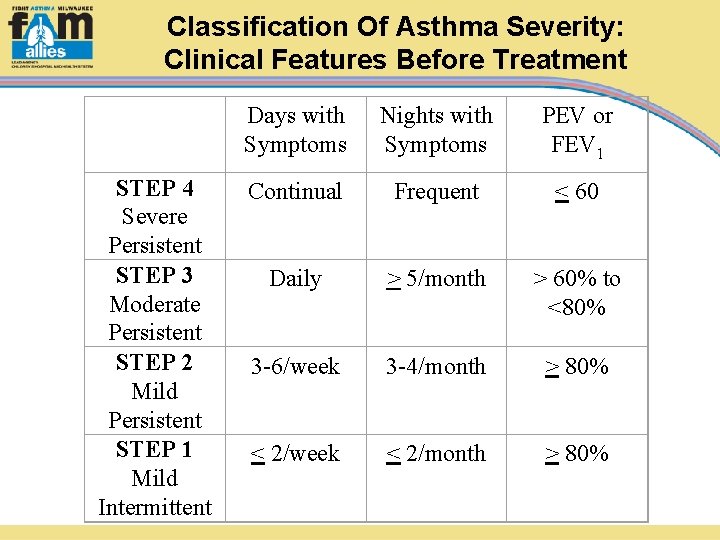
Classification Of Asthma Severity: Clinical Features Before Treatment Days with Symptoms Nights with Symptoms PEV or FEV 1 STEP 4 Severe Persistent STEP 3 Moderate Persistent STEP 2 Mild Persistent STEP 1 Mild Intermittent Continual Frequent < 60 Daily > 5/month > 60% to <80% 3 -6/week 3 -4/month > 80% < 2/week < 2/month > 80%
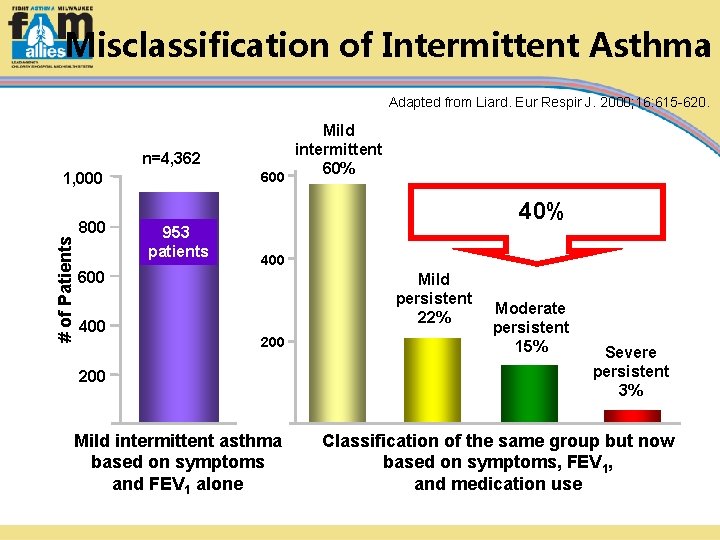
Misclassification of Intermittent Asthma Adapted from Liard. Eur Respir J. 2000; 16: 615 -620. n=4, 362 # of Patients 1, 000 800 953 patients Mild intermittent 60% 600 40% 400 600 400 Mild persistent 22% 200 Mild intermittent asthma based on symptoms and FEV 1 alone Moderate persistent 15% Severe persistent 3% Classification of the same group but now based on symptoms, FEV 1, and medication use
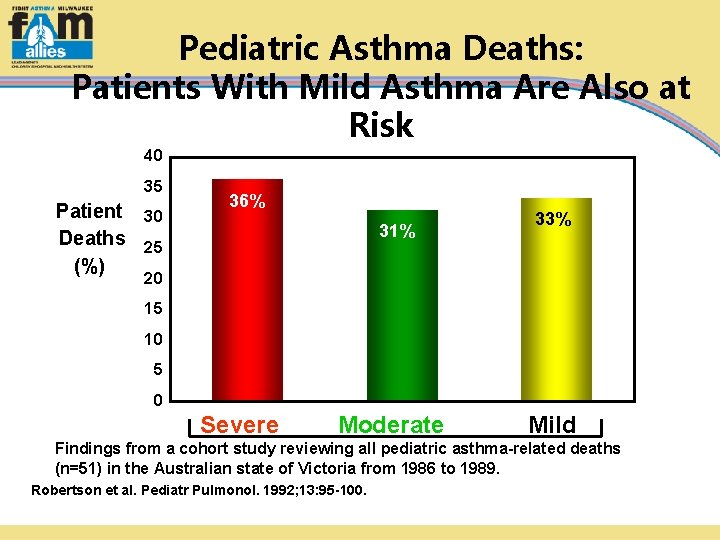
Pediatric Asthma Deaths: Patients With Mild Asthma Are Also at Risk 40 35 Patient 30 Deaths 25 (%) 36% 31% 33% 20 15 10 5 0 Severe Moderate Mild Findings from a cohort study reviewing all pediatric asthma-related deaths Patient Assessment (n=51) in the Australian state of Victoria from 1986 to 1989. Robertson et al. Pediatr Pulmonol. 1992; 13: 95 -100.

How Can Asthma Control Be Measured? Inflammation? Direct or indirect? Lung function? Nighttime awakenings? Utilization of healthcare resources? Satisfaction with care? Functional status? Daytime symptoms? Asthma Control Missed work and/or school? Use of “quick relief” inhaler and/or nebulizer? Patient self-report of control?
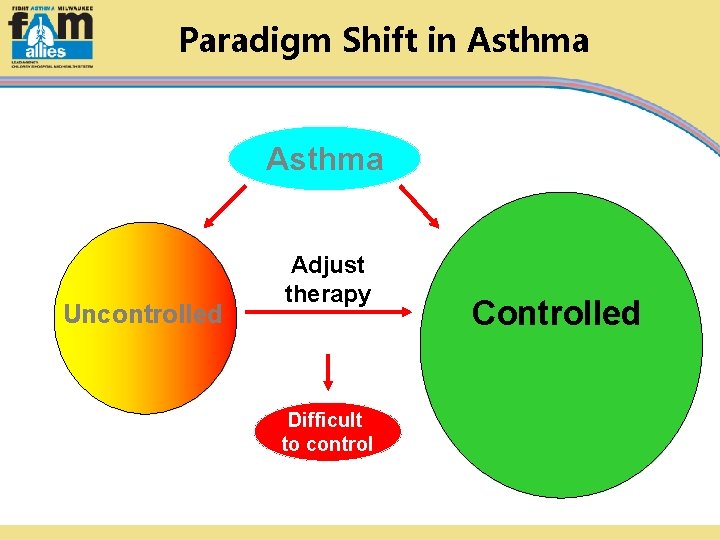
Paradigm Shift in Asthma Uncontrolled Adjust therapy Difficult to control Controlled

Asthma Control and Steroid Doses After Early or Delayed Intervention § Patients with asthma started on budesonide were compared based on duration of asthma at budesonide initiation Asthma for <2 years Asthma for 2 years § Outcomes assessed Lung function: FEV 1, PEF Persistent need for inhaled corticosteroid Persistent symptoms Selroos et al. Respir Med. 2004; 98: 254 -262.
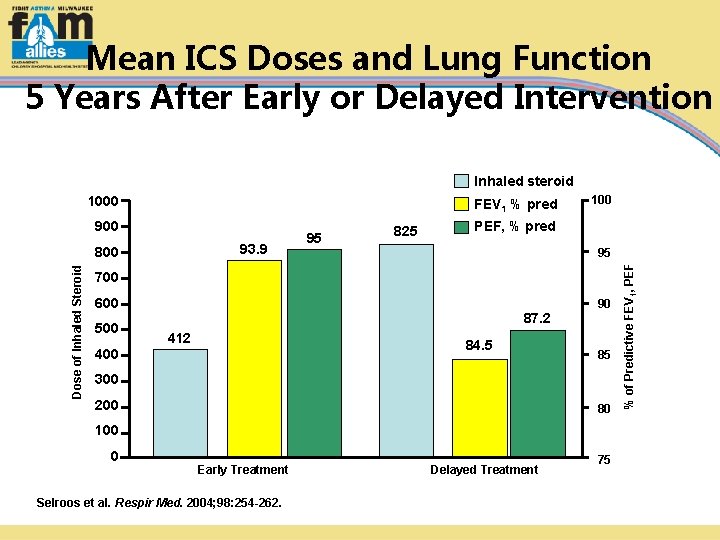
Mean ICS Doses and Lung Function 5 Years After Early or Delayed Intervention Inhaled steroid FEV 1 % pred 900 93. 9 Dose of Inhaled Steroid 800 95 825 100 PEF, % pred 95 700 600 500 400 87. 2 412 84. 5 90 85 300 200 80 100 0 Early Treatment Selroos et al. Respir Med. 2004; 98: 254 -262. Delayed Treatment 75 % of Predictive FEV 1, PEF 1000

Does chronic use of inhaled corticosteroids improve long-term outcomes for children with mild or moderate asthma, compared to other asthma medications? “Strong evidence” established that inhaled corticosteroids improve asthma control for children with mild-moderate asthma § None of the alternatives “listed alphabetically” cromolyn, leukotriene modifier, nedocromil, sustained release theophylline are as effective § “Low dose” inhaled corticosteroids are the “preferred” treatment for mild asthma § “Low dose” inhaled corticosteroids plus long acting inhaled beta 2 agonists are the NIH Publication No. 02 -5075, June 2002 “preferred” treatment for moderate asthma §

Inhaled Glucocorticoids Versus Leukotriene Receptor Antagonists as Single Agent Asthma Treatment: Systematic Review of Current Evidence Ducharme FM. BMJ 2003; 326: 621 -625. § Objective: To compare the safety and efficacy of leukotriene modifiers (LTM) with inhaled corticosteroids (ICS) as monotherapy in patients with asthma § Primary Outcome: Rate of exacerbations that required treatment with systemic corticosteroids § Secondary Outcomes: Lung function (FEV 1, AM PEF), nocturnal awakenings, use of rescue

Results - Primary Outcome Patients receiving LTM were 60% more likely to experience an exacerbation than those treated with ICS (11 trials; RR 1. 6, 95% CI 1. 2 -2. 2) § No difference in risk for exacerbations was found in the one pediatric trial reviewed (RR 0. 78, 0. 32 -1. 85) Ducharme FM. BMJ 2003; 326: 621 -625. §

What are the long-term adverse effects of chronic inhaled corticosteroid use in children: growth, bone density, ocular, HPA? “Strong evidence” shows that inhaled corticosteroids at recommended doses do not have clinically significant or irreversible effects on these outcomes § Low to medium doses of inhaled corticosteroids have the potential to decrease growth velocity 1 cm in the first year but this is NOT sustained, progressive, and may be reversible § Observational studies up to 6 years reveal no adverse effect on bone density, cataracts, NIH Publication No. 02 -5075, June 2002 glaucoma, or clinically significant HPA axis §
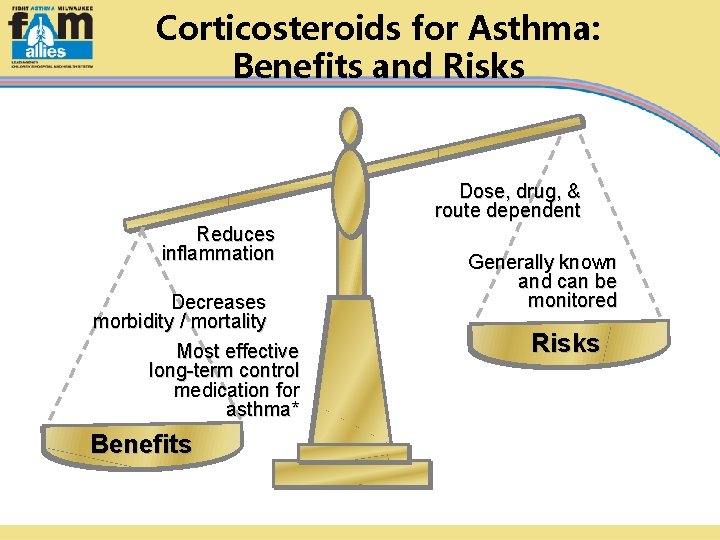
Corticosteroids for Asthma: Benefits and Risks Dose, drug, & route dependent Reduces inflammation Decreases morbidity / mortality Most effective long-term control medication for asthma* Benefits Generally known and can be monitored Risks

In patients with moderate persistent asthma who are on ICS, does the addition of another long-term control agent improve outcomes? “Strong evidence” consistently indicates that the addition of a long acting inhaled ß 2 agonist leads to improvement in lung function, symptoms & reduced additional ß 2 agonist use § Adding an LTM or theophylline to an ICS or doubling the ICS dose improves outcomes “but the evidence is not as substantial” § For children less than 5 the preferred treatment is low dose ICS + a long acting inhaled ß 2 NIH agonist Publicationor No. 02 -5075, June 2002 medium dose ICS §

What have we learned from all of the studies? low-dose ICS + LABA vs. “otherapy” results in: § § § Lung function Symptoms Albuterol use Exacerbations Reduces need to increase ICS dose Replicated numerous times by other investigators Greening et al. Lancet. 1994; 344: 219 -224. Woolcock et al. Am J Respir Crit Care Med. 1996; 153: 1481 -1488 Nelson et al J Allergy Clin Immunology 2000; 106: 1088 -1095

Infants and Young Children— When to Start Controllers >3 episodes of wheezing in the last year and § Parental history of asthma or physician diagnosis of eczema § Or 2 of the following § Physician diagnosis of allergic rhinitis, wheezing apart from colds, peripheral eosinophilia § Courses of oral steroids more often than every 6 wk

Principles of Maintenance Therapy Start high. § Step down once control is achieved. § Maintain at lowest dose of medication that controls asthma. § Step up and down as indicated. §
Step-down Therapy Step down once control is achieved. § After 2– 3 mo. § 25% reduction over 2– 3 mo. Follow-up monitoring § Every 1– 6 mo. § Assess symptoms. § Review medication use. § Objective monitoring (PEFR or spirometery). § Review medication.
Step-up Therapy Indications: symptoms, need for quick-relief medication, exercise intolerance, decreased lung function. May need short course of oral steroids. § Continue to monitor. Follow and reassess every 1– 6 mo. Step down when appropriate. §

Acute Exacerbations Principle: Gain control as quickly as possible. Treat all asthma exacerbations promptly and aggressively. § Inhaled ß 2 -agonist inhalants for quick relief § Access to quick relief medication § Written action plan Indications Medications When to contact physician or emergency medical services § Short course of oral corticosteroids

Acute Exacerbations Office Management Assess severity. § § § § Symptoms, signs, lung function, pulse oximetry (if available) Oxygen recommended Short acting ß 2 -agonist inhalant every 20– 30 min Ipratropium—metered-dose inhaler, inhalation solution Corticosteroid—orally, intravenous if vomiting Intravenous favored if dehydrated Follow-up—hours (phone) to 1– 7 d

Stepwise Approach to Therapy for Children 5 Years Step 4 Severe Persistent Step 3 Moderate Persistent Step 2 Mild Persistent Step 1 Mild Intermittent Preferred: Low-dose ICS No Daily Medication Alternative: Cromolyn or LTRA Preferred: Low-dose ICS + LABA or Medium-dose ICS (+ LABA if needed) High-dose ICS + LABA (+ systemic corticosteroids if needed) Alternative: Low- to Med-dose ICS + LTRA or Theophylline ICS = inhaled corticosteroid; LABA = long-acting 2 -agonist; LTRA = leukotriene receptor antagonist NIH/NHLBI Guideline Update. June 2002. NIH Publication No. 02 -5075.
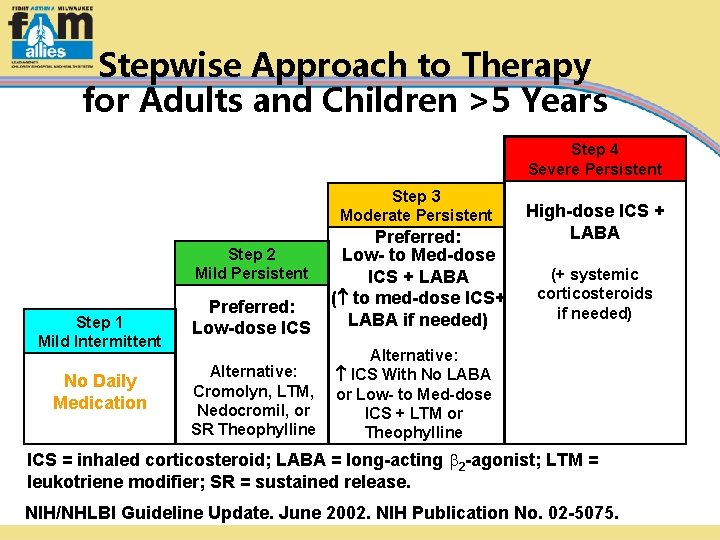
Stepwise Approach to Therapy for Adults and Children >5 Years Step 4 Severe Persistent Step 3 Moderate Persistent Step 2 Mild Persistent Step 1 Mild Intermittent No Daily Medication Preferred: Low-dose ICS Alternative: Cromolyn, LTM, Nedocromil, or SR Theophylline Preferred: Low- to Med-dose ICS + LABA ( to med-dose ICS+ LABA if needed) High-dose ICS + LABA (+ systemic corticosteroids if needed) Alternative: ICS With No LABA or Low- to Med-dose ICS + LTM or Theophylline ICS = inhaled corticosteroid; LABA = long-acting 2 -agonist; LTM = leukotriene modifier; SR = sustained release. NIH/NHLBI Guideline Update. June 2002. NIH Publication No. 02 -5075.

Tools to Improve Asthma Documentation & Quality Care Living with Asthma Questionnaire § Asthma Control Test § Progress Note Template § Asthma Action Plan § More QI information see: www. eqipp. org www. improvingchroniccare. org
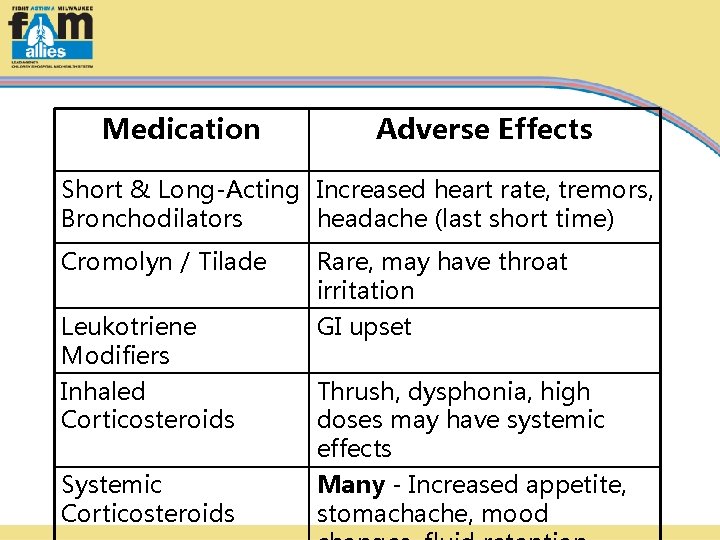
Medication Adverse Effects Short & Long-Acting Increased heart rate, tremors, Bronchodilators headache (last short time) Cromolyn / Tilade Rare, may have throat irritation Leukotriene Modifiers Inhaled Corticosteroids GI upset Systemic Corticosteroids Many - Increased appetite, stomachache, mood Thrush, dysphonia, high doses may have systemic effects

Education for Partnership in Care Develop a written asthma management plan Agree on therapy goals Outline daily treatment and monitoring measures Prepare an action plan to handle worsening symptoms § Provide routine education on patient selfmanagement How and why to take medications Correct technique for devices §

Asthma Medications and Devices Rhonda J. Duerst, RRT-NPS, AEC Children’s Hospital of Wisconsin

Objective: § Teach caregivers to administer daily anti-inflammatory control medications as needed and quick relief medicines for patients with persistent asthma

Asthma Can be Managed With proper therapy, the child can be symptom free § Goal is to use the least amount of medication as possible, increasing on an as-needed basis § Long-term goal of reducing or even stopping regular medications § Emphasis on as little as possible address parents’ fears of over§

What makes Asthma Management so hard for Parents and Children? § § § Here today, gone tomorrow: periods of symptoms interspersed with symptom-free periods Daily medicines even when feeling well Unpredictability: don’t know exactly what triggers the episode Complicated medication plan varies with symptom intensity and disease severity Need to monitor asthma symptoms Fears about medication side-effects

Explaining How to Take Medicines § Clinician Message: Demonstrate use of inhaler and spacer Show to use peak flow meter Give step-by-step instructions § Parent Message: Feel comfortable with “technology ” Know how and where to get equipment

Fears About Asthma Medicines 39% Believe medicines are addictive 36% Believe medicines are not safe to take over a long period 58% Believe regular use will reduce effectiveness

Quick Relief Medicines § § § Act fast, generally within 15 -20 minutes Relaxes the smooth muscles around the bronchial tubes Parents need to know how often child is using Must have available at all times Is only medicine that helps child breathe quickly

ASTHMA MEDICATIONS § Beta 2 agonists - bronchodilators Albuterol (Proventil, Ventolin) Pirbuterol (Maxair) Levalbuterol (Xopenex) Terbutaline (Brethine) Metaproterenol (Alupent)

Explain About Quick-Relief Medications § Provider message: –Quick-relief medications relax the muscles after they have tightened during an attack –Parents are in charge of helping their children breathe through the quickrelief medications –Quick- relief medications act fast, § Parent Message: –Know that medicines will open up lungs and child won’t suffocate –Know that reaction is not instant; may take a few minutes –Quick relief medicines are parents’ ticket to helping child breathe

Communication Tip for Quick-Relief Medications Use a physical example: Unclamp fist to show medicines work § Ask parent about fears they have regarding child’s asthma episode § Discuss concerns parents may have about medications Jitteriness; anxiety & other side effects parents may fear (“dependence”) § Be accurate about risks but reinforce message that medicines work! §

Explaining about Long-term Control Medications § Provider Message: –Anti-inflammatory medicines don’t relieve symptoms –Do reduce inflammation and prevent frequent or severe episodes –Needed if symptoms more than 2 X/week in day or 2 X/month at night § Parent Message: –Anti-inflammatory meds are like a flu shot, to help keep away the “bad” asthma episodes –Anti-inflammatory medicines are like vitamins; they need to be taken all the time, even if not sick

Communication Tips about Long-term Control Medicines Explain the different types of controllers (parents want to know the names), and why more than one may be used § Convey clearly information about any risks or side effects § Discuss fears about medication “dependence” Low Doses of Inhaled Corticosteroids do not cause side effects §

ASTHMA MEDICATIONS § Long-acting beta 2 agonists Salmeterol (Serevent) Formoterol (Foradil) Combine with ICS (ADVAIR available)
Corticosteroids § Inhaled (ICS) Beclomethasone (Vanceril, Beclovent, QVAR) Budesonide (Pulmicort) Flunisolide (Aerobid) Fluticasone (Flovent, ADVAIR) Triamcinolone acetonide (Azmacort) § Systemic Prednisone/Predniso lone Methylprednisolone (Solu-Medrol, Medrol)

ASTHMA MEDICATIONS Mast cell stabilizers Cromolyn sodium (Intal) Nedocromil (Tilade) § Anticholinergic Ipratropium bromide (Atrovent) § Methylxanthines Theophylline Aminophylline §

ASTHMA MEDICATIONS § Leukotriene inhibitors Oral, QD-BID Montelukast (Singulair) Zafirlukast (Accolate) Zileuton (Zyflo) Some evidence of effectiveness in preventing premenstrual asthma 1. J Allergy Clin Immunol 1999; 104: 585 -8. exacerbations 1
Teaching Checklist ü ü ü Use of inhaler/spacer Use of nebulizer Use of Peak Flow Meter Give step by step directions Instruct how/where to get spacers/nebs/PFM Instruct what to do if run out of medicine or can’t get devices ü Ask parent/child to demonstrate technique at each visit ü Reassure parent about using alternative treatments with medications ü

Spacers/Holding Chambers

Spacers/Holding Chambers Recommended with all medium to high dose ICS § Enhance delivery, especially with children § Improves coordination and medication delivery some provide auditory feedback § Minimize adverse effects from ICS decrease oral bioavailability reduce oral candidias (thrush) §
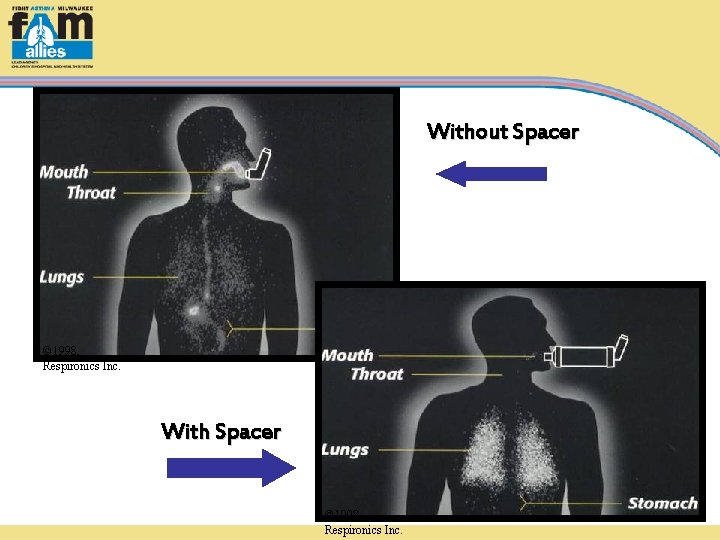
Without Spacer © 1998, Respironics Inc. With Spacer © 1998, Respironics Inc.

Dry Powder Inhalers (DPI) Spacers can not be used with DPI § Turbuhaler®, Diskus®, Aerolizer™ § Must be able to do mouthpiece treatment § Deep rapid inhalation §

Peak Flow Meters

Peak Flow Monitoring § § § Provides objective information Documents personal best Detects worsening asthma before changes occur Useful only if breathing is monitored regularly Indicates need for quick-relief medications

Determine Personal Best Peak Flow Take peak flow reading at least once per day for 2 -3 weeks § Measure peak flow at these times: § Between noon and 2 pm each day Each time quick-relief meds are taken for symptoms Any other time your doctor suggests § Use same peak flow meter over time

Proper PF Technique 1 - Set meter to Zero 2 - Stand up straight 3 - Take deep breath in 4 - Blow out hard & fast 5 - Repeat two more times 6 - Record your highest number

Teaching Peak Flow § § § Instruct in how to establish child’s personal best Demonstrate to child/parent how to set child’s zones (red, yellow & green) Help parent establish a routine for peak flow measurements Remind parent to adjust medications according to peak flow number Encourage parent to bring PF diary with to all
- Slides: 72