TCPI Project Pathway Session 6 of 8 Coordinated

























- Slides: 27

TCPI Project Pathway: Session 6 of 8 Coordinated Care – Milestone # 8, 9, 10 (11, 12, 13, 14 for primary care) Improving heart care quality, patient experience and costs

About the TCPI Milestones Ø 22 Milestones for specialty practices Ø 27 Milestones for primary care Ø Scores on each milestone determine Phase completion Ø For example, to complete Phase 1, as score of 3 is necessary on milestone 13 (setting an aim). Ø Other phases require various scores for other milestones.

Milestone Classes Review Scoring and Strategies for Meeting Them (numbers in parentheses indicate milestone numbers for primary care) Each Milestone-Group Class will be held live 3 times: ü Quality Improvement Strategies and Action –milestones 14, 15, 16 (19, 20, and 21) (already held- recording available) ü Improvement Goals – milestones 1, 2, 3, 13 (1, 2, 3, 18) ü Staff Engagement: Teamwork and Joy – milestones 6 and 19 (6 and 24) ü Identifying Patient Risk and Using Best Practices – milestones 7, 11 (8, 9, 10, 16) ü Streamlining Clinical and Office Work – milestone 22 (27) 6. Coordinated Care – milestones 8, 9, 10 (11, 12, 13, 14) 7. Person and Family-Centered Care – milestones 4, 5, 12, 17 (4, 5, 7, 15, 17 and 22 for primary care) 8. Business Strategies – milestones 18, 20, 21 (23, 25, 26)

Today’s Objectives Ø Review scoring for coordinated care-related milestones: 8, 9, 10 (11, 12, 13, 14 for primary care) Ø Outline strategies for meeting each of these milestones Ø Review relevance of milestones’ scores to phases Ø Open discussion

Coordinated Care Ø Specialty milestones: 8, 9, 10 Ø Primary care milestones: 11, 12, 13, and 14

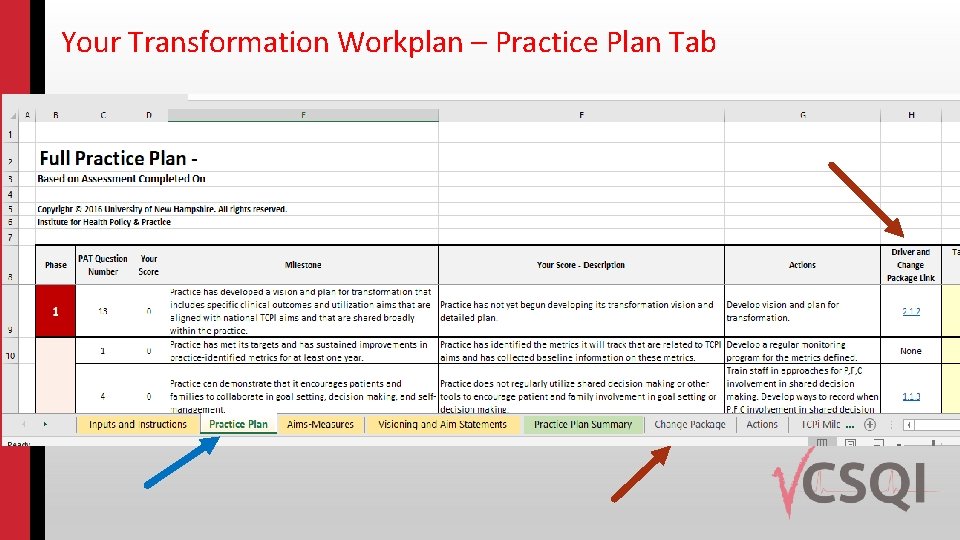
Your Transformation Workplan – Practice Plan Tab

Related Specialty Milestones Milestone 8: Practice facilitates referrals to appropriate community resources, including community organizations and agencies as well as direct care providers. (Primary care milestone 11 is identical to this one. ) Ø Milestone 9: Practice works with the primary care practices in its medical neighborhood to develop criteria for referrals for episodic care, comanagement, and transfer of care/ return to primary care, processes for care transition, including communication with patients and family. Ø Milestone 10: Practice identifies the primary care provider or care team of each patient seen and (where there is a primary care provider) communicates to the team about each visit/ encounter. Ø

Milestone 8 (11 for primary care): Practice facilitates referrals to appropriate community resources, including community organizations and agencies as well as direct care providers. a score of 3 is needed to complete Phase 4

Strategies for Meeting Milestone 8 (#11 for primary care) Change Package – 1. 4. 4 Ø Vet all potential referral providers and agencies Ø Leverage personal relationships to cultivate referral opportunities Ø Maintain an inventory of community resources that may be available to patients Ø Work with community agencies to enhance services available to patients Ø Maintain formal (referral) links to community-based chronic disease self-management support programs, exercise programs and other wellness resources with the potential for bidirectional flow of information Ø Provide a guide to available community resources

Strategies for Meeting Milestone 8 (#) Change Package – 1. 4. 4 - continued Ø As a provider, employ the philosophy “You should only refer to a provider you would send your loved one to” Ø Create and maintain referral lists for medical residents in academic settings Ø Engage local health coalitions to identify resources in areas where resources are scarce Ø Find out how patients define quality of care and build those definitions into the practice model Ø Maintain a referral tracking system to assure “loop closure” (i. e. that patients make and keep appointments and that a report is received)

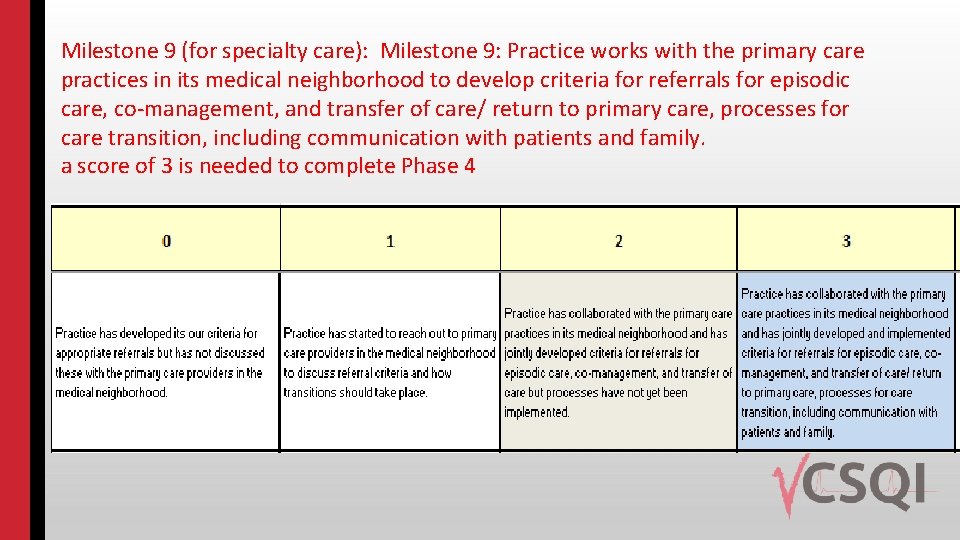
Milestone 9 (for specialty care): Milestone 9: Practice works with the primary care practices in its medical neighborhood to develop criteria for referrals for episodic care, co-management, and transfer of care/ return to primary care, processes for care transition, including communication with patients and family. a score of 3 is needed to complete Phase 4

Strategies for Meeting Milestone 9 Change Package – 1. 5. 2 Ø Define the medical neighborhood with which the practice works most closely Ø Develop both personal and electronic relationships among medical neighborhood providers to ensure information sharing Ø Develop formal written agreements or compacts that define information needs of all parties Ø Formalize lines of communication with local care settings in which empaneled patients receive care to ensure documented flow of information and clear transitions in care. Ø Ensure that useful information is shared with patients and families at every care transition; partner with patients and families in developing processes and tools to make that happen Ø Engage payer disease management and complex care management staff to help avoid patient/family confusion

https: //www. advisory. com/research/care-transformation-center/caretransformation-center-blog/2015/11/medical-neighborhood-step-one

https: //www. advisory. com/research/physician-executivecouncil/resources/posters/crossing-the-communicationchasm? WT. ac=Gray. Box. P_PEC_Info_Physician. Issues___CTC_20 15 NOV 11_

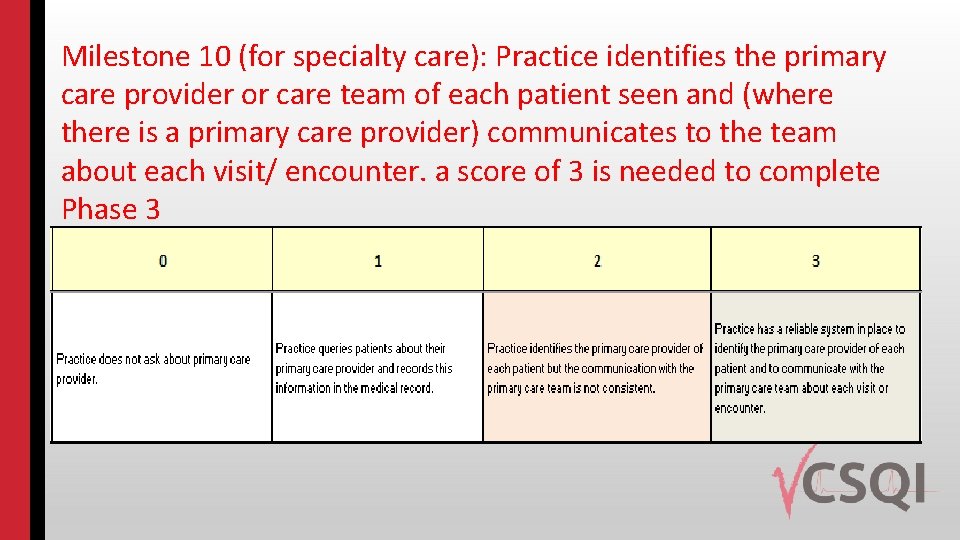
Milestone 10 (for specialty care): Practice identifies the primary care provider or care team of each patient seen and (where there is a primary care provider) communicates to the team about each visit/ encounter. a score of 3 is needed to complete Phase 3

Strategies for Meeting Milestone 10 Add “Who is your primary care physician (PCP)? ” question to appointment information/form patient completes and/or to list of questions intake person asks. Ø Train all staff who conduct intake interviews to document the PCP in the patient’s medical record. Ø Add PCP’s phone number/email/fax number to patient’s record Ø Establish process for updating PCP after each visit by patient. Ø

Related Primary Care Milestones Milestone 11: Practice facilitates referrals to appropriate community resources, including community organizations and agencies as well as direct care providers. (COVERED PREVIOUSLY as specialist milestone #8) Ø Milestone 12: Practice has defined its medical neighborhood and has formal agreements in place with these partners to define roles and expectations. Ø Milestone 13: Practice follows up via phone, visit, or electronic means with patients within a designated time interval (24 hours/ 48 hours/ 72 hours/ 7 days) after an emergency room visit or hospital discharge. Ø Milestone 14: Practice clearly defines care coordination roles and responsibilities and these have been fully implemented within the practice. Ø

Milestone 12: Practice has defined its medical neighborhood and has formal agreements in place with these partners to define roles and expectations. A score of 3 is needed to complete Phase 4.

Strategies for Meeting Milestone 12 Change Package – 1. 5. 2 Ø Define the medical neighborhood with which the practice works most closely Ø Develop both personal and electronic relationships among medical neighborhood providers to ensure information sharing Ø Develop formal written agreements or compacts that define information needs of all parties Ø Formalize lines of communication with local care settings in which empaneled patients receive care to ensure documented flow of information and clear transitions in care. Ø Ensure that useful information is shared with patients and families at every care transition; partner with patients and families in developing processes and tools to make that happen Ø Engage payer disease management and complex care management staff to help avoid patient/family confusion

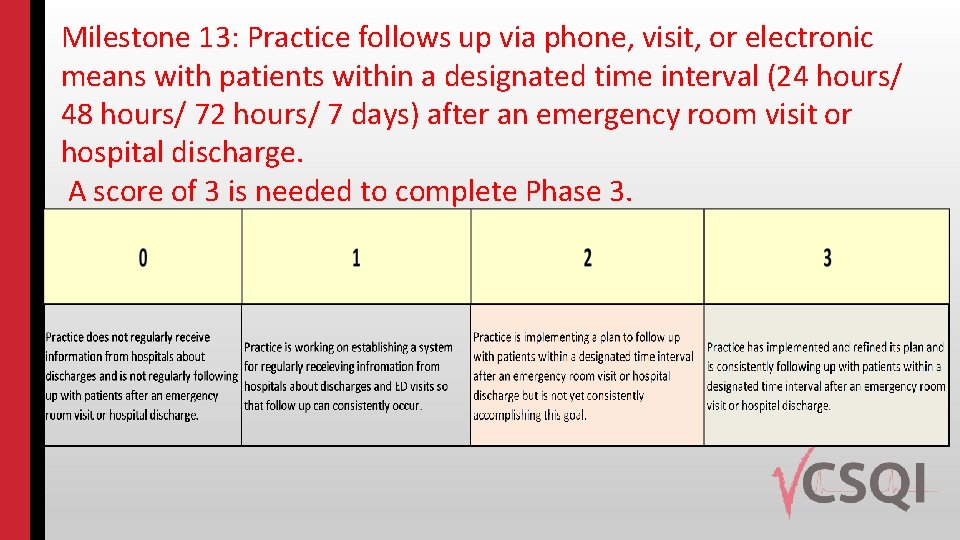
Milestone 13: Practice follows up via phone, visit, or electronic means with patients within a designated time interval (24 hours/ 48 hours/ 72 hours/ 7 days) after an emergency room visit or hospital discharge. A score of 3 is needed to complete Phase 3.

Strategies for #13 (primary care) Change package 1. 5. 1 Ø Assign responsibility for care management of individuals at high risk for emergency department visits or hospital readmission Ø Follow up after every hospital discharge and ED visit with a phone call, home or office visit Ø Assure patients can get access to their care team when they need it to support reduction in emergency department use Ø Partner with community or hospital-based transitional care services Ø Routine and timely follow-up to hospitalizations Ø Routine and timely follow-up to emergency department visits Ø Encourage patients to rely on multiple team members as experts

Strategies for #13 (primary care) - continued Change package 1. 5. 1 Ø Establish a mutual understanding of the information that should be shared when care is transferred or shared among providers Ø Develop agreements with specialists in the community that identify goals for communication Ø Have someone talk with patient and family to prior to each transition so they understand what the next step is and what it may mean Ø Review when care transitions are NOT optimal and look for themes Ø Use pharmacists to co-manage chronic disease states under collaborative agreements Ø Pre-plan transition of care appointments when able to Ø Ensure that useful information is shared with patients and families at every care transition Ø Engage payer disease management and complex care management staff to help avoid patient/family confusion

Milestone 14: Practice clearly defines care coordination roles and responsibilities and these have been fully implemented within the practice. A score of 3 is needed to complete Phase 4.

Strategies for #14 (primary care) Change package 1. 5. 3 Ø Develop compacts between primary care and specialists Ø Assign responsibility to specific staff members for care coordination and referral management Ø Establish systems for two-way exchange of information within the medical neighborhood Ø Follow up on all referrals to assure loop closure on information flow to care team and to patients Ø Participate in Health Information Exchange if available. Ø Use structured referral notes to standardize information shared and facilitate appropriate referrals

Strategies for #14 (primary care - continued Change package 1. 5. 3 Ø Establish care coordination agreements with frequently used consultants that set expectations for documented flow of information and provider expectations between settings Ø Track patients referred to specialists through the entire process Ø Systematically integrate information from referrals into the plan of care. Ø Allow primary care team to request urgent appointments for specialist consults Ø Have a shared care plan for co-managed patients Ø Establish a mutual understanding of the information that should be shared when care is transferred or shared among providers Ø In specialty practices, for each referral, notify the referring care team of the date of scheduled appointments, as well as of any cancellations and no shows


Coming Next Week – Class 7 Person and Family-Centered Care Ø Specialty milestones 4, 5, 12, 17 Ø Primary care milestones 4, 5, 7, 15, 17, 22