TBHIV PublicPrivate Partnership for MARGs in Jakarta Indonesia

TB/HIV: Public-Private Partnership for MARGs in Jakarta, Indonesia Dr Flora Tanujaya, MSc Senior Clinical Officer, FHI Indonesia Dr Halim Danusantoso*, Dr Wia Melia*, Dr Janto G Lingga **, Dr Chawalit Natpratan***, Robert J Magnani***, Julietty Leksono***, Kekek Apriana*** * Indonesian Tuberculosis Control Association, Jakarta Branch, Indonesia ** Dr Sulianti Saroso Infectious Disease Hospital, Jakarta, Indonesia *** Family Health International – Indonesia, Aksi Stop AIDS Program

Outline of Presentation • • • Context Partners Background Program Outcome Recommendation

Context • Indonesia: 3 rd world rank re TB incidence • HIV epidemic: concentrated in MARGs • TB is observed: most common OI/co-infection reported in Indonesia (Mo. H), cause of 40% death among PLHA • Routine TB screening among PLHA has not been emphasized in National CST Guideline. But more often done • National TB-HIV coordination is stronger since 2007

Partners • Indonesian Tuberculosis Control Association (PPTI) – private non profit. TB clinic serving urban poor; popular among MARGs • Dr Sulianti Saroso Infectious Diseases Hospital (RSPI), Public Hospital in North Jakarta • FHI and donors (governmental, personal, private company, community associations)

Background • PPTI saw increasing non-specific PTB & EPTB and wondered ‘Could it be HIV? ’ • 2003: 10 TB-HIV (self reported by patients) • Early ‘ 04: capacity building efforts (FHIUSAID, IHPCP-Aus. AID) • 1 Sept 04: VCT service started at TB clinic, supported by FHI-USAID
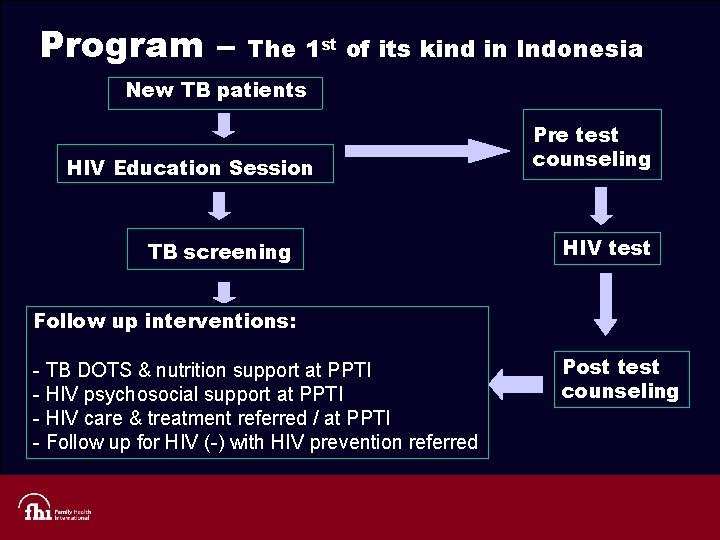
Program – The 1 st of its kind in Indonesia New TB patients HIV Education Session TB screening Pre test counseling HIV test Follow up interventions: - TB DOTS & nutrition support at PPTI - HIV psychosocial support at PPTI - HIV care & treatment referred / at PPTI - Follow up for HIV (-) with HIV prevention referred Post test counseling

Program (2) All TB-HIV cases: 1. 2. 3. 4. 5. 6. 7. Pay ID card 0. 5 USD + Chest X-Ray 3 USD (can be waived) Food supplement from WFP Free DOTS for 6 months from NTP. Free additional 3 months OAT (personal donors / adopters) Case management service (psychosocial support, home visit) Mobile DOTS dispensing (radius 70 km) Care & Treatment for HIV referred to nearby hospitals 2004. Starting February 2005, provided at PPTI 8. Secondary prophylaxis One-stop TB-HIV services for urban poor MARGs
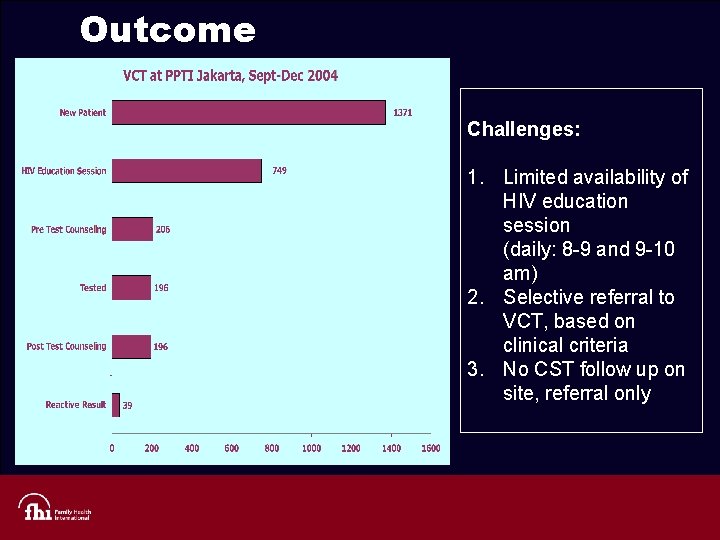
Outcome Challenges: 1. Limited availability of HIV education session (daily: 8 -9 and 9 -10 am) 2. Selective referral to VCT, based on clinical criteria 3. No CST follow up on site, referral only
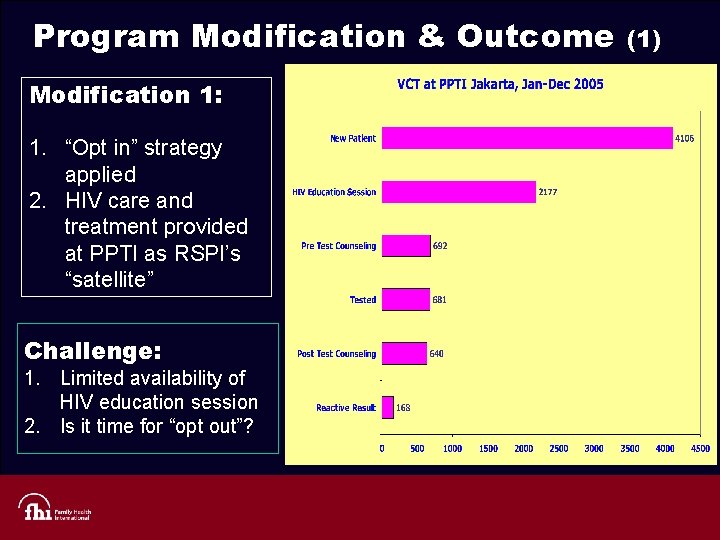
Program Modification & Outcome Modification 1: 1. “Opt in” strategy applied 2. HIV care and treatment provided at PPTI as RSPI’s “satellite” Challenge: 1. Limited availability of HIV education session 2. Is it time for “opt out”? (1)
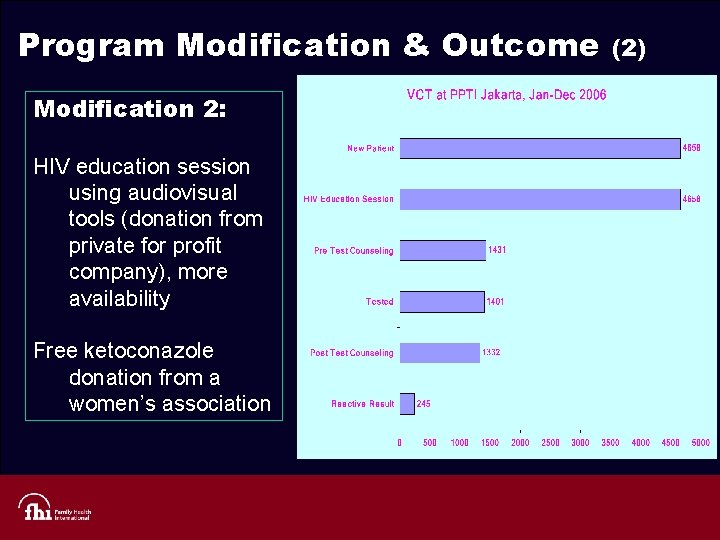
Program Modification & Outcome Modification 2: HIV education session using audiovisual tools (donation from private for profit company), more availability Free ketoconazole donation from a women’s association (2)
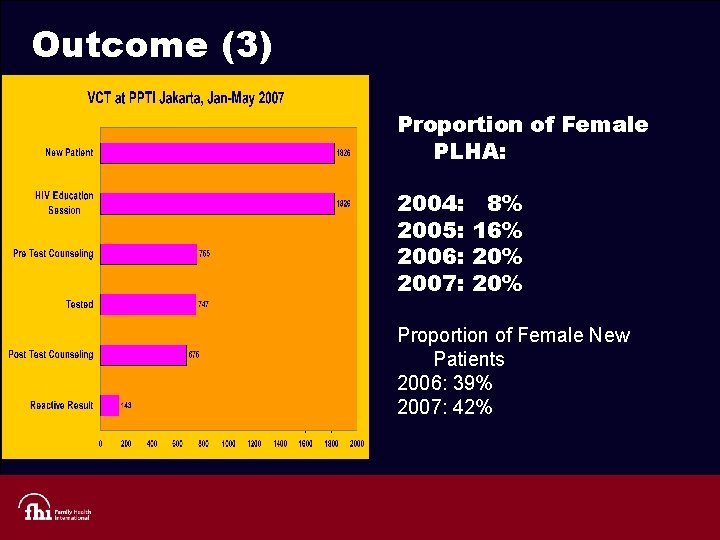
Outcome (3) Proportion of Female PLHA: 2004: 2005: 2006: 2007: 8% 16% 20% Proportion of Female New Patients 2006: 39% 2007: 42%

What’s next? • National Policy, Framework, and Guidelines are needed. • This model can become learning site for decision makers as well as other service providers • It is time for “opt out” strategy at PPTI and others of its kind • The model service should be brought to scale: serving patients’ best interest, comprehensiveness, responsiveness, multi-party collaboration under one roof and coordination mechanism
- Slides: 12