TBH V Coinfection by Dr Ker Hong Bee

TB-H V Co-infection by Dr. Ker Hong Bee 1

LEARNING OBJECTIVES • To know & understand about TB-HIV coinfection in relation to: – interaction & prevalence – diagnosis & treatment – Isoniazid Prophylaxis Therapy (IPT) – Highly Active Antiretroviral Therapy (HAART) – Immune Reconstitution Inflammatory Syndrome (IRIS) – Co-trimoxazole (CTX) Prophylaxis 2

TB & HIV: A DEADLY HUMAN SYNDEMIC TB is one of the leading causes of death among HIV patients 3
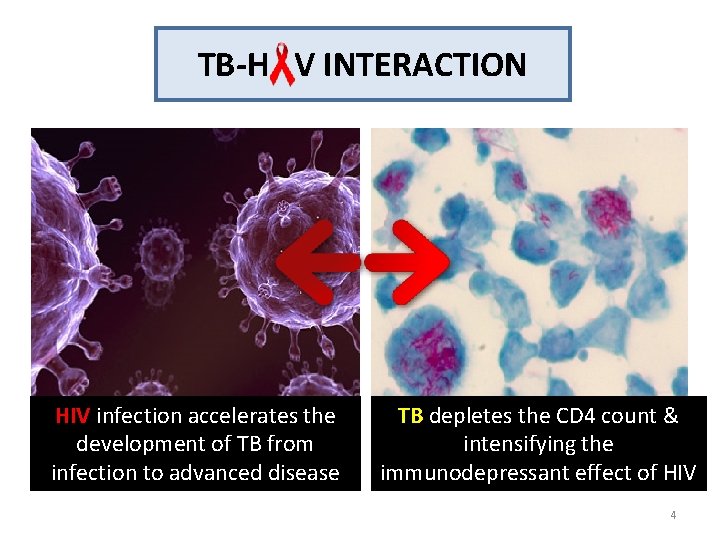
TB-H V INTERACTION HIV infection accelerates the development of TB from infection to advanced disease TB depletes the CD 4 count & intensifying the immunodepressant effect of HIV 4
TB-H V INTERACTION • HIV-positive patients have more than 2 x risk of primary MDR-TB. 1, 2 • Risk of mortality is 2. 6 x higher in HIV-positive patients who develop TB compared to those who do not. 3 1 Conaty SJ et al. , Epidemiol Infect, 2004 S et al. , PLo. S ONE, 2009 3 Straetemans et al. , PLo. S ONE, 2010 2 Suchindran 5

PREVALENCE OF TB-H V CO-INFECTION • At least one-third of HIV-positive persons worldwide are infected with MTB. • 8 - 10% of them develop clinical disease every year 1 1 Swaminathan S et al, Clin Infect Dis. 2010 6
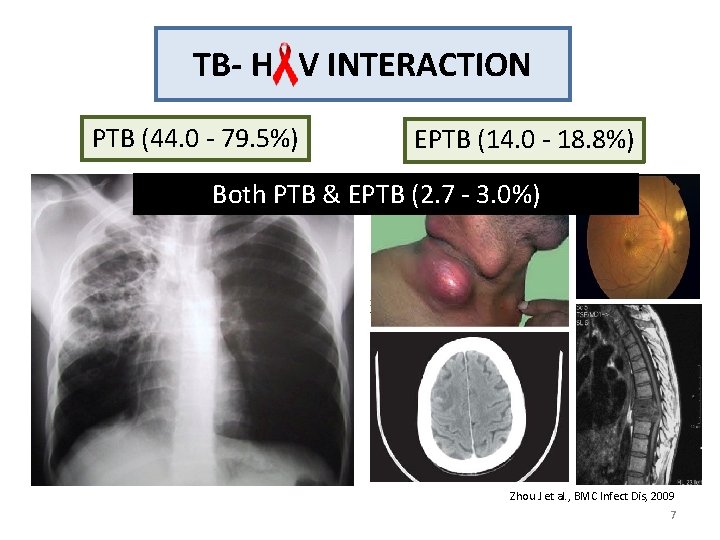
TB- H V INTERACTION PTB (44. 0 - 79. 5%) EPTB (14. 0 - 18. 8%) Both PTB & EPTB (2. 7 - 3. 0%) Zhou J et al. , BMC Infect Dis, 2009 7
DIAGNOSTIC CHALLENGES Many HIV-TB co-infected patients: • Have no cough & negative sputum AFB smears • Have lower AFB { } in sputum – AFB density in sputum decreases with decreasing CD 4 • Have normal CXR even in cultureconfirmed PTB • Have less cavitary disease on initial CXR 8
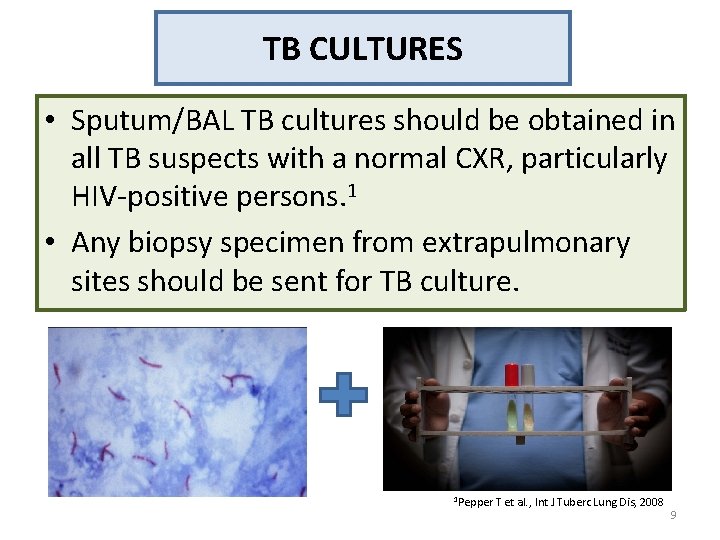
TB CULTURES • Sputum/BAL TB cultures should be obtained in all TB suspects with a normal CXR, particularly HIV-positive persons. 1 • Any biopsy specimen from extrapulmonary sites should be sent for TB culture. 1 Pepper T et al. , Int J Tuberc Lung Dis, 2008 9

DIAGNOSTIC TESTS 10

ANTITB FOR TB-H V CO-INFECTION • Require prompt initiation of TB treatment 1 • Treatment complicated by higher rate of TB relapse & increased mortality rate during treatment Panel on Antiretroviral Guidelines for Adults and Adolescents. Guidelines for the use of antiretroviral agents in HIV-1 -infected adults and adolescents. Department of Health and Human Services. 11 1

ANTITB FOR TB-H V CO-INFECTION • 6 month regimen consisting of 1, 2 – 2 EHRZ /4 HR when the disease is caused by organisms that are known or presumed to be susceptible to the first-line drugs 1 CDC. Guidelines for Prevention and Treatment of Opportunistic Infections in HIV-Infected Adults and Adolescents: 2 Blumberg HM et al, , Am J Respir Crit Care Med, 2003 12

ANTITB FOR TB-H V CO-INFECTION • Prolong the continuation phase if: – there is a slow or suboptimal response (e. g. cultures are still positive after 2 months of therapy) – patients with EPTB • All HIV patients should receive DAILY TB treatment in maintenance phase. 13

TREATMENT REGIMEN FOR TB-H V COINFECTION 14

RIFAMYCIN & ANTIRETROVIRAL (ARV) DRUGS • Includes rifampin (rifampicin) & rifabutin • Regimens in which rifampin is only used for the first 2 months higher rates of Rx failure & relapse 1 • Recommend to include rifamycin for the full course of TB treatment unless • the Mycobacterium is resistant to rifamycin • the patient has a severe side effect that is clearly due to the rifamycin 1 Jindani A et al. , Lancet, 2004 15

RIFAMYCIN & ARV DRUGS • Rifampicin: – the most potent inducer of CYP 450 system – significant interactions with most ARVs including all protease inhibitors (PIs) • Rifabutin* – has much less effect on drugs metabolism through the CYP 3 A system – as effective as rifampicin 1 *Not registered in Malaysia 1 Panel on Antiretroviral Guidelines for Adults and Adolescents. Guidelines for the use of antiretroviral agents in HIV-1 infected adults and adolescents. Department of Health and Human Services 16
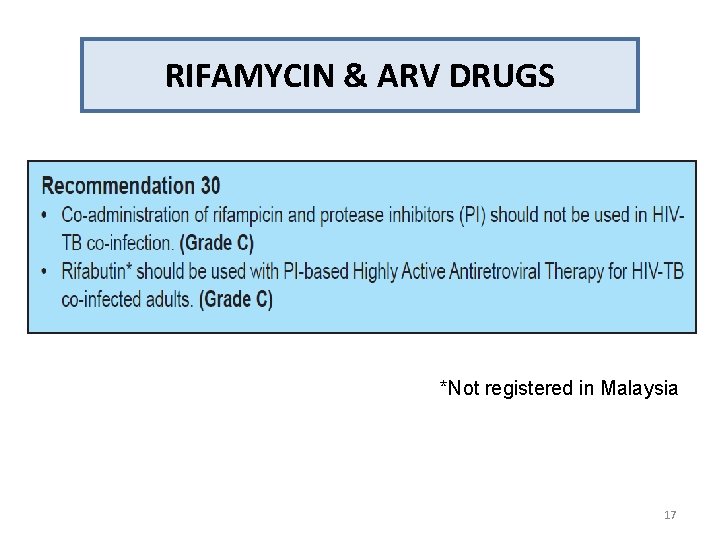

RIFAMYCIN & ARV DRUGS *Not registered in Malaysia 17
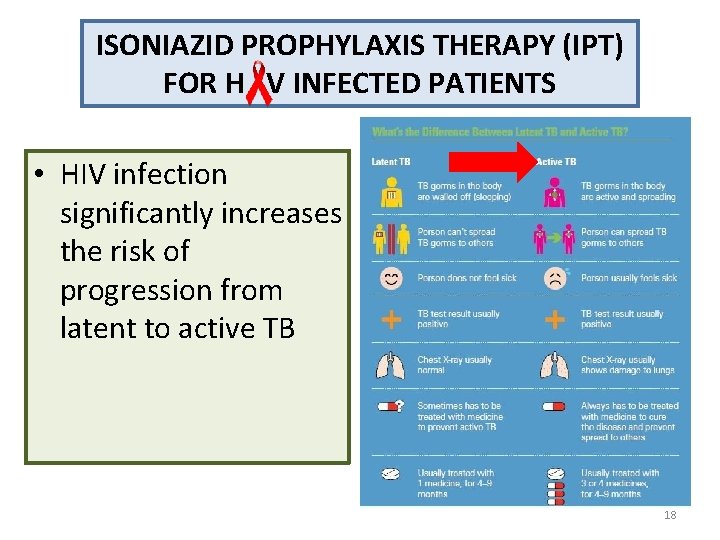
ISONIAZID PROPHYLAXIS THERAPY (IPT) FOR H V INFECTED PATIENTS • HIV infection significantly increases the risk of progression from latent to active TB 18
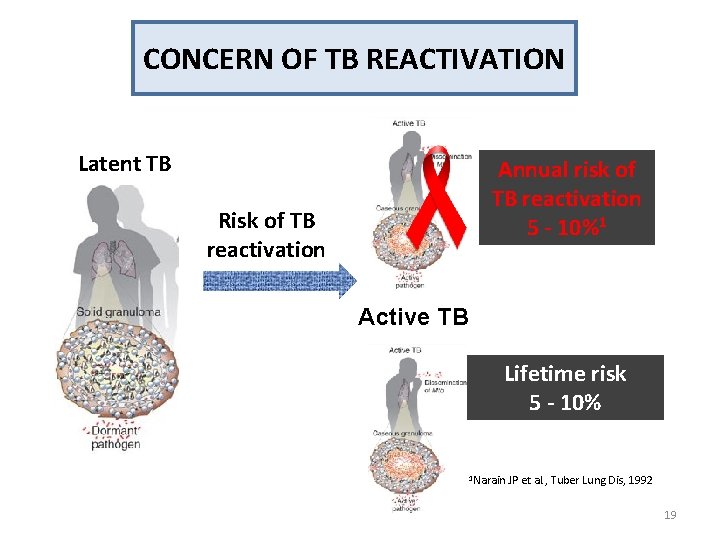
CONCERN OF TB REACTIVATION Latent TB Annual risk of TB reactivation 5 - 10%1 Risk of TB reactivation Active TB Lifetime risk 5 - 10% 1 Narain JP et al. , Tuber Lung Dis, 1992 19

IPT FOR H V INFECTED PATIENTS 20
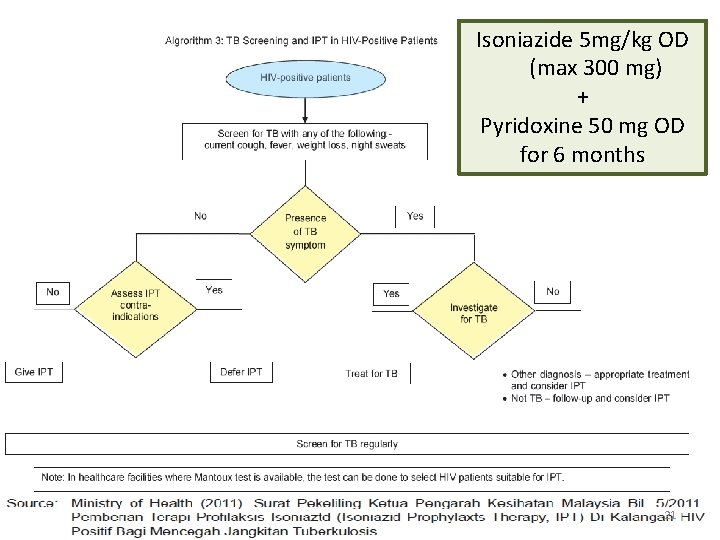
Isoniazide 5 mg/kg OD (max 300 mg) + Pyridoxine 50 mg OD for 6 months 21

ANTITB + HAART = SURVIVAL • Highly Active Antiretroviral Therapy (HAART) during TB treatment 1 o protective against mortality o result in earlier conversion of sputum & cultures to negative 1 Nahid P et al. , Am J Respir Crit Care Med, 2007 22

TIMING TO INITIATE HAART • Initiation of earlier-HAART in patients with CD 4 <50/cubic ml improves survival. 1 • In HIV-associated TB meningitis, immediate HAART is associated with an increase in grade 4 adverse events safer to defer HAART. 2 1 Abdool Karim SS et al. , N Engl J Med. 2011 ME et al. , Clin Infect Dis 2011 2 Torok 23
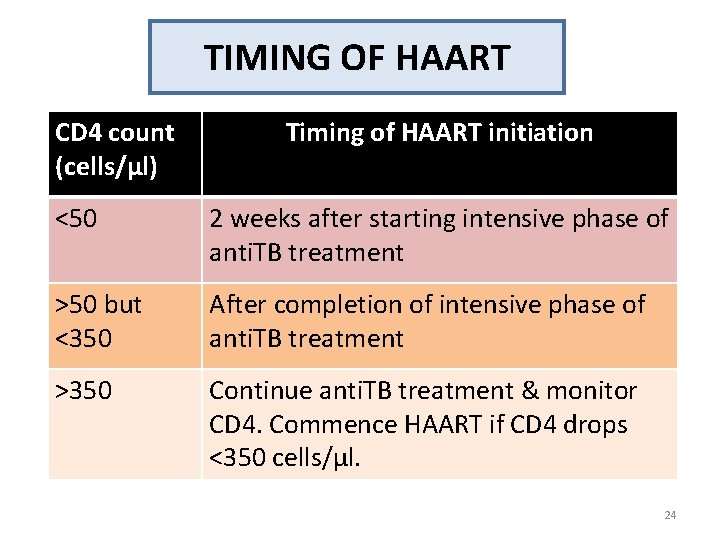
TIMING OF HAART CD 4 count (cells/µl) Timing of HAART initiation <50 2 weeks after starting intensive phase of anti. TB treatment >50 but <350 After completion of intensive phase of anti. TB treatment >350 Continue anti. TB treatment & monitor CD 4. Commence HAART if CD 4 drops <350 cells/µl. 24
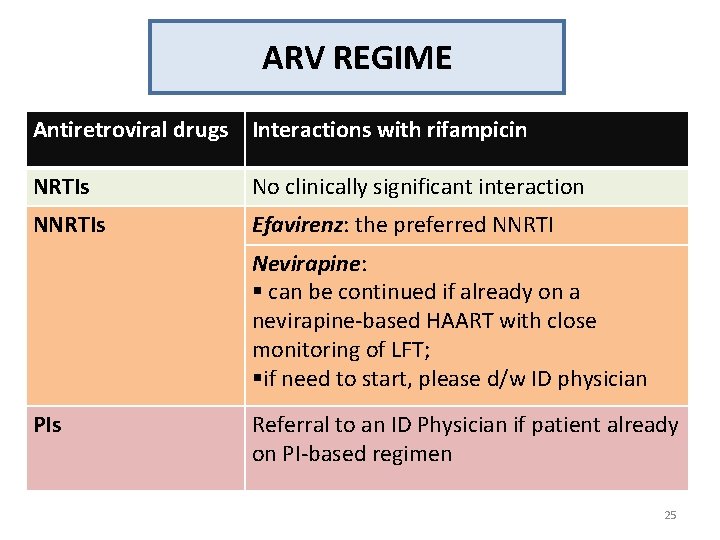
ARV REGIME Antiretroviral drugs Interactions with rifampicin NRTIs No clinically significant interaction NNRTIs Efavirenz: the preferred NNRTI Nevirapine: § can be continued if already on a nevirapine-based HAART with close monitoring of LFT; §if need to start, please d/w ID physician PIs Referral to an ID Physician if patient already on PI-based regimen 25

HAART IN H V-TB CO-INFECTION 26
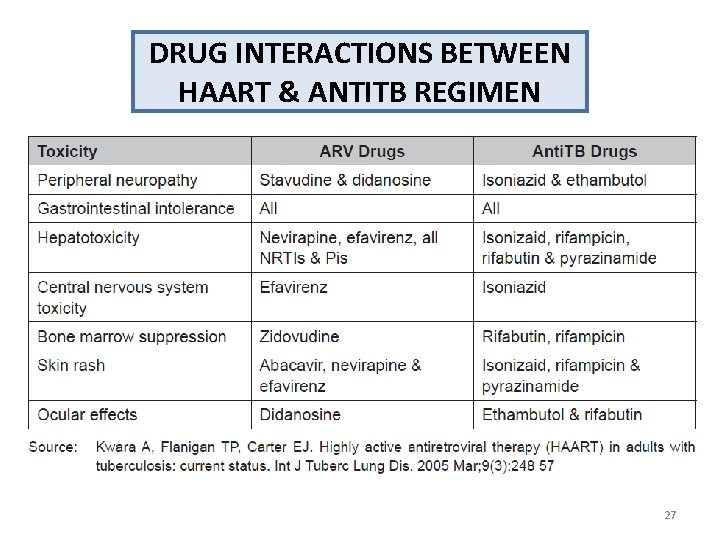

DRUG INTERACTIONS BETWEEN HAART & ANTITB REGIMEN 27

IMMUNE RECONSTITUTION INFLAMMATORY SYNDROME (IRIS) • An augmented inflammatory response that occurs in patients started on HAART & anti. TB • Usually occurs within 3 months of TB treatment o typically within 2 to 12 weeks after the initiation of HAART 28

IRIS • The major manifestations of IRIS are fever & lymphadenitis. 1 • HAART & anti. TB treatment should not be stopped while managing IRIS. 1 Dibyendu D et al. , Braz J Infect Dis 2011 29

CO-TRIMOXAZOLE (CTX) PROPHYLAXIS IN TB-H V CO-INFECTION • A RCT showed that CTX prophylaxis in TB-HIV co-infected adults was associated with a 21% reduction in all cause mortality. 1 • CTX is generally safe & well-tolerated. 1, 2 • CTX should be initiated as soon as possible & given throughout TB treatment. 3 1 Nunn 2 Boeree AJ et al. , BMJ, 2008 MJ et al. , Trop Med Int Health, 2005 3 WHO, 2010 30

TAKE HOME MESSAGES 1. Active TB should be ruled out in all HIV-positive patients. 2. Sputum TB culture should be done regardless of CXR/smear AFB status in TB-HIV suspect. 3. Anti. TB regimen offered to HIV +ve adults should be the same as for HIV -ve individual. o Caution on drug interaction with HAART o Daily maintenance phase 31

TAKE HOME MESSAGES 4. IPT for 6 months should be offered to all HIV patients with LTBI after ruling out active TB. 4. For patients with CD 4 <50 cells/μl, initiate HAART 2 weeks after starting anti. TB treatment. 4. CTX prophylaxis should be given to HIV patients on anti. TB treatment. 32

THANK YOU Økerhb@hotmail. com 33
- Slides: 33