Tallaght October 2010 Where Are We Now Margaret

Tallaght October 2010 Where Are We Now ? Margaret Bourke GP Coordinator

Partnership l This is the story of what I see as a very successful partnership to provide treatment to a very disadvantaged group in society. Also to bring dignity and caring to the workplace and to provide it to this cohort. Those of you who were here in the early days will remember when treatment was provided in less than ideal venues and we were not provided with a red carpet welcome and serious attempts were made to stop us providing treatment.

Addiction Is a chronic recidivist illness l The object should be a functioning lifestyle on treatment, with abstinence for those who can achieve it. l It is a disease of neuro chemical pathways. Specific opiate receptors have been identified. l

Changing Attitudes “Addictive disorders should be considered in the category with other disorders that require long-term or life long treatment. The treatment of addiction is about as successful as treatment of disorders such as hypertension, diabetes and asthma. It is clearly cost effective……. and as with treatment of these other chronic conditions there is no cure”

Background l l l The epidemic of heroin in the mid 1980 s and the explosion in the 1990 s which continues into the 21 st century has led to enormous problems with healthcare Addiction is an illness which needs treatment There is an increasing need to respond with a statutory duty to provide a multidisciplinary service

Advent of HIV l l Led to a demand for stabilization and maintenance treatment programs with methadone. In response, then Eastern Health Board set up services. (1992) What commenced as a HIV prevention programme rapidly became a response to the problem of heroin use. Increasing evidence of Hepatitis C in injecting drug users fueled the need for treatment.

Needle Exchange First Exchange 1988 l Statutory Services 10 l Back Packing l Out Reach l N G O large city centre N E funded by HSE and Private Donations l Tallaght JADD Oct. 2002, St. Aengus 203 l

Treatment Prior to 1992 most treatment was abstinence orientated l Prior to the Protocol most treatment was based in Central Services l Community a Number of Untrained Practitioners Prescribing for a Large Number of Patients l

Background Significant Heroin Problem l Problematic use concentrated in Dublin l Advent of HIV Epidemic led to a change in Policy l Harm Reduction Philosophy Embraced l Most Treatment Methadone Maintenance l

Central Service Addiction Treatment Centers l Satellite Clinics l Drug Treatment Centre l Prisons l Cuan Dara l

Central Treatment Services August 1992 first Addiction Treatment centers opened. There are now 23 centers in the Dublin area. l March 1995 first Satellite clinic opened in Tallaght. There are now 43 such clinics in the Dublin area. l The Drug Treatment Centre (Trinity Court) l

Addiction Treatment Centre More Challenging Patient Cohort ¨ Polydrug Use - Alcohol, Benzodiazepine, Cocaine ¨ Multidiscipliniary. Treatment Team ¨ On Site Dispensing ¨

Developments Treatment Centers l l l Have increased in number from the two opened in 1992 to twelve with the agreement of local communities. Staffed by G. P. S specialising in substance misuse working as part of a multidisciplinary team. All methadone is dispensed on site.

Satellite Clinics Partnership between Health Service and Communities ¨ Treatment Provided by Statutory Services ¨ Members of a Multidisciplinary Team attend on a sessional basis. ¨ Methadone Dispensed in Community Pharmacies ¨ Prescribers: General Practitioners Specialized in Substance Misuse ¨

Drug Treatment Center Board (DTCB) l l Staffed by Consultant Psychiatrists and NCHDs More difficult patients Serious psychiatric illness l Serious behavioral issues l l l Amacus service Temporary Transfer Patients where no service available in area Homelessness

Treatment Services Other HSE areas provide treatment l Not adequate, patient transfer difficult l Prisons, treatment provided to l l Those already in treatment l HIV positive l If agreed with HSE Addiction Services

Detox/ Abstinent Services Medical Supervision Cuan Dara: six week programme also stabilisation programme especially for those pregnant l Keltoi: Post detox three months l Link with other agencies l l Lantern l Cuan Mhuire l Coolmine l Simon Community (Alcohol Detox)

Treatment Provision l l A protocol for the prescribing of Methadone in the community was set up in October 1998. Treatment continues to be mainly centred in Dublin but has expanded to different areas of the country Prior to the protocol most treatment services were provided in Central Services. There were a number of untrained G. P. s prescribing for a large number of patients

Background ¨ March 1993 ¨ ¨ March 1995 ¨ ¨ Department of Health and Children (Do. HC) published a report on the establishment of a protocol for the prescribing of methadone A pilot project for the implementation of the protocol was commenced October 1998 ¨ Protocol which had been signed into law in July was implemented

Protocol Objectives To normalize patient attendance in community based services l To encourage G. P. s and Community Pharmacists to become involved in prescribing and dispensing methadone l To provide ongoing training and education for G. P. s and Pharmacists l

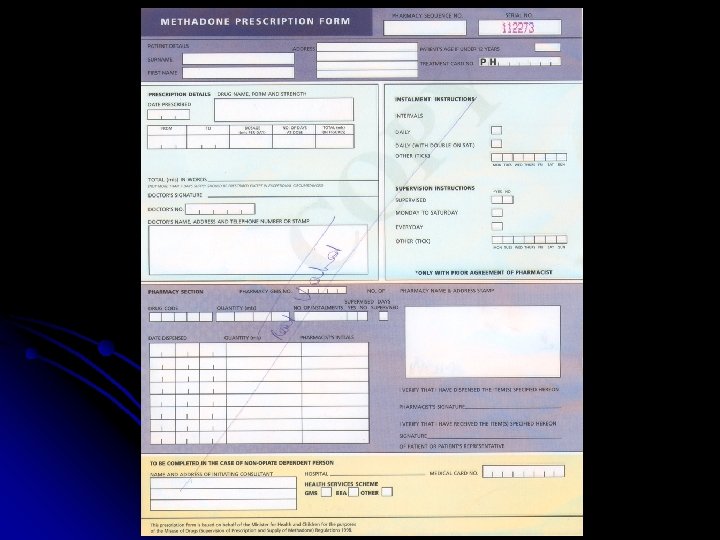
Protocol Structure Methadone is a controlled drug l Oral Methadone D. T. F 1 mg/ml is the only available preparation l Specific Protocol Prescriptions issued l Treatment Cards provided for each client and held at the designated pharmacy l

Treatment Card ¨ ¨ ¨ Name and Address of Patient Designated PH Number Photograph Name, Address and Tel of G. P and Pharmacist Signature of Patient

Structure l National Central Treatment List Established l Confidential l Access only by doctors and pharmacists Treatment is Free to all patients l Special Payments to G. P. s and Pharmacists l

Structure l Level I G. P. s l l Providing treatment for up to 15 stabilised patients Level II G. P. s Providing and/or initiating treatment for up to 35 less-stable patients l l Maximum of 50 patients per practice l l G. P. or Pharmacy Appointment of GP Coordinator and Liaison Pharmacist

GP Coordinator and Liaison Pharmacist l l l Encourage Community G. P. s and Pharmacists to prescribe and dispense methadone Initial and Ongoing Training and Education Provide ongoing support and back up to community G. P. s

Overview of Protocol ¨ Specialised Training for GPs and Pharmacists ¨ Guidelines issued by Irish College of General Practitioners ¨ Evidence based consistent with Eurometh Guidelines

On-Going Developments l l l On-Going Training for G. P. s and pharmacists Continuous Liaison and back-up services provided by GP Coordinator and Liaison Pharmacist Auditing of GP patient profile Initiation of patients by G. P. s (Level II) Transfer of stabilised patients to Level I G. P. s

Aim of Methadone Treatment l Reduce illegal heroin use l Improve Social stability l Reduce morbidity and death l Prevent transmission of blood borne viruses l Coincidently it reduces crime

Treatment Options - Medical Methadone Programmes l Detoxification associated with high relapse rates l Reduction Programme stabilisation and dose reduction over a period of six months or longer. l Maintenance Programmes The most evaluated treatment and probably the most successful l Counselling

Other Treatment Options Buprenorphine Substitution treatment available for a feasibility study l Lofexidine Used in Detoxification programmes l Naltrexone Used Post detoxification l

A blockade dose is the individual dose, which prevents : l Opioid abstinence syndrome including subjective symptoms of withdrawal as well as objective findings. l Reduction or elimination of drug hunger or craving. l The blockade of the euphoric effect of any illicitly self administered illegal drugs.

Blockade Dose l Blockade Dose is usually 80 mg + 20 mg. l Most patients blockade at 80 mg. l Patients with a high tolerance 90 mg – 120 mg. l About 7% of patients require a higher dose.

Side Effects of methadone Constipation l Antitussive effect l Myosis l Increased bladder tone l Overdose l Blushing l Itching l Sweating l Flushing. l Prolonged QTc l Respiratory depression l

Buprenorphine Partial mu agonist l Less respiratory depression l Quicker safer induction l Cost l Street diversion ( injected ) l

PROBLEMS IN STABLE PATIENTS Misuse of legally prescribed drugs l Use of illegal drugs l Alcohol l Increase in psychiatric illness l Pregnancy l Hepatitis C l HIV Infection l

Other Illegal Drugs of Misuse Cocaine l Ecstasy l Cannabis l Head Shop Substances l Methamphetamine l

Cocaine is a powerful and addictive central nervous system stimulant l Use leads to euphoric state known as a “high” l Neurobiological studies suggest it taps into the brain reward system l Increased use since 1998 as a ‘street drug’ l

Peak Concentrations Nasal inhalation - 5 to 20 minutes l Smoking: free based or as “crack” – seconds l Intravenous – seconds l

Ecstasy Use began in the late 1980 s with the advent of the Rave culture and emerged as a problem in the 1990 s. l Oral use, effects occur within 30 minutes can last for 4 hours. l Mood Change – Euphoric – Confident l “Crash”, severe lassitude and fatigue l

Cannabis Adolescent use can induce serious psychiatric illness l Affects concentration l Drop out l Do poorly in education l l Gateway

Head Shops l Still available, Mephadrone, BZP-derivatives, ‘Spice’, Skunk Under the counter l Street l Internet l l l Hallucinogenic: Mescaline and LSA compounds Kratom opioid agonist Salvia Magic Mint Sida Cordifolia ephedrine Caffeine with Guarana 100 times more potent injected

Methamphetamine U S Canada (Vancouver) l Eastern Europe Russia l Injecting culture l Meth Labs ( Mexico U S) l Pseudo ephedrine containing compound l Cough bottles (antihistamine) l

Misuse of prescription medications Benzodiazepines High rate of misuse in methadone maintained patient Misuse of Drugs Act 1993 Rohypnol, Temazepam. Report of Benzodiazapine Committee 2002 l Antidepressants Triptyzol, Prothiaden, Zispin l Antipsychotic medication olanzepine l Hypnotics Zimovane, Dalmane l

Misuse of OTCs l Codeine l New Pharmaceutical Society Guidance Aug 2010 Antihistamine l Cough Bottles l

ALCOHOL l l l l Most common ‘drug’ of misuse in Ireland Gateway Cross addiction is common May revert to alcohol when opiate stable Safe prescribing is necessary Acamprosate (Campral EC), Disulfiram (Antabuse) Detox Inpatient, Chlordiazepoxide (Librium)

HEALTH Poor health is common in this group of patients. l Lifestyle l Poverty l Immunosuppressive effect of opiates and cocaine.

Dual Diagnosis l Many with substance misuse have co-morbid psychiatric problems. l Increased level of symptoms in polydrug users. l Higher risk of suicides in this group of patients l Higher incidence of depression, some studies show 50% of opioid & cocaine users to report life time depression

Psychiatric Illness l Paranoia and Psychosis l Can be induced by ecstasy, cocaine, amphetamines l Personality Disorders

Pregnancy : Management l Prioritized access to treatment programmes l Stabilizing heroin addiction l Central l Services Maintaining stability l Prevents use cycling effects of unstable drug

HIV l 10 years after infection, 50% of patients have had a HIV related illness l 10 % of patients on M. M. in Dublin are HIV+ve l HIV related illness -

Treatment Long term chronic illness l Triple Therapy l Varying combinations of antiretrovirals appropriate to the individual l

Hepatitis C l 70 – 80% of drug users (Ireland) are Hepatitis C positive -75% asymptomatic -PCR positive – genotypes 1 and 3 l Cirrhosis - Alcohol End Stage Liver Disease Treatment – Pegylated Interferon/Ribavirin New treatments to come on stream in 2011 l l l

Hepatitis B All Health care professionals must have hepatitis B vaccinations l Hepatitis B vaccination protects you -bite -needle stick injury -blood splash l

Needle stick injury l Risk -HIV 0. 3% -Hepatitis B 40 – 60% (if patient E antigen +ve) -Geographical -Hepatitis C 5 -8% -risk dependant on degree of penetration -amount of blood inoculated l l Universal Precautions Treatment / PEP

Overdose l l l Higher risk 2 weeks following prison release Post detoxification Treatment induction Cocktail -benzodiazepine -alcohol -heroin/methadone Cocaine Ecstasy

Overdose l l l Greater risk in older persons, increased risk of death if injecting into the 30 s 69% of illicit drug users have experienced a non fatal overdose Homelessness Poly drug Use Depression Suicide

Overdose l Emergency assistance is sought in only 25 – 50% of cases -peer based management -CPR/ Naloxone (minijet) / Information leaflets

STUDY IN S. W. A. H. B. (Norway Europad) l l Retrospective analysis of data collected prior to and after the implementation of the protocol in specific postal districts of the SWAHB. The post implementation figures are between Oct 98 and May 02 Impact of the protocol on a deprived suburban area with a population of 90, 000 is also described. Numbers of patients now treated in General Practice are shown.

RESULTS G. P. participation increased by 185% l The number of Level One G. P. S increased by 157% l The number of Level Two G. P. S increased by 400% l There was an increase by 318% of patients treated at level one. l Increase by 255% of patients at level two There was a 95% increase in pharmacies dispensing to patients prescribed in general practice l
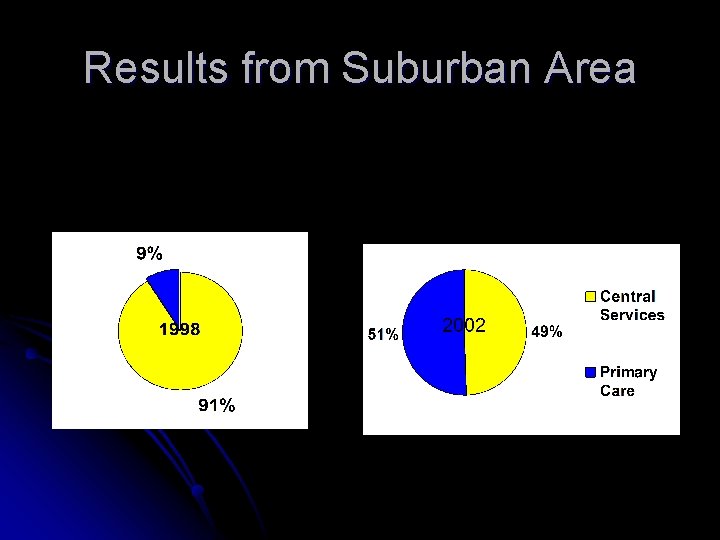
Results from Suburban Area
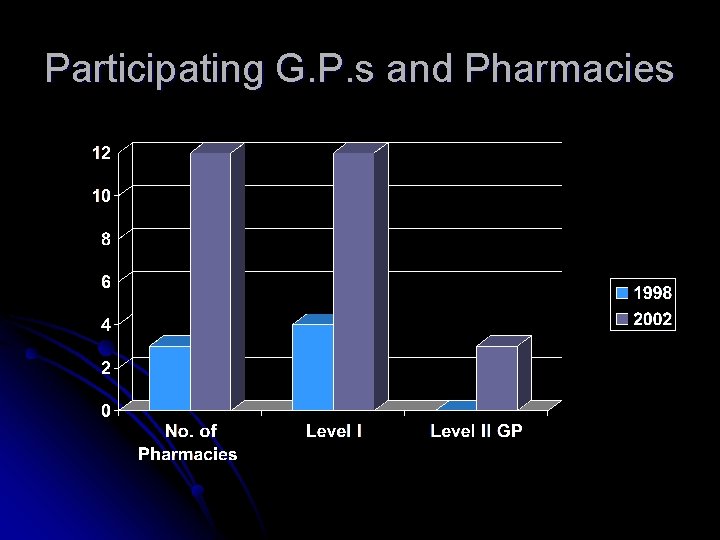
Participating G. P. s and Pharmacies

Conclusions 1998 - 2002 ¨ Significant Increase in number of Patients in Treatment ¨ Facilitated by Partnerships with Communities in Satellite Clinics ¨ Facilitated by implementation of Protocol enabling General Practitioners and Pharmacies to Prescribe and Dispense ¨

Tallaght Satellite Suburban City Population 100, 00 ¨ Explosive Building Expansion in the last 30 years ¨ Poor Amenities ¨ Crime ¨ Heroin ¨ Disempowered Communities ¨

Attempts to Implement Services Communities Disempowered by Addiction ¨ Community Fears around Treatment of Drug Users attracting undesirable antisocial behaviour ¨ “Not in my Backyard” Syndrome (NIMBY) ¨ Led to Opposition to Provision of Treatment ¨ Expressed through Anger, Marches ¨

Difficulties Communities were threatened by Treatment Services, perceived as Medicalization of “Heroin Problem” l Issues of Patient Confidentiality l Boundary Issues l

Relationship Building Consultation and Dialogue through Meetings ¨ Conflict Prevention ¨ Building Trust ¨ Strategy for Empowerment of Communities ¨ Conflict Resolution ¨

National Drug Task Force Set up in 1996 to ¨ Help Communities combat the Epidemic of Heroin Use ¨ Provide Funding for Local Community Projects ¨ Representation: Health Service Executive (HSE), Departments of Justice, Education, Enterprise and Employment ¨ Local Community and Voluntary Organisations

1996 June, first patient transferred to a Level 1 GP during the Protocol Pilot. ¨ 1996 November, first Satellite Clinic opened. ¨ 1997 March 1997 two further satellite clinics opened. ¨ 1998 October, an Addiction Treatment Centre opened as an evening service only. ¨ 1998 October, two farther satellites came under the umbrella of the HSE. ¨

2001 August a Mobile Bus service commenced as a Central Addiction Treatment Service. ¨ 2005 March a large Addiction Treatment Clinic. ¨ With the opening of this service the evening clinic and mobile clinic were incorporated into the Addiction Treatment Centre. ¨

Outcome Community partnerships with Health Services ¨ Catchment Service Provision ¨ Statutory Services Enabled to Provide Treatment ¨
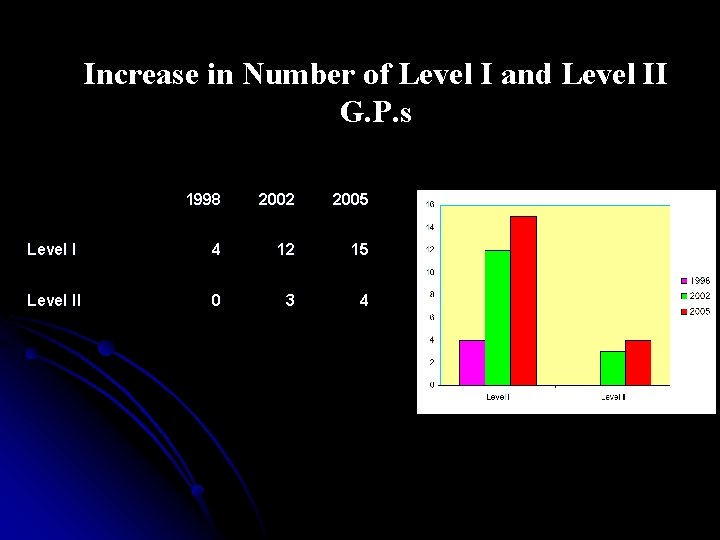
Increase in Number of Level I and Level II G. P. s 1998 2002 2005 Level I 4 12 15 Level II 0 3 4
Total number of patients in Treatment 1998 2002 2005 204 593 745
Total Number of Patients in Treatment in Community Practice Year Patients 1998 2002 2005 18 292 304
Total Number of Community Pharmacies Dispensing Year 1998 2002 2005 Pharmacy 3 12 15
Total Number of Patients in Central Services Year 1998 2002 2005 Central Services 186 286 422

2002 - 2005 ¨ Opening of Addiction Centre ¨ Further Expansion of Community General Practice and Pharmacy Service ¨ Led to enormous reduction in Waiting Lists and Increased Access to Treatment ¨ Use of Treatment Services to facilitate Employment and further education ¨

2005 to Date l l l Waiting time for treatment from Initial Assessment 2 to 3 weeks ---- administrative time Change in age profile Most patients re-applying for treatment (patients know to us) Referrals from Hospital and Prison Patients in Secondary / Tertiary Education accommodated regardless of stability unless difficult polydrug user not suitable for pharmacy Easy access to Hepatitis C treatment

Total Numbers in Treatment End of July 2010 Total number in treatment 9581 l Outside Dublin in clinics 321 l Prison 730 l Dublin DML and DNE Clinics 4641 l Drug Treatment Board 525 l Community Practice DML and DNE 3100 l Community Practice (outside Dublin) 565 l Number in Pharmacies Dublin 4999 l

Numbers in Treatment in Tallaght End of July 2010 l l l l Number in Addiction Treatment Center 249 Number in Satellite Clinics 250 Number in Community Practice 314 Number dispensed in Pharmacies 564 Level I G. P. s 16, Level II G. P. s 4 Number of community pharmacies in Tallaght 15 Number of fringe pharmacies 4
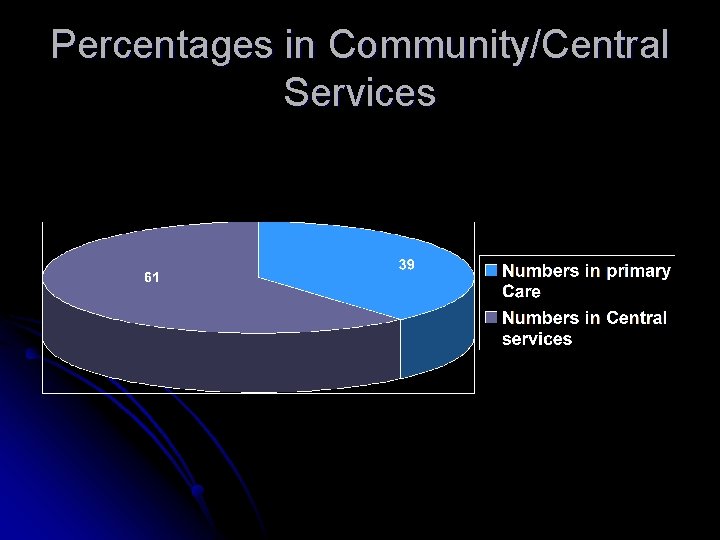
Percentages in Community/Central Services

Applications for treatment Vast majority are people who have previously been in treatment l A number of treatment naive persons over 40 have applied in past 12 months l Few applications for treatment persons under 25 l Age profile older l

Homelessness l l Greater prevalence of substance use among the homeless population Predominant public health issue in this cohort Higher incident of psychiatric co-morbidity Particular difficulties in treatment provision -residential instability -poor economic and employment status -social disaffiliation

Services l l l Structure on provision of service by Multi Disciplinary Health Link Team in Dublin City South Once clients linked remain even if transferred to another area Advocacy and contact with voluntary services e. g. Simon Community and statutory agencies Transitory homeless residency Transfer to city

Caring l l Addiction is an illness which needs to be treated Only by working with drug users and trying to understand the risks they run can we begin to be accepted by them in a caring role and so be in a position to engage with them. We need to help patients who wish to deal with their drug habit, we do not refuse to treat alcoholics or nicotine dependant patients so why judge opiate dependant patients? Patience and flexibility are a necessary component of this work. A non confrontational, non judgmental, caring approach is very important.
- Slides: 85