Take Action Against Acute Liver Failure By Gloria
Take Action Against Acute Liver Failure By Gloria J. Gdovin, RN, CCRN, TNCC, MSN Nursing made Incredibly Easy! September/October 2009 2. 3 ANCC contact hours Online: www. nursingcenter. com © 2009 by Lippincott Williams & Wilkins. All world rights reserved.

Statistics ¡ Affects 2, 000 Americans each year ¡ Mortality is as high as 80%; in the absence of liver transplantation, patients with nondrug-induced acute liver failure will either completely recover or die within days ¡ Prognosis is especially poor for patients younger than age 10 and those over age 40 ¡ Outcomes are worsened with obesity ¡ Increased risk in patients with diabetes
The Liver ¡ Located in the right upper quadrant of the abdomen ¡ The largest internal organ; has a dual blood supply ¡ Divided into left and right lobes; right lobe further divided into caudate and quadrate lobes ¡ Within the lobes are lobules consisting of hepatocytes, or liver cells ¡ Critical functions: • Bile production • Metabolic detoxification • Metabolism of nutrients, vitamins, and minerals • Synthesis and deactivation of clotting factors
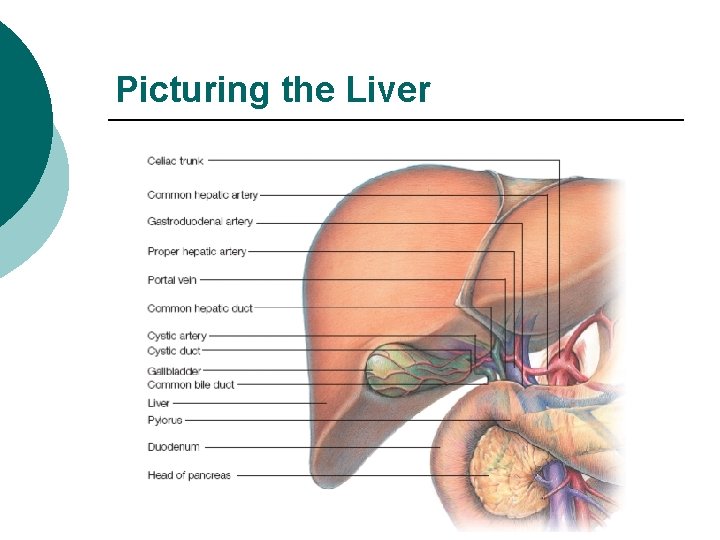
Picturing the Liver
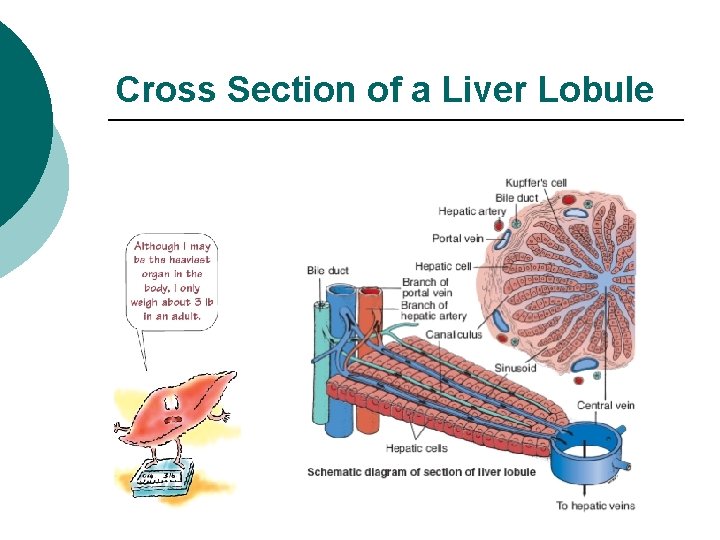
Cross Section of a Liver Lobule

Acute Liver Failure ¡ Characterized by massive necrosis of hepatocytes ¡ The liver is initially enlarged during the acute inflammatory stage; ultimately, it atrophies as hepatocellular necrosis advances ¡ Defined by the American Association for the Study of Liver Diseases as: • evidence of coagulation abnormality • usually an international normalized ratio greater than or equal to 1. 5 • any degree of mental alteration (encephalopathy) in a patient without preexisting cirrhosis and with an illness of less than 26 weeks’ duration

Hepatic Encephalopathy ¡ May consist of reversible metabolic encephalopathy, brain atrophy, cerebral edema, or any combination of these ¡ Mechanisms may include the effects of cerebral edema, impaired cerebral perfusion, and impairment of neurotransmitter systems ¡ Metabolic factors are also implicated, especially ammonia and impaired circulation of amino acids ¡ Ammonia is considered the primary neurotoxin precipitating hepatic encephalopathy; levels are increased in approximately 90% of patients experiencing this symptom

Drug Toxicity and Other Causes ¡ Acetaminophen toxicity is the leading cause of acute liver failure ¡ The second leading cause of acute liver failure is idiosyncratic drug reactions ¡ Other causes include: • Infection • Injury • Parenchymal disease • Vascular abnormalities (Budd-Chiari syndrome) • Fatty liver of pregnancy • Primary graft nonfunction following liver transplant

Signs and Symptoms ¡ Fatigue ¡ Dark urine ¡ Weakness ¡ Light-colored stools ¡ Nausea ¡ Itching ¡ Anorexia ¡ Right upper quadrant pain ¡ Malaise ¡ Bloating ¡ Jaundice

Advanced Signs and Symptoms ¡ ¡ Hyperventilation, respiratory alkalosis, and respiratory failure Hepatic encephalopathy with rapid progression to hepatic coma ¡ Profound coagulopathy ¡ Hypoglycemia ¡ Hepatorenal syndrome (reversible acute renal failure brought on by acute liver failure) ¡ Sepsis with metabolic acidosis ¡ Intracranial hypertension and brainstem herniation ¡ Hyperdynamic circulation (an increase in BP and pulse, often leading to sinus tachycardia) ¡ Systolic ejection murmur ¡ Eventual cardiovascular collapse

Diagnostic Tests ¡ Lab studies will show: • Increased liver enzymes • Increased blood urea nitrogen and creatinine levels; decreased glucose level • Prolonged prothrombin time and international normalized ratio • Decreased hemoglobin and hematocrit, along with a decrease in white blood cells ¡ Body fluid cultures, serologic hepatitis tests or autoimmune markers, urine toxicology screens, tests to ascertain HIV status, and stool guaiac tests may be ordered ¡ Chest X-rays, computed tomography scans, and cerebral perfusion scans may also be ordered

Pharmacologic Management ¡ Prompt administration of N-acetylcysteine should be performed for acetaminophen overdose; carnitine should be administered for valproate overdose ¡ Elevated ammonia levels will require the administration of lactulose ¡ Signs of infection or sepsis require the prompt administration of antibiotics ¡ Stress ulcer prophylaxis should be initiated ¡ Fresh frozen plasma is indicated for active hemorrhage

Other Treatments ¡ For associated renal failure: Hemodialysis ¡ For hepatorenal syndrome: Administration of sympatholytic agents to reduce renal vascular tone and renal vascular resistance and norepineprine with albumin infusions to increase mean arterial pressure ¡ For refractory ascites: Transjugular intrahepatic portosystemic shunt ¡ For bleeding from esophageal or gastric varices: esophagogastroduodenoscopy and sclerotherapy; octreotide and vasopressin
Liver Transplantation ¡ Most common, and successful, treatment available for acute liver failure patients. ¡ Survival rate is 65% to 80% ¡ Transplant liver from cadaver or living donor ¡ Living donor gives 60% of liver; matched by age, size, and blood type (usually donor is between ages 21 and 45) ¡ Postop period includes monitoring for primary functioning of the liver, improvement in mentation and lab results, and signs of infection
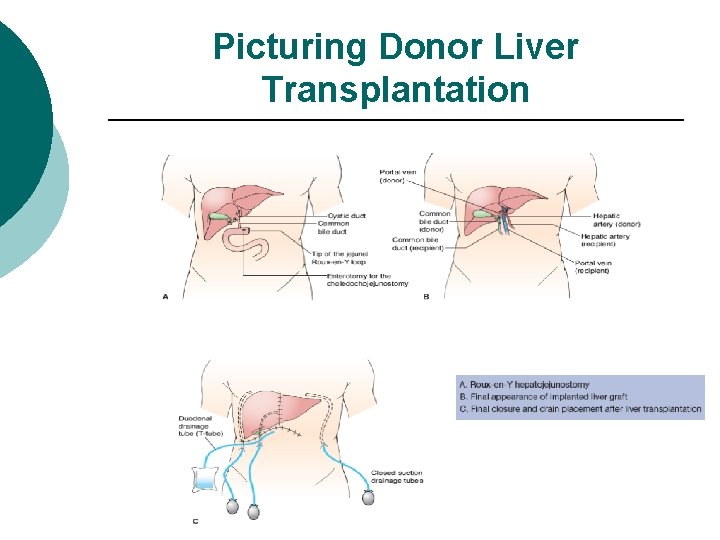
Picturing Donor Liver Transplantation

Patient Care ¡ Patient should be monitored in the ICU and contact with a transplant center made ¡ Goals of care include: • Optimize liver function • Monitor and treat complications correct metabolic abnormalities • Stabilize the patient for liver transplant, if appropriate

Patient Care ¡ Complete a thorough history on admission, including the patient’s risk factors for liver disease and a timeline outlining the onset of signs and symptoms ¡ Assessment should include identification of any of the following: • Jaundice • Spider angiomata • Bruising or hematomas • Changes in mental status • Splenomegaly or hepatomegaly • Ascites

Patient Care ¡ Monitor for any normalization or worsening of liver, kidney, and neurologic functions and vital signs ¡ Monitor for signs of coagulopathy and provide corrective treatments, as ordered ¡ Assess for signs of infection or active and occult bleeding ¡ Observe for signs of multiple organ failure, which may occur secondary to sepsis ¡ Maintain scrupulous infection control practices to prevent hospital-acquired infection

Patient Care ¡ Position the patient with the head of the bed at 30 degrees for prevention or treatment of elevated ICP ¡ Monitor skin integrity for breakdown and reposition the patient frequently per your facility’s policy ¡ Maintain scrupulous skin care and protection to guard against scratching due to the itching of jaundice ¡ Maintain nutrition through the use of special enteral and parenteral solutions; control protein intake ¡ Mechanical ventilation may be needed for the patient with hepatic enchepalopathy

Patient Care ¡ Meeting the psychosocial needs of the patient and his family is essential due to the profound acuity of the illness ¡ Discuss the potential need for transplant and end-of-life care ¡ Collaboration with social and chaplancy services may be helpful ¡ Ongoing psychosocial support should be provided, especially if the patient’s condition deteriorates or if he doesn’t respond to treatment
- Slides: 20