Systemic lupus erythematosus SLE is multisystem pleomorphic disease

















- Slides: 19

Systemic lupus erythematosus

SLE is multisystem, pleomorphic disease in which inflammation, antibody production and complement-fixing immune complex deposition result in tissue damage Types of lupus erythematosus: 1) cutaneous lupus 2) systemic lupus erythematosus 3) drug-induced lupus erythematosus 4) neonatal lupus erythematosus

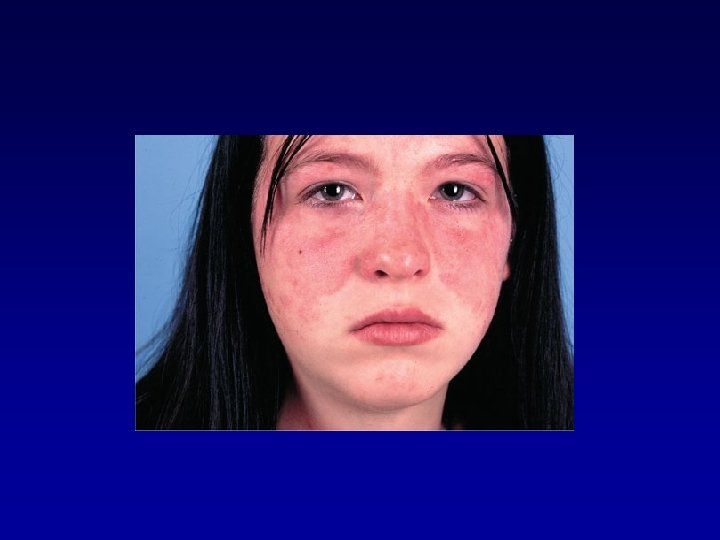
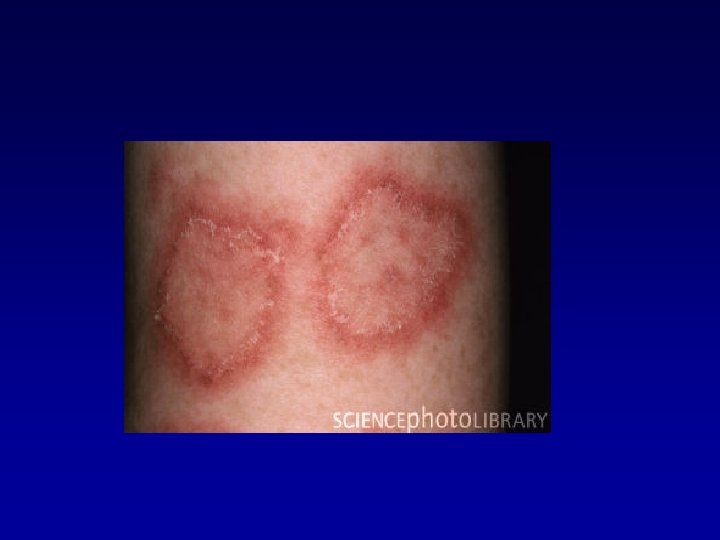
The American College of Rheumatology revised criteria 1. Malar rash 2. Discoid rash 3. Photosensivity 4. Oral ulcers 5. Arthritis 6. Serositis: pleuritis or pericarditis 7. Renal disorder: persistent proteinuria >0, 5 g/day or cellular casts of any type 8. Neurologic disorder 9. Hematologic disorder: hemolytic anemia or leukopenia<4000, lymphopenia <1500 or thrombocytopenia<100000 10. Antinuclear antibodies test positive; 11. Immunologic disorder: Positive anti-Smith, anti-ds DNA, antiphospolipid antibody



2012 SLICC SLE Criteria • Requirements : 4 or more criteria ( at least 1 clinical and 1 labolatory criteria) • Or • Biopsy- proven lupus nephritis with positive ANA or Anti-DNA

Clinical criteria • 1. Acute cutaneous lupus • 2. Chronic cutaneous lupus • 3. Oral or nasal ulcers • 4. Non- scaring alopecia • 5. Arthritis • 6. Serositis • 7. Renal • 8. Neurologic • 9. Hemolytic anemia • 10. Leukopenia • 11. Thrombocytopenia (<100 000/mm 3)

Immunologic Criteria • 1. ANA • 2. Anti-DNA • 3. Anti- Sm • 4. Antiphospholipid Ab • 5. Low complement (C 3, C 4, CH 50) 6. Direct Coombs’ test ( do not count in the presence of hemolytic anemia)

Sex. Lupus is more common in women. Age. Although lupus affects people of all ages, it's most often diagnosed between the ages of 15 and 40. Race. Lupus is more common in African Americans, Hispanics and Asians. Diagnosing lupus is difficult because signs and symptoms vary considerably from person to person. Signs and symptoms of lupus may vary over time and overlap with those of many other disorders. No one test can diagnose lupus. The combination of blood and urine tests, signs and symptoms, and physical examination findings leads to the diagnosis.

Laboratory tests Complete blood count. This test measures the number of red blood cells, white blood cells and platelets as well as the amount of hemoglobin, Erythrocyte sedimentation rate Kidney and liver assessment Urinalysis Antinuclear antibody (ANA) test- the most sensitive screening test for evaluation the most widely used method is indirect immunofluorescence. The pattern of fluorescence suggests the type of antibody present in the patient's serum. ANA screening yields positive results in many connective tissue disorders and other autoimmune diseases, and may occur in normal individuals.

Subtypes of antinuclear antibodies include anti-Smith and antidouble stranded DNA (ds. DNA) antibodies (which are linked to SLE) and anti-histone antibodies (which are linked to drug-induced lupus). Anti-ds. DNA antibodies are highly specific for SLE; they are present in 70% of cases, whereas they appear in only 0. 5% of people without SLE. [2] The anti-ds. DNA antibody titers also tend to reflect disease activity, although not in all cases. [2] Other ANA that may occur in SLE sufferers are anti-U 1 RNP, SS-A (or anti-Ro) and SSB (or anti-La; both of which are more common in Sjögren's syndrome). SS-A and SS-B confer a specific risk for heart conduction block in neonatal lupus.

Other tests routinely performed in suspected SLE are complement system levels (low levels suggest consumption by the immune system), Chest X-ray Echocardiogram Biopsy

LUPUS NEPHRITIS • In the US approximately 35% of adults with SLE have clinical evidence of nephritis at the time of diagnosis, with an estimated total of 50 -60% developing nephritis during the first 10 years of disease. • The presence of LN significantly reduces survival to approximately 88% at 10 years ( without is 92%)

SLE is considered incurable, but highly treatable. In the 1950 s, most people diagnosed with SLE lived fewer than five years. Advances in diagnosis and treatment have improved survival to the point where over 90% now survive for more than ten years, and many can live relatively asymptomatically. Prognosis is normally worse for men and children than for women; however, if symptoms are present after age 60, the disease tends to run a more benign course. Early mortality, within 5 years, is due to organ failure or overwhelming infections, both of which can be modified by early diagnosis and treatment. The mortality risk is fivefold when compared to the normal population in the late stages, which can be attributed to cardiovascular diseases acquired from corticosteroid therapy. To reduce potential for cardiovascular issues, high blood pressure and high cholesterol should be prevented or treated aggressively. Steroids should be used at the lowest dose for the shortest possible period, and other drugs that can reduce symptoms should be used whenever possible.

Treatment for lupus depends on signs and symptoms. Medications most commonly used to control lupus include: Corticosteroids (side-effects: osteoporosis, elevated blood pressure, cataracts weight gain, easy bruising, diabetes and increased risk of infection. The risk of side effects increases with higher doses and longer term therapy. Disease-modifying antirheumatic drugs a) antimalarials such as Hydroxychloroquine ( plaquenil ) - Side effects can include stomach upset and, very rarely, damage to the retina of the eye b) immunosuppressants (e. g. methotrexate and azathioprine (Imuran), leflunomide (Arava) ) c) Cyclophosphamide is used for severe glomerulonephritis or other organ-damaging complications. d) Mycophenolic acid is also used for treatment of lupus nephritis

a) Intravenous immunoglobulins may be used to control SLE with organ involvement, or vasculitis. It is believed that they reduce antibody production or promote the clearance of immune complexes from the body, even though their mechanism of action is not well-understood. [64] Unlike immunosuppressives and corticosteroids, IVIGs do not suppress the immune system, so there is less risk of serious infections. b) Belimumab

Lifestyle changes Avoiding sunlight is the primary change to the lifestyle of SLE sufferers, as sunlight is known to exacerbate the disease, as is the debilitating effect of intense fatigue. These two problems can lead to patients becoming housebound for long periods of time. Drugs unrelated to SLE should be prescribed only when known not to exacerbate the disease. Occupational exposure to silica, pesticides and mercury can also make the disease worsen.

Systemic lupus erythematosus and pregnancy Pregnant mothers with SLE should remain under medical care until delivery. Women pregnant and known to have anti-Ro (SSA) or anti-La antibodies (SSB) often have echocardiograms during the 16 th and 30 th weeks of pregnancy to monitor the health of the fetus’s heart The overall live-birth in SLE patient has been estimated to be 72% Contraception and other reliable forms of pregnancy prevention is routinely advised for women with SLE, since getting pregnant during active disease was found to be harmful. Lupus nephritis was the most common manifestation.

Drug-induced lupus erythematosus is a (generally) reversible condition that usually occurs in people being treated for a longterm illness. Drug-induced lupus mimics SLE. However, symptoms of drug-induced lupus generally disappear once the medication that triggered the episode is stopped. More than 38 medications can cause this condition, the most common of which are procainamide, isoniazid, hydralazine, quinidine, and phenytoin. Other: inliximab, etanercept, isoniazid, carbamazepine, minocycline, pyrazinamide, chlorpromazine, minoxidil.