SYSTEMIC LUPUS ERYTHEMATOSUS SLE By Rian Asmeida Farha

SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) By: Rian Asmeida Farha binti Ahmad Rejab Wan Fadhilah binti Wan Ibrahim

INTRODUCTION Systemic lupus erythematosus (SLE) is a chronic autoimmune disease that can be fatal; however, with recent medical advances, fatalities are becoming increasingly rare. The immune system attacks the body’s cells and tissue, resulting in inflammation and tissue damage. SLE can affect any part of the body, but most often harms the heart, joints, skin, lungs, blood vessels, liver, kidneys, and nervous system. Lupus can occur at any age, and is most common in women, particularly of non-European descent.

EPIDEMIC About 90% of SLE sufferers are women while about 10% are men and children. About 90% of women with SLE are in their childbearing years, within the range of 15 to 50 years old. Ratio of SLE sufferers : In the West, among Afro-Carribeans 1 in 250 -500 people USA - 1 in 2, 000 people China - 1 in 1, 000 people In Malaysia, it is estimated that more than 10, 000 people have been diagnosed with SLE over the past 30 years. However, this number may be only the tip of the iceberg. The Malaysian SLE Association believes that there are many more SLE sufferers in Malaysia who have not been diagnosed.
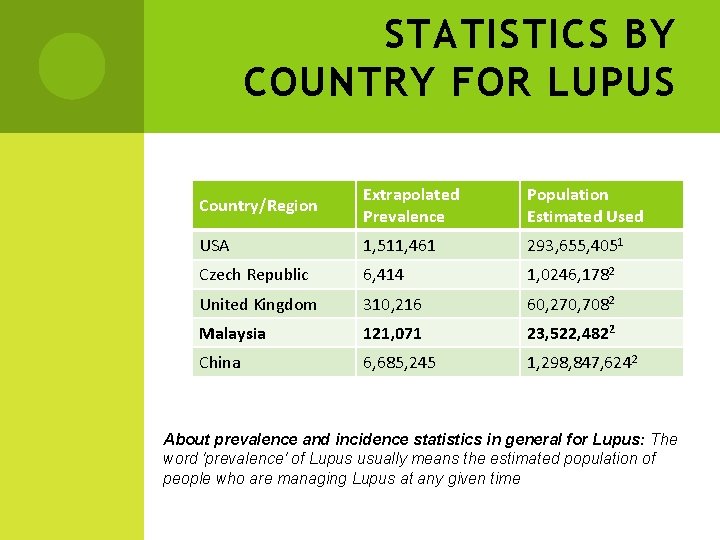
STATISTICS BY COUNTRY FOR LUPUS Country/Region Extrapolated Prevalence Population Estimated Used USA 1, 511, 461 293, 655, 4051 Czech Republic 6, 414 1, 0246, 1782 United Kingdom 310, 216 60, 270, 7082 Malaysia 121, 071 23, 522, 4822 China 6, 685, 245 1, 298, 847, 6242 About prevalence and incidence statistics in general for Lupus: The word 'prevalence' of Lupus usually means the estimated population of people who are managing Lupus at any given time

ETIOLOGY The cause(s) of lupus is currently unknown, but there are environmental and genetic factors involved. Some environmental factors which may trigger the disease include : Ø Infections Ø antibiotics (especially those in the sulfa and penicillin groups) Ø ultraviolet light Ø extreme stress Ø certain drugs Ø hormones.

SYMPTOMS PERCENTAGE (%) Achy joints / arthralgia 95 Fever of more than 100 degrees F / 38 degrees C 90 Arthritis / swollen joints 90 Prolonged or extreme fatigue 81 Skin Rashes 74 Anemia 71 Kidney Involvement 50 Pain in the chest on deep breathing / pleurisy 45 Butterfly-shaped rash across the cheeks and nose 42 Sun or light sensitivity / photosensitivity 30 Hair loss 27 Abnormal blood clotting problems 20 Fingers turning white and/or blue in the cold 17 Mouth or nose ulcers 12
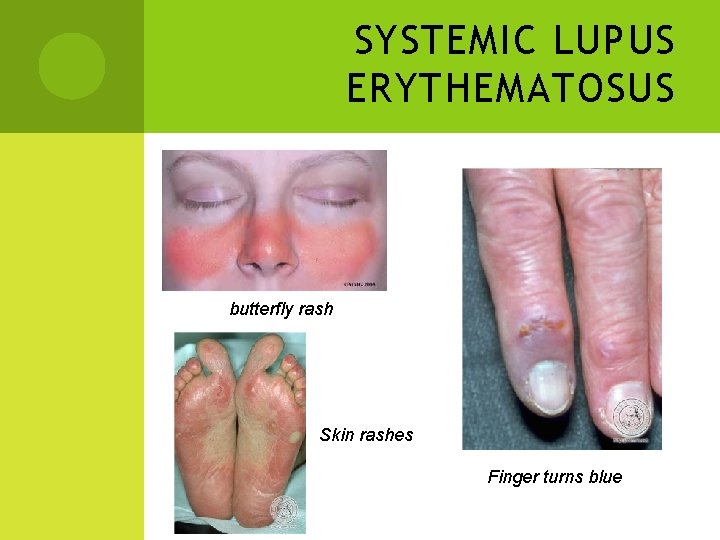
SYSTEMIC LUPUS ERYTHEMATOSUS butterfly rash Skin rashes Finger turns blue

DIAGNOSIS Criterion Definition Malar Rash over the cheeks Discoid Rash Red raised patches Photosensitivity Reaction to sunlight, resulting in the development of or increase in skin rash Oral Ulcers in the nose or mouth, usually painless Arthritis Nonerosive arthritis involving two or more peripheral joints (arthritis in which the bones around the joints do not become destroyed) Serositis Pleuritis or pericarditis (inflammation of the lining of the lung or heart) Renal Disorder Excessive protein in the urine (greater than 0. 5 gm/day or 3+ on test sticks) and/or cellular casts (abnormal elements the urine, derived from red and/or white cells and/or kidney tubule cells)

DIAGNOSIS Criterion Definition Neurologic Seizures (convulsions) and/or psychosis in the Disorder absence of drugs or metabolic disturbances which are known to cause such effects Hematologic Hemolytic anemia , leukopenia , lymphopenia or Disorder thrombocytopenia. The leukopenia and lymphopenia must be detected on two or more occasions. The thrombocytopenia must be detected in the absence of drugs known to induce it. Antinuclear Positive test for antinuclear antibodies (ANA) in the Antibody absence of drugs known to induce it. Immunologic Positive anti-double stranded anti-DNA test, Disorder positive anti-Sm test, positive antiphospholipid antibody such as anticardiolipin, or false positive syphilis test (VDRL). Adapted from: Tan, E. M. , et. al. The 1982 Revised Criteria for the Classification of SLE. Arth Rheum 25: 1271 -1277.

BLOOD TESTS IN THE DIAGNOSIS OF SLE The anti-nuclear antibody test (ANA) to determine if autoantibodies to cell nuclei are present in the blood. The anti-DNA antibody test to determine if there antibodies to the genetic material in the cell. The anti-Sm antibody test to determine if there antibodies to Sm, which is a ribonucleoprotein found in the cell nucleus. Tests to examine the total level of serum (blood) complement (a group of proteins which can be consumed in immune reactions), and specific levels of complement proteins C 3 and C 4.

TREATMENTS Drug therapy nonsteroidal anti-inflammatory drugs and antimalarials Disease-modifying antirheumatic drugs (DMARDs) Immunomodulating Drugs Anticoagulants Lifestyle changes avoiding direct sunlight, covering up with sun-protective clothing, and using strong UVA/UVB sunblock lotion can also be effective in preventing photosensitivity problems. Weight loss is also recommended in overweight and obese patients to alleviate some of the effects of the disease, especially where joint involvement is significant.

REFERENCES http: //www. lupus. org/webmodules/webarticles net/templates/new_aboutintroduction. aspx? arti cleid=75&zoneid=9 http: //en. wikipedia. org/wiki/Systemic_lupus_ery thematosus http: //www. lupusmalaysia. org/e/what-is-sle/ http: //www. cureresearch. com/l/lupus/statscountry. htm

- Slides: 13