SYSTEMIC COMPLICATIONS IN LOCAL ANAESTHESIA Whenever any drug




























































- Slides: 67

SYSTEMIC COMPLICATIONS IN LOCAL ANAESTHESIA

Whenever any drug is administered, 2 types of action may be observed DESIRABLE & UNDESIRABLE 3 PRINCIPLES SHOULD BE REMEMBERED No drug exerts a single action No clinically useful drug is entirely devoid of toxicity Toxicity lies in the hand of the user

Classification of Adverse drug reactions 1. Toxicity caused by direct extension of the usual pharmacological effects of the drug Side effects Overdose reactions Local toxic effects

2. Toxicity caused by alteration in the drug recipient Disease process Emotional disturbances Genetic Aberrations Idiosyncrasy

3. Toxicity caused by alteration in the drug recipient

Overdose Dose related Systemic distribution Extension of pharmacologic effects Selective CNS or CVS depression

Allergic Reactions Not dose related May be systemic or localized Unrelated to pharmacological effects Exaggerated immune system response

Idiosyncrasy Reaction Unexplained by any known mechanism of the drug’s action Neither overdose nor allergic reaction Unpredictable; treat symptoms

Predisposition - Overdose Patient factors Age Weight Sex Medications

Predisposition - Overdose Patient factors Disease Genetics Psychological attitude

Predisposition - Overdose Drug factors Vasoactivity Concentration Dose Route of administration

Predisposition - Overdose Drug factors Rate of injection Vascularity of site Vasoconstrictors

Cause of Overdose Levels Total dose is too large Absorption is too rapid Intravascular injection Biotransformed too slowly Eliminated too slowly

Excessive Dose Maximum dose should be based on: Age Physical status Weight

Rapid Absorption Vasoconstrictors should be used unless specifically contraindicated

Intravascular Injection Occurrence varies with type of injection: Nerve Block % positive aspirate Inf. alveolar 11. 7 Mental/Incisive 5. 7 Post. sup. alv. 3. 1 Ant. sup. alv. / Buccal < 1

Prevention Use aspirating syringe Use needle - 25 g or larger Aspirate in 2 planes Inject slowly

CLINICAL MANIFESTATIONS of OVERDOSE

Minimal to Moderate Signs Talkativeness Apprehension Slurred speech Excitability Stutter Euphoria Dysarthria Nystagmus Muscular twitching / tremors

Minimal to Moderate Signs (cont. ): Elevated BP Sweating Elevated heart rate Nausea/vomiting Elevated resp. rate Disorientation Failure to follow commands / reason Lack of response to painful stimuli

Minimal to Moderate Symptoms: Restless Visual disturbances Nervous Auditory disturbances Numbness Metallic taste

Minimal to Moderate Symptoms (cont. ): Light-headed and dizzy Drowsy and disoriented Losing consciousness Sensation of twitching (before actual twitching is observed)

Moderate to High Generalized tonic-clonic seizure activity followed by Generalized CNS depression Depressed BP, heart rate Depressed respiratory rate

Pathophysiology Local anesthetics cross blood-brain barrier, producing CNS depression as level rises


MANAGEMENT of OVERDOSE

Mild Reaction -slow onset Reassure patient Administer O 2 Monitor vital signs Consider IV anticonvulsant Allow recovery or get medical help esp. if possibility of metabolic or renal dysfunction

Severe Reaction - rapid onset Stop all treatment Place patient in supine position, feet up Establish airway, give O 2 (BLS) If convulsions, protect patient Summon emergency medical help Consider anticonvulsant drugs, vasopressors

Allergic Reactions Type Mechanism Time Clinical Example I Antigen induc. sec/min Angioedema, Anaphylaxis IV Cell mediated 48 hrs Contact dermatitis

Allergens in Local Esters - usually to the Para-amino-benzoic-acid product Na bisulfite or metabisulfite - found in anesthetics as perservative for vasoconstrictors Methylparaben - no longer used as perservative in dental cartridges

Management of Allergy Pts. If the patient gives a history of allergy to local anesthetics - Assume that an allergy exists Elective procedures Postpone until work-up is completed

Management of Allergy Pts. Emergency treatment Protocol #1 - no invasive treatment ( I&D, analgesics, antibiotics) Protocol #2 - use general anesthesia Protocol #3 - Histamine blocker (Benadryl) Protocol #4 - Others: electronic dental anesthesia, hypnosis, adjunctive N 2 O

Allergy - signs/symptoms Dermatologic: Urticaria - wheals, pruritis Angioedema Minor rash

Allergy - signs/symptoms Respiratory: Laryngeal edema Bronchospasm distress dyspnea anxiety cyanosis or flushing wheezing tachycardia diaphoresis use of accessory muscles

Anaphylaxis Typical progression * Skin reactions Smooth muscle spasms (GI, GU, respiratory) Respiratory distress Cardiovascular collapse *may occur rapidly, with considerable overlap

Management of Reactions Delayed skin reaction Benadryl - 50 mg stat & Q 6 H X 3 -4 days Immediate skin reaction Epinephrine 0. 3 mg IM or SC Benadryl - 50 mg IM Observation, medical consultation Benadryl - 50 mg Q 6 H X 3 -4 days

Management of Reactions Bronchial constriction Semi-erect position, O 2 - 6 L/min Inhaler or Epinephrine 0. 3 mg IM or SC Benadryl - 50 mg IM Observation, medical consultation Benadryl - 50 mg Q 6 H X 3 -4 days

Management of Reactions Laryngeal edema Place supine, O 2 - 6 L/min Epinephrine 0. 3 mg IM or SC Maintain airway Benadryl - 50 mg IV or IM Hydrocortisone - 100 mg IV or IM Perform Cricothyrotomy

Management of Reactions Anaphylaxis Place supine, on flat surface ABCs of CPR, call for medical help Epinephrine 0. 3 mg IV or IM (Q 5 mins) O 2 - 6 L/min, monitor vital signs After clinical improvement, Benadryl and Hydrocortisone

Differential Diagnosis Psychogenic reaction (Syncope) Overdose reaction Hypoglycemia Stroke (CVA) Acute adrenal insufficiency Cardiac arrest

PREVENTION of SYSTEMIC COMPLICATIONS

Prior to Treatment Complete review of medical status (including vital signs) Anxiety / Fear should be assessed and managed before administering anesthetic

Administration of Anesthetic Place pt. supine or semi-supine position Dry site, apply topical X 1 min Select appropriate drug for treatment (time) Vasoconstrictor unless contraindicated

Administration (cont. ) Weakest anesthetic in the minimum volume (compatible with successful anesthesia) Inject slowly (minimum of 60 sec / 1. 8 ml) Continually observe Never leave patient alone after injection

Administration (cont. ) Use only aspirating syringe Aspirate in two planes, before injecting Use sharp, disposable needles of adequate diameter and length

Malignant hyperthermia

• Etiology Autosomal dominant with variable penetrance Mutation in the ryanodine receptor 50% of children of MH susceptible parents are potentially at risk.

Unsafe drugs • Depolarizing muscle relaxants (Sch) • Potent inhalation agents (halothane, isoflurane, enflurane, desflurane, sevoflurane · Insufficient data / controversial • d-Tubocurarine • Phenothiazines • AMIDE GROUP – Local Anesthetics

• • Discontinue LA/ GA Hypercarbia Tachycardia Ventricular arrhythmia • Muscle rigidity Hyperthermia: 39 - 42 dc • Oxygen : 100 % Anti arrhythmic therapy Dantrolene Sodium Body cooling

• Cardiac arrest due to hypokalemia • Hypertension • Acidosis • Myoglobinuria • • • Sodium bicarbonate Forced diuresis FOLEYS CATHETER ICU PREVENTION

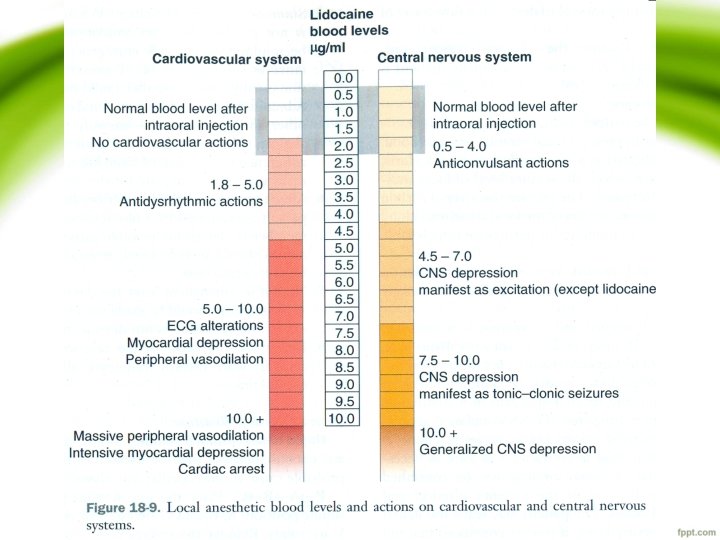
SYSTEMIC ACTIONS OF LOCAL ANESTHETICS • Block APs of excitable membranes CNS & CVS most affected CNS • Analgesia: pain reaction threshold • Mood elevation (cocaine) • Convulsions: a) Anticonvulsive level 0. 5 -4µg/ml b) Preseizure signs 4. 5 -7µg/ml c) Tonic clonic seizure >7. 5µg/ml • Anticonvulsive action: Depresses cortical neurons around epileptic focus used in epileptics • Preconvulsive signs: doses above therapeutic level (excitation)

region Preconvulsive signs & symptoms Warm, flushed feeling of skin SIGNS (OBSERVED) Slurred speech Shivering Muscular twitching Tremors Dizziness Visual & auditory disturbances Drowsiness Disorientation Pleasant dreamlike state

• Convulsive phase: • Further elevation (7. 5 -10µg/ml) gen tonic clonic seizures • p. CO 2 prolonged seizure duration Convulsions Cerebral metabolism & blood flow l. a delivery to brain & met. acidosis Prolonged seizure activity • Further increase: – CNS depression – Cessation of seizures & flat EEG tracings – Respiratory depression & arrest

CVS Direct action on myocardium: • Depression decreased rate of conduction & force of contraction. Lignocaine 1. 8 -6µg/ml: Rx of dysrrythmia (PVS, ventricular tachycardia) 1 -1. 5 mg/kg bod wt i. v for 3 -5 mins • Further increase circulatory collapse Direct action on peripheral vasculature: • Vasoconstriction cocaine, ropivacaine (cutaneous VC) • All other agents : vasodilation hypotension Local tissue toxicity • i. m injections skeletal muscle alterations

Respiratory System: • Non overdose levels: bronchial smooth musc relaxant • Overdose levels: resp arrest (CNS depression) Miscellaneous actions: • Drug interactions: Potentiates action of muscle relaxants & CNS depressants (barbiturates, opioids etc) • Malignant hyperthermia: Tachycardia, tachypnea, unstable BP, cyanosis, resp & met acidosis, fever upto 108 F

Composition : 1) Local anesthetic agent : Lignocaine 2) Vasoconstrictor : epinephrine 3) Reducing agent : vasoconstrictors are unstable in solution and may oxidize, especially on a prolonged exposure to sunlight. Sodium metabisulphite (0. 05% and 0. 1%) competes for the available oxygen 4) Preservative : stability is maintained by adding caprylhydrocuprinotoxin and methyl paraben. 5) Fungicide : Thymol. 6) Vehicle : Na. Cl or RL 7) Distilled water

PHARMACOLOGY OF VASOCONSTRICTORS Actions: • Vasoconstriction Decreases blood flow to site of injection • Slows absorption of l. a into CVS decreases blood levels • Decreases risk of l. a toxicity • Increases the duration of action (l. a remains at injected site for longer) • Decreased bleeding at site of administration (hemostasis)

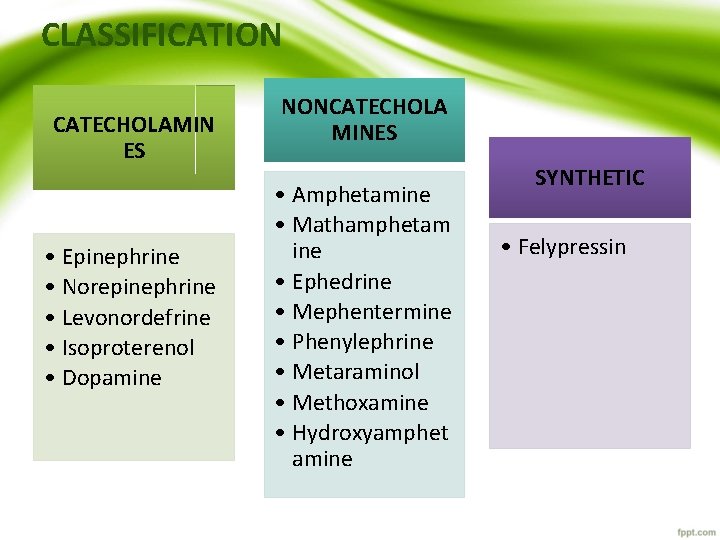
CLASSIFICATION CATECHOLAMIN ES • Epinephrine • Norepinephrine • Levonordefrine • Isoproterenol • Dopamine NONCATECHOLA MINES • Amphetamine • Mathamphetam ine • Ephedrine • Mephentermine • Phenylephrine • Metaraminol • Methoxamine • Hydroxyamphet amine SYNTHETIC • Felypressin

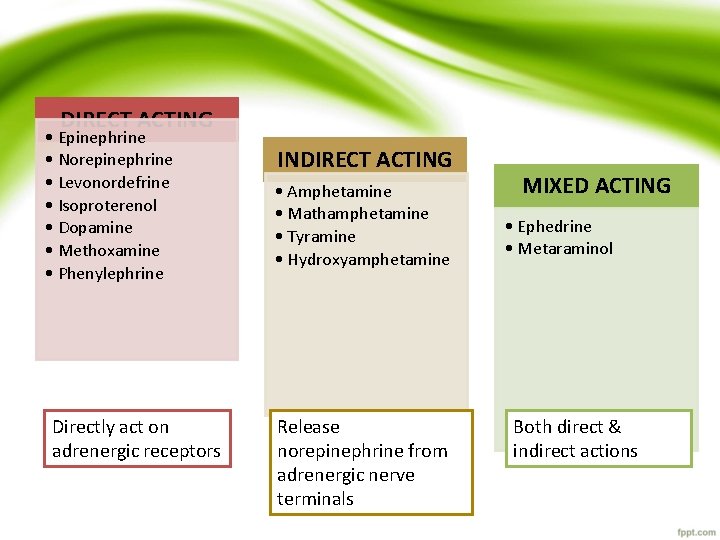
DIRECT ACTING • Epinephrine • Norepinephrine • Levonordefrine • Isoproterenol • Dopamine • Methoxamine • Phenylephrine Directly act on adrenergic receptors INDIRECT ACTING • Amphetamine • Mathamphetamine • Tyramine • Hydroxyamphetamine Release norepinephrine from adrenergic nerve terminals MIXED ACTING • Ephedrine • Metaraminol Both direct & indirect actions

Adrenergic receptors α receptors (vasoconstriction): b. v of skin & mucous membranes • α 1: excitatory post-synaptic • α 2: inhibitory post-synaptic β receptors • β 1: heart & small intestine cardiac stimulation (inc HR & FOC) & renin release • β 2: bronchi, vascular beds, uterus – Relaxn of bronchial muscles bronchodilation – Relaxn of muscles in bl. vessel vasodilation – Relaxn of uterus • β 3: adipose tissue lipolysis

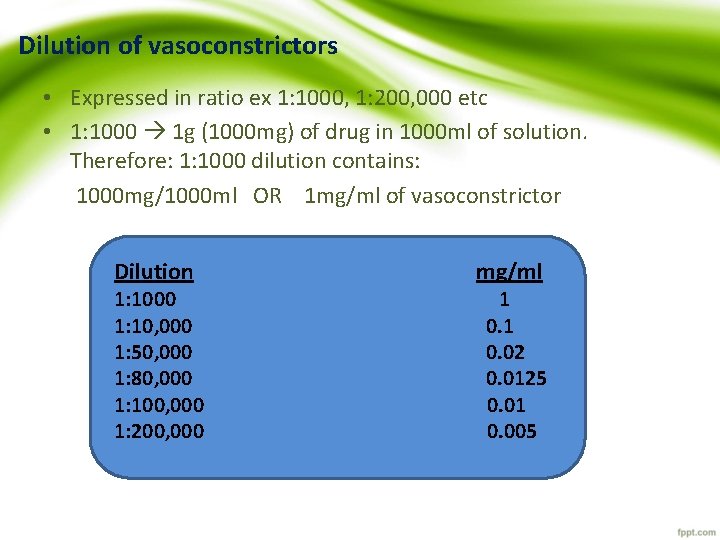
Dilution of vasoconstrictors • Expressed in ratio ex 1: 1000, 1: 200, 000 etc • 1: 1000 1 g (1000 mg) of drug in 1000 ml of solution. Therefore: 1: 1000 dilution contains: 1000 mg/1000 ml OR 1 mg/ml of vasoconstrictor Dilution mg/ml 1: 1000 1 1: 10, 000 0. 1 1: 50, 000 0. 02 1: 80, 000 0. 0125 1: 100, 000 0. 01 1: 200, 000 0. 005

PHARMACOLOGY OF SPECIFIC AGENTS v EPINEPHRINE (Proprietary name: adrenaline) • Chemical properties: – Stable in the form of acid salt (hydrochloride) – Readily gets oxidized – Source: synthetic/adr. medulla of animals – Acts on α & β receptors, β action predominates • Maximum recommended dose (MRD): (American Heart Association+ADA) – Normal healthy patient: 0. 2 mg/appointment ie 8 cartridges (16 ml) of 1: 80, 000 or 10 cartridges (20 ml) of 1: 100, 000 – Significant cardiovascular disease (ASAIII & IV): 1/5 th of normal dose ie 0. 04 mg/appt

• Systemic actions: 1) CVS: - Increased heart rate, cardiac output, FOC, myocardial O 2 consumption, SBP & DBP 2) Blood vessels: - Microcirculation (skin, muc. memb): α receptors VC - Skeletal muscle vessels (α & β): small doses: β 2 dominates VD large doses: α stimulated VC - Coronary arteries (β receptors) VD “Rebound phenomenon” 3) Respiratory system: - β 2 stimulation: bronchodilation used in asthmatics

4) CNS: - Excessive doses: CNS stimulant 5) Metabolism: - β stimulation glycogenolysis elevated blood sugar levels - Action terminated by: i) Uptake by adrenergic nerves ii) Inactivated by hepatic enzymes (MAO) iii) 1% excreted unchanged in urine Clinical applications: a) b) c) d) e) f) Allergic reactions, anaphylaxis (1: 1000) Bronchospasm Cardiac arrest Hemostasis (1: 50, 000 or 1: 1 lakh) In L. A solutions To produce mydriasis

v NOREPINEPHRINE (Noradrenaline) • 1/4 th as potent as epinephrine. Not recommended with L. A • Acts on both α & β α predominates prolonged mucous memb VC palatal mucosal necrosis • Does not increase HR or cause bronchodilation • More potent increase in BP v FELYPRESSIN (Octapressin) • Synthetic analogue of ADH vasopressin • No significant alterations in heart rate as it does not act on adrenergic receptors & has direct effect on the vascular smooth muscle • Acts on the venous circulation and does not have an arterial, cardiac or potential arrhythmogenic effect • Ind: hyperthyroidism, MAO inhibitors • CI: pregnancy (oxytocic actions)

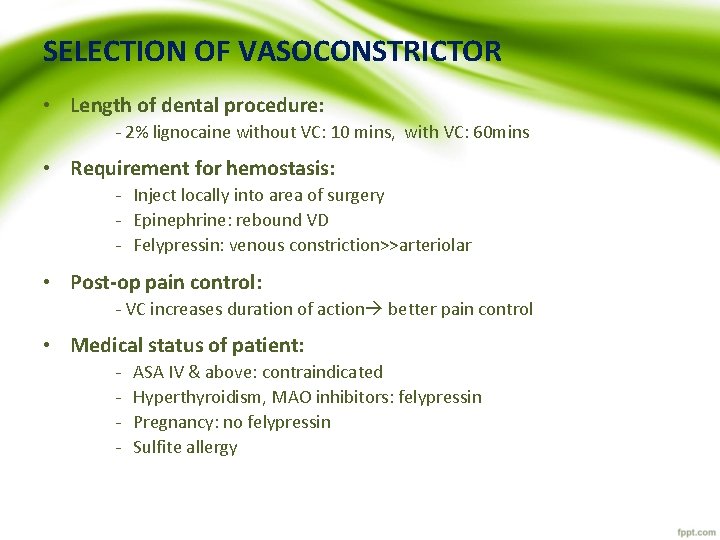
SELECTION OF VASOCONSTRICTOR • Length of dental procedure: - 2% lignocaine without VC: 10 mins, with VC: 60 mins • Requirement for hemostasis: - Inject locally into area of surgery - Epinephrine: rebound VD - Felypressin: venous constriction>>arteriolar • Post-op pain control: - VC increases duration of action better pain control • Medical status of patient: - ASA IV & above: contraindicated Hyperthyroidism, MAO inhibitors: felypressin Pregnancy: no felypressin Sulfite allergy

Thank you •