SYNOVIAL FLUID ANALYSIS BY DR KAREN DSA INDEX

SYNOVIAL FLUID ANALYSIS BY DR. KAREN D’SA

INDEX � � � � � DEFINITION HISTORY EMBRYOLOGY ANATOMY NORMAL CONTENT FUNCTIONS ABNORMAL SYNOVIAL FLUID : NONINFLAMMATORY , INFLAMMATORY, SEPTIC AND HAEMORRHAGIC TECHNIQUE PHYSICAL AND BIOCHEMICAL EXAMINATION OF THE ASPIRATE

DEFINITION “ IT IS AN ULTRADIALYSATE OF BLOOD PLASMA TO WHICH PROTEOGLYCAN HAS BEEN ADDED BY THE JOINT TISSUE. ”

HISTORY � PARACELSUS named synovial fluid. “Synovia” means joint fluid. � 1743 : JOHN HUNTER – “ synovial fluid is proper fluid for lubrication. ” � 1936 : JONES – mixed lubrication. - fluid film : during movement. - solid friction : starting and stopping points.
EMBRYOLOGY MESENCHYMAL CELLS Centrally CHROMBOBLAST Condensed on 14 th day PRIMITIVE JOINT PLATE/ ARTICULAR DISC 3 rd month FLUID FILLED CLEFTS 4 th month SYNOVIAL CAVITY
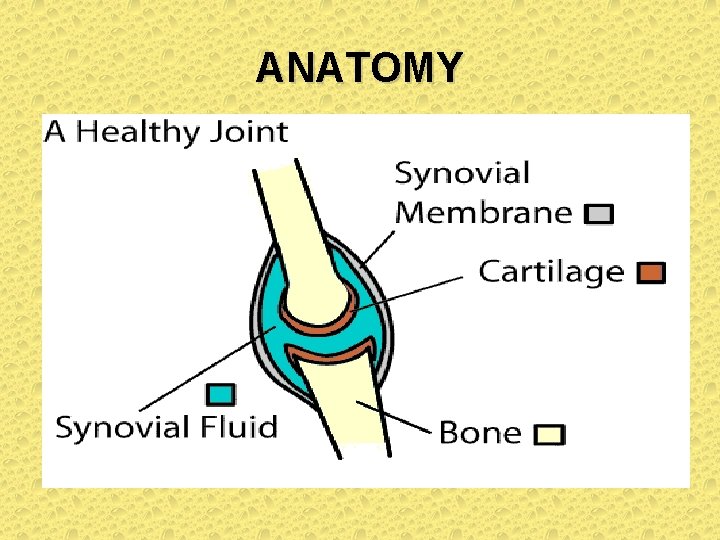
ANATOMY
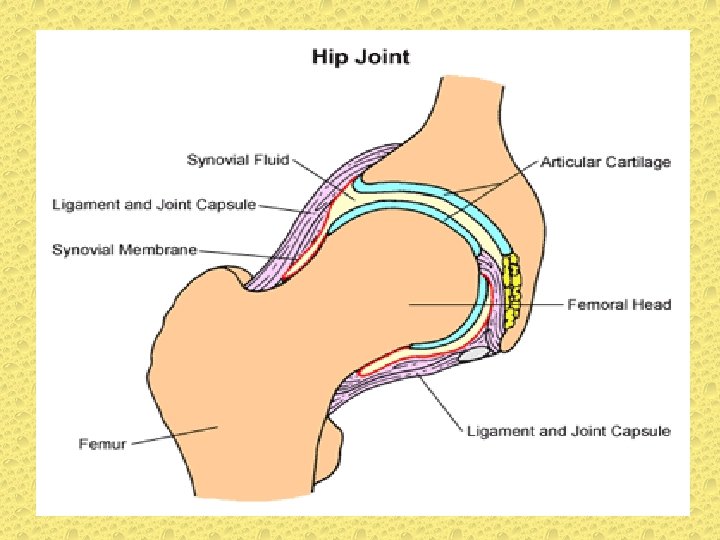

SYNOVIAL FLUID NORMAL CONTENT � � � � VOLUME : 0. 13 To 3. 5 ml COLOR : Clear/pale yellow VISCOSITY : High CLOT : No CLARITY : Transparent TOTAL WBC COUNT: 200 cells/ml approx DIFFERENTIAL WBC � PMNS : 25% � LYMPHOCYTES : 25% � MONOCYTES : 50%

� � � � CRYSTALS : None PROTEIN : 2. 5 gm/ml GLUCOSE : 90% of blood glucose CULTURE : Sterile SPECIFIC GRAVITY : 1. 008 TO 1. 015 INTRA-ARTICULAR PRESSURE: -8 TO-12 cms/ H 2 O ENZYMES : AMYLASE PROTEASE LIPASE ALKALINE PHOSPHATE

FUNCTION OF SYNOVIAL FLUID � � Lubrication Nutritive Protective Encourage motion

ABNORMAL SYNOVIAL FLUID � Disease that affects the joint may change the normal characteristic of synovial fluid like changes in volume , viscosity, ability to clot, clarity, color. � � � These changes are classified into 4 groups: NON- INFLAMMATORY SEPTIC HAEMORRHAGIC

NON-INFLAMMATORY � � � � Trauma Internal derangement OA Aseptic Necrosis Osteochondritis Dissecans Polymyalgia Rheumatica Amyloidosis AIDS
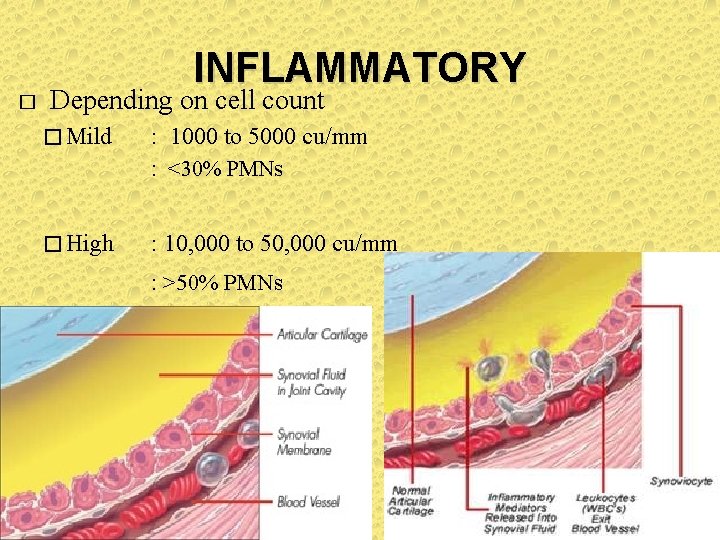
INFLAMMATORY � Depending on cell count � Mild : 1000 to 5000 cu/mm : <30% PMNs � High : 10, 000 to 50, 000 cu/mm : >50% PMNs
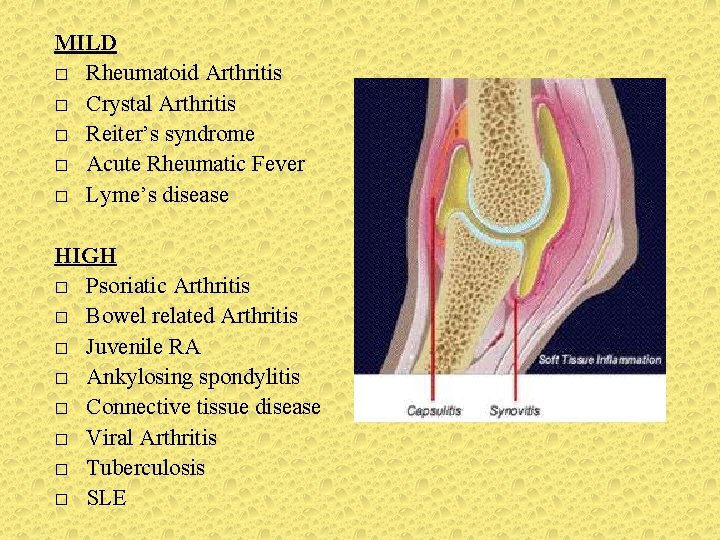
MILD � Rheumatoid Arthritis � Crystal Arthritis � Reiter’s syndrome � Acute Rheumatic Fever � Lyme’s disease HIGH � Psoriatic Arthritis � Bowel related Arthritis � Juvenile RA � Ankylosing spondylitis � Connective tissue disease � Viral Arthritis � Tuberculosis � SLE
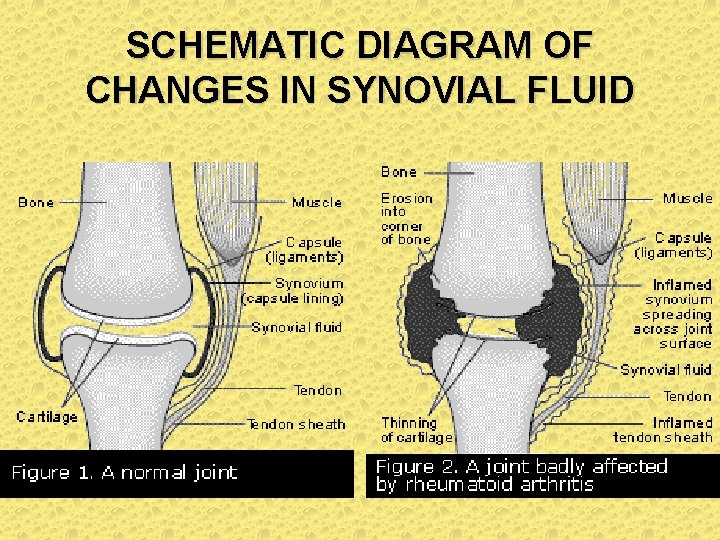
SCHEMATIC DIAGRAM OF CHANGES IN SYNOVIAL FLUID
HAEMORRHAGIC � � � Trauma Hemorrhagic Diseases � Thrombocytopenia � Anticoagulant therapy � Hemophilia � Sickle cell disease � Malignancy Neuropathic: Charcot joint Joint prosthesis Tumor : � Pigmented Villonodular Synovitis � Synovial Haemangioma

SEPTIC � � Bacterial infections Tubercular or Fungal arthritis

ARTHROCENTESIS INDICATIONS : Acute joint swelling after injury Suspected infection Acute synovitis in adults Chronic synovitis �
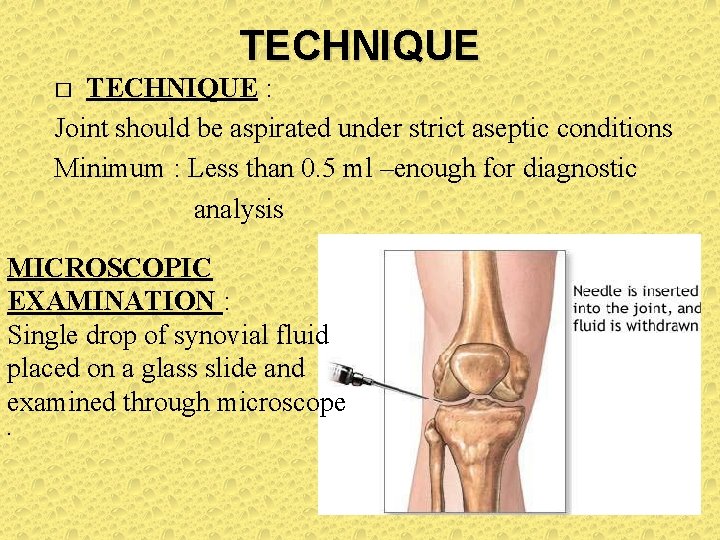
TECHNIQUE : Joint should be aspirated under strict aseptic conditions Minimum : Less than 0. 5 ml –enough for diagnostic analysis � MICROSCOPIC EXAMINATION : Single drop of synovial fluid placed on a glass slide and examined through microscope .
SYNOVIAL FLUID ANALYSIS

PHYSICAL AND BIOCHMEICAL EXAMINATION 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Volume Viscosity Clarity Colour Cell count Crystals Protein Sugar Microscopy Cell type

1. VOLUME Measured by the ASPIRATING SYRINGE. � LOW VOLUME: DOES NOT SIGNIFY disease � Repeated collection: SEPTIC ARTHRITIS.

2. VISCOSITY � Reduced viscosity results either from Degradation of Hyaluronate caused by inflammation or rapid accumulation of fluid after trauma which dilutes Hyalurate concentration � INCREASED : Degenerative Arthritis. DECREASED: Septic arthritis, RA � � Assessment of viscosity by : 1. STRING test 2. MUCIN test
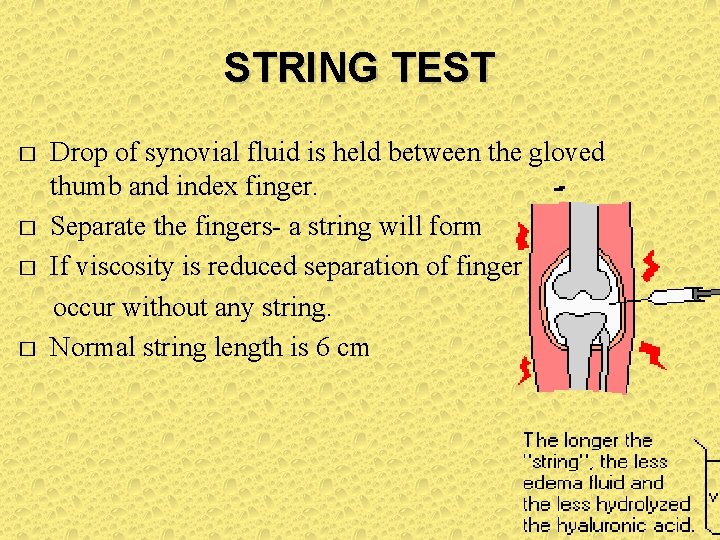
STRING TEST Drop of synovial fluid is held between the gloved thumb and index finger. � Separate the fingers- a string will form � If viscosity is reduced separation of finger occur without any string. � Normal string length is 6 cm �
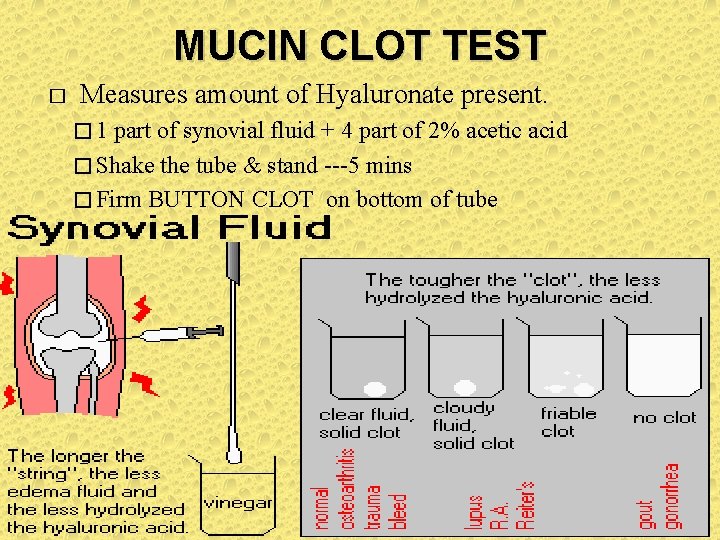
MUCIN CLOT TEST � Measures amount of Hyaluronate present. � 1 part of synovial fluid + 4 part of 2% acetic acid � Shake the tube & stand ---5 mins � Firm BUTTON CLOT on bottom of tube

� Grading : � GOOD: Ropy clump which does not break on shaking � FAIR: Friable clump break on shaking � POOR: Flocculent precipitate in cloudy � solution. STRING test is simple, so mostly performed

3. CLARITY � � � Placing BLACK TEXT on white back ground (NEWS PRINT) behind the test tube containing synovial fluid. If text can be read through fluid indicates clear fluid If text is not visible it indicates turbid fluid

4. COLOUR � Observed visually � Inflammation- deep yellow � Septic- serous or serosangunious � Trauma- Hemorraghic � #prosthesis----Gray

5. CELL COUNT � Total count : normal saline as diluvent, if effusion is bloody 0. 3% saline as a dilution solution. � Differential count: Centrifuged sediment smeared on glass slide and stained with LEISHMANNS stain & seen under oil immersion of microscope to study neutrophils, lymphocyte

6. CRYSTALS

� � � Wet mount preparation. A drop of synovial fluid on a slide free of dust or scratch, placing a cover slip over the drop and seal the 4 sides with nail polish then wet mount seen under compensated polarized light microscope with rotating stage 4 types of crystals : � MONO SODIUM MONO HYDRATE: gout � CALCIUM PYROPHOSPHATE DIHYDRATE: pseudo gout � CALCIUM OXALATE: chronic dialysis arthropathy � HYDROXY APATITE: rotator cuff syndrome
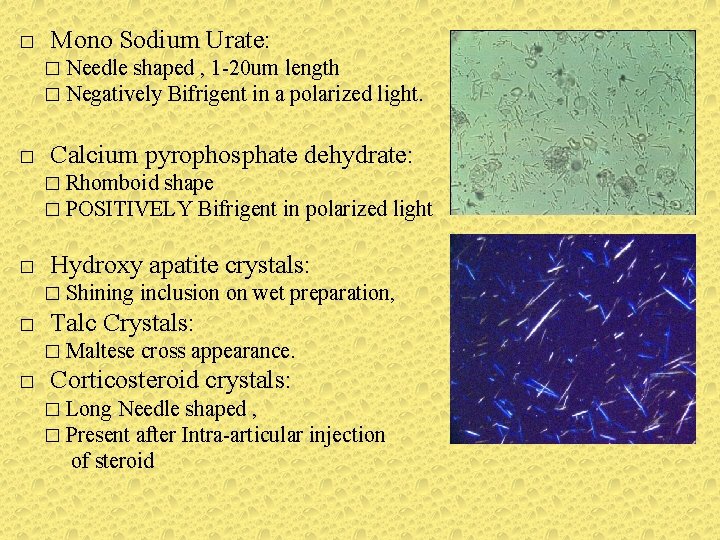
� Mono Sodium Urate: � Needle shaped , 1 -20 um length � Negatively Bifrigent in a polarized light. � Calcium pyrophosphate dehydrate: � Rhomboid shape � POSITIVELY Bifrigent in polarized light � Hydroxy apatite crystals: � Shining inclusion on wet preparation, � Talc Crystals: � Maltese cross appearance. � Corticosteroid crystals: � Long Needle shaped , � Present after Intra-articular injection of steroid

7. PROTEIN � BIURATE method : 5. 9 ml of Na. Cl 2 + 0. 1 ml of synovial fluid + biurate reagent Mixed & incubated for 10 mins at 37 o. C Reading on the calorimeter using green filter

8. SUGAR ESTIMATION � Reading taken on colorimeter using Blue filter � Sugar content reduced � RA � Septic arthritis � inflammatory condition

9. BACTERIOLOGICAL EXAMINATION STAINING 3 cc synovial fluid Centrifuged sediment smeared Dried & Fixed GRAM stain / Z-N stain oil immersion microscopy �

10. CELLS � Neutrophils polymorphs: � � Small Lymphocytes: � � � Rare in synovial fluid. Presence indicate RA Reider cell: � � Present in Inflammatory Arthritis. Along with LE cells indicate SLE Plasma cells: � � � >90% in Septic Arthritis. Seen exclusively in RA Mott cell : � Resemble Plasma cell except that they contain Intra cytoplasmic Russel body






THANK YOU
- Slides: 42