Syncope Faints Funny Turns When to reassure or


























- Slides: 28

Syncope: Faints & Funny Turns. When to reassure or refer Dr Peter Lillitos Paediatric Cardiology Registrar Leeds Children’s Hospital

House keeping QUESTIONS AT THE END MICROPHONES ON MUTE NO RECORDING PLEASE

Objectives • Understand the range of presentations of syncope from infancy to young person • Appreciate the physiology behind syncope • Understand the diagnostic usefulness of taking a good history, clinical examination and 12 lead-ECG • Know the Red-Flags in history • When to reassure; When to refer

Resources: Harris M, Bu’Lock F. Arch Dis Child Educ Pract Ed 2016; 101: 26– 30. doi: 10. 1136/archdischild-2015 -308422 - https: //www. networks. nhs. uk/nhs-networks/yorkshire-andhumber-congenital-cardiac-network STARS. org



Pre-syncope - definition • Feeling one is about to pass out, transient loss of postural tone

Syncope - definition • Syncope is a transient, but complete, loss of consciousness (with associated loss of muscle tone) due to global cerebral hypoperfusion By definition: ▸ rapid onset ▸ short duration (<1 min) ▸ Recovery is – quick – spontaneous – complete

What is not syncope: This excludes: • Falls, without loss of consciousness • States of altered consciousness • Prolonged LOC • Epileptic seizures • Psychogenic collapse/movements

Prevalence • 15 -20% children & YP have syncopal event between 8 -18 yrs • Before 6 yrs syncope is unusual – unless breath holds, reflex anoxic faints

Johnson, E. R. , Etheridge, S. P. , Minich, L. L. et al. Pediatr Cardiol (2014) 35: 753. https: //doi. org/10. 1007/s 00246 -013 -0848 -4 • Referrals for tertiary opinions occupy a lot of time in paediatric cardiology and neurology clinics (5. 8% of paediatric cardiology clinic referrals in a 1 year period in a US Centre) • Sudden cardiac death is rare (0. 6– 8. 5 deaths/100 000 patient years) • Sensitivity of screening using history, examination and 12 -lead ECG findings can be 100% sensitive for the cardiac causes of syncope

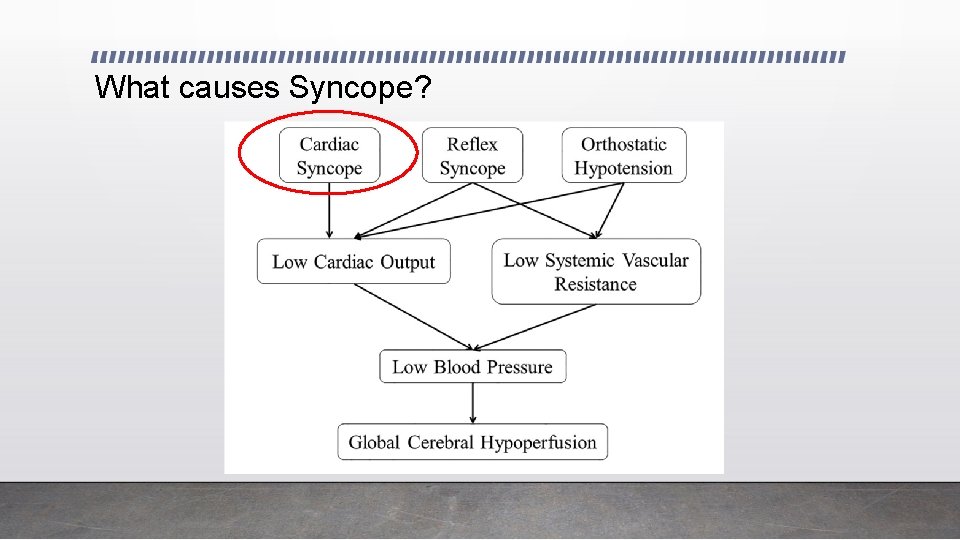
What causes Syncope?

Non-cardiac causes Exclude Cardiac FIRST Orthostatic intolerance Situational **((Exercise))** Neurogenic/ Endocrine Vasovagal Breath holding/Anoxic Venous pooling Epilepsy Orthostatic hypotension Cough, micturition, defecation Underhydrated Head injury Postural orthostatic tachycardia syndrome (POTS) Carotid sinus hypersenistivity Autonomic Hypoglycaemia Endocrine Metabolic

Cardiac syncope Electrical Structural/ Functional

Cardiac causes of syncope Electrical Structural AND functional Bradycardia (pathological) - SA node or AV node dysfunction; - Complete Heart Block - Implanted device dysfunction Severe outflow tract obstruction Eg: severe Aortic Stenosis - VT (channelopathies eg: long QT) Cardiomyopathies Myocarditis - Prolonged SVT/Atrial Tachycardia Drug induced Coronary anomalies Severe pulmonary hypertension (usually exertional dyspnoea)

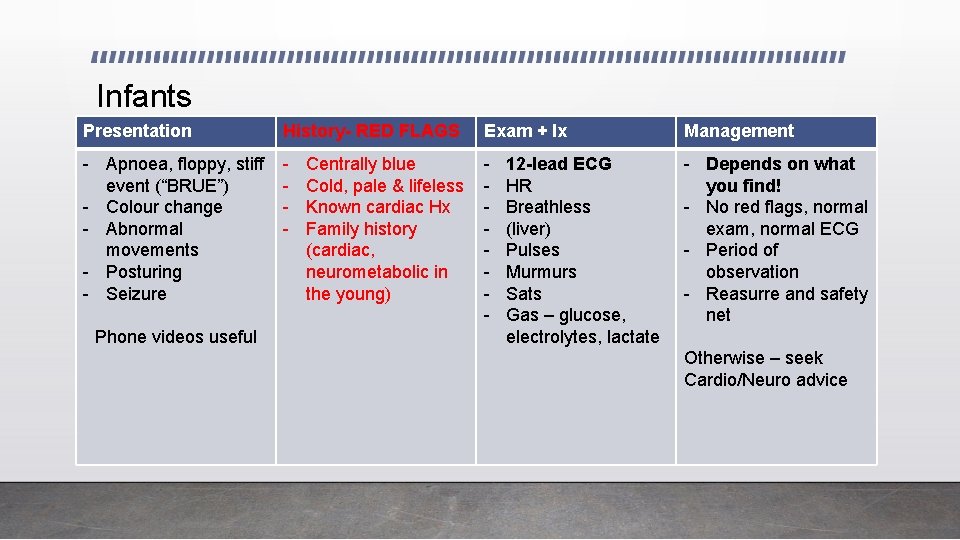
Infants Presentation History- RED FLAGS Exam + Ix Management - Apnoea, floppy, stiff event (“BRUE”) - Colour change - Abnormal movements - Posturing - Seizure - - - Depends on what you find! - No red flags, normal exam, normal ECG - Period of observation - Reasurre and safety net Phone videos useful Centrally blue Cold, pale & lifeless Known cardiac Hx Family history (cardiac, neurometabolic in the young) 12 -lead ECG HR Breathless (liver) Pulses Murmurs Sats Gas – glucose, electrolytes, lactate Otherwise – seek Cardio/Neuro advice

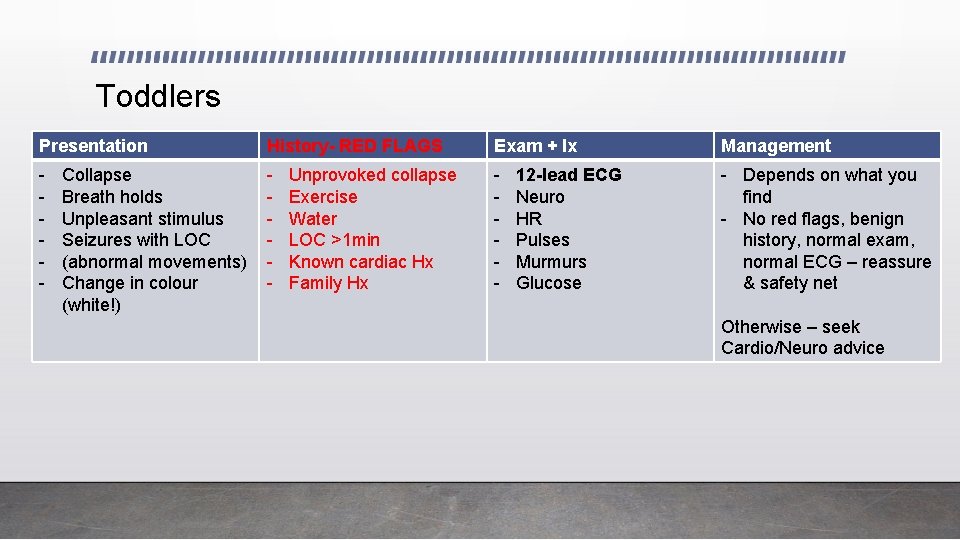
Toddlers Presentation History- RED FLAGS Exam + Ix Management - - Depends on what you find - No red flags, benign history, normal exam, normal ECG – reassure & safety net Collapse Breath holds Unpleasant stimulus Seizures with LOC (abnormal movements) Change in colour (white!) Unprovoked collapse Exercise Water LOC >1 min Known cardiac Hx Family Hx 12 -lead ECG Neuro HR Pulses Murmurs Glucose Otherwise – seek Cardio/Neuro advice

Breath holding • Age 1– 5 years. Two types: 1. Cyanotic (“Blue” breath-holding attacks) • More common than Anoxic form • Frustration or anger • During spells, children cry vigorously and then hold their breath in expiration • Apnoea is followed by cyanosis and LOC • Recovery usually quick within 1 minute. 2. Pallid (Reflex anoxic seizures) • Sudden fright or minor injuries • Gasps or cries briefly, abruptly becomes quiet, LOC, pale and limp • Maybe clonic jerks • Recovery usually quick within 1 minute • Anaemia is an association

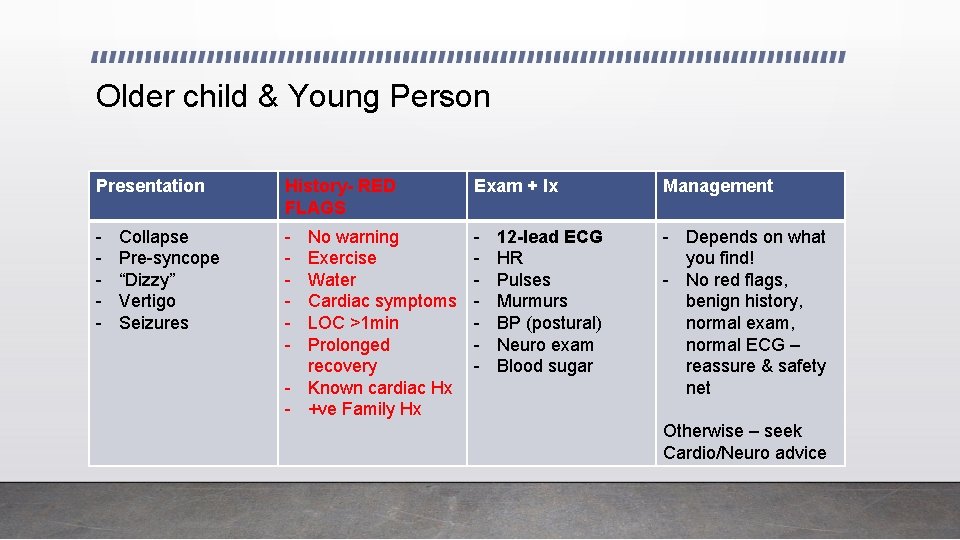
Older child & Young Person Presentation History- RED FLAGS Exam + Ix Management - - Depends on what you find! - No red flags, benign history, normal exam, normal ECG – reassure & safety net Collapse Pre-syncope “Dizzy” Vertigo Seizures No warning Exercise Water Cardiac symptoms LOC >1 min Prolonged recovery - Known cardiac Hx - +ve Family Hx 12 -lead ECG HR Pulses Murmurs BP (postural) Neuro exam Blood sugar Otherwise – seek Cardio/Neuro advice

History – key! • The BEFORE, DURING & AFTER • Witness • Confirm whether loss of consciousness • Physical activity & type? • Warning? • Cardiac symptoms preceding? • Duration? • Should be loss of postural tone • Spontaneous recovery? • Sequale? • Generalised seizures: non-specific to neuro or cardiac • Life style: skipping meals, fluid intake

Classical warning symptoms for vasovagal syncope

Reflex syncope “VASOVAGAL” Look pale white Orthostatic syncope

Cardiac red-flags - under age of 40 yrs Non-cardiac syncope can coexist with cardiac, so investigate if suspicious

Examination • Often normal • Pulse – rhythm, rate • Chest: heaves, thrills, murmurs • BP (postural advocated in Y&H guideline) Lying down for 10 mins, standing at 0 mins, 1 min and 3 mins >20 mm. Hg sys and >10 mm. Hg dias

Other investigations for syncope • Echo – not sensitive • Exercise testing – exercise/exertional symptoms (CPVT or Long QT) • Holters – depends on frequency • Loop recorders and Implantable devices • Patient activated recorders – not for syncope • Tilt Table. .

POSTURAL ORTHOSTATIC TACHYCARDIA SYNDROME (POTS) • Syncope (usually) not a feature • Females 4: 1 • Chronic fatigue, IBS, hypermobility associated • Orthostatic symptoms • Rise in HR >30 bpm whilst standing for 10 mins, above baseline sitting • No drop in BP • Normal ECG and examination • ? Tilt table test. . • Management: reassurance, exercise conditioning, hydration, β-blocker, fludrocortisone • POTS-UK; STARS. org. uk

Management for Orthostatic symptoms • Lifestyle (hydration, meals, add salt in diet) • Postural exercises • Muscle pump exercises • Head down, lie down, legs up

Summary: When to reassure or refer • History typical of non-cardiac (non-neuro-metabolic) • No cardiac red flags in history or family history • Normal CVS examination • Normal ECG - Reassure • Non-typical history for benign causes or suggests neurological • Red-flags for cardiac in history/family history • Abnormal examination • Abnormal ECG - Refer https: //www. networks. nhs. uk/nhs-networks/yorkshire-and-humber-congenital-cardiac-network