Syncope diagnostic algorithm and management MUDr Jakub Honk

Syncope diagnostic algorithm and management MUDr. Jakub Honěk MUDr. Martin Horváth Kardiologická klinika, 2. LF UK a FN Motol, Praha
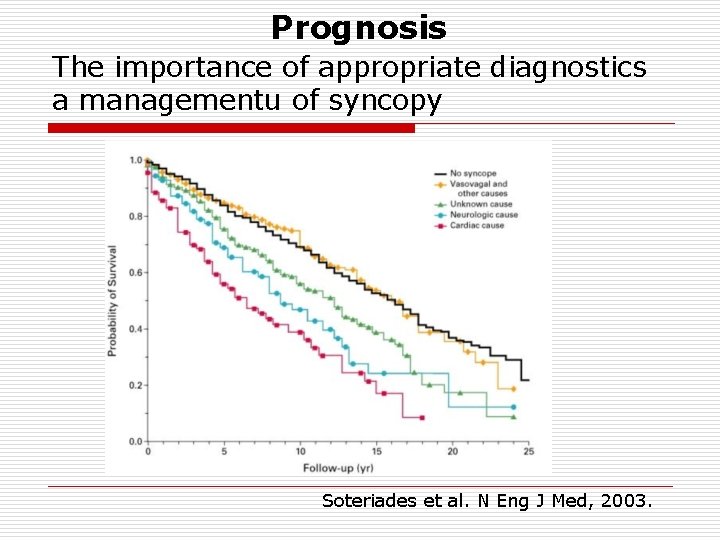
Prognosis The importance of appropriate diagnostics a managementu of syncopy Soteriades et al. N Eng J Med, 2003.

Definition o Syncope is a T-LOC due to transient Loss of consciousness global cerebral hypoperfusion Transient global hypoperfusion of brain characterized by rapid onset, short - circulatory cause duration, and spontaneous complete recovery. Sudden o T-LOConset – wider term– all losses of consciousness Short duration independent of the pathophysiological Spontaneous and fullcause recovery ESC Guidelines for the diagnosis and management of syncope (version 2009): Moya et al. Eur Heart J, 2009.
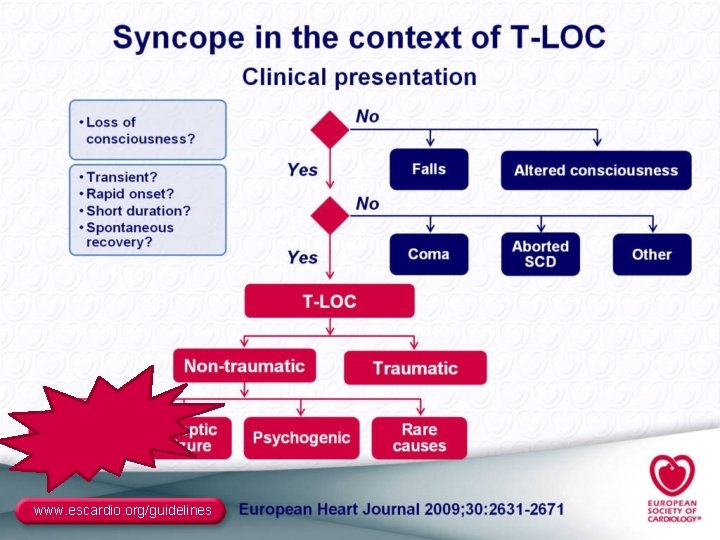
www. escardio. org/guidelines

Clasification of syncope Reflex syncope • Vasovagal • Situational • Carotid sinus hypersensitivity • Atypical forms • • Orthostatic hypotension Cardiac syncope Primary ANF Secondary ANF Iatrogenous Volume depletion • Arrhythmia as a primary cause • Structural heart disease

www. escardio. org/guidelines

Initial workup o Thorough history n circumstances preceding the syncope, prodromal symptoms, what hapenned during (bystanders) n Personal/family history, sudden death? , medication, has it happened before? o Physical examination o Blood pressure lying down (5 mins) and standing (1 st and 3 rd min. ) o ECG

Key questions Syncope? Diagnosis? Risk? • What it really a syncope? • Has a diagnosis been made? + • High risk of cardiovascular event or sudden death?
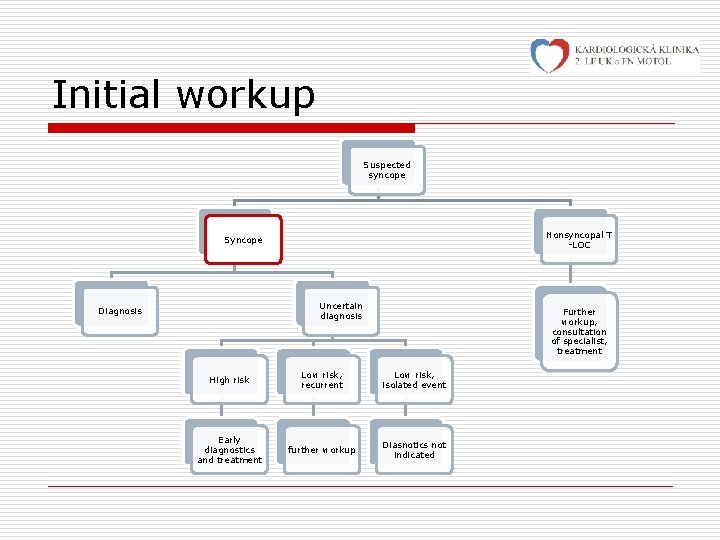
Initial workup Suspected syncope Nonsyncopal T -LOC Syncope Uncertain diagnosis Diagnosis Further workup, consultation of specialist, treatment High risk Low risk, recurrent Low risk, isolated event Early diagnostics and treatment further workup Diasnotics not indicated

Risk stratificaion o Structural heart disease n CAD (previous MI), heart failure, aortic stenosis, HCM o Clinical and ECG signs of arrhythmic etiology n Syncope lying down, physical activity, palpitations n Family history of sudden death n Bifascicular blocade, ns. VT, susp. SSS, preexcitation, ↑QTc, Brugada, susp. ARVC n Age >40 let + recurrent syncope (50% arrhytmia) o Serious comorbidities n Anemia, ionic imbalances

Further examination Diagnostic methods o Carotid massage n Pause > 3 s, BP drop > 50 mm. Hg n Uncertain cause in pts > 40 -yrs o Tilt test n Reflex syncope – cardioinhibitory, vasodepressor and mixed reacions X orthostatic hypotension n Suspected reflex syncope, high risk pts. without cardiac cause, susp. OH, difdg. falls, epilepsy, pseudosyncopies
Further examination Diagnostic methods o ECG monitoration n During hospiralization o Suspected arrhythmic cause, high risk n Holter ECG (24 h, 48 h, 7 d) o Recurrent syncopies/presyncopies n Implantable/external loop recorderd (ILR) o Recurent syncopies of unknown etiology, susp. VT with negative EP study n Diagnosis: syncope + arrhythia, serious arrhythmia n Syncope without ECG correlation rules out arrhythmic cause

Further examination Diagnostic methods o Electrophysiologic study n Restricted indications, suspected arrhythmic cause whithout non-invasice proof n Echocardiography n Risk stratification, dg. SOS o Stress test o Psychiatric examination o Neurological examination
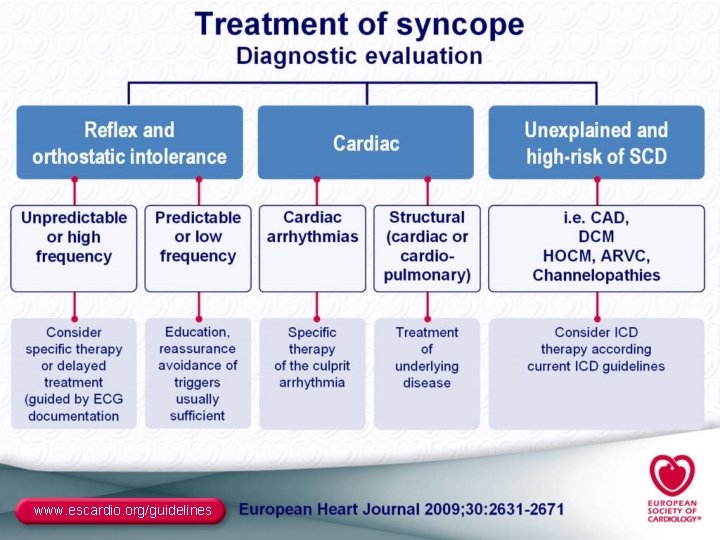
www. escardio. org/guidelines

Take home messages o Not every LOC is a syncope. o A thorough history is utmost important. o Initial workup yields in diagnosis in about 25 -40% of cases, in the other cases we stratify risk. o There are various diagnotic tests and therapeutic options. The basis is their reasonable and well-targeted use.

www. escardio. org/guidelines
- Slides: 16