Sustainability Transition Cofinancing STC Policy Progress Challenges EANNASO

Sustainability, Transition & Co-financing (STC): Policy, Progress & Challenges EANNASO DOMESTIC REOURCE MOBILIZATION TRAINING 4 OCTOBER 2019 DR. GEMMA M. OBERTH, REGIONAL PLATFORMS COORDINATOR (GLOBAL FUND CRG SI)
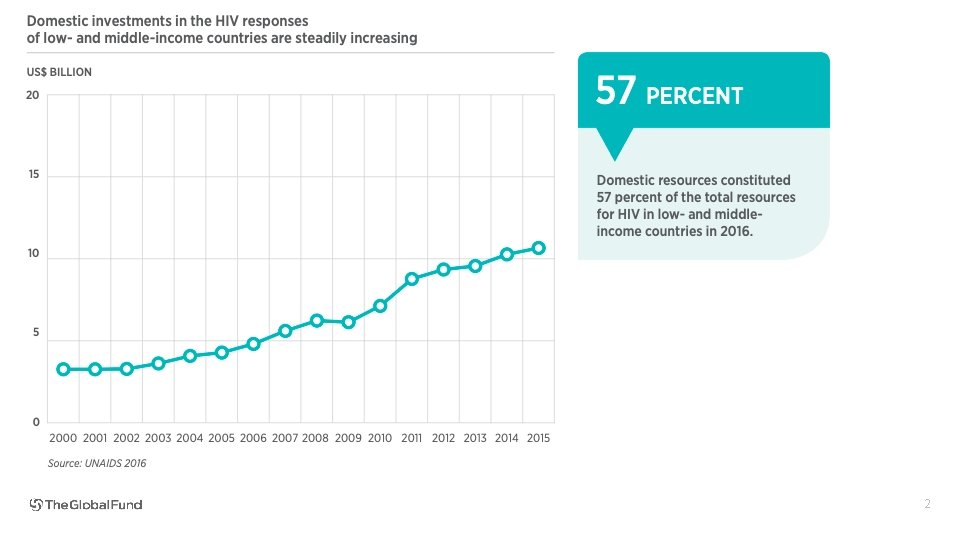
2
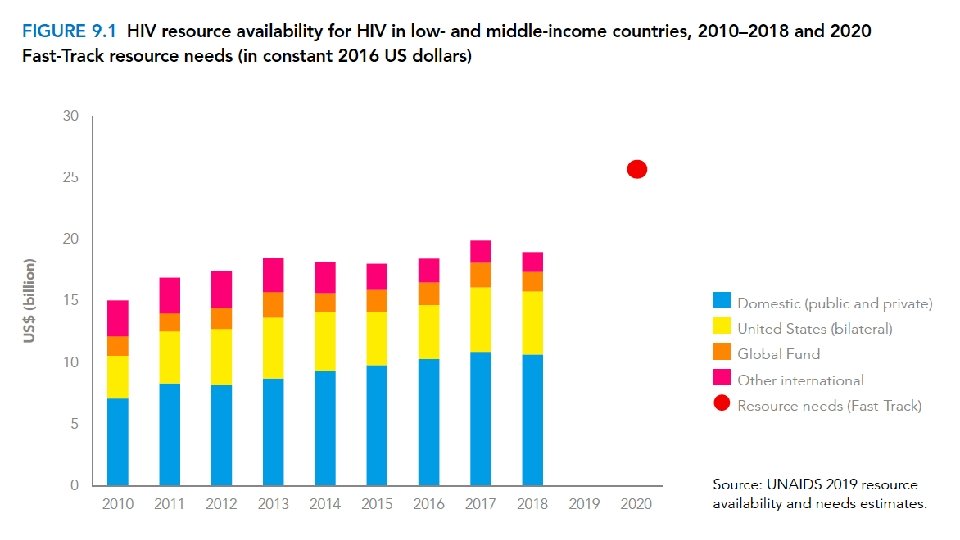
3
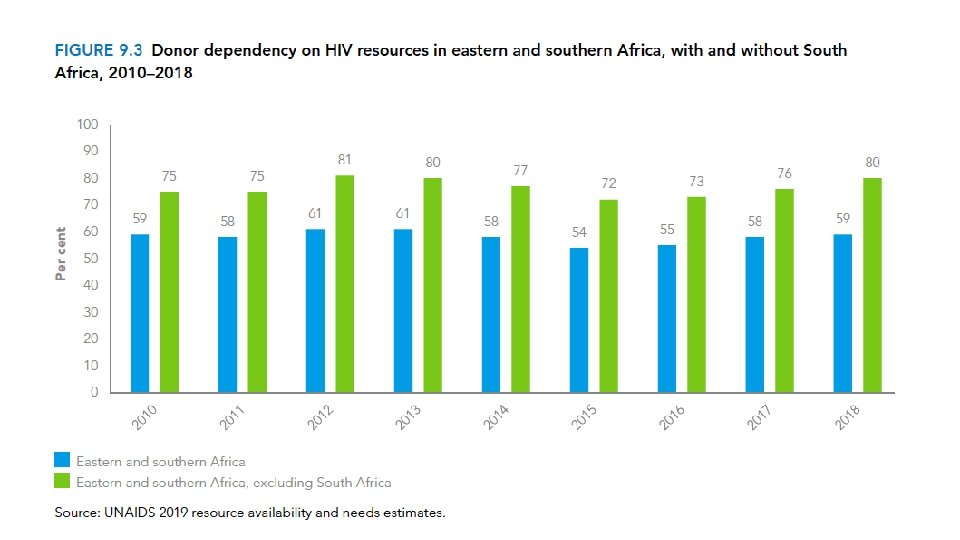
4

The Policy Approved at the 35 th Global Fund Board Meeting in April 2016 in Côte d'Ivoire Key points: • Long-term sustainability is a fundamental aspect of development and global health financing • Experience shows that supporting countries to sustainably transition from Global Fund support requires significant time • The revised application focus and co-financing requirements align domestic financing incentives to ensure that as countries move closer to transition they take up key programs such as interventions for key and vulnerable populations 5

6
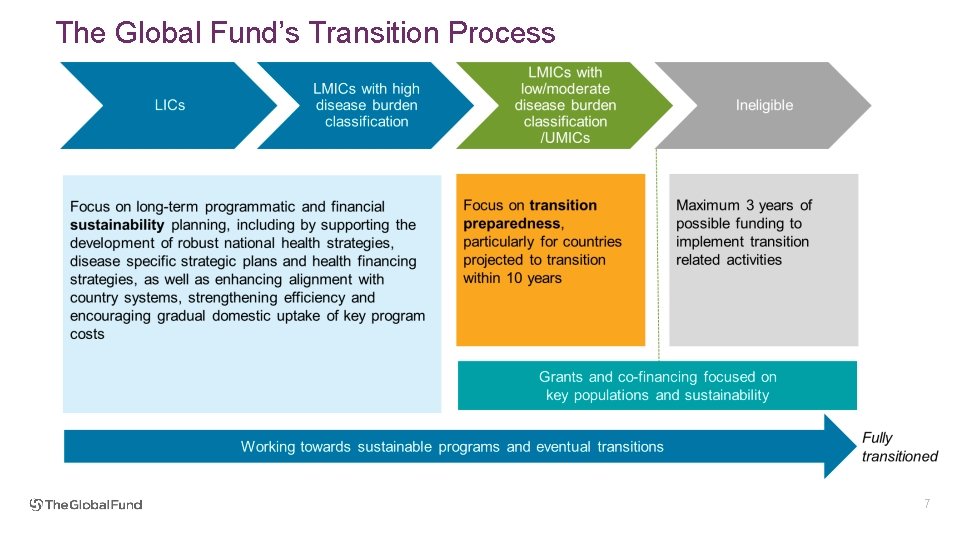
The Global Fund’s Transition Process 7
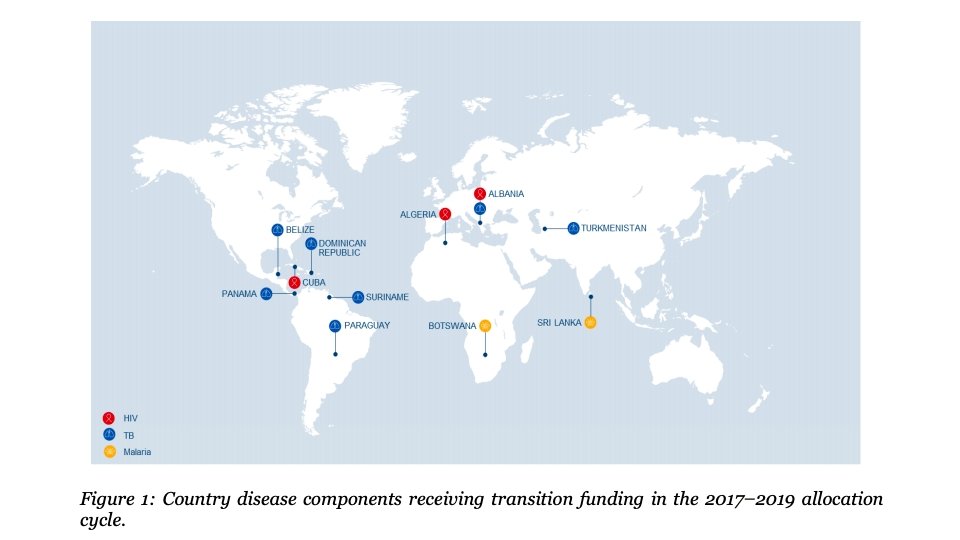
8
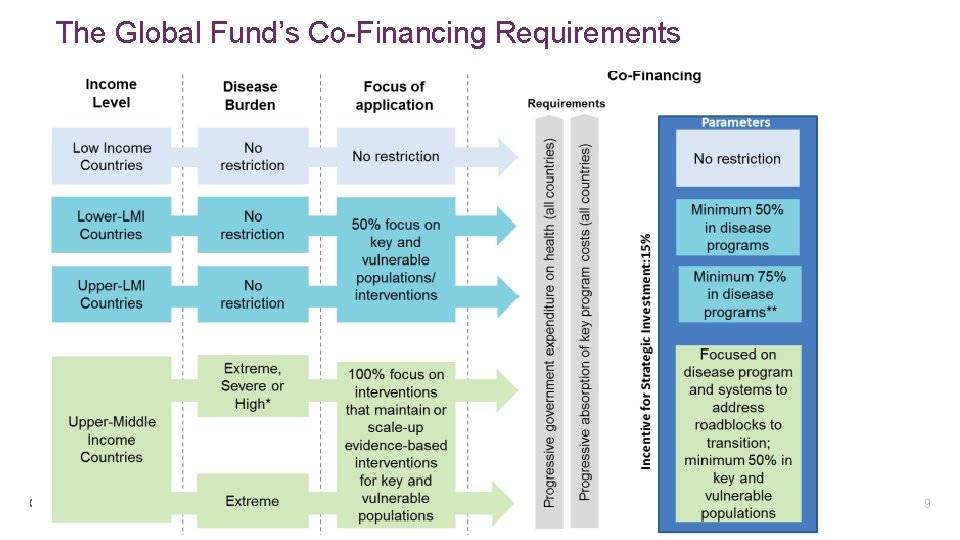
The Global Fund’s Co-Financing Requirements 9

2014 -2016 Co-financing commitment areas: Examples Source: Aidspan (2015) The “fair share” of shared responsibility 10
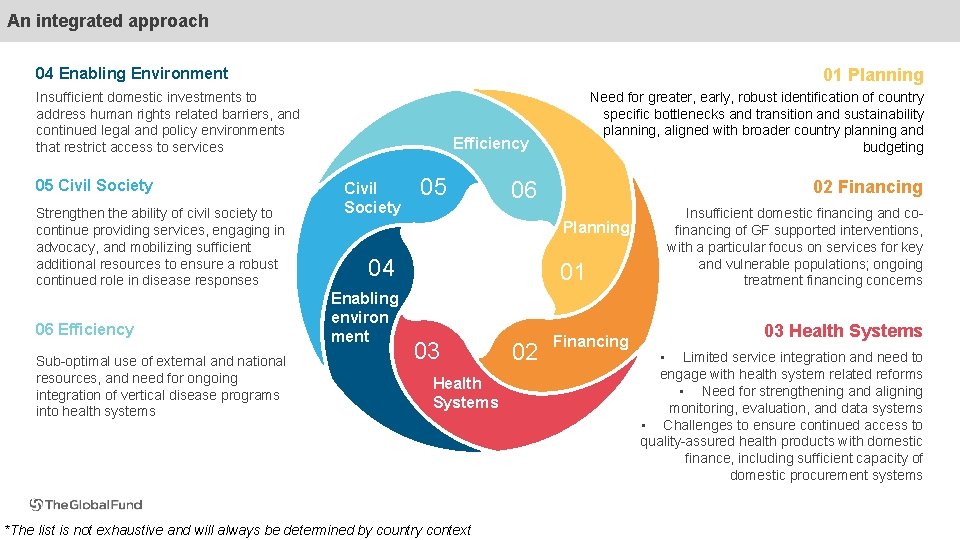
An integrated approach 04 Enabling Environment 01 Planning Insufficient domestic investments to address human rights related barriers, and continued legal and policy environments that restrict access to services 05 Civil Society Strengthen the ability of civil society to continue providing services, engaging in advocacy, and mobilizing sufficient additional resources to ensure a robust continued role in disease responses 06 Efficiency Sub-optimal use of external and national resources, and need for ongoing integration of vertical disease programs into health systems Need for greater, early, robust identification of country specific bottlenecks and transition and sustainability planning, aligned with broader country planning and budgeting Efficiency Civil Society 05 06 02 Financing Planning 04 Enabling environ ment 01 03 Health Systems *The list is not exhaustive and will always be determined by country context 02 Financing Insufficient domestic financing and cofinancing of GF supported interventions, with a particular focus on services for key and vulnerable populations; ongoing treatment financing concerns 03 Health Systems • Limited service integration and need to engage with health system related reforms • Need for strengthening and aligning monitoring, evaluation, and data systems • Challenges to ensure continued access to quality-assured health products with domestic finance, including sufficient capacity of domestic procurement systems
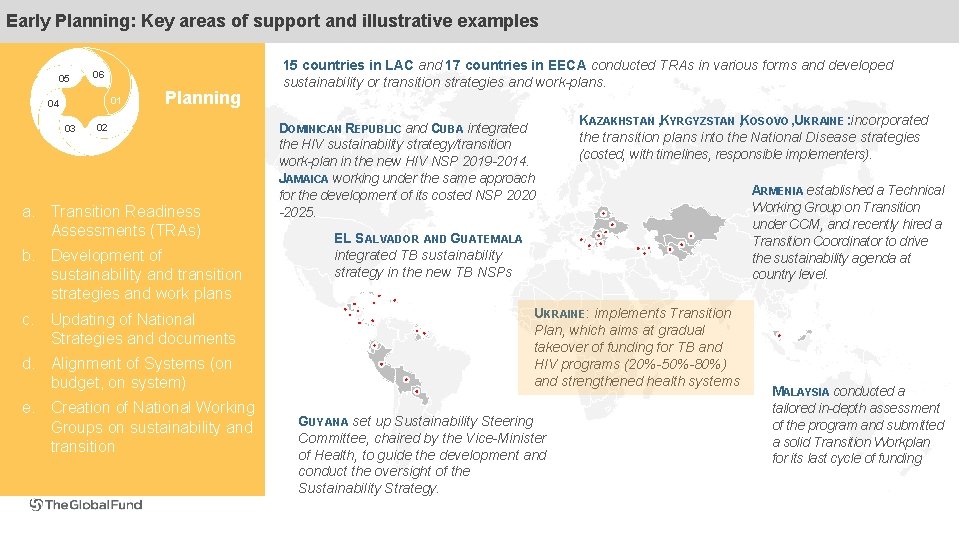
Early Planning: Key areas of support and illustrative examples 05 06 01 04 03 Planning 02 a. Transition Readiness Assessments (TRAs) b. Development of sustainability and transition strategies and work plans c. Updating of National Strategies and documents d. Alignment of Systems (on budget, on system) e. Creation of National Working Groups on sustainability and transition 15 countries in LAC and 17 countries in EECA conducted TRAs in various forms and developed sustainability or transition strategies and work-plans. DOMINICAN REPUBLIC and CUBA integrated the HIV sustainability strategy/transition work-plan in the new HIV NSP 2019 -2014. JAMAICA working under the same approach for the development of its costed NSP 2020 -2025. KAZAKHSTAN , KYRGYZSTAN , KOSOVO , UKRAINE : incorporated the transition plans into the National Disease strategies (costed, with timelines, responsible implementers). EL SALVADOR AND GUATEMALA integrated TB sustainability strategy in the new TB NSPs UKRAINE: implements Transition Plan, which aims at gradual takeover of funding for TB and HIV programs (20%-50%-80%) and strengthened health systems GUYANA set up Sustainability Steering Committee, chaired by the Vice-Minister of Health, to guide the development and conduct the oversight of the Sustainability Strategy. ARMENIA established a Technical Working Group on Transition under CCM, and recently hired a Transition Coordinator to drive the sustainability agenda at country level. MALAYSIA conducted a tailored in-depth assessment of the program and submitted a solid Transition Workplan for its last cycle of funding

Financing: Key areas of support and illustrative examples 05 06 01 04 03 Financing 02 a. Emphasis on co-financing commitments to cover key transition risks, including uptake of services for key populations and critical health system investments EECA: effectively used the co-financing requirements to increase MOH commitment and budgeting for specific interventions (BELARUS - for ARV and anti-TB drugs; MOLDOVA – co-funding HIV prevention services; MONTENEGRO and SERBIA increased x 2/3 times commitments for HIV prevention services; KAZAKHSTAN increased the governmental share of total HIV funding from 70% to 87% in 2016). EECA: effective absorption of ART procurement by governments: domestic financing increased CUBA: committed to provide additional from 18% in 2015 to 80% in 2020 funding for ARVs and started in 2019 purchasing ARV through the PAHO Strategic Fund. HAITI: Global Financing Facility launched aiming synergies between donors, MOH and MOF for sustainability strategy and increased domestic funding for health. b. Support Health Financing Strategies at country level KOSOVO: government has committed to funding 100 % of commodities for key populations by 2021 SRI LANKA: grant with significant component of ensuring government commitment to co-financing and piloting CSO funding via governmental PR DOMINICAN REPUBLIC: government fully absorbed the financing of ARVs, committed to scale up treatment with domestic funds and to fund 10 -25% of costs of prevention activities for key populations by 2021. c. Support National Health Accounts reporting PANAMA committed to fully absorb HIV adherence counsellors and to absorb prevention and testing interventions for key populations currently funded by Global Fund (50% by year 2 and 100% by the year-3), while continuing expanding the scale of those interventions. SURINAME and GUYANA: coordinated support with partners for completion of National Health Accounts and tracking of co-financing commitments as part of grant agreement *Source: Programmatic Gap Tables for 2017 -2019 Allocation Cycle
Health Systems: Key areas of support and illustrative examples 05 06 01 04 03 02 Health Systems a. Support the definition and costing of HIV and TB service packages and their inclusion in mandatory coverage b. Advocacy for health reforms to improve costs and quality of service provision c. Strengthen national capacities for procurement of quality affordable drugs d. Strengthen M&E system, including integration of reporting MOLDOVA, KYRGYZSTAN: Mandatory health insurance covers HIV and TB services DOMINICAN REPUBLIC: supporting the expansion of HIV/TB service integration. Coordinated support with partners to advocate and provide technical support to ensure coverage treatment under health insurance. UKRAINE, AZERBAIJAN, TURKMENISTAN: strengthened access to quality assured affordable drugs via international procurement platforms. KYRGYZSTAN, TAJIKISTAN, UZBEKISTAN: access to quality assured affordable drugs via in-country drug registration. HAITI: ongoing support for integration of reporting in DHIS 2 platform and analysis of Health Facility Assessment data to assess cost-effectiveness of interventions (focus on HRH) by health site SRI LANKA: cross-programmatic efficiency analysis that supports integration of disease specific services through ongoing Primary Health Care restructuring. BOLIVIA, CUBA, ECUADOR, EL SALVADOR, HONDURAS, GUATEMALA, NICARAGUA and PARAGUAY: Collaboration project with PAHO to strengthen public health national supply chains to promote technical independence and long term sustainability. BOLIVIA , PARAGUAY , HONDURAS and EL SALVADOR : Collaboration with PAHO and UNAIDS to support definition of HIV comprehensive package of services for key populations and integrated national information systems that permit measurement and analysis of data on coverage and quality of services for key populations
Enabling Environment: Key areas of support and illustrative examples 05 06 01 04 03 02 Enabling Environment a. Assessment of legal and regulatory barriers for access to services for key affected populations JAMAICA AND HONDURAS, ARMENIA, UKRAINE, KYRGYZSTAN: Comprehensive assessment and work plans of legal and regulatory barriers for access to services for key and affected populations, leading to increasing investments on human rights related interventions in the countries and building the case to include costed-comprehensive human rights programs in the National Strategic Plans. BELARUS, BOSNIA AND HERZEGOVINA, KYRGYZSTAN, MOLDOVA, MONTENEGRO, SERBIA, TAJIKISTAN, UKRAINE AND UZBEKISTAN: using UNDP framework, countries completed assessment of legal framework related to CSO contracting as providers of prevention services for key and affected population. b. Support to CSOs for advocacy towards improved access and service quality monitoring c. Support CSOs inclusion in decision-making LATIN AMERICA AND CARIBBEAN MULTI-COUNTRY: Key actors in HIV and TB responses join forces to advocate for good quality and fully funded accessible services for key and vulnerable populations as well as enabling legal and policy environments for the HIV and TB responses. *Multicountry grant covers Bhutan, Lao, Malaysia, Sri Lanka, Mongolia, Papua New Guinea, Philippines and Timor-Leste SOUTH EAST ASIA MULTI-COUNTRY*: grant on ensuring sustainability of services for key populations via i) appropriate scale-up of service delivery for key populations including securing an enabling environment; ii) ensuring long-term programmatic and financial sustainability; and iii) enhancing capacity and leadership for continued advocacy from within key populations.
Community System Strengthening: Key areas of support and illustrative examples 05 06 01 04 03 02 Community System Strengthening a. Capacity building for CSOs to access public funding b. Support to MOH/CCM in the assessing optimal arrangements for public procurement of health services delivered by CSOs c. Budget advocacy for CSOs d. Step-by-step support to organizing public procurement of health services delivered by CSOs (from technical specifications, to contracts, to M&E) MONTENEGRO, SERBIA, GEORGIA, UKRAINE: alignment of unit costs for HIV prevention services of key population for improved efficiency and basis of domestic takeover of services. MACEDONIA: extensive support to ensure no disruption of service upon transition, advocacy and capacity building, resulting in $1 m annual domestic funding of HIV prevention services KOSOVO: comprehensive TA to set up policy and procedures for public procurement of health services delivered by CSOs. BELIZE: Support the setting up of an umbrella CSO network that helps organize and coordinate smaller CSOs to represent them in accessing public funding. COSTA RICA, DOMINICAN REPUBLIC, KAZAKHSTAN, MONGOLIA: Piloting CSO contracting under MOH with domestic co-financing GUYANA: coordinated support with partners to advocate and support development of procedures and implementation of public funding for CSOs. Launch of first public call for proposals in 2019. PANAMA: support to set up the policy and procedures for public procurement of health services delivered by CSOs BELIZE, BOLIVIA, PERU, PANAMA and DOMINICAN REPUBLIC: support to conduct social dialogues in countries to better prepare civil society for engaging on sustainability and transition discussions and planning, developing civil society priorities, and identifying key technical assistance gaps
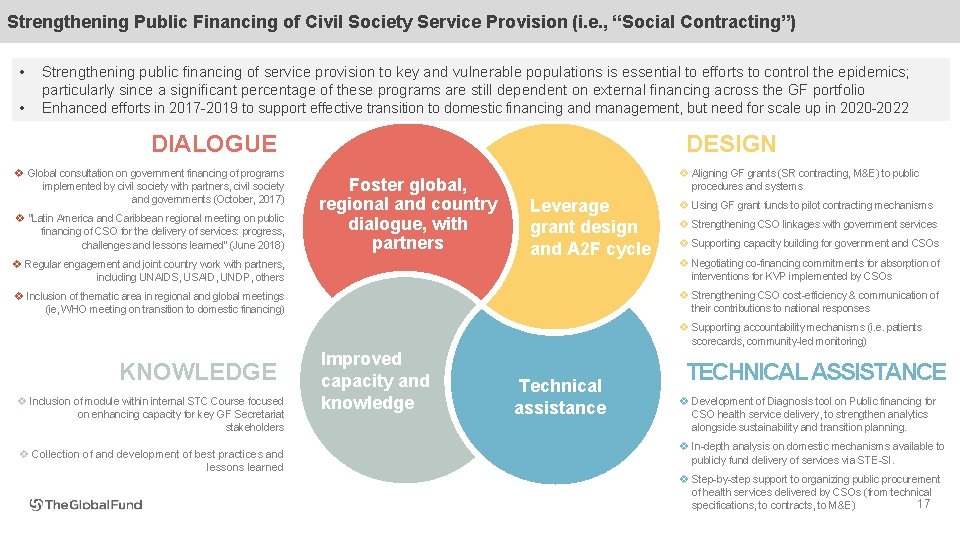
Strengthening Public Financing of Civil Society Service Provision (i. e. , “Social Contracting”) • • Strengthening public financing of service provision to key and vulnerable populations is essential to efforts to control the epidemics; particularly since a significant percentage of these programs are still dependent on external financing across the GF portfolio Enhanced efforts in 2017 -2019 to support effective transition to domestic financing and management, but need for scale up in 2020 -2022 DIALOGUE v Global consultation on government financing of programs implemented by civil society with partners, civil society and governments (October, 2017) v “Latin America and Caribbean regional meeting on public financing of CSO for the delivery of services: progress, challenges and lessons learned” (June 2018) DESIGN Foster global, regional and country dialogue, with partners v Regular engagement and joint country work with partners, including UNAIDS, USAID, UNDP, others v Aligning GF grants (SR contracting, M&E) to public procedures and systems Leverage grant design and A 2 F cycle v Using GF grant funds to pilot contracting mechanisms v Strengthening CSO linkages with government services v Supporting capacity building for government and CSOs v Negotiating co-financing commitments for absorption of interventions for KVP implemented by CSOs v Strengthening CSO cost-efficiency & communication of their contributions to national responses v Inclusion of thematic area in regional and global meetings (ie, WHO meeting on transition to domestic financing) v Supporting accountability mechanisms (i. e. patients scorecards, community-led monitoring) KNOWLEDGE v Inclusion of module within internal STC Course focused on enhancing capacity for key GF Secretariat stakeholders v Collection of and development of best practices and lessons learned Improved capacity and knowledge Technical assistance TECHNICAL ASSISTANCE v Development of Diagnosis tool on Public financing for CSO health service delivery, to strengthen analytics alongside sustainability and transition planning. v In-depth analysis on domestic mechanisms available to publicly fund delivery of services via STE-SI. v Step-by-step support to organizing public procurement of health services delivered by CSOs (from technical 17 specifications, to contracts, to M&E)
Strengthening Public Financing of Civil Society Service Provision (i. e. “Social Contracting”) Illustrative Examples MONTENEGRO, SERBIA, GEORGIA, UKRAINE: alignment of unit costs for HIV prevention services of key population for improved efficiency and basis of domestic takeover of services. KAZAKHSTAN, TAJIKISTAN: strengthening of CSOs capacity to deliver services + advocacy towards long-term sustainability DOMINICAN REPUBLIC, PANAMA, COSTA RICA: UKRAINE, BELARUS: grant support multiple pilots to setco-financing commitments+ key milestones up and strengthen CSO contracting at municipal, set in performance framework to ensure regional and national level institutional follow-up BELIZE: Support the setting up of an umbrella CSO network that helps coordinate smaller CSOs to represent them in accessing public funding. PANAMA, ALBANIA, KOSOVO: comprehensive TA to set up policy and procedures for public procurement of health services delivered by CSOs. GUYANA: coordinated support with partners to advocate and support development of procedures and implementation of public funding for CSOs + costing of CSOs services. Launch of first public call for proposals in Q 2 2019. PERU, BOLIVIA, PARAGUAY, SURINAME, HONDURAS, ECUADOR: Conducted Diagnosis tool on Public financing for CSO health service delivery COLOMBIA: grant designed to allow replication of the public contracting of CSO after GF exit MONTENEGRO, SERBIA: GF and domestic funds are managed together through national CSO contracting mechanisms. MOROCCO: manual outlining the modalities of engagement of CSOs with the MOH + trainings for CSOs on social contracting BOTSWANA: along with partners supported government to define a roadmap to put social contracting in place + support to develop the mechanisms. MULTI-COUNTRY GRANTS IN AELAC & MENA: grants focused on the sustainability of services for key and vulnerable populations, including increasing of domestic funding for interventions targeting KVP, strengthening/expanding CSO contracting mechanisms.

Efficiency: Key areas of support and illustrative examples 05 06 01 04 03 Efficiency 02 a. Support allocative efficiency studies b. Supporting technical efficiency (costing) studies c. Treatment and service delivery integration and optimization d. Encouraging crossprogrammatic integration analysis EECA: in partnership with UNAIDS is updating OPTIMA HIV estimates to prepare for 2020 -2022 Allocation cycle country dialogues ARMENIA, AZERBAIJAN, BELARUS, MOLDOVA, TAJIKISTAN, UKRAINE: piloting and evaluation of BELARUS: OPTIMA HIV results used in allocation performance-based financing for scaling up TB of resources for the next National Strategy and HIV case finding, OST schemes (shifted resources from general population prevention to PWID services) or using OST GEORGIA, MONGOLIA: Integration costing studies to support scale-up advocacy of HIV and Hepatitis C activities HAITI: Modelling to assess optimal size and geo-location of Community Health Workers nationally in collaboration with World Bank. JAMAICA and DOMINICAN REPUBLIC: Assessment of the integration of HIV program in the rest of the health system in terms of governance, health financing, health management system and service delivery and development of roadmap for incremental integration. HONDURAS, DOMINICAN REPUBLIC, GUYANA, JAMAICA, GUATEMALA, OECS: conducted technical efficiencies studies on prevention for key populations to identify opportunities for efficiency and quality improvement for prevention and testing services. Latin America: Increasing use of pool procurement mechanisms, resulting in significant efficiencies for certain country programs LAO: Integration of service delivery is encouraged through Payment for Result scheme at provincial level, and alignment with country systems is achieved via joint investment with WB NEPAL and PNG: Integration of service delivery at primary level and integration of support services and/or Integration of communicable disease programs with other vertical programs

Leveraging Catalytic Funding to Support STC Objectives Summary: Catalytic funding directly contributes to STC policy implementation by addressing strategic sustainability, transition and domestic financing challenges • Sustainability, Transition, and Efficiency Strategic Initiative (STE SI) ensures funds for technical assistance to strengthen transition planning, address specific transition challenges, strengthen capacity of key stakeholders on transition and sustainability, strengthen health expenditure tracking, provide TA for implementation of health financing strategies in priority portfolios, support domestic health financing advocacy in priority portfolios, and improve investment efficiency of GF supported programs by supporting allocative, cross-programmatic, and technical efficiency assessments across the GF portfolio • CRG Strategic Initiative supports engagement of community and key population groups in transition and sustainability processes, targeted TA and advocacy activities • Key Populations and Sustainability Multi-Country Funding provide 59. 5 million in funding to support multi-country and regional strategies to address key transition and sustainability challenges 20
- Slides: 20