Surviving sepsis campaign update By HP Shum 161107

Surviving sepsis campaign update By HP Shum 16/11/07

n Very boring

Introductions n Sepsis is a complex syndrome that is difficult to define, diagnose, and treat common definition for sepsis among the medical community would be a significant step toward better treatment doctors are eager for a breakthrough in treating sepsis symptoms of sepsis can easily be misattributed to other conditions Sepsis: a study of doctors’ knowledge about sepsis in five European countries and the US; ESICM and SCCM: January 2001

Introductions n n n Severe sepsis is the leading cause of death in the noncoronary ICU About 1/3 of the 750, 000 new cases that occur in the US each year are fatal More than 18 million cases of sepsis occur worldwide each year Sepsis kills some 1, 400 people worldwide every day The mortality rates associated with sepsis are extremely high: 30% to 50% for severe sepsis and 50% to 60% for septic shock Sepsis places a significant burden on healthcare resource, account for 40% of total ICU expenditure and costing up to $7. 6 billion annually in Europe and $16. 7 billion in the United States in 2000 Crit Care Med 2001; 29: 1303 -1310
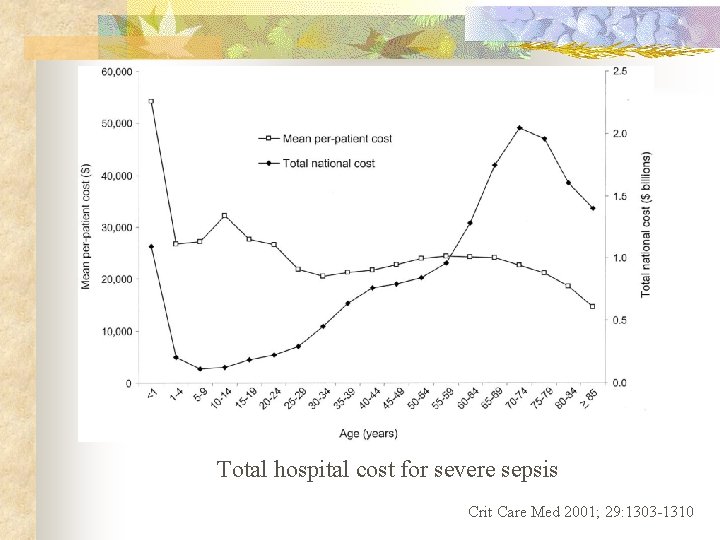
Total hospital cost for severe sepsis Crit Care Med 2001; 29: 1303 -1310

Introductions n The Society of Critical Care Medicine, the European Society of Intensive Care Medicine and the International Sepsis Forum joined forces to develop a threephase Surviving Sepsis Campaign

First phase n Campaign leaders introduced the initiative at major international critical care medicine conferences. They developed a six-point action plan to reduce global mortality from severe sepsis by 25% by 2009 n n n Building awareness of sepsis Improving early and accurate diagnosis Increasing the use of appropriate treatments and interventions Educating all healthcare professionals about diagnosis, treatment, and management of sepsis Improving access to post-ICU care for sepsis patients Developing global standards of care

Second phase n n Creating guidelines for sepsis management Publication of the guideline n n 3/04: CCM 4/04: ICM

Third phase n n Translating the guidelines into clinical practice Partnered with the Institute for Healthcare Improvement (IHI) to develop two sepsis bundles and to create a database-centered change measurement process

Bundles n n A "bundle" is a group of interventions related to a disease process that, when executed together, result in better outcomes than when implemented individually The individual bundle elements are built upon evidence-based practices

Severe Sepsis Resuscitation Bundle n n Seven tasks that should begin immediately, and must be accomplished within the first 6 hours of presentation for patients with severe sepsis or septic shock The goal is to perform all indicated tasks 100 percent of the time within the first 6 hours of identification of severe sepsis

Sepsis Management Bundle n n Four management goals. Efforts to accomplish these tasks should begin immediately, but these items may be completed within 24 hours of presentation for patients with severe sepsis or septic shock

Sepsis Resuscitation Bundle – 7 tasks

Check lactate Take blood c/st Give antibiotic MAP >=65 CVP >=8 mm. Hg Scv. O 2>=70 or Sv. O 2>=65 Compliance with all bundles

Measure serum lactate level n n n Hyperlactatemia is typically present in patients with severe sepsis or septic shock May be secondary to anaerobic metabolism due to hypoperfusion Significant prognostic values Circulation. 1970; 41: 989– 1001 Critical Care Medicine. 1983; 11: 449– 451 Critical Care Medicine. 1995; 23: 1184– 1193 n Even greater prognostic value than oxygenderived variables Chest. 1991; 99: 956– 962

Limitations n n n Interpretation not straight forward Elevated lactate levels may result from cellular metabolic failure in sepsis rather than from global hypoperfusion Also result from decreased clearance by the liver
Implication and turn-around time n All patients with elevated lactate > 4 mmol/L (36 mg/dl) will enter the early goal-directed therapy, regardless of blood pressure New England Journal of Medicine. 2001; 345: 1368– 1377 n n n Result must be available rapidly An arterial blood gas analyzer can be used The technique of obtaining serum lactate by venipuncture typically carries a 24 - to 48 -hour turn-around time and will not be suitable to care for septic patients

Obtain blood culture before antibiotic administration n 30 to 50 percent of patients presenting with a clinical syndrome of severe sepsis or shock have positive blood cultures European Journal of Clinical Microbiology and Infectious Diseases. 1998; 17: 377 – 384 New England Journal of Medicine. 2003; 348: 1546– 1554 n Collecting blood cultures prior to antibiotic administration offers the best hope of identifying the organism

Collect strategy n Two or more blood cultures are recommended Reviews of Infectious Diseases. 1983; 5: 35– 53 n n For suspected catheter-related infection, paired blood cultures obtained through the catheter hub and a peripheral site Volume of blood may also be important (7 -10 ml vs. <=3. 5 ml) Annals of Internal Medicine. 1993; 119: 270– 272

Indications of blood cultures n n n Fever, chills, hypothermia, leukocytosis, left shift of neutrophils, neutropenia, and the development of otherwise unexplained organ dysfunction Blood cultures should be taken as soon as possible Peaking fever appears to be more sensitive than leukocytosis to predict bacteremia Clinical and Diagnostic Laboratory Immunology. 2001; 8: 1189– 1195

Early administration of broad spectrum antibiotics n Reduces mortality in patients with Grampositive and Gram-negative bacteremias J Intern Med. 1998; 244: 379– 386 Chest. 1999; 115: 462– 474 Chest. 2000; 118: 146– 155 n From the time of presentation, broadspectrum antibiotics administered within 3 hours for ED admissions and 1 hour for non-ED ICU admissions Intens Care Med. 2004; 30(7): 1327 -1333

Choice of antibiotics n n Guided by the susceptibility of likely pathogens in the community, hospital, as well as any specific knowledge about the patient, including drug intolerance, underlying disease, the clinical syndrome Failure to initiate appropriate therapy promptly has adverse consequences on outcome Chest. 1999; 115: 462– 474 Chest. 2000; 118: 146– 155

Choice of antibiotics n Patients with severe sepsis or septic shock warrant broad-spectrum therapy until the causative organism and its antibiotic susceptibilities are defined

24 – 72 hr re-evaluation n Once the causative agent and antibiotic susceptibilities have been identified n n n Restrict of the number of antibiotics used Narrow the spectrum of antimicrobial therapy Minimizing the development of resistant pathogens Decreasing potential toxicity Containing costs The duration of therapy should typically be 7 to 10 days and guided by clinical response

Dosing of antibiotics n n n Full loading dose should be given Adjustment based on underlying renal / hepatic functions and abnormal volume of distribution ICU pharmacist should be consulted for maximize efficacy and minimize toxicity Ann Intern Med. 1996; 124: 717– 725 Clin Infect Dis. 1997; 24: 796– 809 Clin Pharm. 1995; 28: 143– 160

If hypotension and/or lactate >4 mmol/l, give initial minimum of 20 m. L/kg of crystalloid n n n Ineffective arterial circulation due to the vasodilatation associated with infection or impaired cardiac output Poorly perfused tissue beds result in global tissue hypoxia and give rise to elevated serum lactate level IVF expand their circulating volume and effectively restore perfusion pressure
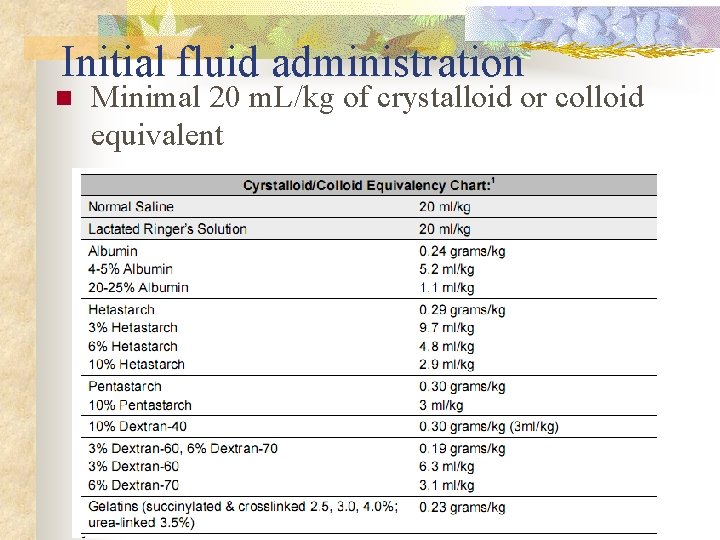
Initial fluid administration n Minimal 20 m. L/kg of crystalloid or colloid equivalent

Fluid challenge = Increased in maintenance fluid ? ? n n Fluid challenge = initial volume expansion period in which the response of the patient to fluid administration is carefully evaluated. Large amounts of fluids may be administered over a short period of time under close monitoring Require the definition of four components n n type of fluid rate of fluid infusion end points (eg improved MAP >=65 or HR <=100) safety limits (eg development of any pulmonary edema)

Type of fluid used n n Based on SAFE study (compare 4% albumin and NS), no mortality difference between 2 groups Subgroup analysis revealed that albumin might have some (albeit not statistically significant) benefit in patients with severe sepsis N Engl J Med. 2004; 350: 2247– 2256 n Meta-analyses of clinical studies comparing crystalloid and colloid resuscitation in general and surgical patient populations indicate no clinical outcome difference Crit Care Med. 1999; 27: 200– 210 Annals of Internal Medicine. 2001; 135: 205– 208 BMJ. 1998; 316: 961– 964

End points n Sv. O 2 >65% or Scv. O 2 >70% N Engl J Med. 2001; 345: 1368– 1377 Intens Care Med. 2004; 30: 1572– 1578 n n MAP >=65 mm. Hg Urine output, apparent skin perfusion, level of consciousness may be useful Carefully observed for evidence of pulmonary and systemic edema Input/output ratio is of no utility to judge fluid resuscitation needs during the initial 24 hr

Vasopressor use n n If not response to fluid challenge and MAP <65 mm. Hg May also be required transiently to sustain life and maintain perfusion in the face of life-threatening hypotension, even when hypovolemia has not been resolved or when a fluid challenge is in progress

Problems with vasopressors n n In inadequately volume-resuscitated patient, vasopressor may worsen already inadequate organ perfusion May raise blood pressure at the expense of the perfusion of vulnerable organs eg gut and kidney If an unnecessarily high blood pressure is targeted, may increase left ventricular work Continuous invasive blood pressure monitoring needed

Choice of vasopressor n Noradrenaline n n Potent -adrenergic agonist with some -adrenergic agonist effects Increase MAP by vasoconstrictive effect with elevated SVR Crit Care Med. 1987; 15: 134– 137 Crit Care Med. 1988; 16: 663– 666 Crit Care Med. 1989; 17: 179– 180 n n Can successfully increase blood pressure without causing the feared deterioration in organ function (splanchnic and renal vascular beds) Improving renal blood flow and renal vascular resistance in septic condition Intens Care Med. 1993; 19: 151– 154 Crit Care Med. 1989; 17: 426– 429 Crit Care Med. 1990; 18: 282– 285 n More effective than dopamine at reversing hypotension in septic shock patients Chest. 1993; 103: 1826– 1831

Choice of vasopressor n Dopamine n Increases MAP primarily by increasing cardiac index with minimal effects on systemic vascular resistance Am J Med. 1973; 54: 421– 432 Crit Care Med. 1997; 25: 399– 404 n n Increased SV more than HR May decrease intestinal mucosal p. H and impair gastroduodenal motility Intens Care Med. 2000; 26: 901– 907
CVP target n n n In the event of persistent hypotension despite fluid resuscitation (septic shock) and/or lactate > 4 mmol/L (36 mg/d. L), achieve central venous pressure (CVP) of > 8 mm Hg If a patient is both hypovolemic and anemic with a hematocrit less than 30 percent of blood volume, it is appropriate to transfuse packed red blood cells In mechanically ventilated patients, a higher target CVP of 12 to 15 mm Hg is recommended

Central venous oxygen target n n In the event of persistent hypotension despite fluid resuscitation (septic shock) and/or lactate > 4 mmol/L (36 mg/d. L) achieve central venous oxygen saturation (Scv. O 2) of > 70 percent or Mixed venous oxygen saturation (Sv. O 2) > 65 percent Evidence is not conclusive on attempting to maximize a patient’s cardiac index to surpranormal levels to overcome increased oxygen demand, abnormalities in oxygen extraction, and myocardial depression associated with sepsis N Engl J Med. 1995; 333: 1025– 1032 Crit Care Med. 1998; 26: 1011– 1019

Sepsis Management Bundle n n Four management goals. Efforts to accomplish these tasks should begin immediately, but these items may be completed within 24 hours of presentation for patients with severe sepsis or septic shock

Administer low dose steroid n n n Recommended in patients with septic shock who despite adequate fluid replacement require vasopressor therapy to maintain adequate blood pressure high-dose glucocorticoid trials have failed to improve outcome low-dose glucocorticoid trials refer to a daily dose of 200 to 300 mg of hydrocortisone or equivalent administered for 5 to 7 days or longer Crit Care Med. 1999; 27: 723– 732 Crit Care Med 1999; 27(1 S): 33 A Crit Care. 2002; 6: 251– 259

Hydrocortisone, Why? n Most of the experience with low-dose corticosteroid treatment in septic shock has been with the use of hydrocortisone JAMA. 2002; 288: 862– 871 Crit Care Med. 1998; 26: 645 -650 Intens Care Med. 2000; 26: 1747– 1755 n n Synthetic equivalent to the physiologic final active cortisol, therefore direct action independent of metabolic transformation Intrinsic mineralocorticoid activity

Role of corticotropin stimulation test n n Test is optional Clinicians should not wait for ACTH stimulation results to administer corticosteroids

Whether patients without relative adrenal insufficiency should be excluded from low-dose corticosteroid therapy? n NO !! n n n Response to corticosteroids may be less effective or even not effective in some responders Consensus concerning reference values for baseline and stimulated cortisol concentrations is missing patients with adequate adrenocortical function may also respond to low-dose corticosteroids

Mineralocorticoid use n Low-dose hydrocortisone plus fludrocortisone improve survival in septic shock JAMA. 2002; 288: 862– 871

Mineralocorticoid use n n However, no comparative study on hydrocortisone alone vs hydrocortisone plus fludrocortisone Absolute primary adrenal insufficiency is very rare Crit Care Med. 1998; 26: 627– 629 n Use is optional

Low dose hydrocortisone n Promote shock reversal Crit Care Med 1999; 27(1 S): 33 A Crit Care. 2002; 6: 251– 259 AJRCCM. 2003; 167: 512– 520 n Reduce vasopressor use Crit Care Med. 1998; 26: 645 -650 Crit Care Med. 1999; 27: 723– 732 n Decline of both, pro-inflammatory and antiinflammatory markers without immunosuppression AJRCCM. 2003; 167: 512– 520 n May improve survival JAMA. 2002; 288: 862– 871 Cochrane Database Systematic Review. 2005; 1: CD 002243

Use of Recombinant Activated Protein C n Recommended in patients at high risk of death n n n APACHE II > 25 sepsis-induced multiple organ failure septic shock sepsis-induced ARDS no absolute contraindication related to bleeding risk N Eng J Med. 2001; 344: 699– 709 Crit Care Med. 2003; 31: 12– 19 Crit Care Med. 2003; 31: 834– 840

PROWESS trial n n n Phase 3, multinational, double-blind, placebocontrolled trial evaluating rh. APC in patients with severe sepsis Trial was stopped early due to a statistically significant difference observed between the treatment and the placebo groups after recruited 1520 patients Significant reduction in the 28 -day all-cause mortality: absolute reduction of mortality, -6. 1 percent (30. 8 percent to 24. 7 percent); relative risk reduction of mortality by 19. 4 percent; reduction of in-hospital mortality (29. 4 percent vs. 34. 6 percent in the placebo group) N Eng J Med. 2001; 344: 699– 709 Chest. 2002; 122: 51 S

Potential side effects n Bleeding n n 24. 9 percent in the rh. APC group vs. 17. 7 percent in the placebo group ICH occurred and severe thrombocytopenia and a meningeal infection indicate high risk group

Practical recommendations n n rh. APC can only be administered until 12 hours after surgery or a major invasive procedure Patients with severe thrombocytopenia seem to carry a special risk of severe bleeding events (< 30, 000/mm 3 should not receive rh. APC) DIC patients can receive rh. APC except in severe consumption coagulopathy (platelets < 30, 000/mm 3; fibrinogen < 1, 000/mm 3; prothrombin time < 30 percent) Heparin might reduce the efficacy of rh. APC Crit Care Med. 2003; 31: 834– 840 Intens Care Med. 2003; 29: 894– 903

Cost effectiveness n n Analysis of the PROWESS trial could document a $27, 400 cost per qualityadjusted life-year when limited to patients with an APACHE II score of 24 Cost ineffective in patients with a lower risk of death N Eng J Med. 2002; 347: 993– 999 Crit Care Med. 2003; 31: 1– 11

Cost effectiveness

Maintain adequate glycemic control n n n Insulin resistance is a common finding in intensive care unit patients Conventional wisdom in the ICU has been that hyperglycemia is beneficial and that hypoglycemia is dangerous However, controlling blood glucose levels by intensive insulin therapy decreased mortality and morbidity (infection, dialysis needs, prolonged mechanical ventilation) in surgical critically ill patients New England Journal of Medicine. 2001; 345: 1359– 1367

How tight? n n Aim 4. 4 -6. 1 mmol/l significantly increased risk of hypoglycemia Achieve target of 8. 3 mmol/l still can improve outcome but risk of hypoglycemia lower

Nutritional support n n Strategy of glycemic control should include a nutrition protocol with the preferential use of the enteral route Initiating glycemic control without adequate provision of calories and carbohydrates will increase the risk of hypoglycemia

Insulin vs normoglycemia n Insulin has been shown to inhibit TNF- , provide favorable effects on coagulation / fibrinolysis, and on macrophage function Journal of the National Cancer Institute. 1985; 74: 1255– 1260 Journal of Diabetes and its Complications. 2001; 15: 44– 54 Journal of Clinical Endocrinology and Metabolism. 2001; 86: 3257– 3265 Journal of Parenteral and Enteral Nutrition. 1997; 21: 91– 95 n Is insulin alone rather than normoglycemic effect resulting in improved outcome ? ? n n n Van den Berghe et al. reanalyzed the data daily dose of insulin and the mean blood glucose level were independent positive predictors of mortality low level of blood glucose, rather than a high insulin dose protect against ICU complications Critical Care Medicine. 2003; 31: 359– 366

Prevent excessive insp. plateau pressure n n Nearly 50 percent of patients with severe sepsis will develop ALI / ARDS Use low tidal volume (6 m. L·kg-1·lean body weight-1) and maintaining end-inspiratory plateau pressures of < 30 cm H 2 O can achieve 9% decrease in mortality compared with conventional methods New Engl J Med. 2000; 342: 1301– 1308 n Moderate hypercapnia Crit Care Med. 1994; 22: 1568– 1578 JAMA. 1994; 272: 957– 962 n Setting PEEP based on severity of oxygenation deficit and guided by the FIO 2 required

Chart review database n n n A database to record the management issues of septic patients following the guideline Help collect data across units and institutions in order to gauge success with the surviving sepsis campaign quality indicators Program will generate graphs and reports on the overall progress and compliance








The End

Advantage of “bundle” n n n Clearly articulate a framework that promote changes Eliminate the piecemeal or inappropriate application of standards for sepsis care Achieve clinical improvement

How to set up a bundle? n n Identify a set of four to six evidence-based interventions that apply to a cohort of patients with a common disease or a common location. An example might be patients with sepsis admitted to the intensive care unit. Develop the will in the providers to deliver the interventions every time they are indicated.

How to set up a bundle? n n n Measure compliance as “All” or “None” Redesign the delivery system to ensure the interventions in the bundle are delivered. Measure related outcomes to ascertain the effects of the changes in the delivery system.

How to use the bundles? n n n Hospitals should use the bundles to create customized protocols and pathways that will function well within their institutions However, all of the elements in the bundles must be incorporated in those protocols. Addition of other strategies not found in the bundles is not recommended
- Slides: 73