Surveillance of MethicillinResistant Staphylococcus From the Ocular Surface









- Slides: 12

Surveillance of Methicillin-Resistant Staphylococcus From the Ocular Surface of Cataract Surgery Patients Eric Donnenfeld, MD 1; Randall Olson, MD 2; Kerry Solomon, MD 3; R. Bruce Wallace, MD 4; Taryn Conway, BS 5; Rhett Schiffman, MD 5; David Hollander, MD 5 1 Ophthalmic Consultants of Long Island Connecticut, Rockville Centre, NY; 2 The John A. Moran Eye Center, University of Utah, Salt Lake City, UT; 3 Ophthalmology, Medical University of South Carolina, Charleston, SC; 4 Wallace Eye Surgery, Laser and Surgery Center, Alexandria, LA; 5 Allergan, Inc. , Irvine, CA Financial Disclosures This study was funded by Allergan, Inc. , Irvine, CA. Drs. E. Donnenfeld, R. Olson, K. Solomon, and R. B. Wallace are consultants to Allergan, Inc. Ms. T. Conway and Drs. R. Schiffman and D. Hollander are employees of Allergan, Inc.

INTRODUCTION Endophthalmitis is a rare, yet potentially devastating complication following cataract extraction. 1 -4 The ocular surface (lids and conjunctiva) and nasal flora are the predominant source of bacteria leading to postoperative endophthalmitis. 5 -7 The Endophthalmitis Vitrectomy Study (EVS) demonstrated that the vast majority of cases of postcataract endophthalmitis arise secondary to Gram-positive organisms, including Staphylococcus epidermidis and S aureus. 8 Methicillin-resistant staphylococcal infections are on the rise and no longer confined to healthcare workers. 4, 9 -12 This study was designed to determine the bacteria present on the ocular surface (lids and conjunctiva) in patients undergoing cataract surgery. An additional goal of the study was to evaluate the presence of oxacillin (methicillin)–resistant bacterial species on the ocular surface of both healthcare and non-healthcare workers.

METHODS A multicenter (10 sites), prospective study. Swabs were performed on the superior lid lash margin and inferior tarsal conjunctiva of the nonsurgical eye of patients undergoing cataract surgery at the time of operation. Gram-negative bacteria were speciated by the BBL™ Enterotube™ II. Gram-positive bacteria were tested for the presence of catalase to separate Staphylococcus species from other Gram-positive bacteria. § Staphylococcal species were identified using the API® Staph kit (bio. Mérieux , Inc. ; Durham, NC). Susceptibility to oxacillin was tested by Etest® (oxacillin [OX], AB Biodisk; Solna, Sweden) in Staphylococcus species. § The oxacillin breakpoints were ≤ 2 µg/m. L (sensitive) and ≥ 4 µg/m. L (resistant) for S aureus and S lugdunensis and ≤ 0. 25 µg/m. L (sensitive) and ≥ 0. 5 µg/m. L (resistant) for all other coagulase-negative staphylococci.

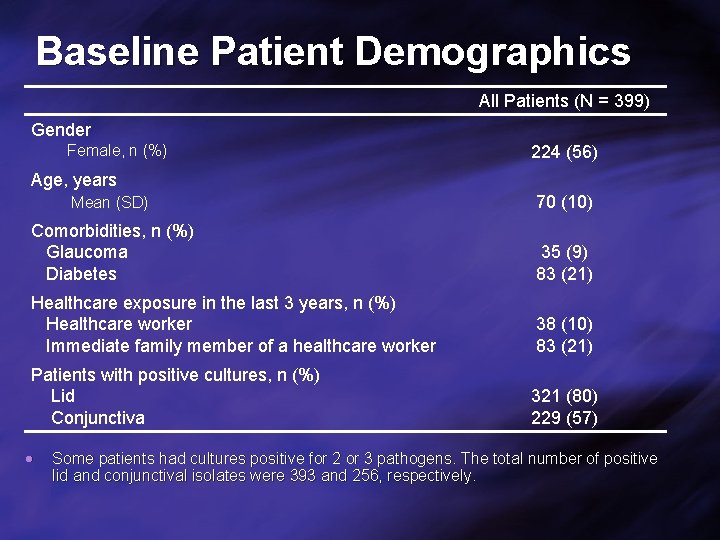
Baseline Patient Demographics All Patients (N = 399) Gender Female, n (%) 224 (56) Age, years Mean (SD) 70 (10) Comorbidities, n (%) Glaucoma Diabetes 35 (9) 83 (21) Healthcare exposure in the last 3 years, n (%) Healthcare worker Immediate family member of a healthcare worker 38 (10) 83 (21) Patients with positive cultures, n (%) Lid Conjunctiva 321 (80) 229 (57) Some patients had cultures positive for 2 or 3 pathogens. The total number of positive lid and conjunctival isolates were 393 and 256, respectively.

Bacterial Species on the Ocular Surface of Cataract Surgery Patients Lid Conjunctiva S aureus n = 31 (12%) S aureus n = 60 (15%) S epidermidis n = 243 (62%) Micrococcus species %) 5 ( 18 n= S xylosus n = 12 (3%) n = 9 (2%) S warneri n n == 9 (2%) S lugdunensis n = 7 (2% ) 2 n S capitis = 1 1 (5% ) Other Gram-positive 4( 4% ) bacteria 3 =1 S epidermidis n = 165 (64%) Gram-negative bacteria (N = 393) (5 %) Micrococcus species S capitis ) n (3% 7 n = = 6 (2%) S warneri n n = 6 (2%) S lugdunensis n = 12 (5 %) Other Gram-positive n= bacteria n = 9 (4% ) Enterobacter 7( 3% agglomerans ) Other Gram-negative bacteria (N = 256) The majority of positive lid (303/393; 77%) and conjunctival (196/256; 76%) isolates were either S epidermidis or S aureus.

Oxacillin (Methicillin) Susceptibility of Lid Staphylococcus Species S epidermidis (n = 224)a 34% S aureus (n = 59)a S xylosus (n = 12) 8)a S warneri (n = S lugdunensis (n = 9) 48% 51% 59% 58% 42% 0% 88% 33% 66% 17% S capitis (n = 6) Oxacillin Resistant Oxacillin Susceptible 83% S hominis (n = 4) 0% 100% S caprae (n = 2) 50% S haemolyticus (n = 2) 50% S saprophyticus (n = 2)a 0% S lentus (n = 1) 0% 50% 100% S sciuri (n = 1) 0% S cohnii spp urealyticus (n = 1) 100% 0% Percentage of Staphylococcus Species a. Four (7%) S aureus, 2 (1. 0%) S epidermidis, 1 (50%) S saprophyticus, saprophyticus and 1 (12%) S warneri were intermediately resistant to oxacillin. Oxacillin (methicillin) susceptibility was tested on 331 (92%) of 358 lid staphylococci. The rate of oxacillin (methicillin) resistance was highest among lid S xylosus (58%), followed by S epidermidis (48%) and S aureus (34%).

Oxacillin (Methicillin) Susceptibility of Conjunctival Staphylococcus Species 45% S epidermidis (n = 154)a 21% S aureus (n = 29)a S warneri (n = 5) S lugdunensis (n = 5) 100% 0% 100% 25% S caprae (n = 3)a 75% 33% 0% S haemolyticus (n = 3) S xylosus (n = 2) 76% 0% S capitis (n = 4) S hominis (n = 3) Oxacillin Resistant Oxacillin Susceptible 52% 0% 100% 33% 67% 100% Percentage of Staphylococcus Species a. Four (3%) S epidermidis, 1 (3%) S aureus, and 1 (33%) S caprae were intermediately resistant to oxacillin. Oxacillin (methicillin) susceptibility was determined for 208 (92%) of 227 conjunctival staphylococci. The rate of oxacillin (methicillin) resistance was 45% among conjunctival S epidermidis and 21% among S aureus species.

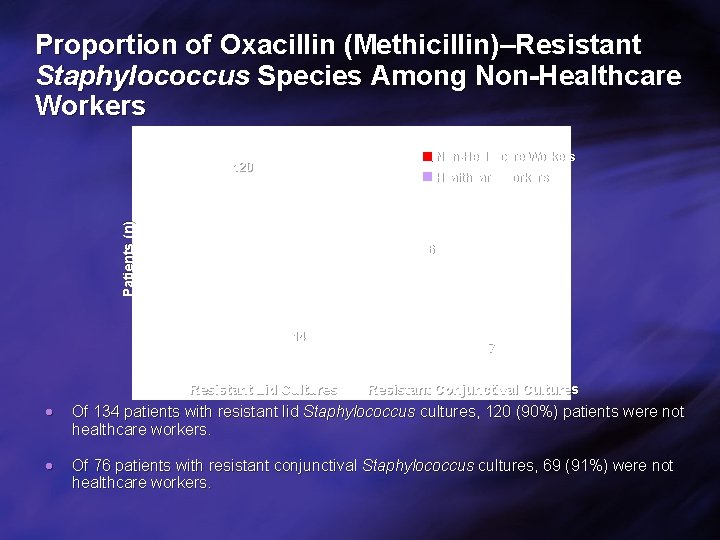
Proportion of Oxacillin (Methicillin)–Resistant Staphylococcus Species Among Non-Healthcare Workers 120 Patients (n) Healthcare Workers 69 14 Resistant Lid Cultures 7 Resistant Conjunctival Cultures Of 134 patients with resistant lid Staphylococcus cultures, 120 (90%) patients were not healthcare workers. Of 76 patients with resistant conjunctival Staphylococcus cultures, 69 (91%) were not healthcare workers.

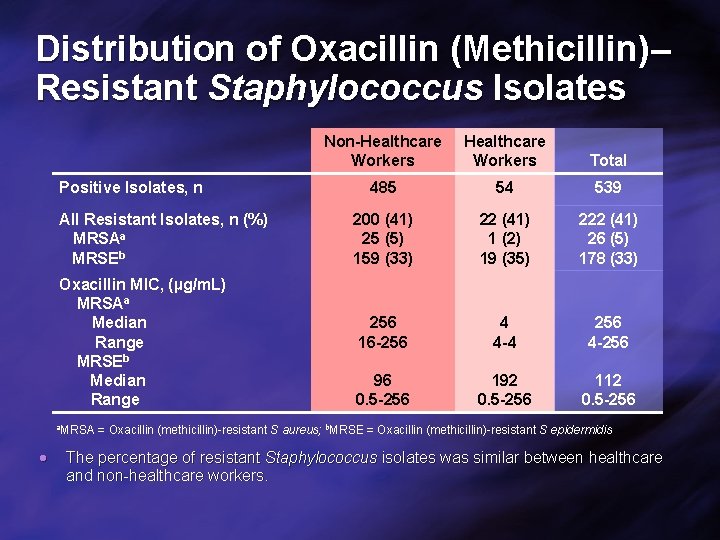
Distribution of Oxacillin (Methicillin)– Resistant Staphylococcus Isolates Positive Isolates, n All Resistant Isolates, n (%) MRSAa MRSEb Oxacillin MIC, (µg/m. L) MRSAa Median Range MRSEb Median Range a. MRSA Non-Healthcare Workers Total 485 54 539 200 (41) 25 (5) 159 (33) 22 (41) 1 (2) 19 (35) 222 (41) 26 (5) 178 (33) 256 16 -256 4 4 -4 256 4 -256 96 0. 5 -256 192 0. 5 -256 112 0. 5 -256 = Oxacillin (methicillin)-resistant S aureus; b. MRSE = Oxacillin (methicillin)-resistant S epidermidis The percentage of resistant Staphylococcus isolates was similar between healthcare and non-healthcare workers.

DISCUSSION Over 75% of bacterial isolates on the ocular surface (lids and conjunctiva) of cataract surgery patients were either S epidermidis or S aureus. Overall, approximately one-half of S epidermidis isolates and onequarter of S aureus isolates were resistant to oxacillin (methicillin). The percentage of Staphylococcus isolates resistant to oxacillin (methicillin) was similar between healthcare and non-healthcare workers. The high rate of oxacillin (methicillin)–resistant Staphylococcus species on the ocular surface of cataract surgery patients underscores the need to use an antibiotic in the perioperative period with a favorable profile against Gram-positive species, including Oxacillin (methicillin)–resistant S aureus (MRSA) and Oxacillin (methicillin)–resistant S epidermidis (MRSE).

CONCLUSIONS • S epidermidis and S aureus were the most common bacterial species identified on the ocular surface of cataract surgery patients. • A significant portion of ocular surface staphylococcal species were resistant to oxacillin (methicillin), even among non-healthcare workers.

References 1. Barry et al. J Cataract Refract Surg. 2006; 32(3): 407 -410. 2. Jensen et al. J Cataract Refract Surg. 2008; 34(9): 1460 -1467. 3. Lalwani et al. Ophthalmology. 2008; 115(3): 473 -476. 4. Miller et al. Ophthalmic Surg Lasers Imaging. 2007; 38(6): 446 -451. 5. Speaker et al. Ophthalmology. 1991; 98(5): 639 -649. 6. Bannerman et al. Arch Ophthalmol. 1997; 115(3): 357 -361. 7. Kenchappa et al. BMC Ophthalmol. 2006; 6: 1 -5. 8. Han et al. Am J Ophthalmol. 1996; 122(1): 1 -17. 9. Cavuoto et al. Ophthalmology. 2008; 115(1): 51 -56. 10. Freidlin et al. Am J Ophthalmol. 2007; 144(2): 313 -315. 11. Klevens et al. JAMA. 2007; 298(15): 1763 -1771. 12. Blomquist. Trans Am Ophthalmol Soc. 2006; 104: 322 -345.