Surgicopathology Presented by Dr Ryan Fernandes Moderator Dr

Surgico-pathology Presented by- Dr Ryan Fernandes Moderator- Dr Ramdas Rai

� Name: Mrs x � Age: 47 yrs � Sex: Female � Residence: Kannur � Occupation: Home maker �Chief Complaint: �Lump in her left breast for 1 month

History of present illness: Patient was admitted with C/O lump in the left breast for 1 month. It was about 4 cm in size when first noticed, with mild increase in size thereafter over 1 month. The lump was not associated with pain. No H/O trauma to the breast. No H/O fever. No H/O skin changes or discharge from the nipple. No H/O weight loss.

Past history: No history suggestive of benign breast disease in the past. No past surgical history. No h/o HTN, TB, bronchial asthma, DM. Personal history: diet : mixed appetite: normal sleep: undisturbed bowel and bladder habits: normal No history of substance abuse

OBG History : Menarche at 14 years First child birth at 24 yrs Two children (FTND), both were breast fed for one and half years. No history of abortions. Menstrual cycles regular – 30/4 -5 days Family history: No history of carcinoma breast or ovary among her mother or sisters. No history of GI malignancies in her family.

General Physical Examination: Moderately built and nourished No pallor, icterus, cyanosis , clubbing, pedal oedema. Vital Signs: Afebrile Pulse rate: 80 b/min BP : 126/80 mm. Hg in the rt arm supine position.

Examination of breast: INSPECTION : Both the breasts were normal in shape and position : Peau de orange appearance of skin over the left breast in relation to the upper margin of the areola : No engorged veins, no ulceration : Both the nipples and areola were normal in shape & position. : No discharge from the nipple.

PALPATION Left breast : No local rise in temperature : No tenderness : A single lump was palpated in the upper inner quadrant measuring vertically 5 cm × horizontally 4 cm : Surface of the lump was irregular with ill defined margin. : Hard in consistency

: The lump was mobile : Tethered to the skin : It was not fixed to the pectoralis major or serratus anterior muscles : Three lymph nodes were palpated in the central group of axilla, largest measuring 2*2 cm. firm, nontender, mobile, discrete. No supraclavicular lymph nodes palpated. Palpation of Right breast and axilla were normal.

Systemic examination: Ø P/A: Soft, non-tender, no palpable mass, BS- heard PV/PR - Normal Ø RS: NVBS, No added sounds Ø CVS: S 1 and S 2 heard. Ø CNS: Normal

Diagnosis Carcinoma left breast with axillary lymph node involvement, with no signs of distant metastasis (T 4 N 1 M 0)

Investigations: >Hb: 13. 5 g% >Tc: 7800 cells/cumm >DC: N- 68%, L-30%, E-02% >ESR: 15 mm/1 hr >RBS: 184 mg/dl >RFT: Urea-22 mg/dl : Creatinine- 0. 7 mg/dl

Urine: Within normal limits >HIV: -ve >HBs. Ag: -ve >Chest X-ray: Normal >USG Abdomen: Normal study >FNAC: infiltrating duct carcinoma

The patient underwent a Left Modified Radical Operative Procedure Mastectomy under GA on 2 -01 -2012 �Breast tissue containing nipple-areola complex and 3 cm of skin circumferentially, and axillary pad of fat containing multiple lymph nodes, was excised. �Level II lymph nodes were excised after dividing the pectoralis minor muscle. �Both specimens were sent for histopathological evaluation.

HISTOPATHOLOGY 1) BREAST + Axillary fat containing lymph nodes 2) Level II lymph node IMP- Infiltrating ductal carcinoma, NOS with 7 lymph nodes showing tumor deposits. ER/PR - Positive

Breast Cancer -Discussion �The overall incidence of breast cancer has been rising because of increases in average life span, lifestyle changes that increase risk for breast cancer & improved survival from other diseases. �Breast cancer is the most common cause of death in middle aged women in western countries �In India - 28. 9 women per 100, 000 population suffer from breast cancer.

Risk Factors �Age - Commonly seen after 30 yrs of age �Gender -(female>>Male) �Age at Menarche - 10% with each year that its delayed �Age at Menopause - Late onset �Age at 1 st child birth after 30 yrs of age �Breast Feeding

Risk Factors - Contd • Exogenous hormone use – OCPs /HRT • Family History • History of previous breast cancer • Diet

Genetic Factors �BRCA 1, CHR 17 - 40% of familial breast cancer syndromes. � BRCA 2, CHR. 13 - 30% of familial breast cancer Associated with increased breast cancer risk in males. Women with a mutation in BRCA 2 also have a 20% to 30% lifelong risk of ovarian cancer.

Clinical Presentations �Lump in the breast , hard & painless, commonly upper & outer quadrant �Discharge from nipple �Axillary lymph node enlargement, suprclavicular �Peau d’Orange – obstruction of cutaneous lymphatics �Dimpling of skin- infiltration of ligament of Cooper �Retraction of nipple – due to infiltration of lactiferous duct �Ulceration �Cancer –en- cuirasse- fixity to chest wall

Modes of Spread �Local Spread Tumour increases in size & invades other portion s of the breast. It tends to involve the skin , pectoral muscles & chest wall if diagnosed late

Modes Of spread �Lymphatic Spread - Occurs primarily to the axillary & internal mammary lymph nodes - Tumors in the posterior 1/3 rd of the breast drain into the internal mammary nodes Lymphatic Permeation Lymphatic Embolisation Opposite breast- through dermal lymphatics

Haematogenous Spread �Bone- Lumbar, femur, thoracic, ribs, skull �Lungs & Pleura �Soft tissues �Liver �Brain �Adrenals

Management

TRIPLE ASSESSMENT �CLINCAL ASSESSMENT. �RADIOLOGICAL IMAGING. �TISSUE DIAGNOSIS
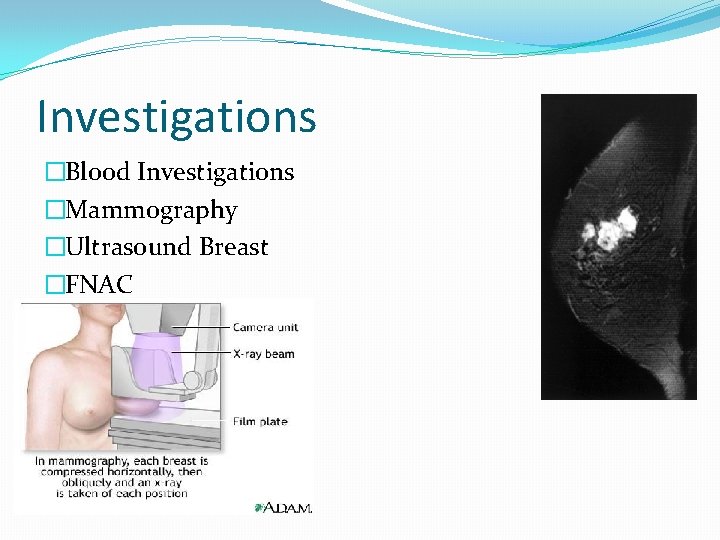
Investigations �Blood Investigations �Mammography �Ultrasound Breast �FNAC
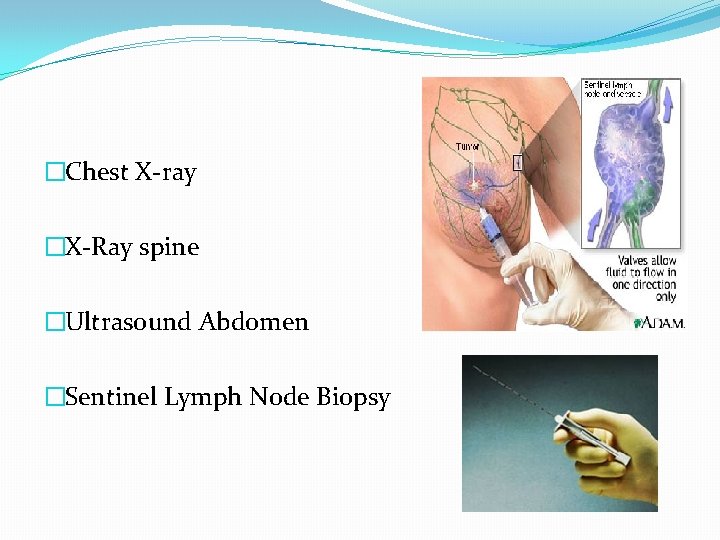
�Chest X-ray �X-Ray spine �Ultrasound Abdomen �Sentinel Lymph Node Biopsy
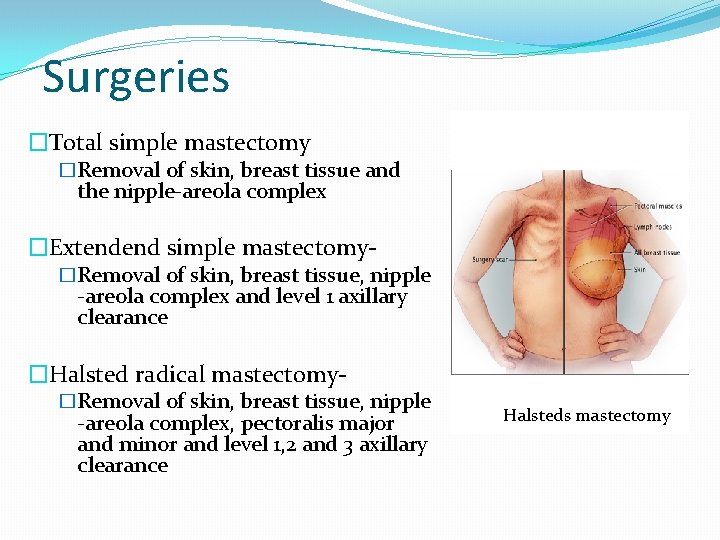
Surgeries �Total simple mastectomy �Removal of skin, breast tissue and the nipple-areola complex �Extendend simple mastectomy- �Removal of skin, breast tissue, nipple -areola complex and level 1 axillary clearance �Halsted radical mastectomy- �Removal of skin, breast tissue, nipple -areola complex, pectoralis major and minor and level 1, 2 and 3 axillary clearance Halsteds mastectomy
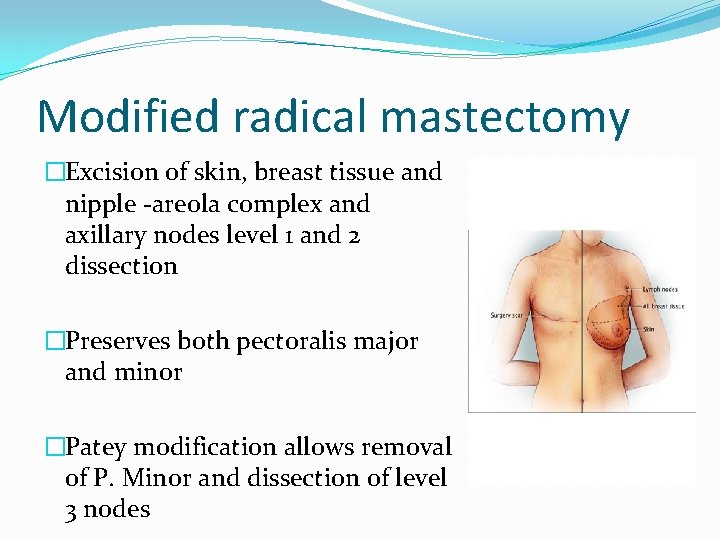
Modified radical mastectomy �Excision of skin, breast tissue and nipple -areola complex and axillary nodes level 1 and 2 dissection �Preserves both pectoralis major and minor �Patey modification allows removal of P. Minor and dissection of level 3 nodes
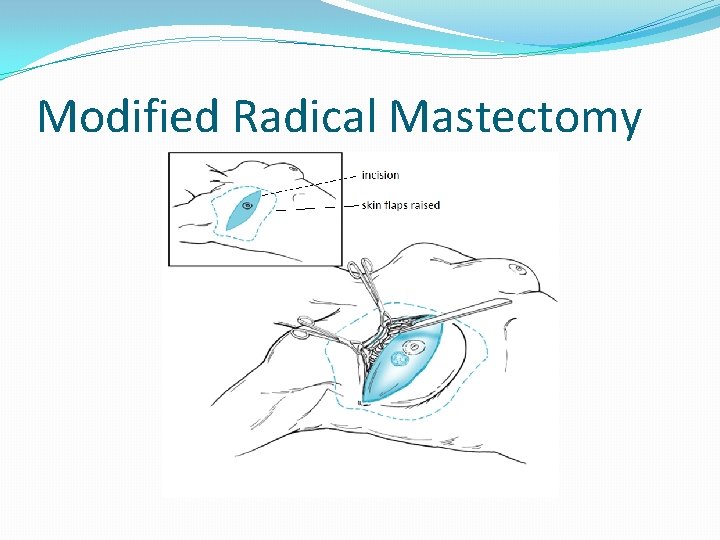
Modified Radical Mastectomy
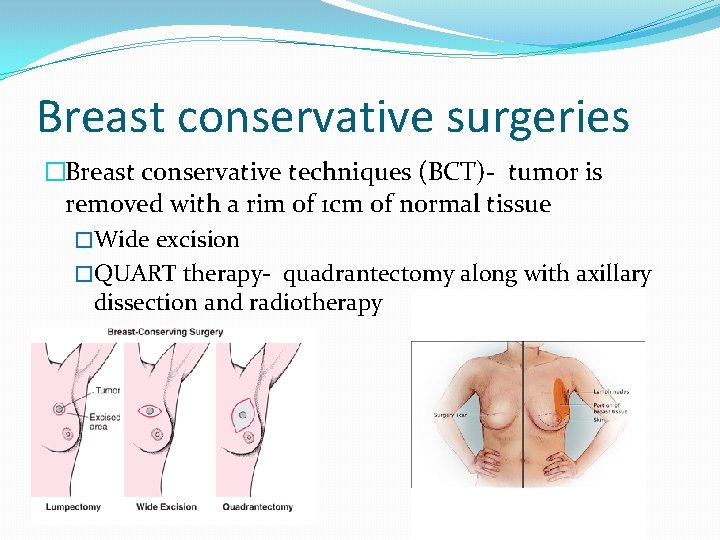
Breast conservative surgeries �Breast conservative techniques (BCT)- tumor is removed with a rim of 1 cm of normal tissue �Wide excision �QUART therapy- quadrantectomy along with axillary dissection and radiotherapy

Radiotherapy �Necessary for patients who undergo conservative breast surgeries �After total mastectomy, radiation to the axilla �Useful in bone secondaries to palliate pain and swelling �As a pre operative procedure to de bulk the tumor
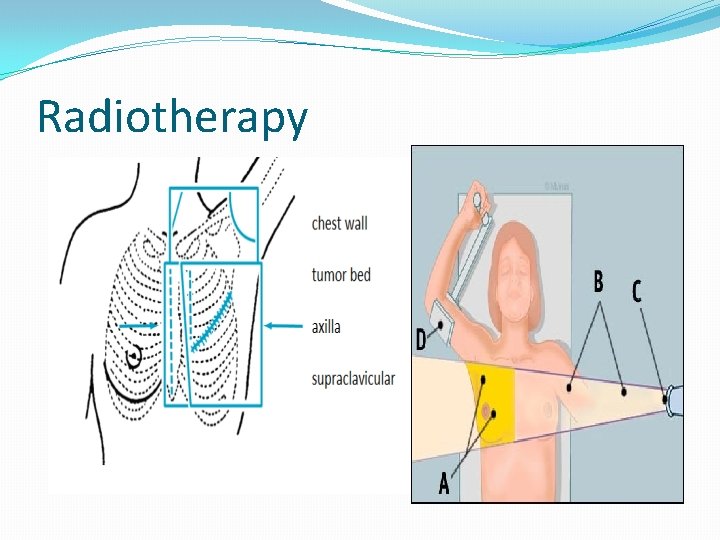
Radiotherapy

�Whole breast radiation (WBR) given over �Breast �Axilla �Internal mammary nodes �Supraclavicular node � 200 c. GY units daily administered 5 days a week for 6 weeks �Total dosage 5000 c. GY units and additional 1000 units to the tumor bed

Systemic therapy �Chemotherapy �Hormonal therapy

Chemotherapy �In poorly differentiated tumors �All node positive patients �In stage 4 with secondaries �Commonly monthly cycles for 6 months �Also neo-adjuvant therapy to decrease the size of the tumor

Regimes �CMF- ◦ Cyclophosphamide ◦ Methotrexate ◦ 5 -fluorouracil �CAF- ◦ Cyclophosphamide ◦ Adriamycin ◦ 5 -fluorouracil alopecia bone marrow suppression cystitis megaloblastic anemia GIT disturbances nephritis �MMM- ◦ Methotrexate ◦ Mitomycin- C ◦ Mitozantrone Newer agents like doxorubicin, taxanes like paclitaxel, docetaxel are recently used

Hormonal therapy �Used in ER/PR positive patients �Prophylaxis against carcinoma of opposite breast �Useful after wide local excision �Reduces recurrence rate and improves quality of life and increases life span

�Includes �Tamoxifen- 10 mg bd for 5 years �Oral aromatose inhibitors like letrozole & anastrozole for post menopausal women �Ovarian ablation by surgery- B/L oophorectomy �Adrenalectomy or pituitary ablation �LHRH agonists (medical oopherectomy) �Herceptin for HER-2 positive patients

NEOADJUVANT CHEMO THERAPY �SYSTEMIC CHEMOTHERAPY GIVEN BEFORE LOCAL THERAPY �SYNONYMSPRIMARY CHEMOTHERAPY INDUCTION CHEMOTHERAPY � 10 -30% SHOW COMPLETE RESPONSE � 50 -60% PATIENTS SHOW PARTIAL RESPONSE

RATIONALE �TO ACHIEVE EARLY CONTROL OF DISTANT METS �TO DOWN STAGE THE DISEASE �FOR INVIVO ASSESSMENT OF TUMOUR RESPONSIVENESS �TO REDUCE THE TUMOUR BURDEN AT THE PRIMORY SITE

DISADVANTAGES �RISK OF DRUG RESISTANCE �SURGERY/ RADIOTHERAPY COULD BE DELAYED IN CASE OF NONRESPONDERS �INACCURATE PATHOLOGICAL STAGING

A H T U O Y K N
- Slides: 43