Surgical treatment analysis of 809 thoracolumbar and lumbar

Surgical treatment analysis of 809 thoracolumbar and lumbar major adult deformity cases by a new adult scoliosis classification system F Schwab, JP Farcy, K Bridwell, S Berven, S Glassman, W Horton, M Shainline Spinal Deformity Study Group September 28, 2005. Philadelphia Zorab Symposium 2006
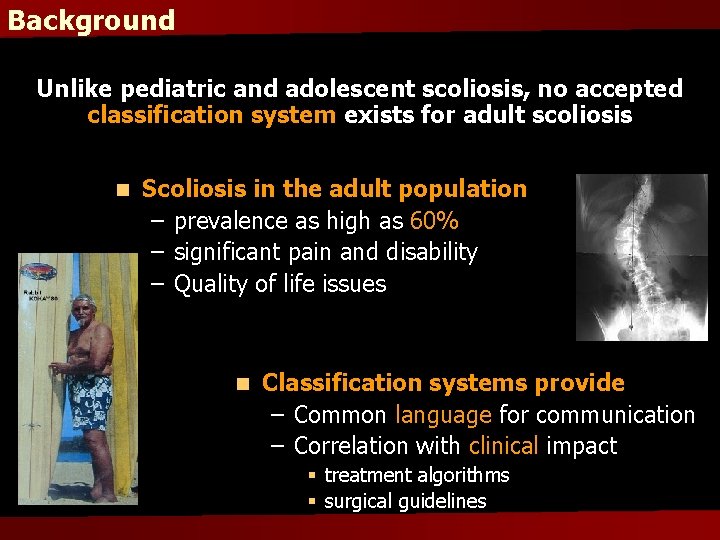
Background Unlike pediatric and adolescent scoliosis, no accepted classification system exists for adult scoliosis n Scoliosis in the adult population – prevalence as high as 60% – significant pain and disability – Quality of life issues n Classification systems provide – Common language for communication – Correlation with clinical impact § treatment algorithms § surgical guidelines
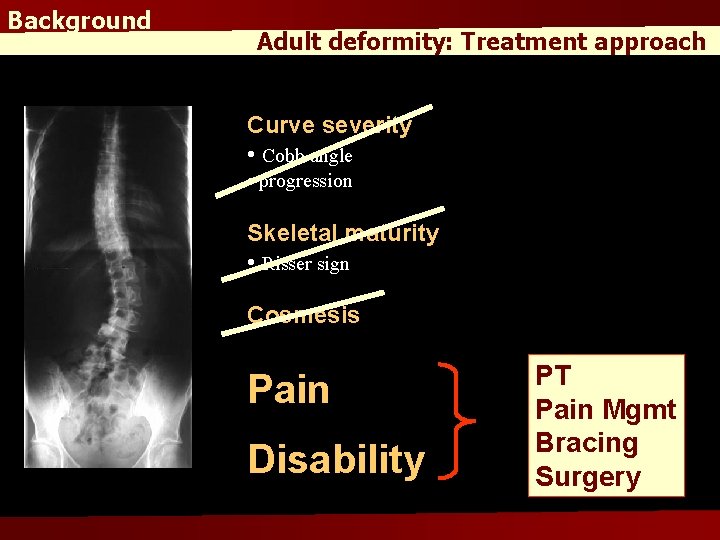
Background Adult deformity: Treatment approach Curve severity • Cobb angle • progression Skeletal maturity • Risser sign Cosmesis Pain Disability PT Pain Mgmt Bracing Surgery
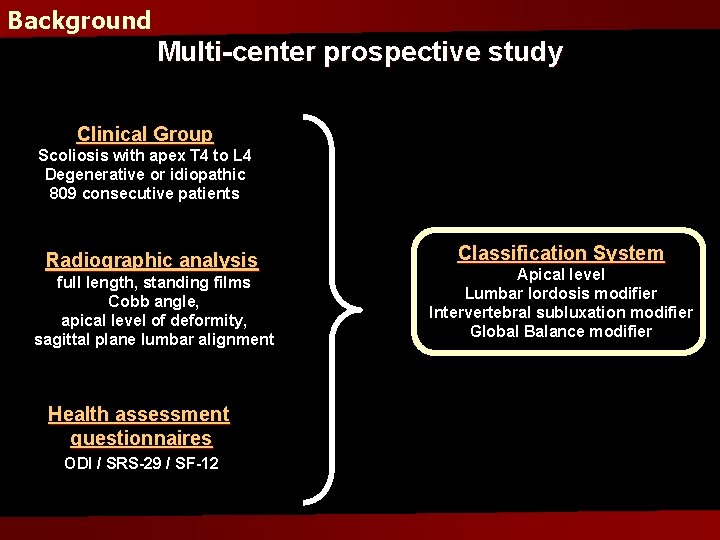
Background Multi-center prospective study Clinical Group Scoliosis with apex T 4 to L 4 Degenerative or idiopathic 809 consecutive patients Radiographic analysis full length, standing films Cobb angle, apical level of deformity, sagittal plane lumbar alignment Health assessment questionnaires ODI / SRS-29 / SF-12 Classification System Apical level Lumbar lordosis modifier Intervertebral subluxation modifier Global Balance modifier
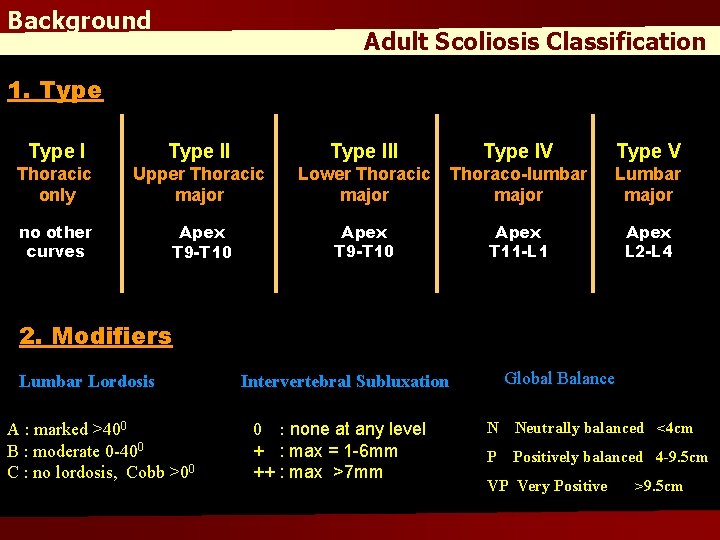
Background Adult Scoliosis Classification 1. Type III Type IV Type V Thoracic only Upper Thoracic major Lower Thoracic major Thoraco-lumbar major Lumbar major no other curves Apex T 9 -T 10 Apex T 11 -L 1 Apex L 2 -L 4 2. Modifiers Lumbar Lordosis A : marked >400 B : moderate 0 -400 C : no lordosis, Cobb >00 Global Balance Intervertebral Subluxation 0 : none at any level + : max = 1 -6 mm ++ : max >7 mm N Neutrally balanced <4 cm P Positively balanced 4 -9. 5 cm VP Very Positive >9. 5 cm
Purpose Adult Scoliosis Classification Reliable classification with significant correlation to clinical symptoms Prediction of treatment patterns and surgical rates ? ? ?

Materials & Methods 1. Clinical group • • Spinal Deformity Study Group database Prospective, consecutive 809 patients review Ages > 18 y. o. Thoracolumbar or lumbar major scoliosis • Type IV and Type V deformities only. 2. Health questionnaires • Oswestry Disability Index (ODI) ODI • Scoliosis Research Society instrument (SRS-22) SRS-22 • Short From 12 (SF-12) SF-12
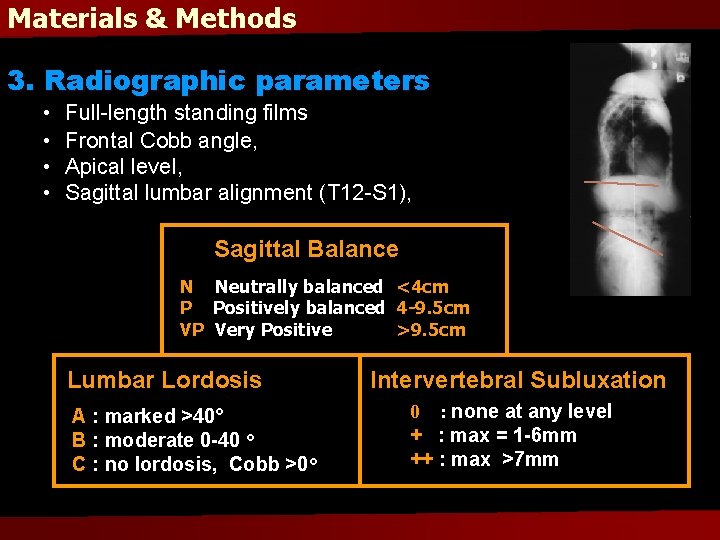
Materials & Methods 3. Radiographic parameters • • Full-length standing films Frontal Cobb angle, Apical level, Sagittal lumbar alignment (T 12 -S 1), Sagittal Balance N Neutrally balanced <4 cm P Positively balanced 4 -9. 5 cm VP Very Positive >9. 5 cm Lumbar Lordosis A : marked >40° B : moderate 0 -40 ° C : no lordosis, Cobb >0° Intervertebral Subluxation 0 : none at any level + : max = 1 -6 mm ++ : max >7 mm

Materials & Methods 4. Treatment approach • Surgical vs. non-surgical • If Surgical: • Anterior, Posterior, circumferential • Use of osteotomies • Extension of fusion to sacrum 5. Data Analysis • Treatment Analysis regarding • HRQOL measures • SRS-22, ODI, SF-12 • Correlation analysis • Classification types vs. treatment given
Results Patients Distribution 806 thoracolumbar/lumbar major deformities – Type IV – Type V – – – n=311 n=495 Mean age 53. 1 y. o. (+/- 15. 3) 700 Females (87%) 106 Males (13%)

Results n Surgical rates Rates of operative treatment – Lordosis modifier § B vs. A (51% vs. 37%, p<0. 05), trend for A vs. C (46%) – Subluxation modifier § ++ vs. 0 (52% vs. 36 %, p<0. 05), trend vs. + (42 %) – Sagittal Balance § N vs. VP: 39% vs. 59%, p<0. 05

Results Treatment Analysis: Type IV, V curves 92% highest level of fixation above apex of major curve. 97% lowest level of fixation below apex of major curve. 10% to level of sublux, 87% at least one level beyond Fusion to sacrum Apical Level Trend for type V patients more likely to have fixation to sacrum (p=. 074) Lordosis Modifier mod B patients more likely fusion to sacrum than mod A patients (p=. 041) Sagittal Balance Modifier increasing positive balance: more likely fixation extended to the sacrum. (mod N: 59%, mod P: 80%, mod VP: 88%) (all p<0. 05)
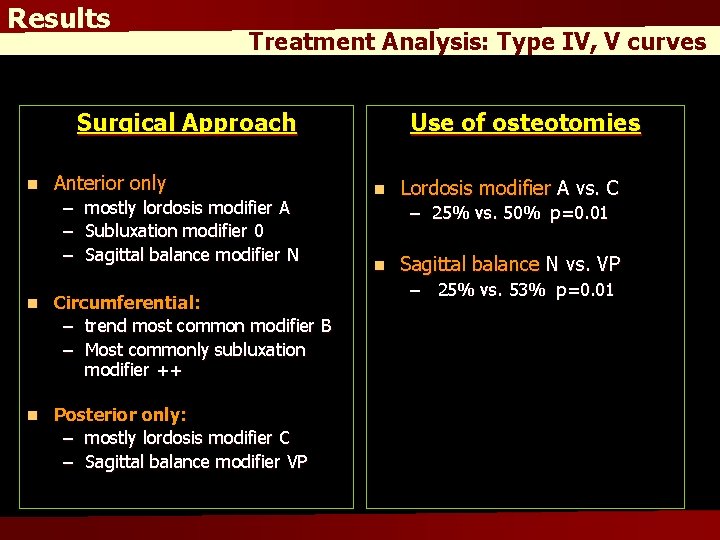
Results Treatment Analysis: Type IV, V curves Surgical Approach n Anterior only – mostly lordosis modifier A – Subluxation modifier 0 – Sagittal balance modifier N n Circumferential: – trend most common modifier B – Most commonly subluxation modifier ++ n Posterior only: – mostly lordosis modifier C – Sagittal balance modifier VP Use of osteotomies n Lordosis modifier A vs. C – 25% vs. 50% p=0. 01 n Sagittal balance N vs. VP – 25% vs. 53% p=0. 01

Results Main findings Treatment • Good lordosis (modifier A) less likely to have surgery • Most likely to require surgery: • loss of lordosis (C), • marked subluxation (++) • sagittal plane imbalance (VP) If surgery • Cross level of subluxation • Osteotomies to realign sagittal plane • lordosis modifier C gets most likely to require osteotomy • fusion to sacrum: with increasing sagittal imbalance, lost lordosis

Discussion - Conclusion n Adult scoliosis classification Clinical Impact established: – – – HRQOL Treatment…. non-op vs. surgical Surgical strategy…we’re getting there How about results of treatment ? Work toward surgical guidelines 2 yr f/u
Discussion - Conclusion Adult scoliosis classification Reliable Clinical impact • disability • surgical rate Surgical strategy ? Can we broaden to a: Comprehensive Adult Deformity Classification

Classification of Adult Deformity Type I II IV V Type K thoracic-only curve (no other curves) upper thoracic major, apex T 4 -8 lower thoracic major, apex T 9 -T 10 thoracolumbar major curve, apex T 11 -L 1 lumbar major curve, apex L 2 -L 4 no scoli (<100), principal sagittal plane deformity Lumbar Lordosis Modifier A B C marked lordosis >400 moderate lordosis 0 -400 no lordosis present Cobb >00 Subluxation Modifier 0 + ++ no intervertebral subluxation any level maximal measured subluxation 1 -6 mm maximal subluxation >7 mm Sagittal Balance Modifier N P VP normal, <4 cm positive SVA positive, 4 -9. 5 cm very positive, >9. 5 cm
Next Steps Adult scoliosis classification Refine Classification • Pelvic modifier • Co-morbidity index • Patient expectation scale Longitudinal follow up • who responds well to conservative care • who benefits (how much) from surgery • Complications ? Surgical analysis (2 yr f/u) • what strategies are most effective
- Slides: 18