Surgical Resection and Ablative Therapies for Hepatocellular Carcinoma
Surgical Resection and Ablative Therapies for Hepatocellular Carcinoma Kim M. Olthoff, MD Associate Professor of Surgery Liver Transplantation and Hepatobiliary Surgery University of Pennsylvania Philadelphia, Pennsylvania, USA Penn Cancer Center

University of Pennsylvania Medical Center Penn Transplant Center and Cancer Center First School of Medicine in United States First Teaching Hospital in the US 2 nd Nationally in NIH grand dollars

Hepatobiliary Tumor Conference Weekly multidisciplinary case presentations • Weekly discussion of all patients with possible hepatobiliary tumors Review history and imaging § Determine options for treatment § • Review of all pathology § Determine adjuvant therapy • Follow-up on cases • Potential clinical trials • Transplant and Hepatobiliary surgeons • Surgical oncology • GI surgeons • Oncologists • Radiologists • Interventional radiologists • Nuclear Medicine • Hepatologists

Background: Hepatocellular carcinoma (HCC) • One of the most common fatal tumors worldwide § 80 -90% of primary malignant tumors • Mostly associated with cirrhosis Rising incidence in US due to Hepatitis C § Seen after 20 - 30 years after HCV infection § • In the year 2000 - an estimated 8, 000 -10, 000 deaths in US from HCV • Mortality rate expected to double or triple by 2015 § Much of this mortality due to development of HCC • Younger population, increasing mortality • 2 -8% annual incidence of HCC in HCV cirrhosis • 5 year cumulative incidence 15 -20%

Background: Natural history of HCC in cirrhosis • Prognosis – not dependent only on tumor stage § If “Resectable” • may exceed 70% 5 yr § Untreated intermediate/advanced • 10 -50% 3 yr survival § Severity of disease determines outcome • Child’s A - 82% at 2 years • Child’s B/C - 36% at 2 yrs • Child’s C, large tumors • no survivors > 6 months

Tumor surveillance Defining high risk populations • Cohort studies § § § Male Advanced age HCV positivity/cirrhosis Functional impairment High AFP • Other parameters Proliferation rate § Irregular regeneration § Dysplasia § Viral genotype § • Columbo et al NEJM 1991 • Tsukuma et al NEJM 1993 • Liver Cancer Study Group Cancer 1994 • Bolondi et al Gut 2001 • Degos et al Gut 2000 • Chen et al Int J Cancer 2002 • Esnaola et al Ann Surg 2003

Tumor surveillance HCC and Alpha Feto-protein (AFP) • Prognosis of HCC with treatment § • Prognosis of HCC Rx with OLT § AFP <15 associated with better outcome • Iwatsuki 2000, • Shumihito 2001 • Fong 1999 § AFP > 400 associated with poorer outcome Pre-operative AFP not independently associated with survival § AFP > 1000 RR=2. 96, P=0. 04 • Yao, 2001 • CLIP Investigators, 2000 § AFP > 700 • Shetty, 2004
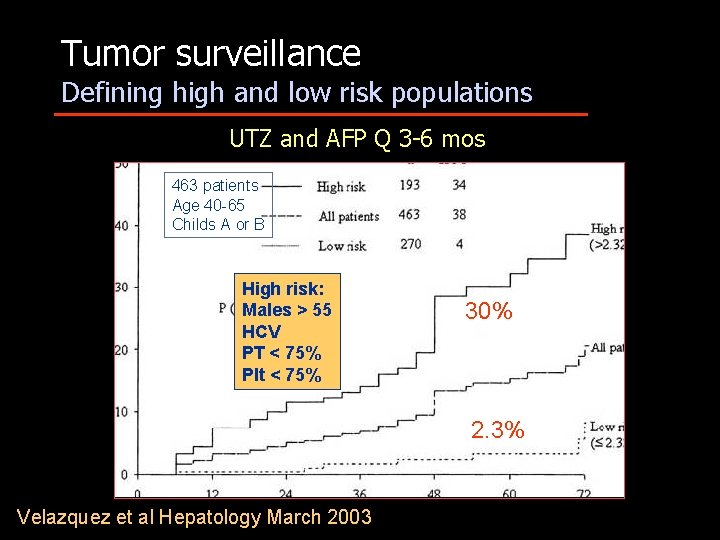
Tumor surveillance Defining high and low risk populations UTZ and AFP Q 3 -6 mos 463 patients Age 40 -65 Childs A or B High risk: Males > 55 HCV PT < 75% Plt < 75% 30% 2. 3% Velazquez et al Hepatology March 2003

Treatment of HCC “Curative” Treatment Options • Surgical resection is only proven curative treatment • Spectrum of therapy • Surgical Options: Resection § OLT § • Nonsurgical “Curative” Options: § Ablative therapies • Percutaneous Ethanol Infusion • Radiofrequency Ablation • Acetic acid Infusion • Which is best? § Surgery vs. ablation? • Caveats Only 30% of patients referred are surgical candidates § No good randomized controlled trials § Apples and oranges § Limitation of center expertise and treatment availability §
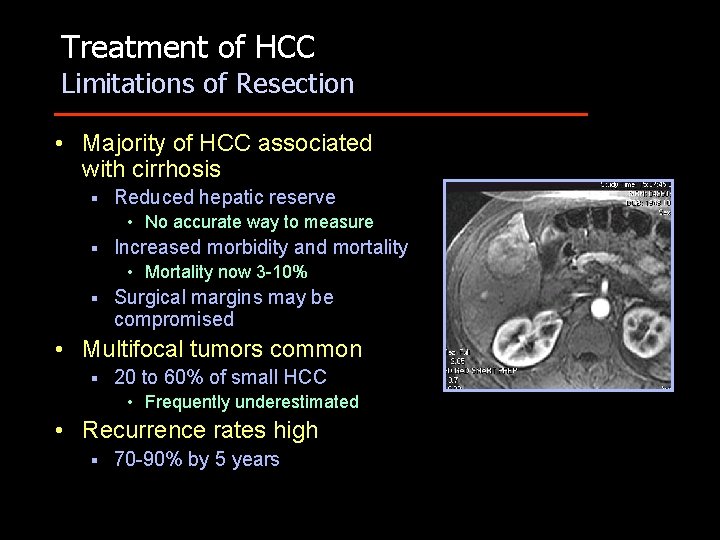
Treatment of HCC Limitations of Resection • Majority of HCC associated with cirrhosis § Reduced hepatic reserve • No accurate way to measure § Increased morbidity and mortality • Mortality now 3 -10% § Surgical margins may be compromised • Multifocal tumors common § 20 to 60% of small HCC • Frequently underestimated • Recurrence rates high § 70 -90% by 5 years

Surgical Resection of HCC Predictors of Recurrence • 164 patients resected for HCC (99 -2001) § 55% developed recurrence with median f/u of 26 months • Median time to recurrence - 24 mos § 5 yr survival 40%, 25% RF survival • Predictors of recurrence – Univariate § § § Tumor > 5 cm Multifocality Cirrhosis (40% of patient population) Vascular invasion Tumor satellites • Predictors of recurrence – Multivariate § Vascular invasion Cha et al JACS 2003 MSKCC
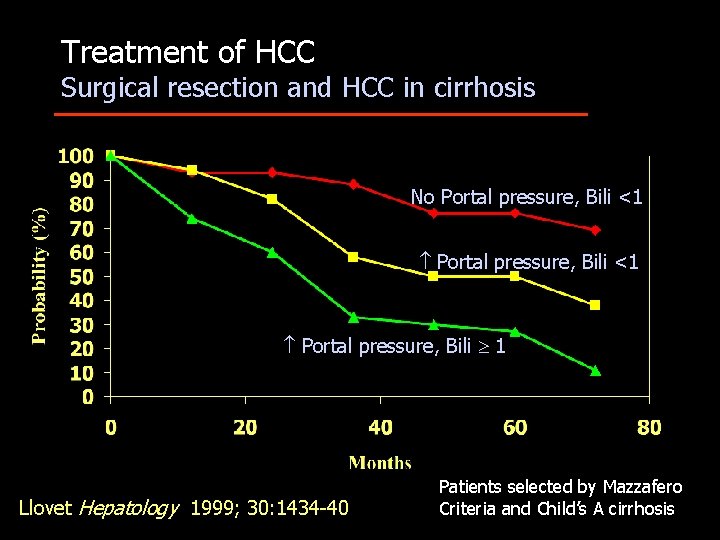
Treatment of HCC Surgical resection and HCC in cirrhosis No Portal pressure, Bili <1 Portal pressure, Bili 1 Llovet Hepatology 1999; 30: 1434 -40 Patients selected by Mazzafero Criteria and Child’s A cirrhosis

Surgical Resection of HCC Who are candidates? • Best candidates § § § § Well-compensated liver disease Asymptomatic Single lesion Normal bilirubin No evidence of portal hypertension No medical comorbidities Limited resection Minimize operative time
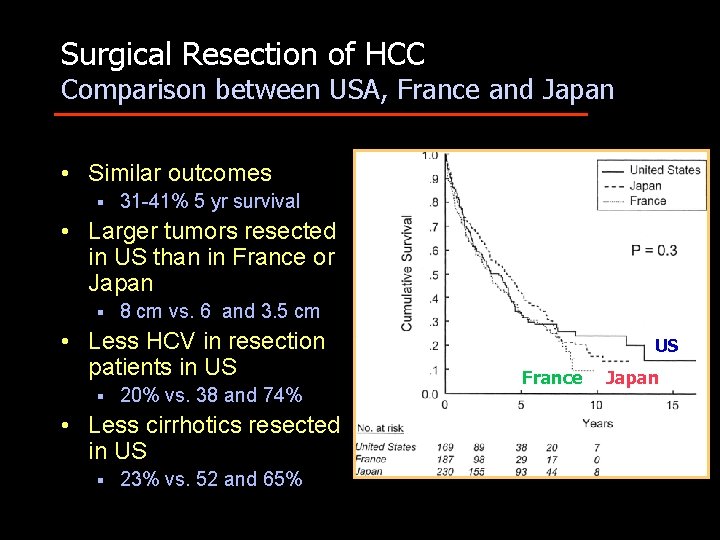
Surgical Resection of HCC Comparison between USA, France and Japan • Similar outcomes § 31 -41% 5 yr survival • Larger tumors resected in US than in France or Japan § 8 cm vs. 6 and 3. 5 cm • Less HCV in resection patients in US § 20% vs. 38 and 74% • Less cirrhotics resected in US § 23% vs. 52 and 65% US France Japan

Surgical Resection of HCC Operative Risks • Potential complications § § § § Estimated 25 -30% Bleeding from coagulopathy and portal hypertension Inadequate margins Liver failure Long LOS Hospital death Recurrent disease • Strategies to decrease risk § § § Liver anesthesiologist Minimize crystalloid Transfuse FFP/plts early Keep CVP low Minimize OR time Minimize blood loss • Pringle if necessary § Careful post-op management
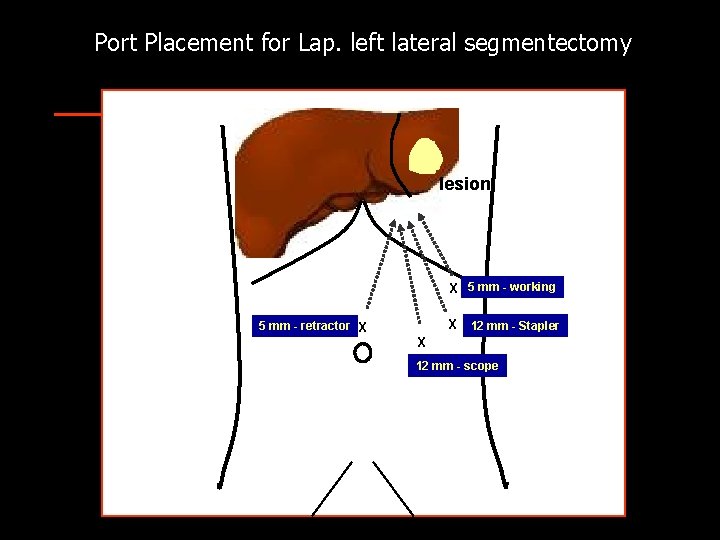
Port Placement for Lap. left lateral segmentectomy lesion X 5 mm - working 5 mm - retractor X X 12 mm - Stapler X 12 mm - scope
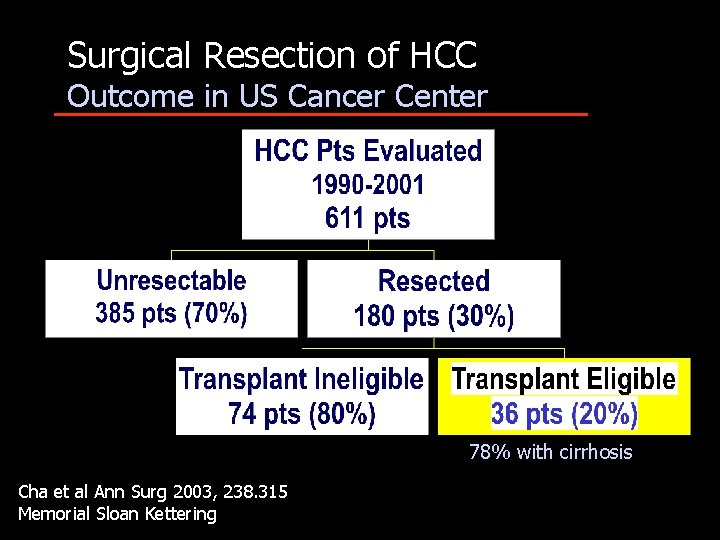
Surgical Resection of HCC Outcome in US Cancer Center 78% with cirrhosis Cha et al Ann Surg 2003, 238. 315 Memorial Sloan Kettering
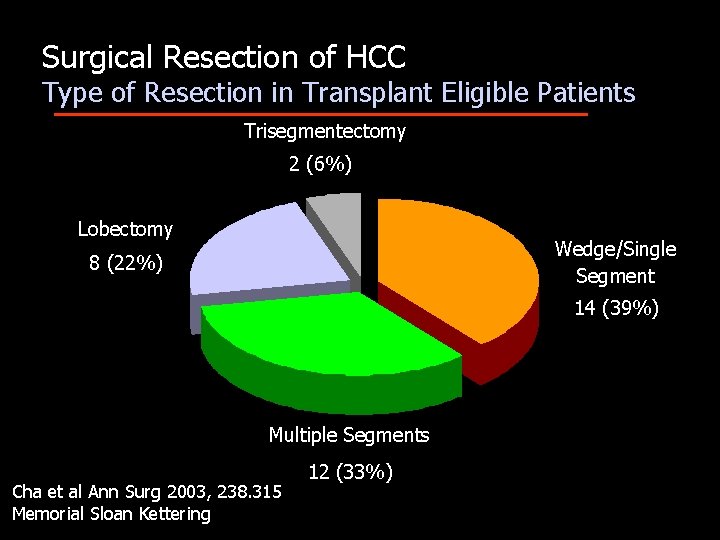
Surgical Resection of HCC Type of Resection in Transplant Eligible Patients Trisegmentectomy 2 (6%) Lobectomy Wedge/Single Segment 8 (22%) 14 (39%) Multiple Segments Cha et al Ann Surg 2003, 238. 315 Memorial Sloan Kettering 12 (33%)
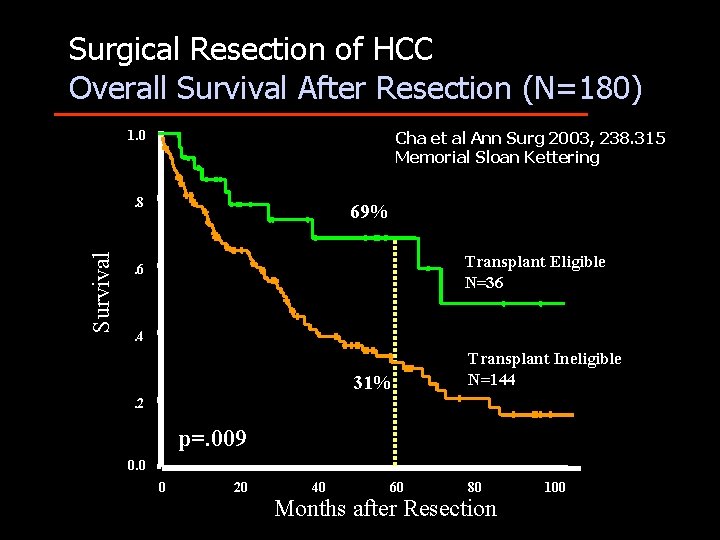
Surgical Resection of HCC Overall Survival After Resection (N=180) 1. 0 Cha et al Ann Surg 2003, 238. 315 Memorial Sloan Kettering Survival . 8 69% Transplant Eligible N=36 . 4 31% Transplant Ineligible N=144 . 2 p=. 009 0. 0 0 20 40 60 80 Months after Resection 100
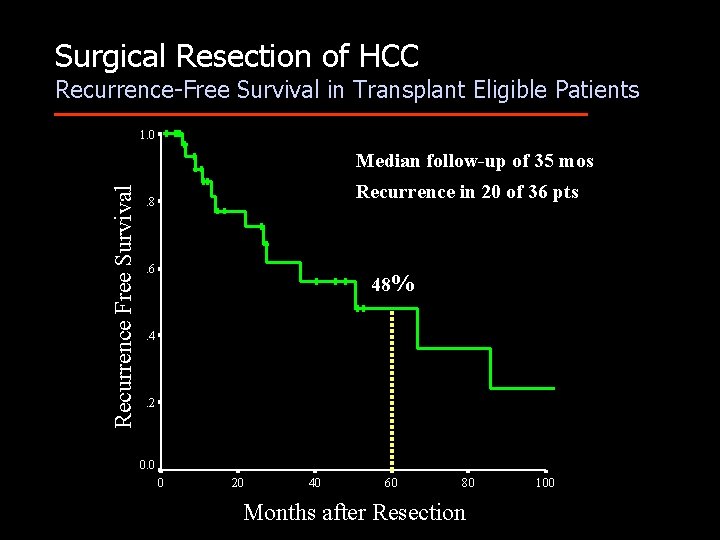
Surgical Resection of HCC Recurrence-Free Survival in Transplant Eligible Patients 1. 0 Recurrence Free Survival Median follow-up of 35 mos Recurrence in 20 of 36 pts . 8 . 6 48% . 4 . 2 0. 0 0 20 40 60 80 Months after Resection 100
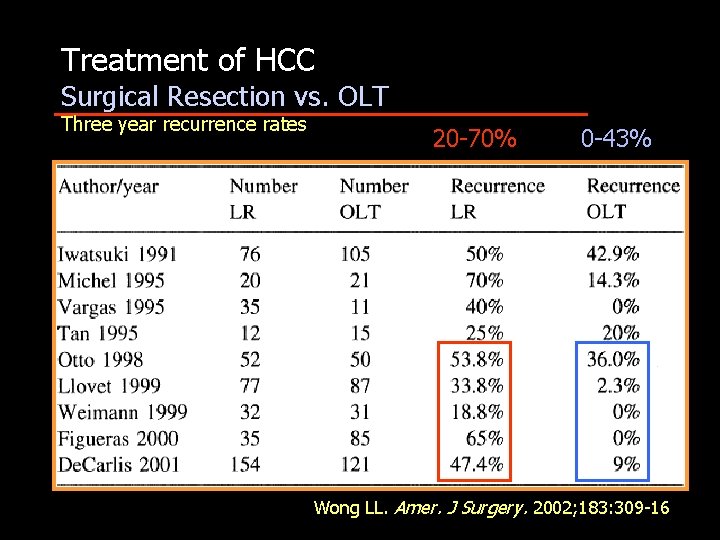
Treatment of HCC Surgical Resection vs. OLT Three year recurrence rates 20 -70% 0 -43% Wong LL. Amer. J Surgery. 2002; 183: 309 -16
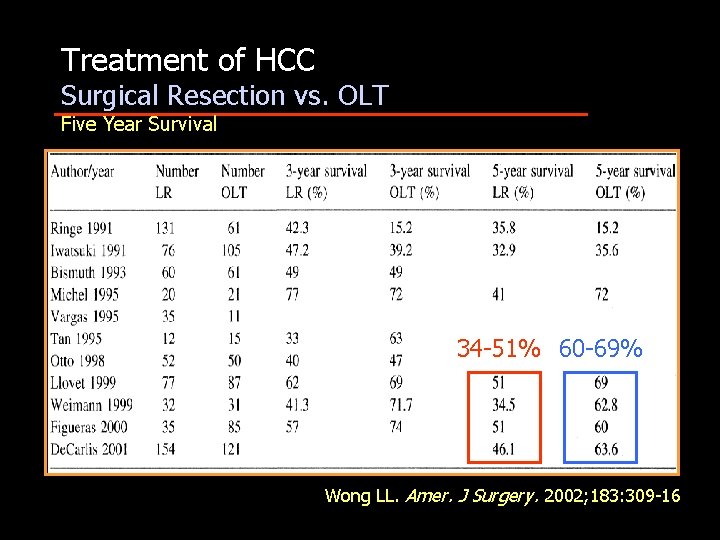
Treatment of HCC Surgical Resection vs. OLT Five Year Survival 34 -51% 60 -69% Wong LL. Amer. J Surgery. 2002; 183: 309 -16

Treatment of HCC Ablative therapies • Direct tissue ablation § Thermal • • § Radiofrequency Ablation (RFA) Cryoablation Microwave coagulation therapy (MCT) Laser Induced Thermotherapy (LITT) Chemical • Et. OH • Acetic acid • Chemoembolization • Radioembolization

Ablative Therapy of HCC Goals of Ablation • Equivalent to surgical resection in survival and local recurrence • Bridge therapy to stabilize disease while awaiting transplant • Palliation of unresectable, nontransplantable disease • Conversion from unresectable to resectable

Ablative Therapy of HCC Patient Selection for RFA • Unresectable lesions • Treatable under § Good • < 3 lesions • < 3 cm. § Extended • < 4 lesions • < 5 cm. § Heroic! • > 4 lesions • > 5 cm. US/CT/MR guidance: Can you see it? § Can you reach it? § • Adequate clotting function: Platelets >50 K § INR <1. 5 § • Adjacent structures § Bowel, gallbladder, diaphragm, vessels, bile ducts
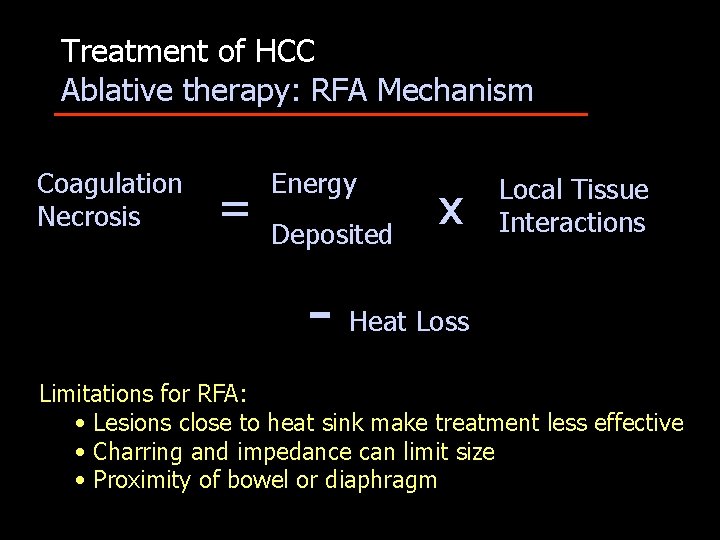
Treatment of HCC Ablative therapy: RFA Mechanism Coagulation Necrosis = Energy Deposited - x Local Tissue Interactions Heat Loss Limitations for RFA: • Lesions close to heat sink make treatment less effective • Charring and impedance can limit size • Proximity of bowel or diaphragm
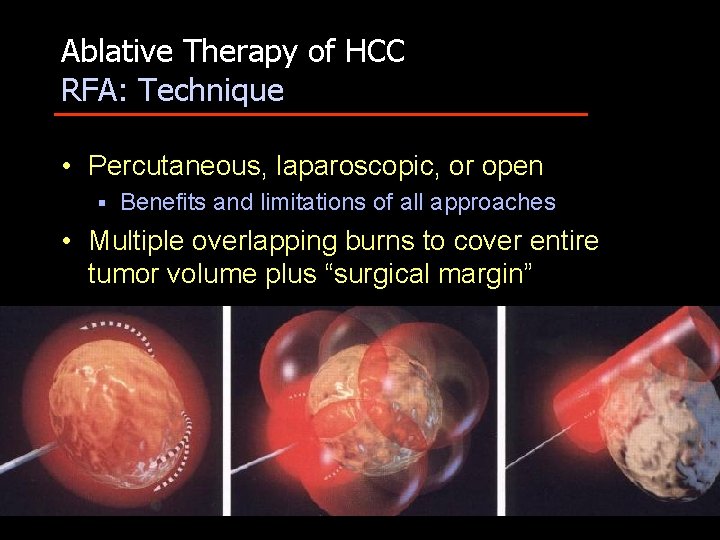
Ablative Therapy of HCC RFA: Technique • Percutaneous, laparoscopic, or open § Benefits and limitations of all approaches • Multiple overlapping burns to cover entire tumor volume plus “surgical margin”
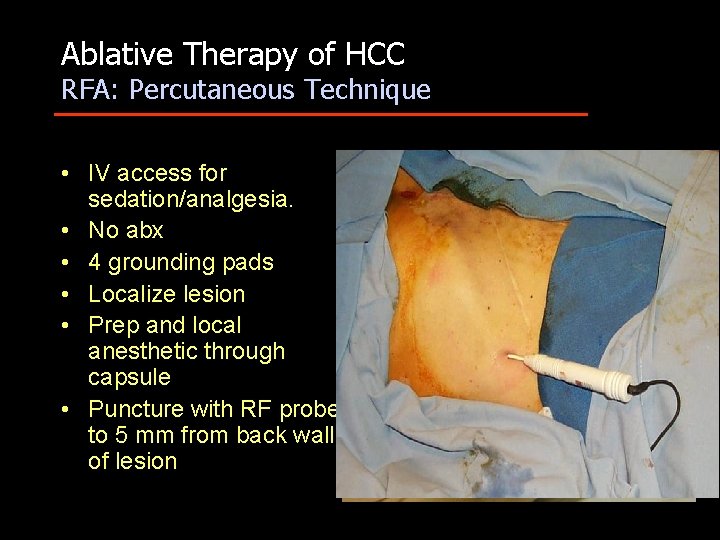
Ablative Therapy of HCC RFA: Percutaneous Technique • IV access for sedation/analgesia. • No abx • 4 grounding pads • Localize lesion • Prep and local anesthetic through capsule • Puncture with RF probe to 5 mm from back wall of lesion
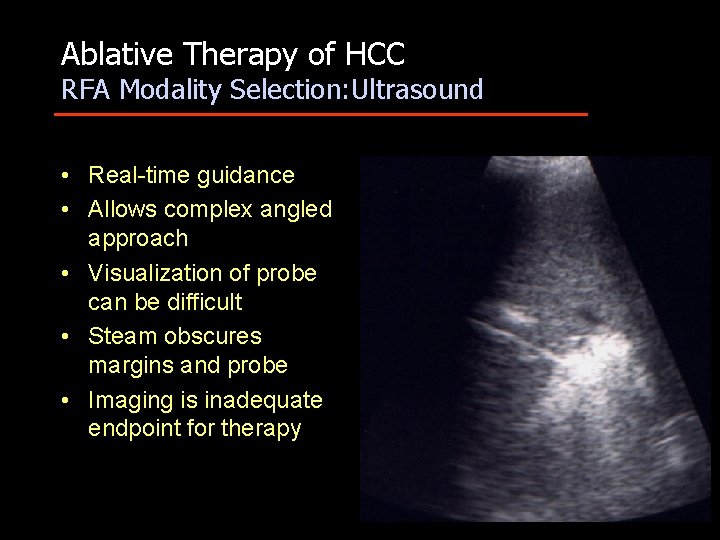
Ablative Therapy of HCC RFA Modality Selection: Ultrasound • Real-time guidance • Allows complex angled approach • Visualization of probe can be difficult • Steam obscures margins and probe • Imaging is inadequate endpoint for therapy
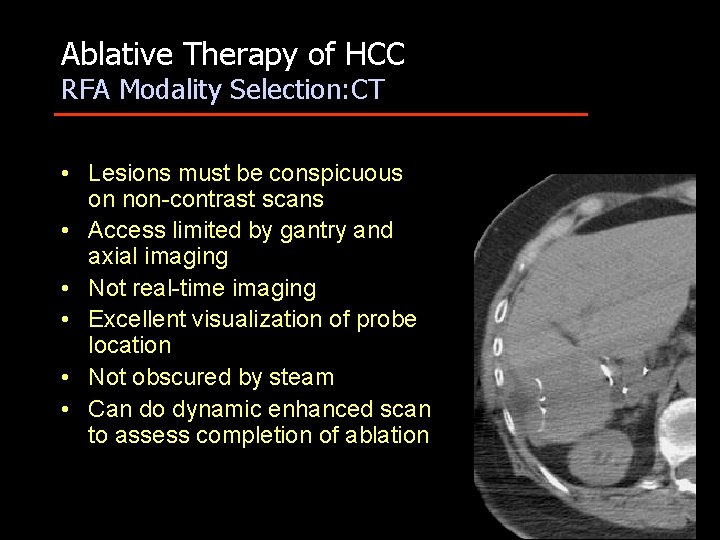
Ablative Therapy of HCC RFA Modality Selection: CT • Lesions must be conspicuous on non-contrast scans • Access limited by gantry and axial imaging • Not real-time imaging • Excellent visualization of probe location • Not obscured by steam • Can do dynamic enhanced scan to assess completion of ablation
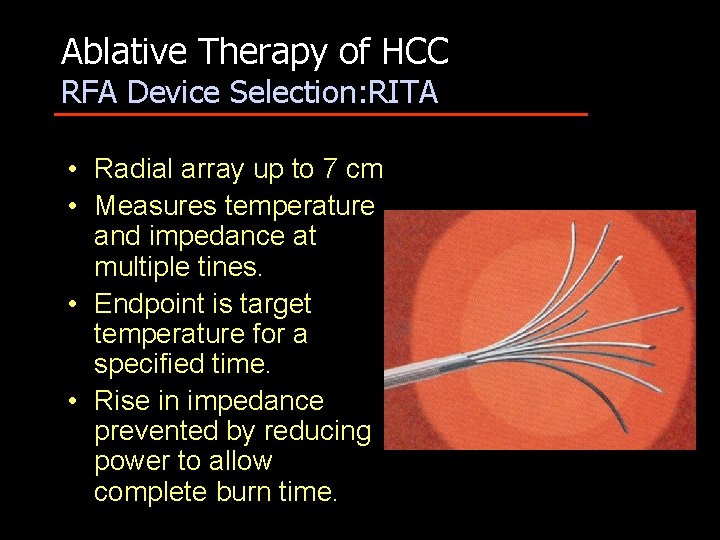
Ablative Therapy of HCC RFA Device Selection: RITA • Radial array up to 7 cm • Measures temperature and impedance at multiple tines. • Endpoint is target temperature for a specified time. • Rise in impedance prevented by reducing power to allow complete burn time.
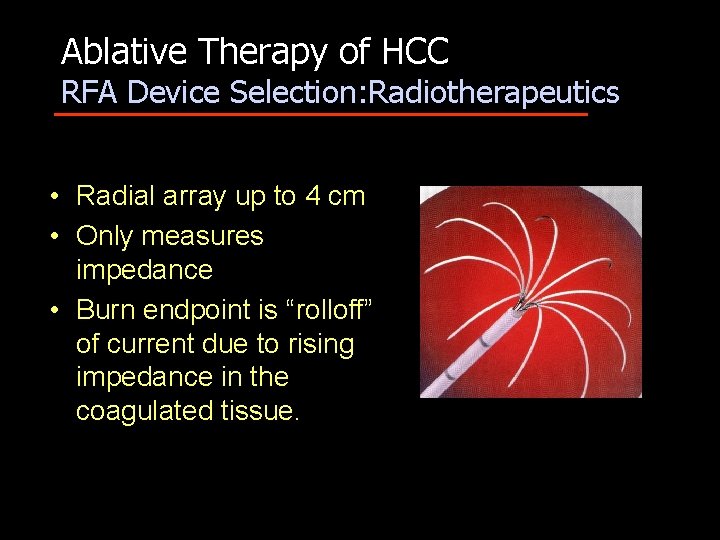
Ablative Therapy of HCC RFA Device Selection: Radiotherapeutics • Radial array up to 4 cm • Only measures impedance • Burn endpoint is “rolloff” of current due to rising impedance in the coagulated tissue.
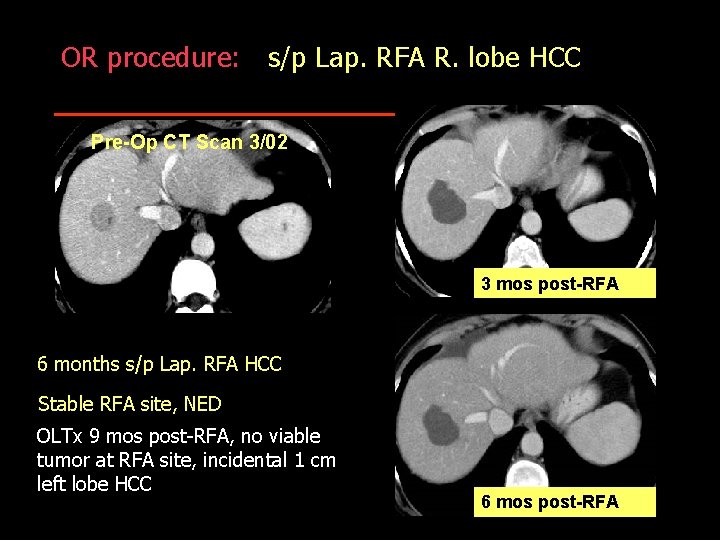
OR procedure: s/p Lap. RFA R. lobe HCC Pre-Op CT Scan 3/02 3 mos post-RFA scan 6 months s/p Lap. RFA HCC Stable RFA site, NED OLTx 9 mos post-RFA, no viable tumor at RFA site, incidental 1 cm left lobe HCC 6 mos post-RFA scan

Ablative Therapies of HCC Complications of RFA • • Pain Fever Vasovagal/Hypotension Oversedation Pleural Effusion (0. 6%) Pneumothorax Hemorrhage (0. 5%) • • • Ascites Cholangitis Abscess Hepatic Infarct Biliary Stricture Tract Tumor Seeding Skin burns
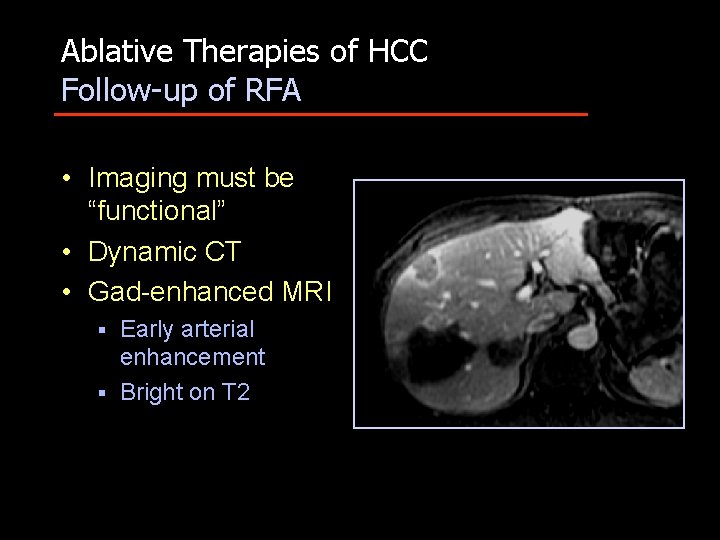
Ablative Therapies of HCC Follow-up of RFA • Imaging must be “functional” • Dynamic CT • Gad-enhanced MRI Early arterial enhancement § Bright on T 2 §

Ablative Therapies of HCC Follow-up of RFA: Results • “Complete” necrosis in 70 -75%. § HCC 80%-90% • Local recurrence in 13%-60%. • Disease-free survival 1 year 56% § 2 years 29% § 3 years 14% § • 65% new/distant lesions Dodd GD III; Solbiati L; RSNA 2000

Ablative Therapies of HCC Follow-up of RFA vs. PEI: HCC 5 cm • N # lesions § # sessions § • 1, 2 yr survival • Local failure • Complications PEI RF 50 52 73 5. 4 69 1. 1 77%, 43% 86%, 64% 26% 6% 0 0 Lencioni et al. Radiology 2003; 228: 235 -240

Treatment of HCC Explant pathology post RFA: Methods • Patients listed for OLT at Penn Retrospective study, between 1996 -2004 § 28 patients (40 HCC) had neoadjuvant image-guided therapy 1 -392 days prior to OLT § • Solitary lesions: (19 pts) 2. 2 -5. 0 cm • Multifocal HCC (9 pts) 1. 1 -6. 0 cm diameter • Exemption to UNOS criteria: 4 patients Soulen et al 2004

Treatment of HCC Explant pathology post RFA: Methods Pathology • Viable tumor was seen in 35/40 treated nodules, but only 1 patient is completely free of tumor • 11 of the treated HCC’s had either satellite nodules or microvascular invasion • 3 patients had macroscopic extrahepatic extension or portal vein tumor thrombus, from 2 treated HCC’s and from 1 new lesion

Treatment of HCC Explant pathology post RFA: Results • 35 of the 40 treated HCC had residual viable tumor (87. 5%) • 27/28 patients had viable tumor anywhere in the explanted liver at the moment of OLT (total of 55 nodules) • In 6/18 patients, imaging studies were false negative for treated and occult tumors • Recurrence-free post transplant survival is 85% with a follow-up of 1 -61 months (mean 15 mos)

Treatment of HCC Explant pathology post RFA: Conclusions • Although image-guided therapy is proven to be effective to provide local control of HCC, viable local or remote tumor is identified on explanted liver in the majority of patients • Contrast enhanced follow-up CT and MRI tend to underestimate the amount of viable tumor in the treated lesions and miss additional sites of disease.
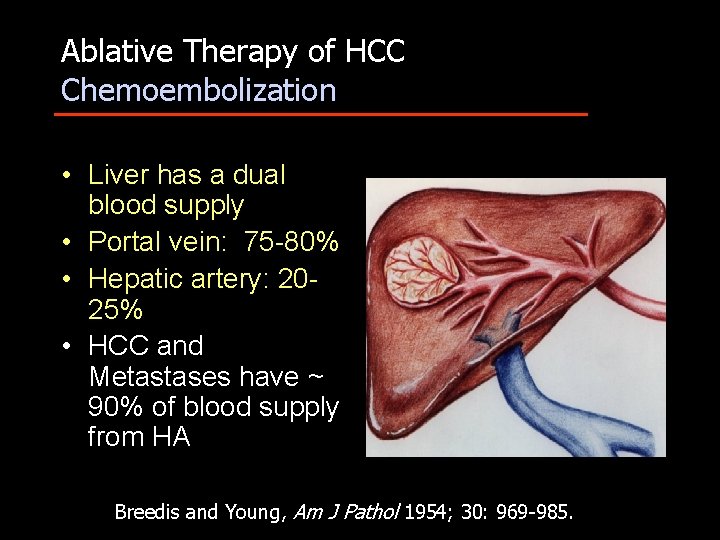
Ablative Therapy of HCC Chemoembolization • Liver has a dual blood supply • Portal vein: 75 -80% • Hepatic artery: 2025% • HCC and Metastases have ~ 90% of blood supply from HA Breedis and Young, Am J Pathol 1954; 30: 969 -985.

Ablative Therapy of HCC Chemoembolization • No standards: § § § Patient selection Number and type of embolics Number and type of drugs Volume of liver treated Frequency and end-point of treatment Measurement of response

Ablative Therapy of HCC Chemoembolization: Eligibity at Penn • Tissue diagnosis § unless AFP>400 • Unresectable disease • No contraindication to angiography • No contraindication to HA embolization • No active extrahepatic disease § hepatic failure risk § >50% tumor • No biliary obstruction § LDH>425 § AST>100 AND § bili>2

Chemoembolization CAM-Oil-Particle 100 mg Cisplatin in 50 mg Adriamycin 10 mg Mitomycin-C 8. 5 cc Contrast 1. 5 cc H 2 O emulsified with 0. 1 cc/kg Ethiodol plus 150 -250 µ PVA
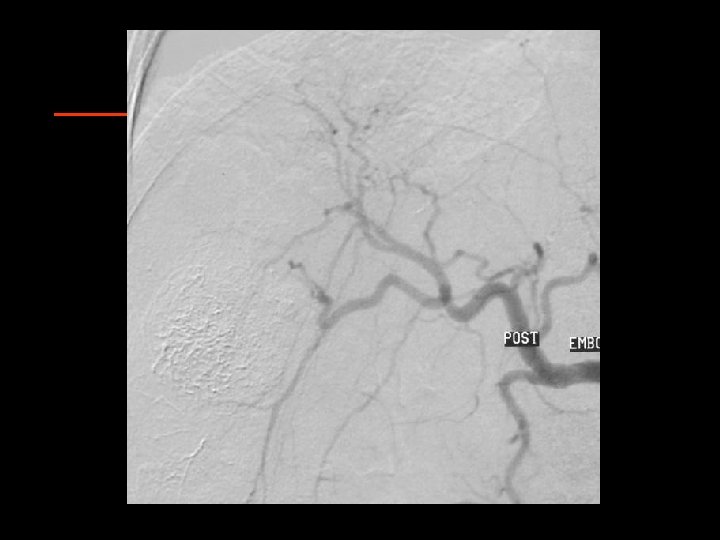
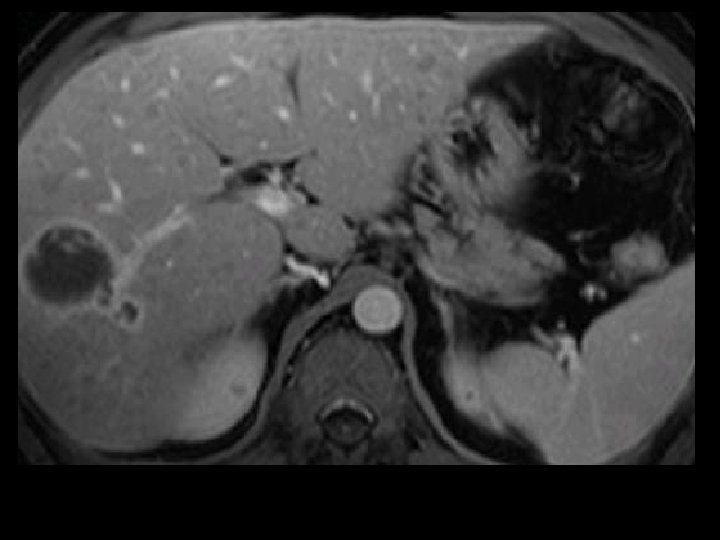

Ablative Therapy of HCC Chemoembolization RCTs: Barcelona Study • 112 Patients with HCC • Majority had Hepatitis C • Stratified by tumor burden and Okuda stage • Patients randomized to CE, bland embolization, or supportive care • CE had 2 year survival of 63% vs. 50% with bland embo and 27% with no therapy Llovet et al. Lancet 2002; 359: 1734 -39.

Ablative Therapy of HCC Chemoembolization RCTs: Hong Kong Study • 80 Patients with HCC • 80% HBSAg positive • Equal proportions of Okuda I/II • Randomized to CE or supportive care • CE performed with cisplatin/lipiodol/Gelfoam sponge • 2 year survival 31% vs. 11% Lo, Hepatology 2002; 35: 1164 -71.
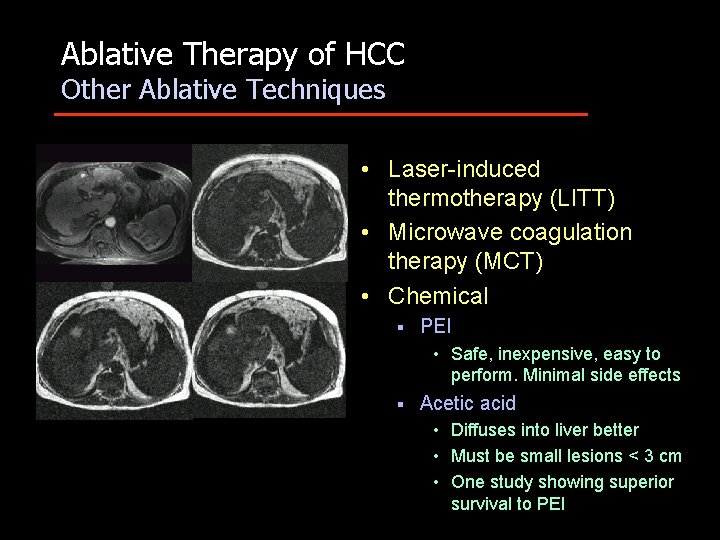
Ablative Therapy of HCC Other Ablative Techniques • Laser-induced thermotherapy (LITT) • Microwave coagulation therapy (MCT) • Chemical § PEI • Safe, inexpensive, easy to perform. Minimal side effects § Acetic acid • Diffuses into liver better • Must be small lesions < 3 cm • One study showing superior survival to PEI
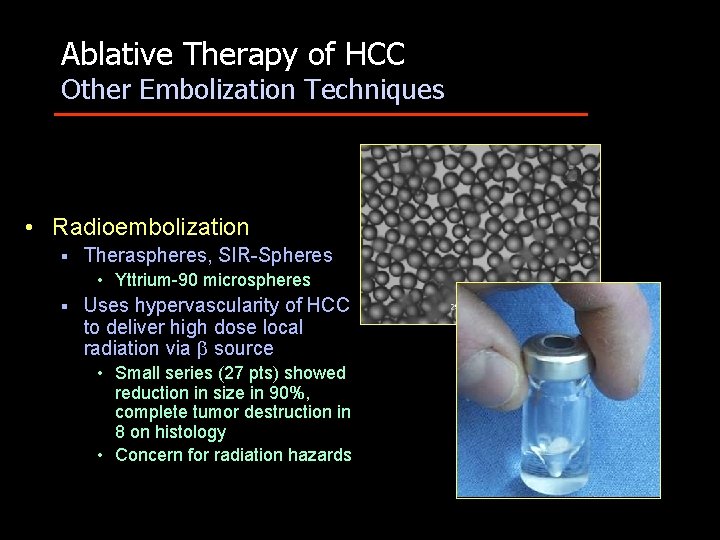
Ablative Therapy of HCC Other Embolization Techniques • Radioembolization § Theraspheres, SIR-Spheres • Yttrium-90 microspheres § Uses hypervascularity of HCC to deliver high dose local radiation via source • Small series (27 pts) showed reduction in size in 90%, complete tumor destruction in 8 on histology • Concern for radiation hazards

Treatment of HCC Surgery vs. Percutaneous local ablation therapy • Comparison of surgery vs. PLAT • Surgical resection (5 studies) § Recurrence free survival • 3 yr 38 -64% 5 yr 23 -58% • PLAT (7 studies – 4 PEI, 3 RFA) Recurrence free survival • 2 yr 41 -64% 4 yr 18 -39% § RFA superior to PEI § Lau et al, Annals of Surgery 2003
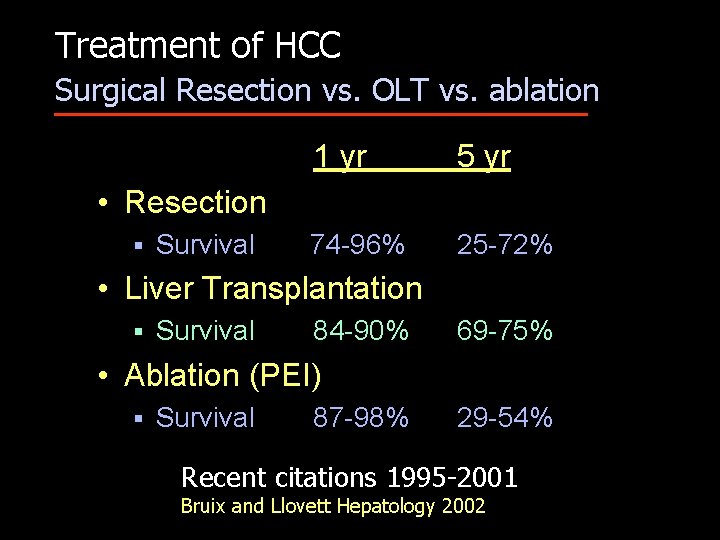
Treatment of HCC Surgical Resection vs. OLT vs. ablation 1 yr 5 yr 74 -96% 25 -72% • Resection § Survival • Liver Transplantation § Survival 84 -90% 69 -75% • Ablation (PEI) § Survival 87 -98% 29 -54% Recent citations 1995 -2001 Bruix and Llovett Hepatology 2002

Treatment of HCC Surgery vs. Percutaneous Ethanol Injection • Compared resection vs. PEI for small single nodule HCC 197 eligible, 82 matched § Matched for age, CTP, date of diagnosis § • 1 and 3 yr survival PEI 91% 65% § Resection 82% 63% § Concluded no significant difference § • Higher cost and morbidity with resection • Randomized trial needed Daniele et al, CLIP, J Clinical Gastro 2003

Ablative Therapy for HCC Conclusions • Thermal ablation, chemoembolization, radioembolization part of multimodality approach to HCC • Paucity of randomized trials • Unstable and evolving technology • Combination of therapies likely to be of most benefit • Multidisciplinary approach essential
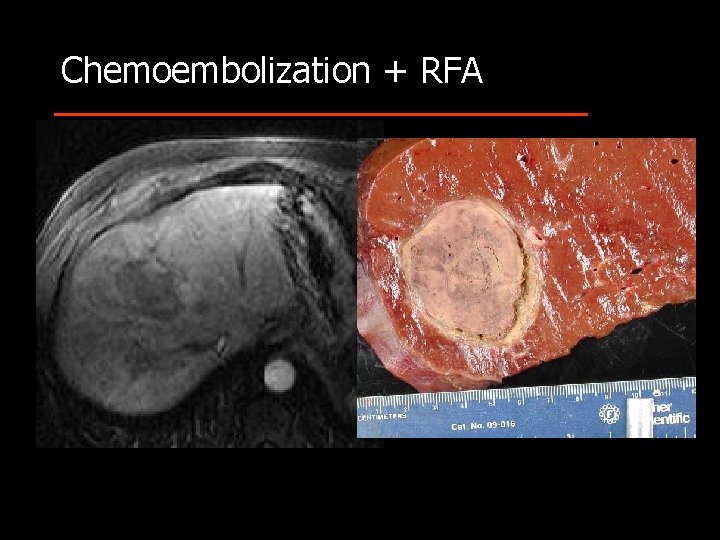
Chemoembolization + RFA

Therapy of HCC Combined Modalities • • • TACE and surgery TACE and PEI, RFA and surgery Portal vein embolization and surgery Laparoscopic techniques § § § Diagnosis Determine resectability Biopsy RFA Resection
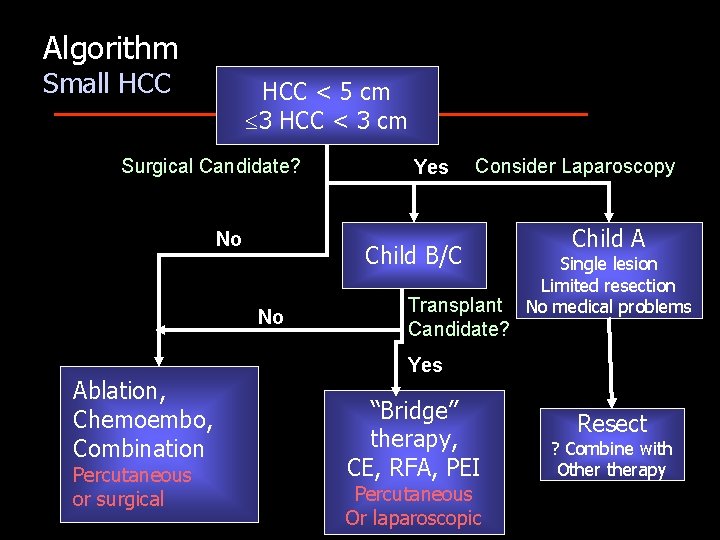
Algorithm Small HCC < 5 cm 3 HCC < 3 cm Surgical Candidate? No Percutaneous or surgical Consider Laparoscopy Child B/C No Ablation, Chemoembo, Combination Yes Transplant Candidate? Child A Single lesion Limited resection No medical problems Yes “Bridge” therapy, CE, RFA, PEI Percutaneous Or laparoscopic Resect ? Combine with Otherapy
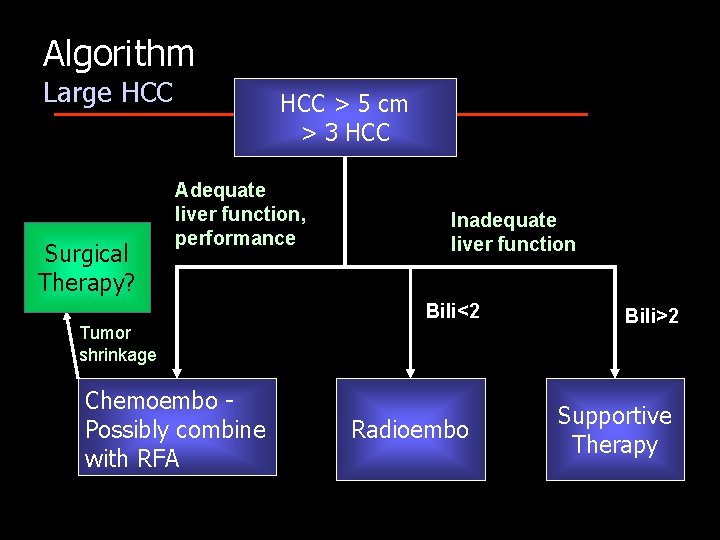
Algorithm Large HCC Surgical Therapy? HCC > 5 cm > 3 HCC Adequate liver function, performance Inadequate liver function Bili<2 Tumor shrinkage Chemoembo Possibly combine with RFA Radioembo Bili>2 Supportive Therapy

Treatment options for HCC Basic principles • Assess tumor burden § Up to date imaging • Vascular invasion • Focality • AFP • Assess liver function Cirrhosis § Portal hypertension § Child’s score § • Assess patient status Surgical candidate? § Transplant candidate? § Chemotherapy candidate? § • Develop multidisciplinary approach
- Slides: 62