Surgical Patient Positioning Prepared by Cecile Cherry RN

Surgical Patient Positioning Prepared by Cecile Cherry, RN, MSN, CNOR CVOR UAB Hospital

Objectives Discuss the factors that determine the surgical position Describe the mechanism of common positioning injuries Discuss surgical team considerations in patient positioning, including employee safety Describe the basic surgical positions, equipment required for each position, and cite specific safety considerations for each position 1. 2. 3. 4. 5. 6. Supine Prone Fowler’s Lateral decubitus Kraske/jackknife Lithotomy

Considerations in Positioning Surgical position is determined by: n 1. ) the surgical procedure to be performed and n 2. ) the individual surgeon’s preference. The patient’s physical condition is also a considerationsome patients may have special positioning needs due to physical limitations: contractures, injuries, etc Patients with respiratory distress may require special accommodations in positioning especially prior to anesthesia induction

The Surgical Team & Patient Positioning the surgical patient requires a coordinated, team approach involving anesthesia, the surgeon or his/her designee, and the OR staff Patient safety is the primary consideration when positioning a patient

Anesthesia Considerations Patient who will be receiving general anesthesia patient will be anesthetized in the supine position regardless of what the surgical position is to be. Patient is positioned following induction of general anesthesia after the ETT is secured ALWAYS coordinate moving an anesthetized patient with the anesthesia provider!

OR Team Safety Employee safety is also an important consideration in patient positioning! Do not lift or transfer patients without an adequate number of people Remember to use correct body mechanics Use assistive devices, such as rollers, whenever possible

Why is patient positioning such an important issue? Positioning injuries (either pressure injuries or nerve damage) causes increased patient pain, increased length of hospitalization stays and increased costs Patient positioning-related injuries can be either temporary or permanent Exact incidence of post-surgical pressure injuries not available – estimates range from 12% - 45% of surgical patients

Types of Pressure Injuries Pressure sores – caused by unrelieved pressure n n Shearing and prolonged and duration of pressure are major contributing factors Most often occurs over bony prominences Nerve injuries – caused by compression or prolonged stretching n Can vary greatly in severity, cause numbness and/or motor weakness and can be temporary or permanent

Causes of Positioning Injuries Pressure n Compresses skin, bone, muscle and capillary perfusion. Affects tissue perfusion & may cause ischemia of affected tissue Friction n Occurs when the patient’s skin rubs against rough stationary surfaces Shearing n Occurs when the patient’s subcutaneous tissue moves while the skin remains stationary – ex: can occur if the patient is “dragged” when repositioned instead of using a drawsheet

What are the signs of positioning injuries? The appearance of surgery –related pressure sores is variable: n n Patient may have reddened skin at a pressure point immediately after surgery or may not show signs of a pressure ulcer for several days after the procedure Unlike typical pressure ulcers, pressure sores after surgery often start forming in the muscle tissue and progresses outward toward the skin

Does reddened skin = pressure sore? No – the appearance of reddened skin may indicate reactive hyperemia Reactive hyperemia = temporarily reddened skin as blood flow is restored to a body part that has experienced sustained pressure Reactive hyperemia resolves without treatment Can be distinguished from a pressure injury by applying brief pressure with your fingertip – if reactive hyperemia the reddened area will blanch when pressure is applied

Other Positioning Considerations The patient’s: n n Age Skin condition Nutritional status Preexisting conditions such as peripheral neuropathy, chronic diseases, etc.

When Positioning Patients: Maintain neutral body alignment whenever possible. Pad all pressure points. Avoid pressure on/or stretching of peripheral nerves; avoid hyperextension of neck When changing positions (ex: turning patient from supine to prone) maintain proper body alignment

Patients Factors Indicating an Increased Risk for Positioning-Related Injuries Procedures>3 hours Geriatric patients Pediatric patients Malnourished patients Obese patients Diabetic patients Patients with certain bone & joint conditions: osteoporosis, rheumatoid arthritis Patients with peripheral vascular disease Patients with paralysis

Potential Complications Of Surgical Positioning Injury to peripheral nerves-pressure on, or stretching of nerves can cause either temporary or permanent nerve damage, resulting in numbness or motor weakness Nerves especially vulnerable to positioning injuries: Brachial Plexus: avoid excess stretching of neck, abduction of arms greater than 90° Radial & ulnar nerves: avoid pressure or compression, provide adequate padding

Other Positioning-Associated Complications Respiratory compromise-some positions restrict check expansion Circulatory Compromise – some positions (ex: lithotomy) may promote thrombus formation: some positions (ex: sitting) promote venous pooling Air embolism – risk increased for patients in the sitting (or Fowler’s) position

Padding pressure points: One study found that gel pads and gel OR bed overlays are more effective at reducing pressure than foam padding (Armstrong, Bortz & Halter, 2001)

Positioning Safety When transferring patient the stretcher and the OR bed should always be in the LOCKED position!

Positioning Safety Patient with a diagnosed or suspected C -spine injury—the surgeon should be present to direct positioning Patient with an un-splinted fracture-the surgeon will assume responsibility for protection of/positioning the affected limb

Positioning Safety Avoid allowing tubing to pneumatic hoses to lie on top of the patient – this may create a pressure area Scrubbed team members should avoid leaning on the patient

Nursing Care Planning for Patient Positioning Patient assessment Planning Implementation Evaluation Documentation

Patient Assessment Is patient physically able to transfer from stretcher to bed? Does the patient have any health conditions or previous surgery that may indicate special positioning needs (ex: patient with history of shoulder repair, patient with previous total hip arthroplasty) Assess patient for any pre-existing skin condition (broken skin, abrasions, bruises, frail elder with fragile skin, etc)

Planning Where can I find information needed to plan for positioning? n n n the surgery schedule the surgeon’s preference card consultation with surgeon/resident/SA/RNFA, Team Leader or experienced colleagues Obtain all devices/supplies needed for patient positioning: foam padding, gel pads, OR bed attachments, special OR beds (ex: fracture table), etc.

Evaluation Assess patient’s post-operative skin condition, noting and documenting any changes from pre-operative skin condition

Document: Patient position Pre-operative skin condition Pertinent medical history Safety measures taken- placement of padding, correct body alignment maintained, any special positioning measures taken Post-operative skin condition

What are the most common surgical positions? Supine n Modifications: w Trendelenburg w Reverse Trendelenburg Lateral Prone Lithotomy Sitting (Fowler’s) n Modifications w Beach chair or Barber chair Kraske (Jackknife)
Supine Position Examples of procedures performed with patient in the supine position: n n Abdominal surgery Most head and neck procedures Most cardiac/vascular procedures Many procedures on the extremities

Supine Positioning devices needed: Safety Strap Armboards x 2 Foam/gel padding

Supine Positioning Maintain normal body alignment if at all possible Pad pressure points: elbows, heels Arms- if on armboards do not extend more than 90° If arms are to be tucked at sides place the palmar surface of hands against body to reduce strain on nerves

Supine Position If patient having procedure with local or IV regional anesthesia, you may place a pillow under the patient’s distal thighs for comfort (reduces lower back strain)avoid pressure on popliteal area Be sure patient’s legs are not crossed, as this creates a pressure point
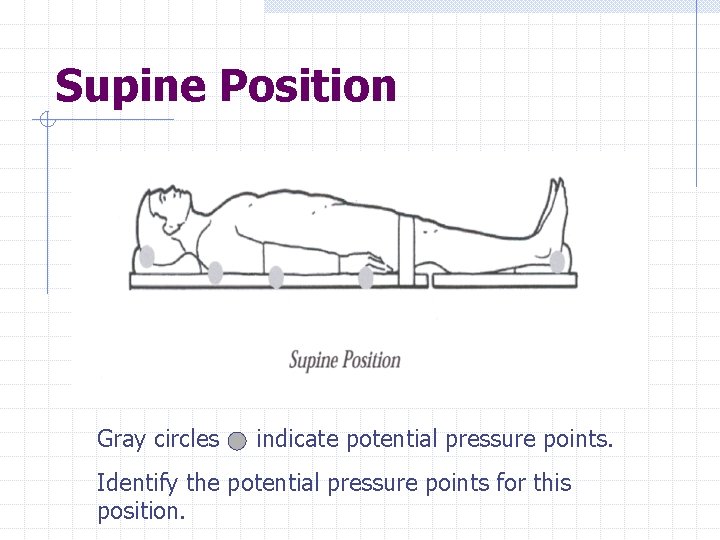
Supine Position Gray circles indicate potential pressure points. Identify the potential pressure points for this position.
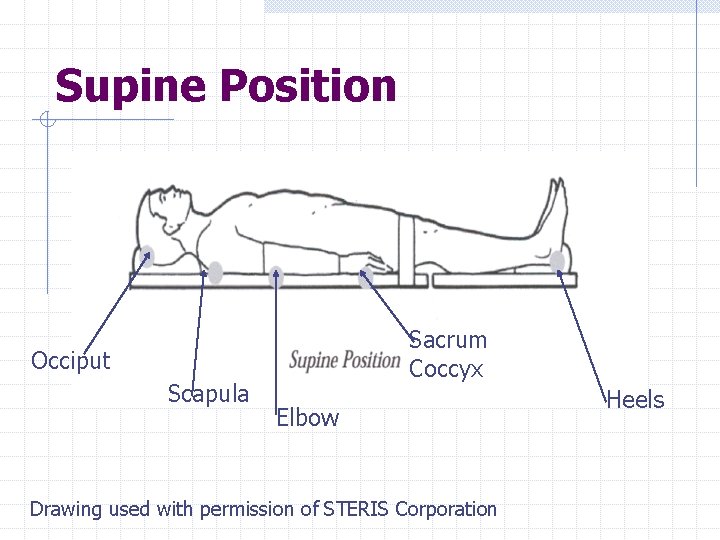
Supine Position Sacrum Coccyx Occiput Scapula Elbow Drawing used with permission of STERIS Corporation Heels

Modified Supine Position Trendelenburg: allows abdominal contents to gravitate upward, providing improved exposure for procedures involving pelvic organs Reverse Trendelenburg: displaces abdominal contents downward; improves visualization in surgery involving upper abdominal organs

Lateral Position Procedures performed in the lateral position Most Hip procedures Some Shoulder procedures Thoracic procedures

Lateral Decubitus Positioning devices needed: Vac-Pac (“Bean Bag”) or Peg Board (depending on surgeon’s preference and procedure being performed) Safety Strap Axillary roll Armboard Foam padding Pillows

Lateral Positioning Considerations: Axillary roll: aids in chest expansion, and prevents compression of peripheral nerves in the axilla. Arms: lower arm will be on padded armboard, upper arm must be supported on pillow, blankets or Mayo stand.

Lateral Positioning Padding between legs and feet, and between bed and bottom knee and ankle, under down-side ear prevents pressure sores. Exception: padding between legs may not be necessary for Orthopedic hip procedures In addition to the safety strap, 3” silk or adhesive tape can be used to stabilize the patient-do not secure so tightly that tape creates a pressure point.
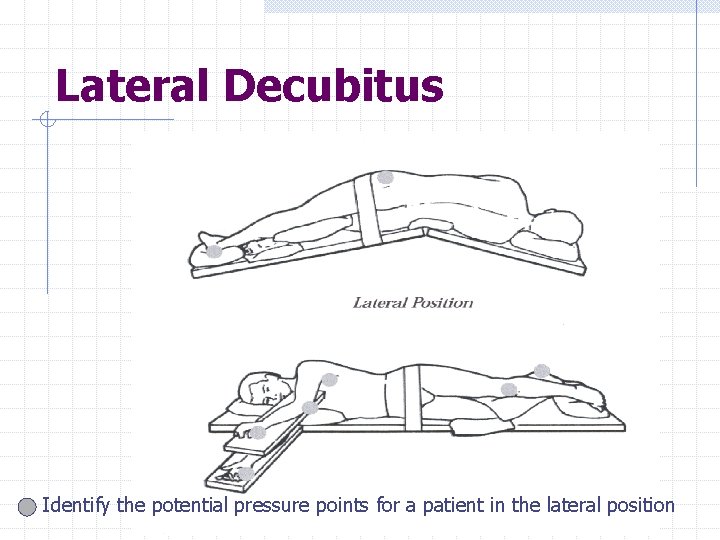
Lateral Decubitus Identify the potential pressure points for a patient in the lateral position
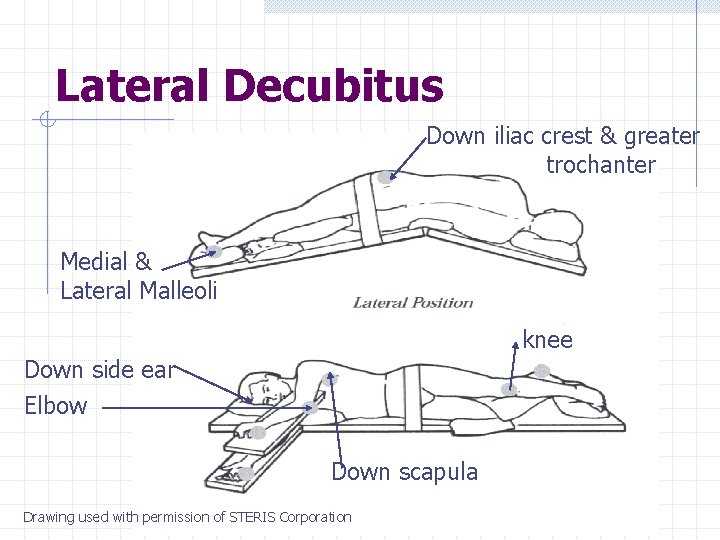
Lateral Decubitus Down iliac crest & greater trochanter Medial & Lateral Malleoli knee Down side ear Elbow Down scapula Drawing used with permission of STERIS Corporation
Prone Position Most spine procedures Some orthopedic procedures (ex: repair of torn Achilles tendon)

Prone Positioning The patient is anesthetized on the stretcher in the supine position. Minimum of 4 people are required to turn patient: one controlling the head, one on each side, and one at the feet Move the patient as a unit- do not hyperextend neck Pad all pressure points: elbows, knees, toes

Prone Positioning Devices Important to allow for normal expansion of the chest when the patient is prone: Chest Rolls, Wilson Frame, Andrew’s Frame, Jackson Table (device required will depend on surgeon’s preference and the scheduled procedure) n n Armboards x 2 Pillows Foam Padding Safety Strap

Prone Positioning Patient at risk for corneal abrasion- anesthesia will usually put ointment in patient’s eye, and tape them shut. Face will be padded by anesthesia provider Male patients: avoid compression of genitals- should hang free. Female patients: breasts should be evenly compressed. Take extra care when positioning a patient with breast implants to avoid damaging the implants.
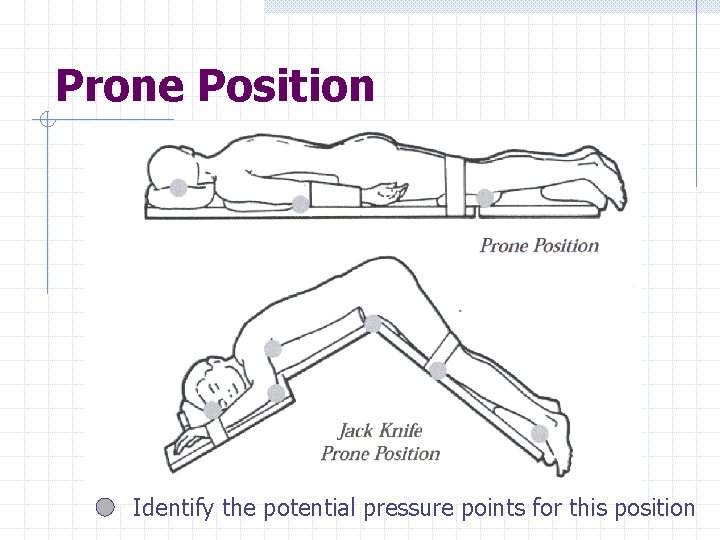
Prone Position Identify the potential pressure points for this position
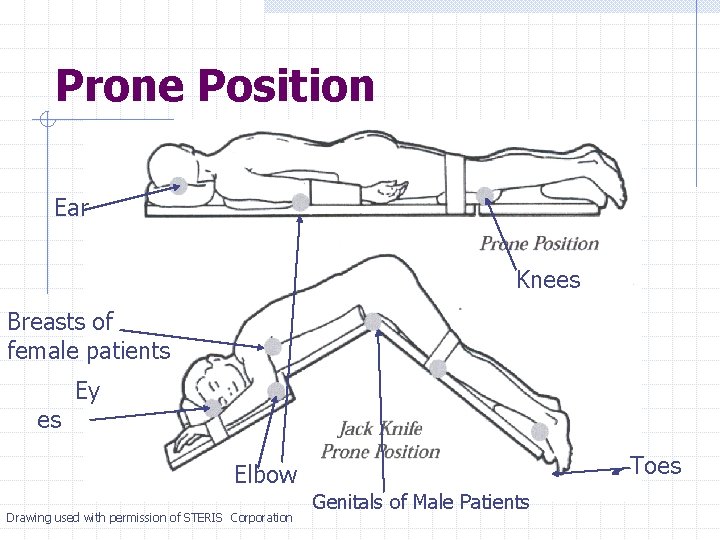
Prone Position Ear Knees Breasts of female patients es Ey Toes Elbow Drawing used with permission of STERIS Corporation Genitals of Male Patients

Safety Consideration for Prone Patients There must be a readily available stretcher for all patients positioned in the prone position—this makes it possible to turn the patient supine quickly in an emergency situation (ex: the patient “codes”, or the patient must be evacuated due to a fire in the area)

Jackknife Rectal procedures (ex: hemorroidectomy)

Lithotomy Position Many Gynecological Procedures: D&C, Vaginal Hysterectomy, GYN Laparoscopy procedures Many Urological procedures: Cystoscopy, perineal prostatectomy, transurethral resection of the prostate Some general surgery procedures: anteriorposterior colon resection

Lithotomy Positioning devices needed: Stirrups – Allen or J-stirrups (Candy Cane) depending on surgeon’s preference Foam padding Armboards x 2

Lithotomy Position Patient usually anesthetized in the supine position Both legs should be raised and lowered into the stirrups simultaneously-this prevents joint and nerve damage, and minimizes hemodynamic changes from positioning Take care not to over-abduct or over-flex the patient’s joints

Lithotomy Position Patient’s legs should be padded to prevent pressure from stirrups, and to avoid metal of stirrups from touching patient Take care that patient’s fingers are not caught in bed when the foot of the bed is lowered Venous thrombosis is a possible complication of the lithotomy position—it is very important to avoid pressure on legs from stirrups, especially in the popliteal area.
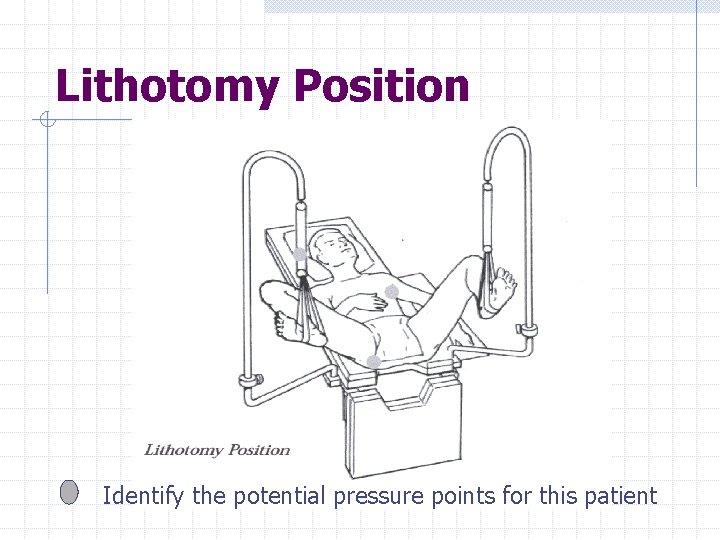
Lithotomy Position Identify the potential pressure points for this patient
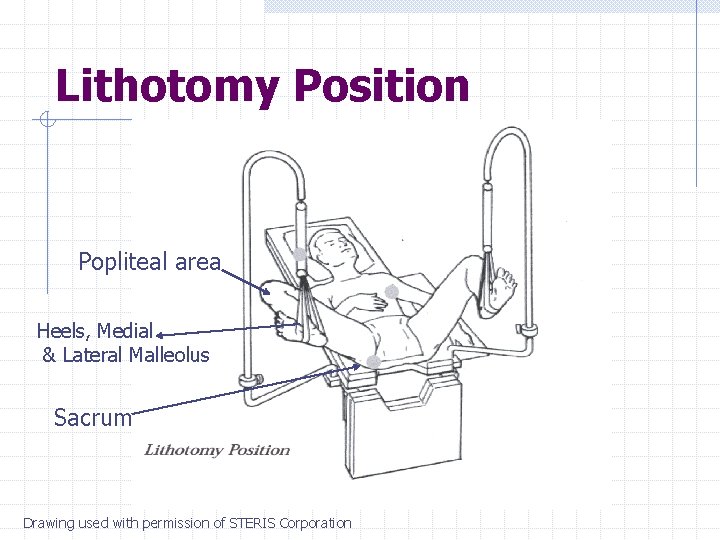
Lithotomy Position Popliteal area Heels, Medial & Lateral Malleolus Sacrum Drawing used with permission of STERIS Corporation

Sitting Position (Fowler’s) Some: n n Shoulder procedures Neurosurgical procedures

Fowler’s Positioning devices needed: Safety Strap Foam padding Pillows Other devices depend on procedure and surgeon’s preference—may need Mayfield headrest, foot board

Sitting Position: Special Concerns Sitting position= negative venous pressure in the head and neck, creating potential for air embolus Anesthesia will use special precautions such as monitoring patient’s heart with a doppler so that an embolus can be audibly detected and placing a central line to allow for withdrawal of air from heart in the event that an embolus occurs

Fowler’s: Positioning Considerations Footboard can be used to prevent foot drop. The patient’s head must be maintained in a stable position until positioning is complete
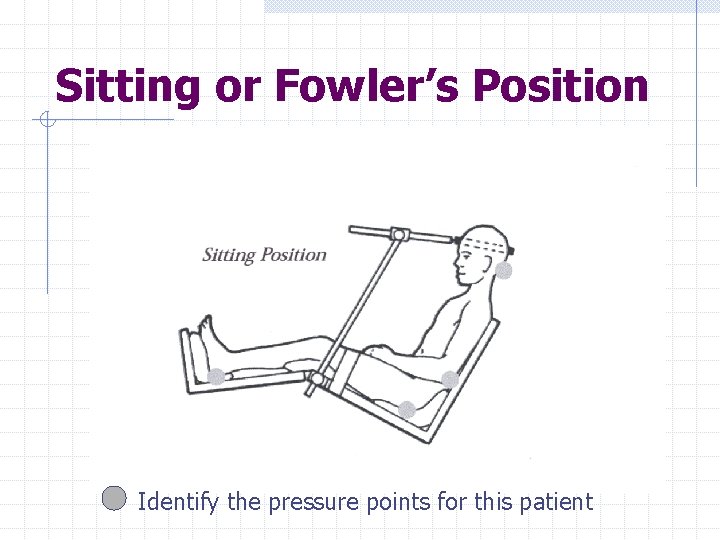
Sitting or Fowler’s Position Identify the pressure points for this patient
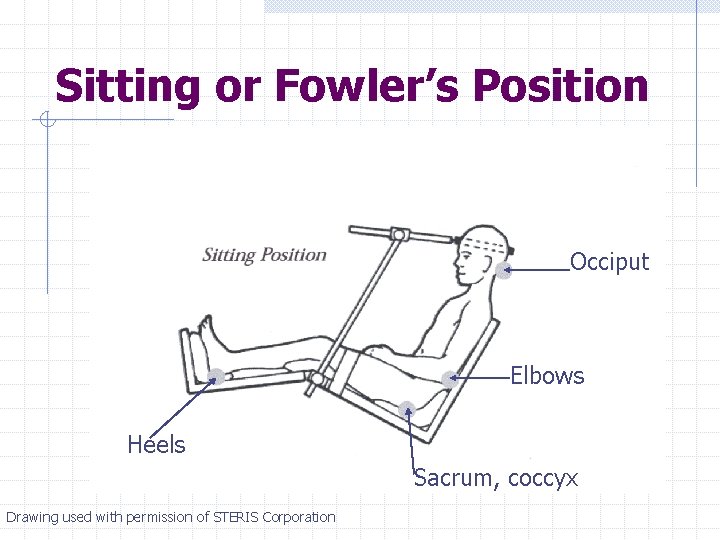
Sitting or Fowler’s Position Occiput Elbows Heels Sacrum, coccyx Drawing used with permission of STERIS Corporation

Positioning Devices
Positioning Devices Arm boards Table brackets for positioning attachments Foot board Foam pads Axillary roll Chest rolls Eggcrate mattress Peg board Wilson Frame Andrews Frame Mayfield® Headrest Vac-Pac (aka “Bean. Bag”) Orthopedic Fracture Table Jackson Table

Safety Strap Never step away from patient on OR bed unless the safety strap is secured! When patient supine, place strap about 2” above knee -- placing the safety strap directly over the knee could cause compression of the popliteal area, and compromise circulation

Armboards Used for most procedures. Armboards should be padded to protect pressure points.
When positioning the patient’s arms: Arms should not be overextended- no more than a 90° from body. Procedures where the arms are positioned at the patients side: position hands with the palmar surface facing the patient’s body-limits pressure on the radial and ulnar nerves

Table Brackets Used to attach positioning devices to OR bed Available in different shapes to accommodate various attachments

Axillary Roll Used for lateral positioning. Aids in chest expansion Prevents pressure on the axillary peripheral nerves Available “ready-made” as pictured, or can be made by covering a 1 L bag of IV fluid with a small towel

Chest Rolls Used for prone positioning Allows for chest expansion in prone patient May reduce blood loss by minimizing pressure on abdominal blood vessels May be made of gel as shown in illustration, or can be “hand-made” using blankets or sheets

Vac-Pac (“Bean Bag”) Used for lateral positioning Can be molded to body contours After patient is positioned, and the vac-pac shaped to support the patient “activate” the vac-pac by using suction tubing to remove air from the bean bag at the air valve—bag will harden. Release bag by squeezing air valve

Foot Board Prevents patient from sliding down in bed when in Reverse Trendelenburg – position Prevents foot drop for patient in sitting position Should be always be well-padded

Mayfield® Headrest Used to position head for neurosurgical procedures Can be used when positioning patient in supine, prone or sitting position When using skull clamp will need Mayfield® pins to hold head in the headrest When using the horseshoe headrest skull pins are not needed
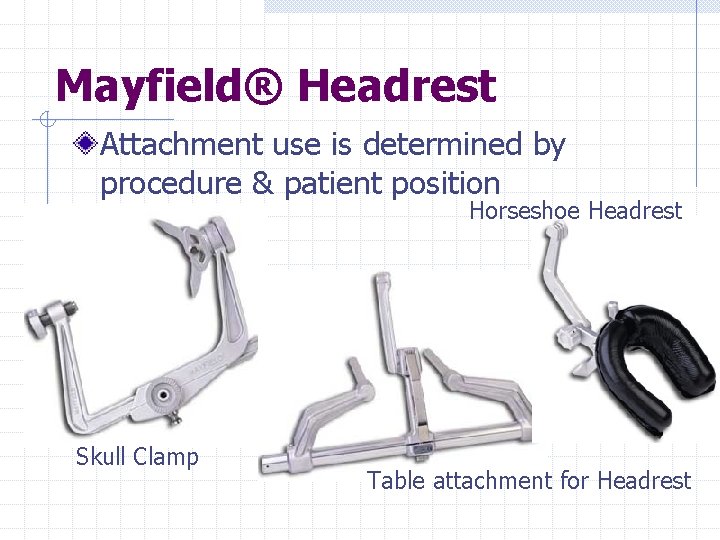
Mayfield® Headrest Attachment use is determined by procedure & patient position Horseshoe Headrest Skull Clamp Table attachment for Headrest

Mayfield® Skull Pins Used to secure patient’s head in Mayfield® Skull Clamp during neurosurgical procedures Pins may be either one-time-use disposable or reusable

Peg Board Used for lateral positioning for orthopedic procedures

Wilson Frame Used for prone positioning Frequently used for spine cases

Andrews Frame Used for prone positioning during spine cases

Jackson Table Used to position patients for spine cases

Fracture Table Allows easy access for intra-operative fluoroscopy

Stirrups Type used depends on procedure/surgeon’s preference “Candy Cane” type stirrups: Allen Stirrups

References AORN (2003) Standards, Recommended Practices and Guidelines Armstrong, D. , Bortz, P. & Halter, M. (2001). An integrative review of pressure relief in surgical patients. AORN Journal, 73, 645 – 674. Mc. Ewen, D. (1996). Intraoperative positioning of surgical patients. AORN Journal, 63, 1059 – 1078. Roth (1995) Perioperative Nursing Core Curriculum Rothrock (2003) Alexander’s Care of the Patient in Surgery Steris (2002) Continuing Education Study Guide Intraoperative Patient Positioning: It’s More than Just Comfort – accessed from the Steris web site: http: //www. steris. com/ UAB Hospital Nursing Standard: Perioperative Plan of Care Warner, M. (2003) 7 Patient Positioning Strategies in Outpatient Surgery Magazine accessed from the web site: http: //www. outpatientsurgery. net/2003/os 08/patient_positioning_strategie s. php? pg=2

Acknowledgements Black and white patient positioning images from: Steris Continuing Education Study Guide- Intraoperative Patient Positioning: It’s More than Just Comfort. Used with permission of Steris Corporation Technical assistance provided by Joann Sharpe Photos of Mayfield® Headrest used with permission of Schaerer Mayfield USA, Inc. Mayfield® is a registered trademark of Schaerer Mayfield USA, Inc. Image of Olympic Vac-Pac used with permission of Olympic Medical
- Slides: 80