Surgical Complications in the General Surgery Bariatric Surgery


Surgical Complications in the General Surgery, Bariatric Surgery, and Endoscopy Population Jennifer C. Yanak, RN, MSN, MBA Brian J. Winkleman, MD

Goals • Increase participants’ understanding of expected vs. unexpected surgical events • Discuss the importance of linking conditions to a surgical procedure and seeking physician clarification when needed • Recognize the difference in “time frame terminology” • Review the impact of documentation on physician profile

What Is a Surgical Complication? • Occurrences and conditions which arise that are not fundamental to the procedure • Deviation from expected operative course • Cause-and-effect relationship • No defined time limit

Defining Proper Terminology • Use proper “time frame” terminology – What does “postoperative” mean? • Adverb: Time relationship • Adjective: Causative relationship • Or. . . eliminate the word “postoperative” altogether to eliminate any confusion • Query in terms of “expected, ” “unexpected, ” or “due to surgery” • The term “status post” can also be misinterpreted as a complication

Impact on Physician Profiles • Better documentation can = worse profile – Complications can be “dings” against a physician’s profile – May lead to physician under documentation – Important to ensure a condition is a “true complication”

Surgical Complications • EVERY surgeon has complications • How to deal with complications: – Basic sciences from medical school – Internship/residency/ fellowship training – Morbidity and mortality conference – Experience from previous complications – Surgical mentor

How to Eliminate Surgical Complications • Achievable by following the “ 3 P’s”: – “Perfect” the surgeon? ? – “Promote” into academia – “Push” into retirement

How Can We Help: Clarify & Query • Clarify the relationship of the patient condition to the surgical procedure – Did the condition exist prior to surgery? • Was the condition present on arrival? • Does the patient have a history of the condition? • A thorough physician preoperative assessment is CRUCIAL, and it must be well DOCUMENTED!!!

How Can We Help: Clarify & Query • Clarify the relationship of the patient condition to the surgical procedure (cont. ) – Did the condition arise after the procedure? • Is the condition a result of the underlying disease, not the surgery? • Is the condition a true complication that occurred during or as a result of the surgery?

Variability • Know that physician responses, coding, and practice guidelines will vary – Nurse to nurse – Coder to coder – Surgeon to surgeon – Hospital to hospital • You can only control the way your CDI team practices at your institution

Acute Blood Loss Anemia • • • Was it present on arrival or before surgery? Dilutional True (lab) anemia Was the anemia treated/monitored? Was the anemia due to a disease process or the surgery? • Transfusions do not necessarily mean a complication – Blood can be given as a prophylactic measure

Acute Blood Loss Anemia: Coding & Documentation • Postoperative anemia 285. 9 • Acute blood loss anemia 285. 1 (cc) – Coding Clinic, first quarter 2007, p. 19 • Hemorrhage complicating a procedure 998. 1 – Coding Clinic, third quarter 2003, p. 13 • Often based on the physician’s clinical judgment, not necessarily labs and transfusions – Coding Clinic, third quarter 2004, p. 4
Ileus • Transient non-mechanical bowel obstruction resulting from aperistalsis of the GI tract • Expected after major abdominal surgery – Exploratory laparotomy for obstruction: 3 to 7 days – Open colon resection: 3 to 5 days – Laparoscopic colon resection: 2 to 4 days • Up to 15% of patients may develop prolonged ileus

Ileus • How to minimize postoperative ileus: – Laparoscopic techniques • Smaller incision sizes • Reduced analgesic requirement – Nasogastric tubes? – Thoracic epidurals – Limit narcotic usage – Ketorolac (Toradol) • NSAID

Ileus: Coding and Documentation • Was it present on arrival or present prior to surgery? • • Was it treated? Paralytic ileus 560. 1 (cc) Intestinal obstruction due to a procedure 997. 4 In order to know if the ileus was expected or a complication, the physician would need to be queried
Surgical Site Infections • Incidence: 2. 6% of hospitalized patients • 500, 000 surgical site infections annually in the U. S. • Increase healthcare costs, length of hospital stay, morbidity and mortality

Surgical Site Infections • Patient factors: – Age – Obesity – Diabetes mellitus – Malnutrition – Depressed immune system – Presence of infection at remote body site – Colonization

Surgical Wounds • Is the wound infected or non-healing? • Wounds intentionally left open should NOT be coded as complications • No time limit for wound infection to occur • Does the patient have risk factors that delay wound healing?

Surgical Wounds: Coding & Documentation • Healing slowly/non-healing 998. 83 – Clarify if delayed wound healing is due to the surgery or due to another disease process/risk factor • Dehiscence 998. 31 and 998. 32 – Used for operative or surgical wounds • Disruption of a traumatic injury wound 998. 33 – Used for a previously closed traumatic wound • Coding Clinic, fourth quarter 2008, pp. 149– 152

Malnutrition • Includes undernutrition and overnutrition • Major impact on wound healing and immune system • Appearance, weight loss, disease process • Look for BMI, albumin, total protein, prealbumin, diet type, dietary supplementation • No definition available from CMS – Set practice criteria with your CDI team and include RD for guidance

Malnutrition • Well-nourished or mildly malnourished patients usually require no additional nutritional support if an oral diet is expected within 4 to 7 days • There is some evidence that patients with preexisting nutritional deficits may benefit from 7 to 10 days of preoperative enteral or parenteral supplementation • Patients at increased risk for postoperative complications: – Esophagectomy with albumin level < 3. 75 g/d. L – Gastrectomy or pancreatectomy with albumin level < 3. 25 g/d. L – Colectomy with albumin < 2. 5 g/d. L

Malnutrition: Coding & Documentation • 263. * (mild, moderate, unspecified - cc) • 261 severe malnutrition (mcc) • 579. 3 malnutrition following GI surgery (cc) – Coding Clinic, fourth quarter 2003, pp. 104– 105

Atelectasis/Respiratory Insufficiency/ Respiratory Failure • Make sure respiratory issue is more than just anesthesia reversal • Is the intubation for safety concerns and not for actual respiratory failure? • Most common respiratory issues after surgery are atelectasis and pneumonia

Atelectasis/Respiratory Insufficiency/ Respiratory Failure: Coding & Documentation • When in doubt, always clarify • Atelectasis 518. 0 (cc) – More than just an incidental finding – Coding Clinic, fourth quarter 1990, p. 25 • Acute respiratory failure (518. 81 - mcc) • Respiratory insufficiency following trauma and surgery (518. 5 - mcc) – Coding Clinic, third quarter 1988, pp. 8– 9 • Look for Bipap/CPAP, not just intubation

Case Studies • General surgery – Appendectomy – Cholecystectomy • Bariatric surgery – Gastric bypass • Endoscopy – Colonoscopy
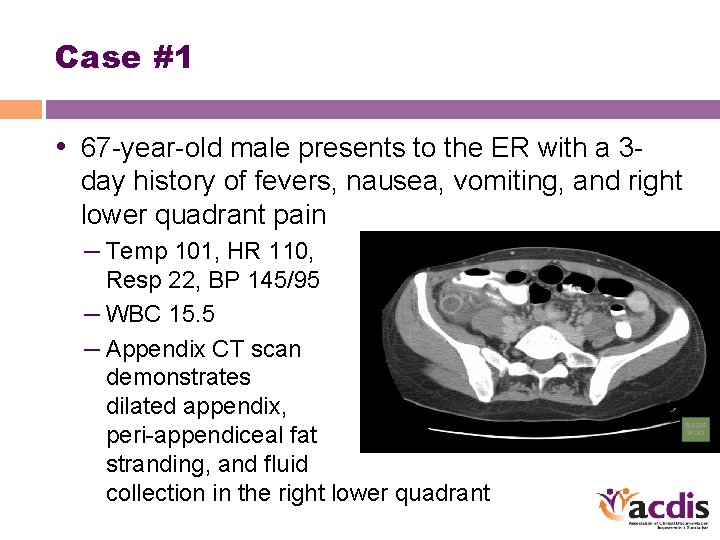
Case #1 • 67 -year-old male presents to the ER with a 3 day history of fevers, nausea, vomiting, and right lower quadrant pain – Temp 101, HR 110, Resp 22, BP 145/95 – WBC 15. 5 – Appendix CT scan demonstrates dilated appendix, peri-appendiceal fat stranding, and fluid collection in the right lower quadrant
Case #1 • Patient taken to the OR for laparoscopic appendectomy – Perforated appendicitis, base of the appendix is retrocecal and “stuck” – Converted to open appendectomy – Abdomen washed out with antibiotic solution – Patient discharged home on POD #2
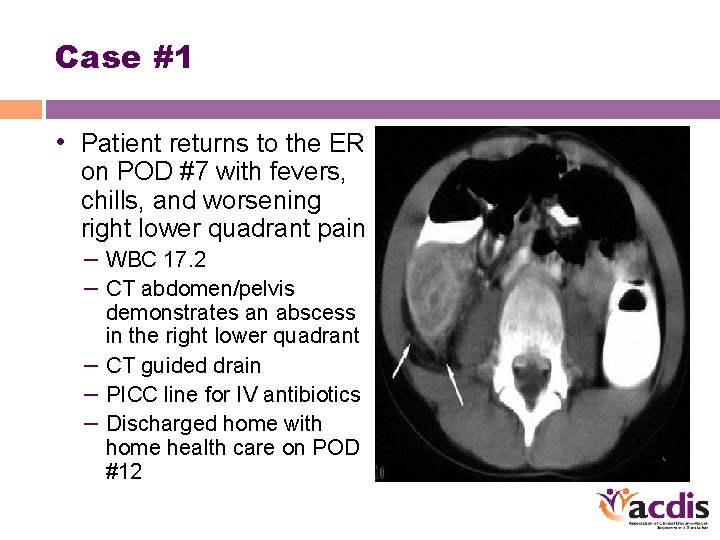
Case #1 • Patient returns to the ER on POD #7 with fevers, chills, and worsening right lower quadrant pain – WBC 17. 2 – CT abdomen/pelvis demonstrates an abscess in the right lower quadrant – CT guided drain – PICC line for IV antibiotics – Discharged home with home health care on POD #12
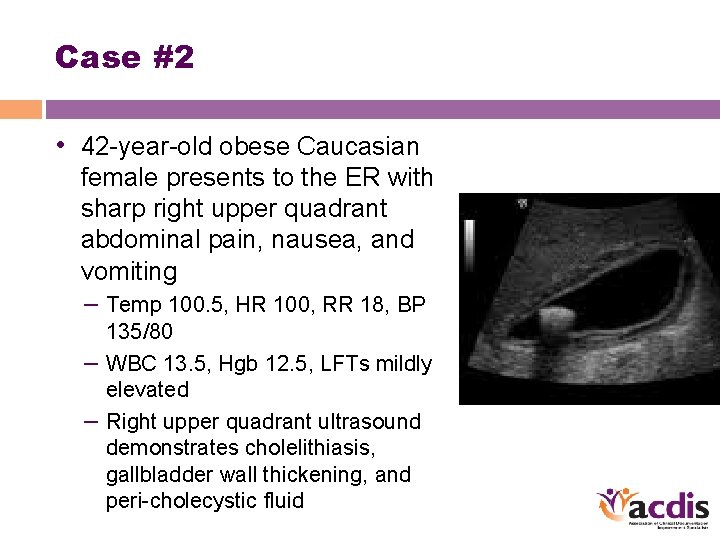
Case #2 • 42 -year-old obese Caucasian female presents to the ER with sharp right upper quadrant abdominal pain, nausea, and vomiting – Temp 100. 5, HR 100, RR 18, BP 135/80 – WBC 13. 5, Hgb 12. 5, LFTs mildly elevated – Right upper quadrant ultrasound demonstrates cholelithiasis, gallbladder wall thickening, and peri-cholecystic fluid
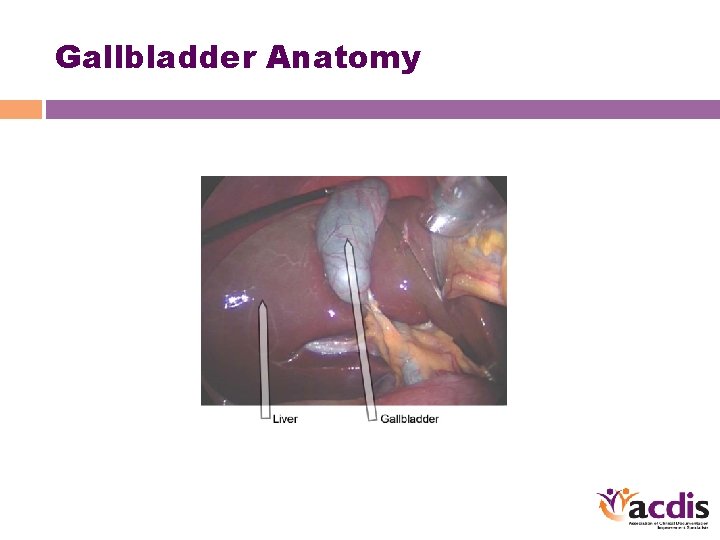
Gallbladder Anatomy
Case #2 • Converted to open cholecystectomy secondary to bleeding from the gallbladder fossa – EBL 350 cc • While in the recovery room: – Patient pale, HR 130, BP 90/60 – Hgb 6. 2 • Patient taken back to OR for exploration – Bleeding from the cystic artery

Case #3 • 55 -year-old female with morbid obesity (BMI 65), hypertension, hyperlipidemia, non-insulindependent diabetes mellitus, sleep apnea on CPAP – Undergoes laparoscopic Roux-en-Y gastric bypass with a 150 cm limb – Intraoperative esophagogastroduodenoscopy demonstrates a patent, hemostatic anastomosis with no evidence of leak
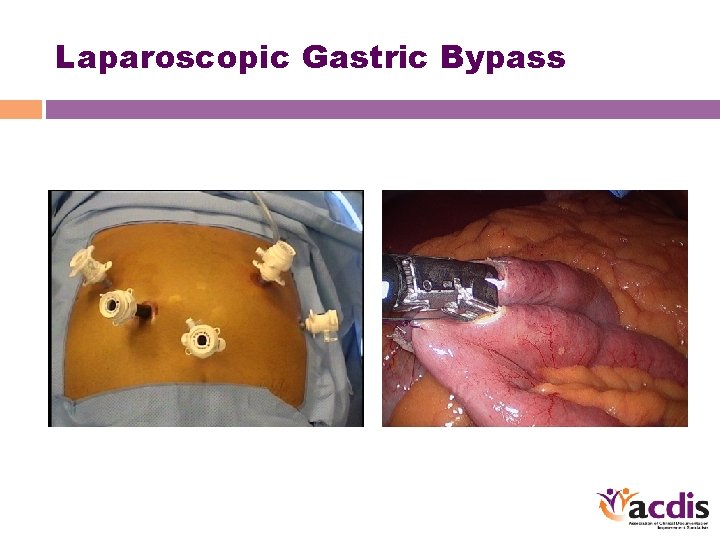
Laparoscopic Gastric Bypass
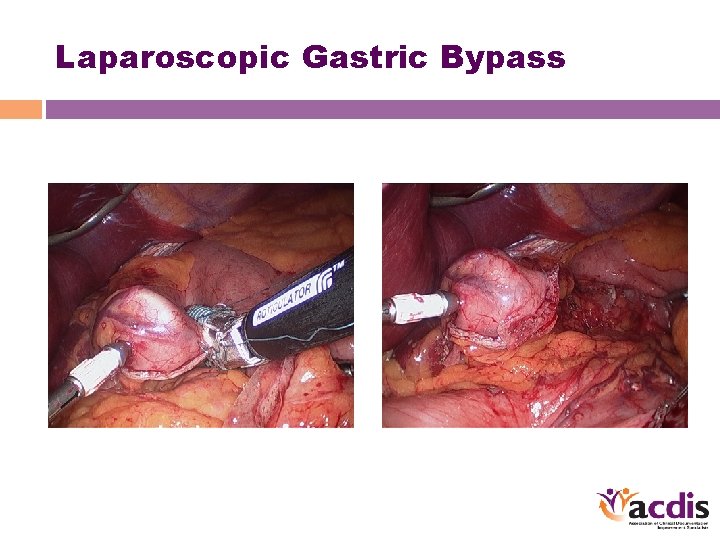
Laparoscopic Gastric Bypass
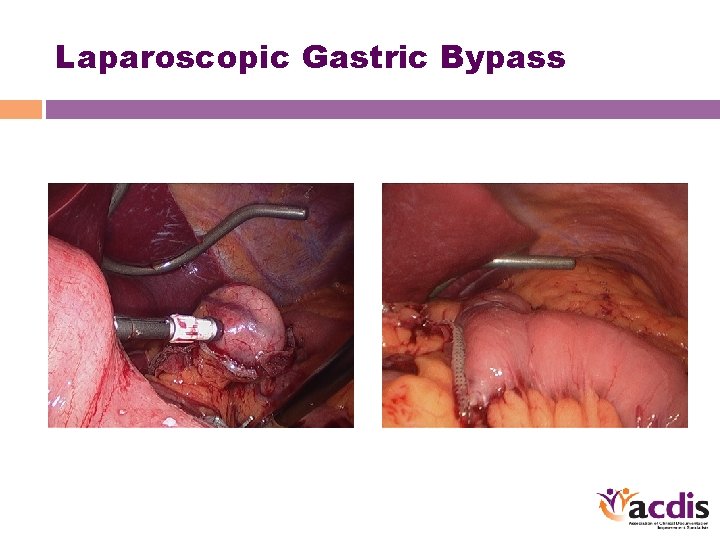
Laparoscopic Gastric Bypass
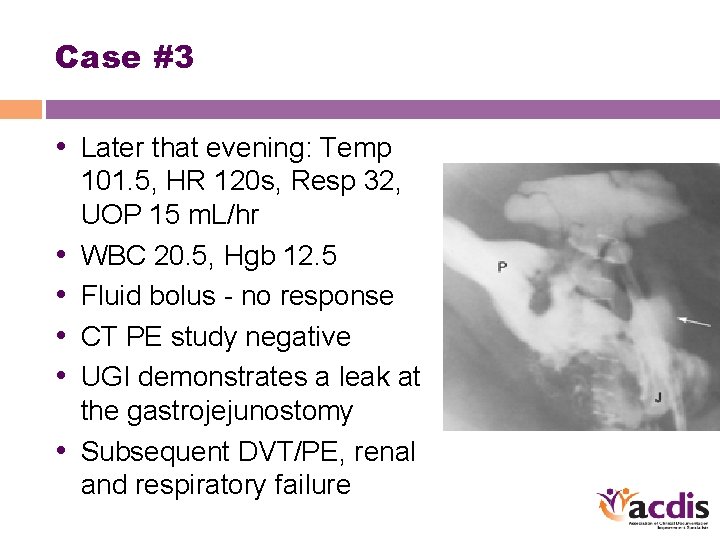
Case #3 • Later that evening: Temp • • • 101. 5, HR 120 s, Resp 32, UOP 15 m. L/hr WBC 20. 5, Hgb 12. 5 Fluid bolus - no response CT PE study negative UGI demonstrates a leak at the gastrojejunostomy Subsequent DVT/PE, renal and respiratory failure
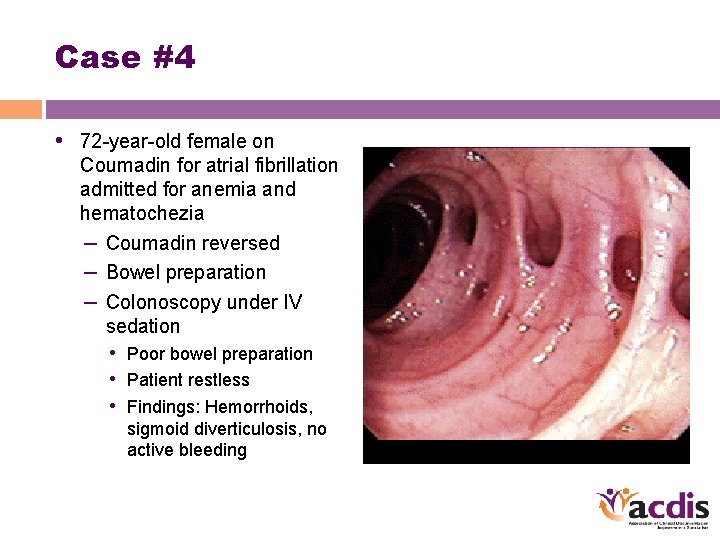
Case #4 • 72 -year-old female on Coumadin for atrial fibrillation admitted for anemia and hematochezia – Coumadin reversed – Bowel preparation – Colonoscopy under IV sedation • Poor bowel preparation • Patient restless • Findings: Hemorrhoids, sigmoid diverticulosis, no active bleeding
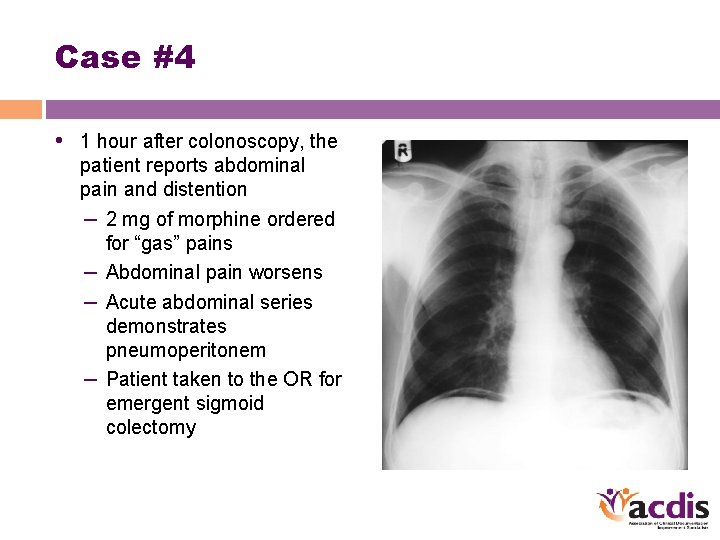
Case #4 • 1 hour after colonoscopy, the patient reports abdominal pain and distention – 2 mg of morphine ordered for “gas” pains – Abdominal pain worsens – Acute abdominal series demonstrates pneumoperitonem – Patient taken to the OR for emergent sigmoid colectomy

Endoscopy • Risks – Anesthesia – Bleeding • 1 in 1000 cases – Perforation • 1 in 1700 cases • 1 in 700 cases with polypectomy

- Slides: 41