Supported in part by Arkansas Blue Cross and

Supported in part by Arkansas Blue Cross and Blue Shield and the Office of the Arkansas Drug Director and in partnership with the Arkansas Academy of Family Physicians (AAFP), the Arkansas Medical Society (AMS), the Arkansas State Medical Board (ASMB), the Arkansas Department of Health (ADH) and its Division of Substance Misuse and Injury Prevention (Prescription Drug Monitoring Program—PDMP) Continuing Education Credit: TEXT: 501 -406 -0076 Event ID: 24857 -23985

AR-IMPACT Team Members • • • Michael Cucciare, Ph. D Johnathan Goree, MD Corey Hayes, Pharm. D Teresa Hudson, Pharm. D, Ph. D Shona Ray-Griffith, MD Leah Tobey, PT, DPT • Graduate Student: Andrea Melgar-Castillo

Flow of the Case Conferences • • General Information: 5 minutes Topic Presentation: 20 minutes Case Conference: 25 minutes Feedback and Thoughts on Future Sessions: 5 minutes

• • AR-IMPACT website: arimpact. uams. edu AR-IMPACT email address: AR-IMPACT@uams. edu Twitter: @Arkansas. Impact Joining the Conference: – Click to join: https: //join. uams. edu/invited. sf? secret=Yt. VKQk. Hso. WTg. Jaguonym. Zw &id=415081971 – Or call in: 1 -844 -885 -1319, then enter 415081971

Faculty Disclosure of Financial Relationships: The planners of this RSS, Corey Hayes, Michael Cucciare, Johnathan Goree, Leah Tobey, Teresa Hudson, Marti Morrison and Cathy Buzbee have no financial relationships with commercial interests to disclose. A planner of this RSS, Shona Ray-Griffith, MD, has a financial relationship with a commercial interest to disclose: Neuronetics, Inc. – Contracted Research. The speaker of this RSS has no financial relationships with commercial interests to disclose. The accreditation compliance reviewers of this RSS, Karen Fleming and Courtney Bryant, have no financial relationships with commercial interests to disclose.

Continuing Education • Accreditation: In support of improving patient care, University of Arkansas for Medical Sciences is jointly accredited by the Accreditation Council for Continuing Medical Education (ACCME), the Accreditation Council for Pharmacy Education (ACPE), and the American Nurses Credentialing Center (ANCC), to provide continuing education for the healthcare team. • Credit Designation: The University of Arkansas for Medical Sciences designates this live activity for a maximum of 1 AMA PRA Category 1 Credit™. Physicians should claim only the credit commensurate with the extent of their participation in the activity. • The University of Arkansas for Medical Sciences designates this live activity for a maximum of 1 ANCC contact hour. Nurses must attend the entire session in order to receive credit. • This knowledge-based activity will provide pharmacists up to 1. 0 contact hours or 0. 1 CEU. ACPE# JA 0000298 -0000 -18 -040 -L 01 -P • AAFP Credit: Submit your AMA credit • Pharmacists: Please email us your NABP number and month and day of birth
Other General Information CISCO IPhone App CISCO Meeting Information • Please mute your microphone in CISCO • Able to ask questions through CISCO Chat

Tips: Chronic Back Pain. Johnathan Goree, MD Director of Interventional Pain Management Services Assistant Professor Department of Anesthesiology University of Arkansas for Medical Sciences

Outline • Anatomy of Chronic Back Pain? • 2 minute lumbar spine examination
Why Back Pain? • 8 out of 10 people experience some type of back pain during their lifetime. • One quarter of adults have reported having low back pain lasting at least one whole day in the past three months. • Total direct costs of chronic lowback pain-related health care utilization are estimated to be $90 billion a year.

Categories of Chronic Back Pain • Axial Pain along the axis of the spine – Usually Isolated in Low back – Sometimes has referral patterns to buttocks, posterior (and even anterior) thighs – Never pain below the knees. • Radicular Pain extending to one of more extremity – Characterized by pain in legs. – Usually burning or electric in character – Usually in a dermatomal pattern or in a specific nerve distribution.

Axial Pain Generating Structures • • • Muscle/Skin Facet Joints Intervertebral Discs Vertebral fractures Sacroiliac Joints

Axial Pain Generating Structures • • • Muscle/Skin Facet Joints Intervertebral Discs Vertebral fractures Sacroiliac Joints
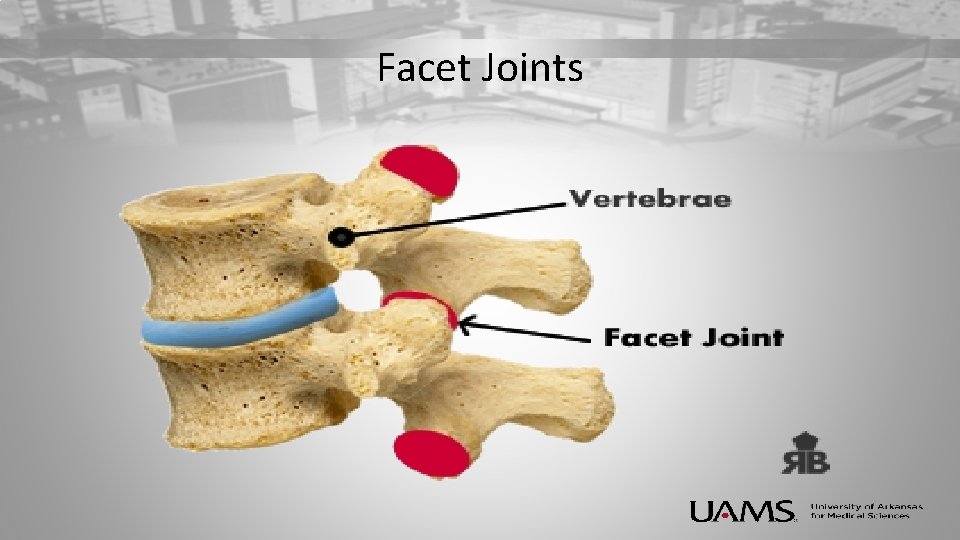
Facet Joints
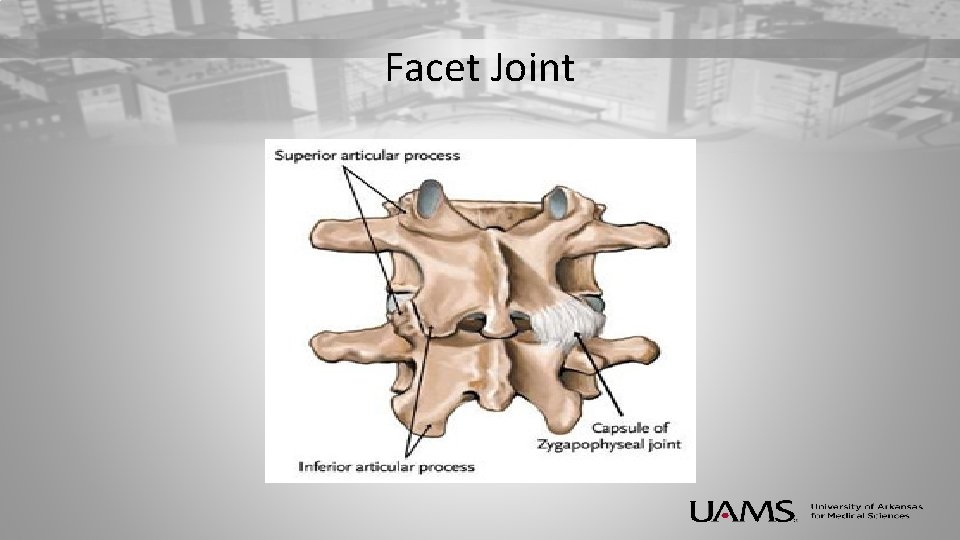
Facet Joint

Facet Mediated Pain/Facet Arthropathy • Diagnosis – Clinical – Based on History of Physical – Can be confirmed with diagnostic facet and medial branch procedures • Typical History – Axial low back pain – Worse when standing or walking – Have to lean on counter when washing dishes or brushing teeth – Osteoarthritis in geriatric population – Car accidents/ Whiplash – Morning stiffness
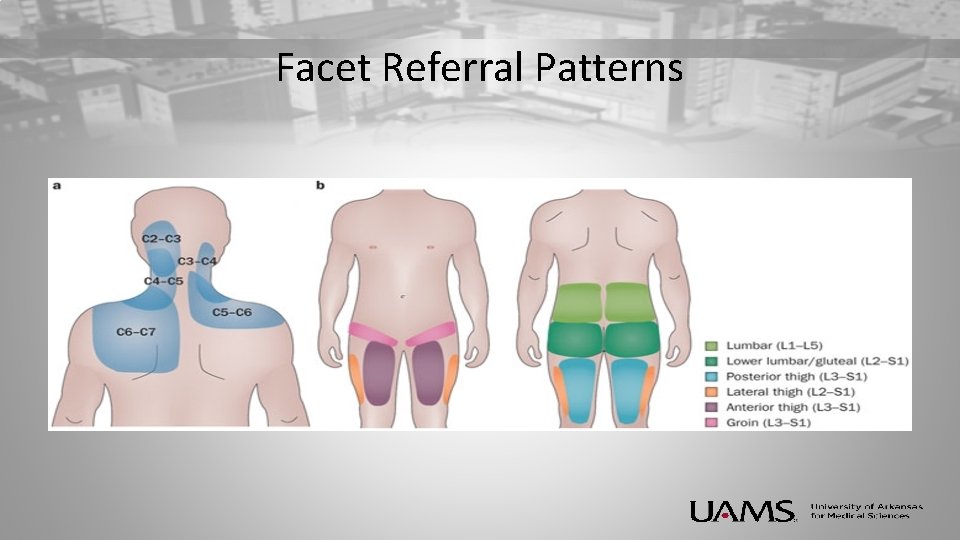
Facet Referral Patterns
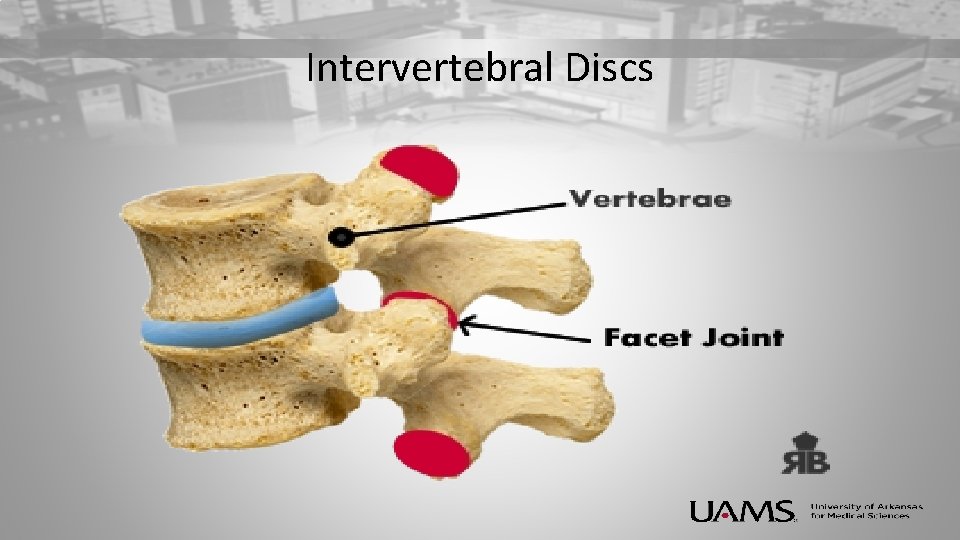
Intervertebral Discs

Discogenic Pain • Diagnosis – Clinical – Based on History of Physical – Can be confirmed with Imaging • Typical History – Axial low back pain – Worse when bending or sitting – Intermittent radicular component – Often after acute event – Often associated with spasm
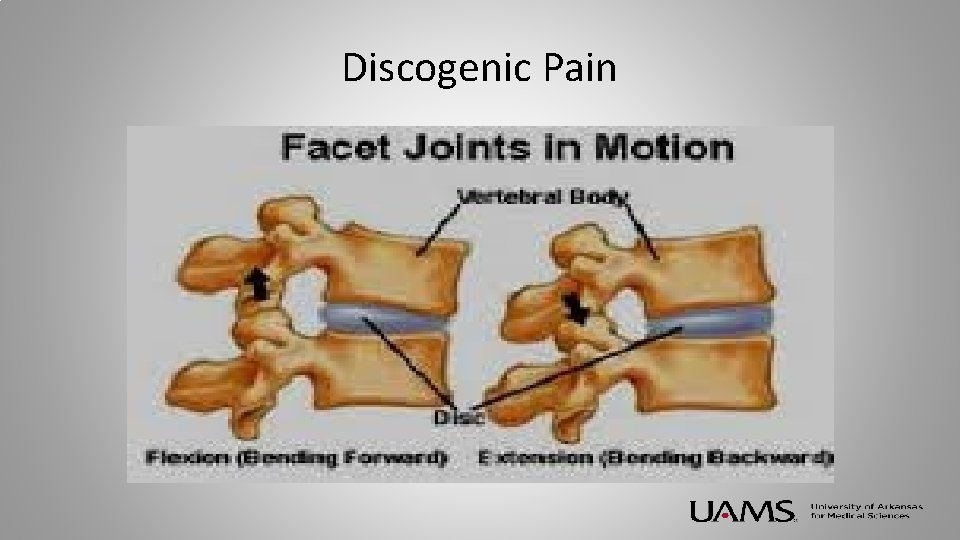
Discogenic Pain
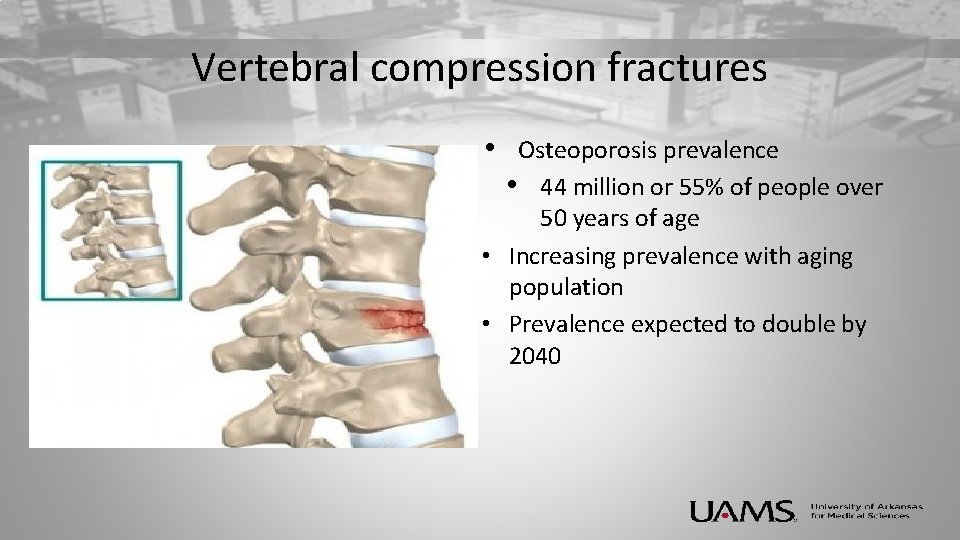
Vertebral compression fractures • Osteoporosis prevalence • 44 million or 55% of people over 50 years of age • Increasing prevalence with aging population • Prevalence expected to double by 2040

Vertebral Compression Fracture • Diagnosis – Initially Clinical – Confirmed with X-ray – MRI will determine age of fracture and what treatment can be offered • Typical History – Sudden axial Low back pain – Often after fall or trauma – Often in geriatric population – High risk for Osteoporosis – Patients with history of fractures at higher risk

Basic Lumbar Spine Examination • Ambulation (can begin in the waiting room) – Could gait be causing pain or be a result of pain? • Inspection – Look for signs of imbalance, skin disease, or trauma – r/o scoliosis, shingles, spasm • Flexion and Extension – Look for worsening/improvement of pain by position – r/o facet disease or disc disease

Basic Lumbar Spine Examination II • Palpation – Midline palpation (r/o compression fractures) – 1 cm from midline (r/o facet disease) – Quadratus lumborum (r/o myofascial disease) • Heel and Toe walk – Screening test for lower leg strength • FABER and Log Roll – r/o causes of hip pain and SI joint pain.
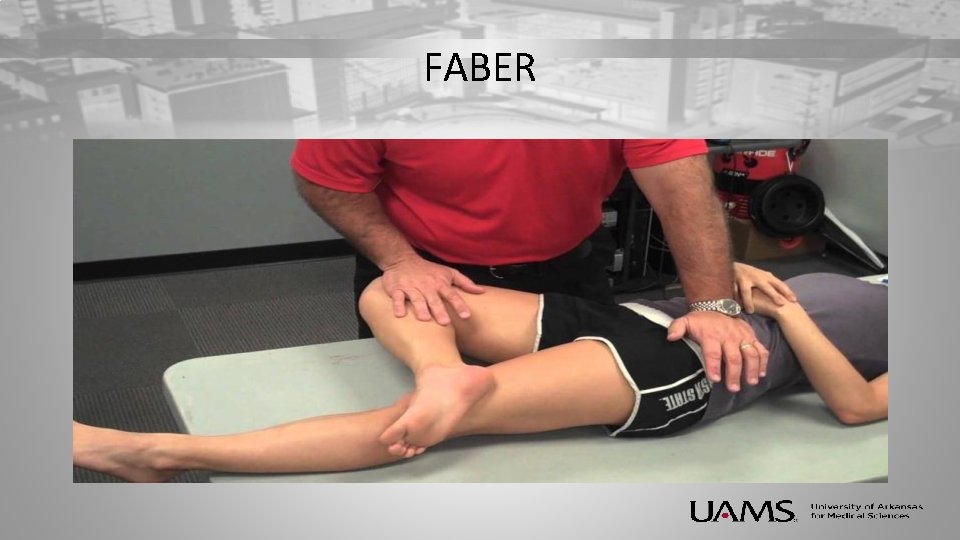
FABER

Summary • The vast majority of lumbar spine pain is myofascial in nature • Ruling out other causes of lumbar spine pain can allow for more expedient treatment if conservative management fails • There are multiple structures that can cause acute or chronic lumbar spine pain • A quick examination of the lumbar spine can be done in less than 2 minutes.

QUESTIONS ABOUT THE TOPIC Continuing Education Credit: TEXT: 501 -406 -0076 Event ID: 24857 -23985

CASE CONFERENCE AND FEEDBACK Continuing Education Credit: TEXT: 501 -406 -0076 Event ID: 24857 -23985
- Slides: 28