Supplies and Instrumentation 1 Case Planning Combines Knowledge

Supplies and Instrumentation 1

Case Planning • Combines – Knowledge of a procedure – Surgical techniques • Surgical categories – Diagnostic – Reconstruction – Repair – Removal – Replacement or implantation 2

Case Preparation • Assignment • Gathering supplies and instruments • Reviewing the surgeon’s preference card – – – – Instruments Special equipment Glove and gown size Skin prep and draping Medications Idiosyncrasies Dressings 3

Instruments • • • Think about what you need Setup varies Place instruments in a specific place Know where you place your instruments If stacking trays, place heavy tray on the bottom 4

The Mayo Stand • Use for placement of frequently needed instruments and supplies • Setup varies • Select method best for you • Standardized set-up may exist at individual facilities • Keep your Mayo neat and clean 5

The Mayo Stand 6

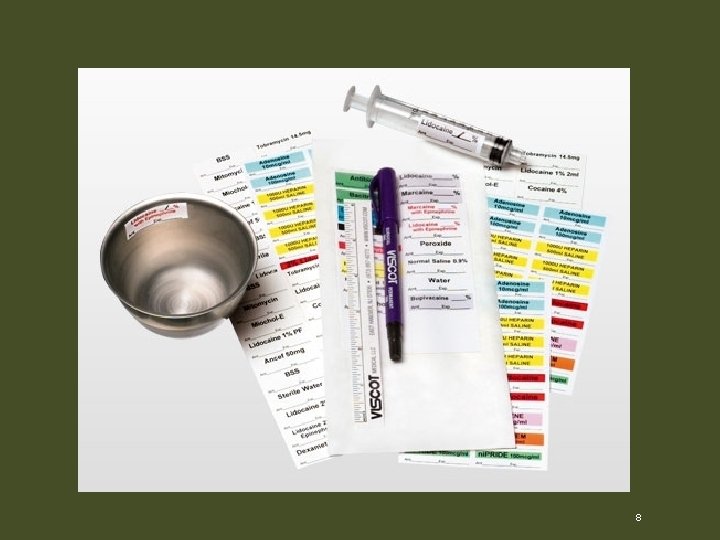
Solutions and Drugs • Irrigations – May be distributed after the start of the case • Label irrigations • Use basin on single- or double-ring stand • May have slush basin or solution warmers • Medications on the field are labeled 7
8

Counts • Purpose – Prevent items from being retained in the patient • Responsibility – Circulator – Ensuring correct count and recording information on the operative report – Surgical technologist – Knowing where all counted items are located throughout the case • Retained items may cause – Injury – Infection – Perforation of an organ – Scarring – Repeat surgery to remove item 9

Counts • When counts are performed – Before the procedure – Before closure of an organ – Before closure of a body cavity – Before skin closure – When there is suspicion of a retained item – When there is permanent change in personnel 10

Counts • Counted items – Instruments – Sponges – Sharps – Vessel loops – Dissectors – Suture – Any item subject to being retained 11

Elsevier items and derived items © 2010, 2007 by Saunders, an imprint of Elsevier Inc. 12

Counts • Procedure for closing counts – Patient (sterile field) – Items on the Mayo – Items on the back table – Items discarded from the field 13

Counts • Search for lost items – Notify surgeon – Look in all trash and waste receptacles – Shift equipment on the back table – Examine the floor and under the OR table – Look between the surgeon and the patient – Use a magnetic roller – Use x-ray study to identify retained items 14

Counts • http: //www. youtube. com/watch? v=bx. Gpk_1 C 1 vg • http: //www. youtube. com/watch? v=GLj. FFauu uao&feature=relmfu • http: //www. youtube. com/watch? v=AA 14 b 6 r. I u 0 g&feature=relmfu 15

Starting the Procedure • • Patient is transported to the OR Patient is transferred to the OR table Anesthesia is administered Patient is prepped by the circulator Patient is draped Items are secured to drape Procedure begins 16

Time Out • A team event that verifies – Correct patient – Correct side and site – Agreement on the procedure being done – Correct position – Availability of correct implants and special equipment 17

Management of the Field • Maintain an orderly setup – Organize items neatly – Use suture bag – Keep instruments off the patient – Clear suction tips – Don’t overmanage – Replace soiled sponges with new ones – Concentrate on the procedure 18

Management of the Field • Lighting – Position for adequate lighting • Sponges – Complete with radiopaque strips • • • Ray-Tec Laparotomy sponge Dissector Tonsil sponge Neurosurgical sponges 19

Sponges Peanut Lap sponge Ray-Tec Tonsil 20 20

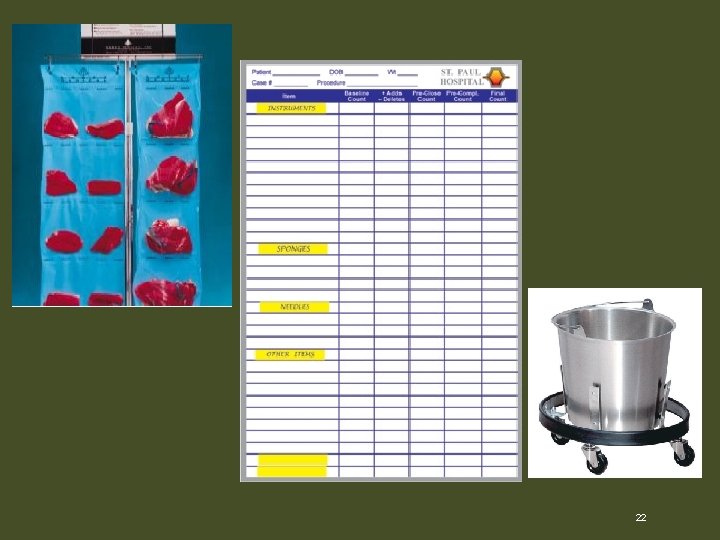
Management of the Field • Managing sponge count – Use kick bucket for use laparotomy and Ray-Tec sponges – Dissection sponges are placed back into their holders on the sterile field – Sponges are placed where the surgical technologist can see them – Additional sponges are added to the initial count 21

22

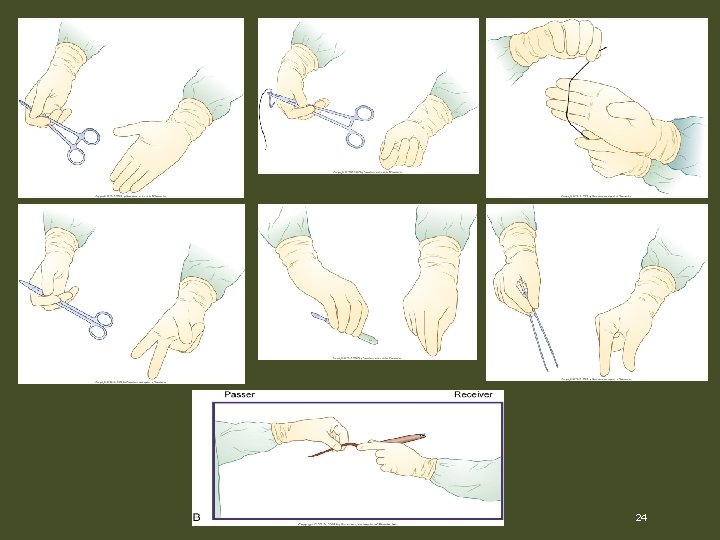
Management of the Field • Handling and passing instruments – Time is needed to develop speed and coordination – Do not rush; rushing leads to mistakes – Pass instruments in their closed position – Pass medium-weighted instruments firmly – Pass delicate instruments lightly – Use hand signals or hand motions 23
24

Management of the Field • Passing instruments – Long instruments – Replace short one when the wound is deep – Microsurgical instruments – Placed in surgeons’ hands so they do not have to remove their eyes from eye piece 25
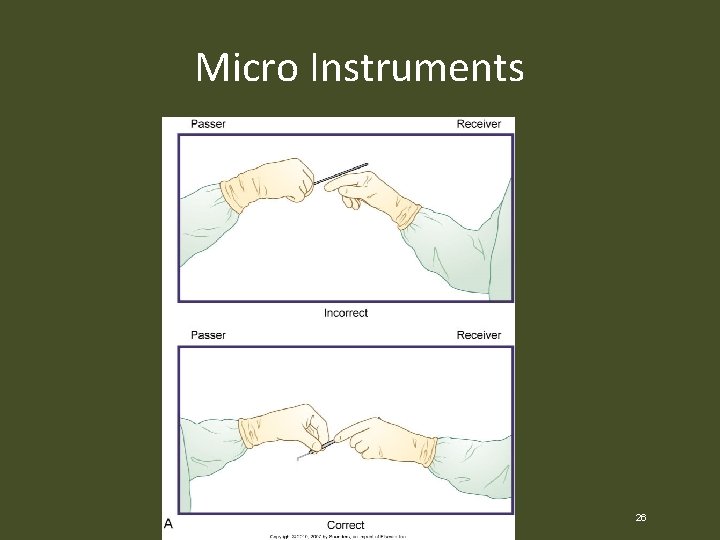
Micro Instruments 26

Management of the Field • Retraction – Placed at wound edges as incision becomes deeper – Sharp-tipped use on skin and subcutaneous tissue – May be • Self retaining • Hand held – May involve delicate tissue – Refrain from use of excessive pressure 27

Management of the Field • Specimens – Removed for pathological studies – Loss of specimen is serious – Mishaps related to specimens • • Incorrect identification Loss of specimen Failure to identify cancerous margins Failure to identify tissue origin 28

Management of the Field • Recommendations for specimen handling – Tag or mark specimen – Identify and label each specimen – Do not pass specimen off until surgeon approves – Do not use sponges to wrap specimen – Do not distort specimen – Never discard any tissue 29

Management of the Field • Receiving specimens from the field – Place in appropriate container – Document time and origin of specimen – Specimen is placed in the proper medium – Surgeon orients specimen to location within the body 30

Management of the Field • Specimen identification – Patient identification – Type of tissue – Origin of tissue – Diagnosis – Special markings – Date and time of surgery 31
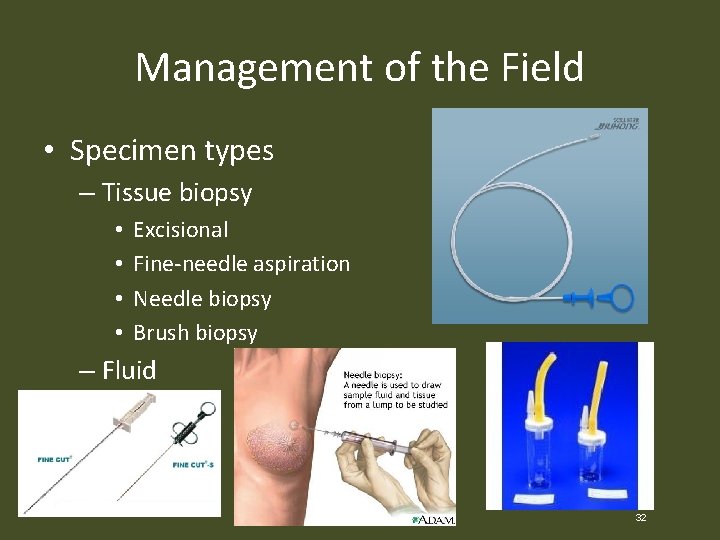
Management of the Field • Specimen types – Tissue biopsy • • Excisional Fine-needle aspiration Needle biopsy Brush biopsy – Fluid 32

Management of the Field • Specimen types (cont. ) – Stones – Foreign body – Amputated limb – Frozen section – Cultures 33

Management of the Field • Wound closure – Irrigated – Before closure, counts are completed – Dressing material can now be opened – Wound is cleaned once closed – Dressing are applied – Patient is covered – Patient is transported to postanesthesia care unit (PACU) 34

Hemostasis • Technical terms – Control bleeding • • Suture Surgical instruments Thermal energy Drugs 35

Hemostasis • Physiological terms – Control bleeding • Conservation of the total volume • Prevention of hematoma – Control oozing – Secure hemostasis 36

Coagulation • Coagulation process – Vasospasm – Platelet plug formation – Coagulation begins 37

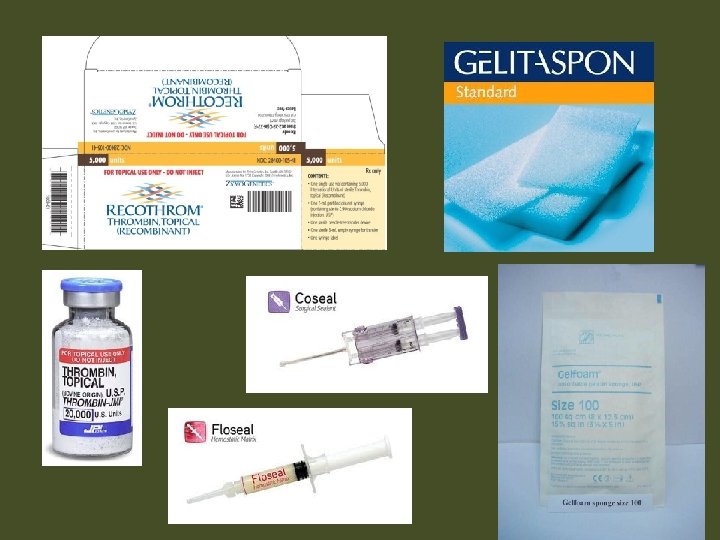
Hemostatic Agents • Chemical agents – Tropical thrombin – Absorbable gelatin – Oxidized cellulose – Collagen absorbable hemostat – Bone hemostasis – Autotransfusion 38
39

Hemostatic Agents • Thermal – ESU (Ethicon Ultracision scalpel) – Laser – Ligasure – Autosonix – Harmonic – PK • Pneumatic tourniquet 40

Harmonic 41

Ligasure 42

PK 43
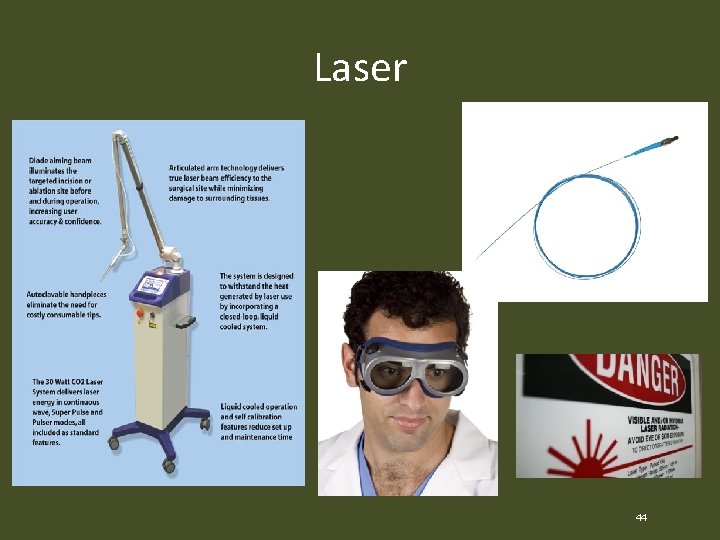
Laser 44

Energy in the OR • Energy use in the operating room (OR) – Cut tissue – Coagulate blood vessels – Destroy diseased tissue • Forms of Energy – – – Electrical Radiofrequency Kinetic Sound Thermal Laser 45

Electrical Energy • Concepts of electrosurgery – Transmits high-frequency electricity – Does not interfere with body functions – Voltage and frequency are easily manipulated 46

Electrical Energy • Most common use of electrosurgery (ESU) – Make an incision – Coagulate blood vessels – Destroy or remove diseased tissue – Weld tissue together 47

Electrical Energy • Components of electrosurgery unit (ESU) – Power unit (generator) – Active electrode (pencil) – Controls – Patient return electrode (Bovie pad) 48

49

Cautery Tips 50

51

Electrical Energy • Circuits used in electrosurgery unit (ESU) – Monopolar – Requires the use of a return electrode (Bovie pad) – Bipolar – No return electrode (Bovie pad) needed 52
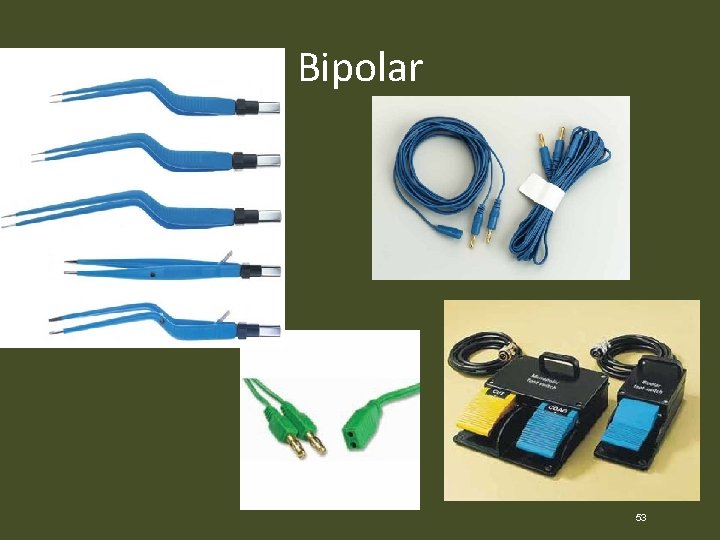
Bipolar 53
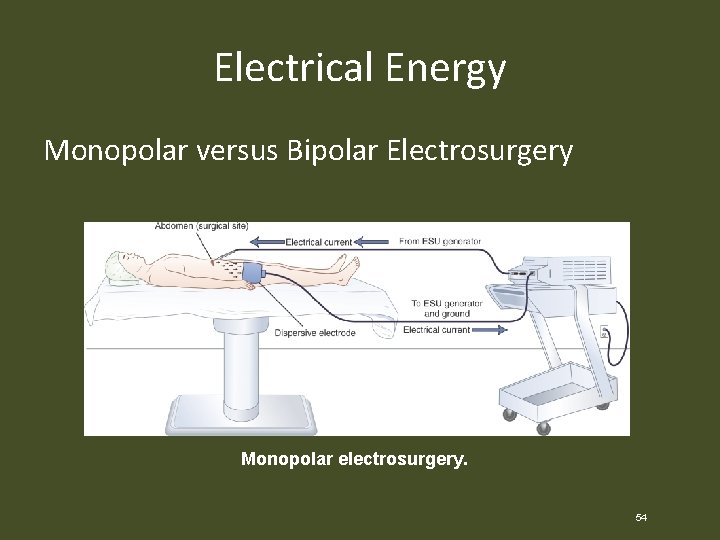
Electrical Energy Monopolar versus Bipolar Electrosurgery Monopolar electrosurgery. 54

Electrical Energy • Electrosurgical unit (ESU) working modes – Cutting – High voltage causes desiccation of tissue – Coagulation – Low voltage results in tissue welding – Fulguration – Coagulation occurs with intermittent applications of energy 55

Electrical Energy • Radiofrequency ablation (RFA) – Destruction of tissue using radio frequency – Used for tumors and endometrial tissue – Electrode inserted into diseased tissue 56
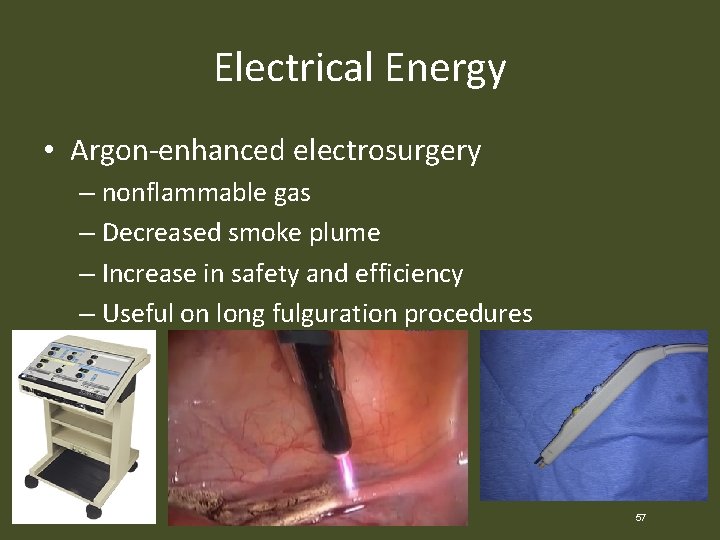
Electrical Energy • Argon-enhanced electrosurgery – nonflammable gas – Decreased smoke plume – Increase in safety and efficiency – Useful on long fulguration procedures 57

Electrical Energy • Electrosurgical hazards (cont. ) – Patients with implanted electrical devices • • • Pacemaker Defibrillator Deep brain stimulator Ventricular assist device Spinal cord stimulator Programmable ventricular shunt Cochlear implant Auditory brainstem implant Bone conduction stimulator 58

Electrical Energy • Kinetic energy – Ultrasonic energy – Transformation of electrical energy into mechanical energy – Ultrasonic ablation – Alternative to electrosurgery • The Cavitron Ultrasonic Surgical Aspirator (CUSA) • Phacoemulsifier 59
Electrical Energy • Cold thermal energy – Cryosurgery – Cold instrument or substance to destroy tissue – Cryoablation – Insertion of a probe into a tumor with injection of argon gas 60

Electrical Energy • Laser categories – Continuous wave – Steady beam of light – Q-switched – Emitted in bursts or pulses • Tissue reaction depends on – Laser wavelength – The power setting – Absorption quality of the cells 61

Electrical Energy • Laser types – Argon (gas) – Visible blue-green beam – Carbon dioxide (gas) – Invisible to the human eye – helium-neon beam used for visibility – Holmium: YAG (yttrium aluminum garnet) (solid) – Outside the visible light range – Neodymium: YAG (solid) – Invisible to the human eye – Helium-neon beam used for visibility 62

Electrical Energy • Laser types (cont. ) – Potassium-titanyl-phosphate (KTP) (solid) – Green laser light – Eximer (gas) – Specialized ultraviolet mirrors and optics are needed to operate safely – Tunable-dye (Solid) – Spectrum of light is tuned to produce light of a particular wavelength (color) 63

Electrical Energy • Laser safety – Classifications of safety risk • • • Class 4 – Causes permanent eye damage Class 3 B – Causes severe eye injury Class 3 A – No injury if viewed momentarily Class 2 – Normally no harm caused Class 1 – Are not hazardous for continued viewing 64

Electrical Energy • Patient and staff protection – Protective eyewear for each specific laser – Filter on optics – Protection of patient’s eyes – Cover reflective surfaces, and post signs – Place protective eyewear outside the room • Airway protection – Wrap endotracheal tube with special metallic foil – Decease flow of volatile gases 65

Suture Preparation • Become familiar with suture combinations – Ties • Free tie • Tie on a passer – Reels – Swaged needles – Controlled release 66

Properties of Sutures • Physical characteristics – Size – Strength • Handling qualities – Pliability – Memory – Tissue drag – Elasticity 67

Properties of Sutures • Absorption – Resistance to digestion • Bioactivity – Effects on tissue • Composition – Origin of material 68

Properties of Sutures • Characteristics (structure) – Monofilament • Single fiber – Multifilament • Many fibers – Twisted • Multiple fibers twisted in the same direction – Braided • Multiple fibers intertwined 69

Properties of Sutures • Classification – Absorbable • Natural (biological) • Synthetic – Nonabsorbable • Natural (biological) • Synthetic 70

Properties of Sutures • Natural absorbable sutures – Surgical gut • Plain • Chromic 71

Properties of Sutures • Synthetic absorbable polymers – – – – Bondek Biosyn Caprosyn Dexon II Dexon S Maxon Monocryl PDS II Polyglycolic acid Polydioxanone Polyglactin 910 Polysorb Vicryl 72

Properties of Sutures • Nonabsorbable – Silk – Cotton – Nylon Polyester – Polypropylene – Stainless steel 73
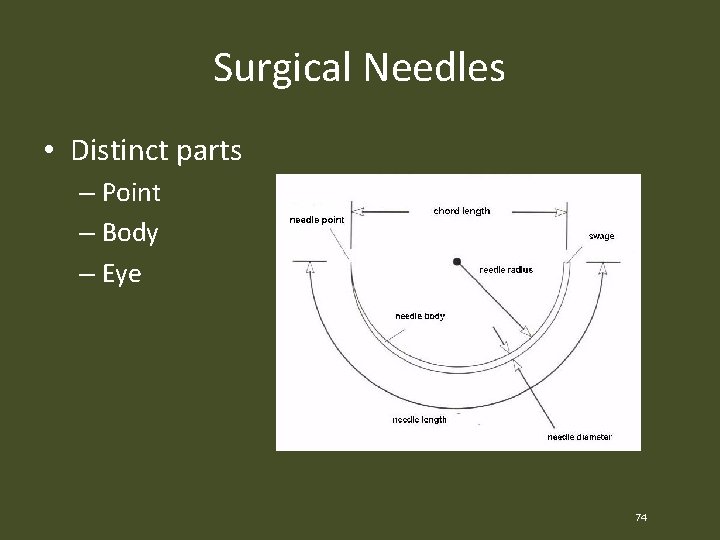
Surgical Needles • Distinct parts – Point – Body – Eye 74
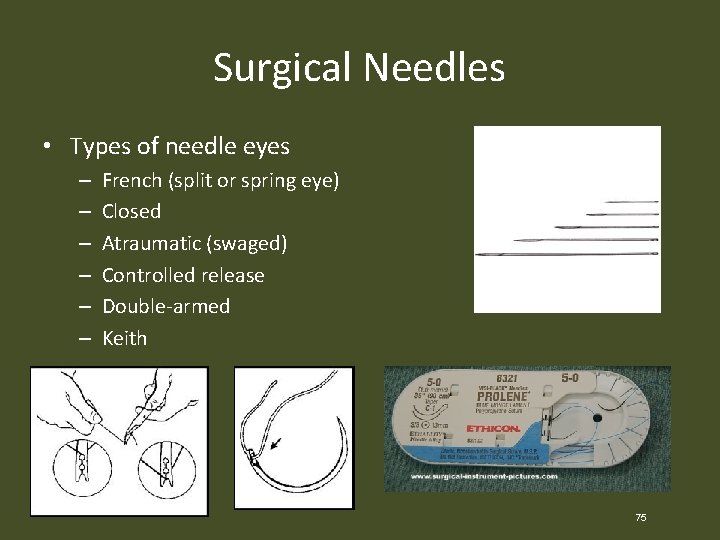
Surgical Needles • Types of needle eyes – – – French (split or spring eye) Closed Atraumatic (swaged) Controlled release Double-armed Keith 75

Surgical Needles • Size – Measured by diameter of the shaft – Measured by the dimension from tip to eye – GU-46 – V-20 – SH – TF – P 2 76
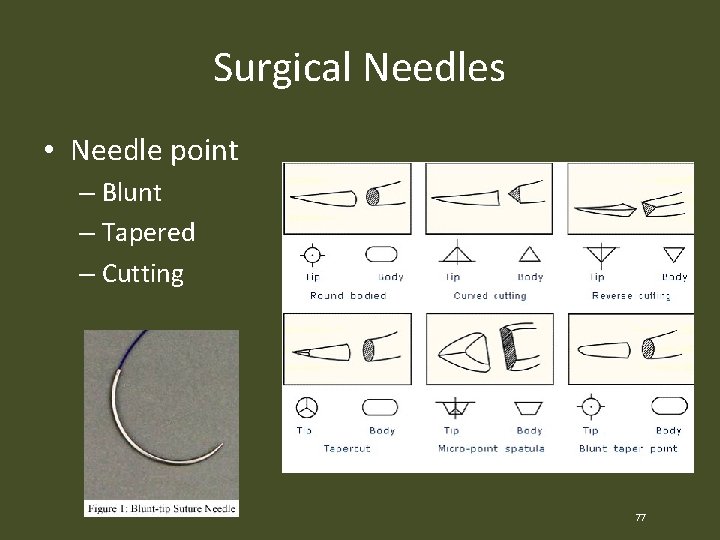
Surgical Needles • Needle point – Blunt – Tapered – Cutting 77

Surgical Needles • Reading a label – Name – Size – Color of suture – Type and size of needle – Lot number – Expiration date 78

Surgical Needles • Dispensing – Suture-needle combination – Multiple suture strands – Suture reel – Multiple suture needles – Double-arm suture – Controlled-release suture 79
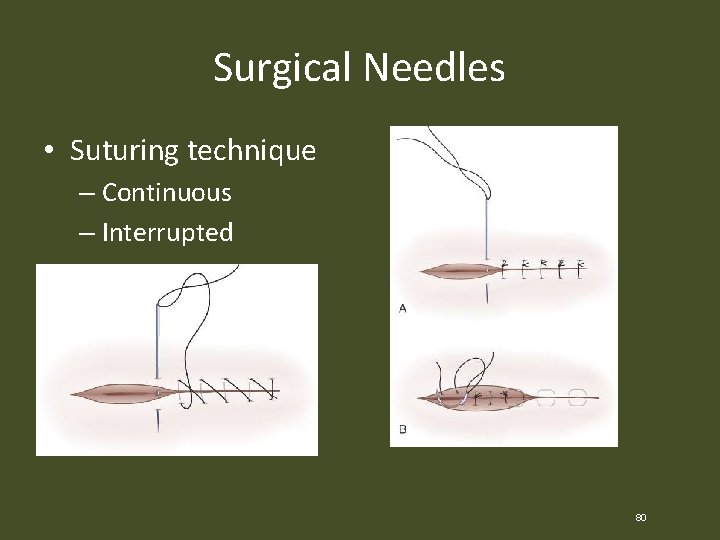
Surgical Needles • Suturing technique – Continuous – Interrupted 80
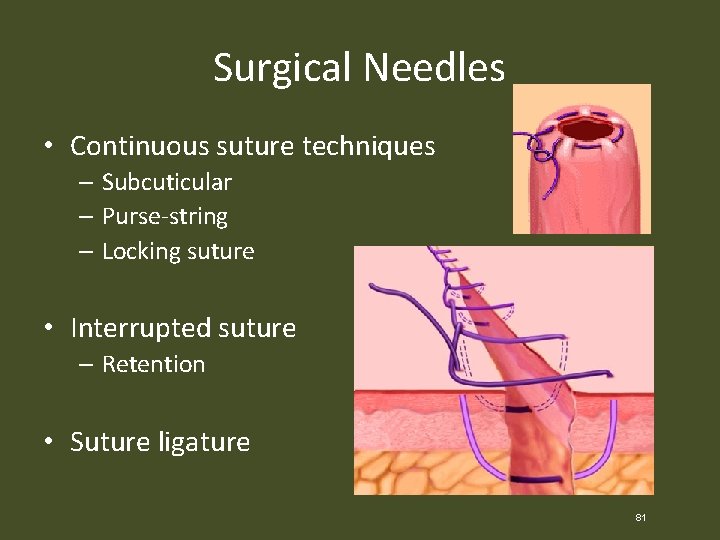
Surgical Needles • Continuous suture techniques – Subcuticular – Purse-string – Locking suture • Interrupted suture – Retention • Suture ligature 81
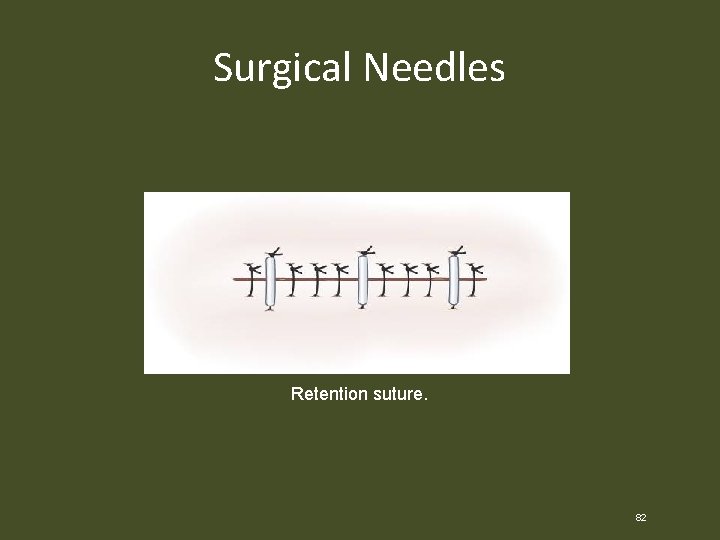
Surgical Needles Retention suture. 82

Surgical Needles • Suture Preparation – Efficiency in passing suture – Conservation use lowers cost – Use good technique to minimize waste – Increased risk of bloodborne contamination – Prevent loss of suture – Choose appropriately sized needle – Properly prepare suture 83

Surgical Needles • Suturing instruments – Needle holder – Tissue forceps • Smooth • Toothed • Vascular 84

Surgical Needles • Considerations for position of the needle – Right-handed – Left-handed – Surgeon is opposite you – Surgeon is next to you – Suture is loaded back-handed Elsevier items and derived items © 2010, 2007 by Saunders, an imprint of Elsevier Inc. 85
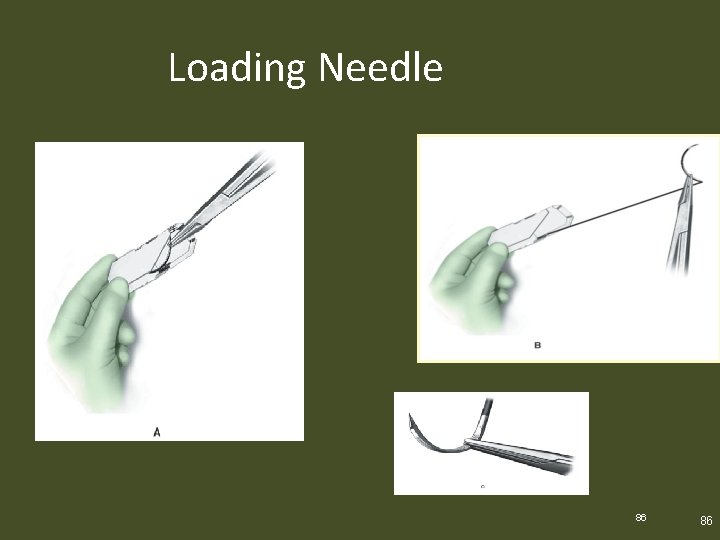
Loading Needle 86 86

Passing Suture 87 87

Surgical Needles • Multiple sutures – Keep suture pack organized – Pass on an exchange basis – Load needle before removal from pack – Use suture bag for suture packs – Avoid frustration: Try to keep pace with the surgeon 88
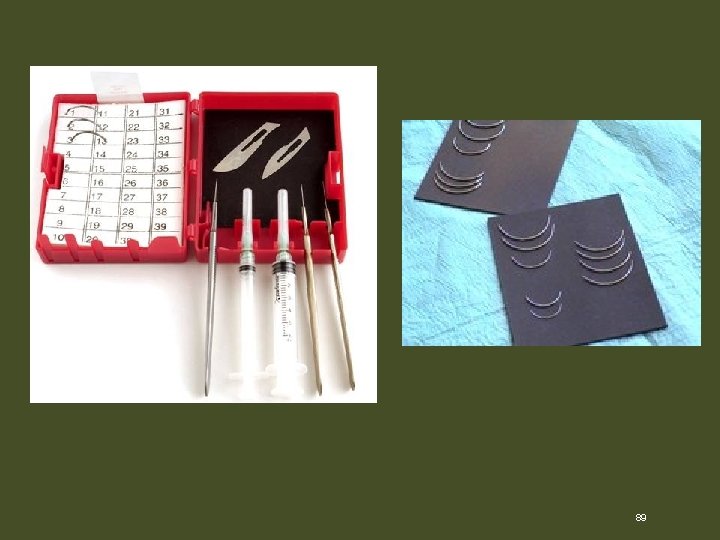
89
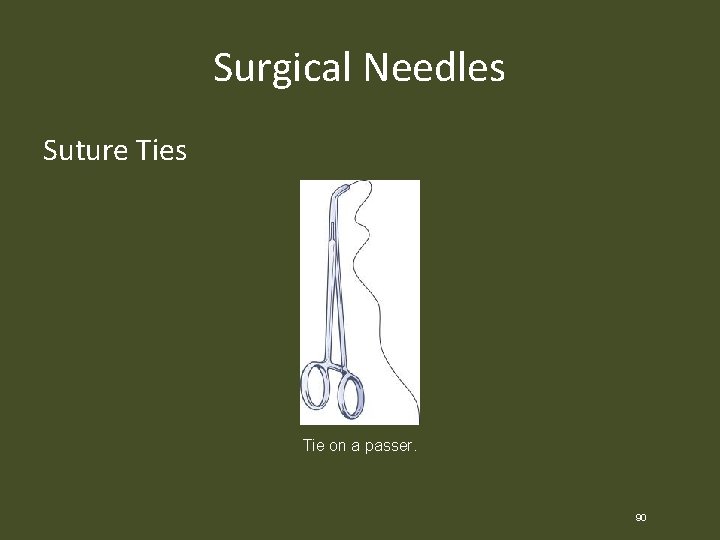
Surgical Needles Suture Ties Tie on a passer. 90
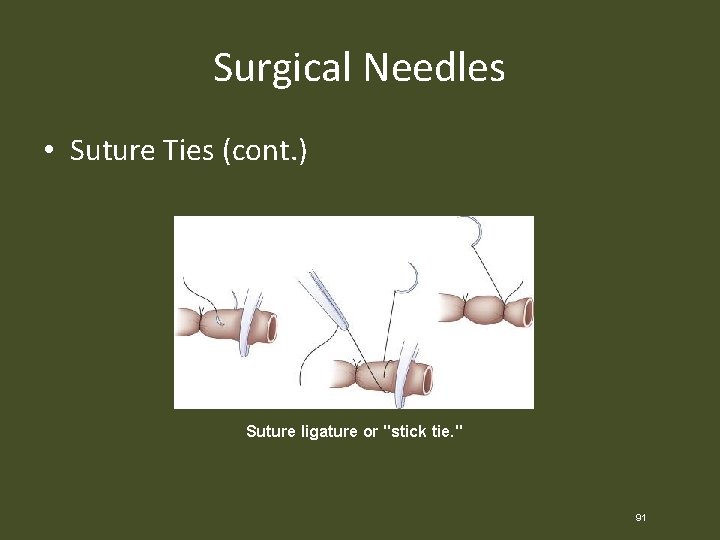
Surgical Needles • Suture Ties (cont. ) Suture ligature or "stick tie. " 91
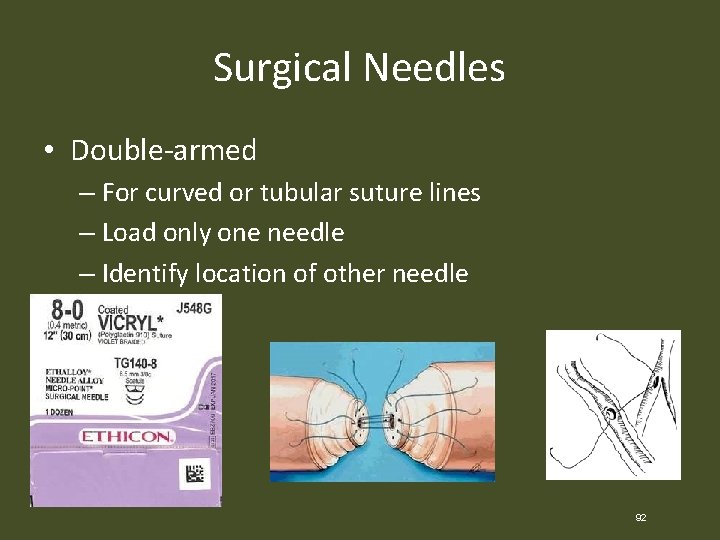
Surgical Needles • Double-armed – For curved or tubular suture lines – Load only one needle – Identify location of other needle 92

Surgical Needles • Cutting suture – Use sharp, straight Mayo scissors or suture scissors – Hold scissors correctly – Steady the scissors, turn to 45 -degree angle – Palm scissors when completing other task – Remove cut suture ends from the field 93
Surgical Stapling and Ligating Devices • Stapling advantages – Minimize tissue handling – Strong suture line – Nonreactive in the body – Noncrushing 94
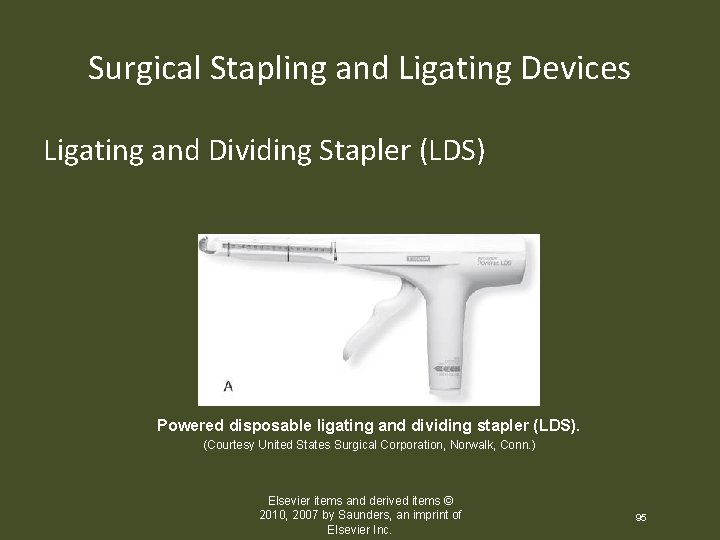
Surgical Stapling and Ligating Devices Ligating and Dividing Stapler (LDS) Powered disposable ligating and dividing stapler (LDS). (Courtesy United States Surgical Corporation, Norwalk, Conn. ) Elsevier items and derived items © 2010, 2007 by Saunders, an imprint of Elsevier Inc. 95
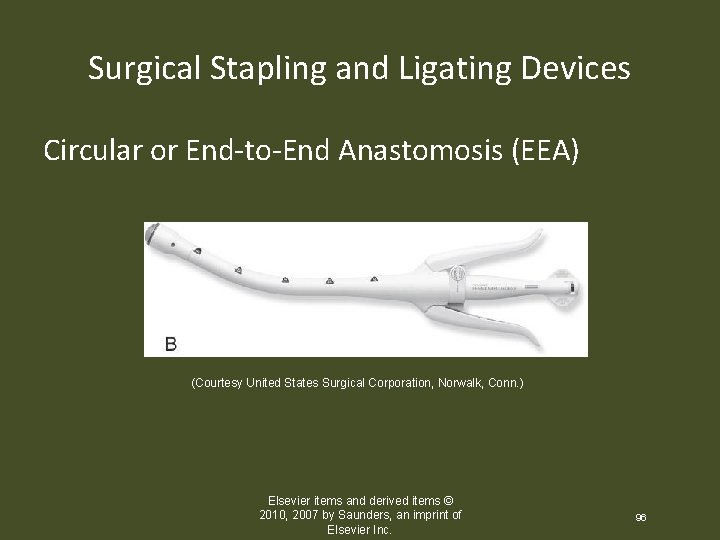
Surgical Stapling and Ligating Devices Circular or End-to-End Anastomosis (EEA) (Courtesy United States Surgical Corporation, Norwalk, Conn. ) Elsevier items and derived items © 2010, 2007 by Saunders, an imprint of Elsevier Inc. 96

Surgical Stapling and Ligating Devices Thoracoabdominal Stapler (TA) (Courtesy United States Surgical Corporation, Norwalk, Conn. ) Elsevier items and derived items © 2010, 2007 by Saunders, an imprint of Elsevier Inc. 97
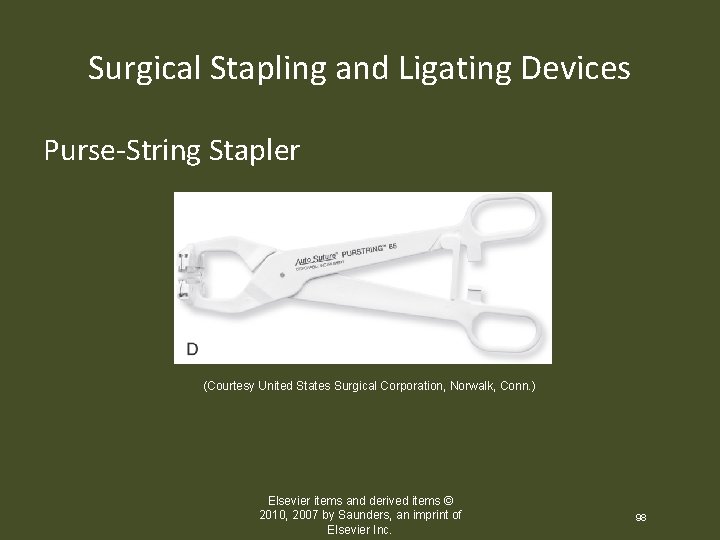
Surgical Stapling and Ligating Devices Purse-String Stapler (Courtesy United States Surgical Corporation, Norwalk, Conn. ) Elsevier items and derived items © 2010, 2007 by Saunders, an imprint of Elsevier Inc. 98
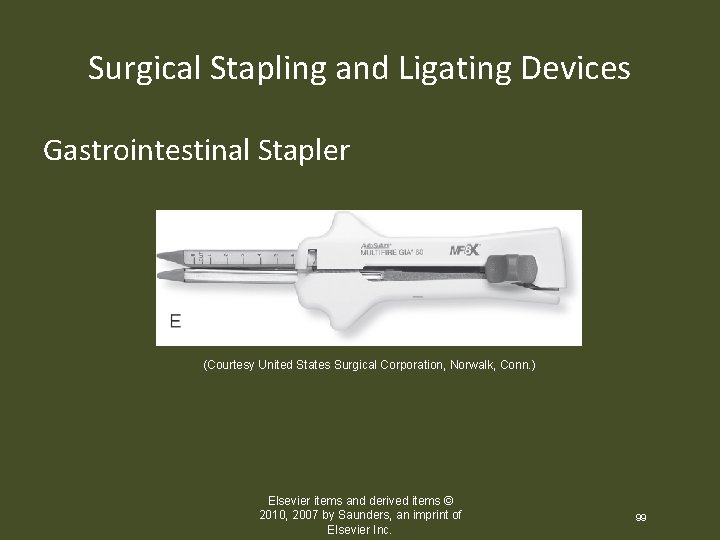
Surgical Stapling and Ligating Devices Gastrointestinal Stapler (Courtesy United States Surgical Corporation, Norwalk, Conn. ) Elsevier items and derived items © 2010, 2007 by Saunders, an imprint of Elsevier Inc. 99
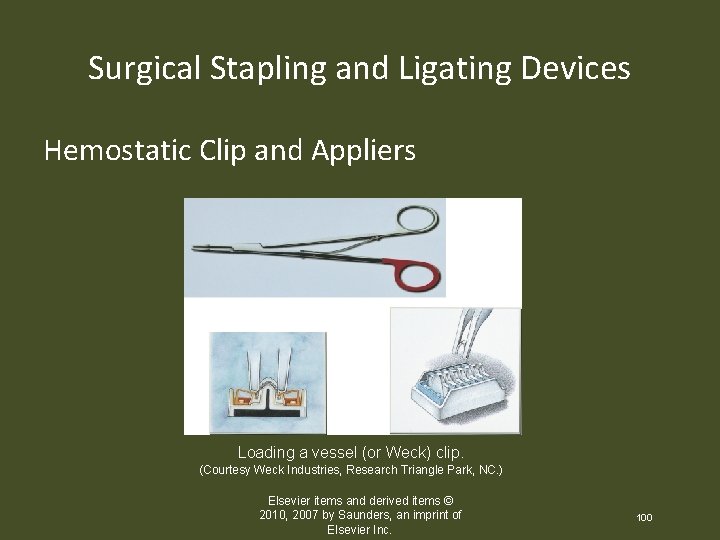
Surgical Stapling and Ligating Devices Hemostatic Clip and Appliers Loading a vessel (or Weck) clip. (Courtesy Weck Industries, Research Triangle Park, NC. ) Elsevier items and derived items © 2010, 2007 by Saunders, an imprint of Elsevier Inc. 100
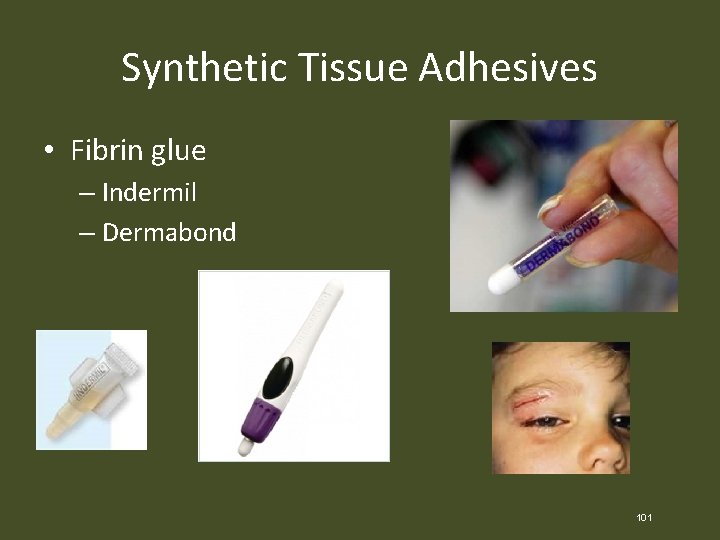
Synthetic Tissue Adhesives • Fibrin glue – Indermil – Dermabond 101

Tissue Implants • Terms – Allograft (same species) – Autograft (autologous) – Bovine graft – Skin Graft – Implant – Porcine graft – Xenograft (different species) – Wound cover – Bone Graft 102

Synthetic Implants • Types – Heart valves – Pacemakers – Defibrillators – Artificial joints 103

Synthetic Implants • Types – Metal – Methyl methacrylate – Resorbable implants – Polyethylene – Silicone – Woven synthetics 104
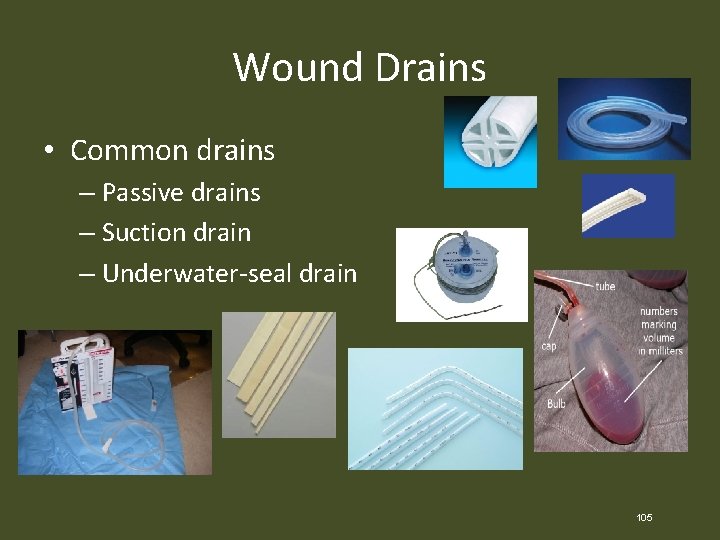
Wound Drains • Common drains – Passive drains – Suction drain – Underwater-seal drain 105
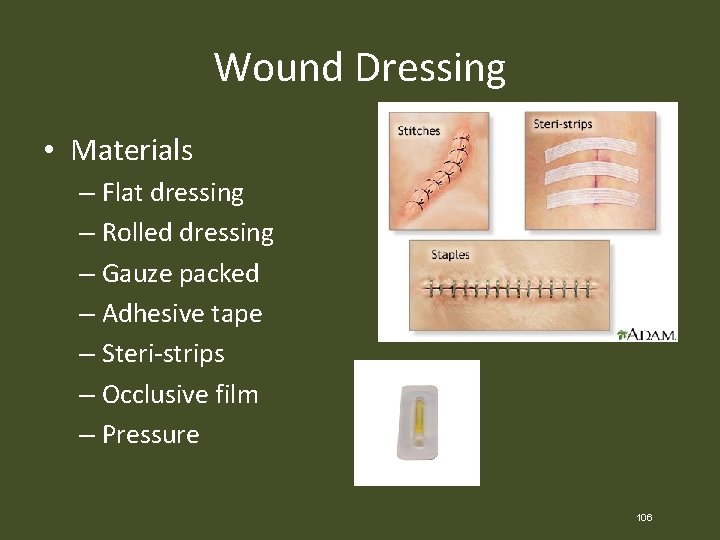
Wound Dressing • Materials – Flat dressing – Rolled dressing – Gauze packed – Adhesive tape – Steri-strips – Occlusive film – Pressure 106

http: //www. dressings. org/dressingsdatacards-by-alpha. html 107

108

Wound Classifications • Class I Clean: • Incision made under ideal conditions • No break in sterile technique during procedure • Primary Closure • No Wound Drain • No entry into aerodigestive or genitourinary tract • Class II Clean Contaminated • Primary Closure • Wound Drained • Minor break in sterile technique during procedure • Controlled entry to aerodigestive or genitourinary tract • Class III Contaminated • Open traumatic wound • Major break in sterile technique occurred • Acute inflammation present • Entry to aerodigestive tract or genitourinary tract with spillage • Class IV Dirty • Open traumatic wound • Microbial contamination prior to procedure • Perforated viscus 109

Wound Healing Categories – First intention (Primary Union) – Second intention (Granulation) • Fails to heal by primary union • Large wounds/infections • Necrotic tissue is debrided and sometimes left open – Third intention (Delayed Primary Closure) • Large wounds/infections • Necrotic tissue is debrided and purposely left open 110

Tissue Repair • Healing phases – Inflammatory or lag Phase • Within minutes lasts 3 -5 days • Heat, Redness, Swelling, Pain • Increased blood flow and platelet aggregation – Proliferative Phase • 3 -20 days • Fibroblasts multiply and bridge wound edges with collagen – Remodeling, Maturation, or Differentiation Phase • 14 days-1 year • Scar appears – Cicatrix – Keloid 111

Wound Healing • Conditions affecting wound healing – Immune system – Chronic disease – Nutritional status – Obesity – Age – Surgical technique – Infection Present – Wound Classification 112

Wound Healing • Complications in wound healing – Infection – Hematoma or serum accumulation – Dead space – Dehiscence – Evisceration – Tissue trauma – Adhesions 113
- Slides: 113