Substance Use Disorder Assessment Melissa Weimer DO MCR

Substance Use Disorder Assessment Melissa Weimer, DO, MCR OHSU Addiction Medicine Section Oregon Pain Guidance 6 th Annual Conference, May 4, 2017

Disclosures Dr. Weimer was a consultant to Indivior, for which she received honorarium. This was a onetime consultation to discuss how to stop taking medication they manufacture.
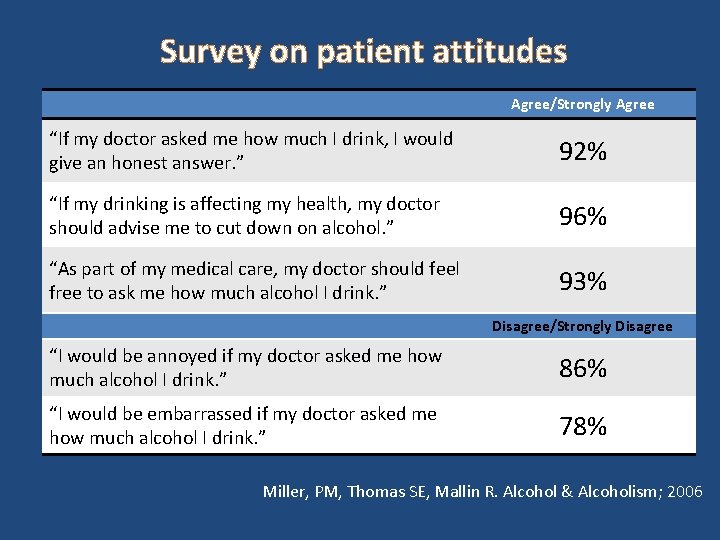
Survey on patient attitudes Agree/Strongly Agree “If my doctor asked me how much I drink, I would give an honest answer. ” 92% “If my drinking is affecting my health, my doctor should advise me to cut down on alcohol. ” 96% “As part of my medical care, my doctor should feel free to ask me how much alcohol I drink. ” 93% Disagree/Strongly Disagree “I would be annoyed if my doctor asked me how much alcohol I drink. ” 86% “I would be embarrassed if my doctor asked me how much alcohol I drink. ” 78% Miller, PM, Thomas SE, Mallin R. Alcohol & Alcoholism; 2006

SCREENING QUESTIONS

Who should you screen? • USPSTF recommends (B) screening ADULTS – The optimal interval for screening and intervention is unknown. • American College of Surgeons requires screening of all level I and level II trauma patients for alcohol misuse. Ann Intern Med 2004; 140: 555 -557. Committee on Trauma, American College of Surgeons, 2006.

Who should you screen? • USPSTF states there is insufficient evidence to screen Adolescents • American Academy of Pediatricians – Recommend that doctors screen all of their young patients for alcohol use starting in middle school. Ann Intern Med 2004; 140: 555 -557. Pediatrics Vol. 125 No. 5 May 2010, pp. 1078 -1087

Four validated screening tools • CAGE – Higher sensitivity for identifying alcohol dependence in African Americans compared to Caucasians – May miss risky drinking • AUDIT-C/AUDIT – Identifies alcohol dependence at roughly the same rate of sensitivity across races. – Has been validated in six countries with disparate cultures, although not across the various cultures in the United States. • CRAFFT - Adolescents • DAST - Drugs Cherpitel and Clark, 1995. Babor, et al. 1992
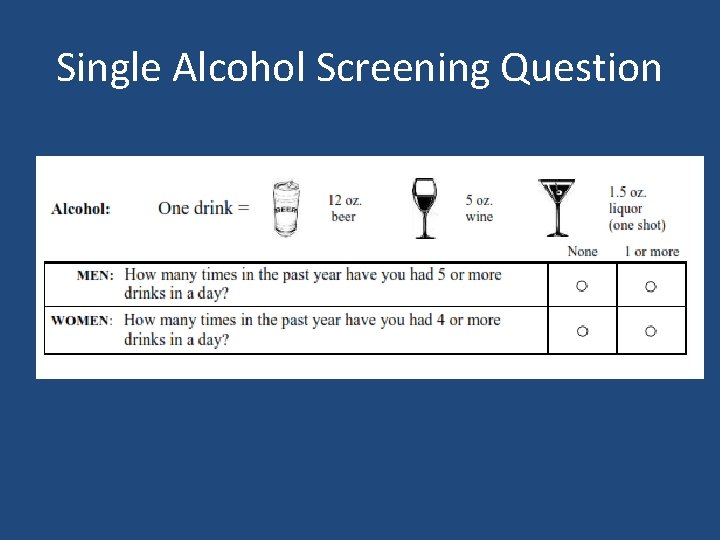

Single Alcohol Screening Question
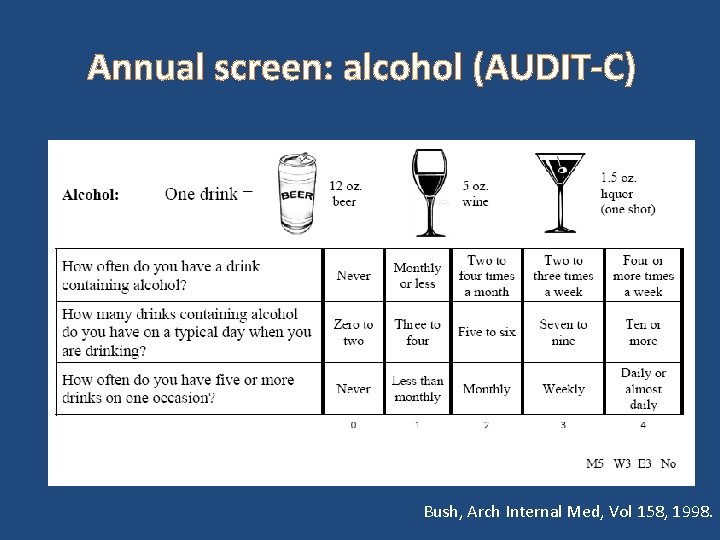
Annual screen: alcohol (AUDIT-C) Bush, Arch Internal Med, Vol 158, 1998.

Standard drinks One drink = . 6 oz of alcohol Volume Standard drinks 5 oz 1 Wine 750 -m. L bottle 5 (12% ABV) 1. 5 liter bottle 9 5 liter box 30 1 mixed drink (1. 5 oz) 1 1 pint (16 oz. ) 11 One fifth (25 oz. ) 17 1. 75 liters (59 oz) 39 Liquor (80 proof, 40% ABV)
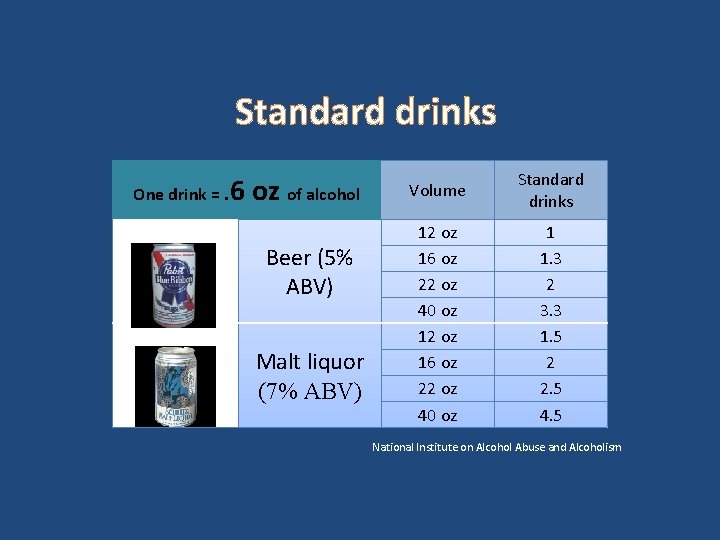
Standard drinks One drink =. 6 oz of alcohol Beer (5% ABV) Malt liquor (7% ABV) Volume Standard drinks 12 oz 16 oz 22 oz 40 oz 1 1. 3 2 3. 3 1. 5 2 2. 5 4. 5 National Institute on Alcohol Abuse and Alcoholism
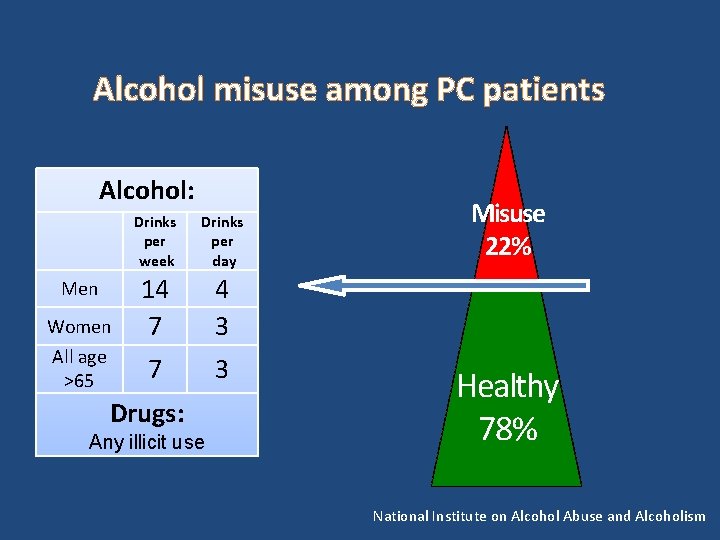
Alcohol misuse among PC patients Alcohol: Drinks per week Drinks per day Women 14 7 4 3 All age >65 7 3 Men Drugs: Any illicit use Misuse 22% Healthy 78% National Institute on Alcohol Abuse and Alcoholism

A Single Question to Detect Drug Use and Drug Use Disorders • “How many times in the past year have you used an illegal drug OR used a prescription medication for nonmedical reasons? ” • 85% sensitive and 96% specific for current drug use • 100% sensitive and 74% specific for a drug use disorder (abuse or dependence). Smith PC, Arch Intern Med. 2010; 170(13): 1155– 1160.

EVALUATION AFTER POSITIVE SCREENING

The “key” to a good history • • • Ask for permission to have the conversation Emphasize your goal – “to help you” Emphasize the protection of the information Address head on Normalize Withhold judgment

A basic substance abuse history • Which substances? “Drug of choice”? • Length of use? • How much? • How often? • What route? • What consequences? • What physical symptoms? • Their experience attempting to quit • Experience with treatment(s), if any
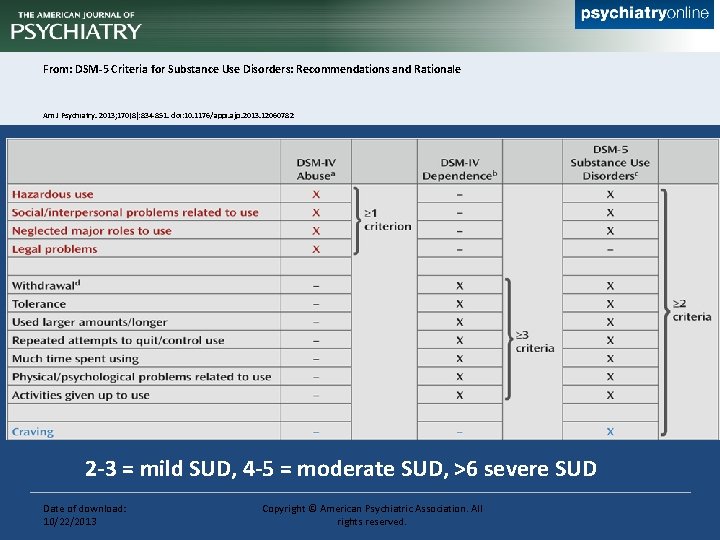
From: DSM-5 Criteria for Substance Use Disorders: Recommendations and Rationale Am J Psychiatry. 2013; 170(8): 834 -851. doi: 10. 1176/appi. ajp. 2013. 12060782 2 -3 = mild SUD, 4 -5 = moderate SUD, >6 severe SUD Date of download: 10/22/2013 Copyright © American Psychiatric Association. All rights reserved.

DSM-V criteria 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. Unable to fulfill major role obligations Social or interpersonal problems due to use Use in hazardous situations Tolerance* Withdrawal/physical dependence* Taken in larger amounts or over longer period than wanted Unsuccessful efforts to cut down or control use Great deal of time spent to obtain substance Important activities given up or reduced Continued use despite harm (physical and psychological) Craving *If opioids are prescribed and taken as prescribed, these criterion do not apply.

Addiction in clinical practice • The 4 C’s – Impaired control over the use of the drug – Compulsive use – Continued use despite harms – Craving

COMPLEX PAIN AND OPIOID USE DISORDER ASSESSMENT
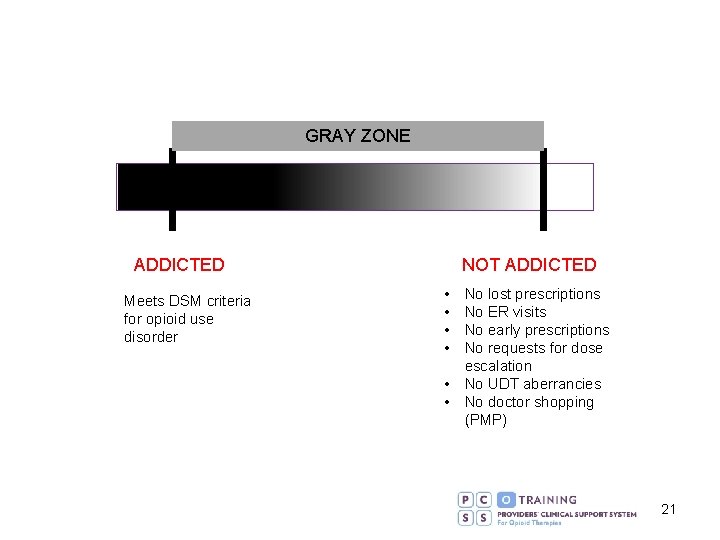
GRAY ZONE ADDICTED Meets DSM criteria for opioid use disorder NOT ADDICTED • • No lost prescriptions No ER visits No early prescriptions No requests for dose escalation • No UDT aberrancies • No doctor shopping (PMP) 21

Continuum of Problematic Opioid Use Mild indiscretion Repeated misuse Opioid use disorder Photo from http: //mediad. publicbroadcasting. net/p/wnpr/files/styles/related/public/201603/Pill. Bottle. jpg Severe Opioid Use Disorder (i. e. addiction) 22
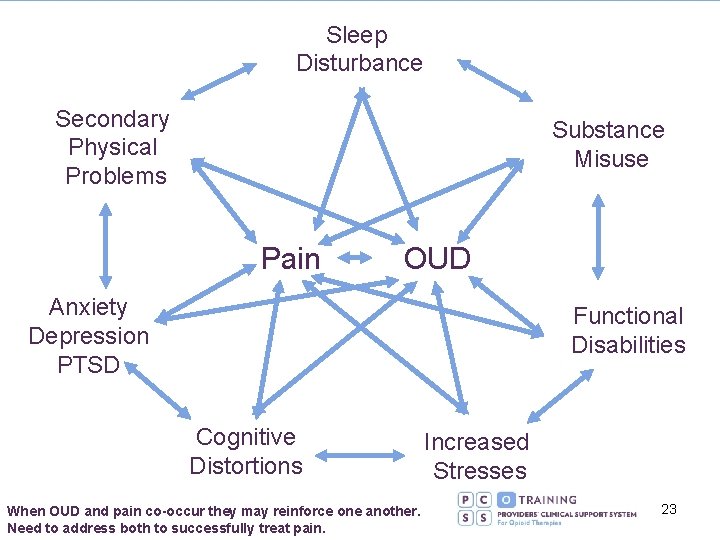
Sleep Disturbance Secondary Physical Problems Substance Misuse Pain OUD Anxiety Depression PTSD Functional Disabilities Cognitive Distortions When OUD and pain co-occur they may reinforce one another. Need to address both to successfully treat pain. Increased Stresses 23

Validated Questionnaires for Opioid Use Disorder Risk ORT SOAPP STAR SISAP PDUQ Opioid Risk Tool Screener & Opioid Assessment for Patients with Pain Screening Tool for Addiction Risk Screening Instrument for Substance Abuse Potential Prescription Drug Use Questionnaire No “Gold Standard”, Not diagnostic All lack rigorous testing in primary care Moore TM, et al. Pain Med. 2009 Nov; 10(8): 1426 -33. populations
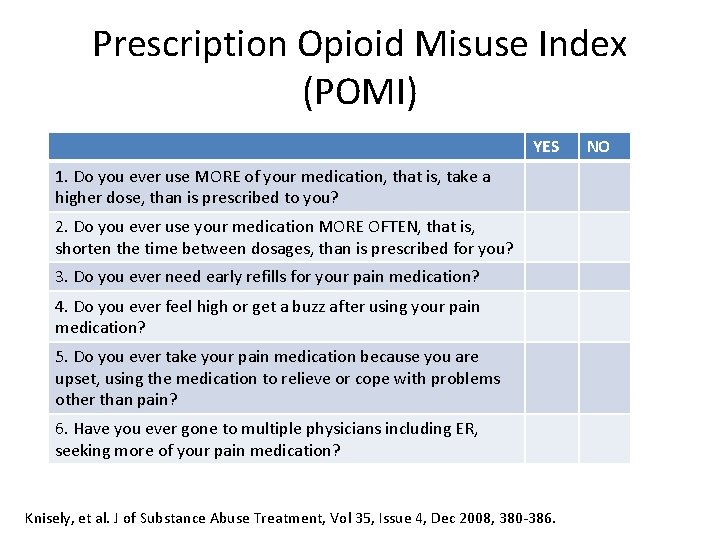
Prescription Opioid Misuse Index (POMI) YES 1. Do you ever use MORE of your medication, that is, take a higher dose, than is prescribed to you? 2. Do you ever use your medication MORE OFTEN, that is, shorten the time between dosages, than is prescribed for you? 3. Do you ever need early refills for your pain medication? 4. Do you ever feel high or get a buzz after using your pain medication? 5. Do you ever take your pain medication because you are upset, using the medication to relieve or cope with problems other than pain? 6. Have you ever gone to multiple physicians including ER, seeking more of your pain medication? Knisely, et al. J of Substance Abuse Treatment, Vol 35, Issue 4, Dec 2008, 380 -386. NO
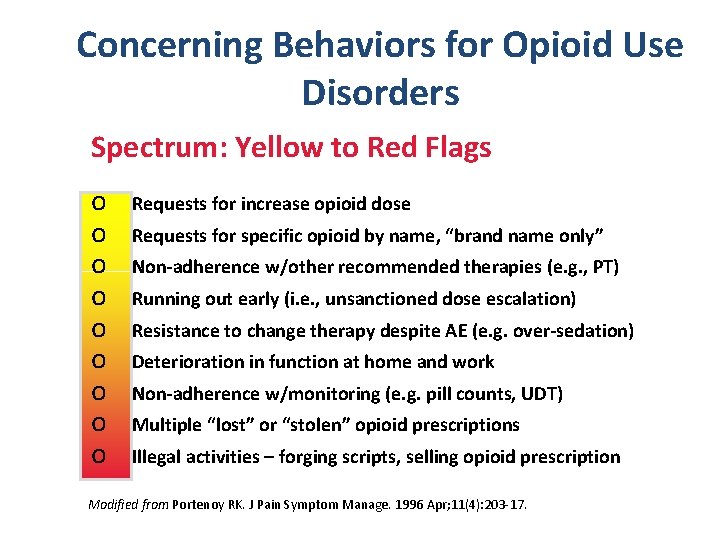

Concerning Behaviors for Opioid Use Disorders Spectrum: Yellow to Red Flags o o o o o Requests for increase opioid dose Requests for specific opioid by name, “brand name only” Non-adherence w/other recommended therapies (e. g. , PT) Running out early (i. e. , unsanctioned dose escalation) Resistance to change therapy despite AE (e. g. over-sedation) Deterioration in function at home and work Non-adherence w/monitoring (e. g. pill counts, UDT) Multiple “lost” or “stolen” opioid prescriptions Illegal activities – forging scripts, selling opioid prescription Modified from Portenoy RK. J Pain Symptom Manage. 1996 Apr; 11(4): 203 -17.

Objective Measures to detect Opioid Use Disorders • Random Urine Drug Testing – Evidence of therapeutic adherence – Evidence of use or non-use of illicit drugs • Prescription Drug Monitoring data • Pill counts • Review of past medical records Heit HA and Gourlay DL. J Pain Symptom Manage Mar; 27(3): 260 -7. Christo PJ et al. Pain Physician. 2011 Mar-Apr; 14(2): 123 -43.

Diagnosis • There is not one test or questionnaire that can confirm prescription opioid use disorder. • The initial PCP evaluation will provide the basis for a risk/benefit determination • This initial evaluation will place a focus not only on concerning behavior, but also on pain and pain care – You can have pain and OUD – Treating pain with opioids in the setting of OUD is risky – Treating OUD without treating pain is also not likely to be effective • Based on initial evaluation, consider referral for diagnosis of an OUD if you do not feel comfortable making it • Ultimately, diagnosis made by DSM V criteria

Questions? weimerm@ohsu. edu
- Slides: 29