Substance Misuse Prevention Priority Setting Connecticut 2020 SEOW

Substance Misuse Prevention Priority Setting: Connecticut, 2020 SEOW Meeting April 29, 2020 Jane A. Ungemack, Dr. PH DMHAS Center for Prevention Evaluation and Statistics (CPES) at UConn Health 1

The Role of the SEOW • Identify and collect data that can be used to assess priority needs for services and evaluate the impact of policies and programs; • Systematically review and analyze data related to behavioral health problems; • Make recommendations regarding state priorities for substance use prevention and mental health promotion.

The Priority Setting Process • Systematically review and analyze data related to substance use in Connecticut. • Consider: • Magnitude, severity, and impact; • Changeability and Connecticut’s readiness to affect; • Subpopulations at risk and health disparities; • Gaps in data. • Make recommendations regarding state priorities for substance use prevention.
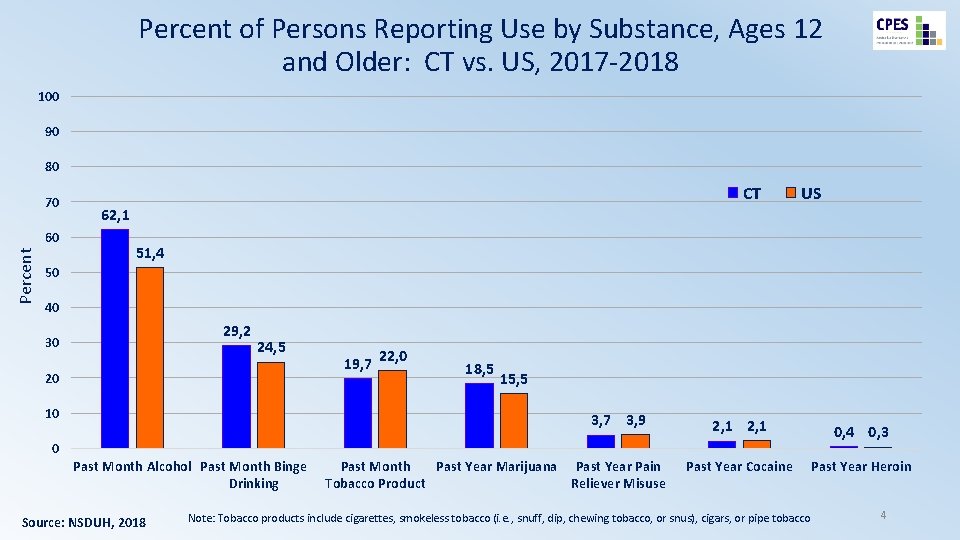
Percent of Persons Reporting Use by Substance, Ages 12 and Older: CT vs. US, 2017 -2018 100 90 80 70 Percent 60 CT US 62, 1 51, 4 50 40 29, 2 30 24, 5 20 10 19, 7 22, 0 18, 5 15, 5 3, 7 3, 9 2, 1 0, 4 0, 3 Past Year Cocaine Past Year Heroin 0 Past Month Alcohol Past Month Binge Drinking Source: NSDUH, 2018 Past Month Past Year Marijuana Past Year Pain Tobacco Product Reliever Misuse Note: Tobacco products include cigarettes, smokeless tobacco (i. e. , snuff, dip, chewing tobacco, or snus), cigars, or pipe tobacco 4

Alcohol 5
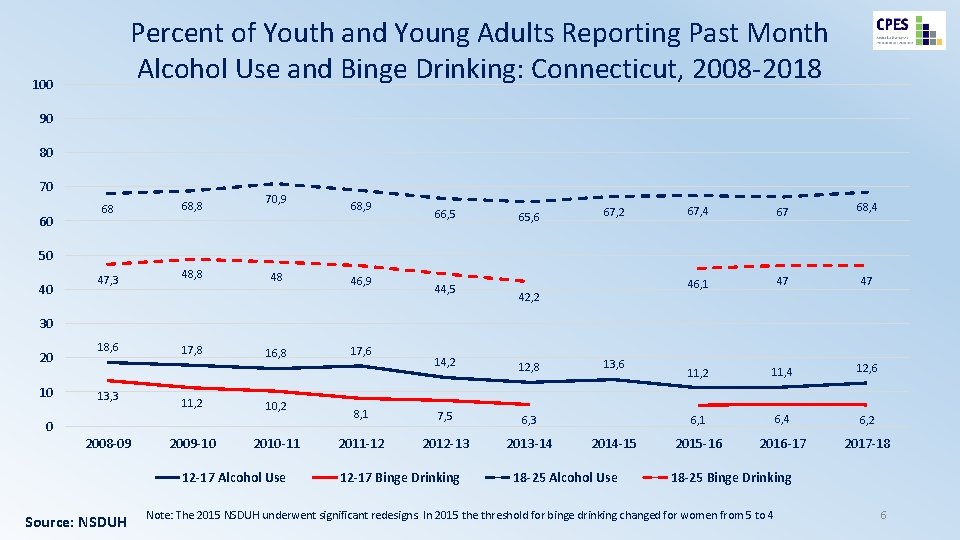
Percent of Youth and Young Adults Reporting Past Month Alcohol Use and Binge Drinking: Connecticut, 2008 -2018 100 90 80 70 60 68 68, 8 47, 3 48, 8 70, 9 68, 9 66, 5 65, 6 67, 2 67, 4 67 68, 4 46, 1 47 47 11, 2 11, 4 12, 6 6, 1 6, 4 6, 2 2015 -16 2016 -17 2017 -18 50 40 48 46, 9 44, 5 42, 2 30 20 10 18, 6 13, 3 17, 8 11, 2 16, 8 10, 2 0 2008 -09 2009 -10 2010 -11 12 -17 Alcohol Use Source: NSDUH 17, 6 14, 2 12, 8 8, 1 7, 5 6, 3 2011 -12 2012 -13 2013 -14 12 -17 Binge Drinking 13, 6 2014 -15 18 -25 Alcohol Use 18 -25 Binge Drinking Note: The 2015 NSDUH underwent significant redesigns. In 2015 the threshold for binge drinking changed for women from 5 to 4 6
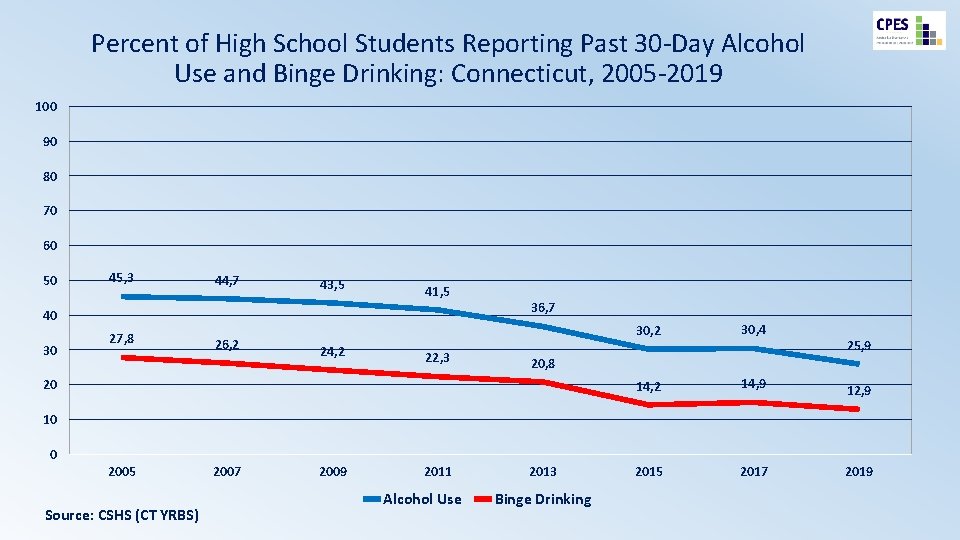
Percent of High School Students Reporting Past 30 -Day Alcohol Use and Binge Drinking: Connecticut, 2005 -2019 100 90 80 70 60 50 45, 3 44, 7 43, 5 41, 5 40 30 27, 8 26, 2 24, 2 22, 3 36, 7 30, 2 30, 4 14, 2 14, 9 12, 9 2015 2017 2019 25, 9 20, 8 20 10 0 2005 Source: CSHS (CT YRBS) 2007 2009 2011 Alcohol Use 2013 Binge Drinking
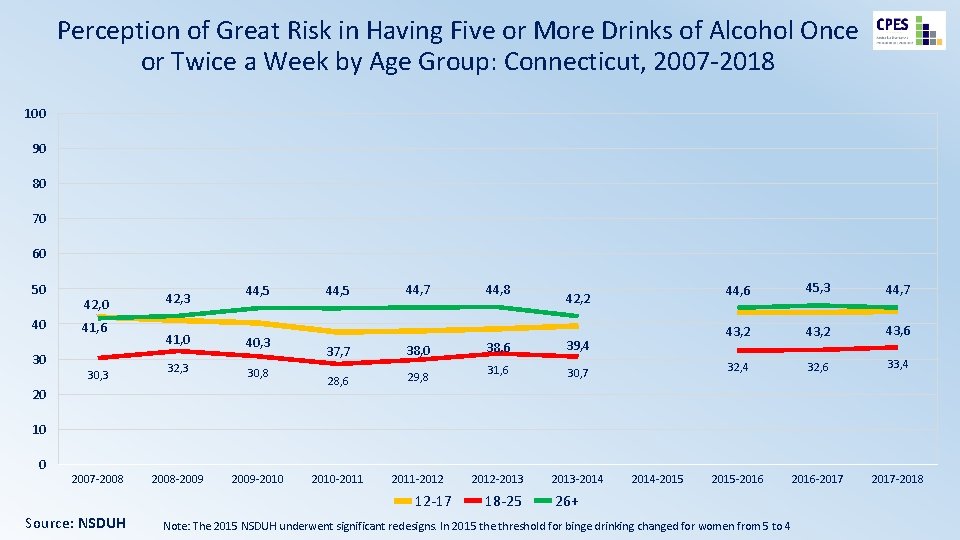
Perception of Great Risk in Having Five or More Drinks of Alcohol Once or Twice a Week by Age Group: Connecticut, 2007 -2018 100 90 80 70 60 50 40 30 42, 0 41, 6 30, 3 42, 3 44, 5 41, 0 40, 3 32, 3 30, 8 2008 -2009 -2010 20 44, 5 44, 7 37, 7 38, 0 28, 6 29, 8 2010 -2011 -2012 44, 8 42, 2 38, 6 39, 4 31, 6 30, 7 2012 -2013 -2014 44, 6 45, 3 44, 7 43, 2 43, 6 32, 4 32, 6 33, 4 2015 -2016 -2017 -2018 10 0 2007 -2008 12 -17 Source: NSDUH 18 -25 2014 -2015 26+ Note: The 2015 NSDUH underwent significant redesigns. In 2015 the threshold for binge drinking changed for women from 5 to 4

Alcohol: Risk and Impact At-risk Populations • Males, although women’s alcohol use and binge drinking has been increasing; • Individuals with serious mental illness; • Native Americans; • Hispanics and Blacks report higher rates of binge drinking; • Hispanics are overrepresented among impaired drivers and DUI fatalities; • Males and whites are overrepresented in substance abuse treatment in Connecticut. Effects and Impacts • Health problems, such as liver cirrhosis, pancreatitis, various cancers, cardiomyopathy, stroke and respiratory infections; • Psychological problems; • Increased risk of motor vehicle injuries, falls, and interpersonal violence; • Drinking during pregnancy can lead to Fetal Alcohol Spectrum Disorders; • Unemployment, disrupted family life, homelessness. 9

Alcohol: Youth Risk and Impact Youth Risk Factors Effects and Impacts • Academic and/or other behavioral health problems in school; • Alcohol-using peers; • Anxiety or depression; • Lack of parental supervision; • Poor parent-child communication; • Parental modeling of alcohol use; • Social norms that encourage or tolerate underage drinking; • Child abuse or neglect. • Impaired judgment, reduced reaction time, slurred speech, and loss of balance and motor skills; • Damage to the developing brain; • Alcohol poisoning; • Increases in risky behavior, such as impaired driving; • Negative impacts on problemsolving skills and school performance; • Increased risk for adult alcohol or drug use disorder. 10

Tobacco and Electronic Nicotine Delivery Systems (ENDS) 11
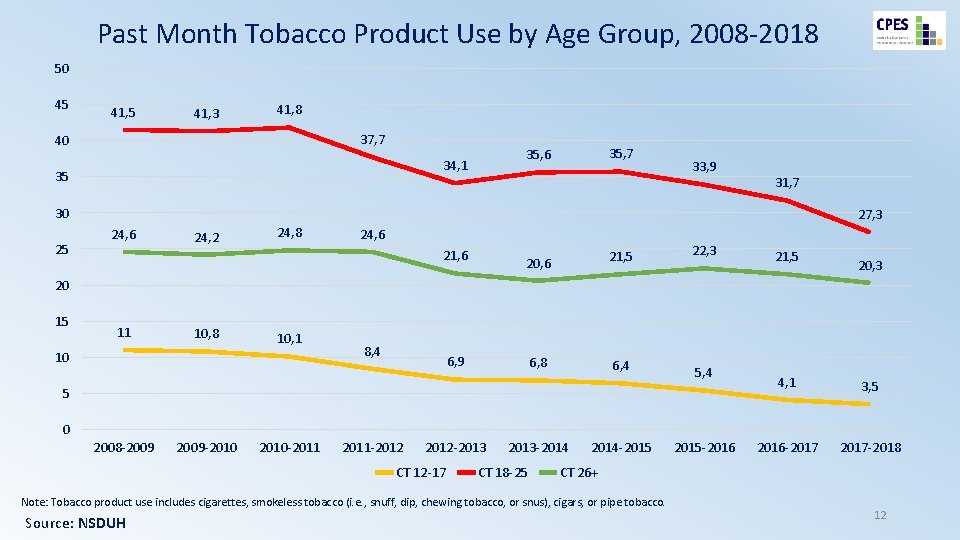
Past Month Tobacco Product Use by Age Group, 2008 -2018 50 45 41, 3 41, 8 37, 7 40 35 35, 7 35, 6 34, 1 33, 9 31, 7 30 25 27, 3 24, 6 24, 2 24, 8 24, 6 21, 6 20, 6 21, 5 6, 8 6, 4 22, 3 21, 5 20, 3 20 15 11 10, 8 10, 1 10 8, 4 6, 9 5, 4 5 4, 1 3, 5 2016 -2017 -2018 0 2008 -2009 -2010 -2011 -2012 -2013 CT 12 -17 2013 -2014 CT 18 -25 2014 -2015 CT 26+ Note: Tobacco product use includes cigarettes, smokeless tobacco (i. e. , snuff, dip, chewing tobacco, or snus), cigars, or pipe tobacco. Source: NSDUH 2015 -2016 12
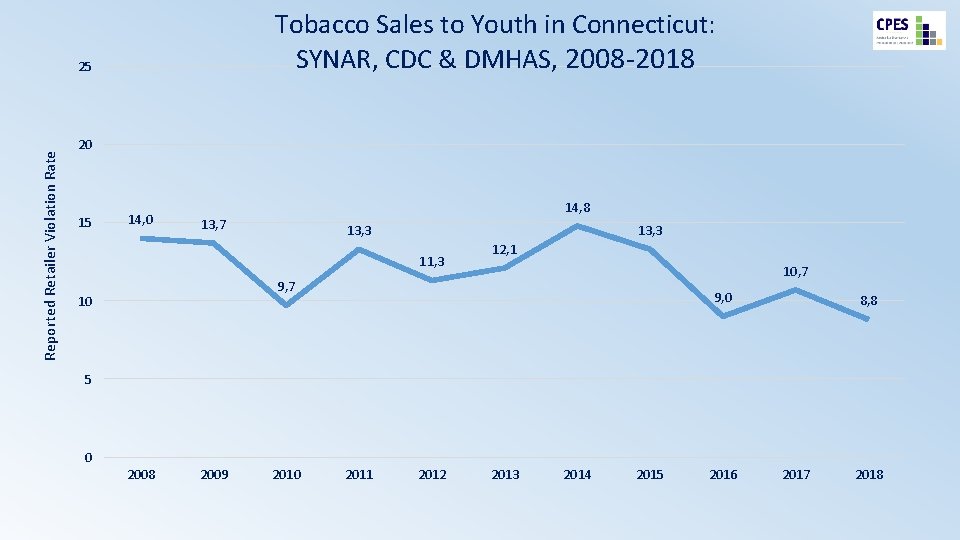
Tobacco Sales to Youth in Connecticut: SYNAR, CDC & DMHAS, 2008 -2018 Reported Retailer Violation Rate 25 20 15 14, 0 14, 8 13, 7 13, 3 11, 3 12, 1 10, 7 9, 7 10 9, 0 8, 8 5 0 2008 2009 2010 2011 2012 2013 2014 2015 2016 2017 2018
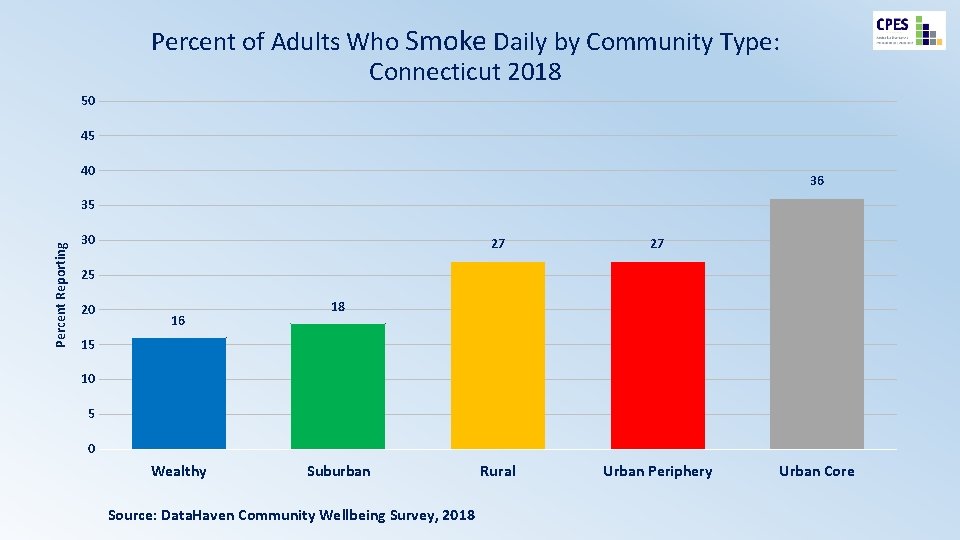
Percent of Adults Who Smoke Daily by Community Type: Connecticut 2018 50 45 40 36 Percent Reporting 35 30 27 27 Rural Urban Periphery 25 20 16 18 15 10 5 0 Wealthy Suburban Source: Data. Haven Community Wellbeing Survey, 2018 Urban Core
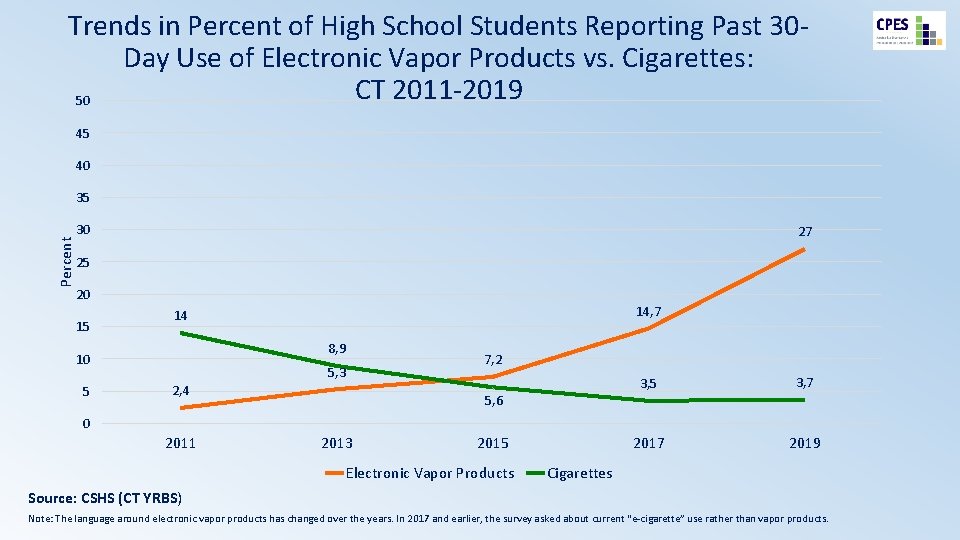
Trends in Percent of High School Students Reporting Past 30 Day Use of Electronic Vapor Products vs. Cigarettes: CT 2011 -2019 50 45 40 Percent 35 30 27 25 20 15 8, 9 10 5 14, 7 14 7, 2 5, 3 2, 4 5, 6 3, 5 3, 7 2019 0 2011 2013 2015 Electronic Vapor Products Cigarettes Source: CSHS (CT YRBS) Note: The language around electronic vapor products has changed over the years. In 2017 and earlier, the survey asked about current “e-cigarette” use rather than vapor products.
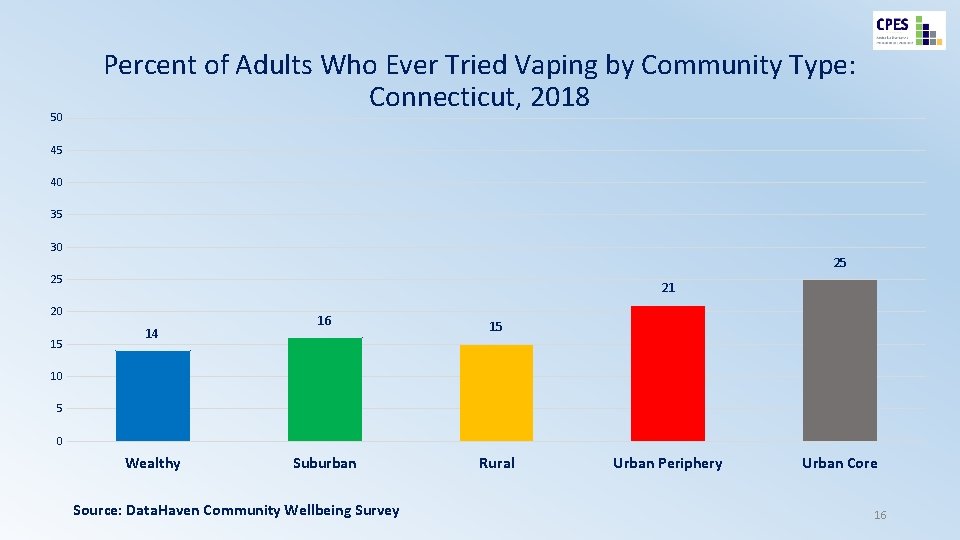
50 Percent of Adults Who Ever Tried Vaping by Community Type: Connecticut, 2018 45 40 35 30 25 25 21 20 15 14 16 15 Suburban Rural 10 5 0 Wealthy Source: Data. Haven Community Wellbeing Survey Urban Periphery Urban Core 16

ENDS: Risk and Impact At-risk Populations Youth and young adults; Males; Hispanics; Current smokers; Those living in urban communities; Adults from households earning less than $35, 000; • Adults with disabilities; • Those with a high school diploma or less; • Adults without health insurance. • • • Effects and Impacts • Increased risk of tobacco and cannabis use disorders later in life; • Nicotine can cause harm to the parts of the adolescent brain that control attention, learning, mood, and impulse control; • Lung injury and disease; • Cancer. 17

Marijuana 18
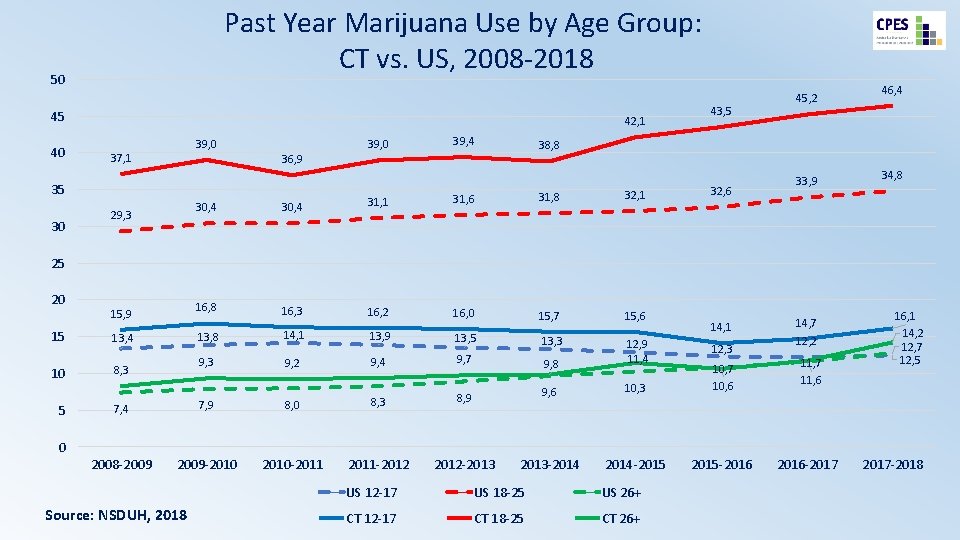
Past Year Marijuana Use by Age Group: CT vs. US, 2008 -2018 50 45 40 42, 1 39, 0 37, 1 39, 0 29, 3 30, 4 31, 1 16, 8 16, 3 16, 2 46, 4 38, 8 36, 9 35 30 39, 4 43, 5 45, 2 31, 6 31, 8 32, 1 16, 0 15, 7 15, 6 32, 6 33, 9 34, 8 25 20 15, 9 15 13, 4 10 8, 3 5 14, 1 13, 8 14, 1 13, 9 13, 5 13, 3 9, 2 9, 4 9, 7 9, 8 12, 9 11, 4 9, 6 10, 3 10, 7 10, 6 2013 -2014 -2015 -2016 7, 4 7, 9 8, 0 8, 3 8, 9 2008 -2009 -2010 -2011 -2012 -2013 12, 3 14, 7 12, 2 11, 7 11, 6 16, 1 14, 2 12, 7 12, 5 0 Source: NSDUH, 2018 US 12 -17 US 18 -25 US 26+ CT 12 -17 CT 18 -25 CT 26+ 2016 -2017 -2018
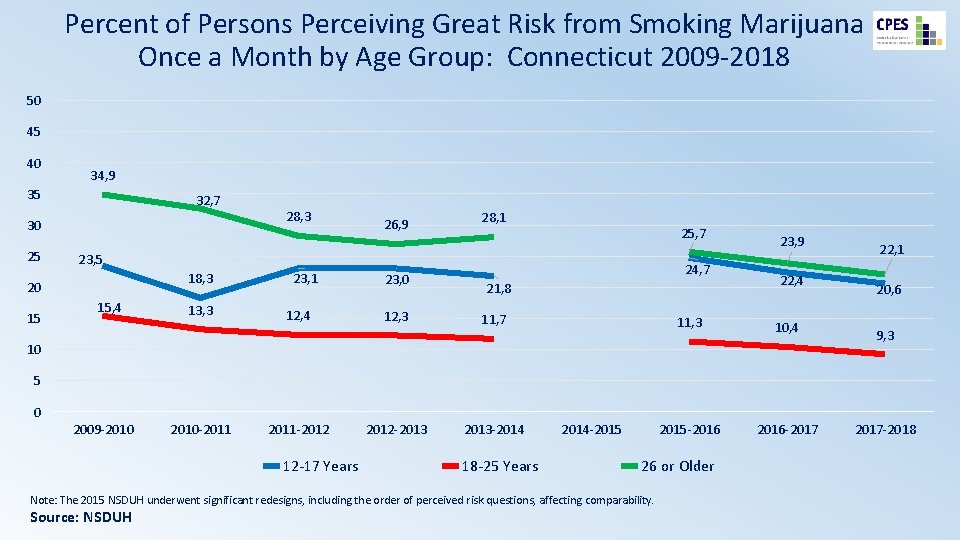
Percent of Persons Perceiving Great Risk from Smoking Marijuana Once a Month by Age Group: Connecticut 2009 -2018 50 45 40 34, 9 35 32, 7 30 25 26, 9 28, 1 25, 7 23, 5 18, 3 20 15 28, 3 15, 4 13, 3 23, 1 12, 4 23, 0 12, 3 24, 7 21, 8 11, 7 23, 9 22, 4 11, 3 10, 4 2015 -2016 -2017 10 22, 1 20, 6 9, 3 5 0 2009 -2010 -2011 -2012 12 -17 Years 2012 -2013 -2014 18 -25 Years 2014 -2015 26 or Older Note: The 2015 NSDUH underwent significant redesigns, including the order of perceived risk questions, affecting comparability. Source: NSDUH 2017 -2018

Marijuana: Risk and Impact Risk Factors • Availability of marijuana; • Favorable parental attitudes towards marijuana; • Academic failure; • Peers who use marijuana; • Low peer disapproval of marijuana use; • Prior use of alcohol/tobacco; • Anxiety and depression; • Sensation-seeking behavior and impulsivity; • Child abuse/trauma. Effects and Impacts • Impaired learning and coordination; • Sleep problems; • Increased risk of use of other illicit drugs; • Potential for addiction to marijuana, as well as other substance use disorders; • Increased risk of bronchitis and chronic cough. 21

Cocaine 22
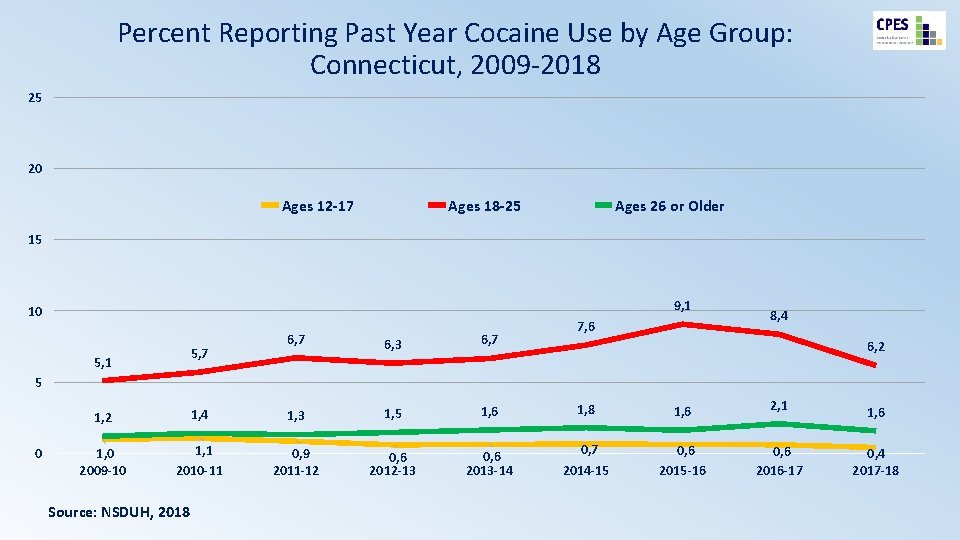
Percent Reporting Past Year Cocaine Use by Age Group: Connecticut, 2009 -2018 25 20 Ages 12 -17 Ages 18 -25 Ages 26 or Older 15 9, 1 10 5, 7 5, 1 6, 7 6, 3 6, 7 7, 6 8, 4 6, 2 5 0 1, 2 1, 4 1, 3 1, 5 1, 6 1, 8 1, 6 2, 1 1, 0 2009 -10 1, 1 2010 -11 0, 9 2011 -12 0, 6 2012 -13 0, 6 2013 -14 0, 7 0, 6 2015 -16 0, 6 2016 -17 Source: NSDUH, 2018 2014 -15 1, 6 0, 4 2017 -18
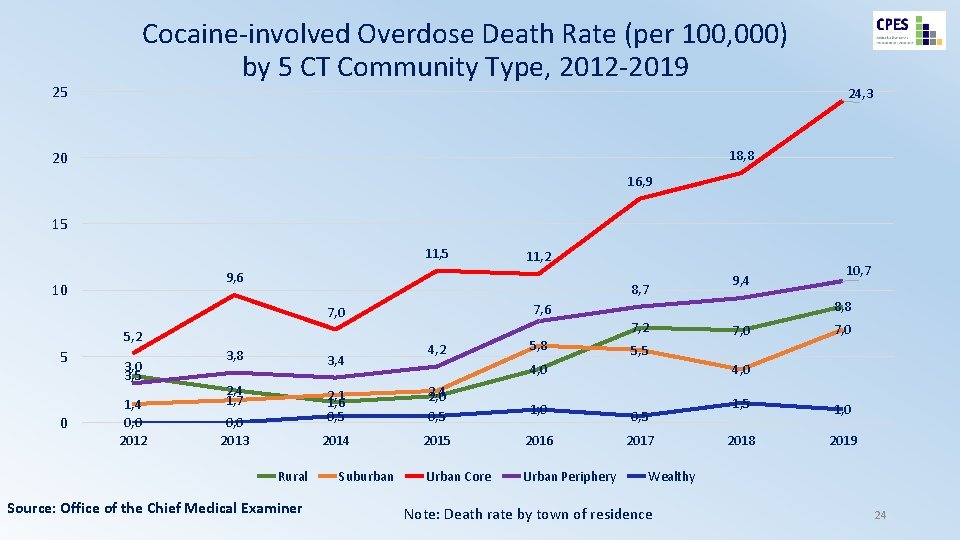
Cocaine-involved Overdose Death Rate (per 100, 000) by 5 CT Community Type, 2012 -2019 25 24, 3 18, 8 20 16, 9 15 11, 5 9, 6 10 8, 7 5, 2 0 3, 5 1, 4 0, 0 2012 3, 8 3, 4 2, 4 1, 7 2, 1 1, 6 0, 5 2014 0, 0 2013 Rural Source: Office of the Chief Medical Examiner Suburban 9, 4 7, 2 4, 2 5, 8 10, 7 8, 8 7, 6 7, 0 5 11, 2 7, 0 5, 5 4, 0 2, 4 2, 0 0, 5 1, 0 2015 2016 2017 2018 2019 Urban Core Urban Periphery Wealthy Note: Death rate by town of residence 24
Cocaine: Risk and Impact At-risk Populations • Young adults; • Males; • Those with prior misuse of other illicit substances; • Individuals with mental health challenges. Among youth, risk factors include: • Family history of substance use; • Lack of parental supervision; • Substance-using peers; • Lack of school connectedness; • Low academic achievement; • Childhood trauma. Effects and Impacts • Impairment of cognitive function; • Tolerance, requiring higher and more frequent doses; • Sensitization, where less cocaine is needed to produce anxiety, convulsions, or other toxic effects (increasing risk of overdose); • Loss of appetite leading to malnourishment; • Increased risk of stroke and inflammation of the heart muscle; • Movement disorders such as Parkinson’s disease. 25

Prescription Drugs: Painkillers 26

Percent of Persons Reporting Past Year Non-Medical Use of Pain Relievers, by Age Group: Connecticut, 2009 -2018 Source: NSDUH, 2018
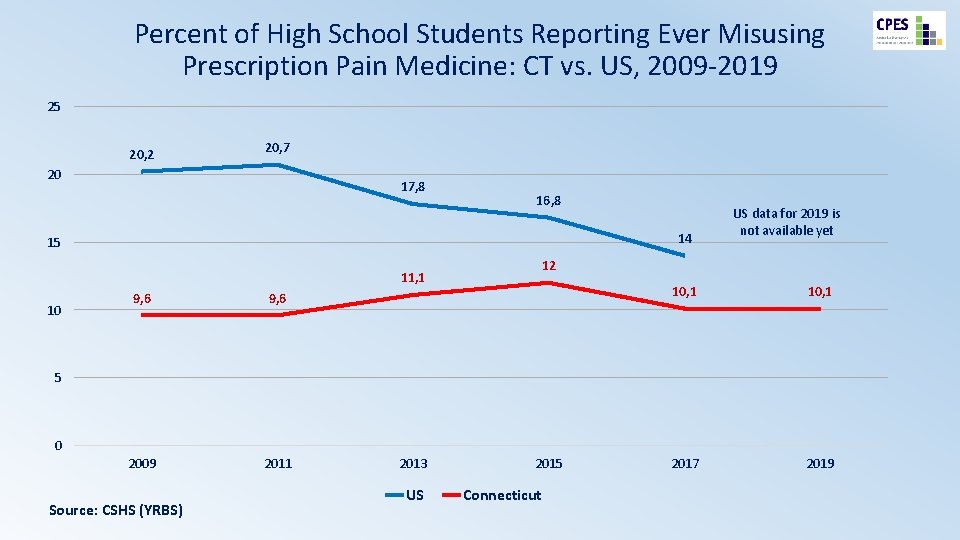
Percent of High School Students Reporting Ever Misusing Prescription Pain Medicine: CT vs. US, 2009 -2019 25 20, 2 20, 7 20 17, 8 16, 8 14 15 12 11, 1 10 9, 6 2009 2011 US data for 2019 is not available yet 10, 1 2017 2019 5 0 Source: CSHS (YRBS) 2013 US 2015 Connecticut
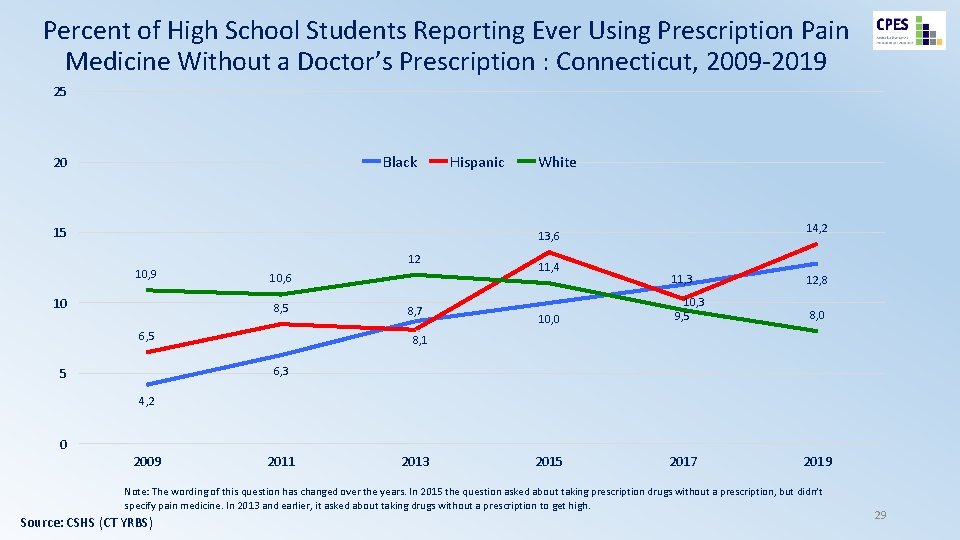
Percent of High School Students Reporting Ever Using Prescription Pain Medicine Without a Doctor’s Prescription : Connecticut, 2009 -2019 25 Black 20 15 Hispanic White 14, 2 13, 6 12 10, 9 10 10, 6 8, 5 6, 5 8, 7 11, 4 10, 0 11, 3 12, 8 10, 3 9, 5 8, 0 8, 1 6, 3 5 4, 2 0 2009 2011 2013 2015 2017 2019 Note: The wording of this question has changed over the years. In 2015 the question asked about taking prescription drugs without a prescription, but didn’t specify pain medicine. In 2013 and earlier, it asked about taking drugs without a prescription to get high. Source: CSHS (CT YRBS) 29

Prescription Drug Misuse: Risk and Impact At-risk Populations Effects and Impacts • Those with past year use of other substances; • People who take high daily dosages of opioid pain relievers; • Persons with mental illness; • People who use multiple controlled prescription medications, often prescribed by multiple providers; • Individuals with disabilities. • Increased risk of heroin and other illicit opioid misuse; • Severe respiratory depression, leading to hypoxia; • Short- and long-term psychological and neurological effects; • Coma; • Permanent brain damage; • Death. 30
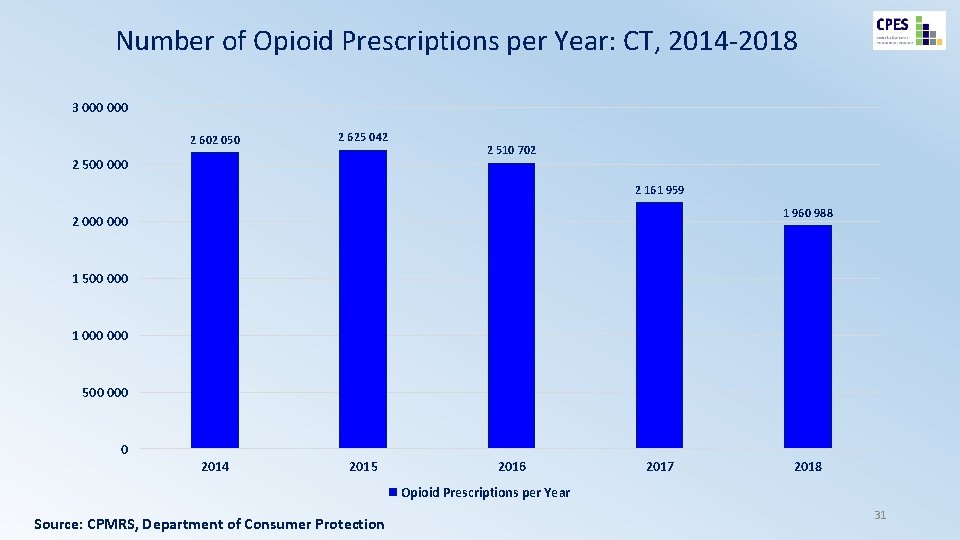
Number of Opioid Prescriptions per Year: CT, 2014 -2018 3 000 2 602 050 2 625 042 2 500 000 2 510 702 2 161 959 1 960 988 2 000 1 500 000 1 000 500 0 2014 2015 2016 2017 2018 Opioid Prescriptions per Year Source: CPMRS, Department of Consumer Protection 31

Opioids 32
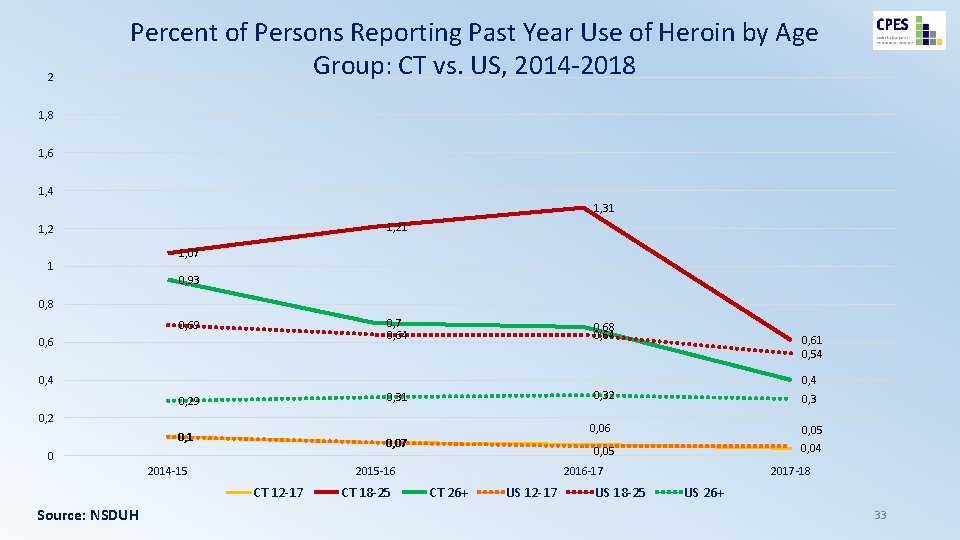
2 Percent of Persons Reporting Past Year Use of Heroin by Age Group: CT vs. US, 2014 -2018 1, 6 1, 4 1, 31 1, 2 1 1, 07 0, 93 0, 8 0, 7 0, 64 0, 68 0, 64 0, 29 0, 31 0, 32 0, 1 0, 07 0, 69 0, 61 0, 54 0, 2 0 2014 -15 Source: NSDUH 0, 06 CT 18 -25 0, 04 0, 05 2015 -16 CT 12 -17 0, 3 2016 -17 CT 26+ US 12 -17 US 18 -25 2017 -18 US 26+ 33
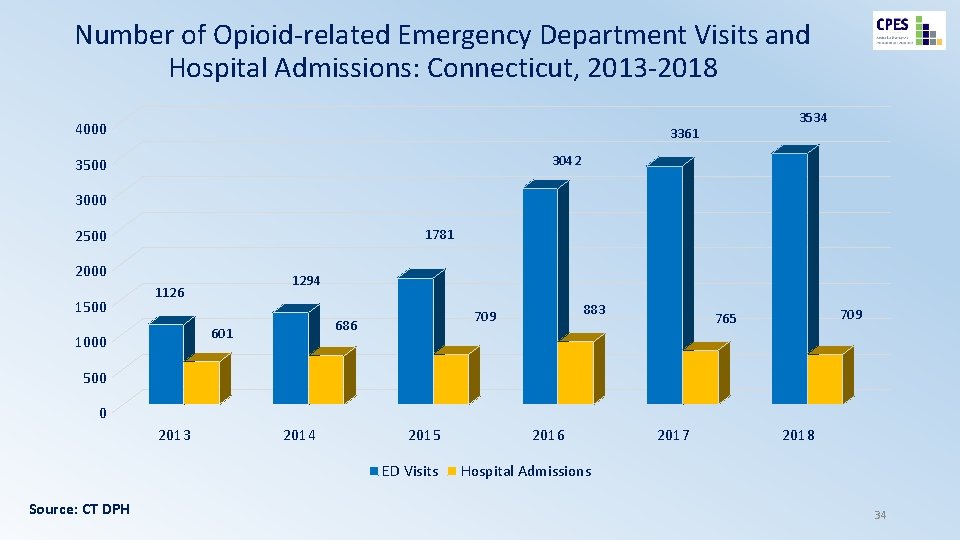
Number of Opioid-related Emergency Department Visits and Hospital Admissions: Connecticut, 2013 -2018 4000 3534 3361 3042 3500 3000 2500 1781 2000 1500 1294 1126 686 601 1000 883 709 765 500 0 2013 2014 2015 ED Visits Source: CT DPH 2016 2017 2018 Hospital Admissions 34
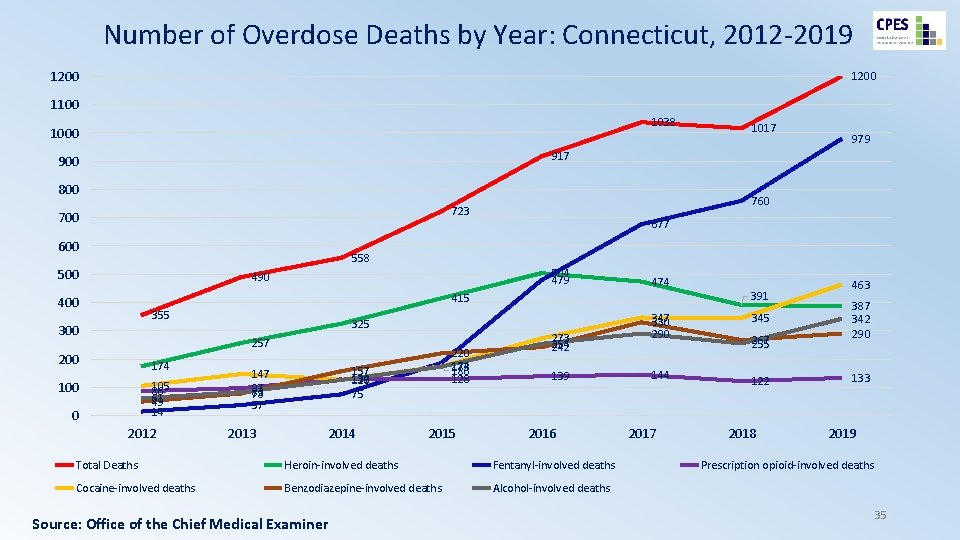
Number of Overdose Deaths by Year: Connecticut, 2012 -2019 1200 1100 1038 1000 1017 979 917 900 800 760 723 700 677 558 500 504 479 490 474 391 415 400 355 300 325 257 200 174 105 86 61 49 14 100 0 2012 157 130 127 126 75 147 97 83 78 37 2013 220 174 173 186 128 2014 2015 273 254 242 139 2016 Total Deaths Heroin-involved deaths Fentanyl-involved deaths Cocaine-involved deaths Benzodiazepine-involved deaths Alcohol-involved deaths Source: Office of the Chief Medical Examiner 347 330 290 144 2017 345 267 255 122 2018 463 387 342 290 133 2019 Prescription opioid-involved deaths 35
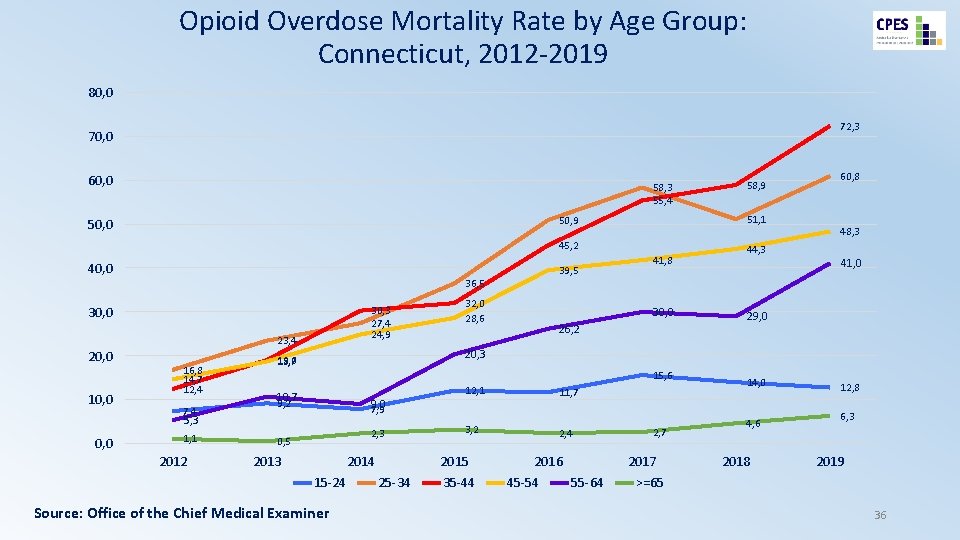
Opioid Overdose Mortality Rate by Age Group: Connecticut, 2012 -2019 80, 0 72, 3 70, 0 60, 0 58, 3 55, 4 51, 1 50, 9 50, 0 45, 2 40, 0 39, 5 36, 5 30, 0 20, 0 10, 0 30, 3 27, 4 24, 9 23, 4 16, 8 14, 7 12, 4 7, 4 0, 0 2012 41, 8 30, 0 26, 2 60, 8 48, 3 44, 3 41, 0 29, 0 20, 3 19, 0 18, 7 15, 6 10, 7 9, 2 9, 0 7, 9 5, 3 1, 1 32, 0 28, 6 58, 9 2, 3 0, 5 2013 2014 15 -24 Source: Office of the Chief Medical Examiner 12, 1 3, 2 2015 25 -34 11, 7 35 -44 2, 4 2016 45 -54 2, 7 2017 55 -64 14, 0 4, 6 2018 12, 8 6, 3 2019 >=65 36
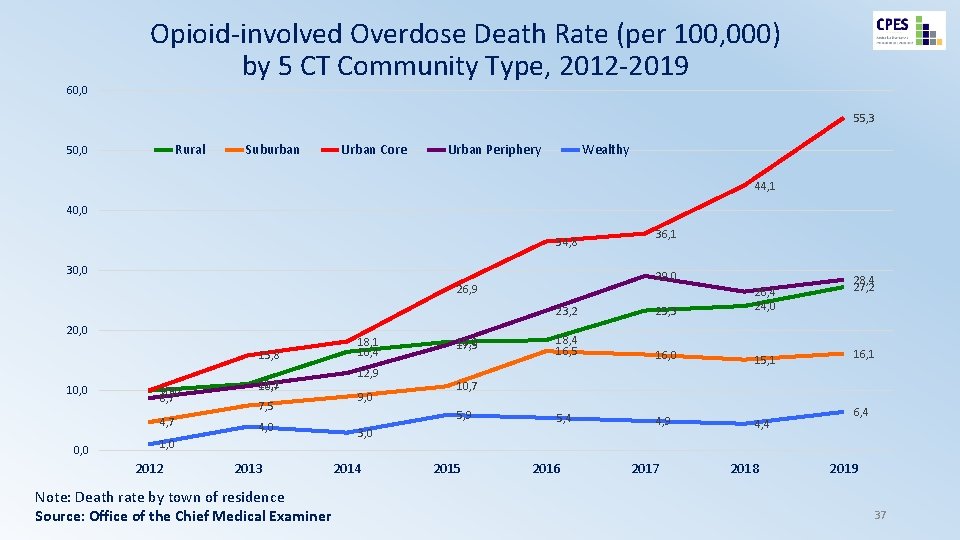
60, 0 Opioid-involved Overdose Death Rate (per 100, 000) by 5 CT Community Type, 2012 -2019 55, 3 Rural 50, 0 Suburban Urban Core Urban Periphery Wealthy 44, 1 40, 0 34, 8 30, 0 29, 0 26, 9 20, 0 15, 8 10, 0 9, 9 8, 7 4, 7 0, 0 11, 1 10, 7 7, 5 4, 0 1, 0 2012 2013 Note: Death rate by town of residence Source: Office of the Chief Medical Examiner 18, 1 16, 4 12, 9 9, 0 18, 0 17, 5 23, 2 23, 3 26, 4 24, 0 18, 4 16, 5 16, 0 15, 1 5, 4 4, 9 4, 4 28, 4 27, 2 16, 1 10, 7 5, 9 3, 0 2014 36, 1 2015 2016 2017 2018 6, 4 2019 37
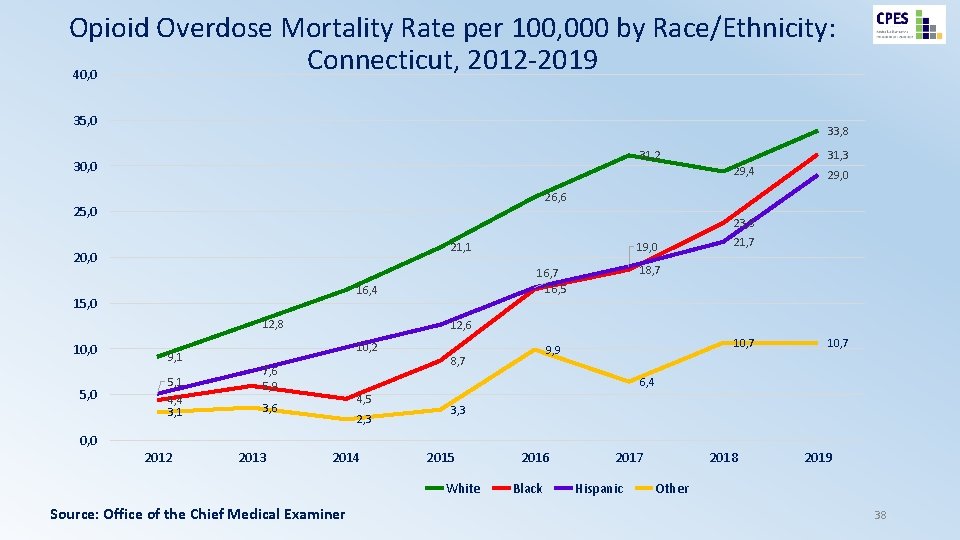
Opioid Overdose Mortality Rate per 100, 000 by Race/Ethnicity: Connecticut, 2012 -2019 40, 0 35, 0 33, 8 29, 4 23, 8 19, 0 21, 1 20, 0 12, 8 9, 1 5, 1 4, 4 3, 1 21, 7 18, 7 16, 5 16, 4 15, 0 29, 0 26, 6 25, 0 10, 0 31, 3 31, 2 30, 0 12, 6 10, 2 7, 6 5, 9 10, 7 9, 9 8, 7 10, 7 6, 4 4, 5 3, 6 2, 3 3, 3 0, 0 2012 2013 2014 2015 White Source: Office of the Chief Medical Examiner 2016 Black 2017 Hispanic 2018 2019 Other 38
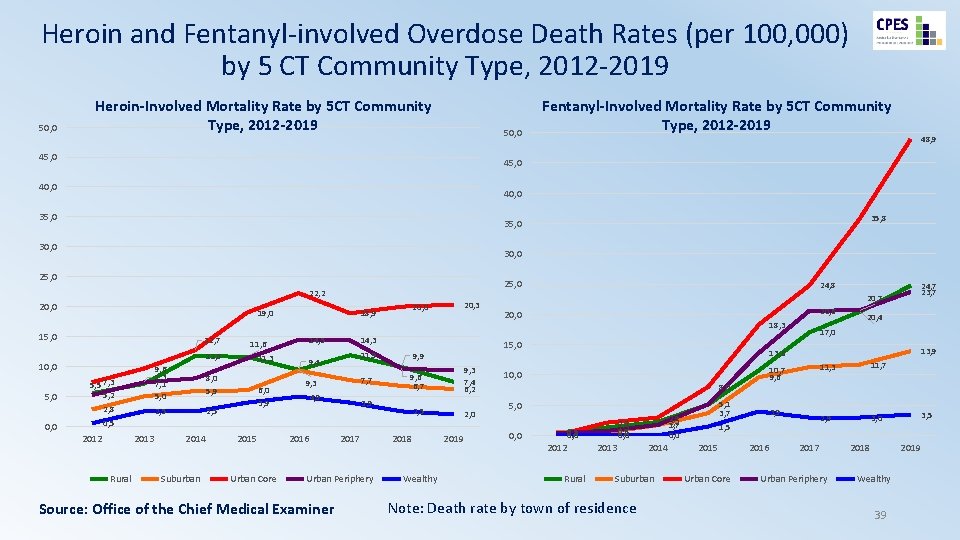
Heroin and Fentanyl-involved Overdose Death Rates (per 100, 000) by 5 CT Community Type, 2012 -2019 50, 0 Heroin-Involved Mortality Rate by 5 CT Community Type, 2012 -2019 50, 0 45, 0 48, 9 45, 0 40, 0 35, 8 35, 0 30, 0 25, 0 22, 2 20, 0 19, 0 15, 0 12, 7 5, 5 7, 3 5, 2 9, 6 7, 3 7, 1 5, 0 8, 0 5, 9 2, 8 2, 5 14, 5 11, 3 6, 0 3, 9 20, 3 20, 0 18, 9 11, 6 11, 8 10, 0 5, 0 Fentanyl-Involved Mortality Rate by 5 CT Community Type, 2012 -2019 14, 3 9, 4 9, 3 4, 9 9, 9 7, 7 9, 6 6, 7 9, 3 7, 4 6, 2 2, 5 2, 0 0, 5 0, 0 2012 2013 Rural 2014 Suburban 2015 Urban Core 2016 2017 Urban Periphery Source: Office of the Chief Medical Examiner 2018 Wealthy 2019 24, 7 23, 7 20, 6 20, 0 18, 3 15, 0 11, 9 3, 9 24, 8 20, 4 17, 0 13, 9 13, 6 10, 7 9, 6 10, 0 8, 0 5, 1 3, 7 1, 5 5, 0 0, 5 0, 4 0, 0 2012 Rural 2, 9 2, 2 1, 7 0, 0 2, 1 1, 3 0, 8 0, 5 0, 0 2013 2014 Suburban Note: Death rate by town of residence 2015 Urban Core 3, 9 2016 11, 3 11, 7 2, 9 3, 0 2017 Urban Periphery 2018 3, 5 2019 Wealthy 39

Fentanyl and Heroin: Risk and Impact At-risk Populations Effects and Impacts • Individuals who are using heroin or illicitly obtained prescription pills; • Fentanyl overdose outbreaks have been linked to fentanyl-contaminated cocaine. • People who are addicted to other substances are at risk of becoming addicted to heroin; • Non-Hispanic whites; • Males; • 18 to 25 year olds; • People without insurance or who are Medicaid; • People living in large metropolitan areas. on • Increased risk for unemployment, disruptions in family environments, and homelessness; • Increased risk for property and violent crime, gang violence, arrest and incarceration; • Hepatitis B virus, Hepatitis C virus, and HIV/AIDS (injection users); • Scarred and/or collapsed veins; • Bacterial infections of the blood vessels and heart valves; • Abscesses and other soft-tissue infections; • Liver or kidney disease. • Lung complications, including various types of pneumonia and tuberculosis; • Fatal overdose. 40
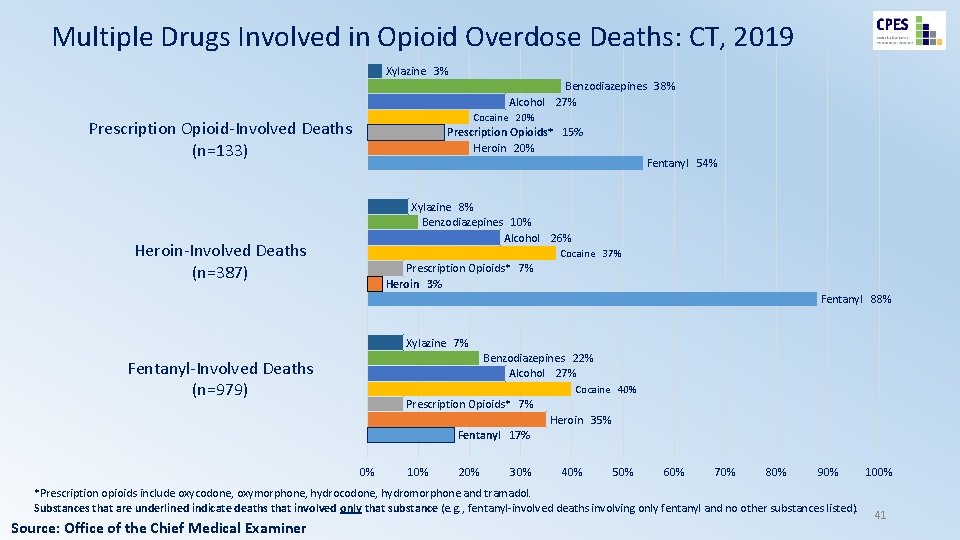
Multiple Drugs Involved in Opioid Overdose Deaths: CT, 2019 Xylazine 3% Benzodiazepines 38% Alcohol 27% Cocaine 20% Prescription Opioid-Involved Deaths (n=133) Prescription Opioids* 15% Heroin 20% Fentanyl 54% Xylazine 8% Benzodiazepines 10% Alcohol 26% Heroin-Involved Deaths (n=387) Cocaine 37% Prescription Opioids* 7% Heroin 3% Fentanyl 88% Xylazine 7% Benzodiazepines 22% Alcohol 27% Fentanyl-Involved Deaths (n=979) Cocaine 40% Prescription Opioids* 7% Heroin 35% Fentanyl 17% 0% 10% 20% 30% 40% 50% 60% 70% 80% 90% *Prescription opioids include oxycodone, oxymorphone, hydrocodone, hydromorphone and tramadol. Substances that are underlined indicate deaths that involved only that substance (e. g. , fentanyl-involved deaths involving only fentanyl and no other substances listed). Source: Office of the Chief Medical Examiner 100% 41
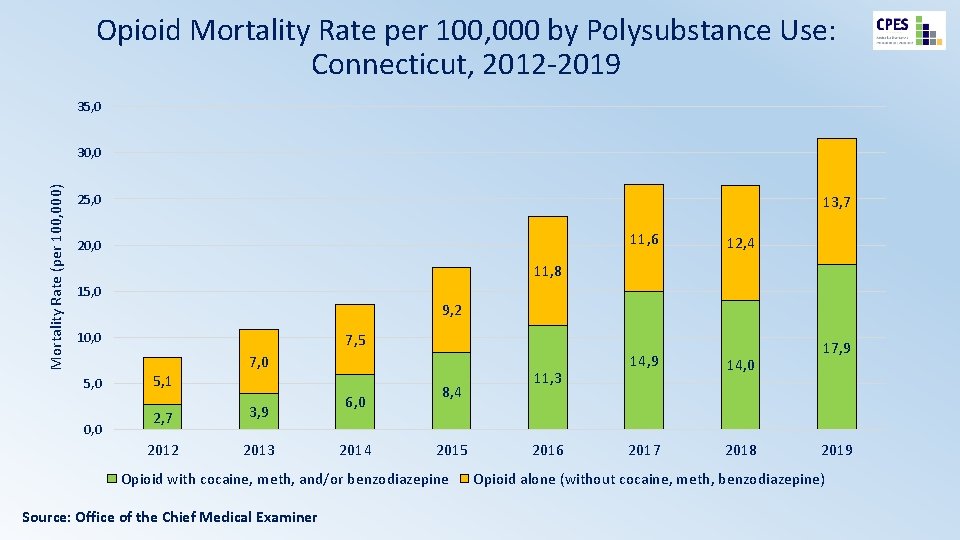
Opioid Mortality Rate per 100, 000 by Polysubstance Use: Connecticut, 2012 -2019 35, 0 Mortality Rate (per 100, 000) 30, 0 25, 0 13, 7 11, 6 20, 0 12, 4 11, 8 15, 0 9, 2 10, 0 7, 5 7, 0 5, 0 0, 0 5, 1 2, 7 3, 9 2012 2013 6, 0 2014 8, 4 2015 Opioid with cocaine, meth, and/or benzodiazepine Source: Office of the Chief Medical Examiner 11, 3 2016 14, 9 14, 0 2017 2018 17, 9 2019 Opioid alone (without cocaine, meth, benzodiazepine)
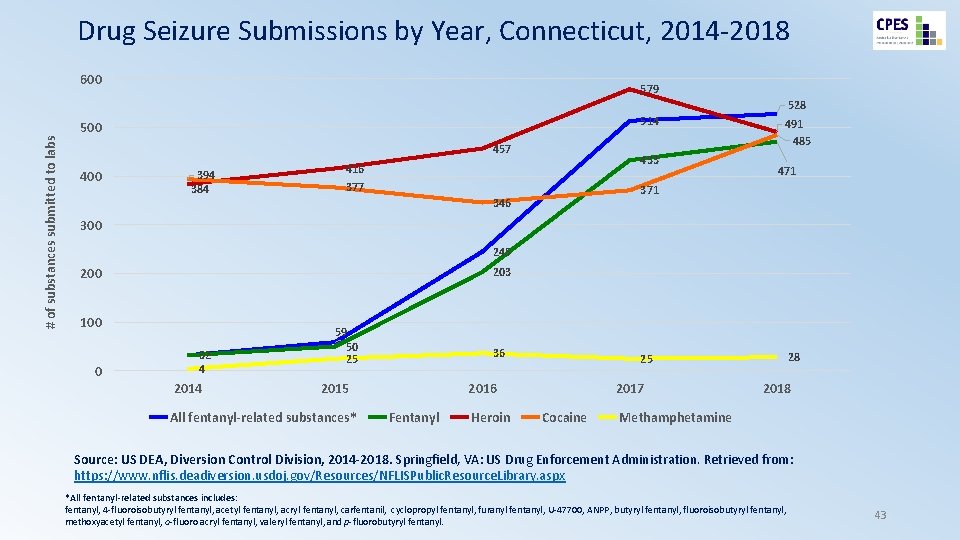
Drug Seizure Submissions by Year, Connecticut, 2014 -2018 600 579 # of substances submitted to labs 528 514 500 457 400 394 384 433 416 377 491 485 471 346 300 245 203 200 100 0 32 4 2014 59 50 25 36 2015 All fentanyl-related substances* 2016 Fentanyl Heroin 28 25 2017 Cocaine 2018 Methamphetamine Source: US DEA, Diversion Control Division, 2014 -2018. Springfield, VA: US Drug Enforcement Administration. Retrieved from: https: //www. nflis. deadiversion. usdoj. gov/Resources/NFLISPublic. Resource. Library. aspx *All fentanyl-related substances includes: fentanyl, 4 -fluoroisobutyryl fentanyl, acetyl fentanyl, acryl fentanyl, carfentanil, cyclopropyl fentanyl, furanyl fentanyl, U-47700, ANPP, butyryl fentanyl, fluoroisobutyryl fentanyl, methoxyacetyl fentanyl, o-fluoro acryl fentanyl, valeryl fentanyl, and p-fluorobutyryl fentanyl. 43
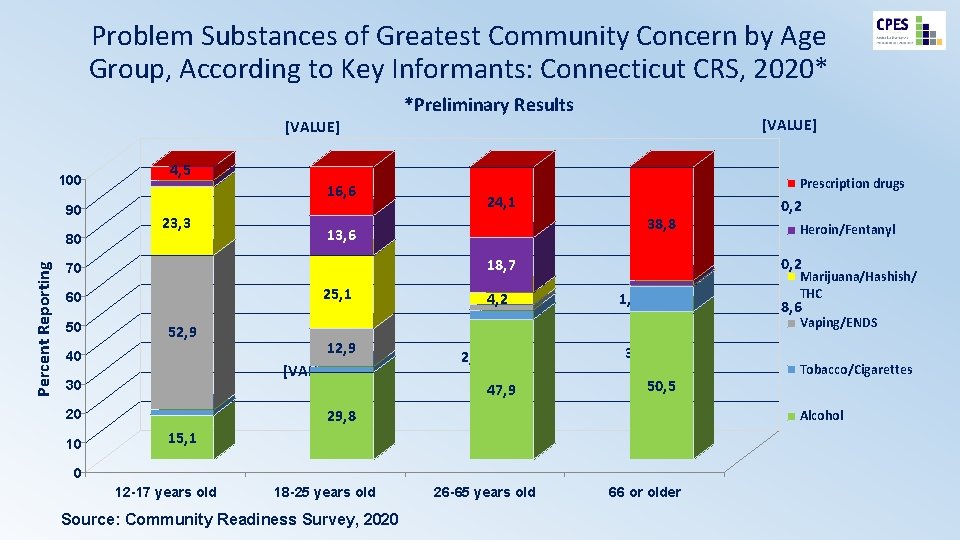
Problem Substances of Greatest Community Concern by Age Group, According to Key Informants: Connecticut CRS, 2020* *Preliminary Results [VALUE] 100 90 Percent Reporting 80 4, 5 Prescription drugs 16, 6 23, 3 24, 1 38, 8 13, 6 25, 1 60 50 52, 9 40 30 Marijuana/Hashish/ THC 1, 8 8, 6 Vaping/ENDS 12, 9 [VALUE] 3, 2 2, 0 47, 9 50, 5 29, 8 20 10 4, 2 0 18 -25 years old Source: Community Readiness Survey, 2020 Tobacco/Cigarettes Alcohol 15, 1 12 -17 years old Heroin/Fentanyl 0, 2 18, 7 70 0, 2 26 -65 years old 66 or older

For more information, contact Jane Ungemack: ungemack@uchc. edu or visit the SEOW Prevention Data Portal at https: //preventionportal. ctdata. org/ 45
- Slides: 45