Substance Misuse Module Diagnosis and Management of People

Substance Misuse Module : Diagnosis and Management of People with co-occurring mental health and alcohol/drug use conditions

Insert name of the LEP Aims and Objectives (from handbook) • To develop understanding of key aspects in the diagnosis and treatment of People with co-occurring mental health and alcohol/drug use conditions • To increase awareness of complications with pharmacological treatment in patients with co-occurring mental health and alcohol/drug use conditions • To develop knowledge of risk issues in people with co-occurring mental health and alcohol/drug use conditions • To understand how local services are implemented to manage people with co-occurring mental health and alcohol/drug use conditions

Insert name of the LEP To achieve this • • • Case Presentation Journal Club 555 Presentation Expert-Led Session MCQs • Please sign the register and complete the feedback

Insert name of the LEP Expert Led Session Diagnosis and Management of People with co-occurring mental health and alcohol/drug use conditions P Horgan Consultant in Substance Misuse, GMMH, Cumbria

Expert Led Session • Diagnosis and Management of People with cooccurring mental health and alcohol/drug use conditions – Concepts – Epidemiology – Case studies

Main references CADMHC 2016 CSUMDE 2015 DMAD 2017 DSM - 5

Terminology in use • • • Dual Diagnosis – World Health Organisation – A general term referring to comorbidity or the co-occurrence in the same individual of a psychoactive substance use disorder and another psychiatric disorder Coexisting severe mental illness and substance misuse: community health and social care services – NICE guideline [NG 58] 2016 Comorbidity of substance use and mental disorders in Europe – The European Monitoring Centre for Drugs and Drug Addiction Guidelines on the management of co-occurring alcohol and other drug and mental health conditions in alcohol and other drug treatment Settings – National Drug and Alcohol Research Centre University of New South Wales SAMHSA (Substance Abuse and Mental Health Services Administration ) USA – “When primary conditions simultaneously co-occur with substance use disorders, they are referred to as comorbidities” WHO
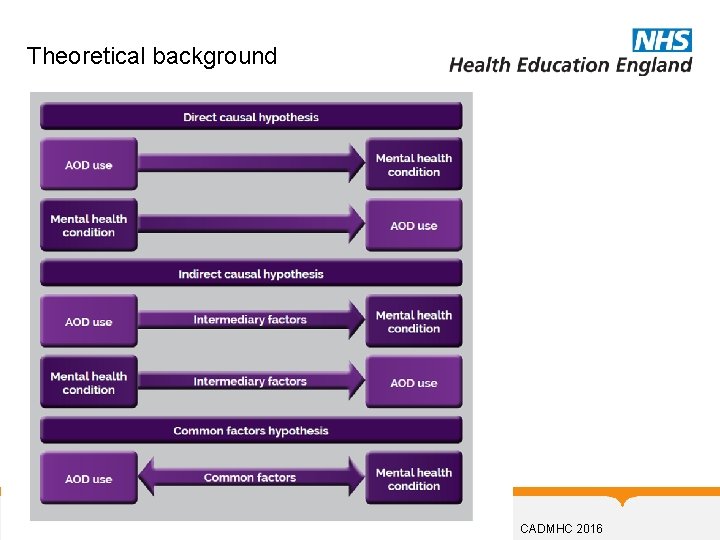
Theoretical background CADMHC 2016

Epidemiology -Methodological issues 1 Ascertainment and sampling a. General population /General hospitals /Patients in drug use services /Patients in mental health services /Drug users not seeking treatment/ Prison populations/ Homeless populations 2 Sociodemographic characteristics e. g. , age, gender 3 Assessment of substance misuse 4 Reliability of interview procedures 5 Medication side effects/ compliance CSUMDE 2015
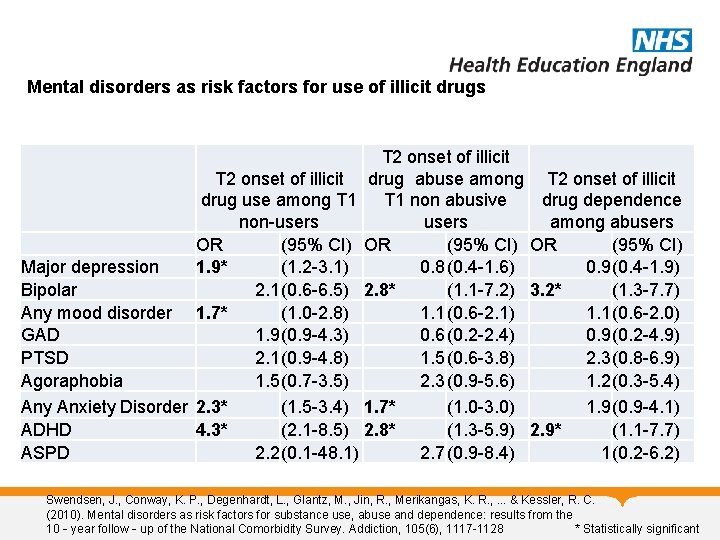
Mental disorders as risk factors for use of illicit drugs T 2 onset of illicit drug abuse among T 2 onset of illicit drug use among T 1 non abusive drug dependence non-users among abusers OR (95% CI) Major depression 1. 9* (1. 2 -3. 1) 0. 8(0. 4 -1. 6) 0. 9(0. 4 -1. 9) Bipolar 2. 1(0. 6 -6. 5) 2. 8* (1. 1 -7. 2) 3. 2* (1. 3 -7. 7) Any mood disorder 1. 7* (1. 0 -2. 8) 1. 1(0. 6 -2. 1) 1. 1(0. 6 -2. 0) GAD 1. 9(0. 9 -4. 3) 0. 6(0. 2 -2. 4) 0. 9(0. 2 -4. 9) PTSD 2. 1(0. 9 -4. 8) 1. 5(0. 6 -3. 8) 2. 3(0. 8 -6. 9) Agoraphobia 1. 5(0. 7 -3. 5) 2. 3(0. 9 -5. 6) 1. 2(0. 3 -5. 4) Any Anxiety Disorder 2. 3* (1. 5 -3. 4) 1. 7* (1. 0 -3. 0) 1. 9(0. 9 -4. 1) ADHD 4. 3* (2. 1 -8. 5) 2. 8* (1. 3 -5. 9) 2. 9* (1. 1 -7. 7) ASPD 2. 2(0. 1 -48. 1) 2. 7(0. 9 -8. 4) 1(0. 2 -6. 2) Swendsen, J. , Conway, K. P. , Degenhardt, L. , Glantz, M. , Jin, R. , Merikangas, K. R. , . . . & Kessler, R. C. (2010). Mental disorders as risk factors for substance use, abuse and dependence: results from the 10‐year follow‐up of the National Comorbidity Survey. Addiction, 105(6), 1117 -1128 * Statistically significant
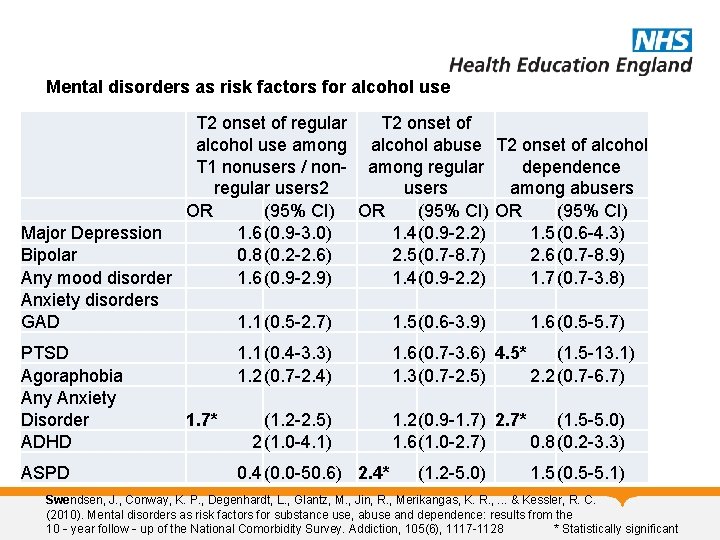
Mental disorders as risk factors for alcohol use T 2 onset of regular T 2 onset of alcohol use among alcohol abuse T 2 onset of alcohol T 1 nonusers / non- among regular dependence regular users 2 users among abusers OR (95% CI) Major Depression 1. 6(0. 9 -3. 0) 1. 4(0. 9 -2. 2) 1. 5(0. 6 -4. 3) Bipolar 0. 8(0. 2 -2. 6) 2. 5(0. 7 -8. 7) 2. 6(0. 7 -8. 9) Any mood disorder 1. 6(0. 9 -2. 9) 1. 4(0. 9 -2. 2) 1. 7(0. 7 -3. 8) Anxiety disorders GAD 1. 1(0. 5 -2. 7) 1. 5(0. 6 -3. 9) 1. 6(0. 5 -5. 7) PTSD Agoraphobia Any Anxiety Disorder ADHD ASPD 1. 1(0. 4 -3. 3) 1. 2(0. 7 -2. 4) 1. 7* (1. 2 -2. 5) 2(1. 0 -4. 1) 0. 4(0. 0 -50. 6) 2. 4* 1. 6(0. 7 -3. 6) 4. 5* (1. 5 -13. 1) 1. 3(0. 7 -2. 5) 2. 2(0. 7 -6. 7) 1. 2(0. 9 -1. 7) 2. 7* (1. 5 -5. 0) 1. 6(1. 0 -2. 7) 0. 8(0. 2 -3. 3) (1. 2 -5. 0) 1. 5(0. 5 -5. 1) Swendsen, J. , Conway, K. P. , Degenhardt, L. , Glantz, M. , Jin, R. , Merikangas, K. R. , . . . & Kessler, R. C. (2010). Mental disorders as risk factors for substance use, abuse and dependence: results from the 10‐year follow‐up of the National Comorbidity Survey. Addiction, 105(6), 1117 -1128 * Statistically significant
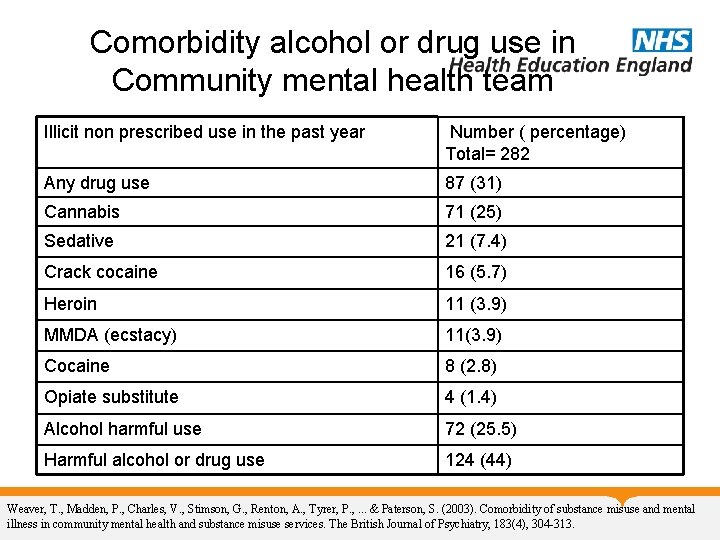
Comorbidity alcohol or drug use in Community mental health team Illicit non prescribed use in the past year Number ( percentage) Total= 282 Any drug use 87 (31) Cannabis 71 (25) Sedative 21 (7. 4) Crack cocaine 16 (5. 7) Heroin 11 (3. 9) MMDA (ecstacy) 11(3. 9) Cocaine 8 (2. 8) Opiate substitute 4 (1. 4) Alcohol harmful use 72 (25. 5) Harmful alcohol or drug use 124 (44) Weaver, T. , Madden, P. , Charles, V. , Stimson, G. , Renton, A. , Tyrer, P. , . . . & Paterson, S. (2003). Comorbidity of substance misuse and mental illness in community mental health and substance misuse services. The British Journal of Psychiatry, 183(4), 304 -313.
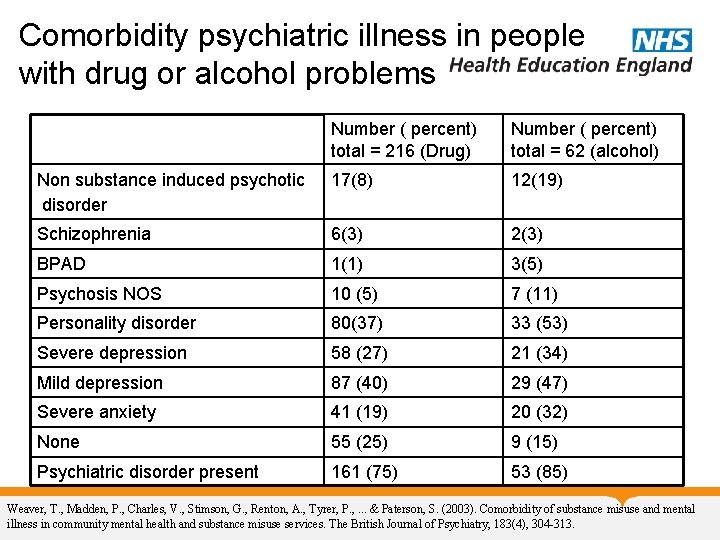
Comorbidity psychiatric illness in people with drug or alcohol problems Number ( percent) total = 216 (Drug) Number ( percent) total = 62 (alcohol) Non substance induced psychotic disorder 17(8) 12(19) Schizophrenia 6(3) 2(3) BPAD 1(1) 3(5) Psychosis NOS 10 (5) 7 (11) Personality disorder 80(37) 33 (53) Severe depression 58 (27) 21 (34) Mild depression 87 (40) 29 (47) Severe anxiety 41 (19) 20 (32) None 55 (25) 9 (15) Psychiatric disorder present 161 (75) 53 (85) Weaver, T. , Madden, P. , Charles, V. , Stimson, G. , Renton, A. , Tyrer, P. , . . . & Paterson, S. (2003). Comorbidity of substance misuse and mental illness in community mental health and substance misuse services. The British Journal of Psychiatry, 183(4), 304 -313.

Substance/Medication-Induced mental disorder (DSM V) A. The disorder represents a clinically significant symptomatic presentation of a relevant mental disorder B. There is evidence from the history /physical examination or laboratory findings of both A. The disorder developed during or within 1 month of a substance intoxication or withdrawal or taking a medication; and B. The involved substance/medication is capable of producing the mental disorder. C. The disturbance is not better explained by a mental disorder that is not substance / medication induced. e. g. , 1. The symptoms preceded the onset of severe intoxication or withdrawal or exposure to the medication 2. The mental disorder persisted for a substantial period of time (e. g. , at least a month) after the cessation of acute withdrawal / severe intoxication/taking the medication D. The disturbance does not occur exclusively during the course of a delirium E. The disturbance causes clinically significant distress or impairment in social, occupation or other important areas of functioning
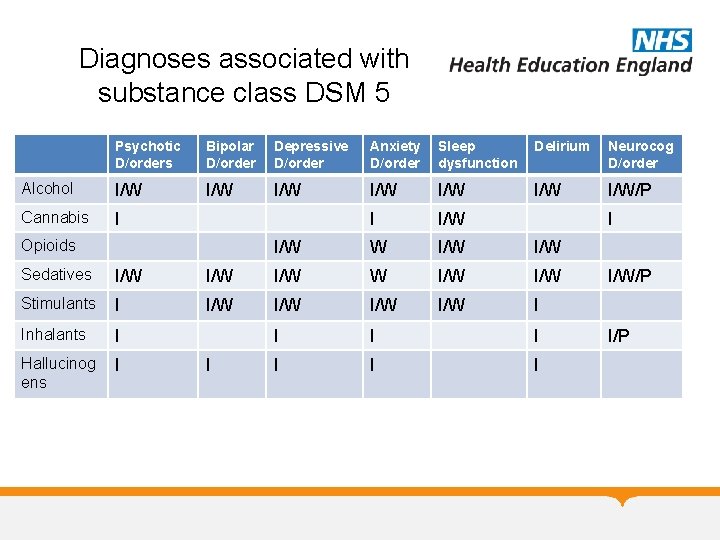
Diagnoses associated with substance class DSM 5 Psychotic D/orders Bipolar D/order Depressive D/order Anxiety D/order Sleep dysfunction Delirium Neurocog D/order Alcohol I/W I/W/P Cannabis I I I/W I/W I/W I/W I/W I I I I Opioids Sedatives I/W Stimulants I Inhalants I Hallucinog ens I I/W/P I/P
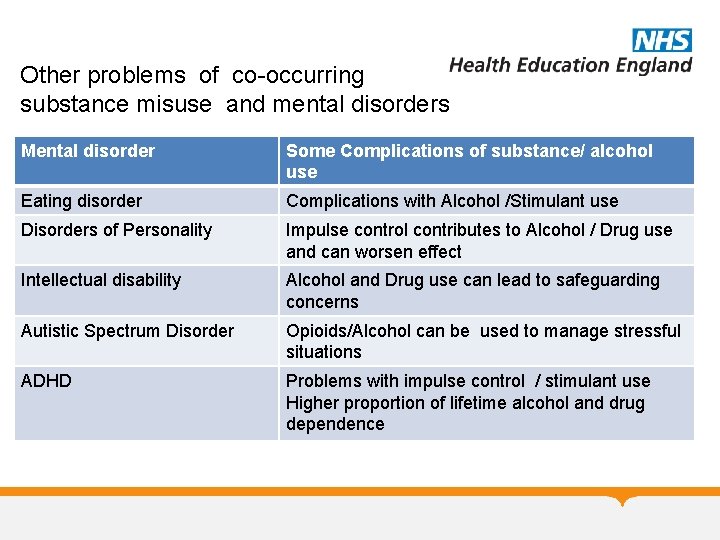
Other problems of co-occurring substance misuse and mental disorders Mental disorder Some Complications of substance/ alcohol use Eating disorder Complications with Alcohol /Stimulant use Disorders of Personality Impulse control contributes to Alcohol / Drug use and can worsen effect Intellectual disability Alcohol and Drug use can lead to safeguarding concerns Autistic Spectrum Disorder Opioids/Alcohol can be used to manage stressful situations ADHD Problems with impulse control / stimulant use Higher proportion of lifetime alcohol and drug dependence

Case Scenarios • In these scenarios consider following elements – Relevant history + examination • Interaction between the substance use and cooccurring mental illness – Diagnosis • Difficulties when effects of substance mimic symptoms of co-occurring mental illness – Treatment options • Evidence base/ consensus view • Safety concerns

Psychosis case 1 • 19 year old person who parents are suspecting is using cannabis every day. Parents have noticed strange smells from his room. Parents note that he has gotten packages in recent months from abroad. He is remaining in his room all day. Has had a change from previously whereby used to go out to see friends. Developed recent interest in the occult. No previous contact with psychiatric service. No other medication or physical symptoms.

Psychosis case 1 key points • Identify what type of cannabis e. g. , Skunk/ Spice/Resin • Get a sense of how much used per day – often best way is to check how much person is spending on this • Review if other drugs used especially from the “dark net” • Family history – can be helpful but can be complex e. g. , a parent with schizophrenia and cannabis dependence • Use education and encourage trial of cannabis abstinence reduction • Consider early intervention + substance misuse intervention coworking
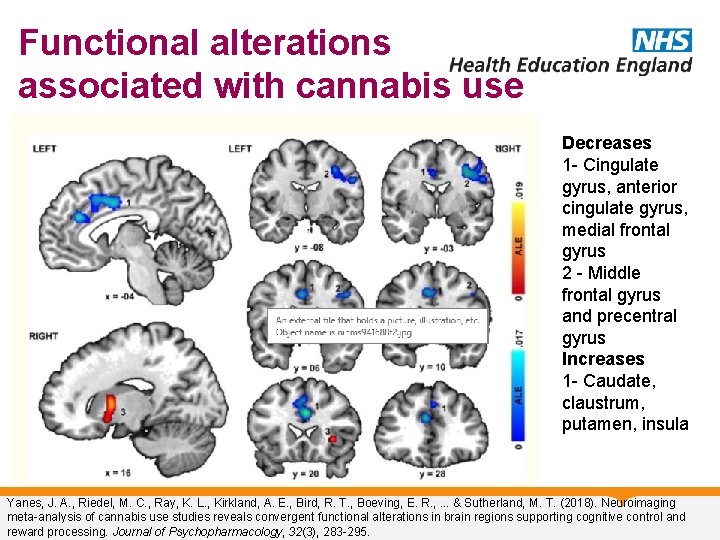
Functional alterations associated with cannabis use Decreases 1 - Cingulate gyrus, anterior cingulate gyrus, medial frontal gyrus 2 - Middle frontal gyrus and precentral gyrus Increases 1 - Caudate, claustrum, putamen, insula Yanes, J. A. , Riedel, M. C. , Ray, K. L. , Kirkland, A. E. , Bird, R. T. , Boeving, E. R. , . . . & Sutherland, M. T. (2018). Neuroimaging meta-analysis of cannabis use studies reveals convergent functional alterations in brain regions supporting cognitive control and reward processing. Journal of Psychopharmacology, 32(3), 283 -295.

Psychosis case 2 • 53 year old person with 30 year history of schizophrenia on depot medication and methadone and ongoing amphetamine use. Has beliefs involving being monitored by the government. Mother aged 84 provides meals. Admissions previously when he has accused his neighbours of spying on him. Often noted to be aggressive prior to admissions but no previous convictions. Prescribed diazepam to help with sleep. Diabetes developed when aged 35. Uses insulin for control but generally poor control.

Psychosis case 2 key points • Explore reason for amphetamine – could this be to overcome sedation • Assess how he takes amphetamine - intravenous or oral. If injecting could be prone to infections due to his diabetes • QTc important to check • Liaise with GP about control of diabetes – e. g. , any recent HBA 1 c • If obesity a factor consider NAFLD and need for viral hepatitis screening • Careful review of link between high amphetamine use and admissions and feedback in an motivation interviewing format • Risk assessment of violence to mother/ neighbours • Consider plan if mother unable to provide input/ becomes unwell • Be aware of effect of schizophrenia on life expectancy in addition to risks due to drug use

Bipolar Affective disorder • 56 year woman old; increased her alcohol use as reported could not sleep well. Lack of sleep was affecting her thinking and she was concerned she becoming unwell and her thinking was muddled. Reports having more rows with neighbours and also with people at work. On lithium for several years but more recently has been not attending appointment for lithium levels. .

Bipolar Affective disorder key points • Assess interaction mood and alcohol use; here alcohol use could be related to or a cause of the worsening of mania/ reduced adherence to lithium • Assessment whether she is safe to continue lithium depending on extent of her alcohol intoxication – consider risk of accidental overdose • Care that episodes of confusion may not be due to alcohol use – could be related to lithium toxicity • Important to educate her on suicidal risks increased by alcohol and reduced by lithium • Care with acamprosate use – need to check serum creatinine levels • Care with sedative drugs for mania – oversedation if also using alcohol

Personality disorder case 1 • 33 year old woman with long history of self harm overdoses and alcohol dependence. Sexually assaulted as a child. Has had a number of abusive relationships. Frequent admissions to psychiatric inpatient units years ago. Seeking community assisted withdrawals as feels could not cope with inpatient setting. Seeking disulfiram post discharge.

Personality disorder case 1 key points – Review history -was there unstable environment growing up? For example, a parent may have been alcohol dependent and other adverse childhood experiences ACE – Explore factors about her concern about inpatient – e. g. , how does she perceive her previous admissions? Were these under MHA? – A planned admission on a different unit could be more acceptable – Is disulfiram a safe option if thoughts of self harm- alcohol use may be most important so may help – Consider naltrexone as alternative or in addition to disulfiram – What forms of psychological treatment used/ available Zarse, E. M. , Neff, M. R. , Yoder, R. , Hulvershorn, L. , Chambers, J. E. , & Chambers, R. A. (2019). The adverse childhood experiences questionnaire: two decades of research on childhood trauma as a primary cause of adult mental illness, addiction, and medical diseases. Cogent Medicine, 6(1), 1581447

Personality disorder case 2 • 28 year old man due for prison release; history of offending since a teenager. Father was a well known criminal and father was violent to children and his wife. Has been in prison for last 9 out of 10 years. Prescribed 80 mgs methadone in prison. History of aggression in pharmacies and drug and alcohol services. Wants buprenorphine on release.

Personality disorder case 2 key points – Clarify nature of offences and liaise with probation – Important to engage and try to reduce drug use that could increase aggression- use joint working between mental health and substance use services with communication of risky behaviour between services – Contingency management may be useful – Risk management and use of boundaries in care settings – Consider reviews at probation setting – Identify warning signs for aggression – Consideration about risk of diversion of buprenorphine

Depression • 35 year old man drinking 35 units of lager per day. No sustained period of abstinence for 10 years. Past history of heroin use but not used since about age 25. Ongoing low mood; loss of weight; poor sleep and thoughts of suicide. Poor appetite; low energy; concentration problems. Three previous overdoses when intoxicated. Reported that fluoxetine and sertraline were not helpful. Not had sustained CBT treatment.

Depression key points • Try to distinguishing depression compared to effects of substance by assessing – Core depression symptoms e. g, ‘sadness’, ‘loss of interest’ – Symptoms unrelated to substance ‘low energy’, ‘difficulty concentrating’, ‘low self-confidence’, ‘thoughts of death’ • Uncertainty about best antidepressant medication to use in this group • Care about assessing overdose – especially using opioids/heroin • Consider how best to use psychological approaches – is it feasible if using high levels of alcohol

Anxiety • 34 year old reports being a worrier for many years- can’t concentrate/reports being unable to relax/ frequently restless/ feeling dizzy with dry mouth. He reports only medication that helps with his anxiety is diazepam which he takes 10 mgs 5 times per day. Also uses 2 to 4 cans of lager per day. Has been prescribed citalopram and fluoxetine in the past but did not help. Has had counselling sessions but did not feel able to relate to therapist. Has been taking illicit diazepam for 15 years.

Anxiety key points • Education about the risks of benzodiazepines – prescribed or illicit • Difficult to distinguish prescribed benzodiazepines from illicit benzodiazepines • Benzodiazepines are complex to use for sleep ( insomnia may be benzodiazepine withdrawal) see CIWA B • Care with initiation of SSRIs /Consideration for buspirone • Models of chronic alcohol use in mice suggest that fear extinction is impaired – suggests alcohol may interfere with psychological approaches for treatment of anxiety

PTSD • 48 year old man previously in the Army; reported exposure to a number of traumatic experiences within the Army. High alcohol use in the Army and currently high alcohol use. Recently has disclosed sexual abuse as a child. This was in the context of an investigation of a football coach who abused a number of children. Investigation expected to continue for several years.

PTSD key points • Check if problems with alcohol started before he was in the army after the events whilst in the army • Assess for any other drug use especially benzodiazepines • Check if treatment for PTSD whilst in the army • Explore treatment options available for veterans • Check about any psychology support available in the context of the investigation and the nature of this treatment • Outline rationale for using trauma focused cognitive behavioural treatment
![Attention deficit hyperactivity disorder: diagnosis and management NICE guideline [NG 87] Published date: March Attention deficit hyperactivity disorder: diagnosis and management NICE guideline [NG 87] Published date: March](http://slidetodoc.com/presentation_image_h/1169b03922a09dff8813dc3b001fe7b8/image-35.jpg)
Attention deficit hyperactivity disorder: diagnosis and management NICE guideline [NG 87] Published date: March 201 ADHD • 41 year old man; reporting using IV amphetamine for 20 years; recent endocarditis but restarted using shortly after valve replacement, usually does not use drug and alcohol services but mother highly concerned. Mother mentions that he had ADHD as child. Staying with mother and had not worked since he was 25.

ADHD –Learning points • Try to confirm diagnosis of ADHD where possible • 60% of children will continue to experience symptoms of ADHD as adults, whilst at least 30% will carry the full disorder through to adulthood • Assess for psychiatric disorders – depression / mania/ personality disorder • Unclear best medication for amphetamine dependence (without ADHD) • Further complexity if person has ADHD consideration for atomoxetine, methylphenidate, dexamphetamine

Neurocognition /ID • 54 Year old man. Long history of alcohol use but abstinent for last two years. Injury 1 year ago fell down stairs – multiple fractures – arms and legs. Since then ongoing pain – multiple medications. Isolated and poor mobility. Daughter reports very poor memory • 45 year old woman known to ID service with unstable alcohol use; accommodation at risk; risks of exploitation; does not want to stop using alcohol Ridley, N. J. , Draper, B. , & Withall, A. (2013). Alcohol-related dementia: an update of the evidence. Alzheimer's research & therapy, 5(1), 3. Lin, E. , Balogh, R. , Mc. Garry, C. , Selick, A. , Dobranowski, K. , Wilton, A. S. , & Lunsky, Y. (2016). Substance-related and addictive disorders among adults with intellectual and developmental disabilities (IDD): an Ontario population cohort study. BMJ open, 6(9), e 011638.

Neurocognition/ID key learning points 1. Case 1 – Consider how alcohol can have effects on cognition other than via Wernicke’s syndrome – Alcohol use increases risks with other medication – Other medication e. g. , pregabalin can also increase confusion and affect mobility 2. Case 2 – Often the issue can be that ID is suspected but not assessed or not to extent that requires input from ID team – Increase risk of of other physical and mental health problems if substance misuse /alcohol and ID
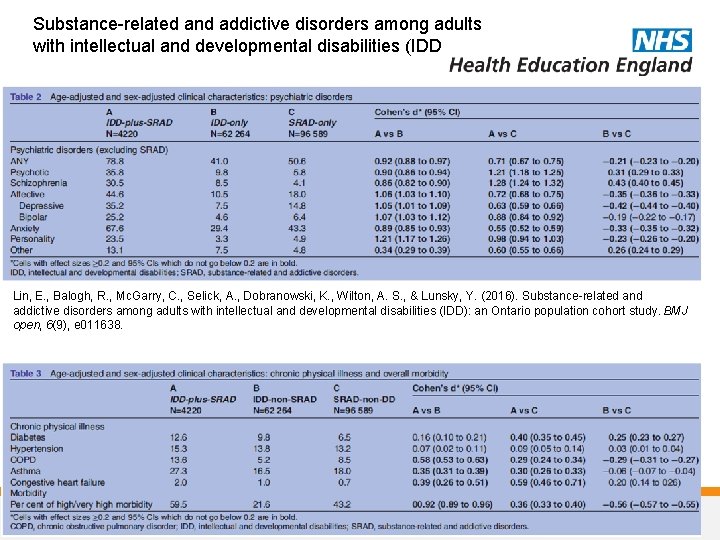
Substance-related and addictive disorders among adults with intellectual and developmental disabilities (IDD Lin, E. , Balogh, R. , Mc. Garry, C. , Selick, A. , Dobranowski, K. , Wilton, A. S. , & Lunsky, Y. (2016). Substance-related and addictive disorders among adults with intellectual and developmental disabilities (IDD): an Ontario population cohort study. BMJ open, 6(9), e 011638.

Eating disorder/OCD • 22 year old woman with BMI of 15 with a history of Anorexia nervosa + features of alcohol dependence; She is concerned about her alcohol use and want assisted withdrawals in the community. • 35 years old man reported distressing symptom relating to order and checking. 5 year history of alcohol dependence. Uses alcohol to manage distress with OCD. . Klostermann, K. C. , & Fals-Stewart, W. (2008). Treatment of co-morbid obsessive-compulsive disorder and substance use disorders. In Anxiety and Substance Use Disorders (pp. 101 -117). Springer, Boston, MA

Eating disorder/OCD key learning points 1. Case 1 – Anorexia nervosa and alcohol dependence can be very challenging to treat as can develop dangerous physical conditions e. g. , refeeding syndrome – Would seem unlikely can manage detox in community – Alcoholic drink may be only source of calories – Joint working between specialist services needed 2. Case 2 – Often not considered as often as should be – 1/10 people with alcohol or drug use may have OCD – Try concurrent treatment for OCD and alcohol and other drug use problems – However due to nature of interventions separate sessions for each modality may be better

Expert Led Session • Diagnosis and Management of People with cooccurring mental health and alcohol/drug use conditions – Concepts – Epidemiology – Case studies

Which of the following have not been used for misuse potential 1. Which of the following have not been associated with misuse potential : A. Acamprosate B. Hyoscine butylbromide C. Loperamide D. Pregabalin E. Codeine phosphate

Which of the following have not been associated with misuse potential 1. Which of the following have not been associated with misuse potential : A. Acamprosate B. Hyoscine butylbromide C. Loperamide D. Pregabalin E. Codeine phosphate

Substance misuse 2. Intoxication of the following substances can be associated with psychosis in DSM 5 except : A. Alcohol B. Cannabis C. Sedatives D. Opioids E. Inhalants

Substance misuse 2. Intoxication of the following substances can be associated with psychosis in DSM 5 except : A. Alcohol B. Cannabis C. Sedatives D. Opioids E. Inhalants

Substance misuse 3. Which of the following symptoms is not associated with Benzodiazepines withdrawal using CIWA B A. Loss of appetite B. Yawning C. Problems sleeping D. Difficulties with concentration E. Sensitivity to light / blurred vision

Substance misuse 3. Which of the following symptoms are not usually associated with Benzodiazepines withdrawal with CIWA B A. Loss of appetite B. Yawning C. Problems sleeping D. Difficulties with concentration E. Sensitivity to light / blurred vision

Substance Misuse MCQs 4. Percentage of patients attending Community Mental Health Teams reporting past-year problem drug use and/or harmful alcohol use has been found to be approximately: A. 24% B. 34% C. 44% D. 54% E. 64%

Substance Misuse MCQs 4. Percentage of patients attending Community Mental Health Teams reporting past-year problem drug use and/or harmful alcohol use has been found to be approximately: A. 24% B. 34% C. 44% D. 55% E. 64%

Substance misuse 5. Which of the following is likely to predate Alcohol and other Drug use disorder in most cases; A. Generalised anxiety disorder (GAD), B. Panic disorder, C. Depression D. Dysthymia E. PTSD

Substance misuse 5. Which of the following tends to predate Alcohol and other drug use disorders in most cases; A. Generalised anxiety disorder (GAD), B. Panic disorder, C. Depression D. Dysthymia E. PTSD

Substance Misuse EMI Drugs that may induce psychiatric symptoms A. Gamma-Hydroxybutyric acid (GHB) B. Lysergic acid diethylamide (LSD) C. Ketamine D. Phencyclidine (PCP) E. Diazepam F. Amphetamine G. Cocaine H. Alcohol I. Cannabis J. Butane (1) This psychoactive component of this drug acts through the type 1 form of the receptors which are found in high concentrations throughout the cerebellum, hippocampus, basal ganglia, cortex, brainstem, thalamus and hypothalamus (2) This compound acts as an agonist at 5 HT 2 A receptor (3) One of the main mechanisms of action of this drug is by reverse transfer of the neurotransmitter dopamine

Substance Misuse EMI (1) This psychoactive component of this drug acts through the type 1 form of the receptors which are found in high concentrations throughout the cerebellum, hippocampus, basal ganglia, cortex, brainstem, thalamus and hypothalamus. Answer: Cannabis (2) This compound acts as an agonist at 5 HT 2 A receptor. Answer: Lysergic acid diethylamide (LSD) (3) One of the main mechanisms of action of this drug is by reverse transfer of the neurotransmitter dopamine. Answer : Amphetamine

Substance Misuse EMI Psychotropic medications used in dual diagnosis patients: A. Diazepam B. Quetiapine C. Risperidone D. Citalopram E. Amisulpride F. Sertraline G. Baclofen H. Olanzapine I. Aripipazole J. Fluoxetine 2 a. Disulfiram can inhibit the metabolism of this compound 2 b. This antipsychotic should be considered in patients with impaired liver function 2 c. This agent may increase risk of compulsive behaviour such as gambling

Substance Misuse EMI 2 a. Disulfiram can inhibit the metabolism of this compound. Answer: Diazepam 2 b. This antipsychotic should be considered in patients with impaired liver function. Answer: Amisulpride 2 c. This agent may increase risk of compulsive behaviour such as gambling Answer: Aripipazole

Supplementary slides References

CIWA B

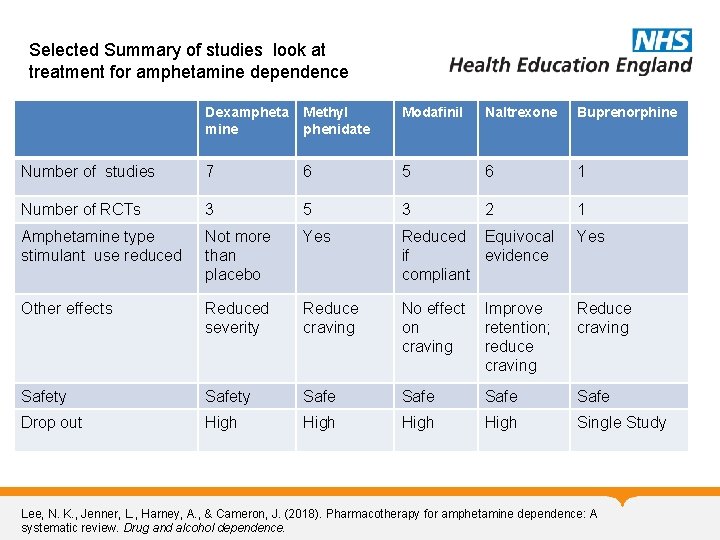
Selected Summary of studies look at treatment for amphetamine dependence Dexampheta mine Methyl phenidate Modafinil Naltrexone Buprenorphine Number of studies 7 6 5 6 1 Number of RCTs 3 5 3 2 1 Amphetamine type stimulant use reduced Not more than placebo Yes Reduced Equivocal Yes if evidence compliant Other effects Reduced severity Reduce craving No effect Improve on retention; craving reduce craving Reduce craving Safety Safe Safe Drop out High Single Study Lee, N. K. , Jenner, L. , Harney, A. , & Cameron, J. (2018). Pharmacotherapy for amphetamine dependence: A systematic review. Drug and alcohol dependence.

Epidemiology references • • • Aichhorn, W. , Santeler, S. , Stelzig-Schöler, R. , Kemmler, G. , Steinmayr-Gensluckner, M. , & Hinterhuber, H. (2008). Prevalence of psychiatric disorders among homeless adolescents. Neuropsychiatrie: Klinik, Diagnostik, Therapie und Rehabilitation: Organ der Gesellschaft Osterreichischer Nervenarzte und Psychiater, 22(3), 180 -188. Beijer, U. , Andréasson, A. , Ågren, G. , & Fugelstad, A. (2007). Mortality, mental disorders and addiction: a 5 year follow-up of 82 homeless men in Stockholm. Nordic Journal of Psychiatry, 61(5), 363 -368. Combaluzier, S. , B. Gouvernet, and A. Bernoussi. "Impact of personality disorders in a sample of 212 homeless drug users. " L'Encephale 35. 5 (2009): 448 -453. Demyttenaere, Koen, et al. "Prevalence, severity, and unmet need for treatment of mental disorders in the World Health Organization World Mental Health Surveys. " Jama 291. 21 (2004): 2581 -2590 Haw, C. M. , & Hawton, K. (2011). Problem drug use, drug misuse and deliberate self-harm: trends and patient characteristics, with a focus on young people, Oxford, 1993– 2006. Social psychiatry and psychiatric epidemiology, 46(2), 85 -93. Martín-Santos, R. , Fonseca, F. , Domingo-Salvany, A. , Ginés, J. M. , Ímaz, M. L. , Navinés, R. , . . . & Torrens, M. (2006). Dual diagnosis in the psychiatric emergency room in Spain. The European Journal of Psychiatry, 20(3), 147 -156. Torrens, M. , Mestre-Pintó, J. I. , & Domingo-Salvany, A. (2015). Comorbidity of substance use and mental disorders in Europe. Publication Office of the European Union.

Psychosis - references • • Crump, C. , Sundquist, K. , Winkleby, M. A. , & Sundquist, J. (2013). Comorbidities and mortality in bipolar disorder: a Swedish national cohort study. JAMA psychiatry, 70(9), 931 -939. Farnia, V. , Shakeri, J. , Tatari, F. , Juibari, T. A. , Yazdchi, K. , Bajoghli, H. , . . . & Aghaei, A. (2014). Randomized controlled trial of aripiprazole versus risperidone for the treatment of amphetamine-induced psychosis. The American journal of drug and alcohol abuse, 40(1), 10 -15. Hunt, G. E. , Siegfried, N. , Morley, K. , Sitharthan, T. , & Cleary, M. (2013). Psychosocial interventions for people with both severe mental illness and substance misuse. Cochrane Database of Systematic Reviews, (10). Shoptaw, S. J. , Kao, U. , & Ling, W. W. (2008). Treatment for amphetamine psychosis. Cochrane database of systematic reviews, (4). Thomsen, K. R. , Thylstrup, B. , Pedersen, M. M. , Pedersen, M. U. , Simonsen, E. , & Hesse, M. (2018). Drug-related predictors of readmission for schizophrenia among patients admitted to treatment for drug use disorders. Schizophrenia research, 195, 495 -500. Tiihonen, J. , Mittendorfer-Rutz, E. , Torniainen, M. , Alexanderson, K. , & Tanskanen, A. (2015). Mortality and cumulative exposure to antipsychotics, antidepressants, and benzodiazepines in patients with schizophrenia: an observational follow-up study. American Journal of Psychiatry, 173(6), 600 -606. Volkow, N. D. , Swanson, J. M. , Evins, A. E. , De. Lisi, L. E. , Meier, M. H. , Gonzalez, R. , . . . & Baler, R. (2016). Effects of cannabis use on human behavior, including cognition, motivation, and psychosis: a review. JAMA psychiatry, 73(3), 292 -297. Xue, X. , Song, Y. , Yu, X. , Fan, Q. , Tang, J. , & Chen, X. (2018). Olanzapine and haloperidol for the treatment of acute symptoms of mental disorders induced by amphetamine-type stimulants: A randomized controlled trial. Medicine, 97(8).

Bipolar Affective Disorder - References • • • Gold, A. K. , Otto, M. W. , Deckersbach, T. , Sylvia, L. G. , Nierenberg, A. A. , & Kinrys, G. (2018). Substance use comorbidity in bipolar disorder: A qualitative review of treatment strategies and outcomes. The American journal on addictions, 27(3), 188 -201. Messer, Thomas, et al. "Substance abuse in patients with bipolar disorder: A systematic review and metaanalysis. " Psychiatry research 253 (2017): 338 -350. Messer, T. , Lammers, G. , Müller-Siecheneder, F. , Schmidt, R. F. , & Latifi, S. (2017). Substance abuse in patients with bipolar disorder: A systematic review and meta-analysis. Psychiatry research, 253, 338 -350. Sepede, G. , Lorusso, M. , Spano, M. C. , Di Nanno, P. , Di Iorio, G. , & Di Giannantonio, M. (2018). Efficacy and Safety of Atypical Antipsychotics in Bipolar Disorder With Comorbid Substance Dependence: A Systematic Review. Clinical neuropharmacology, 41(5), 181 -191. Weiss, R. D. , Griffin, M. L. , Kolodziej, M. E. , Greenfield, S. F. , Najavits, L. M. , Daley, D. C. , . . . & Hennen, J. A. (2007). A randomized trial of integrated group therapy versus group drug counseling for patients with bipolar disorder and substance dependence. American Journal of Psychiatry, 164(1), 100 -107.

Personality disorder - references • • • Dimeff, L. A. , & Linehan, M. M. (2008). Dialectical behavior therapy for substance abusers. Addiction science & clinical practice, 4(2), 39. Fazel, S. , Smith, E. N. , Chang, Z. , & Geddes, J. R. (2018). Risk factors for interpersonal violence: an umbrella review of meta-analyses. The British Journal of Psychiatry, 213(4), 609 -614. Gibbon S, Duggan C, Stoffers J, Huband N, Völlm BA, Ferriter M, Lieb K. Psychological interventions for antisocial personality disorder. Cochrane Database of Systematic Reviews 2010, Issue 6. Art. No. : CD 007668. DOI: 10. 1002/14651858. CD 007668. pub 2. Lee, N. K. , Cameron, J. , & Jenner, L. (2015). A systematic review of interventions for co‐occurring substance use and borderline personality disorders. Drug and alcohol review, 34(6), 663 -672. Messina, N. , Farabee, D. , & Rawson, R. (2003). Treatment responsivity of cocaine-dependent patients with antisocial personality disorder to cognitive-behavioral and contingency management interventions. Journal of consulting and clinical psychology, 71(2), 320.

Depression References • • • Agabio, R. , Trogu, E. , & Pani, P. P. (2018). Antidepressants for the treatment of people with co‐occurring depression and alcohol dependence. Cochrane Database of Systematic Reviews, (4). Hides, L. , Samet, S. , & Lubman, D. I. (2010). Cognitive behaviour therapy (CBT) for the treatment of co‐occurring depression and substance use: Current evidence and directions for future research. Drug and Alcohol Review, 29(5), 508 -517. Mestre-Pintó, J. I. , Domingo-Salvany, A. , Martín-Santos, R. , & Torrens, M. (2014). Dual diagnosis screening interview to identify psychiatric comorbidity in substance users: development and validation of a brief instrument. European addiction research, 20(1), 41 -48. Pettinati, H. M. , Oslin, D. W. , Kampman, K. M. , Dundon, W. D. , Xie, H. , Gallis, T. L. , . . . & O'Brien, C. P. (2010). A double-blind, placebo-controlled trial combining sertraline and naltrexone for treating co-occurring depression and alcohol dependence. American Journal of Psychiatry, 167(6), 668 -675. Tirado-Muñoz, J. , Farré, A. , Mestre-Pintó, J. , Szerman, N. , & Torrens, M. (2018). Dual diagnosis in Depression: treatment recommendations. adicciones, 30(1).

Anxiety - references • • • Baandrup L, Ebdrup BH, Rasmussen JØ, Lindschou J, Gluud C, Glenthøj BY. Pharmacological interventions for benzodiazepine discontinuation in chronic benzodiazepine users. Cochrane Database of Systematic Reviews 2018, Issue 3. Art. No. : CD 011481. DOI: 10. 1002/14651858. CD 011481. pub 2. Busto, U. E. , Sykora, K. & Sellers, E. M. (1989). A clinical scale to assess benzodiazepine withdrawal. Journal of Clinical Psychopharmacology, 9 (6), 412– 416. Darker CD, Sweeney BP, Barry JM, Farrell MF, Donnelly‐Swift E. Psychosocial interventions for benzodiazepine harmful use, abuse or dependence. Cochrane Database of Systematic Reviews 2015, Issue 5. Art. No. : CD 009652. DOI: 10. 1002/14651858. CD 009652. pub 2. Gimeno, C. , Dorado, M. L. , Roncero, C. , Szerman, N. , Vega, P. , Balanzá-Martínez, V. , & Alvarez, F. J. (2017). Treatment of comorbid alcohol dependence and anxiety disorder: review of the scientific evidence and recommendations for treatment. Frontiers in psychiatry, 8, 1730. Kushner, M. G. , Maurer, E. W. , Thuras, P. , Donahue, C. , Frye, B. , Menary, K. R. , . . . & Van Demark, J. (2013). Hybrid cognitive behavioral therapy versus relaxation training for co-occurring anxiety and alcohol disorder: A randomized clinical trial. Journal of consulting and clinical psychology, 81(3), 429. Mc. Hugh, R. Kathryn. "Treatment of co-occurring anxiety disorders and substance use disorders. " Harvard review of psychiatry 23. 2 (2015): 99.

PTSD references • • • Goldstein, R. B. , Smith, S. M. , Chou, S. P. , Saha, T. D. , Jung, J. , Zhang, H. , . . . & Grant, B. F. (2016). The epidemiology of DSM-5 posttraumatic stress disorder in the United States: results from the National Epidemiologic Survey on Alcohol and Related Conditions-III. Social psychiatry and psychiatric epidemiology, 51(8), 1137 -1148. Hoskins, Mathew, et al. "Pharmacotherapy for post-traumatic stress disorder: systematic review and metaanalysis. " The British Journal of Psychiatry 206. 2 (2015): 93 -100. National Institute for Health and Care Excellence (2018). Post-traumatic stress disorder NG 116. (2018). London: National Institute for Health and Care Excellence. Petrakis, I. L. , Poling, J. , Levinson, C. , Nich, C. , Carroll, K. , Ralevski, E. , & Rounsaville, B. (2006). Naltrexone and disulfiram in patients with alcohol dependence and comorbid post-traumatic stress disorder. Biological Psychiatry, 60(7), 777 -783. Roberts, N. P. , Roberts, P. A. , Jones, N. , & Bisson, J. I. (2015). Psychological interventions for posttraumatic stress disorder and comorbid substance use disorder: A systematic review and meta-analysis. Clinical psychology review, 38, 25 -38.

ADHD - references • • • Crunelle, C. L. , Van Den Brink, W. , Moggi, F. , Konstenius, M. , Franck, J. , Levin, F. R. , . . . & Schellekens, A. (2018). International consensus statement on screening, diagnosis and treatment of substance use disorder patients with comorbid attention Deficit/Hyperactivity disorder. European addiction research, 24(1), 43 -51. Lee, N. K. , Jenner, L. , Harney, A. , & Cameron, J. (2018). Pharmacotherapy for amphetamine dependence: A systematic review. Drug and alcohol dependence. Martinez-Raga, J. , Knecht, C. , De Alvaro, R. , Szerman, N. , & Ruiz, P. (2013). Addressing dual diagnosis patients suffering from attention-deficit hyperactivity disorders and comorbid substance use disorders: A review of treatment considerations. Addictive Disorders & Their Treatment, 12(4), 213 -230. National Institute for Health and Care Excellence. (2018). Attention deficit hyperactivity disorder: diagnosis and management NG 87. • London: National Institute for Health and Care Excellence. Osland, S. , Hirsch, L. , & Pringsheim, T. (2017). Smoking, alcohol and drug use in youth and adults with attention-deficit hyperactivity disorder. BJPsych open, 3(3), 141 -146. Van de Glind, G. , van den Brink, W. , Koeter, M. W. , Carpentier, P. J. , van Emmerik-van Oortmerssen, K. , Kaye, S. , . . . & Moggi, F. (2013). Validity of the Adult ADHD Self-Report Scale (ASRS) as a screener for adult ADHD in treatment seeking substance use disorder patients. Drug and alcohol dependence, 132(3), 587 -596. van Emmerik‐van Oortmerssen, K. , van de Glind, G. , Koeter, M. W. , Allsop, S. , Auriacombe, M. , Barta, C. , . . . & Casas, M. (2014). Psychiatric comorbidity in treatment‐seeking substance use disorder patients with and without attention deficit hyperactivity disorder: results of the IASP study. Addiction, 109(2), 262 -272. van Emmerik-van Oortmerssen, K. , van de Glind, G. , van den Brink, W. , Smit, F. , Crunelle, C. L. , Swets, M. , & Schoevers, R. A. (2012). Prevalence of attention-deficit hyperactivity disorder in substance use disorder patients: a meta-analysis and meta-regression analysis. Drug and alcohol dependence, 122(1 -2), 11 -19. van Emmerik-van Oortmerssen, K. , Vedel, E. , Kramer, F. J. , Blankers, M. , Dekker, J. J. , van den Brink, W. , & Schoevers, R. A. (2019). Integrated cognitive behavioral therapy for ADHD in adult substance use disorder patients: results of a randomized clinical trial. Drug and alcohol dependence, 197, 28 -36.
- Slides: 68