Sublobar Resection and Intraoperative Brachytherapy for Lung Cancer

Sublobar Resection and Intraoperative Brachytherapy for Lung Cancer: ACOSOG Update Rodney J. Landreneau, MD Professor of Surgery The Heart Lung and Esophageal Surgery Institute University of Pittsburgh Medical Center Surgical Treatment of Lung Cancer Radiofrequency Ablation to VATS Lobectomy November 13 -14, 2008 Pittsburgh, Pennsylvania

Surgical Resection of the Lung Standard of Care for Peripheral Nodules 1940’s Pneumonectomy 1960’s Lobectomy 1990’s ? Segmentectomy/Wedge (and adjuvant local/systemic Rx)

Background ● Non-small cell lung carcinoma (NSCLC) identified in patients with impaired cardiopulmonary reserve creates important therapeutic challenges. ● Sublobar pulmonary resection is often utilized in these patients, however, local recurrence is high (15 -25%).
How Can Therapy to Customized for Patients with Poor Cardiopulmonary Reserve? ● Primary external beam radiation therapy - ? survival ● Chemotherapy - no defined role as primary therapy ● Radiofrequency Ablation - ? survival ● Sublobar resection with adjuvant radiation therapy
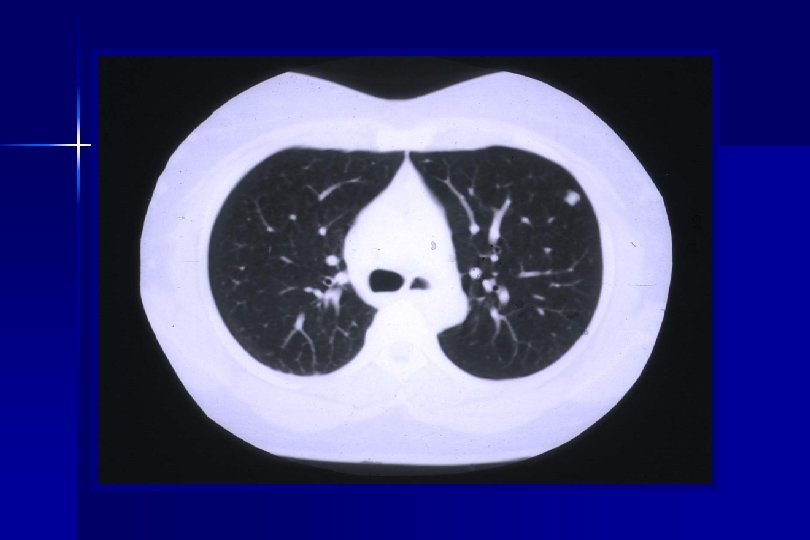
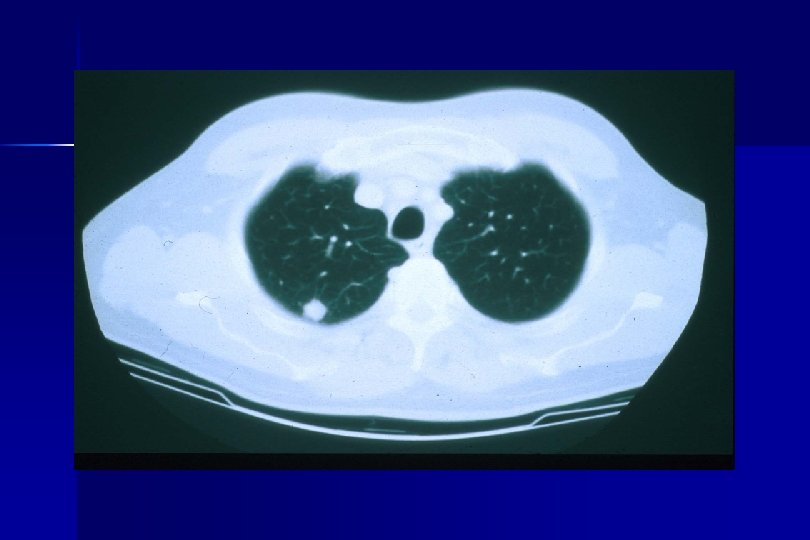

Background ● Postoperative (postop) external radiotherapy following sublobar resection is time consuming and can result in additional loss of pulmonary function. ● We review our experience using intraoperative 125 I lodine brachytherapy following sublobar resection of stage I NSCLC in patients with impaired cardiopulmonary reserve.

Methods ● From 1/1989 to 7/1994, 102 patients (mean age 69. 5 years) with pathologic stage I NSCLC and poor cardiopulmonary reserve (mean % predicated FEV 1 preop = 65%) underwent sublobar resection as primary therapy. ● We have since (1/1997 to 6/2002) introduced adjunctive intraoperative brachytherapy with 125 I to sublobar resection among 96 stage I patients with similar cardiopulmonary compromise (mean % predicted FEV 1 preop = 53%).
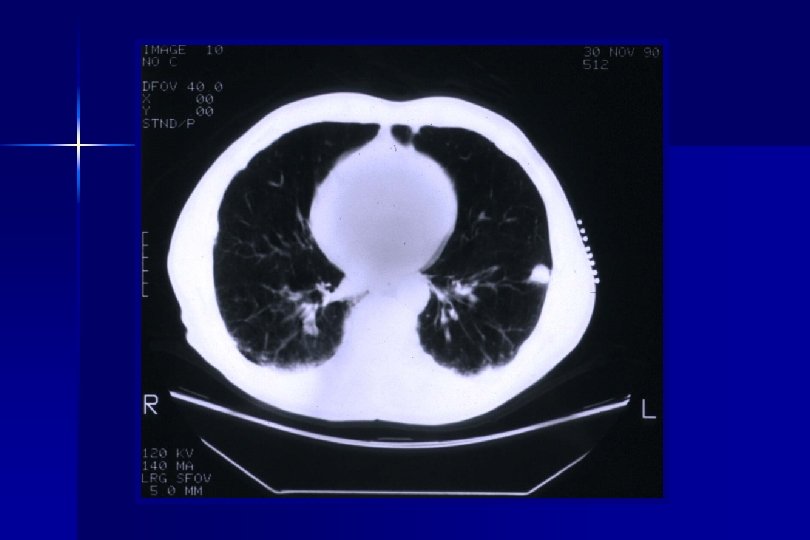

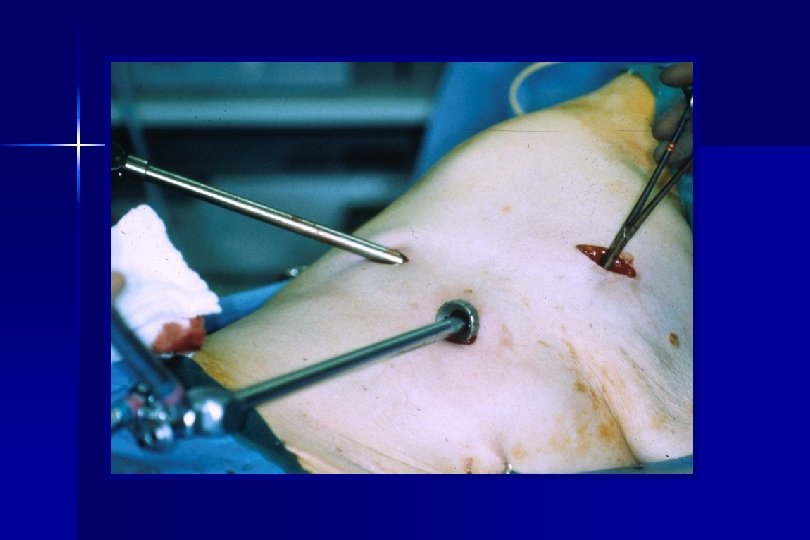
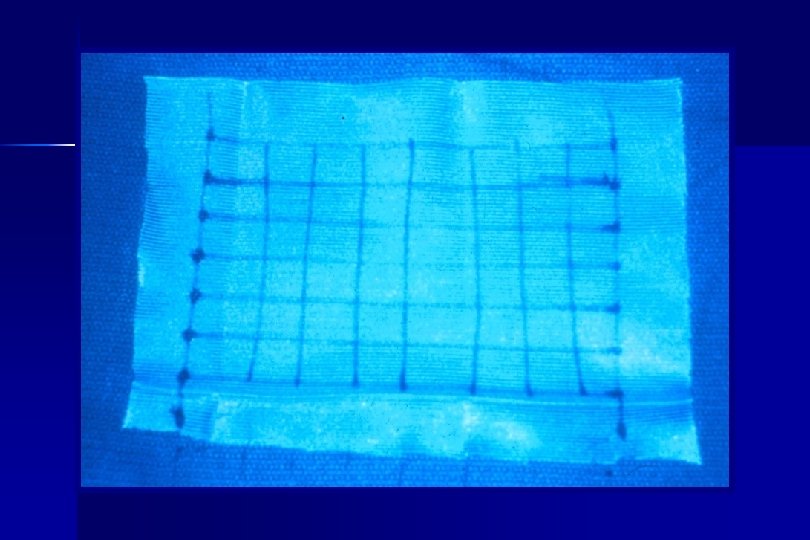
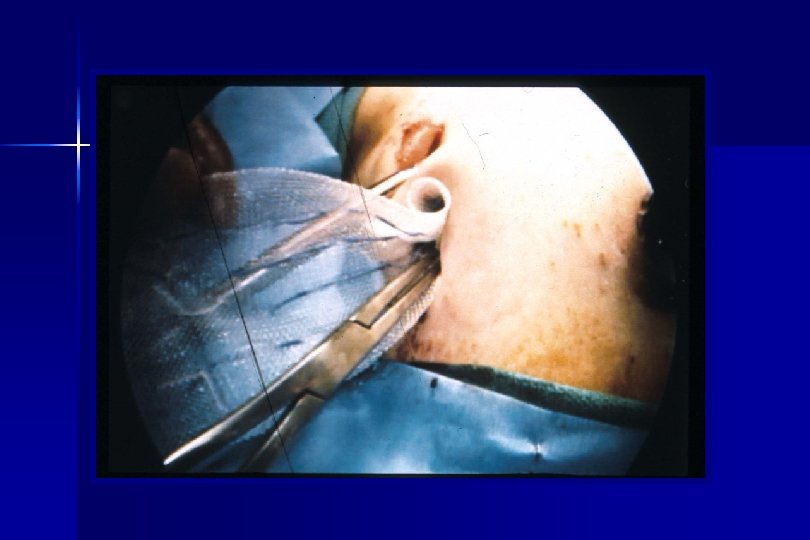
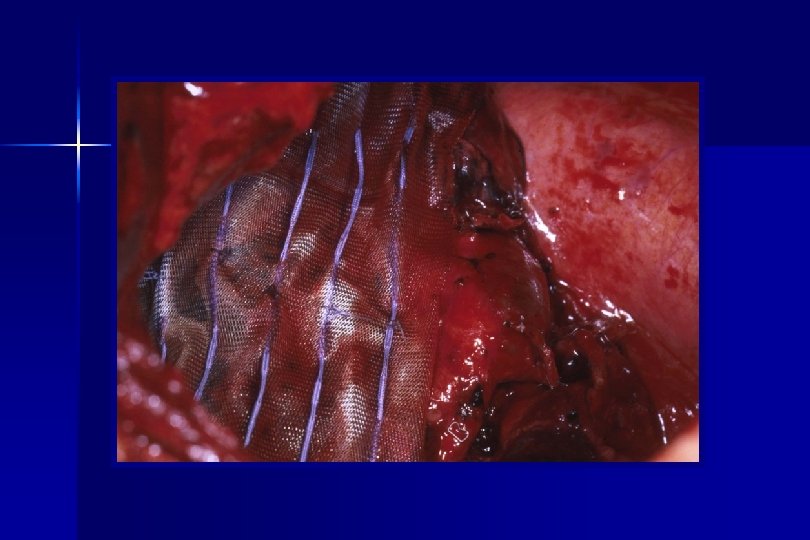
Methods ● After resection, a vicryl™ implant containing 125 I seeds, sewn at 1 cm² intervals, was placed over the resection staple line covering a 2 cm lateral margin. A local radiation does of 10, 000 c. Gy was delivered. ● No post-op patient isolation was required per national radiation safety guidelines ● Mortality and morbidity, local recurrence and disease free survival have been compared.

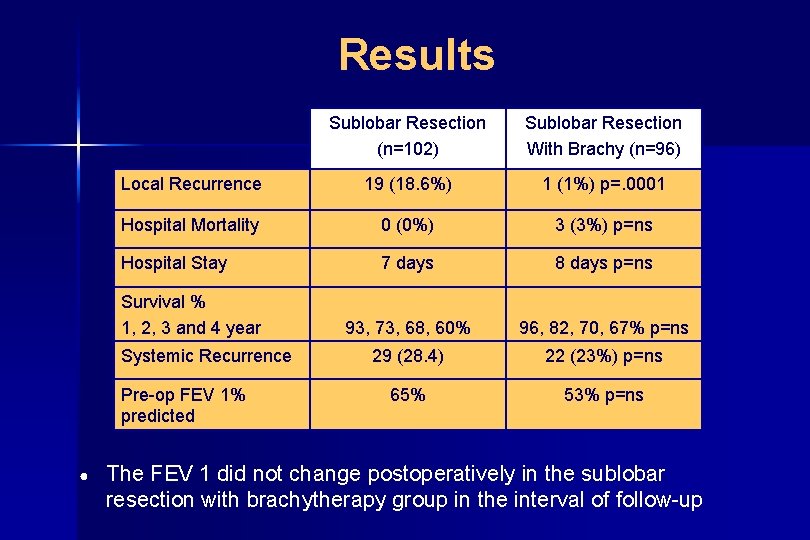
Results Sublobar Resection (n=102) Sublobar Resection With Brachy (n=96) Local Recurrence 19 (18. 6%) 1 (1%) p=. 0001 Hospital Mortality 0 (0%) 3 (3%) p=ns Hospital Stay 7 days 8 days p=ns 93, 73, 68, 60% 96, 82, 70, 67% p=ns 29 (28. 4) 22 (23%) p=ns 65% 53% p=ns Survival % 1, 2, 3 and 4 year Systemic Recurrence Pre-op FEV 1% predicted ● The FEV 1 did not change postoperatively in the sublobar resection with brachytherapy group in the interval of follow-up

Conclusions ● Local recurrence of NSCLC following sublobar resection with intra-operative 125 Ibrachytherapy (1%) appears to be less than following sublobar resection alone (18. 6%). ● This safe, pulmonary function preserving, and practical intra-operative brachytherapy method may be considered when sublobar resection is utilized as compromise therapy of stage I NSCLC.

ACOSOG Z 4032 Sublobar Resection vs. Sublobar Resection with Intraoperative Brachytherapy for High Risk Stage IA Non Small Cell Lung Cancer Patients
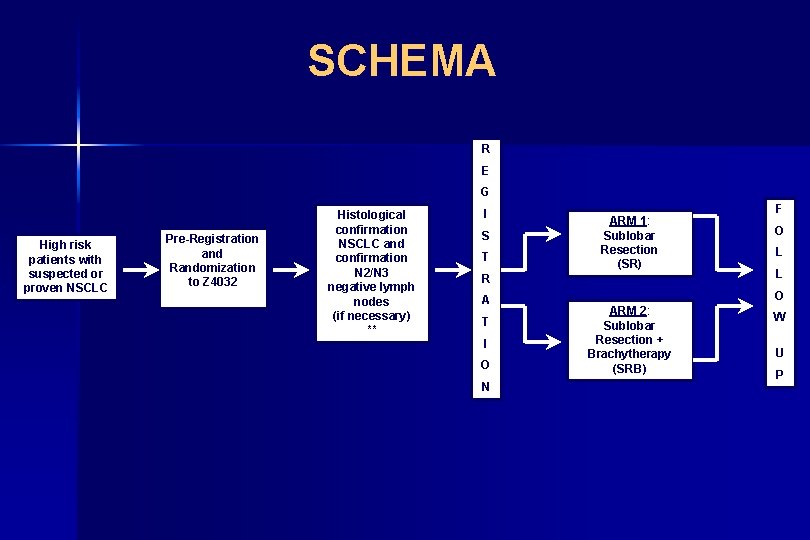
SCHEMA R E G High risk patients with suspected or proven NSCLC Pre-Registration and Randomization to Z 4032 Histological confirmation NSCLC and confirmation N 2/N 3 negative lymph nodes (if necessary) ** I S T ARM 1: Sublobar Resection (SR) F O L R L A O T I O N ARM 2: Sublobar Resection + Brachytherapy (SRB) W U P

Patient Selection

Eligibility Criteria Part I: Pre-Operative Criteria (Pre-Registration/Randomization): ● Patients must have a suspicious lung nodule for clinical Stage I NSCLC. ● Patient must have a mass ≤ 3 cm maximum diameter by CT size estimate: Clinical stage Ia or selected Ib (i. e. , with visceral pleural involvement. ● Patient must have a CT scan of the chest with upper abdomen within 60 days prior to date of pre-registration.

Eligibility Criteria Part I: Pre-Operative Criteria (Pre-Registration/Randomization): ● Patient must meet at least one major criteria or meet a minimum of two minor criteria as described below: Major Criteria - FEV 1 ≤ 50% predicted DLCO ≤ 50% predicted

Eligibility Criteria Part I: Pre-Operative Criteria (Pre-Registration/Randomization): Minor Criteria - Age ≥ 75 FEV 1 51 -60% predicated DLCO 51 -60% predicated Pulmonary hypertension (defined as a pulmonary artery systolic pressure greater than 40 mm. Hg) as estimated by echocardiography or right heart catheterization

Eligibility Criteria Part I: Pre-Operative Criteria (Pre-Registration/Randomization): Minor Criteria - Poor left ventricular function (defined as an ejection fraction of 40% or less) Resting or Exercise Arterial p. O 2 ≤ 55 mm Hg or Sp. O 2 ≤ 88% p. CO 2 45 mm Hg Modified Medical Research Council (MMRC) Dyspnea Scale ≥ 3

Eligibility Criteria Modified Medical Research Council Scale Grade Description 0 No breathlessness except with strenuous exercise 1 Breathlessness when hurrying on the level or walking up a slight hill 2 Walks slower than people of the same age on the level because of breathlessness or has to stop for breath when walking at own pace on the level 3 Stops for breath after walking about 100 yards or a few minutes on the level 4 Too breathless to leave the house or breathless when dressing or undressing

Eligibility Criteria Part I: Pre-Operative Criteria (Pre-Registration/Randomization): ● Patient must not have had previous intra-thoracic radiation therapy. ● Women of child-bearing potential must have negative serum or urine pregnancy test. ● No prior invasive malignancy, unless disease-free for ≥ 5 years prior to pre-registration (Exceptions: non-melanoma skin cancer, in-situ cancers).

Eligibility Criteria Part II: Intra-Operative Criteria (Registration): ● Patient must have biopsy-proven NSCLC. ● Patient must have all suspicious mediastinal lymph (>1 cm short-axis dimension on CT scan or positive on PET scan) assessed by one of the following methods to confirm negative involvement with NSCLC (Mediastinoscopy, endoesophageal ultrasound guided needle aspiration, CT-guided, video-assisted thoracoscopic or open lymph node biopsy).

ACOSOG Z 4032 Accrual Summary ● 174 Patients Accrued Nationally ● Accrual Goal is 226 Patients ● Estimated Study Closure - November 2009

Thank You
- Slides: 32