Subdural Hemorrhage SDH Rachel A Multz MS 4

Subdural Hemorrhage (SDH) Rachel A. Multz, MS 4 Bindu Setty, MD CT MRI

CASE HISTORY A 46 year old otherwise healthy female is brought to the ED following a motor vehicle accident in which she was the restrained driver. She is alert but agitated and complaining of headache.
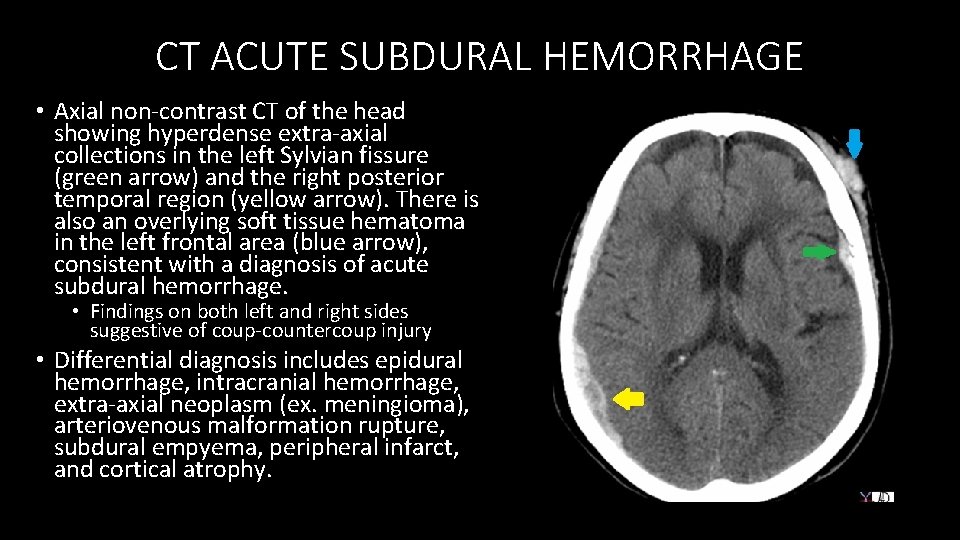
CT ACUTE SUBDURAL HEMORRHAGE • Axial non‐contrast CT of the head showing hyperdense extra‐axial collections in the left Sylvian fissure (green arrow) and the right posterior temporal region (yellow arrow). There is also an overlying soft tissue hematoma in the left frontal area (blue arrow), consistent with a diagnosis of acute subdural hemorrhage. • Findings on both left and right sides suggestive of coup‐countercoup injury • Differential diagnosis includes epidural hemorrhage, intracranial hemorrhage, extra‐axial neoplasm (ex. meningioma), arteriovenous malformation rupture, subdural empyema, peripheral infarct, and cortical atrophy.

CLINICAL FOLLOW UP The patient was medically stabilized and her mental status improved following hospitalization. Follow‐up imaging showed stabilization of bleeding with no residual focal neurologic deficits.

• General Characteristics • • IN A NUTSHELL Crescent‐shaped extra‐axial collection Does not cross dural reflections, but can cross suture lines In acute SDH, will appear homogenously hyperdense Travels diffusely along convexity of cerebral hemisphere (from anterior to posterior falx) • Other Associated Findings • Sulcal/ventricular effacement • Blurring of grey‐white junction • Typically unilateral, but can be bilateral • Potential Complications • Uncal/subfalcine herniation • Midline shift • Remember • In patients with low hemoglobin or platelets, SDH may appear isodense, even in the acute phase • Appearance on CT (and MR, as discussed later) changes over time as the clot ages

VOICE RAD: SUBDURAL HEMORRHAGE BY DR. SETTY
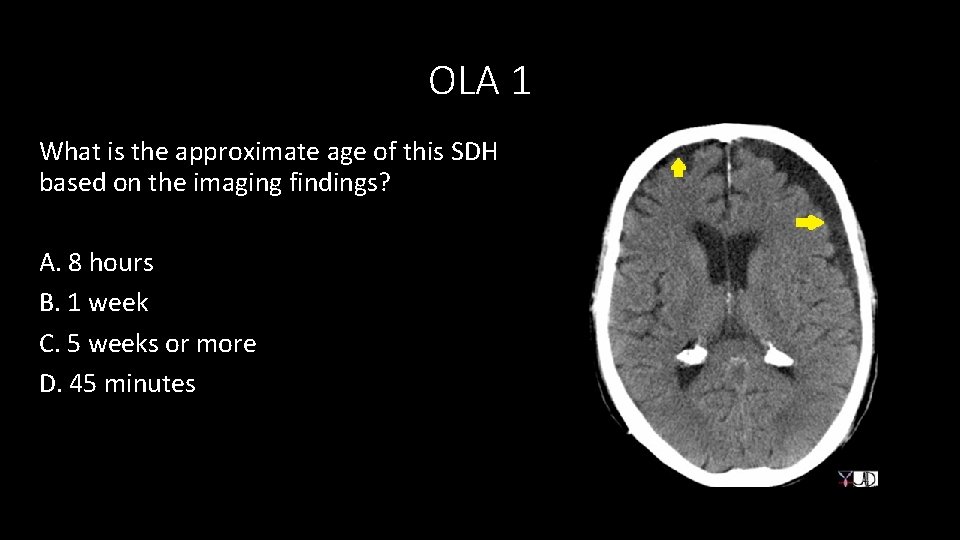
OLA 1 What is the approximate age of this SDH based on the imaging findings? A. 8 hours B. 1 week C. 5 weeks or more D. 45 minutes
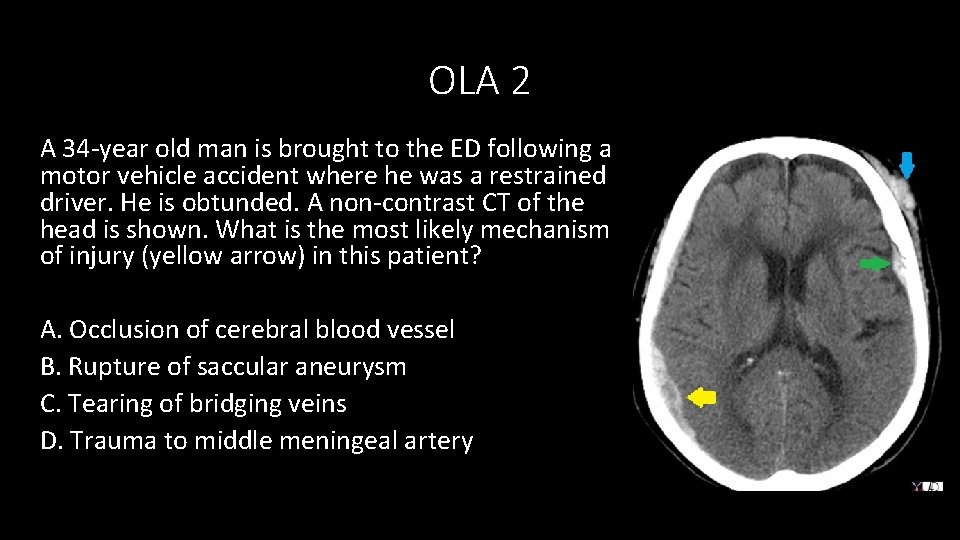
OLA 2 A 34‐year old man is brought to the ED following a motor vehicle accident where he was a restrained driver. He is obtunded. A non‐contrast CT of the head is shown. What is the most likely mechanism of injury (yellow arrow) in this patient? A. Occlusion of cerebral blood vessel B. Rupture of saccular aneurysm C. Tearing of bridging veins D. Trauma to middle meningeal artery

IMAGING SPECTRUM of SUBDURAL HEMORRHAGE Active Bleeding into SDH • Can have “swirled” appearance that is mixture of clot and active bleeding (swirl sign) • “Spot sign”: contrast extravasating into SDH on CTA • Predictor of hemorrhage expansion on follow‐ up imaging
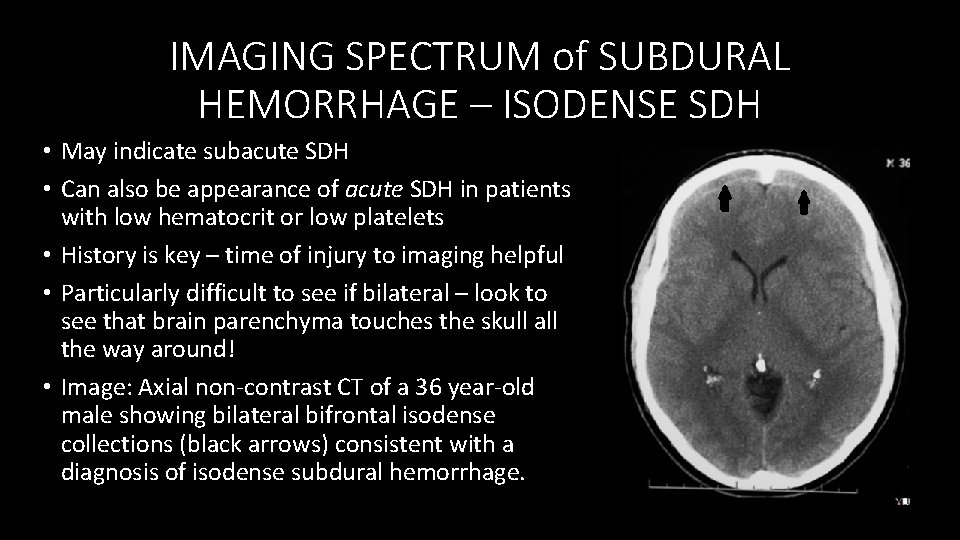
IMAGING SPECTRUM of SUBDURAL HEMORRHAGE – ISODENSE SDH • May indicate subacute SDH • Can also be appearance of acute SDH in patients with low hematocrit or low platelets • History is key – time of injury to imaging helpful • Particularly difficult to see if bilateral – look to see that brain parenchyma touches the skull all the way around! • Image: Axial non‐contrast CT of a 36 year‐old male showing bilateral bifrontal isodense collections (black arrows) consistent with a diagnosis of isodense subdural hemorrhage.
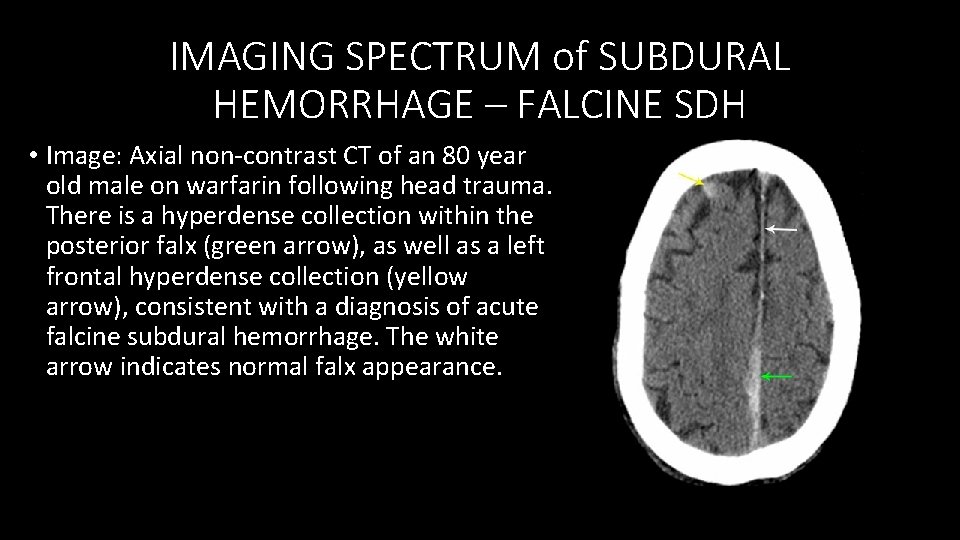
IMAGING SPECTRUM of SUBDURAL HEMORRHAGE – FALCINE SDH • Image: Axial non‐contrast CT of an 80 year old male on warfarin following head trauma. There is a hyperdense collection within the posterior falx (green arrow), as well as a left frontal hyperdense collection (yellow arrow), consistent with a diagnosis of acute falcine subdural hemorrhage. The white arrow indicates normal falx appearance.
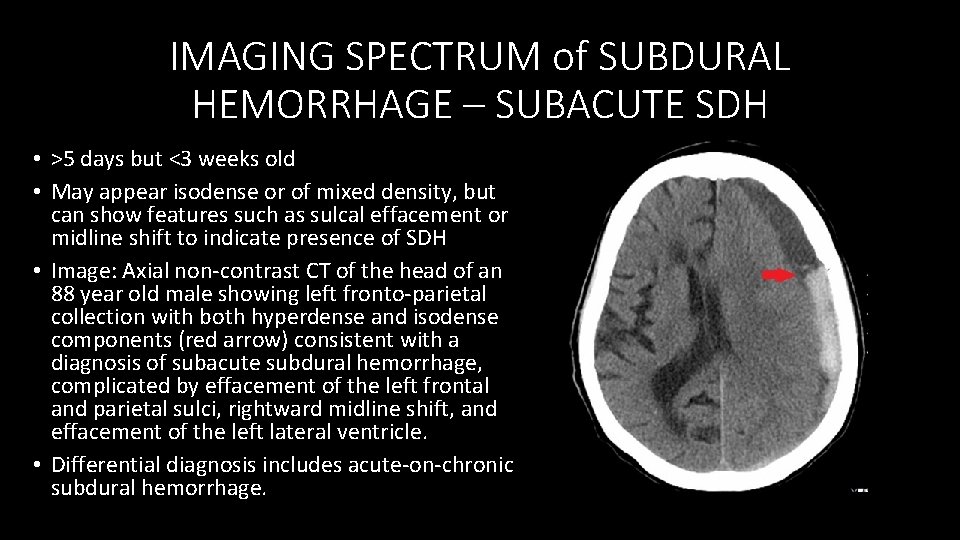
IMAGING SPECTRUM of SUBDURAL HEMORRHAGE – SUBACUTE SDH • >5 days but <3 weeks old • May appear isodense or of mixed density, but can show features such as sulcal effacement or midline shift to indicate presence of SDH • Image: Axial non‐contrast CT of the head of an 88 year old male showing left fronto‐parietal collection with both hyperdense and isodense components (red arrow) consistent with a diagnosis of subacute subdural hemorrhage, complicated by effacement of the left frontal and parietal sulci, rightward midline shift, and effacement of the left lateral ventricle. • Differential diagnosis includes acute‐on‐chronic subdural hemorrhage.

IMAGING SPECTRUM of CHRONIC SUBDURAL HEMORRHAGE Chronic SDH (a. k. a. Cystic Hygroma) • >3 weeks old • Hypodense crescentic extra‐axial fluid collection • Rarely, periphery may calcify • Image: Axial non‐contrast CT showing bilateral frontotemporal hypodense collections (yellow arrows) consistent with a diagnosis of chronic subdural hemorrhage.
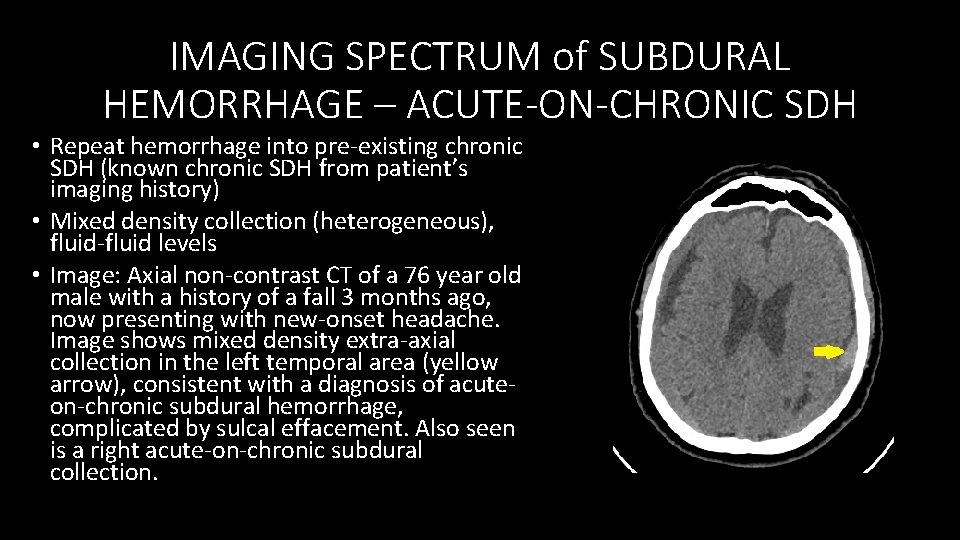
IMAGING SPECTRUM of SUBDURAL HEMORRHAGE – ACUTE-ON-CHRONIC SDH • Repeat hemorrhage into pre‐existing chronic SDH (known chronic SDH from patient’s imaging history) • Mixed density collection (heterogeneous), fluid‐fluid levels • Image: Axial non‐contrast CT of a 76 year old male with a history of a fall 3 months ago, now presenting with new‐onset headache. Image shows mixed density extra‐axial collection in the left temporal area (yellow arrow), consistent with a diagnosis of acute‐ on‐chronic subdural hemorrhage, complicated by sulcal effacement. Also seen is a right acute‐on‐chronic subdural collection.

IMAGING SPECTRUM of SUBDURAL HEMORRHAGE – POSTERIOR FOSSA SDH • Rare variant of SDH, typically as a result of trauma or anticoagulation • Occipital bone fracture • Removal of posterior fossa tumor • High mortality due to potential for brainstem compression and acute fourth ventricle obstruction • Image: Sagittal non‐contrast CT of an 81 year old female with altered mental status showing a hyperdense extra‐axial collection surrounding the posterior cerebellum (yellow arrow), consistent with a diagnosis of posterior fossa subdural hemorrhage, complicated by compression of the cerebellum.

IMAGING SPECTRUM of SDH MRI Evaluation of Subdural Hemorrhage Blood Product Time Magnetic Property Appearance on MRI Oxyhemoglobin Onset‐ 12 hrs Diamagnetic T 1 isointense T 2 iso‐ to hyperintense FLAIR hyperintense Deoxyhemoglobin 1‐ 7 days Paramagnetic T 1 iso‐ to hypointense T 2 hypointense FLAIR hyperintense Methemoglobin 5 days‐ months/years Paramagnetic T 1 hyperintense T 2 hyperintense FLAIR hyperintense Hemosiderin Weeks‐years Paramagnetic T 1 isointense (stable), hyperintense (re‐bleed) T 2 isointense (stable), hypointense (re‐bleed) FLAIR hyperintense FLAIR is the most sensitive sequence for detecting SDH on MRI
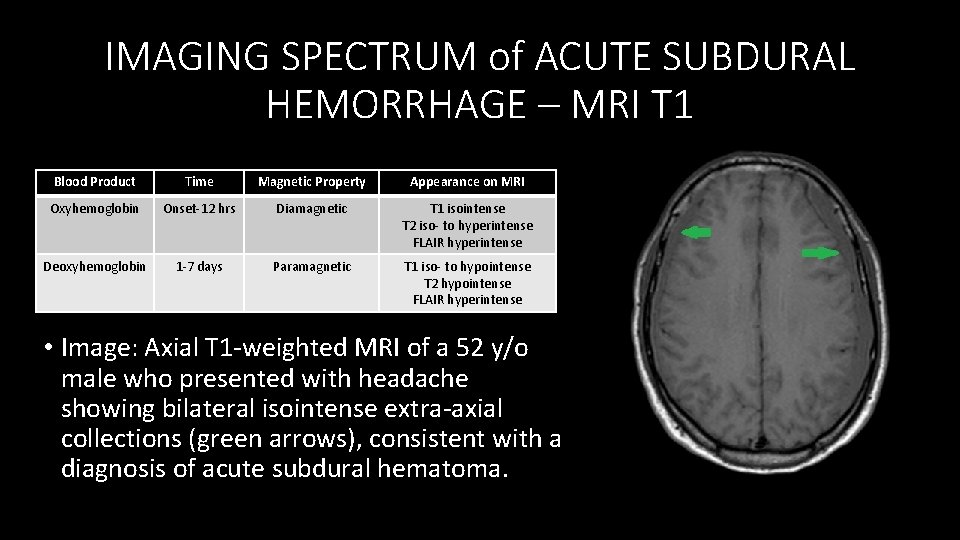
IMAGING SPECTRUM of ACUTE SUBDURAL HEMORRHAGE – MRI T 1 Blood Product Time Magnetic Property Appearance on MRI Oxyhemoglobin Onset‐ 12 hrs Diamagnetic T 1 isointense T 2 iso‐ to hyperintense FLAIR hyperintense Deoxyhemoglobin 1‐ 7 days Paramagnetic T 1 iso‐ to hypointense T 2 hypointense FLAIR hyperintense • Image: Axial T 1‐weighted MRI of a 52 y/o male who presented with headache showing bilateral isointense extra‐axial collections (green arrows), consistent with a diagnosis of acute subdural hematoma.
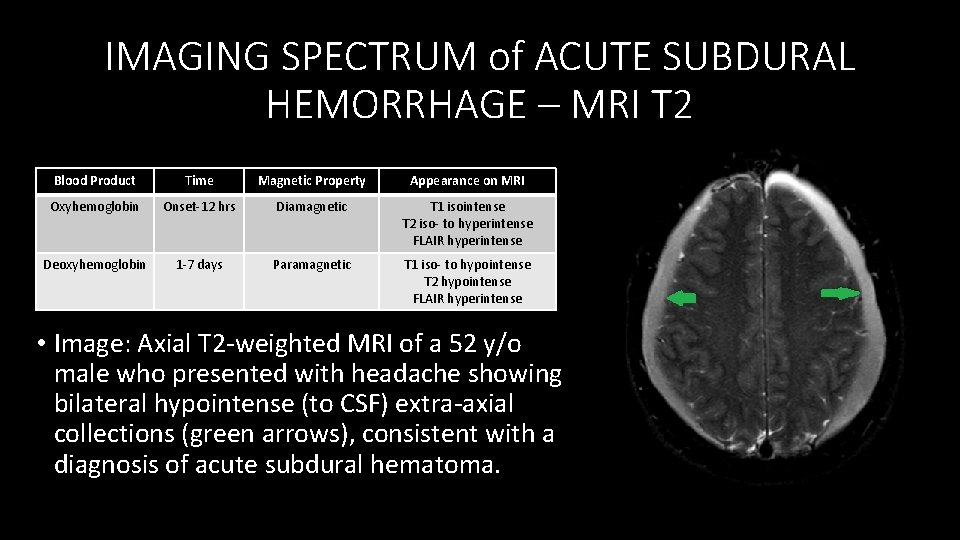
IMAGING SPECTRUM of ACUTE SUBDURAL HEMORRHAGE – MRI T 2 Blood Product Time Magnetic Property Appearance on MRI Oxyhemoglobin Onset‐ 12 hrs Diamagnetic T 1 isointense T 2 iso‐ to hyperintense FLAIR hyperintense Deoxyhemoglobin 1‐ 7 days Paramagnetic T 1 iso‐ to hypointense T 2 hypointense FLAIR hyperintense • Image: Axial T 2‐weighted MRI of a 52 y/o male who presented with headache showing bilateral hypointense (to CSF) extra‐axial collections (green arrows), consistent with a diagnosis of acute subdural hematoma.
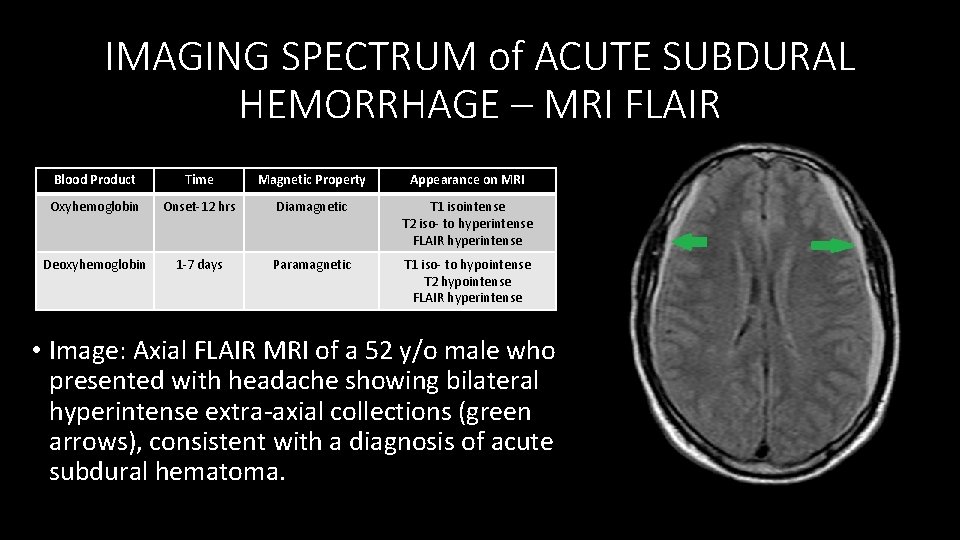
IMAGING SPECTRUM of ACUTE SUBDURAL HEMORRHAGE – MRI FLAIR Blood Product Time Magnetic Property Appearance on MRI Oxyhemoglobin Onset‐ 12 hrs Diamagnetic T 1 isointense T 2 iso‐ to hyperintense FLAIR hyperintense Deoxyhemoglobin 1‐ 7 days Paramagnetic T 1 iso‐ to hypointense T 2 hypointense FLAIR hyperintense • Image: Axial FLAIR MRI of a 52 y/o male who presented with headache showing bilateral hyperintense extra‐axial collections (green arrows), consistent with a diagnosis of acute subdural hematoma.
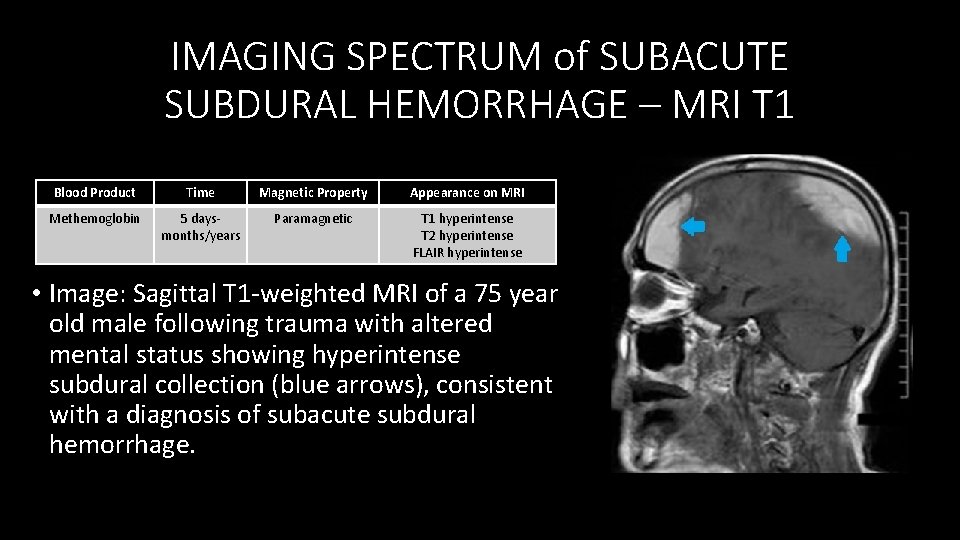
IMAGING SPECTRUM of SUBACUTE SUBDURAL HEMORRHAGE – MRI T 1 Blood Product Time Magnetic Property Appearance on MRI Methemoglobin 5 days‐ months/years Paramagnetic T 1 hyperintense T 2 hyperintense FLAIR hyperintense • Image: Sagittal T 1‐weighted MRI of a 75 year old male following trauma with altered mental status showing hyperintense subdural collection (blue arrows), consistent with a diagnosis of subacute subdural hemorrhage.
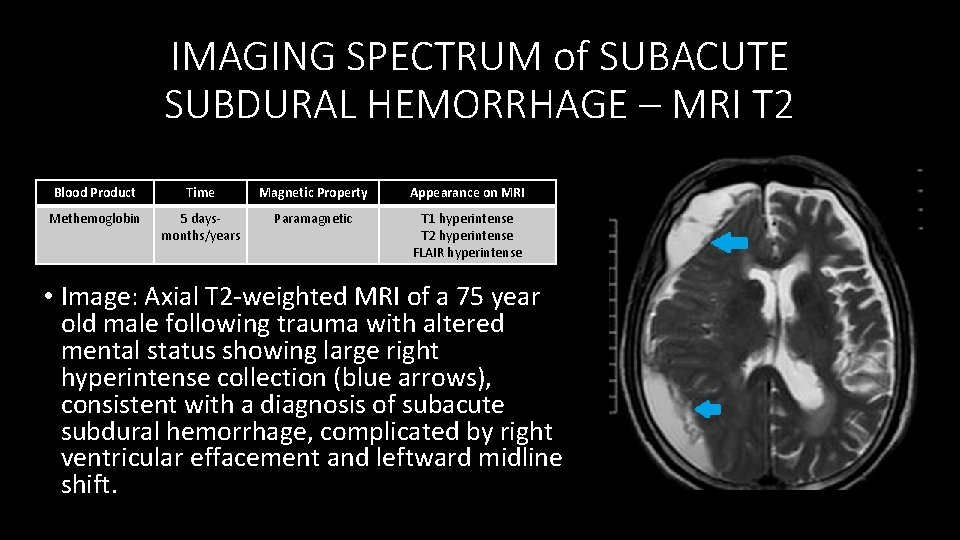
IMAGING SPECTRUM of SUBACUTE SUBDURAL HEMORRHAGE – MRI T 2 Blood Product Time Magnetic Property Appearance on MRI Methemoglobin 5 days‐ months/years Paramagnetic T 1 hyperintense T 2 hyperintense FLAIR hyperintense • Image: Axial T 2‐weighted MRI of a 75 year old male following trauma with altered mental status showing large right hyperintense collection (blue arrows), consistent with a diagnosis of subacute subdural hemorrhage, complicated by right ventricular effacement and leftward midline shift.
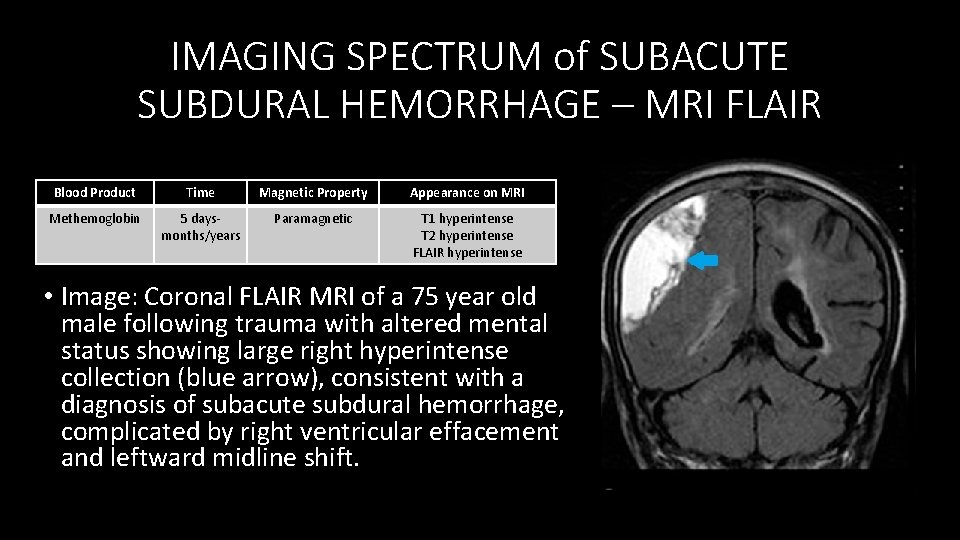
IMAGING SPECTRUM of SUBACUTE SUBDURAL HEMORRHAGE – MRI FLAIR Blood Product Time Magnetic Property Appearance on MRI Methemoglobin 5 days‐ months/years Paramagnetic T 1 hyperintense T 2 hyperintense FLAIR hyperintense • Image: Coronal FLAIR MRI of a 75 year old male following trauma with altered mental status showing large right hyperintense collection (blue arrow), consistent with a diagnosis of subacute subdural hemorrhage, complicated by right ventricular effacement and leftward midline shift.
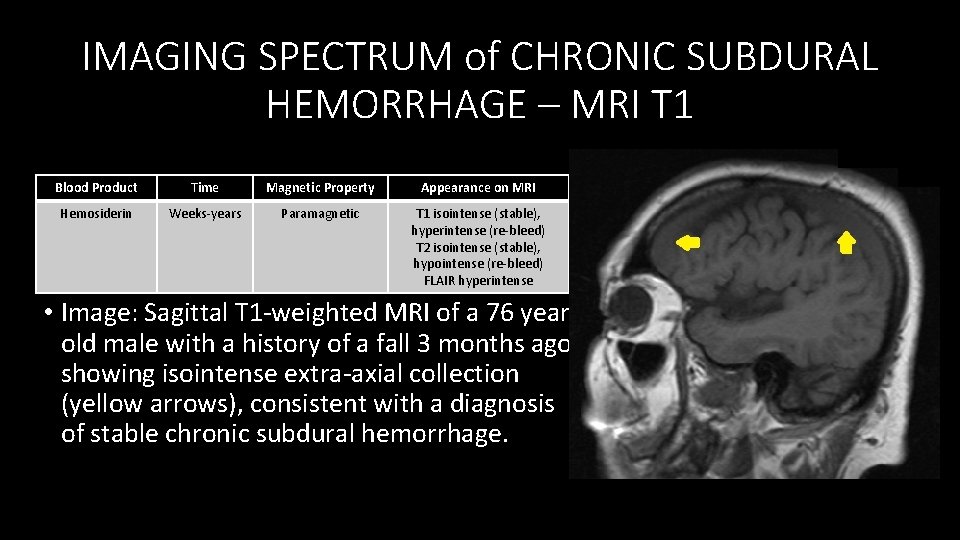
IMAGING SPECTRUM of CHRONIC SUBDURAL HEMORRHAGE – MRI T 1 Blood Product Time Magnetic Property Appearance on MRI Hemosiderin Weeks‐years Paramagnetic T 1 isointense (stable), hyperintense (re‐bleed) T 2 isointense (stable), hypointense (re‐bleed) FLAIR hyperintense • Image: Sagittal T 1‐weighted MRI of a 76 year old male with a history of a fall 3 months ago showing isointense extra‐axial collection (yellow arrows), consistent with a diagnosis of stable chronic subdural hemorrhage.
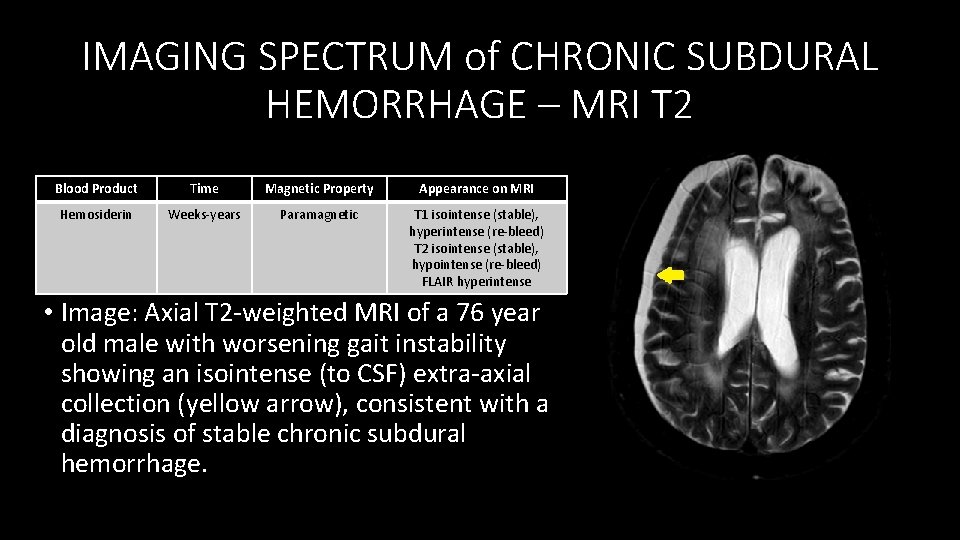
IMAGING SPECTRUM of CHRONIC SUBDURAL HEMORRHAGE – MRI T 2 Blood Product Time Magnetic Property Appearance on MRI Hemosiderin Weeks‐years Paramagnetic T 1 isointense (stable), hyperintense (re‐bleed) T 2 isointense (stable), hypointense (re‐bleed) FLAIR hyperintense • Image: Axial T 2‐weighted MRI of a 76 year old male with worsening gait instability showing an isointense (to CSF) extra‐axial collection (yellow arrow), consistent with a diagnosis of stable chronic subdural hemorrhage.
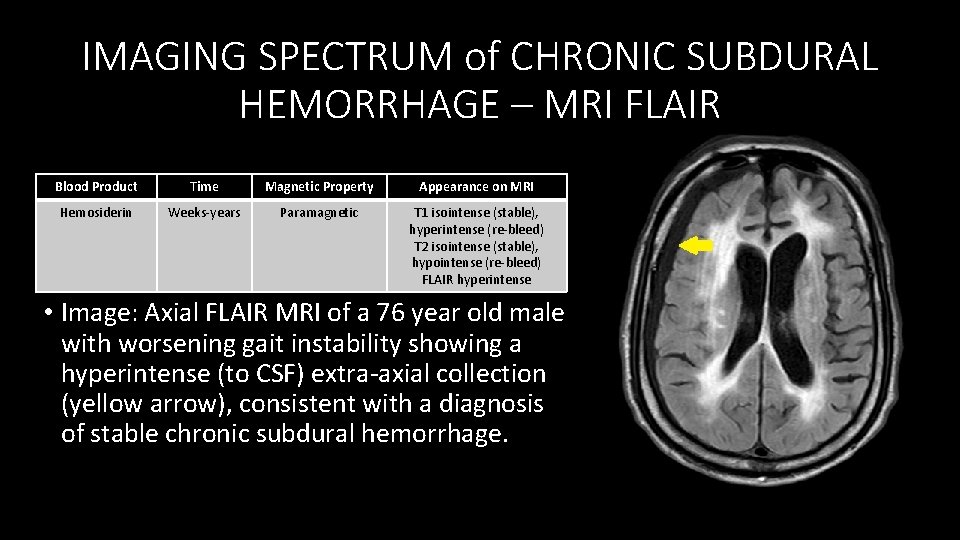
IMAGING SPECTRUM of CHRONIC SUBDURAL HEMORRHAGE – MRI FLAIR Blood Product Time Magnetic Property Appearance on MRI Hemosiderin Weeks‐years Paramagnetic T 1 isointense (stable), hyperintense (re‐bleed) T 2 isointense (stable), hypointense (re‐bleed) FLAIR hyperintense • Image: Axial FLAIR MRI of a 76 year old male with worsening gait instability showing a hyperintense (to CSF) extra‐axial collection (yellow arrow), consistent with a diagnosis of stable chronic subdural hemorrhage.
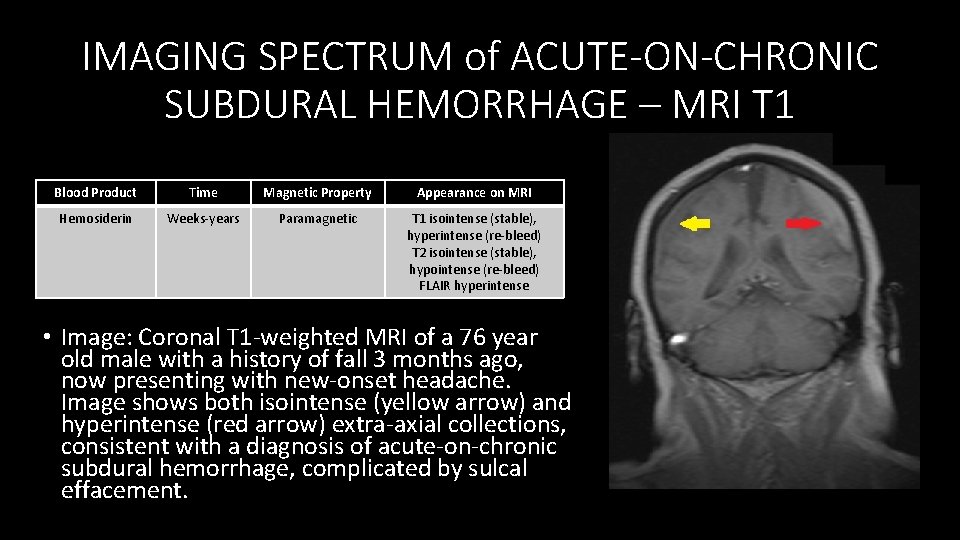
IMAGING SPECTRUM of ACUTE-ON-CHRONIC SUBDURAL HEMORRHAGE – MRI T 1 Blood Product Time Magnetic Property Appearance on MRI Hemosiderin Weeks‐years Paramagnetic T 1 isointense (stable), hyperintense (re‐bleed) T 2 isointense (stable), hypointense (re‐bleed) FLAIR hyperintense • Image: Coronal T 1‐weighted MRI of a 76 year old male with a history of fall 3 months ago, now presenting with new‐onset headache. Image shows both isointense (yellow arrow) and hyperintense (red arrow) extra‐axial collections, consistent with a diagnosis of acute‐on‐chronic subdural hemorrhage, complicated by sulcal effacement.
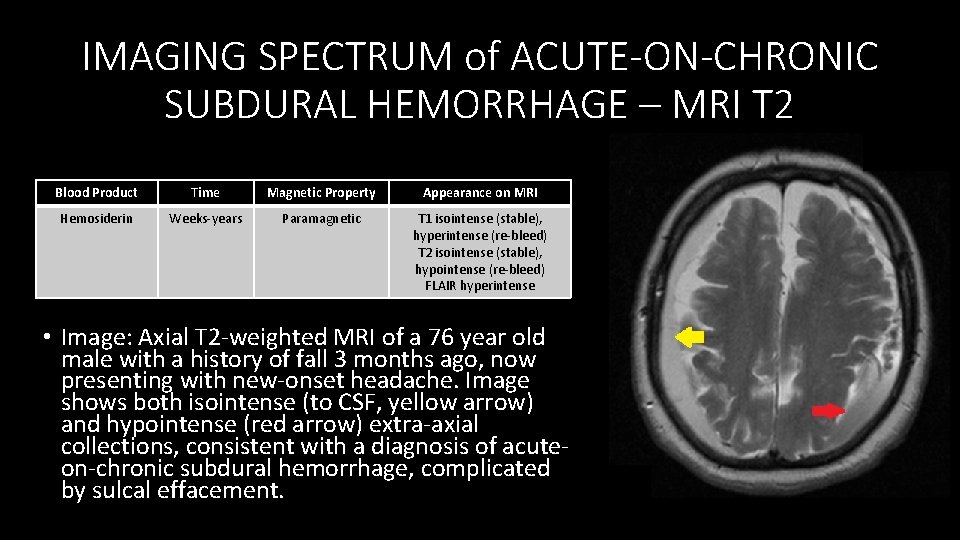
IMAGING SPECTRUM of ACUTE-ON-CHRONIC SUBDURAL HEMORRHAGE – MRI T 2 Blood Product Time Magnetic Property Appearance on MRI Hemosiderin Weeks‐years Paramagnetic T 1 isointense (stable), hyperintense (re‐bleed) T 2 isointense (stable), hypointense (re‐bleed) FLAIR hyperintense • Image: Axial T 2‐weighted MRI of a 76 year old male with a history of fall 3 months ago, now presenting with new‐onset headache. Image shows both isointense (to CSF, yellow arrow) and hypointense (red arrow) extra‐axial collections, consistent with a diagnosis of acute‐ on‐chronic subdural hemorrhage, complicated by sulcal effacement.

IMAGING SPECTRUM of ACUTE-ON-CHRONIC SUBDURAL HEMORRHAGE – MRI FLAIR Blood Product Hemosiderin Time Magnetic Property Appearance on MRI Weeks‐years Paramagnetic T 1 isointense (stable), hyperintense (re‐bleed) T 2 isointense (stable), hypointense (re‐bleed) FLAIR hyperintense • Image: Axial FLAIR MRI of a 76 year old male with a history of fall 3 months ago, now presenting with new‐onset headache. Image shows bilateral hyperintense extra‐axial collections (yellow arrows), consistent with a diagnosis of acute‐on‐chronic subdural hemorrhage, complicated by sulcal effacement. Appearance can be variable from one side to another.

DISCUSSION • Pathology of SDH • Tearing of the bridging veins as they drain into the dural sinuses • Trauma is most common cause (coup‐countercoup injury) • Abuse in children • Deceleration injury in adults • Fall or minor trauma in the elderly or those with other sources of cortical atrophy (ex. alcohol use disorder) • Less commonly caused by aneurysm rupture, arteriovenous malformation, or coagulopathy • ‘Typical’ Presentation • Most common = following trauma (asymptomatic or headache) • Patient may be anywhere from alert to unconscious depending on location and severity

DISCUSSION • BEST INITIAL TEST = NON-CONTRAST CT (best for seeing acute blood collection) • Also important to look for any overlying soft tissue swelling • Treatment • Surgical evacuation if acute and/or severe (mass effect, low GCS) • Mannitol to decrease intracranial pressure • Timing is the most important factor when evaluating SDH! • As time passes and clot dissolves, there is an evolving appearance of SDH on both CT and MRI corresponding to the breakdown of blood products.

LINKS AND REFERENCES • Consistent References: • https: //radiopaedia. org/articles/subdural‐haemorrhage? lang=us • https: //radiopaedia. org/articles/subdural‐haemorrhage‐summary? lang=us • https: //brain. thecommonvein. net/subdural‐hematoma/ • Other Journals and Texts • Brant WE, Helms CA. Fundamentals of Diagnostic Radiology. Lippincott Williams & Wilkins. (2007) ISBN: 0781761352. • Osborn AG. Handbook of Neuroradiology. Mosby Inc. (1991) ISBN: 0815165781. • Osborn AG et al. Diagnostic Imaging: Brain. Amirsys Inc. (2004) ISBN: 0721629059. • Miles J, Medlery AV. Posterior fossa subdural haematomas. J Neurol Neurosurg Psychiatry. 1974; 37(12): 1373‐ 1377. doi: 10. 1136/jnnp. 37. 12. 1373 • Gulsen S, Sonmez E, Yilmaz C, Altinors N. Traumatic acute subdural hematoma extending from the posterior cranial fossa to the cerebellopontine angle. J Korean Neurosurg Soc. 2009; 46(3): 277‐ 280. doi: 10. 3340/jkns. 2009. 46. 3. 277 • Kochi R, Mino M, Sonobe S, Yoshida M, Tominaga T. Spontaneous Development of Encapsulated Subdural Hematoma in the Posterior Cranial Fossa after Cardiac Surgery: A Case Report. NMC Case Rep J. 2018; 5(4): 87‐ 90. Published 2018 Sep 13. doi: 10. 2176/nmccrj. cr. 2017‐ 0230 • OLAS
- Slides: 31