STRUCTURE AND FUNCTION OF BONE JOINTS AND CONNECTIVE

STRUCTURE AND FUNCTION OF BONE, JOINTS AND CONNECTIVE TISSUE

�CLASSIFICATION OF JOINTS �Human joints provide the structures by which bones join with one another and may be classified according to the histologic features of the union and the range of joint motion. There are three classes of joint design: � (1) synovial or diarthrodial joints which articulate with free movement, have a synovial membrane lining the joint cavity, and contain synovial fluid; � (2) amphiarthroses, in which adjacent bones are separated by articular cartilage or a fibrocartilage disk and are bound by firm ligaments permitting limited motion (e. g. , pubic symphysis, intervertebral disks of vertebral bodies, distal tibiofibular articulation, and sacroiliac joint articulation with pelvic bones);

� 3) synarthroses, which are found only in the skull (suture lines) where thin, fibrous tissue separates adjoining cranial plates that interlock to prevent detectable motion before the end of normal growth, yet permit growth in childhood and adolescence. �The synovial joints are classified further according to their shapes, which include ball-and-socket (hip), hinge (interphalangeal), saddle (first carpometacarpal), and plane (patellofemoral) joints. These configurations reflect the varying functions, as the shapes and sizes of the opposing surfaces determine the direction and extent of motion.

PRESENTING PROBLEMS IN MUSCULOSKELETAL DISEASE Pain in a single joint �Principal causes of acute monoarthritis in a previously normal joint �Septic arthritis �Crystal synovitis: gout, pseudogout �Monoarticular presentation of oligo- or polyarthritis �Reactive, psoriatic or other seronegative spondarthritis �Erythema nodosum �Rheumatoid arthritis �Juvenile idiopathic arthritis �Trauma: especially if associated with haemarthrosis �Haemarthrosis associated with clotting abnormality �Foreign body reaction (e. g. plant thorn)

Oligoarthritis �Oligoarthritis affects 2 -4 joints or joint groups (the wrist has many joints but counts as a single site). �Causes of inflammatory oligoarthritis. �Seronegative spondyloarthritis � Reactive arthritis � Psoriatic arthritis � Ankylosing spondylitis � Enteropathic arthritis �Erythema nodosum �Juvenile idiopathic arthritis �Oligoarticular presentation of polyarthritis �Infection, including � Infective endocarditis � Neisseria � Mycobacteria
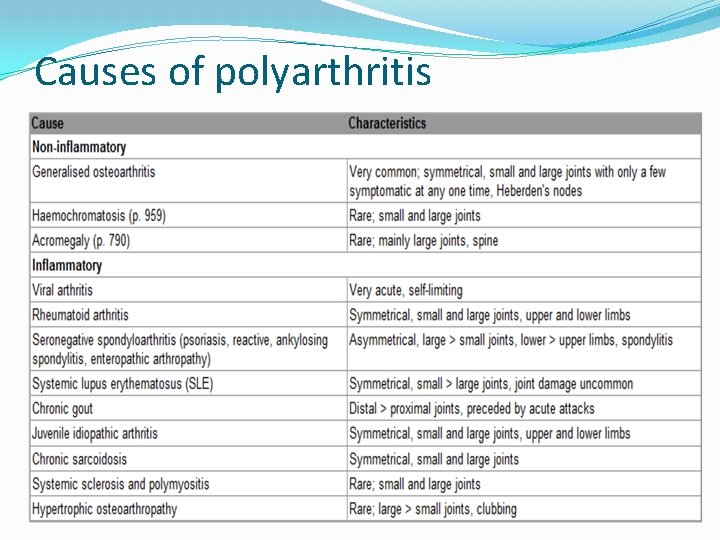
Causes of polyarthritis
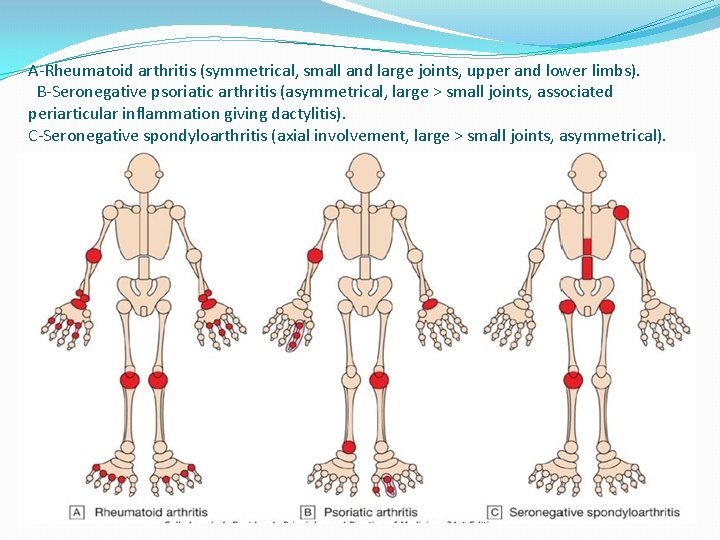
A-Rheumatoid arthritis (symmetrical, small and large joints, upper and lower limbs). B-Seronegative psoriatic arthritis (asymmetrical, large > small joints, associated periarticular inflammation giving dactylitis). C-Seronegative spondyloarthritis (axial involvement, large > small joints, asymmetrical).

MATURE ARTICULAR CARTILAGE �Articular cartilage is a specialized connective tissue that covers the weight-bearing surfaces of diarthrodial joints. � The principal functions of cartilage layers covering bone ends are to permit low-friction, high-velocity movement between bones, to absorb the transmitted forces associated with locomotion, and to contribute to joint stability. �Lubrication by synovial fluid provides frictionless movement of the articulating cartilage surfaces.

�Chondrocytes are the single cellular component of adult hyaline articular cartilage and are responsible for synthesizing and maintaining the highly specialized cartilage matrix macromolecules. �The cartilage extracellular matrix is composed of an extensive network of collagen fibrils, which confers tensile strength, and an interlocking mesh of proteoglycans, which provides compressive stiffness through the ability to absorb and extrude water. �The cartilage is avasculare and aneural.

�Numerous other noncollagenous proteins also contribute to the unique properties of cartilage , (Collagens, Proteoglycans, Other Noncollagenous Proteins (Structural), Or (Regulatory). � Proper distribution and relative composition of these proteins is required for the function of cartilage in protecting the subchondral bone from adverse environmental influences.

�As the single cellular component in adult articular cartilage, chondrocytes are responsible for maintaining the ECM components in a low-turnover state. The composition and organization of matrix macromolecules, unique to this tissue, are determined during chondrocyte differentiation in embryonic and postnatal development of cartilage. �Adult chondrocytes exist in a hypoxic environment within articular cartilage. They are inactive metabolically, partially as a result of an absence of blood vessels and nerves, and display a rounded morphology that reflects their quiescent state.

�Chondrocyte culture models have been developed with the aim of maintaining differentiated phenotypes, characterized by the major collagen and proteoglycan constituents, type II collagen and aggrecan. Chondrocytes interact with specific ECM components via integrins, annexins, and CD 44 on the cell surface.

�The subchondral bone plate beneath the calcified base of articular cartilage may have many effects on the cartilage above it. Its stiffness modifies the compressive forces to which articular cartilage is subjected, its blood supply may be important in cartilage nutrition , and its cells may produce peptides that regulate chondrocyte function.

�Several studies have suggested that the responses of the subchondral bone to mechanical stimulation may transmit signals into the articular cartilage. Tidemark advancement with thickening of the calcified cartilage and thinning of articular cartilage is associated with fibrillation of the cartilage surface during aging.
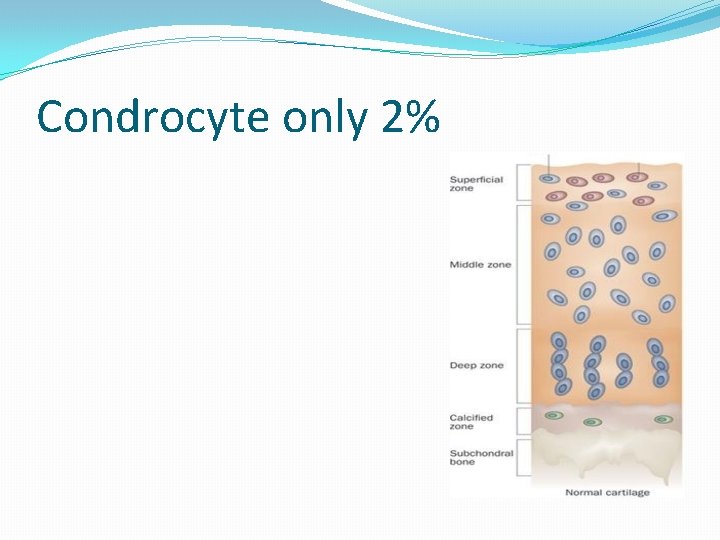
Condrocyte only 2%

SYNOVIAL FLUID AND NUTRITION OF JOINT STRUCTURES �The volume and composition of synovial fluid are determined by the properties of the synovium and its vasculature. �Fluid in normal joints is present in small quantities (2. 5 m. L in the normal knee) sufficient to coat the synovial surface, but not to separate one surface from the other. � Tendon sheath fluid and synovial fluid are biochemically similar. Both are essential for the nutrition and lubrication of adjacent avascular structures, including tendon and articular cartilage, and for limiting adhesion formation, maintaining movement.

�The synovial joint is uniquely adapted to responding to environmental and mechanical demands. The synovial lining is composed of two to three cell layers, and there is no basement membrane separating the lining cells from the underlying connective tissue. �The synovium produces synovial fluid, which provides nutrition and lubrication to the avascular articular cartilage

SYSTEMIC REGULATION OF BONE REMODELING �CALCIUM METABOLISM �Calcium is crucial to many processes in the body, including most signaling cascades and synaptic signaling, creating a requirement for tight control of systemic calcium concentrations. the skeleton is the reservoir for calcium, and bone remodeling is one of the processes crucial to calcium regulation. Hormones involved in calcium homeostasis have profound effects on the skeleton.

Parathyroid hormone �The primary function of PTH is to maintain serum ionized calcium levels within a narrow physiologic range. PTH secretion increases as calcium levels decrease to less than 8 mg/d. L, controlled by decreased binding of the calcium ion to the calcium receptor on the parathyroid cell. When a serum calcium value greater than 10 mg/d. L accompanies a high level of serum PTH, a diagnosis of hyperparathyroidism can be made. Other circulating factors, such as vitamin D, tumor necrosis factor-α, and prostaglandins, also are involved in regulating calcium balance.

�Vitamin D has effects on bone remodeling and calcium homeostasis. A 10 -minute exposure of the skin to ultraviolet light from the sun causes endogenous production of sufficient quantities of vitamin D 3 from 7 dehydrocholesterol to allow normal calcium balance. Vitamin D 3 is first hydroxylated to 25 -hydroxyvitamin D in the liver, followed by 25 -hydroxyvitamin D hydroxylation in the kidney. Often referred to as calcitriol, the active metabolite, 1, 25 -dihydroxyvitamin D, stimulates intestinal absorption of calcium, providing the mineral necessary to build bone.

�supraphysiologic levels induce bone resorption by stimulating the differentiation of osteoclast precursors. � This occurs through the effect of 1, 25 dihydroxyvitamin D of increasing bone stromal cell production of M-CSF and RANKL expression. �Besides the role of vitamin D in ensuring calcium acquisition from the intestine, vitamin D has subtle effects on the formation and resorption of bone.

�STIFFNESS �Stiffness is a common complaint among patients with arthritis. What is meant by stiffness varies from patient to patient, however. Some patients may use the term stiffness to refer to pain, soreness, weakness, fatigue, or limitation of motion. �Rheumatologists generally use the term stiffness to describe discomfort and limitation on attempted movement of joints after a period of inactivity. This “gel” phenomenon occurs usually after an hour or more of inactivity. The duration of stiffness related to inactivity varies, with mild stiffness lasting minutes to severe stiffness lasting hours.
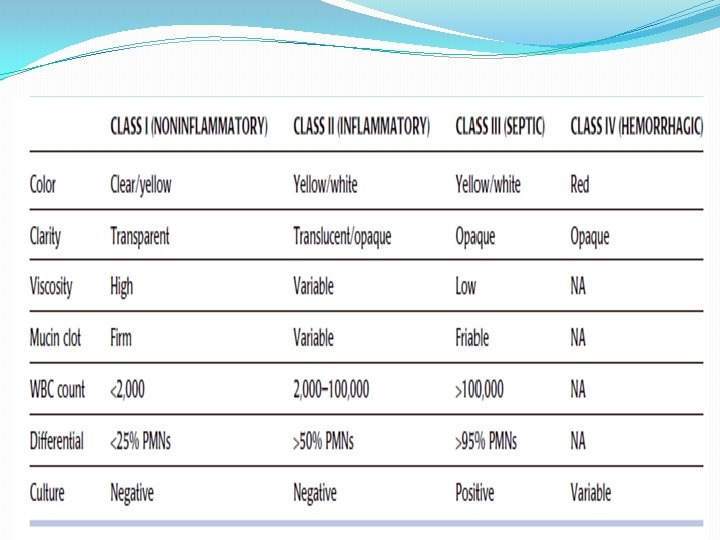
SYNOVIAL FLUID ANALYSIS
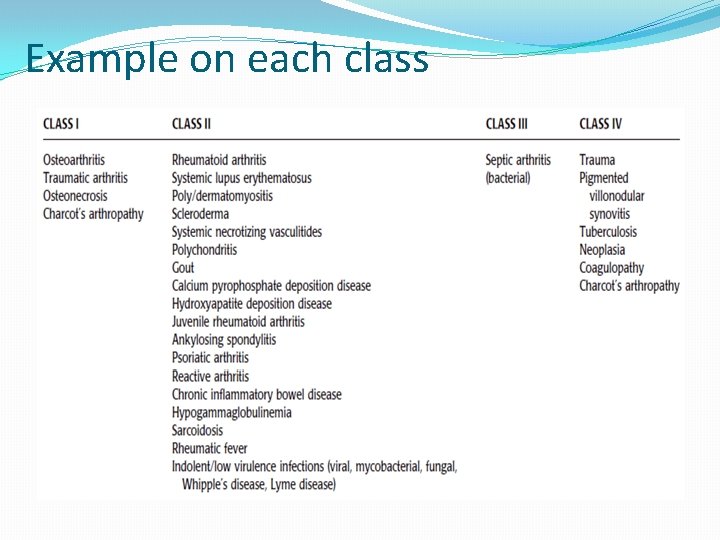
Example on each class

Cell Count �The WBC count and differential are among the most valuable diagnostic characteristics of SF. Normal SF contains fewer than 200 cells/mm 3. � SF from noninflammatory arthropathies may have WBC counts of up to 2000 cells/mm 3. � Noninfectious inflammatory arthropathies have WBC counts that vary widely, ranging from 2000 to 100, 000 cells/mm 3. � Although the autoimmune arthropathies generally present with WBC counts of 2000 to 30, 000 cells/mm 3, cell counts of 50, 000/mm 3 or higher are not unusual in RA.

�Patients with crystal induced arthritis, such as acute gout, usually have WBC counts of greater than 30, 000 cells/mm 3 and counts of 50, 000 to 75, 000 cells/mm 3 are common. �The closer the WBC count gets to 100, 000 cells/mm 3, the greater the likelihood of a septic arthritis. Although a rare patient with crystal-induced arthropathy, RA, or even a seronegative arthropathy may have a WBC count greater than 100, 000 cells/mm 3, such patients should be treated empirically for a septic joint until microbiologic data exclude infection. �A WBC count of less than 100, 000 cells/mm 3 does not preclude the possibility of infection.
- Slides: 26