Stroke Time is Brain Janet Liefso Acute Stroke

Stroke Time is Brain Janet Liefso Acute Stroke Coordinator 1

Acknowledgement to: Richard Wilson Linda Kelloway Andrea Fisher Work revised by: Janet Liefso, 2010 2

Objectives For Session • Increase Stroke Recognition - signs and symptoms • Review Basic Neuroanatomy – the implications of stroke location • Review complications 3

4

Jim • 67 year old semi- retired accountant married to Laura. From Niagara region - visiting friends in Teeswater • Suddenly at 2100 hours wife witnessed right arm weakness and leg weakness, unable to get up on own, speech slurred • Wife called 911 - paramedics responded and redirected Jim to Goderich Hospital on stroke protocol- arrived at 2130. • Diagnosed as an ischemic stroke- given t. PA at new telestroke site at 2220 5

What Happened? 6

Stroke is a Brain Attack • Abrupt development of a focal neurological deficit as a consequence of a local disturbance in the cerebral circulation 7

Know the Warning Signs of Stroke • • • Sudden Weakness Sudden Trouble Speaking Sudden Vision Problems Sudden Headache Sudden Dizziness (especially with any of the above signs) 8

Stroke is undoubtedly one of the most devastating events experienced by humans “Many stroke victims would rather die than live without their dignity and quality of life” Bahle, J. (1998). 9

Key Message Stroke is an Emergency Act Fast *6 Million Neurons a Minute are lost Time is Brain Dr. Lownie 10
Basic Neuro-anatomy 11
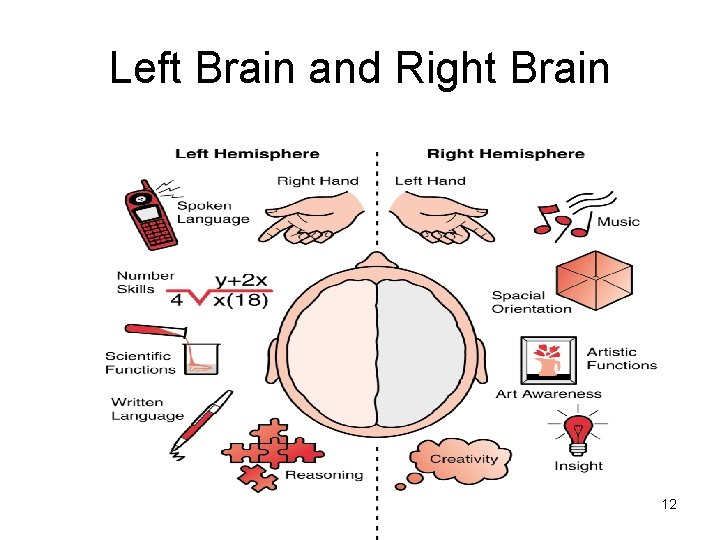
Left Brain and Right Brain 12
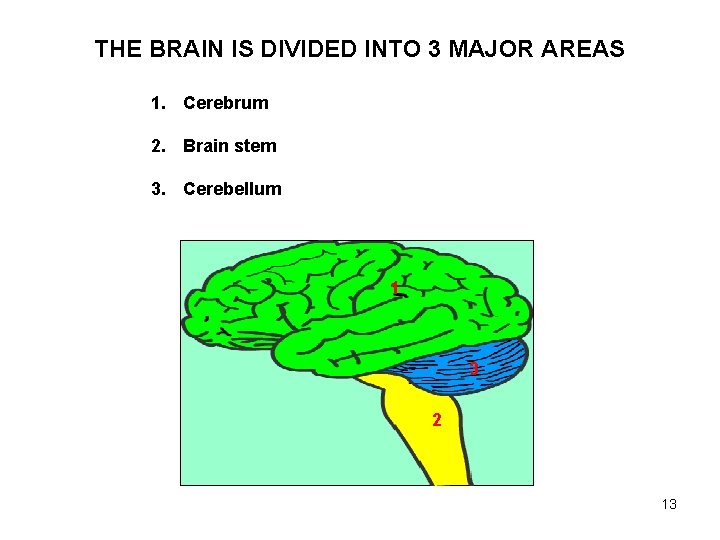
THE BRAIN IS DIVIDED INTO 3 MAJOR AREAS 1. Cerebrum 2. Brain stem 3. Cerebellum 1 3 2 13
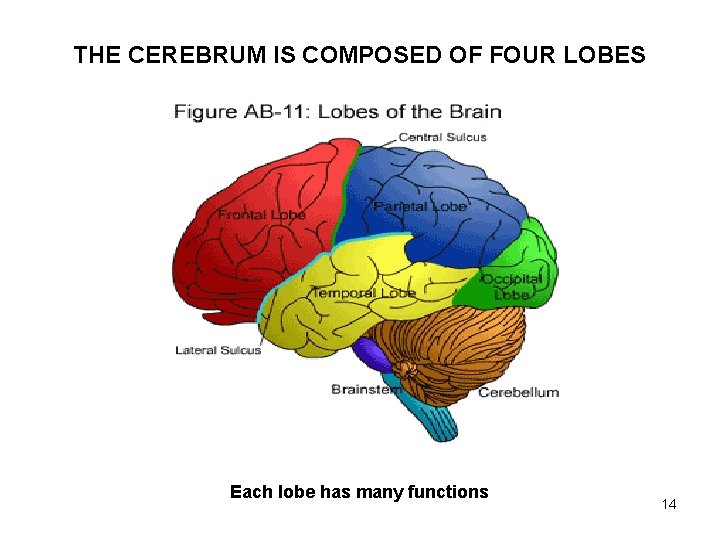
THE CEREBRUM IS COMPOSED OF FOUR LOBES Each lobe has many functions 14
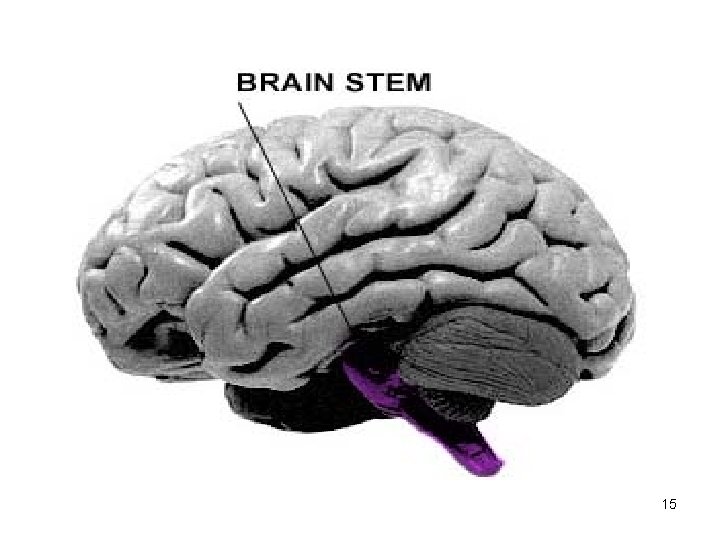
15
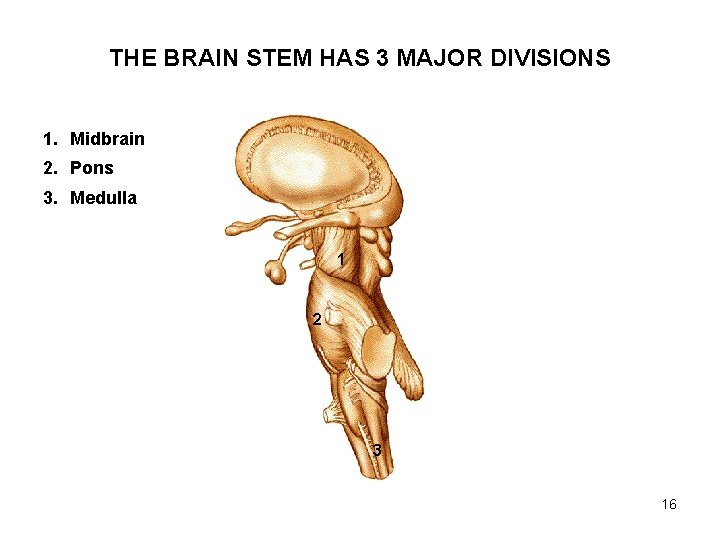
THE BRAIN STEM HAS 3 MAJOR DIVISIONS 1. Midbrain 2. Pons 3. Medulla 1 2 3 16
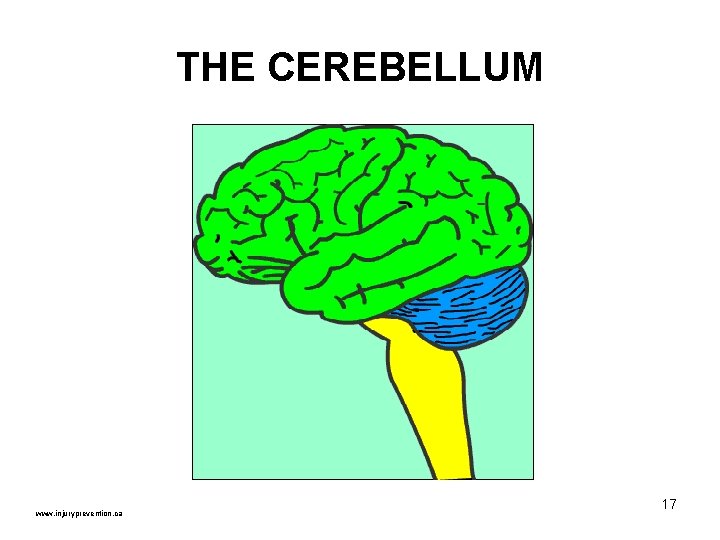
THE CEREBELLUM www. injuryprevention. ca 17

Follow the circulation to the brain in the following slides…. 18
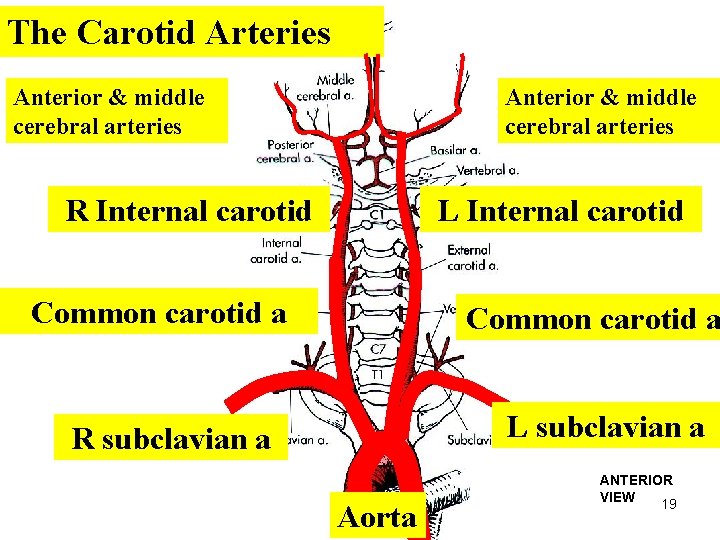
The Carotid Arteries Anterior & middle cerebral arteries R Internal carotid L Internal carotid Common carotid a L subclavian a R subclavian a Aorta ANTERIOR VIEW 19
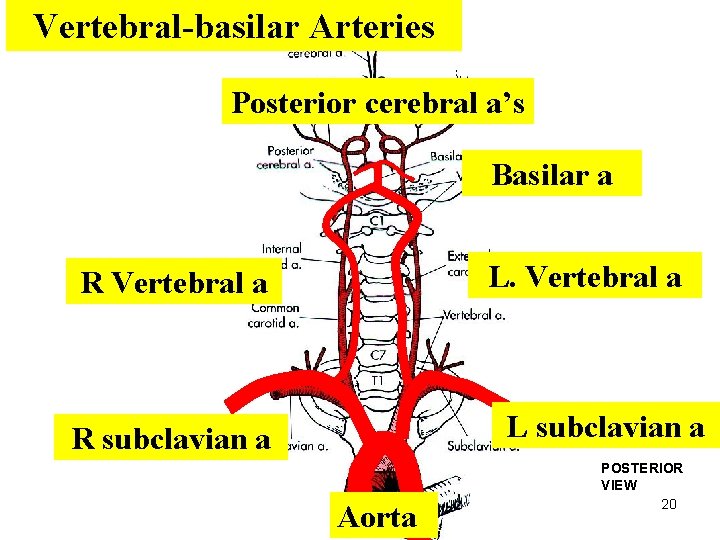
Vertebral-basilar Arteries Posterior cerebral a’s Basilar a L. Vertebral a R Vertebral a L subclavian a R subclavian a Aorta POSTERIOR VIEW 20
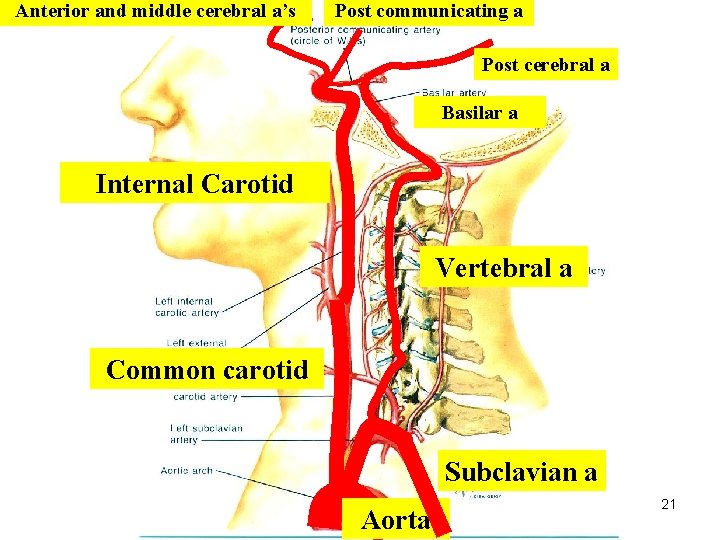
Anterior and middle cerebral a’s Post communicating a Post cerebral a Basilar a Internal Carotid Vertebral a Common carotid Subclavian a Aorta 21
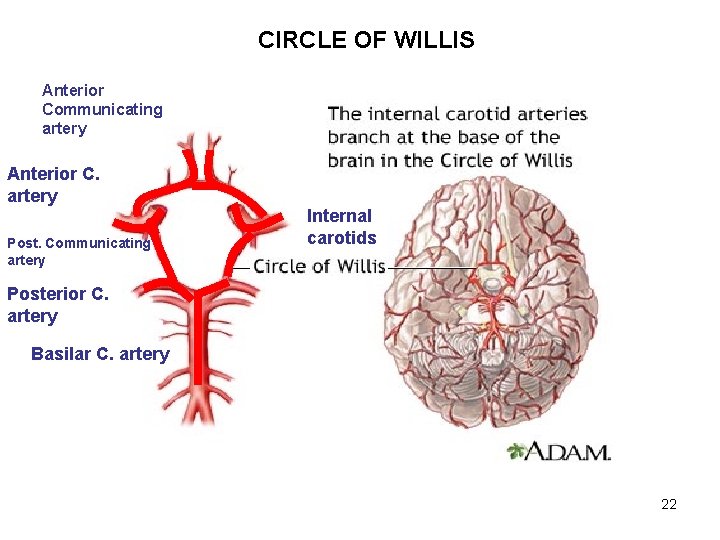
CIRCLE OF WILLIS Anterior Communicating artery Anterior C. artery Post. Communicating artery Internal carotids Posterior C. artery Basilar C. artery 22
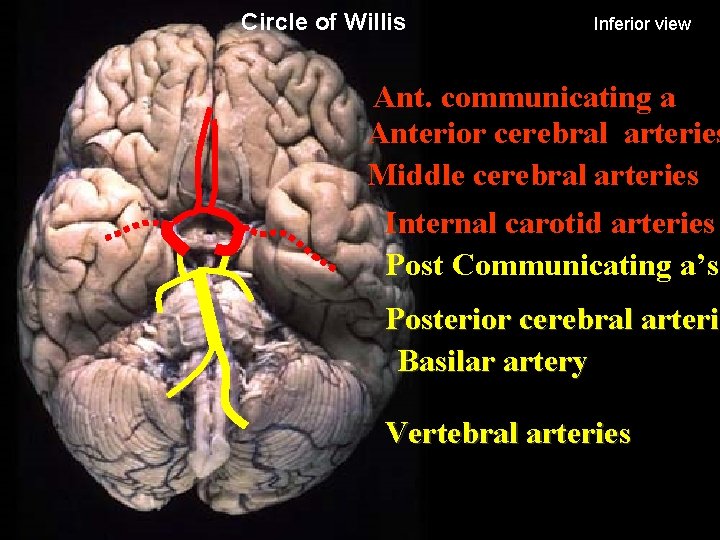
Circle of Willis Inferior view Ant. communicating a Anterior cerebral arteries Middle cerebral arteries Internal carotid arteries Post Communicating a’s Posterior cerebral arterie arteri Basilar artery Vertebral arteries 23

CIRCULATION WITHIN THE LOBES OF THE BRAIN IS OFTEN SUPPLIED BY MORE THAN ONE CEREBRAL ARTERY E. g. . ACA and MCA to the frontal lobe 24
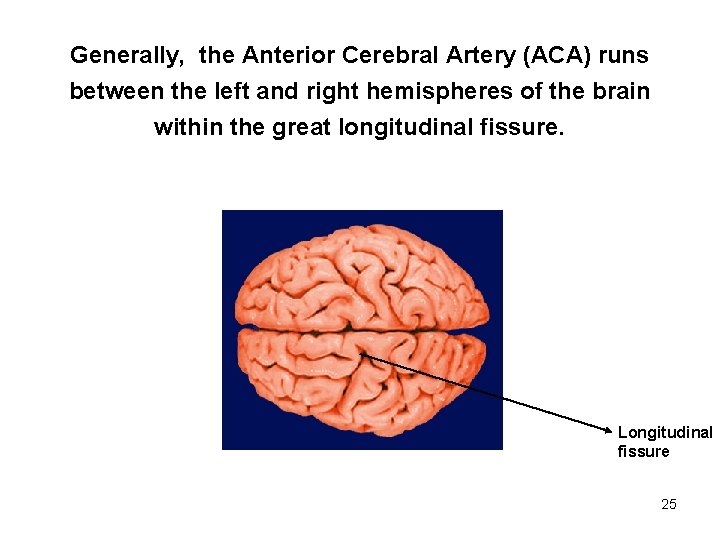
Generally, the Anterior Cerebral Artery (ACA) runs between the left and right hemispheres of the brain within the great longitudinal fissure. Longitudinal fissure 25
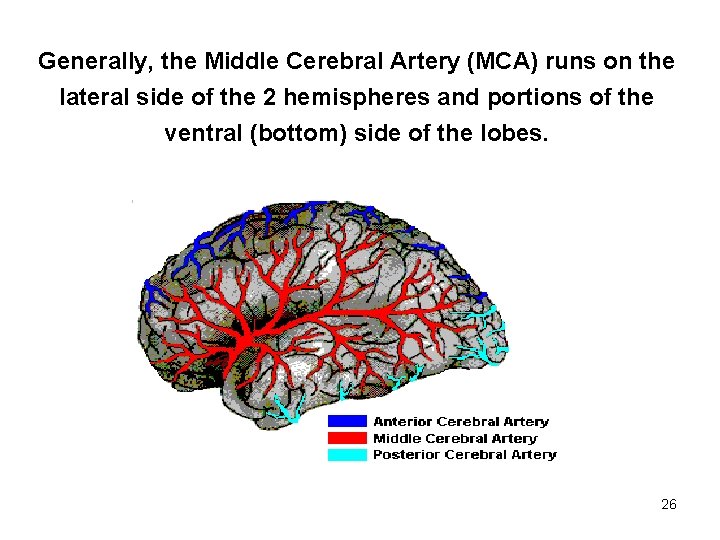
Generally, the Middle Cerebral Artery (MCA) runs on the lateral side of the 2 hemispheres and portions of the ventral (bottom) side of the lobes. 26
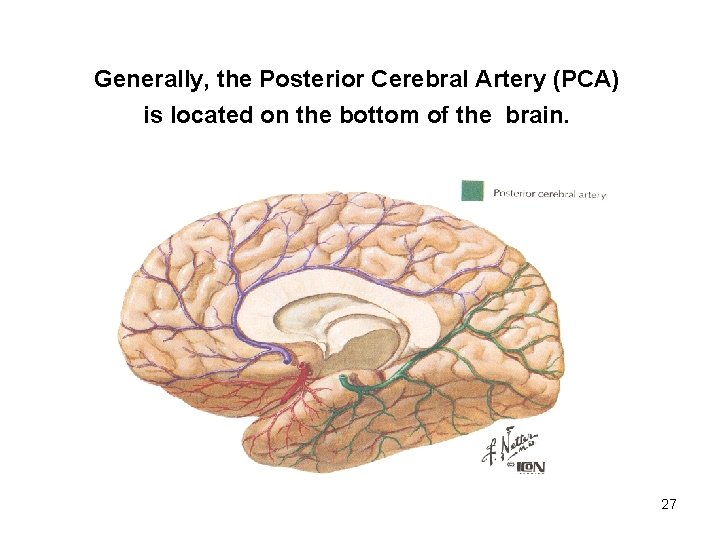
Generally, the Posterior Cerebral Artery (PCA) is located on the bottom of the brain. 27
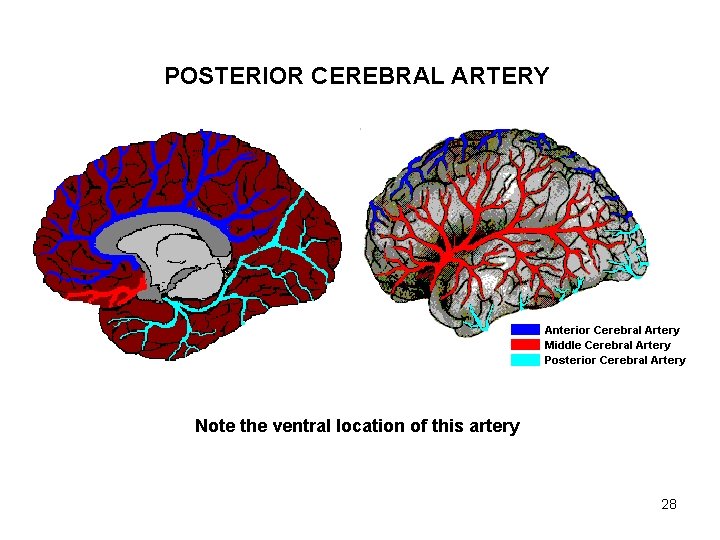
POSTERIOR CEREBRAL ARTERY Note the ventral location of this artery 28
DEFICITS IN A PATIENT WITH A STROKE CAN BE EXPLANED BY: 1. AREAS OF THE BRAIN 2. CIRCULATION OF THE BRAIN 3. AND/OR A COMBINATION OF BOTH 29
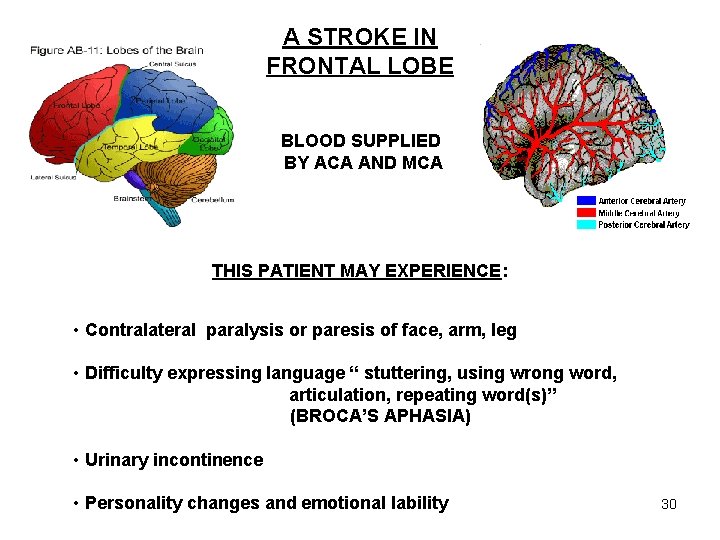
A STROKE IN FRONTAL LOBE BLOOD SUPPLIED BY ACA AND MCA THIS PATIENT MAY EXPERIENCE: • Contralateral paralysis or paresis of face, arm, leg • Difficulty expressing language “ stuttering, using wrong word, articulation, repeating word(s)” (BROCA’S APHASIA) • Urinary incontinence • Personality changes and emotional lability 30

FRONTAL LOBE CONTINUED IMPORTANT STRUCTURES Controls ability to express language 31
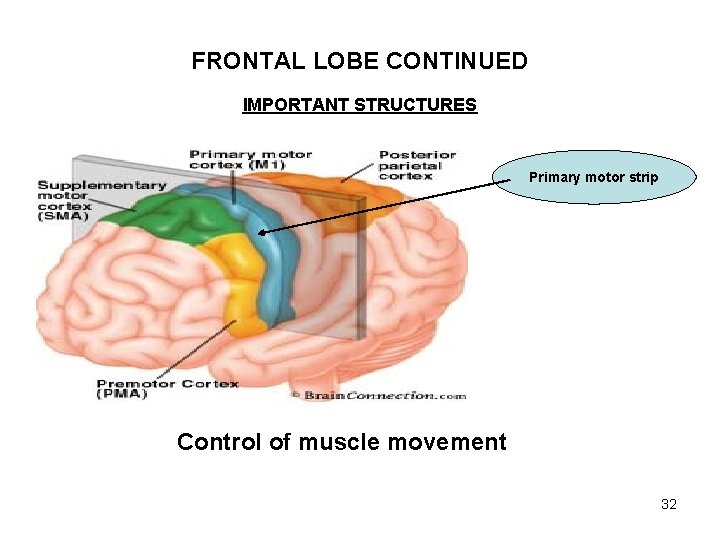
FRONTAL LOBE CONTINUED IMPORTANT STRUCTURES Primary motor strip Control of muscle movement 32
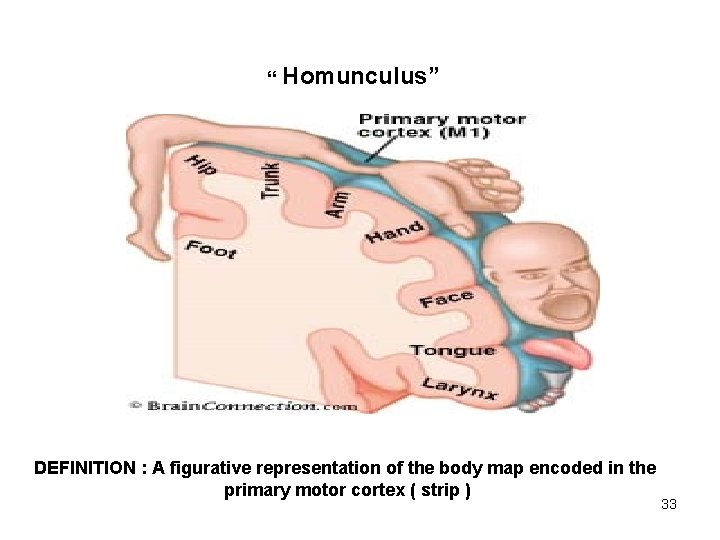
“ Homunculus” DEFINITION : A figurative representation of the body map encoded in the primary motor cortex ( strip ) 33
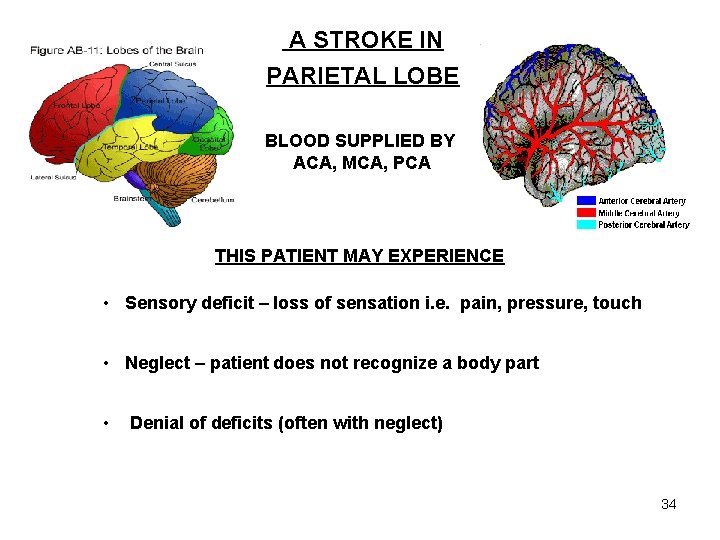
A STROKE IN PARIETAL LOBE BLOOD SUPPLIED BY ACA, MCA, PCA THIS PATIENT MAY EXPERIENCE • Sensory deficit – loss of sensation i. e. pain, pressure, touch • Neglect – patient does not recognize a body part • Denial of deficits (often with neglect) 34
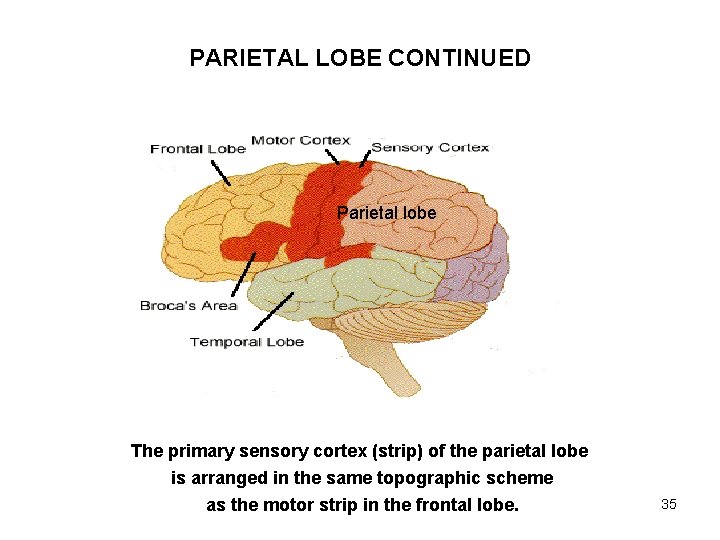
PARIETAL LOBE CONTINUED Parietal lobe The primary sensory cortex (strip) of the parietal lobe is arranged in the same topographic scheme as the motor strip in the frontal lobe. 35

A STROKE IN TEMPORAL LOBE BLOOD SUPPLIED BY MCA AND PCA THIS PATIENT MAY EXPERIENCE • Severe communication problem : loss of comprehension of spoken language ( Receptive Aphasia also called Wernicke’s Aphasia) • Memory loss or disturbances in memory • Aggressiveness 36
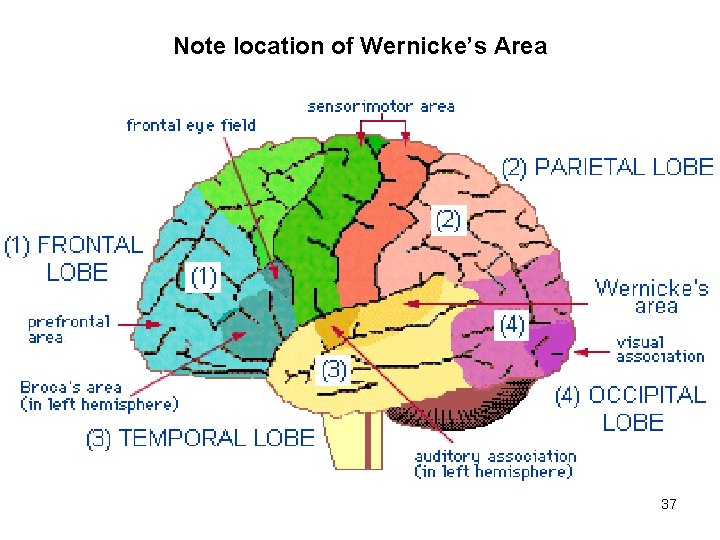
Note location of Wernicke’s Area 37
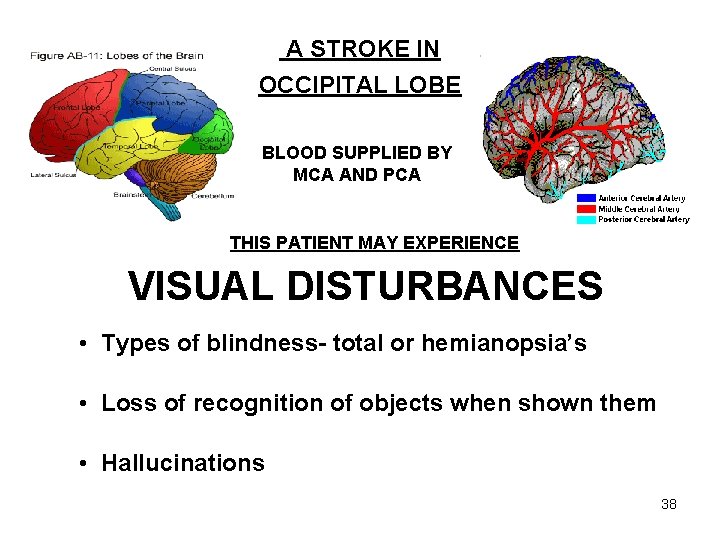
A STROKE IN OCCIPITAL LOBE BLOOD SUPPLIED BY MCA AND PCA THIS PATIENT MAY EXPERIENCE VISUAL DISTURBANCES • Types of blindness- total or hemianopsia’s • Loss of recognition of objects when shown them • Hallucinations 38
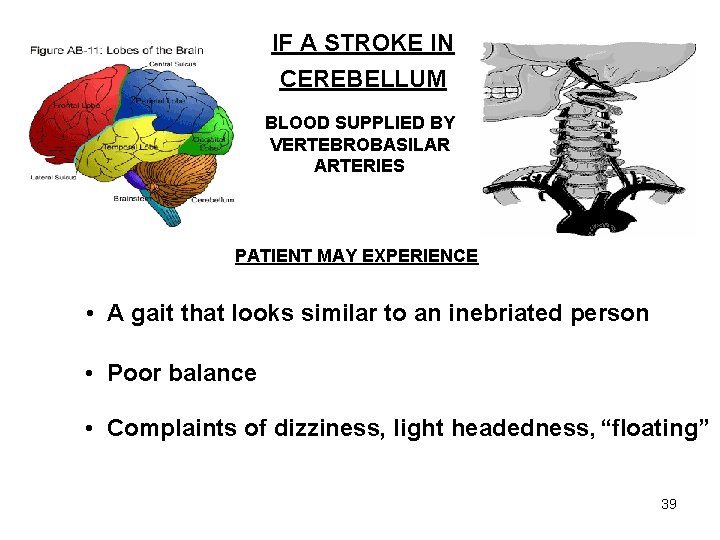
IF A STROKE IN CEREBELLUM BLOOD SUPPLIED BY VERTEBROBASILAR ARTERIES PATIENT MAY EXPERIENCE • A gait that looks similar to an inebriated person • Poor balance • Complaints of dizziness, light headedness, “floating” 39
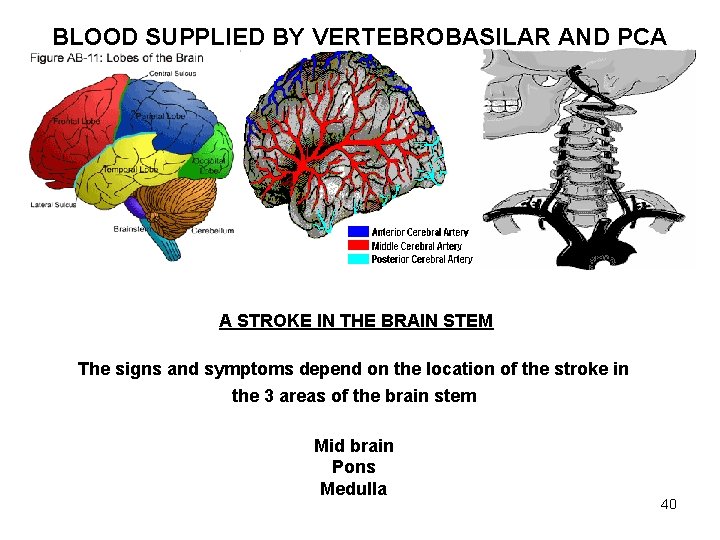
BLOOD SUPPLIED BY VERTEBROBASILAR AND PCA A STROKE IN THE BRAIN STEM The signs and symptoms depend on the location of the stroke in the 3 areas of the brain stem Mid brain Pons Medulla 40
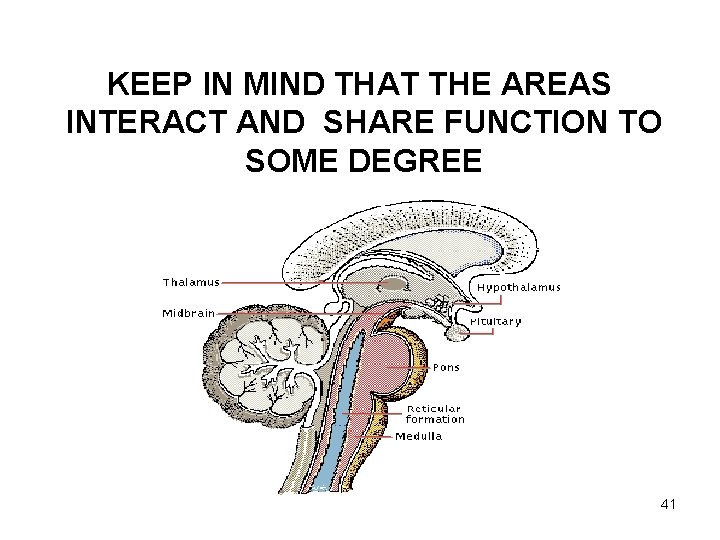
KEEP IN MIND THAT THE AREAS INTERACT AND SHARE FUNCTION TO SOME DEGREE 41
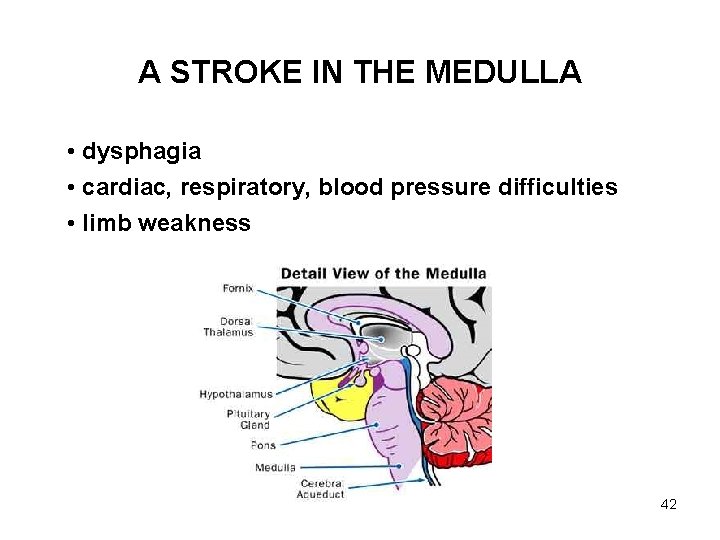
A STROKE IN THE MEDULLA • dysphagia • cardiac, respiratory, blood pressure difficulties • limb weakness 42
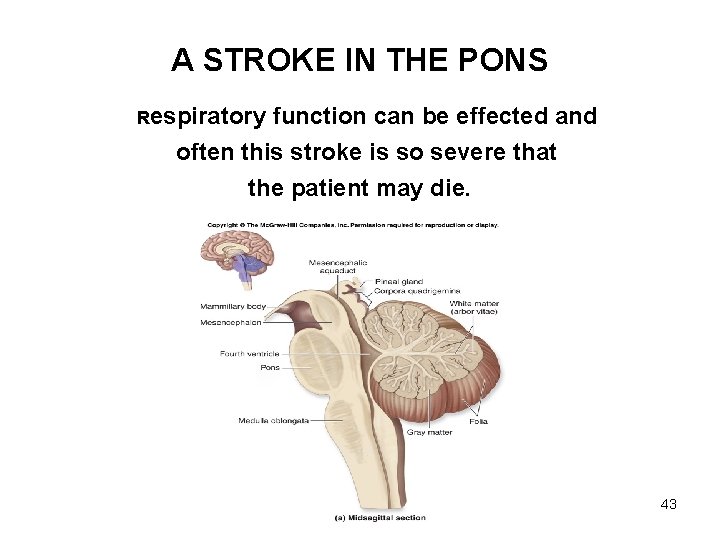
A STROKE IN THE PONS Respiratory function can be effected and often this stroke is so severe that the patient may die. 43

Types of Stroke • Ischemic (80 %) – Caused by blockage of an artery – Usually the result of a blood clot Thrombotic or embolic • Hemorrhagic (20%) - Caused by an arterial rupture Subarachnoid hemorrhage (SAH) Intracerebral Hemorrhage (ICH) 44

Stroke Types CIHI/NACRS, 2005 -06 45

Definition of TIA • TIA = transient ischemic attack – resolution must be complete • Sudden onset of focal neurological dysfunction, presumably of vascular origin, lasting less than 24 hours. – 1/3 last less than 15 min – 70% < 1 hour – 10 % more than 12 hours – No permanent damage 46
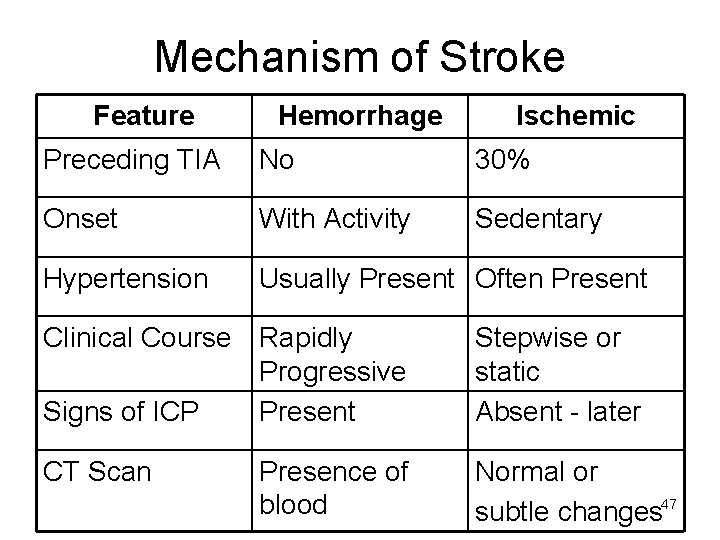
Mechanism of Stroke Feature Hemorrhage Ischemic Preceding TIA No 30% Onset With Activity Sedentary Hypertension Usually Present Often Present Clinical Course Rapidly Progressive Signs of ICP Present Stepwise or static Absent - later CT Scan Normal or subtle changes 47 Presence of blood
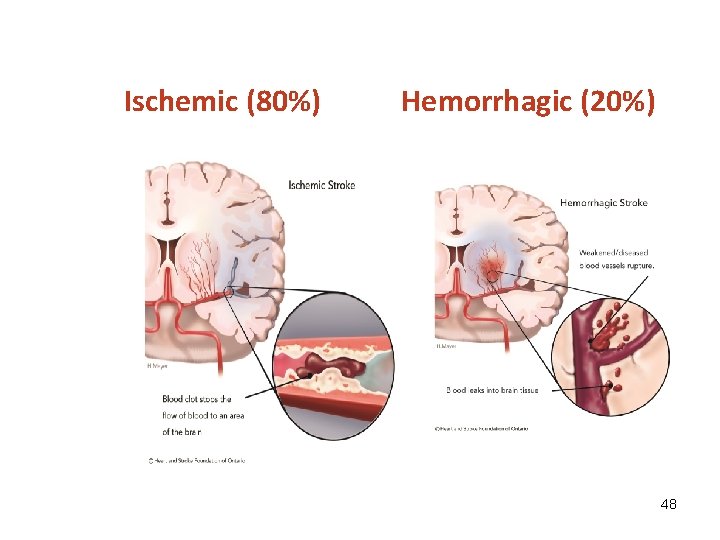
Ischemic (80%) Hemorrhagic (20%) 48

What is t. PA? • Clot buster – Works by dissolving the clot that is blocking the vessel in the ischemic stroke patients – Not all patients are eligible – Must be initiated within 4. 5 hrs. from onset of symptoms – Given by IV bolus and infusion- takes about 1 hour 49
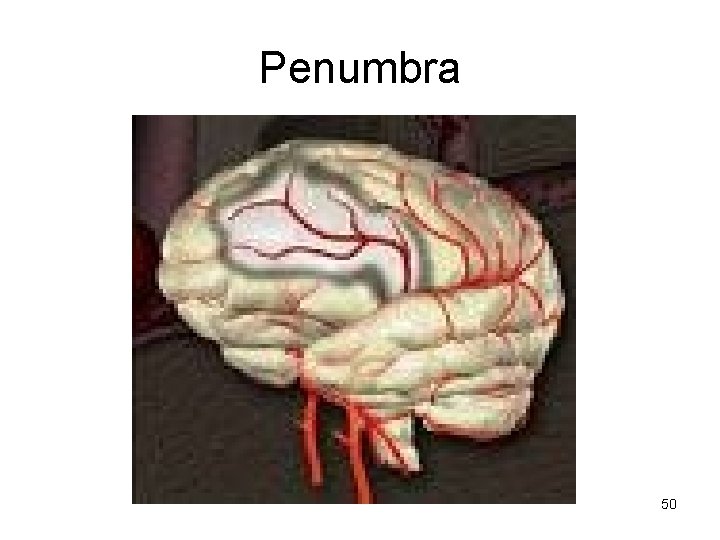
Penumbra 50
Occlusion and Re-canalization

Conclusion • Deficits of a stroke can be explained by area of the brain affected, circulation of the brain or a combination of both. • Rapid Assessment and treatment is critical Time is Brain 52

Coffee Break! 53
- Slides: 53