STROKE RISK STRATIFICATION AND MANAGEMENT PRESENTED BY CAROL

STROKE RISK STRATIFICATION AND MANAGEMENT PRESENTED BY CAROL RIPPLE, MCMSC, PA-C ST. ANTHONY’S NEUROLOGY SPECIALIST GROUP 2021 FAPA SUMMER CONFERENCE MARCO ISLAND, FLORIDA

OBJECTIVES Recognizing Stroke risk factors Preemptive education on stroke risk stratification Understanding the significance of a TIA Understanding the difference between ischemic and hemorrhagic stroke management Understanding the management of an embolic stroke Post stroke education for better outcomes

TEST YOUR KNOWLEDGE What are the five risk factors for stroke (audience participation) What is the significance of a TIA

TEST YOUR KNOWLEDGE What does BEFAST stand for? a. working fast b. slang for breakfast c. updated acronym for stroke symptoms

RECOGNIZING STROKE RISK FACTORS Hypertension- is the number 1 cause of stroke. Primary prevention can reduce 90 % of first time events of which ½ may result in mod-severe disability. -More than 20 percent with HTN are unaware of it. -As blood pressure increases, so does the risk of stroke, -HTN contributed to 34. 6% of the population attributed risk for stroke ( 52% when BP > 160/90.

HYPERTENSION In the Secondary Prevention of Small Sub-cortical Stroke ( PSS 3) trial - a SBP less than 130 mm. Hg was associated with a decrease in the reoccurrence of stroke events. * A very low SPB< 120 mm. Hg after recent stroke was associated with increased risk of recurrent stroke compared with those of normal blood pressure. *A goal BP of approximately 120 -140 systolic and 80 -90 mm. Hg diastolic may be ideal.

DYSLIPIDEMIA High cholesterol is a risk factor for heart disease and stroke, causing about 2. 6 million deaths in the United States every YEAR. -plays a major role in small vessel ischemic disease (lacunar infarcts) and carotid artery disease (embolic stroke) Those patients who achieved a 50% reduction LDL had the most benefit ( 30% effective relative risk reduction) the goal is to achieve a LDL <70 mg/d. L ) Rosuvastatin and Atorvastatin are considered to be the most capable of achieving greater than 50% reduction in LDL New AHA/ASA recommendations for high dose statins after first TIA/ Stroke extremely low LDL less than 50 can place the elderly in jeopardy of having intercerbral hemorrhage. Consider discontinuing and monitor LDL levels and restart if needed.

DIABETES In 2018, 88 million Americans age 18 and older had pre-diabetes. Major risk factor for all vascular disease and known to be an independent factor for stroke DM dx > 3 yrs - 74% increased risk especially with CKD on HD According to statistics from the CDC, in 2016, 1. 7 million diabetics were discharged from hospitals for major cardiovascular diseases, 438, 000 for ischemic heart and 313, 000 for stroke Goal of A 1 c less than 7. 0

SMOKING Cigarette smoking exposes the patient to nicotine and carbon monoxide damaging the cardiovascular system in many ways. -The use of oral contraceptives combined with smoking greatly increases stroke risk. -Vaping was associated with multiple serious health conditions including a large increased risk of stroke, compared to non-smokers –vaper’s experienced a 71% increased risk of stroke. -There is also data indicating that there is also higher rates of aneurysmal rupture and Coronary Artery Disease in cigarette smokers and vaper’s -Passive smoke exposure 25% increased stroke risk. -Counsel, offer programs, smoking cessation aids Ref: Electronic Cigarette Use is Associated with Higher Risk of Stroke, March 12, 2020.

OBESITY AND INACTIVITY Our current obesity rate in the US is currently at 42. 4 percent which is the highest recorded ( PRE COVID ) data. Unfortunately, social and economic factors weight heavily on the distribution of obesity across populations greatly affecting the Black, Hispanic and lower income population Childhood rates of obesity are also increasing with the latest data showing that 19. 3 % of US children ages 2 -19 have obesity, a rise from 5. 5% in the 1970’s. More children are now being diagnosed with hypertension and high cholesterol. Obesity is related to DM, HTN, HLD, Stroke and many types of cancers. *

ADDRESSING OBESITY AND INACTIVITY Strive for addressing obesity by discussion, support and weight loss programs, local dietitians, Noom, WW have been very successful in helping with weight loss. Encourage walking, getting a step counter. Isometric exercises for those with joint, hip problems, mobility and balance can still get an effective work out.

OTHER CAUSES OF TIA/ STROKE Other etiologies of stroke can include: hypercoaguable states/ anti-phospolipid syndrome oral contraceptives/ estrogen cardiac arrhythmias such as Atrial Fibrillation* Carotid Dissection ( 15%) / Patent Foramen Ovale Vasculitis/ Lupus/ Moya Sickle cell disease History of sleep apnea, heavy ETOH use NOTE: Think of the above in the younger patient with stroke!

STROKE AWARENESS AND MANAGEMENT Recognizing symptoms of stroke or TIA
TIME IS BRAIN Time lost is brain lost in acute cerebral ischemia. In a typical middle cerebral artery ischemic stroke, 2 million nerve cells are lost each minute in which reperfusion has not been achieved.

HISTORY AND TIMING IS KEY EMS calls receiving hospital for stroke alert, Upon arrival to the ER, -Stat Ct of the head is performed -It is imperative that a history is taken to include risk factors i. e. previous stroke, HTN, DM, HLD, Smoking, Obesity , Medications, family history. -The timing of onset of symptoms ( last known normal), their presenting features and how long did they last/are still present. -Physical and neurological examination to include NIHSS exam. -Family input is also important. - Walk in patients may have lost time due to private transportation, lack of recognizing symptoms and not providing pertinent information to the ER staff. Remember time is brain. Timing of event, diagnostic imaging and neurological exam will determine course of treatment.

INTEGRAL COMPONENTS OF THE HISTORY Vascular risk factors. HTN, HLD, DM, Obesity, Prior CVA, smoking Medications Anticoagulants, Antiplatelet agents, antihypertensive medications, stimulants (including diet pills), sympathomimetics Recent trauma or surgery Carotid endarterectomy or carotid stenting, as ICH may be related to hyperperfusion after such procedures Dementia Associated with Amyloid angiopathy Alcohol or illicit drug use Cocaine, Methamphetamines and other sympathomimetics drugs are associated with ICH Seizures Liver disease and Cancer/hematologic dz - May be associated with coagulopathy

TRANSIENT ISCHEMIC ATTACK Definition: A TIA or Transient Ischemic Attack is a “ warning stroke” that occurs when a blood clot blocks an artery for a short time. The only difference between a stroke and a TIA is that with a TIA the blockage is temporary. *symptoms occur rapidly and last a relatively short period of time. There is no permanent injury to the brain. *risk of stroke in the future is very high. 9 -17% will have a stroke within 90 days. *Patients should go to the ER immediately to reduce the risk of permanent disability.

ABCD 2 VALIDATED, SEVEN POINT, RISK STRATIFICATION TOOL TO IDENTIFY PATIENTS AT HIGH RISK OF STROKE AFTERTIA. , • Age >= 60 yrs 0 SBP >= 140 or DBP >= 90 Symptoms : Unilateral Weakness + /- Speech w. o weakness Symptoms: Other Symptoms: Speech only Duration <10 mins Duration 10 -59 mins Duration >60 mins hx of Diabetes NO YES +1 0 +1 +2 +1 0 0 +1 +2 +1

ISCHEMIC STROKE Overview • National Institute of Health Stroke Score • Work up for ischemic Stroke/ TIA • Principles of Stroke Management • Thrombolysis . Mechanical Embolectomy • Anti‐platelet agents • Other
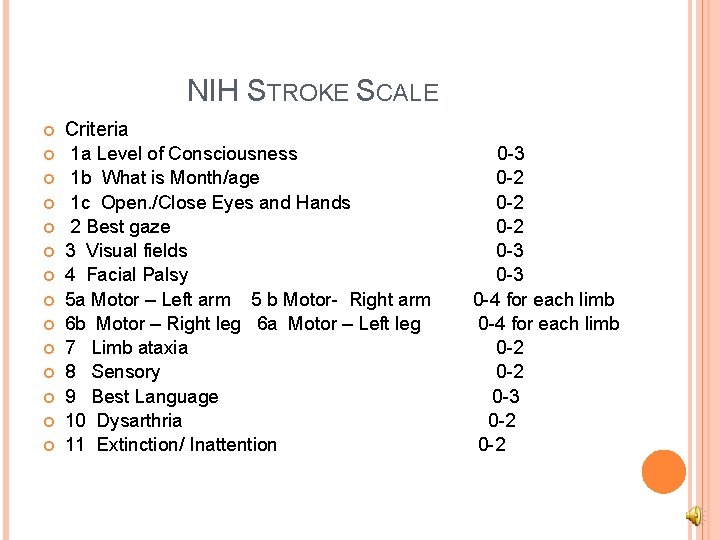

NIH STROKE SCALE Criteria 1 a Level of Consciousness 1 b What is Month/age 1 c Open. /Close Eyes and Hands 2 Best gaze 3 Visual fields 4 Facial Palsy 5 a Motor – Left arm 5 b Motor- Right arm 6 b Motor – Right leg 6 a Motor – Left leg 7 Limb ataxia 8 Sensory 9 Best Language 10 Dysarthria 11 Extinction/ Inattention 0 -3 0 -2 0 -2 0 -3 0 -4 for each limb 0 -2 0 -3 0 -2

TIA/STROKE WORKUP ● ● LABS- in particular AIC, LIPID PANEL, CBC, glucose U/S carotid (Symptomatic Carotid stenosis 50% or higher should be treated within 2 weeks after an event) ● ● ● 2 D echocardiogram MRI- 21 -67% of TIAs will have a positive stroke finding on MRI MRA/ CTA - intracranial atherosclerosis EKG & Tele monitoring- AFIB If young patient consider anticoag w/u, autoimmune w/u

PRINCIPLES OF ACUTE STROKE CARE 1. Achieve timely recanalization of occluded artery and reperfusion of the ischemic tissue. 2. Optimize Collateral flow 3. Avoid secondary brain injury Two evidence based strategies to achieve reperfusion. Chemical thrombolysis Mechanical embolectomy

ANTIPLATELET THERAPY Usually will start with Aspirin 81 mg daily. Aspirin 325 mg had no significant benefit and also carries a higher chance for GI bleed. Dual anti-platelet therapy ( Aspirin and Clopidogrel) indicated for 30 days for those with early arriving minor stroke and high-risk TIA or severe symptomatic intracranial stenosis. Clopidogrel should be discontinued after 30 days unless otherwise indicated

2018 AHA/ASA EARLYSTROKE BP MANAGEMENT In patients with BP ≥ 220/120 mm. Hg who did not receive IV alteplase or EVT and have no co-morbid conditions requiring acute antihypertensive treatment, the benefit of initiating or reinitiating treatment of hypertension within the first 48 to 72 hours is uncertain. It might be reasonable to lower BP by 15% during the first 24 hours after onset of stroke. *Starting or restarting antihypertensive therapy during hospitalization in patients with BP >140/90 mm. Hg who are neurologically stable is safe and is reasonable to improve long-term BP control unless contraindicated.

MANAGEMENT OF HEMORRHAGIC STROKE -Blood pressure SBP 140 -160 DPB 80 -90 -Head of bed at 30 degrees -NO NSAIDS, Antiplatelet, Anticoagulants, Thrombotic medications -Low threshold for Stat repeat CT of the brain with change in mental status or neurologic deficits -Neurosurgery consult often placed to determine evacuation if necessary -Addition of anti seizure medication often used -Recommend ICU monitoring until the patient is stable. -

GOALS FOR IV TPA FORSTROKE

ELIGIBILITY CRITERIA FOR THE TREATMENT OF ACUTE ISCHEMIC STROKE WITH INTRAVENOUS ALTEPLASE (RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OR TPA) Indications Clinical diagnosis of ischemic stroke causing measurable neurologic deficit( regardless of severity Onset of symptoms within 4. 5 hours Wakeup stroke with diffusion weighted imaging=FLAIR mismatch on MRI Age ≥ 18 years Source: Up. To. Date 2021 Eligibility Criteria for the Treatment of acute ischemic stroke with intravenous Plasminogen activator or TPA

EXCLUSION CRITERIA Ischemic stroke or severe head trauma in the previous three months Previous intracranial hemorrhage Suspected subarachnoid hemorrhage Intra-axial or intracranial neoplasm Suspected infective endocarditis Suspected aortic arch dissection Gastrointestinal malignancy or hemorrhage in the previous 21 days Intracranial or intraspinal surgery within 3 months

CONTRAINDICATIONS Active internal bleeding Persistent blood pressure elevation (systolic ≥ 185 mm. Hg or diastolic ≥ 110 mm. Hg)that cannot be lowered safely Bleeding diathesis INR >1. 7 Heparin within 48 hrs with abnormal APTT Low molecular weight heparin full treatment dose with in the previous 24 hours Platelets <100, 000 /mm 2 Current use of direct thrombin inhibitor of factor Xa inhibitor with abnormal coagulation tests CT showing acute hemorrhage CT showing extensive hypo-density ( i. e. 1/3 of the cerebral hemisphere)

WARNINGS¶ Only minor and isolated neurologic signs or rapidly improving symptoms Serum glucose <50 mg/d. L (<2. 8 mmol/L)◊ Serious trauma in the previous 14 days§ Major surgery in the previous 14 days¥ History of gastrointestinal bleeding (remote) or genitourinary bleeding‡ Seizure at the onset of stroke with postictal neurologic impairments† Pregnancy** Arterial puncture at a non-compressible site in the previous seven days¶¶ Large (≥ 10 mm), untreated, non ruptured intracranial aneurysm¶¶ Untreated intracranial vascular malformation¶¶

ADDITIONAL WARNINGS FOR TREATMENT FROM 3 TO 4. 5 HOURS FROM SYMPTOM ONSET Age >80 years Oral anticoagulant use regardless of INR Severe stroke (NIHSS score >25) Combination of both previous ischemic stroke and diabetes mellitus

DEFINITION OF TERMS AND ADDITIONAL GUIDANCE ACS: acute coronary syndrome; a. PTT: activated partial thromboplastin time; ECT: ecarin clotting time; INR: international normalized ratio; PT: Prothrombin time; NIHSS: National Institutes of Health Stroke Scale; t. PA: intravenous alteplase; TT: thrombin time; VTE: venous thromboembolism. Although it is desirable to know the results of these tests, thrombolytic therapy should not be delayed while results are pending unless (1) there is clinical suspicion of a bleeding abnormality or thrombocytopenia, (2) the patient is currently on or has recently received anticoagulants (eg, heparin, warfarin, a direct thrombin inhibitor, or a direct factor Xa inhibitor), or (3) use of anticoagulants is not known. Otherwise, treatment with intravenous t. PA can be started before availability of coagulation test results but should be discontinued if the INR, PT, or a. PTT exceed the limits stated in the table, or if platelet count is <100, 000 mm 3.

¶ With careful consideration and weighting of risk-to-benefit, patients may receive intravenous alteplase despite one or more warnings. Δ Patients who have a persistent neurologic deficit that is potentially disabling, despite improvement of any degree, should be treated with t. PA in the absence of other contraindications. Any of the following should be considered disabling deficits: Complete hemianopsia: ≥ 2 on NIHSS question 3, or Severe aphasia: ≥ 2 on NIHSS question 9, or Visual or sensory extinction: ≥ 1 on NIHSS question 11, or Any weakness limiting sustained effort against gravity: ≥ 2 on NIHSS question 5 or 6, or Any deficits that lead to a total NIHSS >5, or Any remaining deficit considered potentially disabling in the view of the patient and the treating practitioner using clinical judgment

TPA ADDITIONAL GUIDANCE ◊ Patients may be treated with intravenous alteplase if glucose level is subsequently normalized. § The potential risks of bleeding with alteplase from injuries related to the trauma should be weighed against the anticipated benefits of reduced stroke-related neurologic deficits. ¥ The increased risk of surgical site bleeding with alteplase should be weighed against the anticipated benefits of reduced stroke-related neurologic deficits. ‡ There is a low increased risk of new bleeding with alteplase in the setting of past gastrointestinal or genitourinary bleeding. However, alteplase administration within 21 days of gastrointestinal bleeding is not recommended.

TPA ADDITIONAL GUIDANCE † Alteplase is reasonable in patients with a seizure at stroke onset if evidence suggests that residual impairments are secondary to acute ischemic stroke and not to a postictal phenomenon. ** Alteplase can be given in pregnancy when the anticipated benefits of treating moderate or severe stroke outweigh the anticipated increased risks of uterine bleeding. ¶¶ The safety and efficacy of administering alteplase is uncertain for these relative exclusions. ΔΔ Although these were exclusions in the trial showing benefit in the 3 to 4. 5 hour window, intravenous alteplase appears to be safe and may be beneficial for patients with these criteria, including patients taking oral anticoagulants with an INR <1. 7.

MECHANICAL THROMBECTOMY NIHSS>6 Capture Internal Carotid Artery and Middle Cerebral Artery Strokes 24 hour benefit on recent trials Works best with combination of TPA

MECHANICAL THROMBECTOMY

EMBOLIC STROKE Embolic strokes usually caused by blood clot forming from another part of the body often from the heart, carotid arteries, or can be caused by septic emboli, air embolism, heart surgery, Patent foramen Ovale, cancers, and hypercoaguable states. 15% are caused by Atrial Fibrillation. Account for approximately 14 -30 % of ischemic strokes Work up is the same as stroke with the addition of Transesophageal Echocardiogram. Cardiology consult and consideration for anticoagulation in addition to aspirin and/or Plavix, loop recorder as outpatient

POST STROKE FOLLOW UP Your patients will need your support after stroke Medical needs: compliance with Antiplatelet, anticoagulants, blood pressure and lipid control. Periodic labs. May need referrals for PT, OT, Speech therapy, outpatient cardiology /vascular referrals for post stroke follow-up. May need help with assistive devices if not provided on discharge- Walkers, commodes, wheelchairs, disabled vehicle hang tags. Don’t forget to ask about mood, fatigue, memory loss, pain, caregiver fatigue, home health often helpful

MEASURES TO AVOID A SECOND EVENT Blood pressure control - Ideal from 120 - 140 systolic and 70 -80 diastolic. - teach patient to keep a blood pressure diary and review regularly. - compliance with anti-platelets, anti-coags and statins Hyperlipidemia- goal LDL <= 70 2020 – age under 75 - aggressive treatment with high dose Lipitor 4080 mg or Crestor 20 mg Age over 75 - treat with moderate dose statin Lipitor 20 or Crestor 10 mg * If LDL is 70 or less, document no need for aggressive treatment DM - A 1 c <= 7. 0 Obesity- BMI goal 18. 5 - 24. 9 Dietary changes, Dash diet, WW, Noom , exercise, counseling Smoking – use smoking cessation such as Wellbutrin, Chantix if tolerated, Nicoderm products, counseling, support groups, Florida Dept of Health.

MEASURES TO AVOID A SECOND EVENT Diet and Activity Unfortunately social demographics can interfere with our hopes. Continue to encourage for changes, refer to a dietitian, have them look into WW or Noom for guidance. Encourage walking, isometric exercises which although can be done stationary still increase muscle mass, and burn calories. Helpful for those that have balance, mobility issues.

LAST BUT NOT LEAST. . Understand that your patient and their family have been affected by the physical and emotional trauma of a hospitalization, with variable deficits, a huge medical bill, new challenges on learning how to rehab, or live with permanent loss of speech, motor or sensory ability. Stroke victims often have memory loss after a stroke, fatigue, depression, speech difficulty receptive/or aphasic, inability to function like they did before affecting eating, dressing, ADL, driving and working. Family members also are a victim. Please take the time to ask how they are really doing and if possible find resources to help them!

POST PRESENTATION QUESTIONS 1. What are the differences of a TIA and a Stroke? 2. Why is it important to get medical attention as soon as possible? 3. How is the treatment for ischemic vs. hemorrhagic stroke differ-BP parameters, medication 4. What are the common causes of stroke in younger adults under 65? 5. How can you improve your care of post stroke patients?

SOURCES FOR YOUR PATIENT American Heart/ American Stroke Association Stroke support Groups Mental Health Counseling Continuum Lifelong Learning in Neurology Thank you for your attention and for taking care of your Patients. Keep doing what we do best- listen, communicate and Educate!!!

QUESTIONS?
- Slides: 45