STROKE a k a Cerebrovascular Accident CVA Brain

STROKE a. k. a. Cerebrovascular Accident (CVA) & Brain Attack
Stroke Ischemia is inadequate blood flow n Occurs when ischemia to part of the brain results in death of brain cells n

Stroke Movement, sensation, or emotions controlled by affected area are lost or impaired n Loss of function varies with location and extent of damage n

Stroke n Brain attack – Term increasingly being used to describe stroke and communicate urgency of recognizing stroke symptoms and treating their onset as a medical emergency

Risk Factors Nonmodifiable Age n Gender (women more likely to die) n Race (African Americans) n Heredity n

Risk Factors Modifiable Asymptomatic carotid stenosis n Diabetes mellitus n Heart disease, atrial fibrillation n Heavy alcohol consumption n Hypercoagulability n Hyperlipidemia n

Risk Factors Modifiable Hypertension n Obesity n Oral contraceptive use n Physical inactivity n Sickle cell disease n Smoking n

Etiology and Pathophysiology Brain requires continuous supply of O 2 and glucose for neurons to function n If blood flow is interrupted – Neurologic metabolism is altered in 30 seconds – Metabolism stops in 2 minutes – Cell death occurs in 5 minutes n

Etiology and Pathophysiology n Atherosclerosis is a major cause of stroke – Can lead to thrombus formation and contribute to emboli
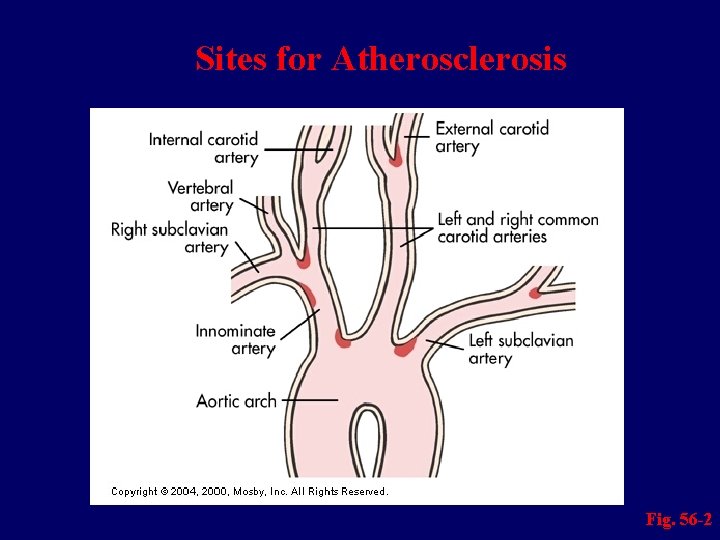
Sites for Atherosclerosis Fig. 56 -2

Etiology and Pathophysiology Around the core area of ischemia is a border zone of reduced blood flow where ischemia is potentially reversible n If adequate blood flow can be restored early (<3 hours) and the ischemic cascade can be interrupted – less brain damage and less neurologic function lost n

Transient Ischemic Attacks (TIA) Temporary focal loss of neurologic function caused by ischemia (analogous to angina in CAD) n Most resolve within 3 hours n May be due to micro-emboli that temporarily block blood flow n A warning sign of progressive cerebrovascular disease n

Types of Stroke n Classification based on underlying pathophysiologic findings – Ischemic n Thrombotic n Embolic – Hemorrhagic
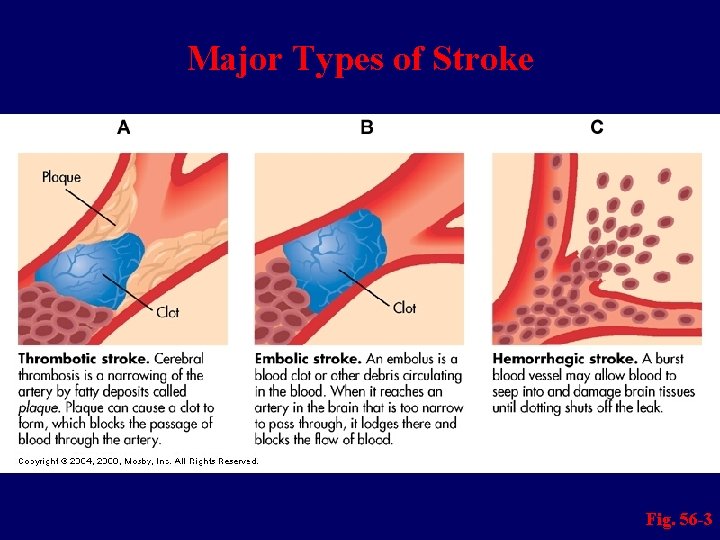
Major Types of Stroke Fig. 56 -3

Ischemic Stroke Result of inadequate blood flow to brain due to partial or complete occlusion of an artery n Constitute 85% of all strokes n Most patients with ischemic stroke do not have a decreased level of consciousness in the first 24 hours n Symptoms often worsen during first 72 hours d/t cerebral edema n

Ischemic Stroke n Thrombotic stroke – Thrombosis occurs in relation to injury to a blood vessel wall → blood clot – Result of thrombosis or narrowing of the blood vessel – Most common cause of stroke

Ischemic Stroke n Thrombotic stroke – Two-thirds are associated with HTN and diabetes – Often preceded by a TIA

Ischemic Stroke n Embolic stroke – Embolus lodges in and occludes a cerebral artery – Results in infarction and edema of the area supplied by the vessel – Second most common cause of stroke

Ischemic Stroke n Embolic stroke – Majority of emboli originate in heart, with plaque breaking off from the endocardium and entering circulation – Associated with sudden, rapid occurrence of severe clinical symptoms

Ischemic Stroke n Embolic stroke – Patient usually remains conscious although may have a headache – Recurrence is common unless the underlying cause is aggressively treated

Hemorrhagic Stroke Account for approximately 15% of all strokes n Result from bleeding into the brain tissue itself or into the subarachnoid space or ventricles n

Hemorrhagic Stroke n Intracerebral hemorrhage – Bleeding within the brain caused by a rupture of a vessel – Hypertension is the most important cause – Commonly occurs during activity

Hemorrhagic Stroke n Intracerebral hemorrhage – Often a sudden onset of symptoms that progress over minutes to hours b/c of ongoing bleeding – Manifestations include neurologic deficits, headache, N & V, decreased levels of consciousness, and HTN

Hemorrhagic Stroke n Subarachnoid hemorrhage – Bleeding into cerebrospinal space between the arachnoid and pia mater – Commonly caused by rupture of a cerebral aneurysm

Clinical Manifestations of Stroke n Affects many body functions n Motor activity n Elimination n Intellectual function n Spatial-perceptual alterations n Personality n Affect n Sensation n Communication

Clinical Manifestations Motor Function Most obvious effect of stroke n Can include impairment of – Mobility – Respiratory function – Swallowing and speech – Gag reflex – Self-care abilities n

Clinical Manifestations Motor Function n Characteristic motor deficits (contralateral) – Loss of skilled voluntary movement – Impairment of integration of movements – Alterations in muscle tone (flaccid → spastic) – Alterations in reflexes (hypo → hyper)

Clinical Manifestations Communication n Patient may experience aphasia when stroke damages the dominant hemisphere of the brain – Aphasia: total loss of comprehension and use of language – Dysphasia: difficulty with comprehension and use of language n Classified as nonfluent or fluent

Clinical Manifestations Communication n Dysarthria – Disturbance in the muscular control of speech – Impairments in pronunciation, articulation, and phonation; NOT meaning or comprehension

Clinical Manifestations Affect May have difficulty controlling their emotions n Emotional responses may be exaggerated or unpredictable n Depression , impaired body image and loss of function can make this worse n May be frustrated by mobility and communication problems n

Clinical Manifestations Intellectual Function Memory and judgment may be impaired n Left-brain stroke: more likely to result in memory problems related to language n
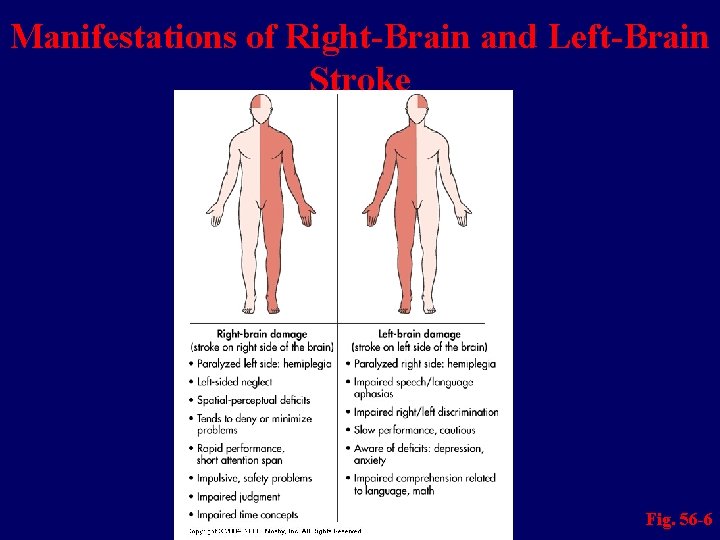
Manifestations of Right-Brain and Left-Brain Stroke Fig. 56 -6

Clinical Manifestations Spatial-Perceptual Alterations Stroke on the right side of the brain is more likely to cause problems in spatialperceptual orientation n However, this may occur with left-brain stroke n

Clinical Manifestations Spatial-Perceptual Alterations n Spatial-perceptual problems may be divided into four categories 1. Incorrect perception of self and illness (may deny illness or body parts) 2. Erroneous perception of self in space (e. g. , neglect all input from affected side; distance judgement)

Clinical Manifestations Spatial-Perceptual Alterations 3. Inability to recognize an object by sight, touch, or hearing 4. Inability to carry out learned sequential movements on command

Clinical Manifestations Elimination Most problems with elimination occur initially and are temporary n Prognosis for normal bladder function is excellent when only one hemisphere of brain is affected. n

Diagnostic Studies When symptoms of a stroke occur, diagnostic studies are done to – Confirm that it is a stroke – Identify the likely cause of the stroke n CT is the primary diagnostic test used after a stroke n

Collaborative Care Prevention Education and management of modifiable risk factors to prevent a stroke n Close management of patients with known risk factors n

Collaborative Care Prevention n Antiplatelet drugs (usually Aspirin) to prevent stroke in those with history of TIA

Collaborative Care Prevention n Surgical interventions for those with TIAs from carotid disease: – Carotid endarterectomy – Transluminal angioplasty – Stenting – Extracranial-intracranial bypass

n Add Figure 56 -7, p. 1533

Collaborative Care Acute Care n Assessment findings – Altered level of consciousness (See GCS, p. 1500) – Weakness, numbness, or paralysis – Speech or visual disturbances – Severe headache – ↑ or ↓ heart rate – Respiratory distress – Unequal pupils

Collaborative Care Acute Care n Assessment findings – Hypertension – Facial drooping on affected side – Difficulty swallowing – Seizures – Bladder or bowel incontinence – Nausea and vomiting – Vertigo

Collaborative Care Acute Care n Interventions – Initial: ABC – Ensure patient airway – Remove dentures – Perform pulse oximetry – Maintain adequate oxygenation – IV access – Maintain BP according to guidelines n (treat if SBP > 220 or MAP > 130)

Collaborative Care Acute Care n Interventions – Initial – Immediate CT scan to determine cause (ischemic vs hemorrhagic) – Measures to control ICP Head & neck in alignment (avoid flexion) n Elevate HOB 30 ° if no symptoms of shock or injury n Avoid hip, knee flexion n Pain management, euvolemia, diuretics if needed n

Collaborative Care Acute Care n Interventions – Initial – Institute seizure precautions – Avoid hyperthermia ( ↑s cerebral metabolism) – Anticipate thrombolytic/fibrinolytic therapy for ischemic stroke

Collaborative Care Acute Care n Thrombolytic/fibrinolytic therapy with recombinant tissue plasminogen activator (t. PA) is used to – Reestablish blood flow and prevent cell death in patients of ischemic stroke

Collaborative Care Acute Care n Thrombolytic/fibrinolytic therapy given within 3 hours of the onset of symptoms – ↓ disability – But at the expense of ↑ in deaths within the first 7 to 10 days and ↑ in intracranial hemorrhage

Collaborative Care Acute Care n For ischemic strokes (24 hr after t. PA): – Antiplatelets – Anticoagulants (Heparin, coumadin) n Must maintain therapeutic levels – PTT, INR

Collaborative Care Acute Care n Interventions – Ongoing – Monitor vital signs and neurologic status n Level of consciousness n Motor and sensory function n Pupil size and reactivity n O 2 saturation n Cardiac rhythm

Collaborative Care Acute Care n Approximately 10 -15% of patients who experience a stroke will have seizures, usually within 24 hours

Collaborative Care Acute Care n Surgical interventions: – Immediate evacuation of hematomas that result from hemorrhagic stroke – Clip, wrap or coli aneurysm to prevent rebleed

Collaborative Care Rehabilitation Care n After the stroke has stabilized for 12 -24 hours, collaborative care shifts from preserving life to lessening disability and attaining optimal functioning

Nursing Management Nursing Assessment n Assess for: – Clinical manifestations – Risk factors – Complications

Nursing Management Nursing Diagnoses Ineffective tissue perfusion (cerebral) n Ineffective airway clearance n Impaired physical mobility n Impaired verbal communication n Unilateral neglect n Impaired urinary elimination n

Nursing Management Nursing Diagnoses Impaired swallowing n Situational low self-esteem n

Nursing Management Planning n Goals – Maintain a stable or improved level of consciousness – Attain maximum physical functioning – Attain maximum self-care abilities and skills – Maximize communication abilities

Nursing Management Planning n Goals – Maintain adequate nutrition – Avoid complications of stroke – Maintain effective personal and family coping

Nursing Management Nursing Implementation n Health Promotion – Teaching patients and families about early symptoms associated with stroke or TIA and when to seek health care for symptoms

Nursing Management Nursing Implementation n Respiratory System – Management of the respiratory system is a nursing priority – Risk for aspiration pneumonia (why? ) – Risks for airway obstruction – May require intubation and ventilation

Nursing Management Nursing Implementation n Neurologic System – Monitor closely for deterioration or improvement

Nursing Management Nursing Implementation n Cardiovascular System – Monitor closely – Risk for DVT

Nursing Management Nursing Implementation n Musculoskeletal System – Prevent joint contractures and muscular atrophy – In the acute phase, range-of-motion exercises and positioning – Trochanter roll at hip to prevent external rotation

Nursing Management Nursing Implementation n Musculoskeletal System – Hand cones to prevent hand contractures – Arm supports with slings and lap boards to prevent shoulder displacement

Nursing Management Nursing Implementation n Musculoskeletal System – Avoid pulling patient by arm to avoid shoulder displacement – Posterior leg splints, footboards or high-topped shoes to prevent foot drop – Hand splints to reduce spasticity

Nursing Management Nursing Implementation n Integumentary System – Skin is susceptible to breakdown related to loss of sensation, ↓ circulation, and immobility – Compounded by age, poor nutrition, dehydration, edema, and incontinence

Nursing Management Nursing Implementation n Integumentary System – Pressure relief by position changes, special mattresses, wheelchair cushions – Good skin hygiene – Emollients for dry skin – Early mobility – Position patient affected side for only 30 minutes

Nursing Management Nursing Implementation n Gastrointestinal System – May require nutrition support – Assess gag and swallowing before first feeding – Scrupulous oral hygiene after meals (food collects) – Place food on unaffected side – Foods with texture are more easily swallowed

Nursing Management Nursing Implementation n Gastrointestinal System – Constipation is common – Manage with n Physical activity n Adequate fluid intake n Laxatives, suppositories, stool softeners

Nursing Management Nursing Implementation n Urinary System – In the acute stage poor bladder control is the primary urinary problem, resulting in incontinence – Avoid indwelling catheters

Nursing Management Nursing Implementation n Communication – Assess ability to speak and understand – Speak slowly and calmly, using simple words or sentences – Provide time to express self

Nursing Management Nursing Implementation n Sensory-Perceptual Alterations – Blindness in the same half of each visual field is a common (homonymous hemianopsia) n Difficult to distinguish from unilateral neglect n Initially approach from, and place needed objects on “good” side. Later, teach to scan and pay attention to affected side
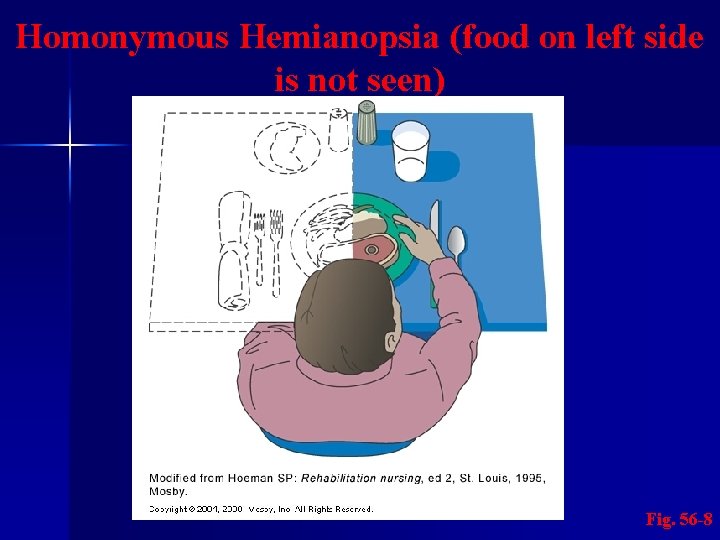
Homonymous Hemianopsia (food on left side is not seen) Fig. 56 -8

Nursing Management Nursing Implementation n Coping – A stroke is often a family disease, affecting the family emotionally, socially, and financially – Changing roles and responsibilities occur

Nursing Management Nursing Implementation n Coping – Clear explanations about what has happened, diagnostic and therapeutic procedures

Nursing Management Nursing Implementation n Ambulatory and Home Care – The patient is usually discharged from the acute care setting to home, an intermediate or long-term care facility, or a rehabilitation facility – Discharge planning should begin early

Nursing Management Nursing Implementation n Ambulatory and Home Care – The nurse initially emphasizes the musculoskeletal functions of n Eating n Toileting n Walking

Nursing Management Nursing Implementation n Ambulatory and Home Care – Most patients begin to show signs of spasticity with exaggerated reflexes within 48 hours following the stroke – Balance training, transferring – Supportive/assistive devices for mobilizing

Nursing Management Nursing Implementation n Ambulatory and Home Care – Interventions to promote self-feeding n Using the unaffected upper extremity n Employing assistive devices such as rocker knives, plate guards, and nonslip pads for dishes

Nursing Management Nursing Implementation n Ambulatory and Home Care – A bowel management program is implemented for problems with bowel control, constipation, incontinence – A high-fiber diet and adequate fluid intake

Nursing Management Nursing Implementation n Ambulatory and Home Care – Family members must cope with 3 aspects of the patient’s behavior 1. 2. 3. Behavioral changes resulting from neurologic deficits Responses to multiple losses Behaviors that may have been reinforced during the early stages of stroke as continued dependency
- Slides: 81