STREPTOCOCCI Dr QuratUlAin Senior Demonstrator Microbiology KEMU Lahore


STREPTOCOCCI Dr. Qurat-Ul-Ain Senior Demonstrator, Microbiology, KEMU, Lahore


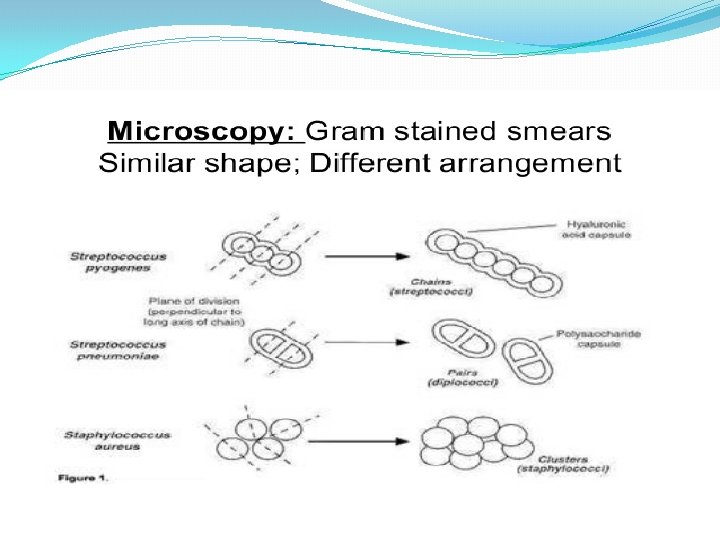
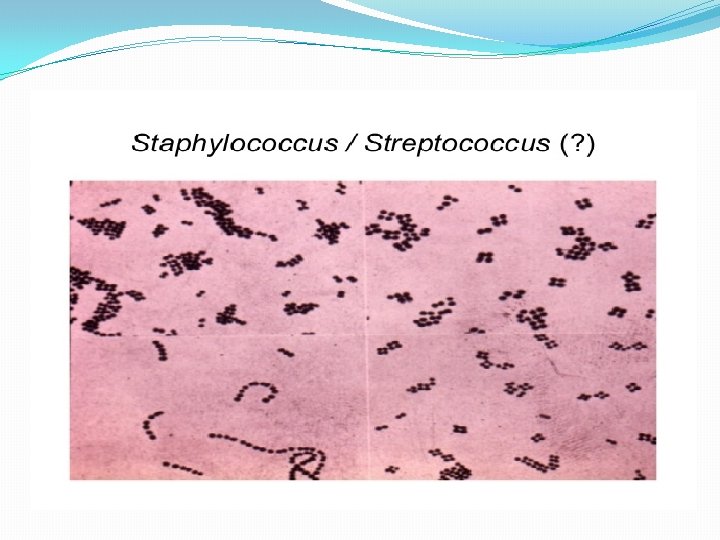
Streptococci � Characters of Streptococci � Gram positive cocci � 1µm in diameter � Chains or pairs � Usually capsulated � Non motile � Capnophili. C � Non spore forming � Facultative anaerobes � Fastidious � Catalase negative (Staphylococci are catalase positive)

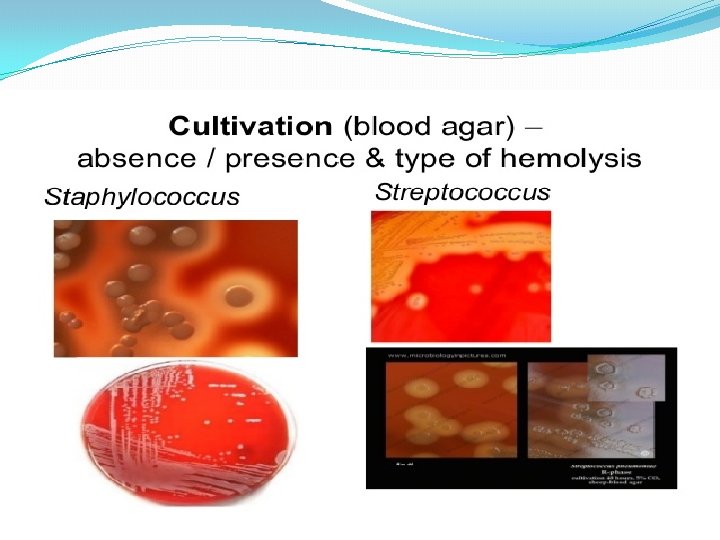
Classification Of Streptococci �Streptococci can be classified according to: �Oxygen requirements � Anaerobic (Peptostreptococcus) � Aerobic or facultative anaerobic (Streptococcus) �Serology (Lanciefield Classification) �Hemolysis on Blood Agar (BA)
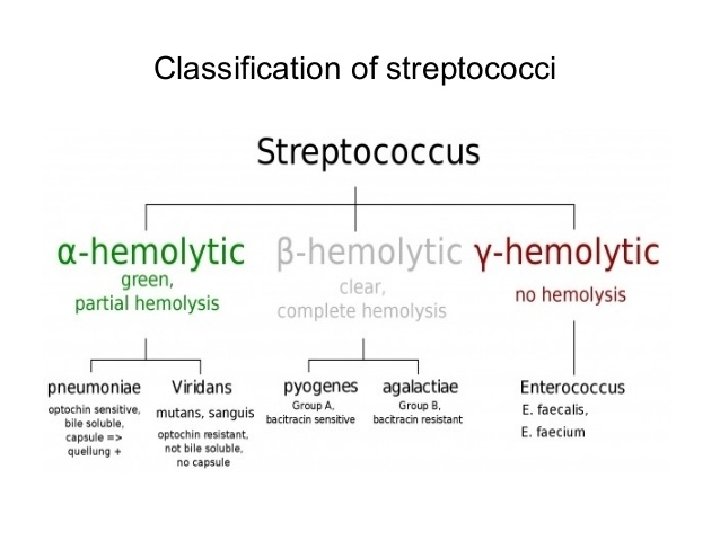
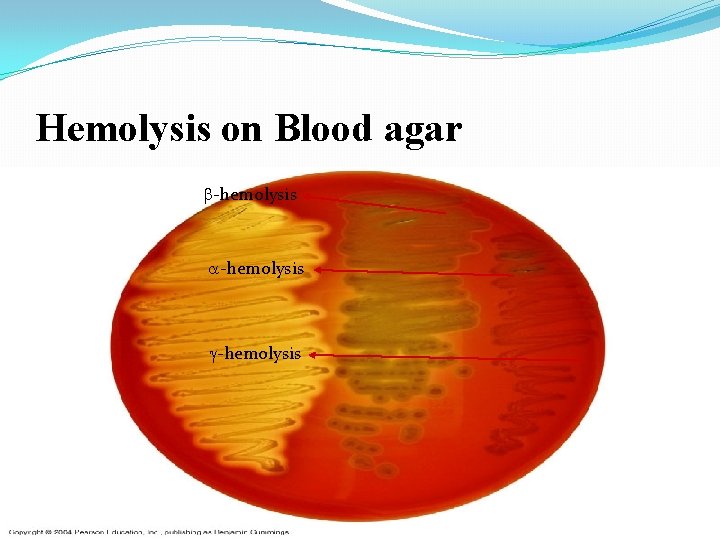
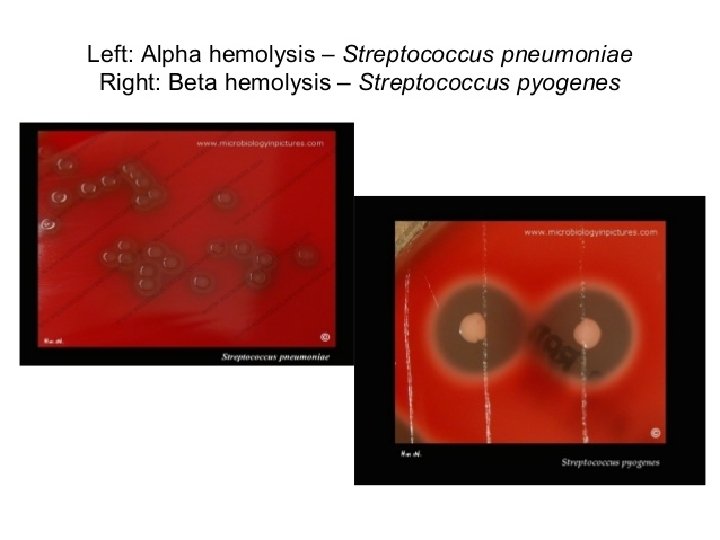
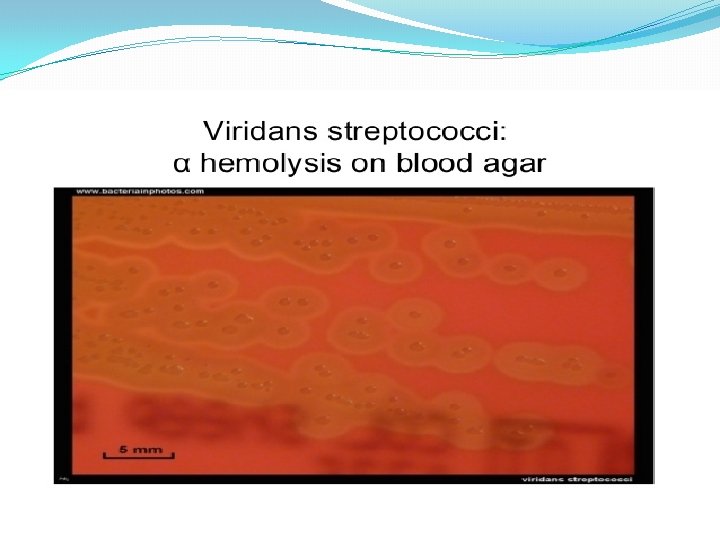
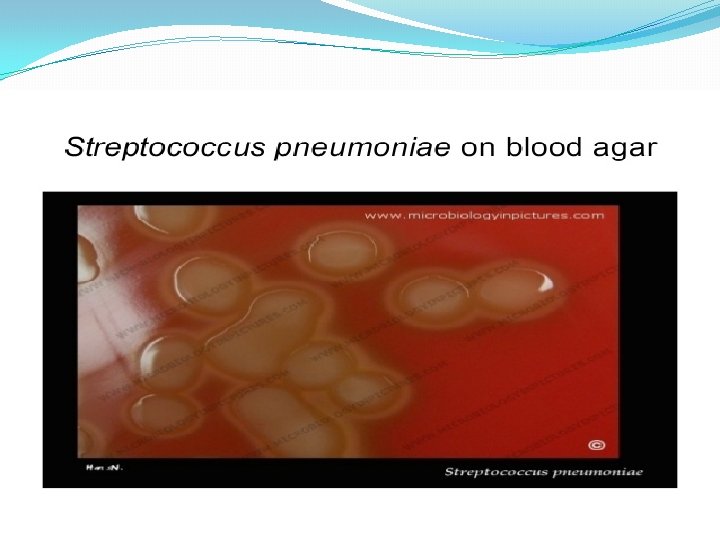
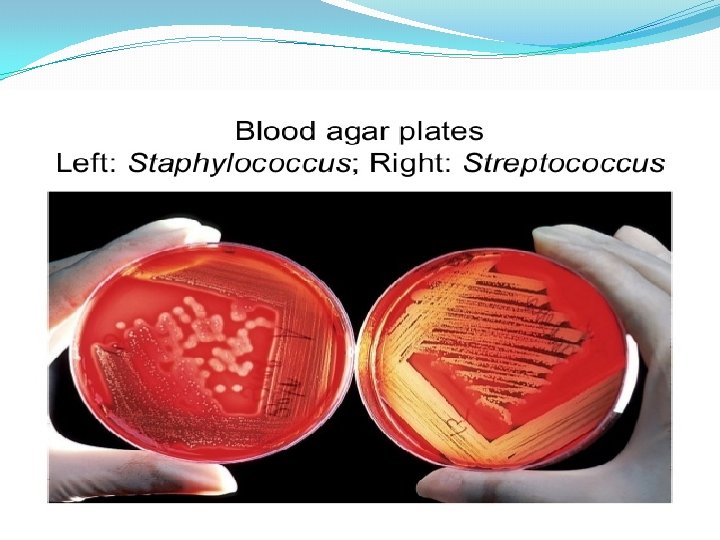
Hemolysis on Blood agar -hemolysis
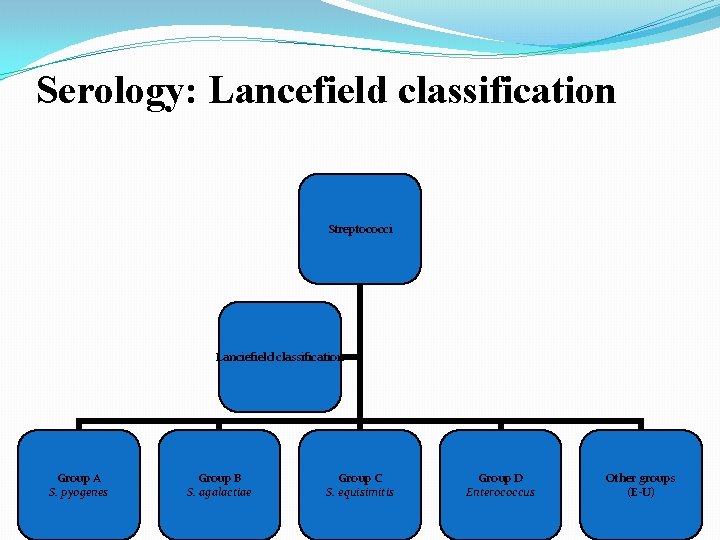
Serology: Lancefield classification Streptococci Lanciefield classification Group A S. pyogenes Group B S. agalactiae Group C S. equisimitis Group D Enterococcus Other groups (E-U)

�Streptococci classified into many groups from A-K & H-V �One or more species per group �Classification based on C- carbohydrate antigen of cell wall �Groupable streptococci � A, B and D (more frequent) � C, G and F (Less frequent) �Non-groupable streptococci � S. pneumoniae (pneumonia) � viridans streptococci �e. g. S. mutans �Causing dental carries




Group A Streptococci �Include only S. pyogenes �Group A streptococcal infections affect all ages peak incidence at 5 -15 years of age � 90% of cases of pharyngitis

GAS: Strep pyogenes

Strep. Virulence Factors

Determinants of Pathogenicity Cellular Virulence Factors 1. Capsule Antiphagocytic; Nonspecific adherence Hyaluronic acid (polysaccharide) mimics animal tissue 2. Lipoteichoic Acid Cytotoxic for wide variety of cells Adherence: Complexes with M protein (LTA-M) and binds to fibronectin on epithelial cells 3. M-Protein LTA-M protein is adhesin Antiphagocytic Inhibits alternate C’ pathway and opsonization 4. M-like Proteins: bind Ig. M and Ig. G 5. F Protein: mediates adherence

Extracellular Virulence Factors Exotoxins: 1. Streptolysin O (SLO): Ø Hemolytic and Cytolytic Ø Prototype of oxygen-labile and thiol-activated cytolytic exotoxins (e. g. , Streptococcus, Bacillus, Clostridium, Listeria) Ø Lytic for variety of cells: bind to cholesterol-containing membranes and form arc- or ring- shaped oligomers that make cell leaky (RBC's, WBC’s, PMN's, platelets, etc. ) Ø Causes sub-surface hemolysis on BAP Ø Stimulate release of lysosomal enzymes Ø SLO titer indicates recent infection (300 -500 in pediatric populations)

Extracellellular Virulence Factors (cont. ) Exotoxins (cont. ): 2. Streptolysin S (SLS): Ø Hemolytic and Cytolytic Ø Oxygen stable, non-antigenic Ø Lytic for red and white blood cells and wall-less forms (protoplast, Lforms) Ø Causes surface hemolysis on BAP

Extracellular Virulence Factors (cont. ) Exotoxins (cont): 3. Pyrogenic (Erythrogenic) Exotoxins (Types A, B &C) Produced by more than 90% of Grp A strep Ø Mediate pyrogenicity (fever) Ø Causes scarlet fever (scarletiniform) rash Ø Increase susceptibility to endotoxic shock Ø Type C toxin increases permeability of blood-brain barrier Ø Mitogenic for T lymphocytes (cause cell division), myocardial and hepatic necrosis, decrease in antibody synthesis Ø Immunomodulators (superantigens): stimulate T cells to release cytokines Cardiohepatic toxin

Extracellular Virulence Factors (cont. ) Enzymes: 1. Nucleases: Four antigenic types (A, B, C, D) Facilitate liquefication of pus generating growth substrates Nucleases A, C have DNase activity Nucleases B, D also have RNase activity 2. Streptokinases: Lyse blood clots: catalyze conversion of plasminogen to plasmin, leading to digestion of fibrin 3. C 5 a Peptidase: destroys C’ chemotactic signals (C 5 a) 4. Hyaluronidase: hydrolyzes hyaluronic acid 5. Others: Proteinase, NADase, ATPase, phosphatase, etc.

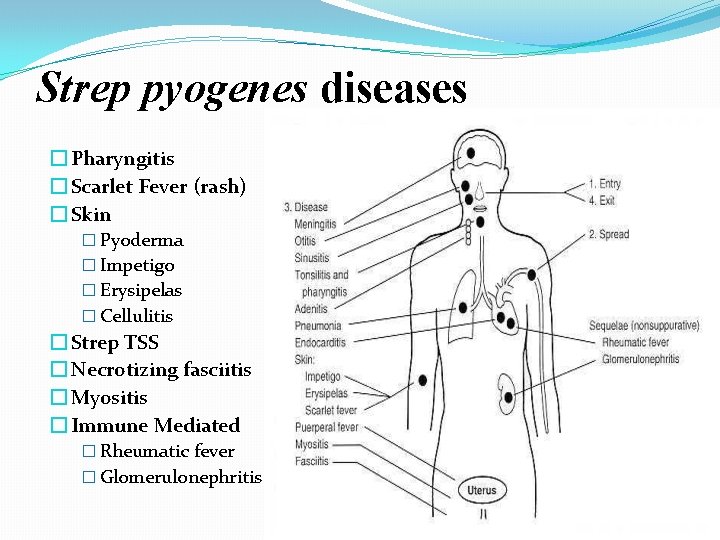
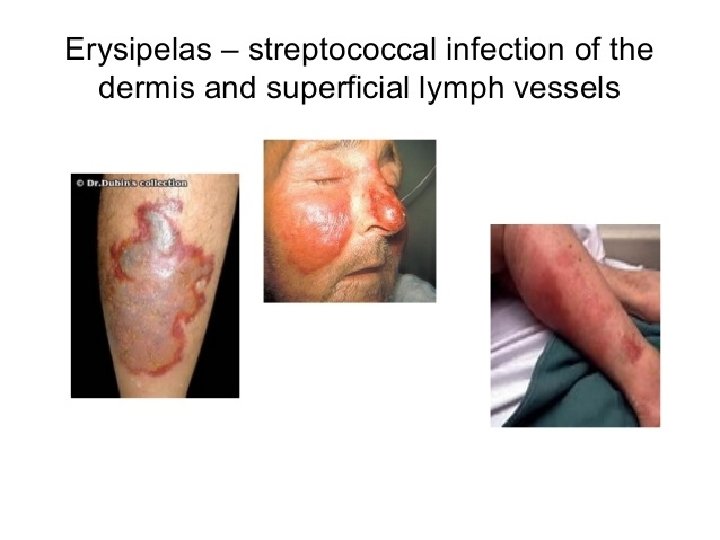
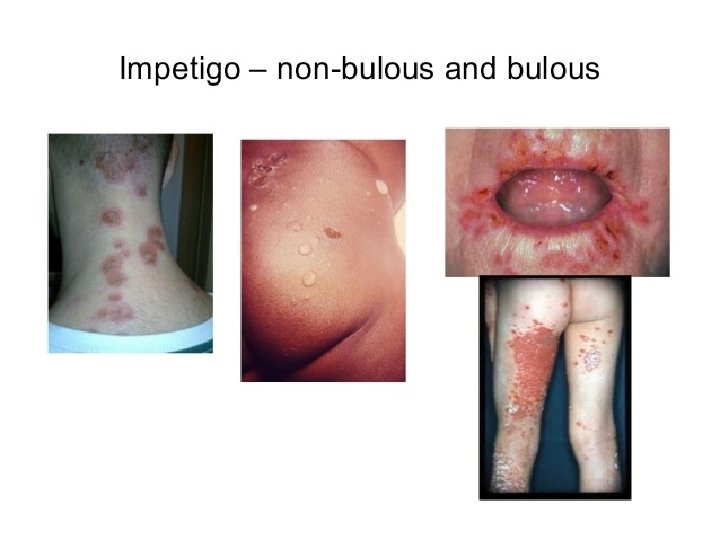
Strep pyogenes diseases � Pharyngitis � Scarlet Fever (rash) � Skin � Pyoderma � Impetigo � Erysipelas � Cellulitis � Strep TSS � Necrotizing fasciitis � Myositis � Immune Mediated � Rheumatic fever � Glomerulonephritis

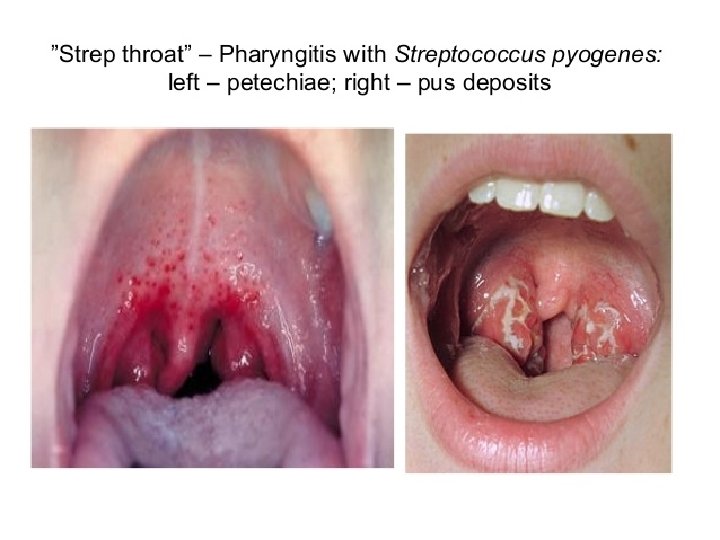
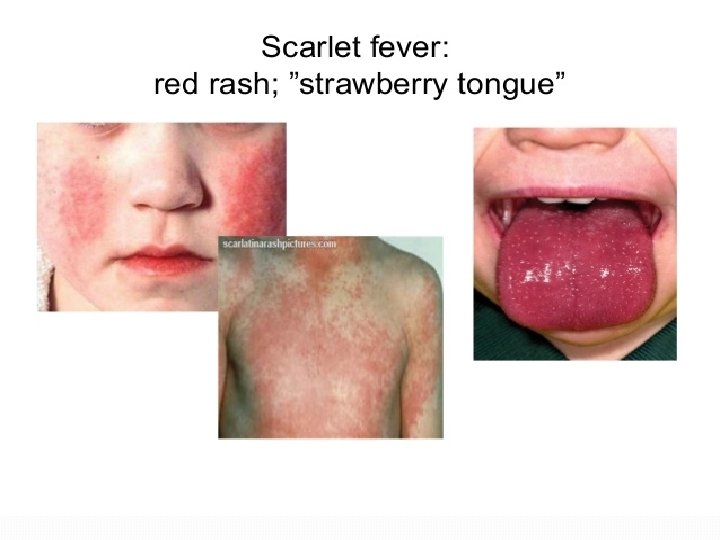
Diseases Caused By S. Pyogenese 1. Suppurative �Non-Invasive: Pharyngitis (“strep throat”)-inflammation of the pharynx � Skin infection, Impetigo � �Invasive Scarlet fever-rash that begins on the chest and spreads across the body � Pyoderma-confined, pus-producing lesion that usually occurs on the face, arms, or legs � Necrotizing fasciitis-toxin production destroys tissues and eventually muscle and fat tissue �

Non Suppurative: �Rheumatic fever: Life threatening inflammatory disease that leads to damage of heart valves muscle �Glomerulonephritits: �Immune complex disease of kidney �inflammation of the glomeruli and nephrons which obstruct blood flow through the kidneys
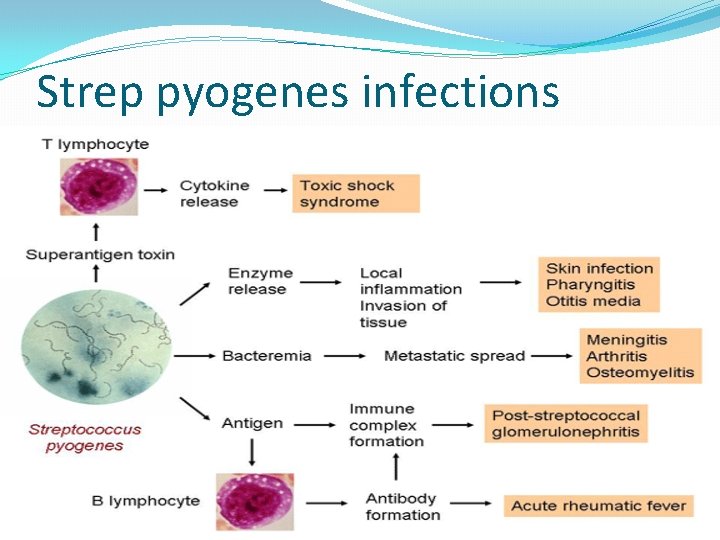
Strep pyogenes infections

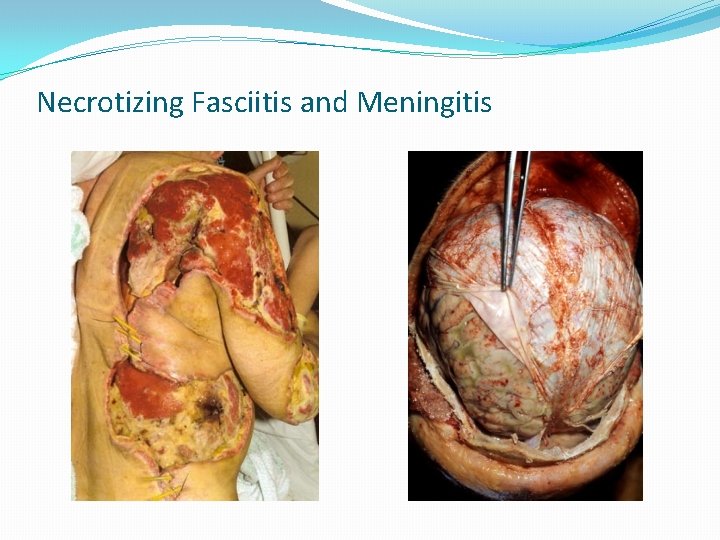
Necrotizing Fasciitis and Meningitis

Nonsuppurative Sequelae of Acute Group A Streptococcal Infection Acute Rheumatic Fever (ARF) Inflammatory reaction characterized by arthritis, carditis, chorea (disorder of CNS with involuntary spastic movements), erythema marginatum (skin redness with defined margin), or subcutaneous nodules Within 2 -3 weeks following pharyngitis Morbidity & mortality linked to subsequent disease of heart valve Heart Disease) (Rheumatic Poorly understood pathogenesis with several proposed theories including crossreactivity of heart tissues & strep AGNs • ? ? (Type ? ? II hypersensitivity, exotoxins, direct invasion)


Nonsuppurative Sequelae of Acute Group A Streptococcal Infection (cont. ) Acute Glomerulonephritis : Follows either respiratory (pharyngitis) or cutaneous (pyoderma) streptococcal infection Associated with well-defined group of M-types Most often seen in children manifesting as dark, smoky urine with RBC's, RBC casts, white blood cells, depressed serum complement, decreased glomerular filtration rate Latent period: 1 -2 weeks after skin infection and 2 -3 weeks after pharyngitis Granular accumulations of immunoglobulin due to deposition of immune complexes within the kidney (Type ? ? III Hypersensitivity)

Differentiation between -hemolytic streptococci �The following tests can be used to differentiate between hemolytic streptococci �Lanciefield Classification �Bacitracin susceptibility Test �Specific for S. pyogenes (Group A) �CAMP test �Specific for S. agalactiae (Group B)

Bacitracin sensitivity �Principle: � Bacitracin test is used for presumptive identification of group A � To distinguish between S. pyogenes (susceptible to B) & non group A such as S. agalactiae (Resistant to B) � Bacitracin will inhibit the growth of gp A Strep. pyogenes giving zone of inhibition around the disk �Procedure: � Inoculate BAP with heavy suspension of tested organism � Bacitracin disk (0. 04 U) is applied to inoculated BAP � After incubation, any zone of inhibition around the disk is considered as susceptible

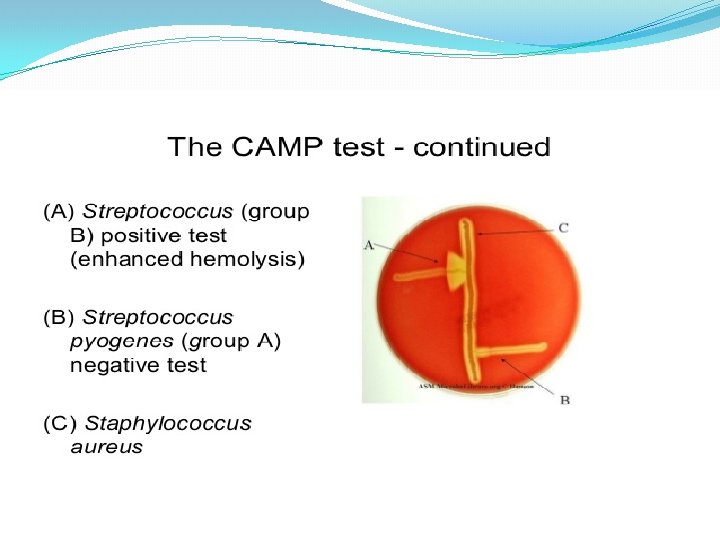
CAMP test � Principle: � Group B streptococci produce extracellular protein (CAMP factor) � CAMP act synergistically with staph. -lysin to cause lysis of RBCs � Procedure: � Single streak of Streptococcus to be tested and a Staph. aureus are made perpendicular to each other � 3 -5 mm distance was left between two streaks � After incubation, a positive result appear as an arrowhead shaped zone of complete hemolysis � S. agalactiae is CAMP test positive while non gp B streptococci are negative

CAMP test

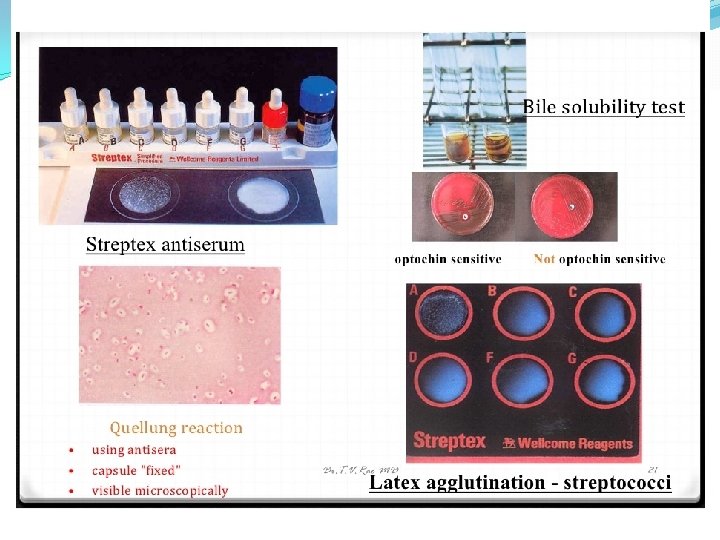
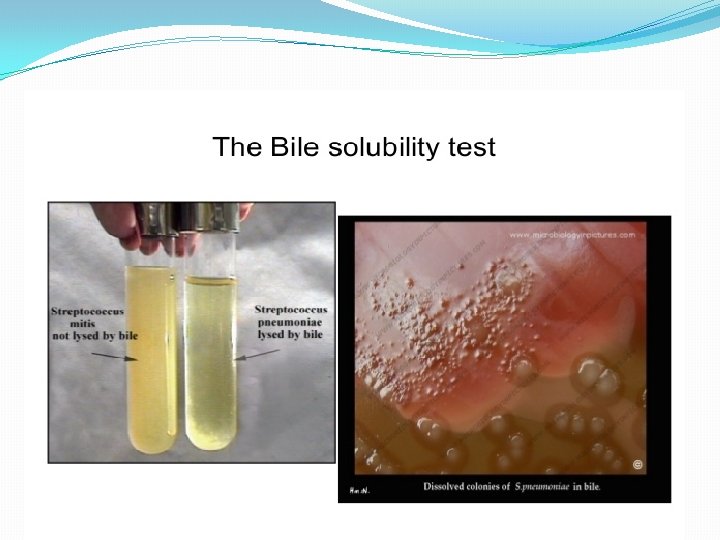
Differentiation between -hemolytic streptococci �The following definitive tests used to differentiate between S. pneumoniae & viridans streptococci �Optochin Test �Bile Solubility Test �Inulin Fermentation
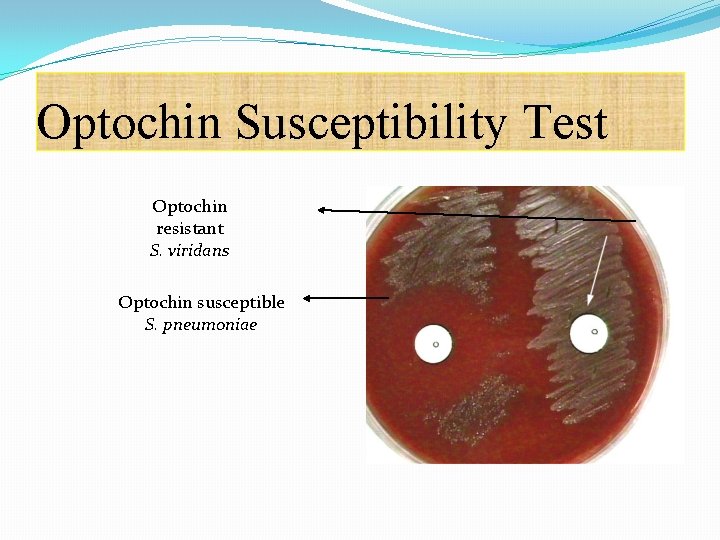
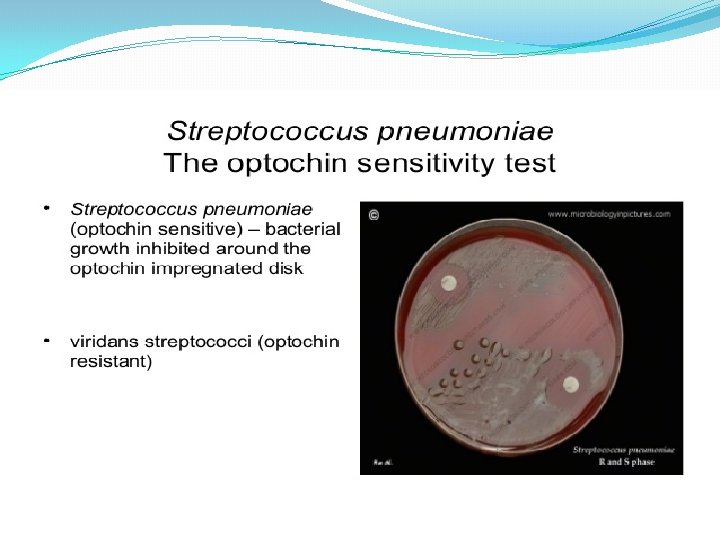
Optochin Susceptibility Test Optochin resistant S. viridans Optochin susceptible S. pneumoniae






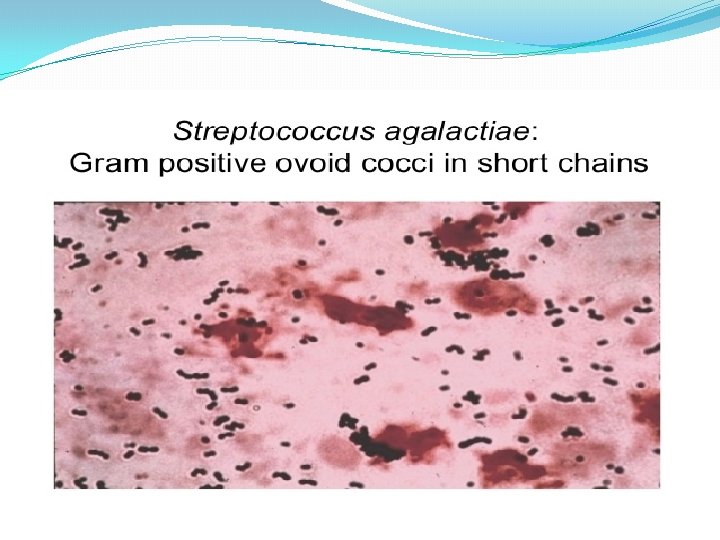
GBS: Strep agalactiae � Epidemiology � GI � Uritogenital � Pathogenicity � Capsule � Enzymes � Proteases � Hemolysins � Beta hemolysis � Hyaluronidase � Disease � Puerperal fever � Vaginitis � UTI � Endocarditis � Osteomyelitis � Newborn � Meningitis, sepsis, pneumonia

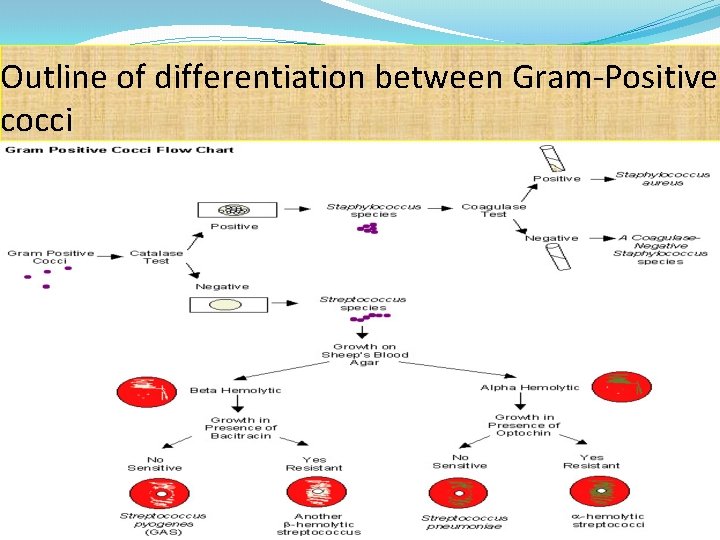
Outline of differentiation between Gram-Positive cocci



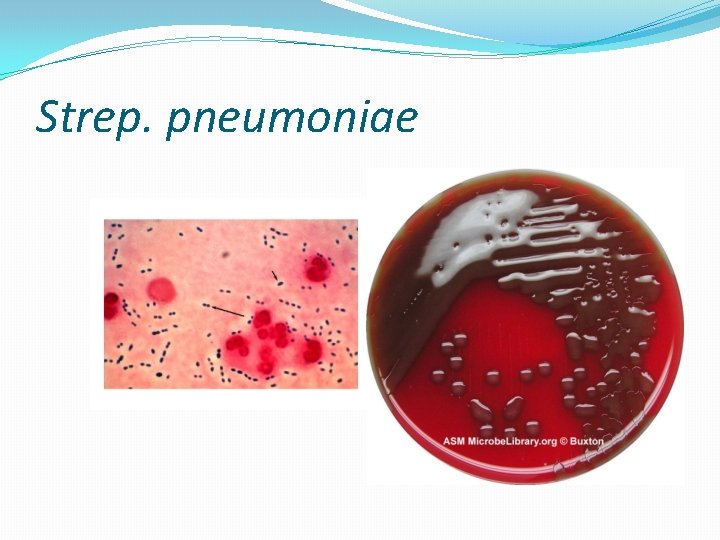
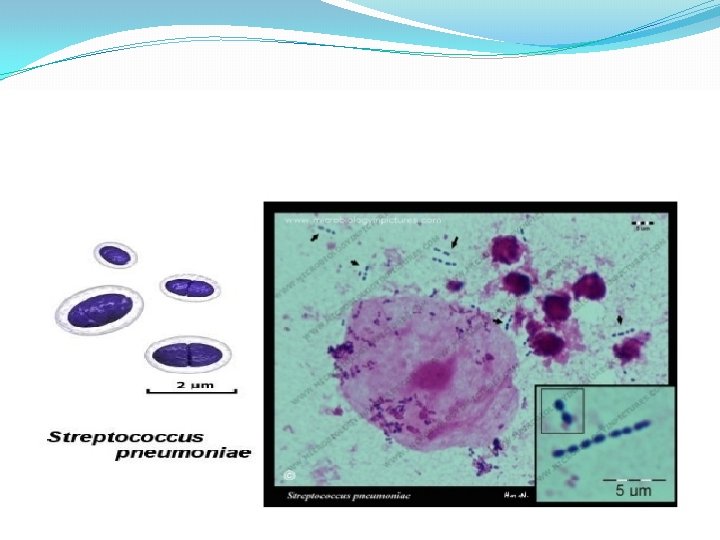
Strep. pneumoniae
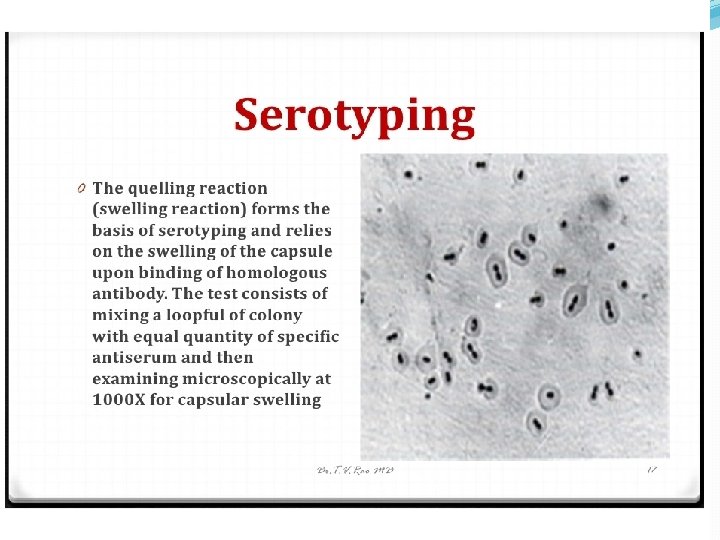
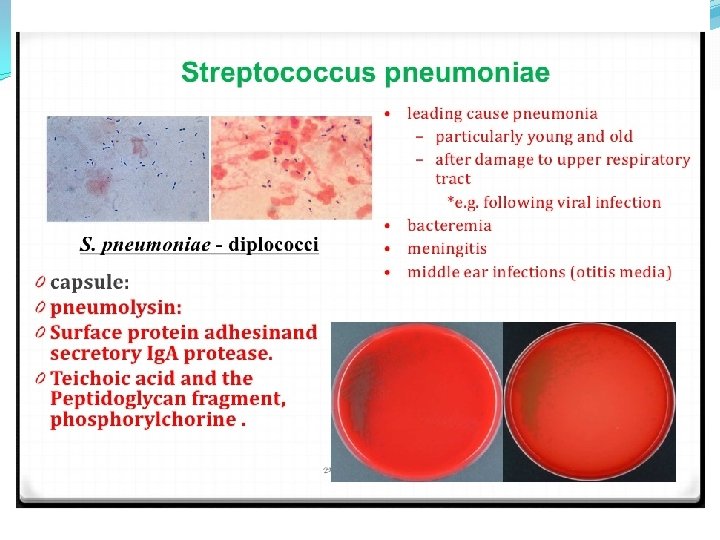
Strep pneumonia capsule
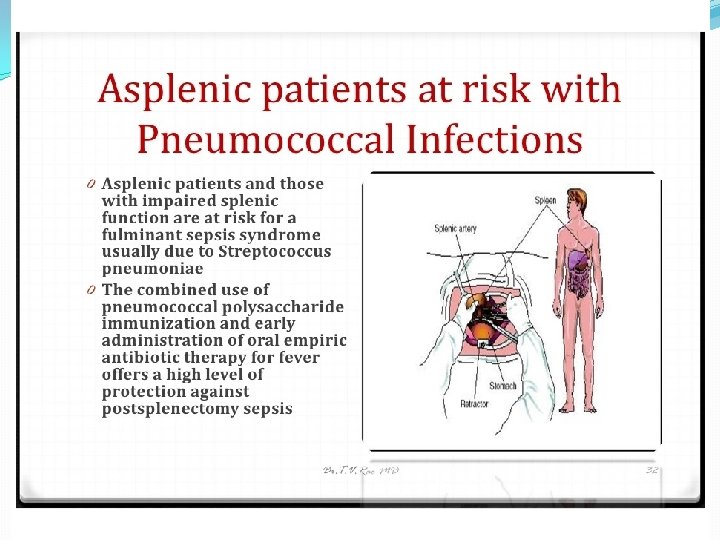
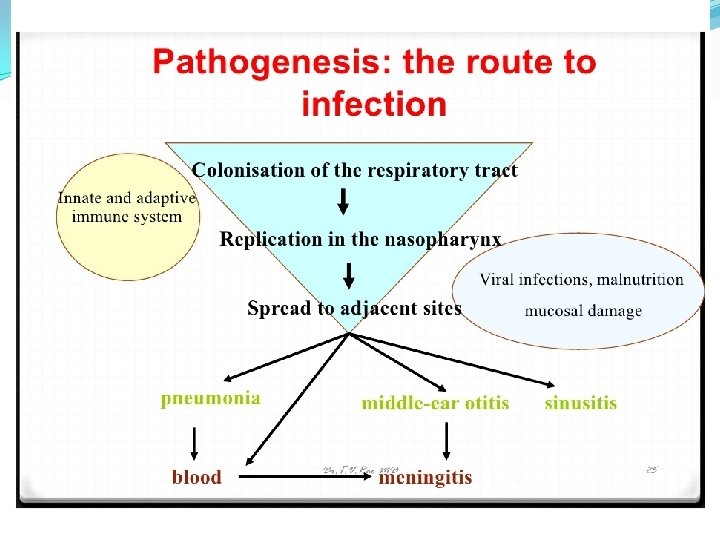
Strep pneumoniae �Epidemiology � Mouth � Upper respiratory � Dz = lungs �Pathogenicity � Capsule � Protein A � Phosphorylcholine � Adhesins � Proteases � Protects from Ig. A �pneumolysins
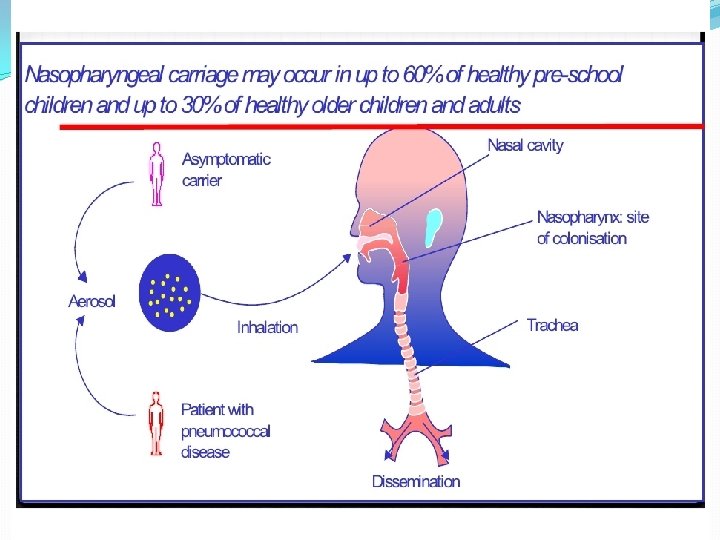
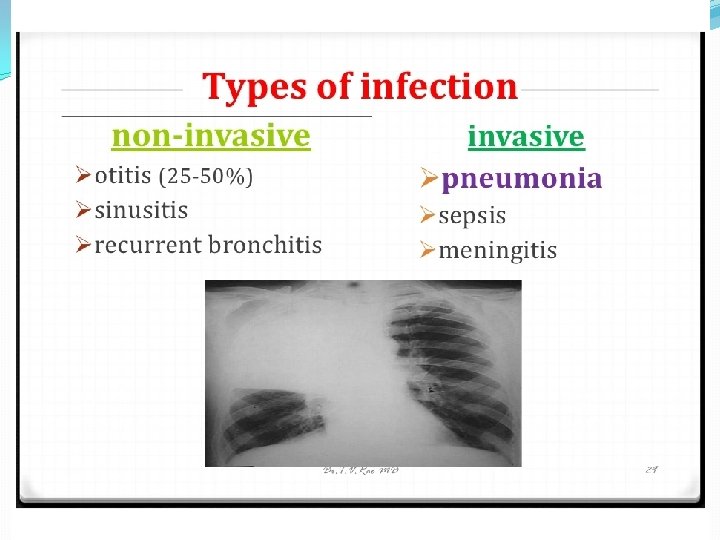
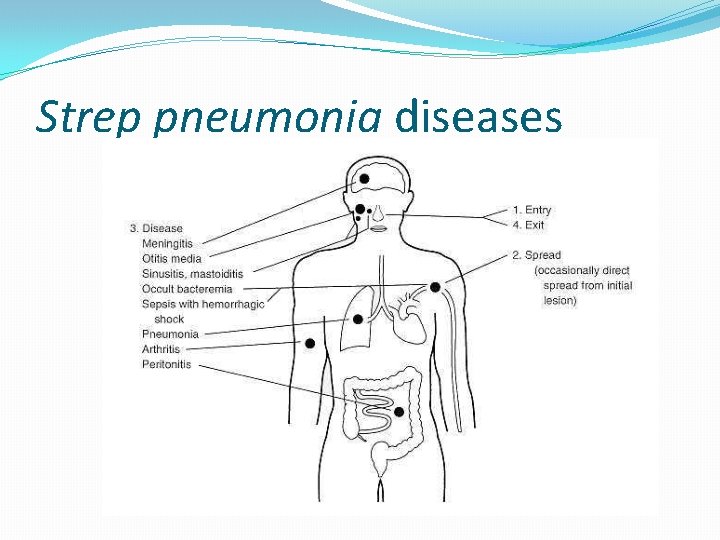
Strep pneumonia diseases






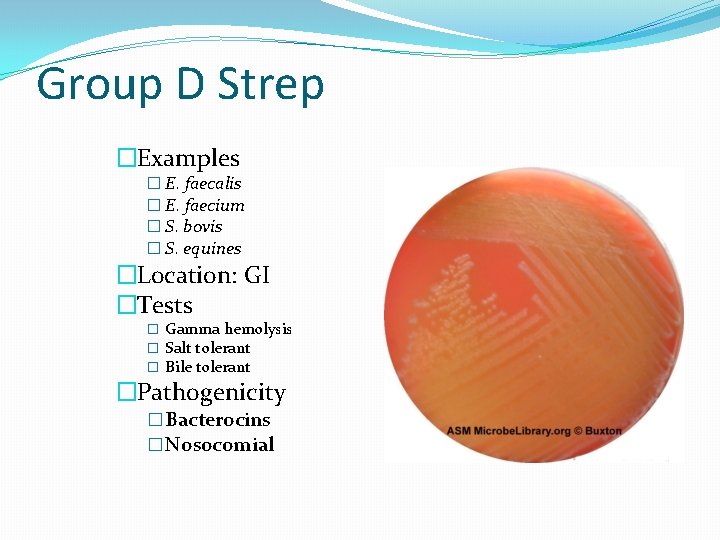
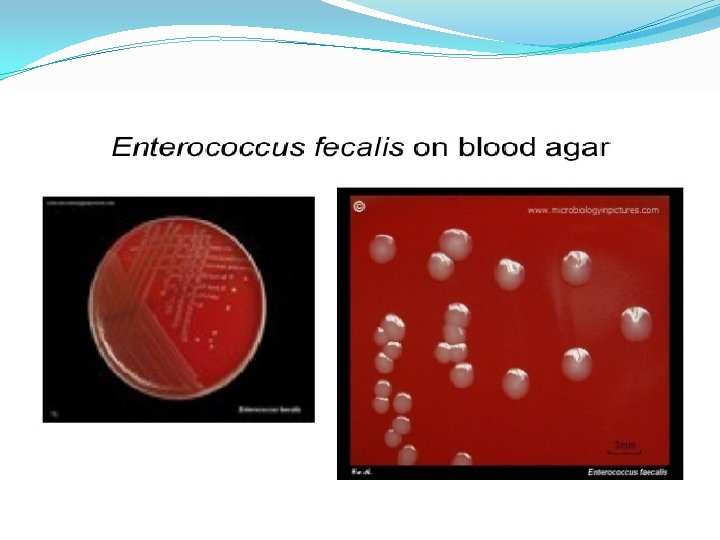
Group D Strep �Examples � E. faecalis � E. faecium � S. bovis � S. equines �Location: GI �Tests � Gamma hemolysis � Salt tolerant � Bile tolerant �Pathogenicity � Bacterocins � Nosocomial
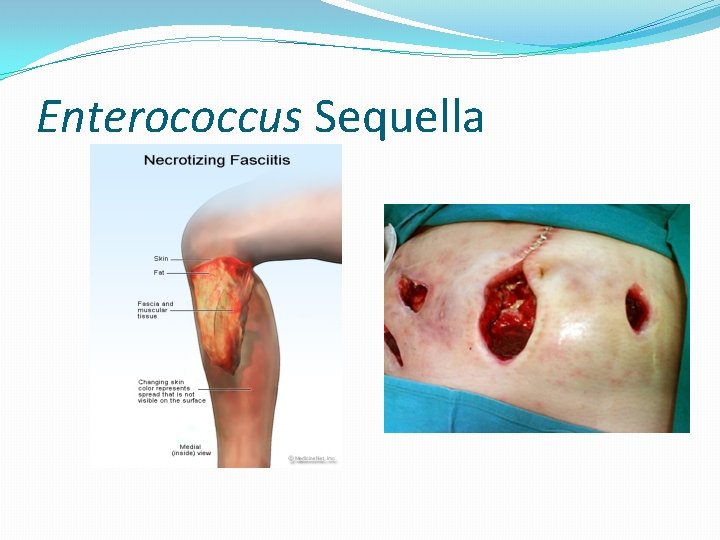
Enterococcus Sequella











- Slides: 94