Strabismus Omar Abughanimeh Seminar content Introduction Definition Causes

Strabismus Omar Abughanimeh

Seminar content • • Introduction Definition Causes Classifications Consequences Approach to patient with strabismus Management

Introduction • Eye movement controlled by: 1 - extraocular muscles 2 -cranial nerves ( III, IV, VI) • 3 - higher cortical functions through the gaze centers

Yoked movement vs. antagonistic movement • Suppose that you ask the patient to look to the right side , which muscles will work ? ? Hering’s law vs sherrington’s law

Normal Vision Actions of EOMs • Normal binocular single vision (BSV) involves the simultaneous use of both eyes with bifoveal fixation directed to the same target, so that each eye contributes to a common single perception of the object of regard. • Stereopsis : the perception of depth produced by the reception in the brain of visual stimuli from both eyes in combination; binocular vision “ 3 D”

• Projection is the subjective interpretation of the position of an object in space on the basis of stimulated retinal elements. • Corresponding ‘points’ areas on each retina that share the same subjective visual direction.
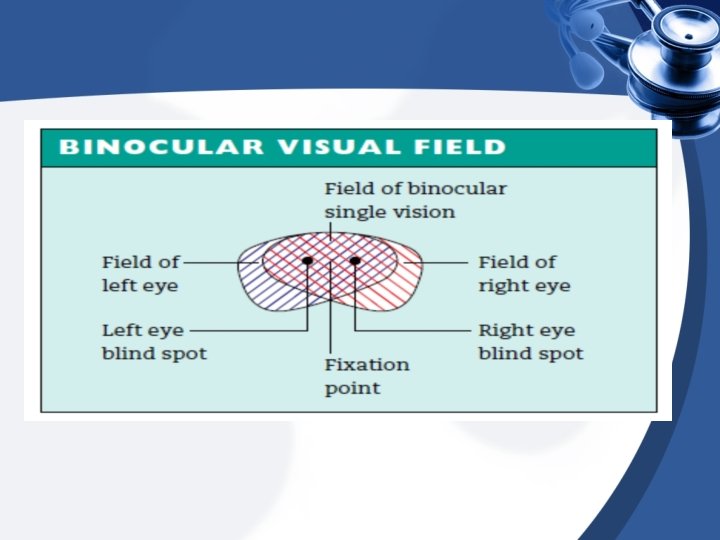

Advantages of Binocular Single Vision & Stereopsis 1 -Increased field of vision 2 -Elimination of blind spot 3 -Binocular acuity (see fine details & color, better than with monocular acuity) 4 -Depth perception (stereopsis)

Abnormal Binocular Single Vision • If the visual axis of the 2 eyes are not aligned , Binuclear vision Is NOT possible. Results in : >>Diplopia ; An object is seen to be in 2 different places. • • >>Visual confusion ; 2 separate objects appear to be at the same point. A non-alignment of the visual axis of the 2 eyes ( SQUINT) results in suppression of the image in the squint eye , this means when vision is tested in the 2 eyes together no diplopea. - If prolonged during period of visual development reduced visual acuity in the squint eye ( strabismic Amblyopia). - Amblyopia will develop only if constant squint affects the same eye. children Alternating the squinting eye will NOT develop Amblyopia but do NOT develop Stereopsis either. -

Definition • Strabismus : is deviation of an eye’s visual axis from it’s normal position. • Strabismus = squint = ﺍﻟﻝ • Strabismus can be either: – a lack of coordination between the extraocular muscles. – a disorder of the brain in coordinating the eyes. – or of one or more of the relevant muscles' power or direction of motion

why squint is important • ● A squint may show that the acuity of the • eye is impaired ● A squint may itself cause amblyopia in a • child ● A squint may be a sign of a life • threatening condition like retinoblastoma

CLASSIFICATION OF STRABISMUS • 1. DIRECTION OF DEVIATION - Hyper deviation - Hypo deviation - Divergent - Convergent • 2. COMITANCY - concomitant / non-paralytic - incomitant / paralytic • 3. CONSTANCY - constant - intermittent

Another classification • Apparent squint or pseudostrabismus • Pseudoesotropia • Pseudoexotropia • Latent squint (heterophoria) is only present after binocular vision has been interrupted, typically by covering one eye • • • Esophoria Exophoria Hyperphoria Hypophoria Cyclophoria (deviation In the ant. post axis)

• Manifest squint (heterotropia) is present while the patient views a target binocularly, with no occlusion of either eye. The patient is unable to align the gaze of each eye to achieve fusion – Concomitant squint ( angle of deviation remains the same whatever the eye movement) the deviating eye accompanies the leading eye in every direction of gaze. • • Esotropia Exotropia Hypertropia Hypotropia – Incomitant squint: result from paralysis of one or more eye muscles , which differs from the first type in that the angle of deviation it’s not constant in every direction of gaze • Paralytic strabismus • ** Concomitant usually occurs in children because it mainly congenital within the first few years of life , whereas Paralytic strabismus primarily affects adults because its usually acquired “post-traumatic.

Terminology !! • Eso : inward • Exo: outward • Hyper: superiorly • Hypo: inferiorly -------------- • Tropia : always deviated ( manifest squint) • Phoria : sometimes deviated (latent squint)

Pseudostrabismus • False appearance of crossed eyes • Occurs in infants and toddlers whose facial features are not fully developed • With age, the nose bridge will narrow and the epicanthal folds in the corner of the eyes will go away. This will cause the eyes to appear wider, and thus not have the appearance of strabismus

Heterophoria • It can be : • • • Esophoria Exophoria Hyperphoria Hypophoria Cyclophoria (deviation In the ant. post axis) • Heterophoria is a latent tendency for misalignment of the two eyes that becomes a manifest only if binocular vision is interrupted such as by covering one eye • Heterophoria only occurs during dissociation of the left eye and right eye, when fusion of the eyes is absent. If you cover one eye (e. g. with your hand) you remove the sensory information about the eye's position in the orbit. Without this, there is no stimulus to binocular fusion, and the eye will move to a position of "rest".

Heterophoria • A minor degree of heterophoria is normal for most individuals • Both esophoria and exophoria can be classified by the distance at which the angle is greater: (respectively, convergence excess or weakness, divergence weakness or excess and mixed). • Treatment – Orthoptic treatment is of most value in convergence weakness exophoria – Symptom relief may otherwise be obtained using temporary stick-on Fresnel prisms and may be subsequently incorporated into spectacles (maximum usually 10– 12 , split between the two eyes) – Surgery may occasionally be required for larger deviations

• So to differentiate by examination paralytic from non paralytic we measure the angle of deviation by prism • The angle of deviation is measured with a cover test in combination with the use of prism lens of various refractive powers • If the angle is the same in all directions then it is non paralytic • If it is different then it is paralytic • This angle is important for follow up and deciding upon surgery

CONCOMITANT(NONPARALYTIC) • Movement of both eyes are full (there is no paresis) but only one eye is directed towards the fixated target. • The angle of deviation is constant and unrelated to the direction of gaze v v Concomitant strabismus almost exclusively in children. In 60 -70% of all cases manifests within the first two years of life • Under age of 6, it is rarely caused by serious neurological disease. It’s usually primary in this age group. • Strabismus arising later in life may have a specific and serious neurological basis. - could be : monocular, alternating or intermittent.

Etiology The causes of concomitant are often unclear. But the following causes have been identified to date : v Genetic factors v Uncorrected refractive errors : Children with hypertropia tend to have esotropia , this is because accommodation always triggers a convergence impulse that can cause esotropia v Unilateral visual impairment : like corneal scarring , cataract , macular changes , retinal disorder “retinoblastoma” etc. . v Insufficient fusion : this occur in conjunction with anisometropia (unequal refractive power in the both eyes ) and aniseikonia (unequal retinal image size ) v Other possible causes: perinatal lesion as preterm &asphyxia syndromes “Noonan syndrome Prader-Willi syndrome cerebral trauma and encephalitis • • incidence. : 60% of children with strabismus have family history of increased
Pathophysiology: Deviation of the visual axis of the deviating eye causes objects to be projected to noncorresponding points on the retina. One would expect these patients suffer from constant double vision because the left and right eyes supply different information to the brain. A central inhibiting mechanism suppresses the visual stimuli from the deviating eye.

Instead of seeing two different images or double vision (diplopia), the brain suppresses the blurrier image. The inhibition process (suppression) can result in a permanent decrease in the vision in the blurry eye that can not be corrected with glasses, lenses, or lasik surgery. This will lead to Amblyopia

Esotropia is one of the most commonly encountered forms of strabismus. v v Esotropia (convergent strabismus) occurs more frequently than Exotropia (divergent strabismus) in Europ and north america.

Types of esotropia strabismus Congenital or infantile : present at birth or after 6 months which characterized by: v large alternating angle of deviation “ as in the next pic” v lack of binocular vision v primary oblique muscle dysfunction “hypertropia” v A or V pattern : a. A pattern deviation : refers to inward angle of deviation that increase in upgaze and decrease in downgaze b. V pattern deviation : refers to inward angle of deviation that decrease in upgaze and increase in downgaze 1)
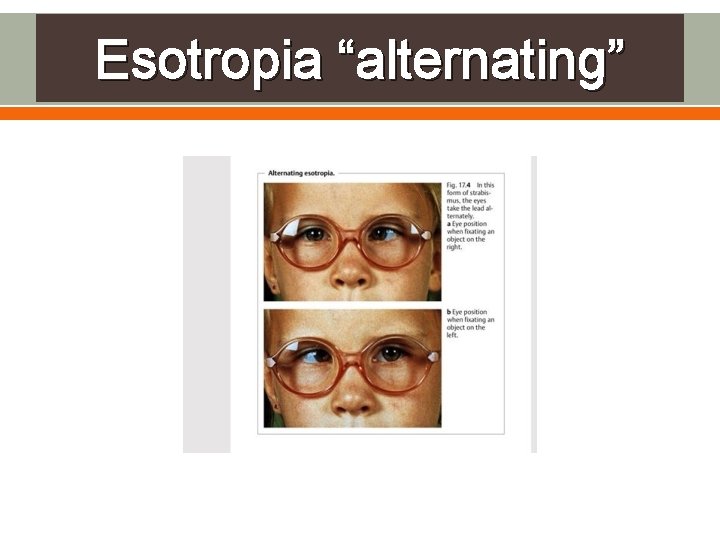
Esotropia “alternating”

Types of esotropia strabismus 2) Acquired strabismus : two forms A. Strabismus begins at the age of incomplete sensory development i. e. between the ages of one to three years and usually the disorder manifests itself at the age of two and lead to sensory adaption syndrome in the form of unilateral strabismus. • B. • Amblyopia is usually already present , and correspondence is primarily anomalous Strabismus manifests itself between the age of three and seven years. This form of late strabismus with normal sensory development is encountered far less frequently than other form As a binocular vision is already well developed cannot immediately suppress the visual of the deviating eye , as a result , they suffer from sudden double vision , which they attempt to suppress by closing one eye

Types of esotropia strabismus Microstrabismus Is defined as unilateral esotropia with minimal cosmetic effect, i. e. , an angle of deviation of 5 degrees or less. As a result, is often diagnosed too late “ only at the age of four to six “ by the time the resulting Amblyopia in the deviating eye may be sever Another sequel is retinal correspondence , However ! It can no longer be improved by treatment , for that treatment is limited to occlusion therapy to correct amblyopia 3)

Types of esotropia strabismus 4) Accommodative esotropia in accommodative esotropia the angle of deviation is larger with close objects than with distant objects this is When the accommodative convergence /accommodation ratio is abnormal , the angle of deviation depending on whether the fixated object is far or near. • This disorder is corrected with bifocal eyeglasses which in this case we have a strong near-field correction • A residual angle of deviation may remain despite the eyeglass , however the angle may also improve to the point that the visual axes are parallel with good binocular vision.

Types of esotropia strabismus


Exotropia (divergent strabismus “outward” ) is less common than esotropia , as it is usually acquired , more often in adults. exotropia less frequently leads to amblyopia because is often alternating. Occasionally what is known as “panorama vision” will occur in which case the patent has an expanded binocular field vision.

Types of exotropia Intermittent exotropia this is the most common form of divergent strabismus , in this case an angle of deviation is present only when the patient gazes into the distance , the patient has normal binocular vision in near fixation. 1) • The intermittent exotropia only become manifest under certain conditions such as fatigue

Types of exotropia

Types of exotropia Secondary exotropia Occurs with reduced visual acuity in one eye resulting from disease or trauma. 2) 3) Consecutive exotropia Occur after esotropia surgery. Often the disorder is overcorrected

=> RECALL <= - Amblyopia will develop only if constant squint affects the same eye. - Children Alternating the squinting eye will NOT develop Amblyopia but do NOT develop Stereopsis either.

Incomitant (paralytic) • The degree of misalignment varies with direction of the gaze. • One or more of the extraocular muscles or nerves may not be functioning properly, or normal movement may be restricted mechanically. • This type of strabismus may indicate either a nerve palsy or extraocular muscle disease.

Peripheral lesion of an extraocular muscle or its nerve supply results in impaired eye movements. The size of the squint is dependent on the direction of the gaze and thus, for nerve palsy, is greatest in the field of action in the affected muscle ( the direction in which the muscle normally take the globe ). Ends with diplopia

Paralytic squint • Isolated nerve palsies • • systemic disease ( DM, hypertension) Orbital disease (neoplasia) Trauma most common cause of palsy of 4 th, 6 th Raised intracranial pressure may cause a 3 rd or 6 th nerve palsy • Extraocular muscle disease • • • Dysthyroid eye disease (thyroid eye disease) Myasthenia gravis Ocular myositis Ocular myopathy Browns syndrome (malfunction of the superior oblique tendon).

mostly in adults, acquired • present mainly with diplopia • greatest deviation in field of action of the • weakened muscle visual acuity is usually unaffected in either • eye, unless CN II is involved

History and examination The patient complain of diplopia, there may be head posture to compensate for the eye to move in particular direction. In third nerve palsy: • failure of adduction, elevation and deprssion of the eye. Ptosis in some cases, a dilated pupil due to involvement of autonomic fibres. A fourth nerve palsy result in defective • depression of eye when attempted in adduction. A sixth nerve palsy results in failure of abduction • of the eye.

Cranial nerve palsy: Each nerve may be affected at any • point along its course from brainstem nucleus to orbit. In most cases there is not a complete • loss of action of a muscle but a partial loss.
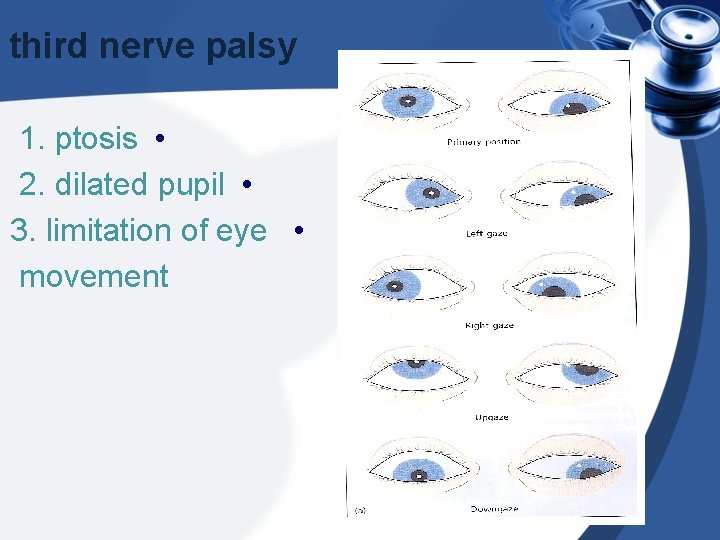
third nerve palsy 1. ptosis • 2. dilated pupil • 3. limitation of eye • movement

4 th nerve palsy the defect is maximal when the patient tries to look “ • down when the left eye is adducted( because the contribution of the superior oblique muscle to downward gaze is greater in this position. ) Vertical diplopia, 2 visiual fields seperated • vertically. To compensate for this, patients learn to tilt the head forward (tuck the chin in) Alfred Bielschowsky's head tilt test is a test for palsy • of the superior oblique muscle. Torsional diplopia, Torsion is a normal response • to tilting the head sideways. torsional diplopia, in which two different visual fields, tilted with respect to each other, are seen at the same time.
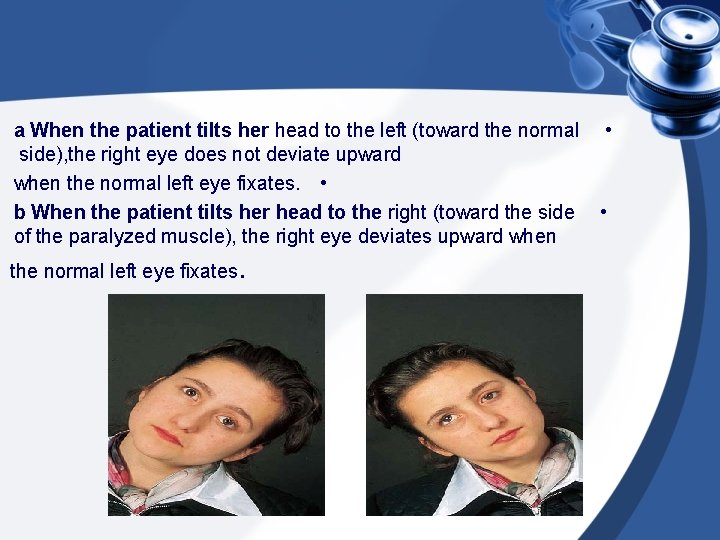
a When the patient tilts her head to the left (toward the normal side), the right eye does not deviate upward when the normal left eye fixates. • b When the patient tilts her head to the right (toward the side of the paralyzed muscle), the right eye deviates upward when the normal left eye fixates . • •
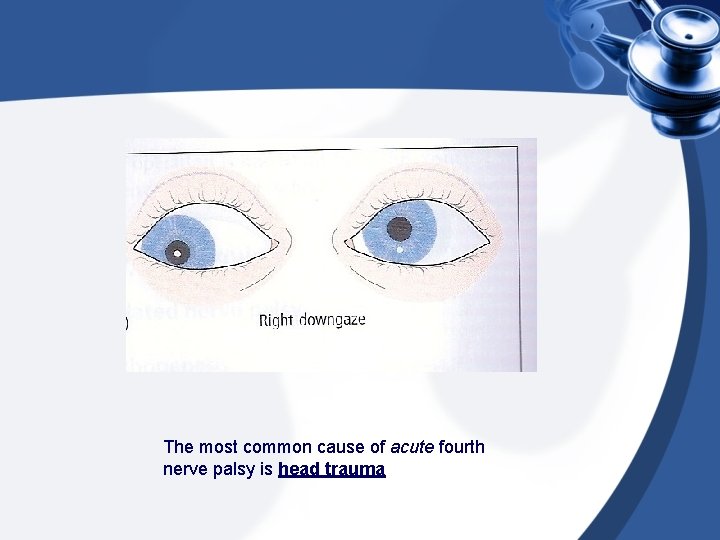
The most common cause of acute fourth nerve palsy is head trauma

6 th nerve palsy The affected individual will have an esotropia or • “convergent squint” on distance fixation. Happens usually unilaterally Horizontal Diplopia • children with the condition will develop amlyiopia. in the long term it can lead to a lack of appropriate development of the visual cortex giving rise to permanent visual loss unilateral abducens nerve palsy is the most common of the isolated ocular motor nerve palsies
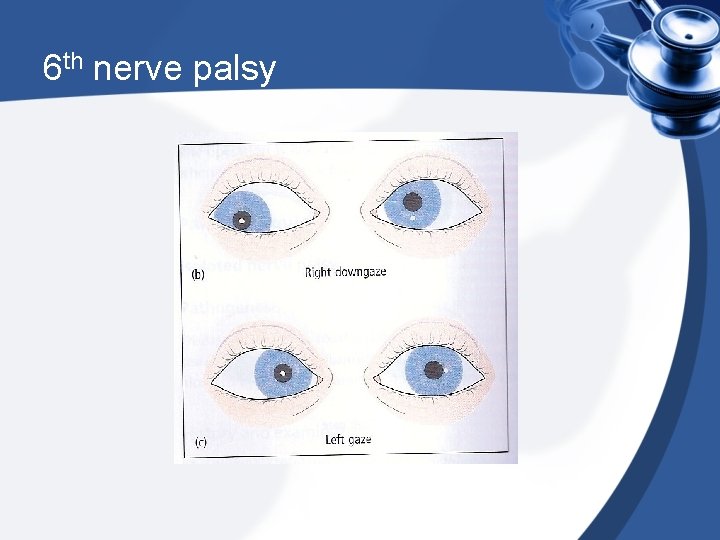
6 th nerve palsy

Consequences of strabismus • • 1) Amblyopia 2)decreased vision acuity 3)Loss of stereopsis 4)double vision

Amblyopia • Amblyopia is the medical term used when the vision in one of the eyes is reduced because the eye and the brain are not working together. Amblyopia is a developmental • problem in the brain, not an organic problem in the eye. The part of the brain corresponding to the visual system from the affected eye is not stimulated properly, and develops abnormally.

Amblyopia presentation : • Most cases are asymptomatic, which make it often goes undetected. In severe cases: poor depth perception may be found. poor spatial acuity , low sensitivity to contrast, reduced sensitivity to motion

Causes of amlyiopia 1 - congenital cataract. • 2 - refractive error. • • 3 - squint(strabismus) 4 -opacity in one eye. • 5 - congenital retinal detachment. Reversible before 7 -8 years •

Amblyopia secondary to suppression. Constant suppression in strabismus can • lead to severe amblyopia, especially in children below the age of six. The prospects for successful treatment decrease with age, and amblyopia becomes irreversible beyond the age of six to eight. Amblyopia only occurs in unilateral strabismus. In alternating strabismus, fixation or deviation alternates between both eyes so that both eyes learn to see.

Amblyopia • Treatment: – Correcting the optical deficit (wearing the necessary spectacle prescription) – Forcing use of the amblyopic eye, either by patching the good eye, or by instilling topical atropine in the eye with better vision
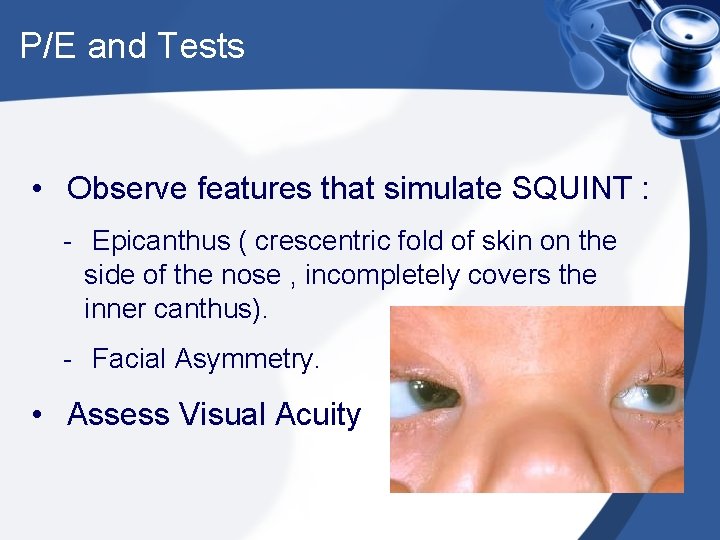
P/E and Tests • Observe features that simulate SQUINT : - Epicanthus ( crescentric fold of skin on the side of the nose , incompletely covers the inner canthus). - Facial Asymmetry. • Assess Visual Acuity

• Do corneal inspection • HIRSCHBURG TEST” • Perform Cover/Uncover Test to detect tropia. • ALTERNATING COVER/ UNCOVER TEST FOR HETEROPHORIA

Corneal inspection Have the patient look at the six cardinal positions of gaze to differentiate between concomitant and nonconcamitant
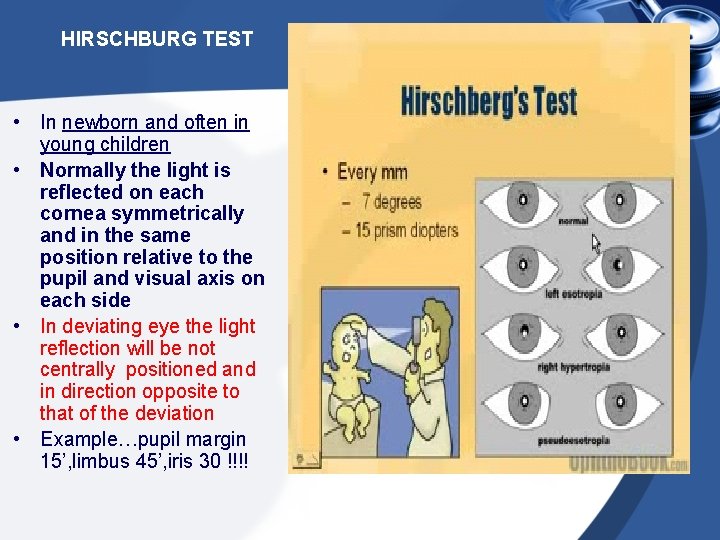
HIRSCHBURG TEST • In newborn and often in young children • Normally the light is reflected on each cornea symmetrically and in the same position relative to the pupil and visual axis on each side • In deviating eye the light reflection will be not centrally positioned and in direction opposite to that of the deviation • Example…pupil margin 15’, limbus 45’, iris 30 !!!!
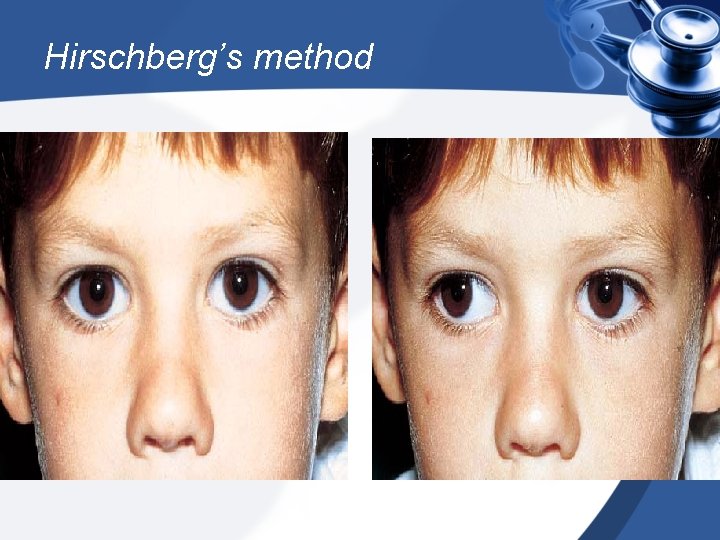
Hirschberg’s method

Cover/Uncover Test • Easy, requires no special equipment and detect almost every case of tropia • patients >6 yrs • patient look at the fixation point • Note which eye seems to be fixating • Cover it and observe the other • If it moves to pick up the fixation=>this eye was not directed toward the object of regard originally • Used to detect tropias • No shift on cover testing means there is no tropia

Alternate test • • In the alternate cover test, the occluder is moved to and front between the eyes. If the eye that has been uncovered moves, then there is a latent squint Used for detection of phroias


• So can you differentiate between heterophoria and heterotropia ? -meaning? - Test ?

Treatment • Early detection is the most important prognostic sign as it helps to prevent permanent visual deficits • Most children eventually recover from amblyopia by around age 10, if they have had the benefit of patches and corrective glasses • The primary therapeutic goal for those with strabismus is comfortable, single, clear, normal binocular vision at all distances and directions of gaze

Treatment is generally for children long-term. The duration may extend from the first months of life to the age of twelve. And the healing process depending also on the child personality and parent’s cooperate , and it’s treatable until 6 year , may be until 9 years but not more And we may divided the course of treatment into 3 phases Eyeglasses such in hyperopia a) c. Eyeglasses + Occlusion therapy to minimize amblyopia (better seeing eye is patched to try and stimulate the amblyopic eye thereby increasing its visual acuity) Surgery: Different muscles in the eye will be made stronger or weaker. • If the strabismus is not treated, the eye that the brain ignores will never see well. This loss of vision is called amblyopia. Another name for amblyopia is "lazy eye. " Sometimes amblyopia is present first, and it causes strabismus v For adult , surgery and it’s for cosmetic improvement.

• Glasses can treat some or all of the esotropia In farsighted and may decrease deviation in near sided with myopia

Treatment • Advanced strabismus is usually treated with a combination of eyeglasses or prisms, vision therapy, and surgery, depending on the underlying reason for the misalignment. – Glasses affect the position by changing the person's reaction to focusing. – Prisms change the way light, and therefore images, strike the eye, simulating a change in the eye position. – Surgery does not change the vision; it attempts to align the eyes by shortening, lengthening, or changing the position of one or more of the extraocular eye muscles and is frequently the only way to achieve cosmetic improvement.

Strabismus surgery • The principle of surgery is to realign the eyes by adjusting the position of the muscles on the globe or by shortening the muscle. • Access to the muscles is gained by making a small incision in the conjunctiva. • Moving the muscle insertion backwards on the globe (recession) • Weakens the muscle. • Removing a segment of the muscle (resection) strengthens the action

• It must be stressed that surgery is not an alternative to glasses and patching when amblyopia • In paralytic strabimus treatment is directed to underlying pathology • Diplopia can be helped by fitting prisms to the patients glasses


Prognosis • With early diagnosis and treatment, the problem can usually be corrected. 90% will have good vision & maintained if treated < 4 years old • Delayed treatment may lead to permanent vision loss in one eye. About one-third of children with strabismus will develop amblyopia. • After surgery, the eyes may look straight but vision problems can remain. • The child may still have reading problems in school, and for adults driving may be more difficult. Vision may affect the ability to play sports. • Because many children will get strabismus or amblyopia again, they need to be monitored closely
- Slides: 72