STOMACH AND DUODENUM Jawad R Alkharasani FCABS FICMS

STOMACH AND DUODENUM Jawad R Alkharasani FCABS FICMS FICS Consultant Gastrointestinal& Hepatobiliary Surgeon

Surgical treatment of Bleeding PU. Ø Indication: ü Continuous bleeding that demands massive blood transfusion. ü Failed endoscopic Rx. ü Rebleeding after endoscopic Rx.
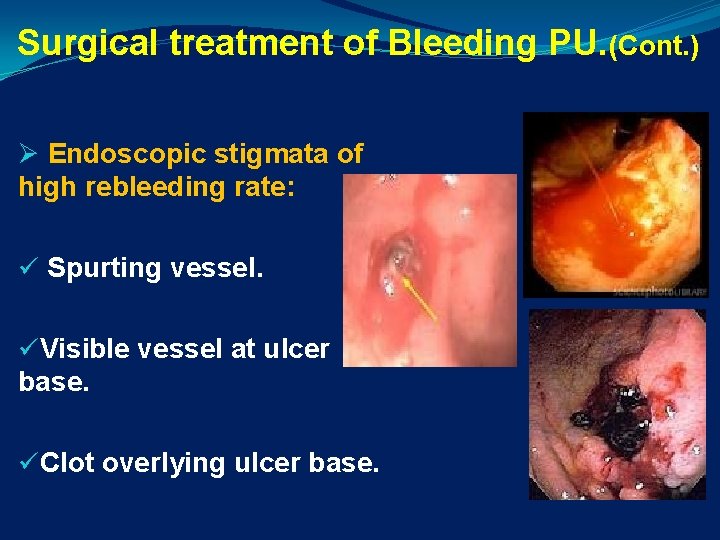
Surgical treatment of Bleeding PU. (Cont. ) Ø Endoscopic stigmata of high rebleeding rate: ü Spurting vessel. üVisible vessel at ulcer base. üClot overlying ulcer base.
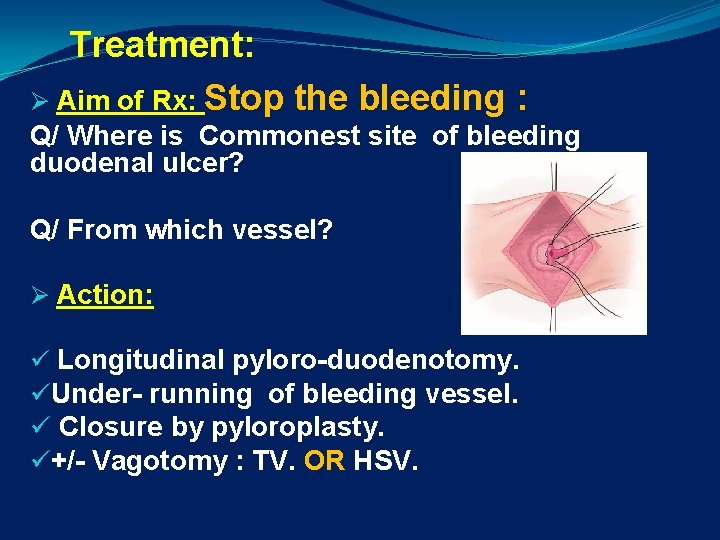
Treatment: Ø Aim of Rx: Stop the bleeding : Q/ Where is Commonest site of bleeding duodenal ulcer? Q/ From which vessel? Ø Action: ü Longitudinal pyloro-duodenotomy. üUnder- running of bleeding vessel. ü Closure by pyloroplasty. ü+/- Vagotomy : TV. OR HSV.
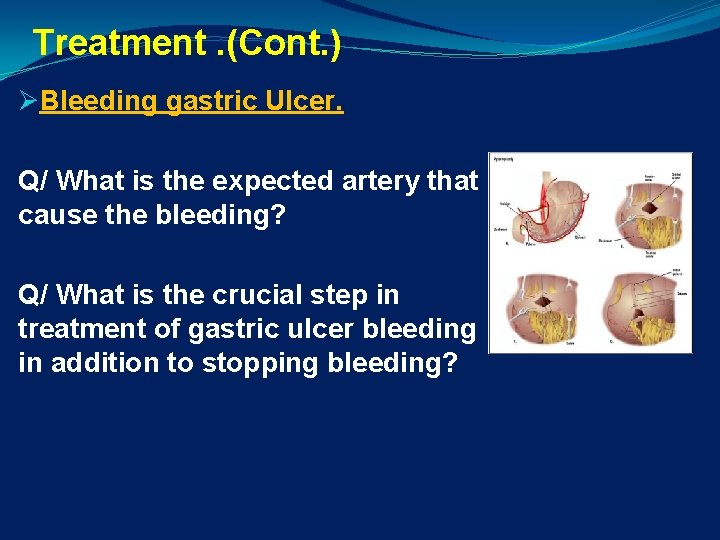
Treatment. (Cont. ) ØBleeding gastric Ulcer. Q/ What is the expected artery that cause the bleeding? Q/ What is the crucial step in treatment of gastric ulcer bleeding in addition to stopping bleeding?

Treatment. (Cont. ) ü Stress ulcer. ü Gastric erosion. ü Mallory-Weiss tear. Same principles of Rx. üDieulafoy’s disease: gastric arterial venous malformation. Rxed by local excision.

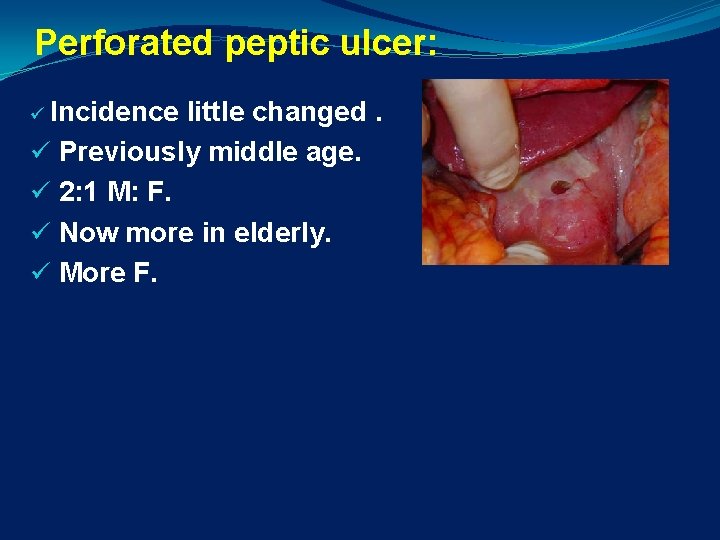
Perforated peptic ulcer: ü Incidence little changed. ü Previously middle age. ü 2: 1 M: F. ü Now more in elderly. ü More F.
Pathogenesis Q/ What is the commonest expected site of perforation of DU? Q/ What is the commonest expected site of perforation in GU?
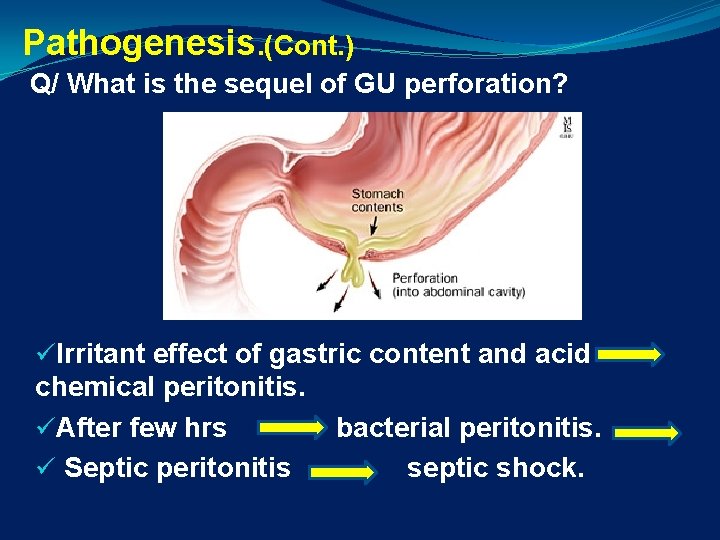
Pathogenesis. (Cont. ) Q/ What is the sequel of GU perforation? üIrritant effect of gastric content and acid chemical peritonitis. üAfter few hrs bacterial peritonitis. ü Septic peritonitis septic shock.
Pathogenesis. (Cont. ) Ø If only leak( small perforation): Q/ How it could mimic acute appendicitis? üThe fluid track down from epigastric through Rt paracolic gutter to Rt. iliac fossa. Q/ Is there any chance for the perforation to be self- limiting? üSome perforation will seal by inflammatory response and adhesion,

Clinical features ØSudden onset severe upper abdo. pain. Q/ What are other DDx? üThen became generalized. ü Hx of PU, NSAID ü Tachycardia or shock state. üFever (late) ü Restricted abdominal movement with respiration. ü Pointing sign (early). üSigns of peritoneal irritation: ü Tenderness, rebound, gaurdining or rigidity (board- like). ü -ve BS. ü Septic shock.
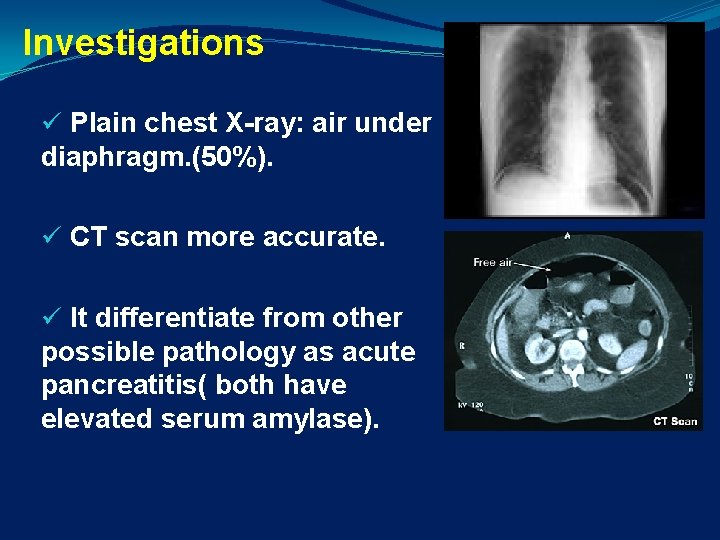
Investigations ü Plain chest X-ray: air under diaphragm. (50%). ü CT scan more accurate. ü It differentiate from other possible pathology as acute pancreatitis( both have elevated serum amylase).
Treatment • Admission, Resuscitation • IV fluid analgesia. • IV Antibiotics. • Opened surgery. OR • Laparoscopic surgery. • Duodenal perforation: • Closure over omental patch( Graham patch). • Through peritoneal toilet(wash) • NG tube. • Eradication of H. pylori.
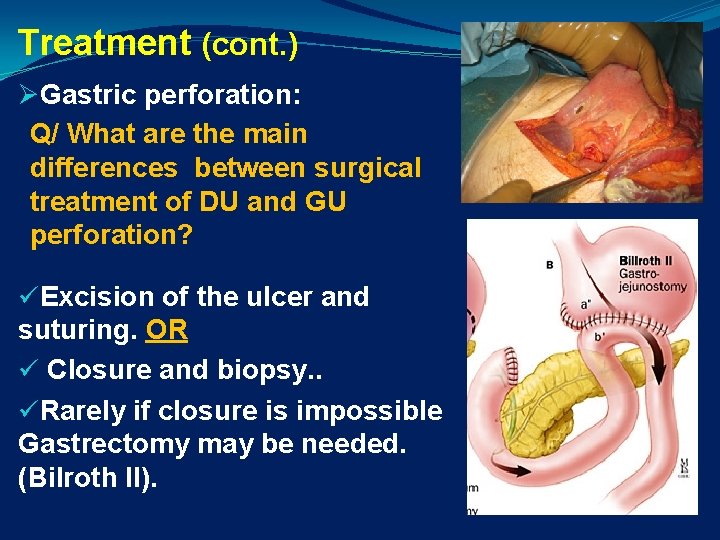
Treatment (cont. ) ØGastric perforation: Q/ What are the main differences between surgical treatment of DU and GU perforation? üExcision of the ulcer and suturing. OR ü Closure and biopsy. . üRarely if closure is impossible Gastrectomy may be needed. (Bilroth II).

Q/ What are common in surgical treatment of DU and GU perforation?

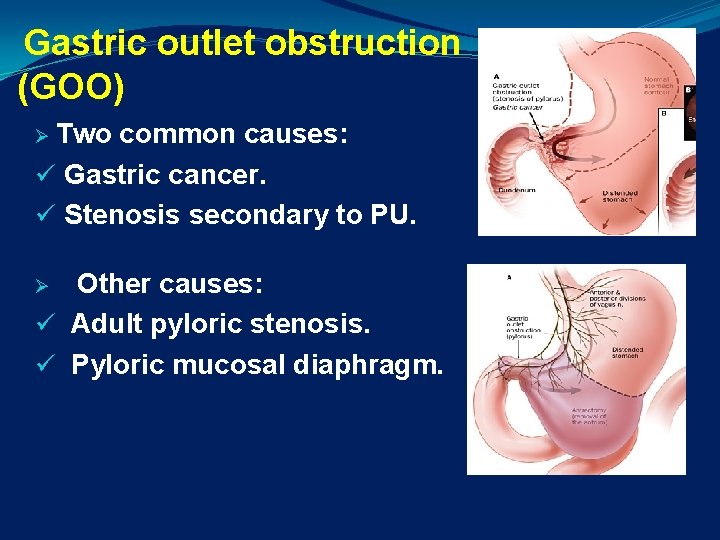
Gastric outlet obstruction (GOO) Ø Two common causes: ü Gastric cancer. ü Stenosis secondary to PU. Other causes: ü Adult pyloric stenosis. ü Pyloric mucosal diaphragm. Ø

Clinical features ü Benign GOO: ü Hx of chr. PU symptoms. ü Vomiting , no bile( if complete), üUndigested food of previous meal. ü Wt loss, un well. ü Dehydration. ü Distended abdomen. ü Succussion splash.

Clinical features (Cont. ). Metabolic effect: üHypochloremic alkalosis. ü Hyponatremia. ü Urine acid paradox. üHypokalemia. üAlkalosis lead to low ionized calcium, üTetany.

Management: Ø Main 2 steps: üCorrection of metabolic abnormality. ü Treating the mechanical obstruction.
Management: ØRehydration 0. 9% Nacl with k+ suplement. Ø Correction of associated anemia. Ø Decompression of stomach. N/GT. Ø Investigation by : üOGD + What and Why? ücontrast radiology. Ø Conservative Rx: ü In early case as the edema subside. ü Endoscopic balloon dilatation / risk. ?
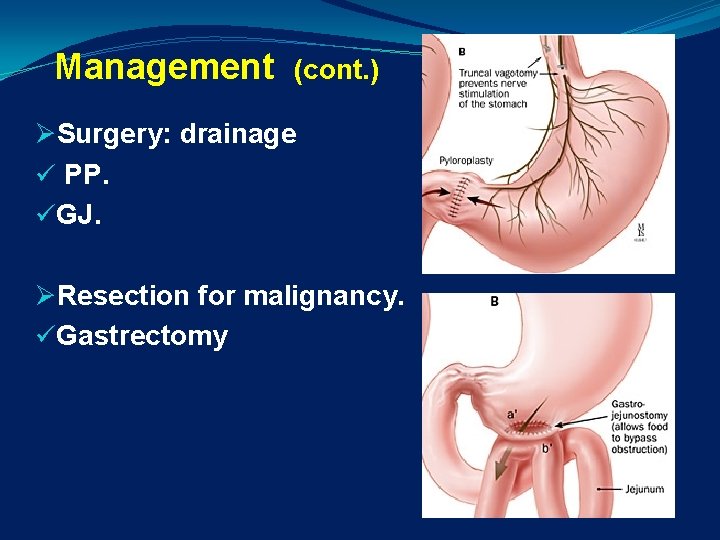
Management (cont. ) ØSurgery: drainage ü PP. üGJ. ØResection for malignancy. üGastrectomy
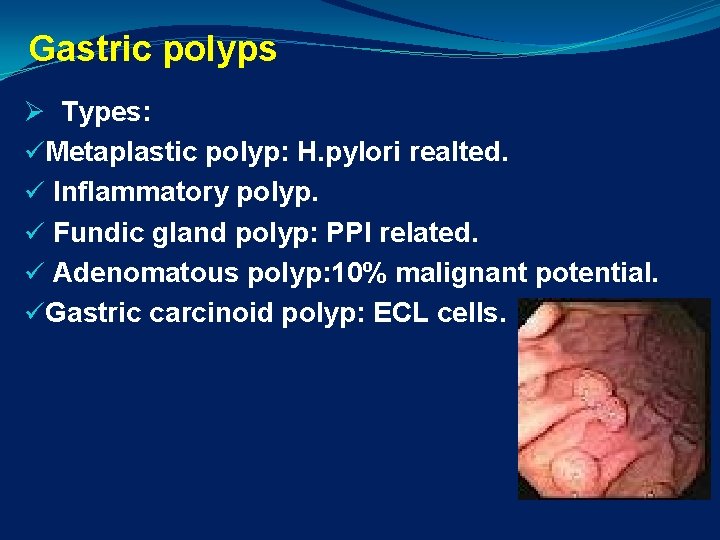
Gastric polyps Ø Types: üMetaplastic polyp: H. pylori realted. ü Inflammatory polyp. ü Fundic gland polyp: PPI related. ü Adenomatous polyp: 10% malignant potential. üGastric carcinoid polyp: ECL cells.
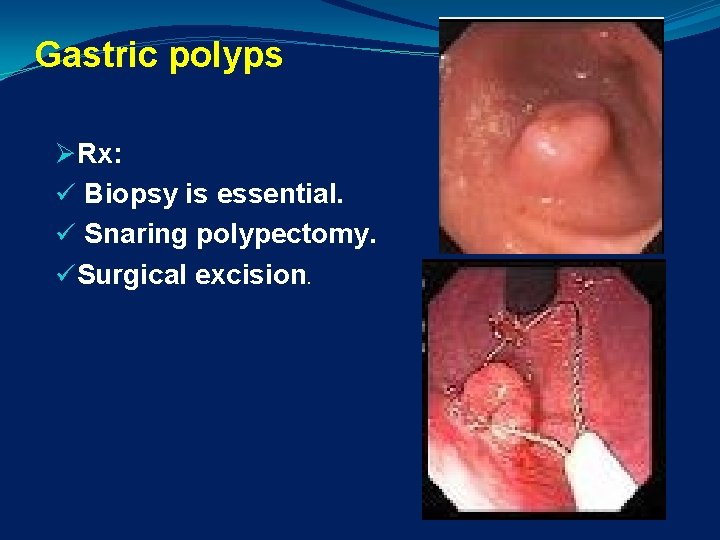
Gastric polyps ØRx: ü Biopsy is essential. ü Snaring polypectomy. üSurgical excision.

Gastric Cancer
- Slides: 26