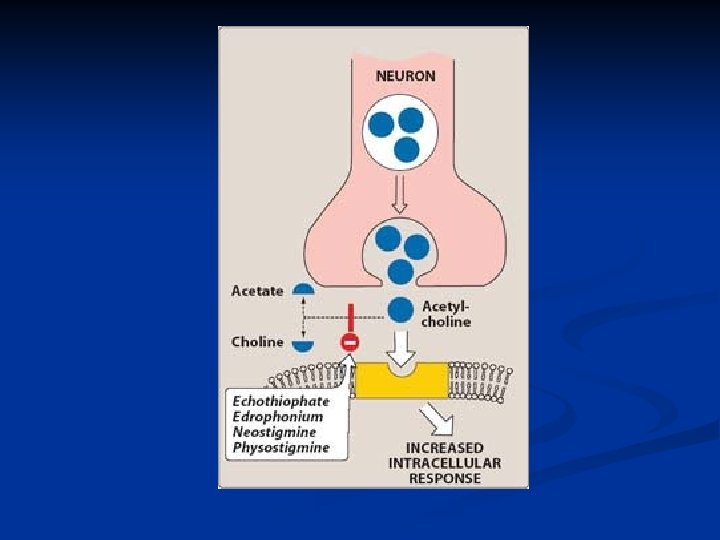
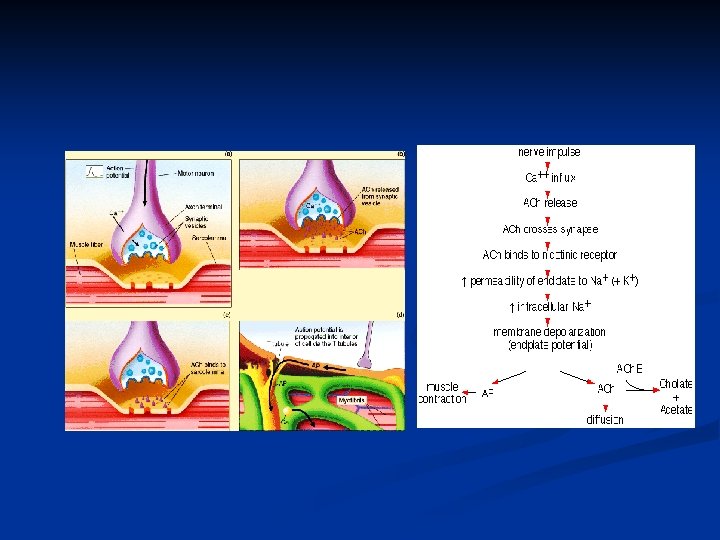
Steps of neurotransmission Steps of cholinergic neurotransmission Transduction




























- Slides: 53




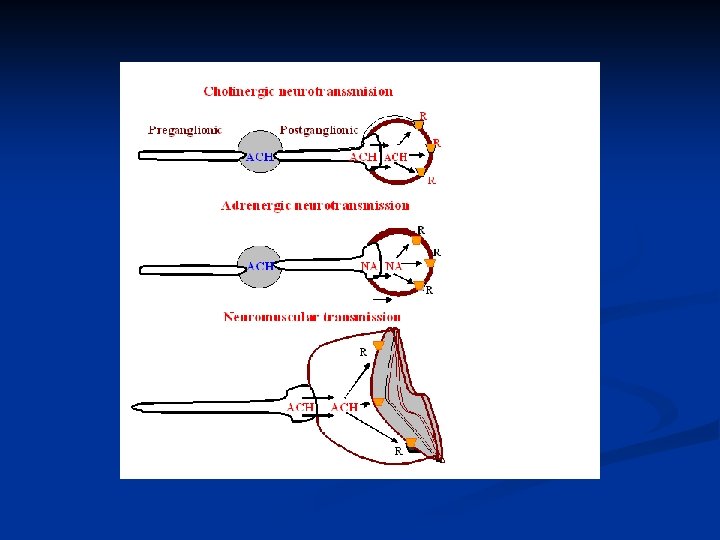
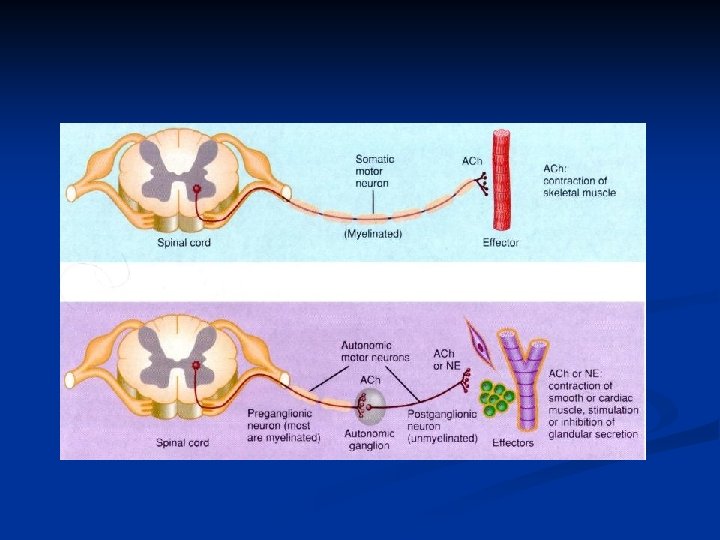
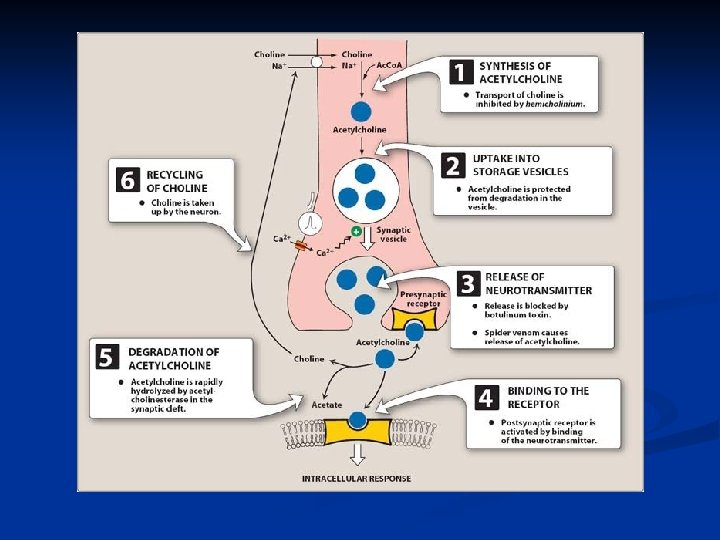
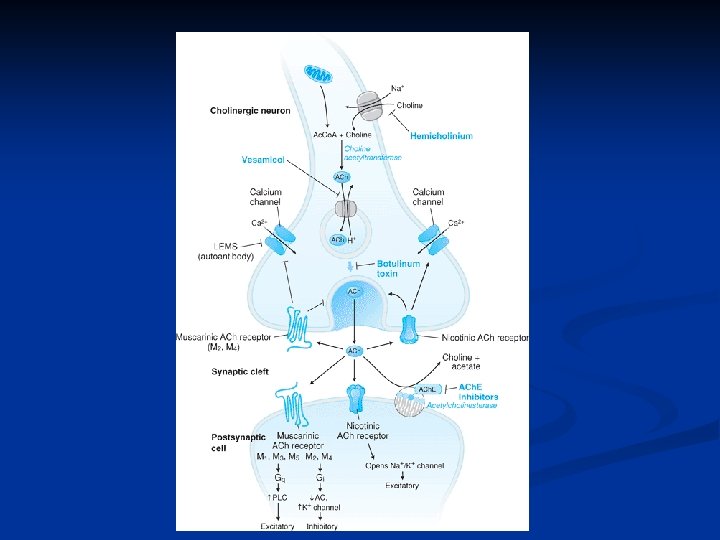
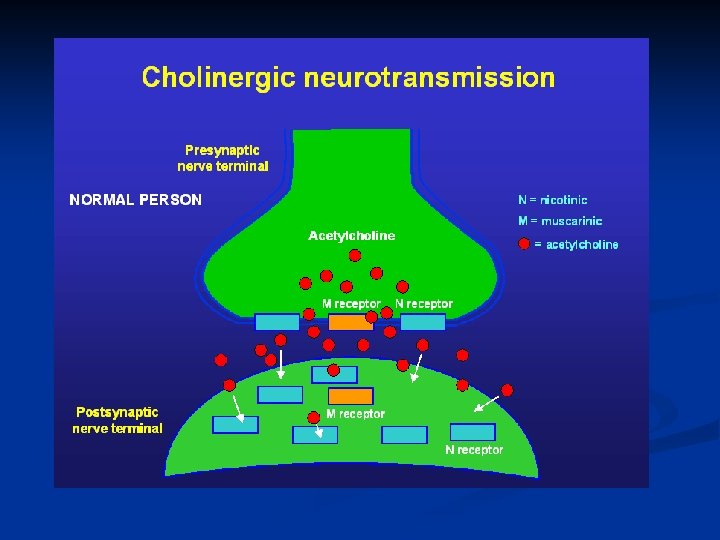
Steps of neurotransmission

Steps of cholinergic neurotransmission





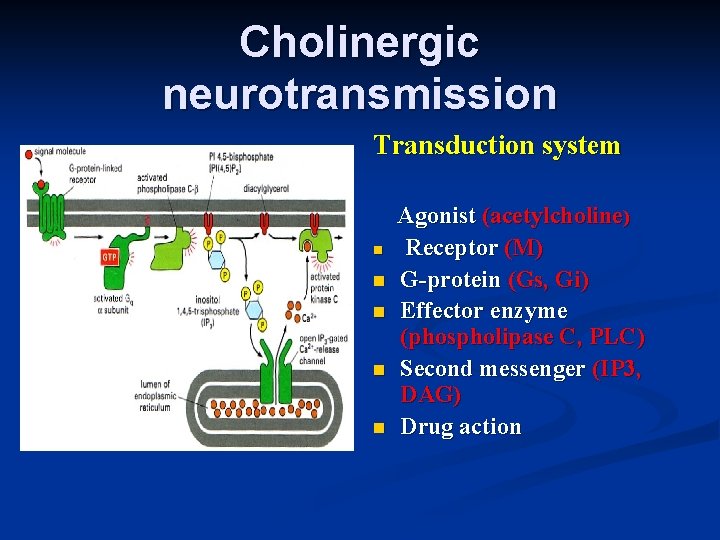
Transduction system

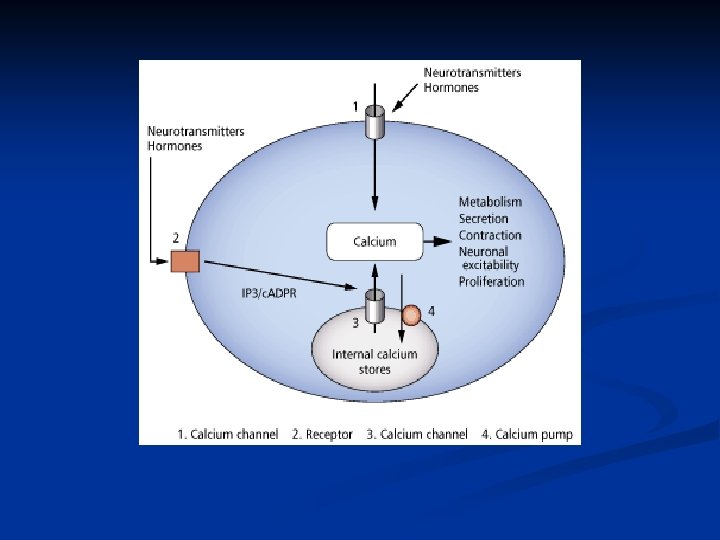
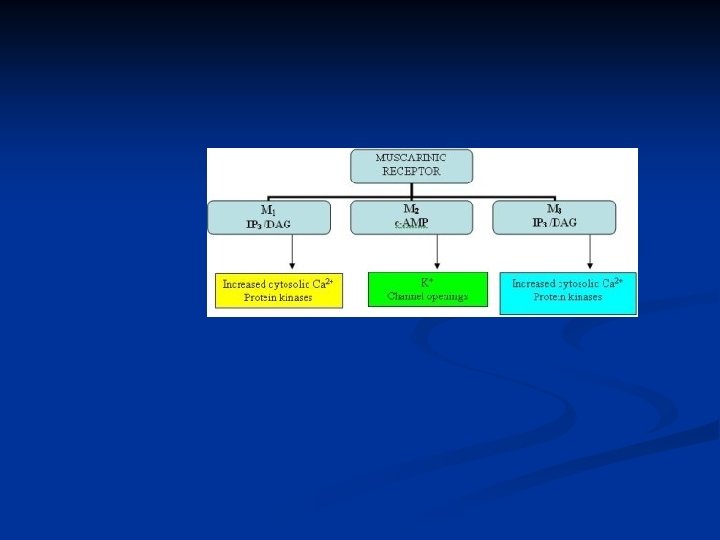
Cholinergic neurotransmission Transduction system n n n Agonist (acetylcholine) Receptor (M) G-protein (Gs, Gi) Effector enzyme (phospholipase C, PLC) Second messenger (IP 3, DAG) Drug action

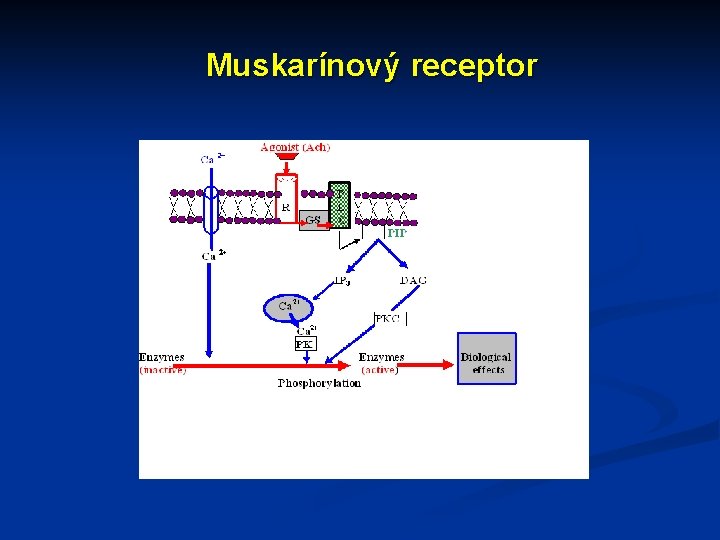
Muskarínový receptor


Interaction with receptors

n Receptors: - adrenergic: α - α 1, α 2 β – β 1, β 2 - cholinergic: M (M 1 -M-3) N

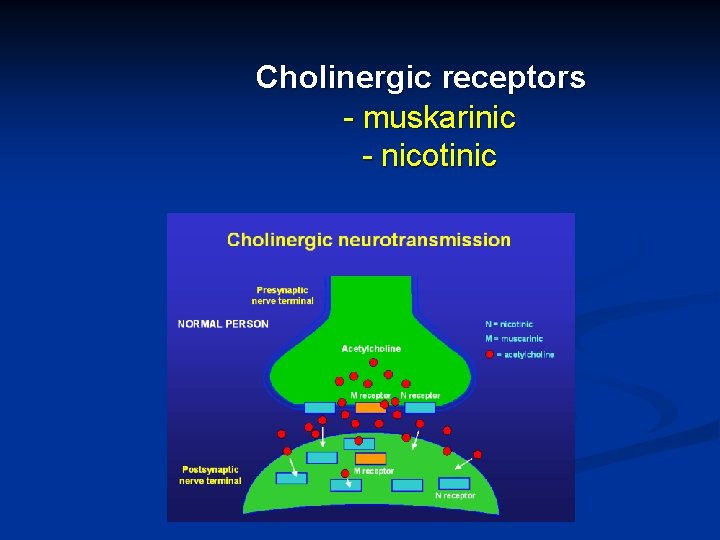
Cholinergic receptors - muskarinic - nicotinic

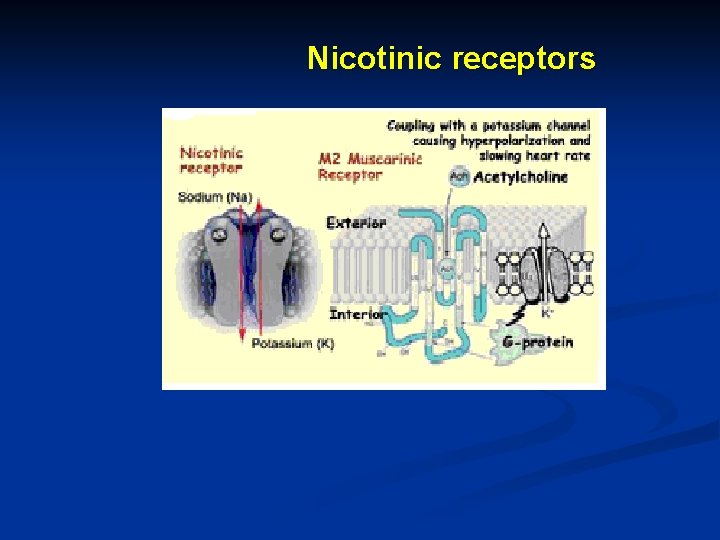
Nicotinic receptors

Nicotinic receptors Muscular typ Ganglionic typ CNS typ Localization Neuromuscular junction Vegetative ganglions Brain membrane effects Excitation increase of permeability for Na/K Excitation: increase of permeability for Ca++ agonists Acetylcholine Nicotine antagonists Tubocurarine Dimecamine Mecamylamíne Mecamylamine - conotoxine

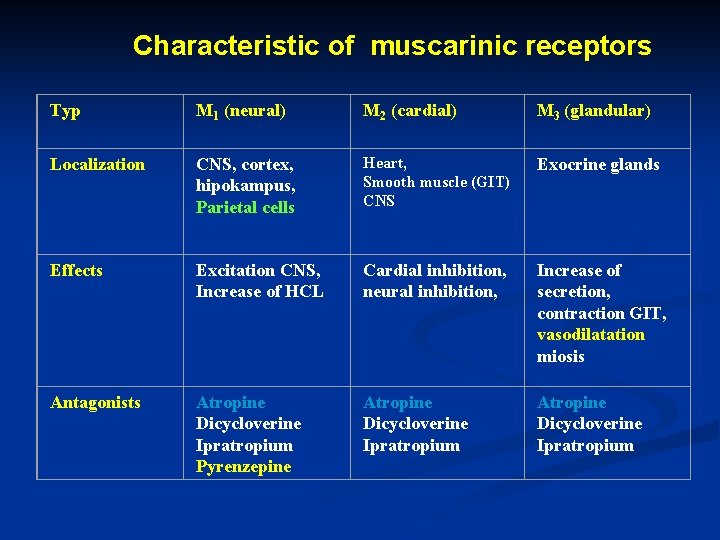
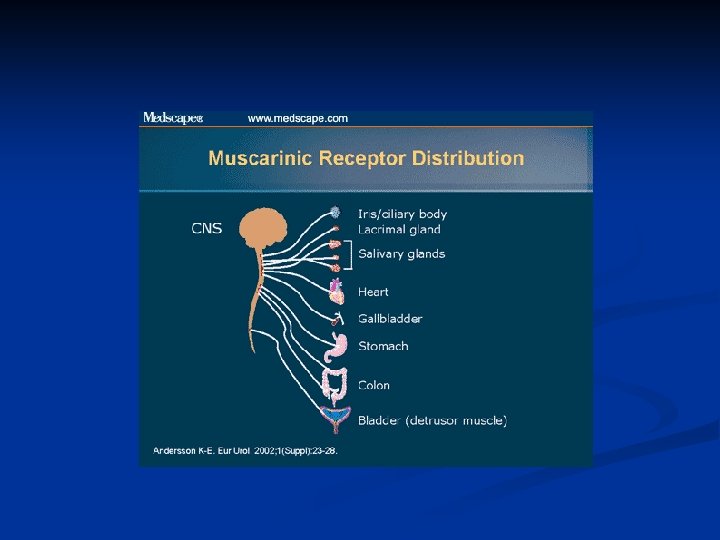
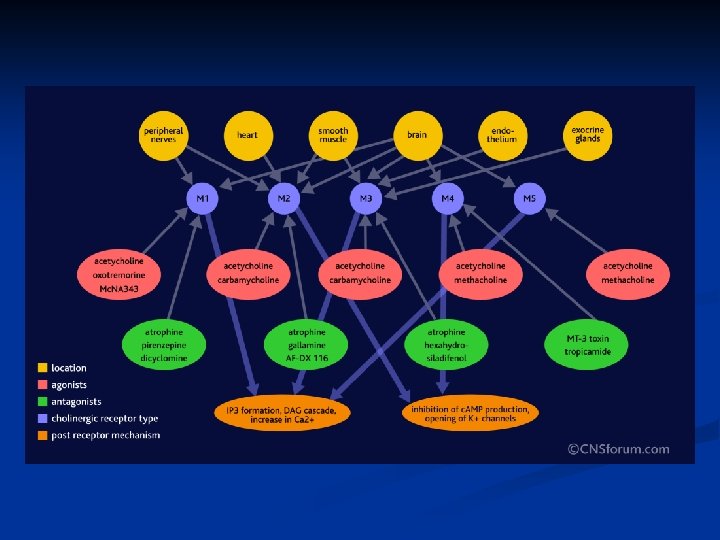
Characteristic of muscarinic receptors Typ M 1 (neural) M 2 (cardial) M 3 (glandular) Localization CNS, cortex, hipokampus, Parietal cells Heart, Smooth muscle (GIT) CNS Exocrine glands Effects Excitation CNS, Increase of HCL Cardial inhibition, neural inhibition, Increase of secretion, contraction GIT, vasodilatation miosis Antagonists Atropine Dicycloverine Ipratropium Pyrenzepine Atropine Dicycloverine Ipratropium





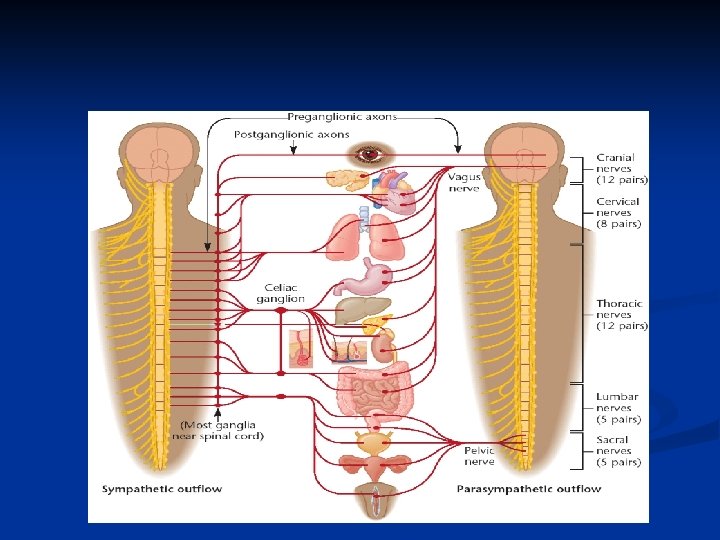
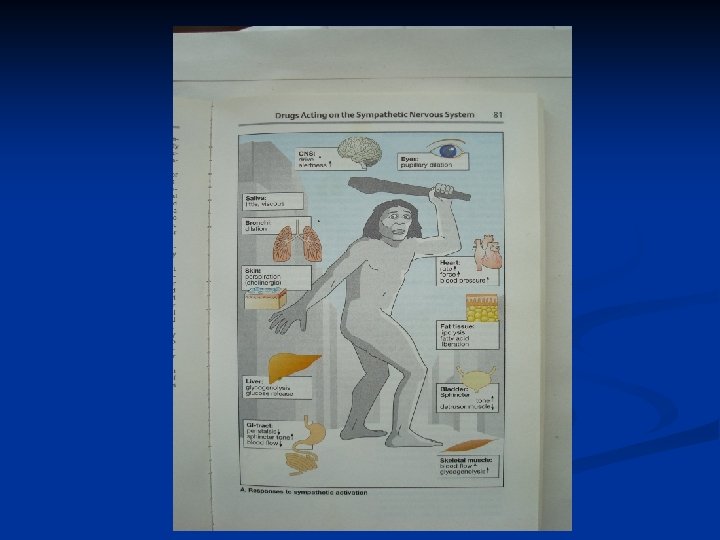
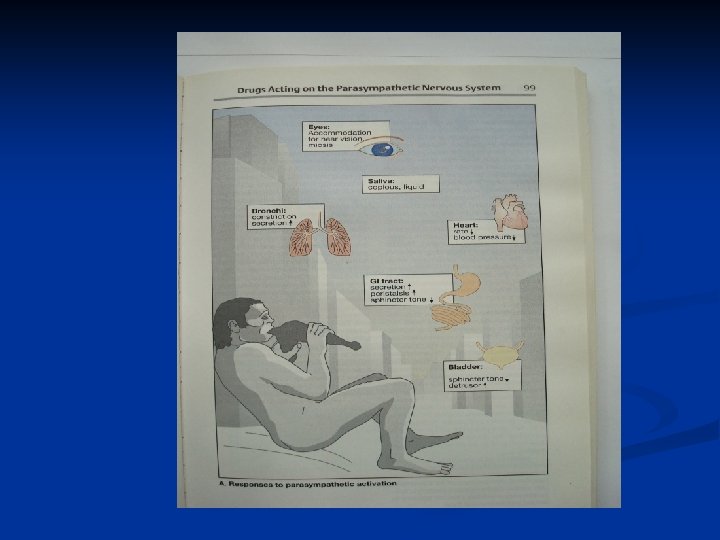
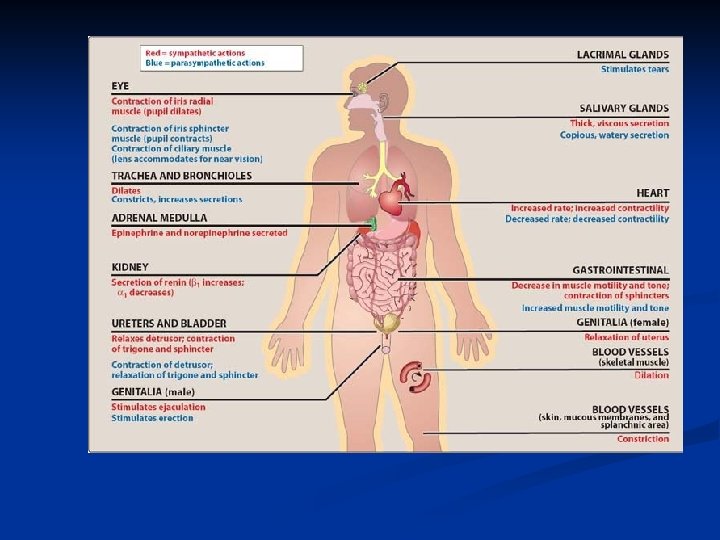
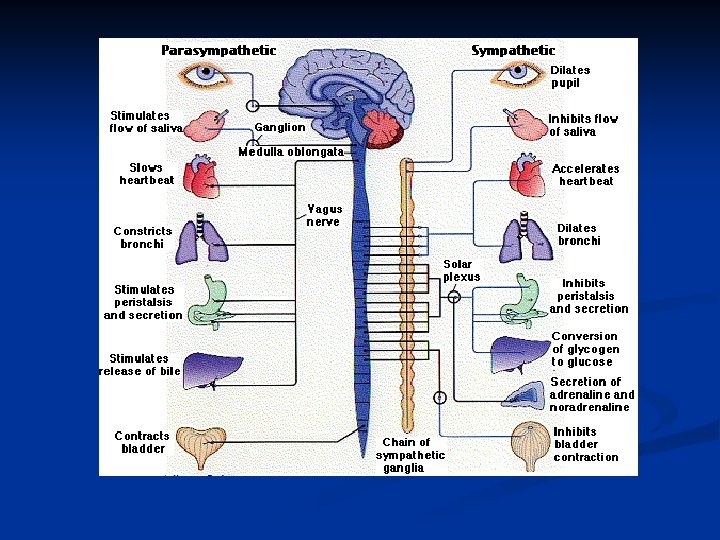
Functions of the autonomic nervous system 1. Sympathetic: activated in response to stressful situations ( fear, hypoglycemia, cold, or exercise). I "fight or 2. Parasympathetic system Dominant over the sympathetic system in flight "rest or digest" situations.






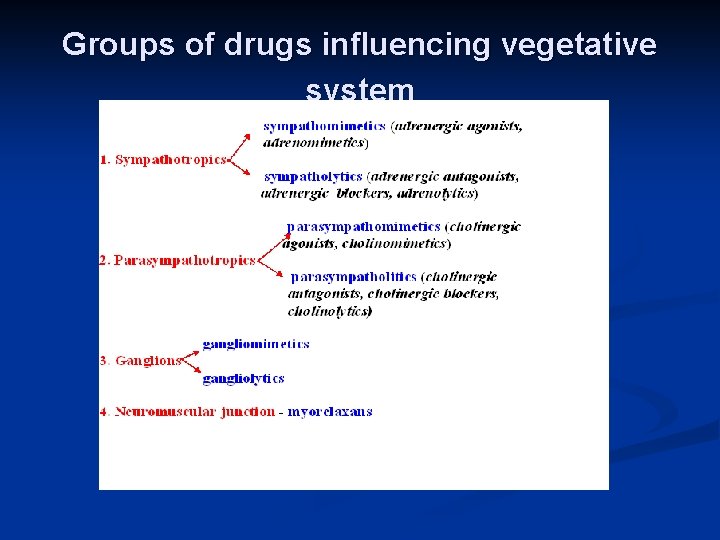
Groups of drugs influencing vegetative system

Muscarinic agonists Parasympathomimetics Representative: acetylcholine

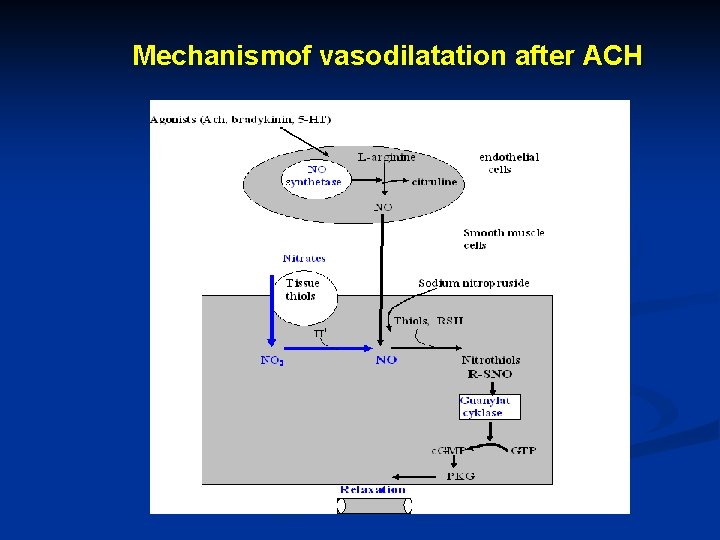
Effects of parasympathomimetics Cardiovascular effets (M 2): cardiac slowing and (reduced automaticity) decreased force of contraction (mainly in atria) inhibition of AV conduction Smooth muscle (except vascular smooth muscle contracts in response to muscarinic agonists peristaltic activity of GIT increase bladder and bronchial smooth muscle also contract Vascular smooth muscle acetylcholine produces vasodilatation - mediator is NO Exocrinne glands stimulation of gastric acid secretion (M 1) sweating, lacrimation, salivation, bronchial secretion (M 3) Effects on eye lower the intraocular pressure, myosis

Mechanismof vasodilatation after ACH

Groups of parasympathomimetics Directly acting a. Acetylcholine - rapid destruction nonselective effect (M and N) b. More stable derivates of Ach: Metacholine, Betanechol, Carbachol c. Alkaloids: muscarine (Amanita muscaria), pilocarpine (Pilocarpus jaborandi) They have no significant nicotinic effect muscarine - toxicologic interest only n Indirectly acting Reversible anticholinesterases - short-acting drugs (edrophonium, ambenonium) - medium-duration anticholinesterases (neostigmine, pyridostigmine, physostigmine) a. b. Irreversible anticholinesterases (organophosphates) tabun, sarin. soman pesticides, as well as war gases: -are usually high lipid-soluble compounds and are rapidly absorbed through mucous membrane, unbroken skin


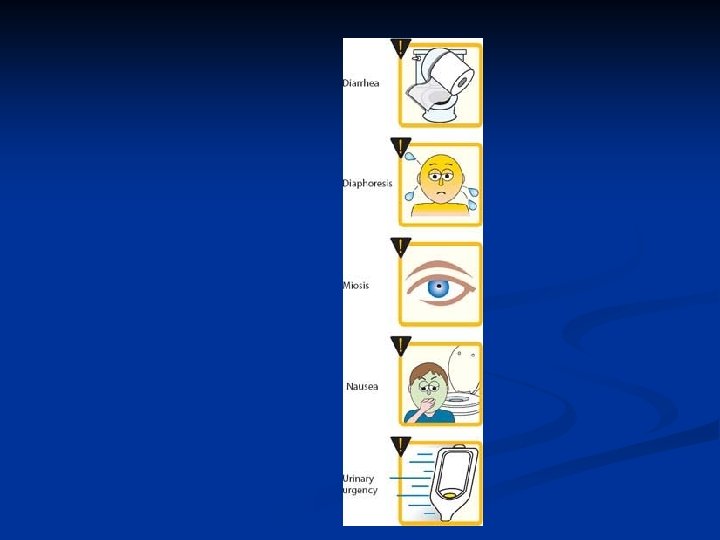
Clinical uses and side effects of parasympathomimetics Clinical uses myasthenia gravis (neostigmine, pyridostigmine, ) glaucoma (physostigmine), antidote - in atropine poisoning (physostigmine) - in curare-like drug-induced muscle paralysis (neostigmine), urinary tract stimulant (neostigmine) GIT postoperative abdominal distension (neostigmine) n - Side effects flush, - salivation, - nausea, vomiting, -diarrhea, hypotension – bronchoconstriction - asthmatic attack


Intoxication by organophosphates Symptoms a. Effects on autonomic cholinergic synapses (M) Glands, GIT, bronchoconstriction Bradycardia, hypotension, disturbancies in vision b. Effects on the neuromuscular junction (N) Muscle contraction, in large doses (poisoning) depolarisation of membrane n neuromuscular block c. Effects on the CNS Excitation, - convulsion - depresion - respiratory failure Treatment 1. first step - remove the source to prevent further exposure, 2. most muscarinic symptoms are blocked by atropine, 3. to restore acetylcholinesterase activity oximes pralidoxime, trimedoxime, obidoxime.

Muscarinic antagonists (parasympatholitics) Representative: atropine

Atroppa belladona

Groups of muscarinic antagonists (parasympatholitics) Tertiary ammonium compounds: 1. - Alkaloids - atropine and scopolamine, atropine - (Atropa belladonna), scopolamine (Datura stramonium) Semisynthetic derivate of atropine - homatrapine - - Selective M 1 - pirenzepine and dicyclomine benztropine and trihexyphenidyl – (CNS- antiparkinsonic drugs) Quarternary synthetic deivates of atropine - Atropine methonitrate - peripheraly very similar to atropine but it dos not cross blood-brain barrier lacks central actions Propantheline - methscopolamine, ipratropium 2.

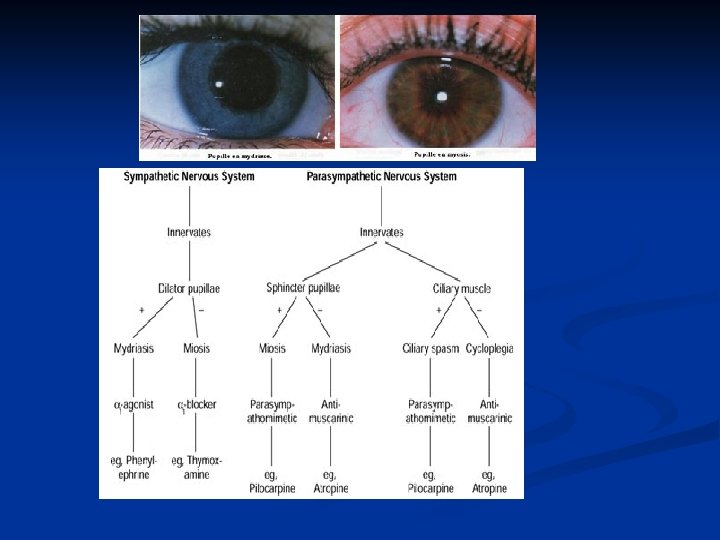
Effects of muscarinic antagonists n n n n n Inhibition of secretion Effects on heart rate Effects on the eye – mydriasis, paralysis of accomodation, cycloplegia) disturbances of near vision, -intraocular pressure may rise Effects on the GIT – inhibition of motility Effects on other smooth muscle -bronchial, biliary and urinary tract smooth muscle are all relaxed Effects on CNS -atropine produced mainly excitatory effects on CNS (low doses - mild restlessness

Clinical uses of muscarinic antagonists n n n Premedication for anesthesia -inhibition of bronchial and salivary secretion, inhibition of reflex bronchoconstriction -reduced bradycardia after some anesthetics GI disorders - to reduce gastric acid secretion (pirenzepine), to reduce gastrointestinal motility (dicyclomine) Ophthalmology -pupilary dilatation - homatropine is often

Clinical uses of muscarinic antagonists (cont. ) Bronchial disorders - ipratropium bromide is useful in treatment of asthma n Motion sickness - scopolamine is used in preventing motion sickness n Other - Parkinson´s disease (benztropine), antidote, diarrhea n

Side effects Atropine like effect -blurred vision, -tachycardia, -dry mouth, -constipation, -urinary retention, -mydriasis

Atropine poisoning mainly in youg children who eat deadly nightshade berries excitement and irritability hyperactivity and rise body temperature result of blocking muscarinic receptors in the brain they are opposed by anticholinesterase drugs (physostigmine)

Myorelaxants


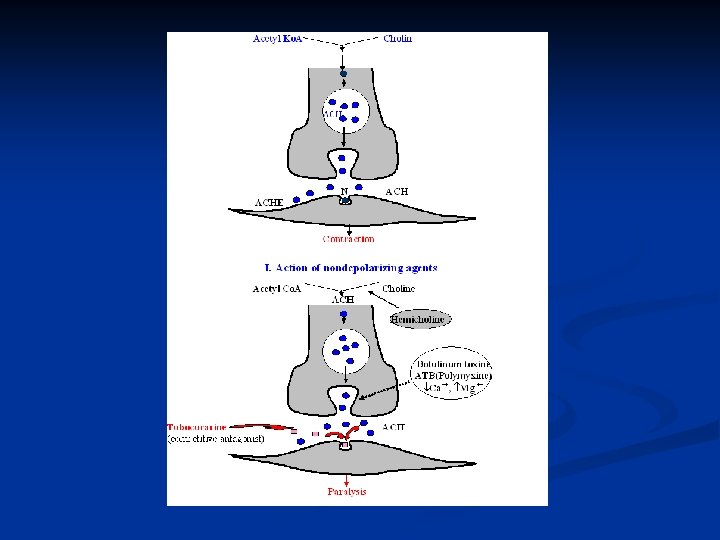
Classification of myorelaxants n I. drugs that act presynaptically by inhibiting of ACH synthesis: hemicholinium by inhibiting ACH release: botulinum toxin, bungarotoxin (venom of various snakes (cobra family) by inhibiting of calcium entry (magnesium ion, aminoglycoside ATB), n n II. drugs that act postsynaptically interfering with the postsynaptic action of ACH: non-depolarising agents tubocurarine, pancuronium, gallamine depolarising agents succinylcholine n


Non-depolarising agents - tubocurarine n Effects n n n Paralysis small muscles of the face and eye are paralyzed first, limb, neck and trunk then intercostal muscles are affected diaphragm muscles. Other effects - release of histamine vasodilatation fall in blood pressure, - bronchospasm consequence of histamine release ��� asthma, - neuromuscular blockade last from 20 min to 1 hour.

Non-depolarising agents – tubocurarine (cont. ) Terapeutic uses are used therapeutically as adjuvant in surgical anesthesia, strychnine intoxication, tetanus, diagnosis of myasthenia gravis, adjunct relaxation during maximal electroshock therapy.

Depolarizing agents succinylcholine n Effects muscular fasciculation last only a few minutes (3 – 5 min), paralysis is slightly different than in non-depolarising drugs, but paralysis of respiratory muscles is the last, does not produce ganglionic block, has weak histamine-releasing action, Unwanted effects � bradycardia � increased intraocular pressure � prolonged paralysis by genetic differences of cholinesterase activity � malignat hyperthermia - sudden rise in body temperature usually treated by dantrolene (prevention of calcium release from sarcoplasmatic reticulum) + rapid cooling